Abstract
Purpose
To explore the disease burden of early-onset colorectal cancer (EO-CRC) in individuals aged 40–49 years and provide baseline evidence for routine recommended age adjustment for CRC screening and other clinical decision-making.
Methods
We collected data stratified by sex, risk factors, and socio-demographic index (SDI) from the Global Burden of Disease Study 2019 Data Resources. Trends in disease burden were analyzed by estimated annual percentage change. The Bayesian age-period-cohort model predicted the burden over the following 10 years.
Results
In 2019, the global rates of incidence, mortality, prevalence, and disability-adjusted life year (DALY) of EO-CRC in people aged 40–44 years were 11.48 (95% uncertainty interval: 10.50–12.59), 4.35 (4.01–4.70), 72.63 (66.48–79.52), 209.82 (193.55–226.59) per 100,000 population. For people aged 45–49 years, the rates of these four estimates were 19.63 (17.97–21.54), 7.76 (7.16–8.41), 121.73 (110.99–133.84), and 335.83 (310.14–362.91), respectively. The incidence and prevalence rates for both age groups increased while the mortality and DALY rates remained stable from 1990 to 2019. In 2019, high-income North America had the highest incidence and prevalence rates. A low milk diet accounted for the largest proportion of global DALYs in EO-CRC, and there was a tendency for the DALY rate first to increase and then decrease with increasing SDI. The incidence and mortality rates were predicted to increase in the next 10 years.
Conclusion
The current and future burden of EO-CRC among people aged 40–49 years is heavy. Substantial variation exists in disease burden across regions and countries. Urgent screening actions and policies are needed.





Similar content being viewed by others
Data availability
The datasets analysed during the current study are available at the https://ghdx.healthdata.org/.
References
Akimoto N, Ugai T, Zhong R, Hamada T, Fujiyoshi K, Giannakis M et al (2021) Rising incidence of early-onset colorectal cancer—a call to action. Nat Rev Clin Oncol 18:230–243. https://doi.org/10.1038/s41571-020-00445-1
Alyabsi M, Algarni M, Alshammari K (2021) Trends in colorectal cancer incidence rates in Saudi Arabia (2001–2016) using Saudi national registry: early-versus late-onset disease. Front Oncol 11:730689. https://doi.org/10.3389/fonc.2021.730689
Araghi M, Soerjomataram I, Bardot A, Ferlay J, Cabasag CJ, Morrison DS et al (2019) Changes in colorectal cancer incidence in seven high-income countries: a population-based study. Lancet Gastroenterol Hepatol 4:511–518. https://doi.org/10.1016/s2468-1253(19)30147-5
Bailey CE, Hu CY, You YN, Bednarski BK, Rodriguez-Bigas MA, Skibber JM et al (2015) Increasing disparities in the age-related incidences of colon and rectal cancers in the United States, 1975–2010. JAMA Surg 150:17–22. https://doi.org/10.1001/jamasurg.2014.1756
Burnett-Hartman AN, Lee JK, Demb J, Gupta S (2021) An update on the epidemiology, molecular characterization, diagnosis, and screening strategies for early-onset colorectal cancer. Gastroenterology 160:1041–1049. https://doi.org/10.1053/j.gastro.2020.12.068
Butterly LF, Siegel RL, Fedewa S, Robinson CM, Jemal A, Anderson JC (2021) Colonoscopy outcomes in average-risk screening equivalent young adults: data from the new hampshire colonoscopy registry. Am J Gastroenterol 116:171–179. https://doi.org/10.14309/ajg.0000000000000820
Du Z, Chen W, Xia Q, Shi O, Chen Q (2020) Trends and projections of kidney cancer incidence at the global and national levels, 1990–2030: a Bayesian age-period-cohort modeling study. Biomark Res 8:16. https://doi.org/10.1186/s40364-020-00195-3
Ferlay J, Colombet M, Soerjomataram I, Mathers C, Parkin DM, Piñeros M et al (2019) Estimating the global cancer incidence and mortality in 2018: GLOBOCAN sources and methods. Int J Cancer 144:1941–1953. https://doi.org/10.1002/ijc.31937
Gausman V, Dornblaser D, Anand S, Hayes RB, O’Connell K, Du M et al (2020) Risk factors associated with early-onset colorectal cancer. Clin Gastroenterol Hepatol 18:2752–59.e2. https://doi.org/10.1016/j.cgh.2019.10.009
GBD 2016 Dementia Collaborators (2019) Global, regional, and national burden of Alzheimer’s disease and other dementias, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol 18:88–106. https://doi.org/10.1016/s1474-4422(18)30403-4
GBD 2019 Colorectal Cancer Collaborators (2022) Global, regional, and national burden of colorectal cancer and its risk factors, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet Gastroenterol Hepatol 7:627–647. https://doi.org/10.1016/s2468-1253(22)00044-9
GBD 2019 Demographics Collaborators (2020) Global age-sex-specific fertility, mortality, healthy life expectancy (HALE), and population estimates in 204 countries and territories, 1950–2019: a comprehensive demographic analysis for the Global Burden of Disease Study 2019. Lancet 396:1160–1203. https://doi.org/10.1016/s0140-6736(20)30977-6
GBD 2019 Diseases and Injuries Collaborators (2020) Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396:1204–1222. https://doi.org/10.1016/s0140-6736(20)30925-9
GBD 2019 Risk Factors Collaborators (2020) Global burden of 87 risk factors in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet 396:1223–1249. https://doi.org/10.1016/s0140-6736(20)30752-2
Hu W, Fang L, Zhang H, Ni R, Pan G (2022a) Global disease burden of COPD from 1990 to 2019 and prediction of future disease burden trend in China. Public Health 208:89–97. https://doi.org/10.1016/j.puhe.2022.04.015
Hu Y, Tong Z, Huang X, Qin JJ, Lin L, Lei F et al (2022b) The projections of global and regional rheumatic heart disease burden from 2020 to 2030. Front Cardiovasc Med 9:941917. https://doi.org/10.3389/fcvm.2022.941917
Jung YS, Ryu S, Chang Y, Yun KE, Park JH, Kim HJ et al (2015) Risk factors for colorectal neoplasia in persons aged 30 to 39 years and 40 to 49 years. Gastrointest Endosc 81:637–645. https://doi.org/10.1016/j.gie.2014.09.031. (e7)
Khan NA, Hussain M, ur Rahman A, Farooqui WA, Rasheed A, Memon AS (2015) Dietary practices, addictive behavior and bowel habits and risk of early onset colorectal cancer: a case control study. Asian Pac J Cancer Prev 16:7967–7973. https://doi.org/10.7314/apjcp.2015.16.17.7967
Kim JY, Jung YS, Park JH, Kim HJ, Cho YK, Sohn CI et al (2016) Different risk factors for advanced colorectal neoplasm in young adults. World J Gastroenterol 22:3611–3620. https://doi.org/10.3748/wjg.v22.i13.3611
Knoll M, Furkel J, Debus J, Abdollahi A, Karch A, Stock C (2020) An R package for an integrated evaluation of statistical approaches to cancer incidence projection. BMC Med Res Methodol 20:257. https://doi.org/10.1186/s12874-020-01133-5
Kolb JM, Hu J, DeSanto K, Gao D, Singh S, Imperiale T et al (2021) Early-age onset colorectal neoplasia in average-risk individuals undergoing screening colonoscopy: a systematic review and meta-analysis. Gastroenterology 161:1145–1155. https://doi.org/10.1053/j.gastro.2021.06.006. (e12)
Kong C, Liang L, Liu G, Du L, Yang Y, Liu J et al (2022) Integrated metagenomic and metabolomic analysis reveals distinct gut-microbiome-derived phenotypes in early-onset colorectal cancer. Gut. https://doi.org/10.1136/gutjnl-2022-327156
Liu PH, Wu K, Ng K, Zauber AG, Nguyen LH, Song M et al (2019a) Association of obesity with risk of early-onset colorectal cancer among women. JAMA Oncol 5:37–44. https://doi.org/10.1001/jamaoncol.2018.4280
Liu W, Liu J, Song Y, Zeng X, Wang X, Mi L et al (2019b) Burden of lymphoma in China, 2006–2016: an analysis of the Global Burden of Disease Study 2016. J Hematol Oncol 12:115. https://doi.org/10.1186/s13045-019-0785-7
Low EE, Demb J, Liu L, Earles A, Bustamante R, Williams CD et al (2020) Risk factors for early-onset colorectal cancer. Gastroenterology 159:492–501. https://doi.org/10.1053/j.gastro.2020.01.004. (e7)
Mehta RS, Song M, Nishihara R, Drew DA, Wu K, Qian ZR et al (2017) Dietary patterns and risk of colorectal cancer: analysis by tumor location and molecular subtypes. Gastroenterology 152:1944–53.e1. https://doi.org/10.1053/j.gastro.2017.02.015
Montminy EM, Zhou M, Maniscalco L, Abualkhair W, Kim MK, Siegel RL et al (2021) Contributions of adenocarcinoma and carcinoid tumors to early-onset colorectal cancer incidence rates in the United States. Ann Intern Med 174:157–166. https://doi.org/10.7326/m20-0068
Ou Y, Long Y, Ji L, Zhan Y, Qiao T, Wang X et al (2022) Trends in disease burden of chronic lymphocytic leukemia at the global, regional, and national levels from 1990 to 2019, and projections until 2030: a population-based epidemiologic study. Front Oncol 12:840616. https://doi.org/10.3389/fonc.2022.840616
Pan H, Zhao Z, Deng Y, Zheng Z, Huang Y, Huang S et al (2022) The global, regional, and national early-onset colorectal cancer burden and trends from 1990 to 2019: results from the Global Burden of Disease Study 2019. BMC Public Health 22:1896. https://doi.org/10.1186/s12889-022-14274-7
Patel SG, Karlitz JJ, Yen T, Lieu CH, Boland CR (2022) The rising tide of early-onset colorectal cancer: a comprehensive review of epidemiology, clinical features, biology, risk factors, prevention, and early detection. Lancet Gastroenterol Hepatol 7:262–274. https://doi.org/10.1016/s2468-1253(21)00426-x
Riebler A, Held L (2017) Projecting the future burden of cancer: bayesian age-period-cohort analysis with integrated nested Laplace approximations. Biom J 59:531–549. https://doi.org/10.1002/bimj.201500263
Rosato V, Bosetti C, Levi F, Polesel J, Zucchetto A, Negri E et al (2013) Risk factors for young-onset colorectal cancer. Cancer Causes Control 24:335–341. https://doi.org/10.1007/s10552-012-0119-3
Siegel RL, Torre LA, Soerjomataram I, Hayes RB, Bray F, Weber TK et al (2019) Global patterns and trends in colorectal cancer incidence in young adults. Gut 68:2179–2185. https://doi.org/10.1136/gutjnl-2019-319511
Sinicrope FA (2022) Increasing incidence of early-onset colorectal cancer. N Engl J Med 386:1547–1558. https://doi.org/10.1056/NEJMra2200869
Stoffel EM, Murphy CC (2020) Epidemiology and mechanisms of the increasing incidence of colon and rectal cancers in young adults. Gastroenterology 158:341–353. https://doi.org/10.1053/j.gastro.2019.07.055
Sung JJY, Chiu HM, Jung KW, Jun JK, Sekiguchi M, Matsuda T et al (2019) Increasing trend in young-onset colorectal cancer in Asia: more cancers in men and more rectal cancers. Am J Gastroenterol 114:322–329. https://doi.org/10.14309/ajg.0000000000000133
Vuik FE, Nieuwenburg SA, Bardou M, Lansdorp-Vogelaar I, Dinis-Ribeiro M, Bento MJ et al (2019) Increasing incidence of colorectal cancer in young adults in Europe over the last 25 years. Gut 68:1820–1826. https://doi.org/10.1136/gutjnl-2018-317592
Zhou M, Wang H, Zeng X, Yin P, Zhu J, Chen W et al (2019) Mortality, morbidity, and risk factors in China and its provinces, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 394:1145–1158. https://doi.org/10.1016/s0140-6736(19)30427-1
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Study conception and design: XT and JP. Drafting of manuscript, formal analysis, and visualization: XT, JP, SH, HX. Acquisition of data and resources: PW, JJ, WZ, XS, LS, XZ. Revision of manuscript, and final approval of manuscript: ML, XT. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
Not applicable.
Consent to participate
Not applicable.
Consent to publish
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

Supplementary Fig. 1
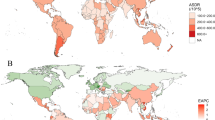
The global mortality rate of early-onset colorectal cancer among people aged 40–44 and 45–49 years in 204 countries and territories. (A The mortality rate of early-onset colorectal cancer among people aged 40–44 years in 2019; B The EAPC of the mortality rate of early-onset colorectal cancer among people aged 40–44 years from 1990 to 2019; C The mortality rate of early-onset colorectal cancer among people aged 45–49 years in 2019; D The EAPC of the mortality rate of early-onset colorectal cancer among people aged 45–49 years from 1990 to 2019.) EAPC estimated annual percentage change (JPG 528 KB)

Supplementary Fig. 2
Proportion of DALYs of early-onset colorectal cancer among people aged 40–44 and 45–49 years attributable to smoking, alcohol use, high BMI, and diets low in calcium, whole grains, and milk for 21 GBD regions in 1990. A 40–44 years old; B 45–49 years old. GBD Global Burden of Diseases, Injuries, and Risk Factors Study, DALYs Disability-Adjusted Life Years, BMI body mass index (JPG 705 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tang, X., Peng, J., Huang, S. et al. Global burden of early-onset colorectal cancer among people aged 40–49 years from 1990 to 2019 and predictions to 2030. J Cancer Res Clin Oncol 149, 16537–16550 (2023). https://doi.org/10.1007/s00432-023-05395-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-023-05395-6