Abstract
Background
Significant improvement in survival outcome with the programmed death 1 (PD-1)/programmed death ligand 1 (PD-L1) inhibitors has been shown in advanced non-small cell lung cancer (NSCLC) patients compared with chemotherapy. However, the full spectrum of toxic events of PD-1/PD-L1 inhibitors was not well characterized. We conducted a comprehensive meta-analysis to state the safety profile of PD-1/PD-L1 inhibitors in NSCLC, and identify the exact incidence and relative risk (RR) of both summary and detailed AEs.
Materials and methods
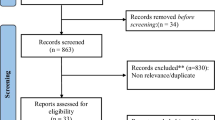
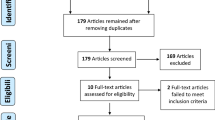
Electronic databases (PubMed, EMBASE and the Cochrane library databases) and major conference proceedings were systematically searched for all clinical trials in lung cancer using PD-1/PD-L1 inhibitors. Eligible studies included randomized controlled trials (RCTs) comparing PD-1/PD-L1 inhibitors with chemotherapy in NSCLC patients reporting all-grade (1–4) or high-grade (3–4) AEs [toxic symptoms, hematologic toxicities, and immune-related AEs (irAEs)], treatment discontinuation due to toxicities, or toxic deaths. The pooled incidence, RR, and corresponding 95% confidence interval (CI) of toxicity outcomes were calculated.
Results
A total of 4413 patients from 8 RCTs (3 with nivolumab; 2 with atezolizumab, and 3 with pembrolizuma) were included. In terms of summary toxic events, PD-1/PD-L1 inhibitors had a significantly lower risk of any all-grade AEs (66.20 vs. 86.08%; RR 0.77) and high-grade AEs (14.26 vs. 43.53%; RR 0.32), treatment discontinuation (5.94 vs. 13.92%; RR 0.44), and toxic deaths (0.48 vs. 1.12%; RR 0.45) than chemotherapy. With regard to detailed toxic events, the risk of toxic symptoms (including all-grade fatigue, nausea, constipation, diarrhea and peripheral sensory neuropathy; high-grade fatigue, anorexia, diarrhea and peripheral sensory neuropathy) and hematologic toxicities (including all-grade and high-grade neutropenia, thrombocytopenia, and anemia) from PD-1/PD-L1 inhibitors was significantly lower than from chemotherapy. However, there was a small but significantly increased risk of irAEs, including all-grade rash, pruritus, colitis, hypothyroidism, hyperthyroidism, ALT/AST elevations and pneumonitis, as well as high-grade pneumonitis.
Conclusion
PD-1/PD-L1 inhibitors are generally safer and better tolerated than chemotherapy for patients with NSCLC with regard to summary toxic events, detailed toxic symptoms and hematologic toxicities. However, PD-1/PD-L1 inhibitors can generate a unique spectrum of irAEs, and several of them can be severe and even life-threatening. Clinicians should be aware of the risk of these AEs, as they may have a potentially negative impact on the patients’ quality of life and survival outcome.


Similar content being viewed by others
Abbreviations
- AEs:
-
Adverse events
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- ASCO:
-
American Society of Clinical Oncology
- CTCAE:
-
The Common Terminology Criteria for Adverse Events version
- CI:
-
Confidence interval
- FDA:
-
Food and Drug Administration
- irAEs:
-
Immune-related AEs
- PD-1:
-
Programmed death 1
- PD-L1:
-
Programmed death ligand 1
- RR:
-
Relative risk
- RCTs:
-
Randomized controlled trials
References
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50(4):1088–1101
Buchbinder EI, Desai A (2016) CTLA-4 and PD-1 pathways: similarities, differences, and implications of their inhibition. Am J Clin Oncol 39(1):98–106
Chae YK, Arya A, Iams W et al (2018) Immune checkpoint pathways in non-small cell lung cancer. Ann Transl Med 6(5):88
Cousin S, Italiano A (2016) Molecular pathways: immune checkpoint antibodies and their toxicities. Clin Cancer Res 22(18):4550–4555
De Velasco G, Je Y, Bosse D et al (2017) Comprehensive meta-analysis of key immune-related adverse events from CTLA-4 and PD-1/PD-L1 inhibitors in cancer patients. Cancer Immunol Res 5(4):312–318
DerSimonian R, Laird N (1986) Meta-analysis in clinical trials. Control Clin Trials 7(3):177–188
Egger M, Davey Smith G, Schneider M et al (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315(7109):629–634
Fay AP, Moreira RB, Nunes Filho PRS et al (2016) The management of immune-related adverse events associated with immune checkpoint blockade. Expert Rev Qual Life Cancer Care 1(1):89–97
Fehrenbacher L, Spira A, Ballinger M et al (2016) Atezolizumab versus docetaxel for patients with previously treated non-small-cell lung cancer (POPLAR): a multicentre, open-label, phase 2 randomised controlled trial. Lancet 387(10030):1837–1846
Herbst RS, Baas P, Kim DW et al (2016) Pembrolizumab versus docetaxel for previously treated, PD-L1-positive, advanced non-small-cell lung cancer (KEYNOTE-010): a randomised controlled trial. Lancet 387(10027):1540–1550
Higgins JP (2011) The Cochrane Collaboration. 2011. Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0. http://www.cochrane-handbook.org. Accessed 21 Jun 2018
Iwai Y, Hamanishi J, Chamoto K et al (2017) Cancer immunotherapies targeting the PD-1 signaling pathway. J Biomed Sci 24(1):26
Li A, Wei ZJ, Ding H et al (2017) Docetaxel versus docetaxel plus cisplatin for non-small-cell lung cancer: a meta-analysis of randomized clinical trials. Oncotarget 8(34):57365–57378
Michot JM, Bigenwald C, Champiat S et al (2016) Immune-related adverse events with immune checkpoint blockade: a comprehensive review. Eur J Cancer 54:139–148
Naidoo J, Page DB, Li BT et al (2015) Toxicities of the anti-PD-1 and anti-PD-L1 immune checkpoint antibodies. Ann Oncol 26(12):2375–2391
National Cancer Institute: Common Terminology Criteria for Adverse Events (CTCAE) 4.0 Available from https://evs.nci.nih.gov/ftp1/CTCAE/CTCAE_4.03/Archive/CTCAE_4.0_2009-05-29_QuickReference_8.5x11.pdf. Accessed 21 Jun 2018
O’Kane GM, Labbe C, Doherty MK et al (2017) Monitoring and management of immune-related adverse events associated with programmed cell death protein-1 axis inhibitors in lung cancer. Oncologist 22(1):70–80
Pai-Scherf L, Blumenthal GM, Li H et al (2017) FDA approval summary: pembrolizumab for treatment of metastatic non-small cell lung cancer: first-line therapy and beyond. Oncologist 22(11):1392–1399
Panic N, Leoncini E, de Belvis G et al (2013) Evaluation of the endorsement of the preferred reporting items for systematic reviews and meta-analysis (PRISMA) statement on the quality of published systematic review and meta-analyses. PloS One 8(12):e83138
Reck M, Rodriguez-Abreu D, Robinson AG et al (2016) Pembrolizumab versus chemotherapy for PD-L1-positive non-small-cell lung cancer. N Engl J Med 375(19):1823–1833
Reeve BB, Mitchell SA, Dueck AC et al (2014) Recommended patient-reported core set of symptoms to measure in adult cancer treatment trials. J Natl Cancer Inst 106(7)
Rittmeyer A, Barlesi F, Waterkamp D et al (2017) Atezolizumab versus docetaxel in patients with previously treated non-small-cell lung cancer (OAK): a phase 3, open-label, multicentre randomised controlled trial. Lancet 389(10066):255–265
Thompson JA (2018) New NCCN guidelines: recognition and management of immunotherapy-related toxicity. J Natl Compr Cancer Netw: JNCCN 16(5 s):594–596
Funding
This study was supported by the Science and Technology Support Program of Sichuan Province (No.2016CZYD0001 to Wemin Li and No.2016SZ0073 to PanwenTian).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest regarding the present study.
Ethical approval
The article does not contain any studies with human participants performed by any of the authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Luo, W., Wang, Z., Tian, P. et al. Safety and tolerability of PD-1/PD-L1 inhibitors in the treatment of non-small cell lung cancer: a meta-analysis of randomized controlled trials. J Cancer Res Clin Oncol 144, 1851–1859 (2018). https://doi.org/10.1007/s00432-018-2707-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00432-018-2707-4