Abstract
Kabuki syndrome (KS) is a well-recognized disorder characterized by postnatal growth deficiency, dysmorphic facial features, skeletal anomalies, and intellectual disability. The syndrome is caused by KMT2D gene mutations or less frequently KDM6A gene mutations or deletions. We report a systematic evaluation of KS patients from Campania region of Italy; data were also compared with literature ones. We collected data of 15 subjects (8 males and 7 females with age range 10–26 years; mean age 16.9 years) with confirmed diagnosis of KS, representing the entire cohort of patients from Campania Region. Each patient performed biochemical testing and instrumental investigation. Neuro-intellectual development, cranio-facial dysmorphisms, and multisystem involvement data were collected retrospectively. For each category, type of defects and frequency of the anomalies were analyzed. Our observation shows that KS patients from Campania region have some particular and previously underscored, neurological and immunological findings. We found high prevalence of EEG’s abnormalities (43%) and MRI brain abnormalities (60%). Microcephaly resulted more common in our series (33%), if compared with major cohorts described in literature. Biochemical features of immunodeficiency and autoimmune diseases including thyroid autoimmunity, polyserositis, and vitiligo were observed with high prevalence (54.5%). Low immunoglobulins levels were a frequent finding. Lymphocyte class investigation showed significantly reduced CD8 levels in one patient.
Conclusions: These data confirm great heterogeneity of clinical manifestations in KS and suggest to introduce further clinical diagnostic criteria in order to perform a correct and precocious diagnosis.
What is Known • Kabuki syndrome is characterized by growth deficiency, dysmorphic facial features, skeletal anomalies, and intellectual disability • Immune dysfunction is a common finding but autoimmune diseases are rarely seen • Neurological features are common | |
What is New • Some particular facial features could help gestalt diagnosis (hypertelorism, broad nasal bridge, micrognathia, tooth agenesis, cutaneous haemangiomas and strabismus) • Higher prevalence of autoimmune disorders than previously reported • Particular neurological features are present in this cohort (EEG and MRI brain abnormalities) |
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Kabuki syndrome (KS, OMIM # 147920 and 300867) was firstly described by Niikawa and Kuroki [1,2,3] and, over the years, has become a well-recognized multiple congenital anomaly/intellectual disability (ID) disorder.
The incidence of KS is about 1/32,000 of live births [4]. The lysine (K)-specific methyltransferase 2 family (KMT2 A-E), originally named the myeloid/lymphoid or mixed-lineage leukemia (MLL1-5) proteins, regulates the expression of genes involved in embryogenesis and development. KMT2D (12q13.12, also known as MLL2, OMIM *602113) was the first gene associated with KS [5,6,7,8,9], and most KS patients bear KMT2D gene mutations. Additionally, a minority of patients have mutations or deletions of KDM6A (Xp11.3, OMIM *300128), which takes part of the same transcription complex as KMT2D [10,11,12,13,14,15,16]. Potential genetic defects remain unknown in about 30% of patients clinically diagnosed with KS [17].
KS is included in the chromatinopathies, a group of hereditary disorders caused by abnormalities of chromatin regulation, determined by variants in the various genes encoding for the components of the epigenetic machinery. Neurological impairments or ID are common features, though these conditions are characterized by clinical heterogeneity [18]. The widespread of next-generation sequencing methods improved diagnosis and expanded knowledge about these disorders [19].
Niikawa et al. [1, 3] initially defined five cardinal features of KS, consisting of postnatal growth deficiency, dysmorphic facial features, skeletal anomalies, persistent fingertip pads, and ID (typically in the mild to moderate range) [20, 21].
The consensus diagnostic criteria for KS were created by an international group of experts in 2018 [22,23,24,25,26,27,28].
Here, we perform a systematic evaluation of a cohort of patients representing the entire medical record of patients from Campania region and compared reported data with the ones reported in the literature [24,25,26,27,28,29,30,31,32].
Subjects and methods
Subjects
Data of 15 subjects with KS, representing the entire cohort of patients from Campania region of Italy were collected. All the patients were followed up in Medical Genetics Units. The study was approved by the Medical Ethics Committee of “Federico II” University of Naples.
In this retrospective study cranio-facial dysmorphisms, neuro-intellectual development, and multisystem involvement data were collected. For each category, the type of defects and the frequency of the single anomalies were analyzed.
Auxological, neurologic, ophthalmologic, ear-nose-throat (ENT), and rheumatologic evaluations were performed.
Laboratory investigation for baseline thyroid profile, autoantibodies for autoimmune thyroiditis, screening for celiac disease and serum immunoglobulins were also recorded.
Lymphocyte class investigation was performed in 5 patients.
Auditory brainstem response (ABR), electroencephalogram (EEG), magnetic resonance imaging (MRI) of brain and cervical spine, echocardiocolor-Doppler, and abdominal ultrasound were also performed.
Molecular analyses
Clinical diagnosis was confirmed in all patients performing molecular studies on DNA extracted from peripheral blood lymphocytes. Genomic DNA was extracted from fresh and/or frozen peripheral blood leukocytes of patients and their available family members using an automated DNA extractor and commercial DNA extraction Kits (Qiagen, Germany). Mutation screening of all 54 coding exons of the KMT2D (MIM #602113, NM_003482.3) gene and 29 coding exons of the KDM6A (MIM #300128, NM_021140.3) gene was performed by PCR amplification and direct sequencing as reported [33].
Results
In this study, 15 patients, 8 males and 7 females with age range 10–26 years (average 16.9 years), have been included; 13 patients present heterozygous mutations in KMT2D (86.7%); and 2 patients present heterozygous mutations in KDM6A (13.3%). Almost all, except one, reported patients had de novo variants. One patient inherited a KMT2D variant from the affected mother, who presents a mild phenotype characterized by typical facial features (long palpebral fissures, lower palpebral eversion, epicanthus) and joint pain, without involvement of other systems.
Main clinical features of patients, compared to literature records, are summarized in Tables 1, 2, 3, 4, 5, and 6 and Figs. 1, 2, and 3. Data in tables are separately shown for children (0–16 years, n = 8) and adults (> 16 years, n = 7). Detailed informations for each patient are available in Tables S1–S2 (see Supplement). Only significant results are reported in the text.
Prevalence of nervous system abnormalities in patients of present cohort and in the patients reported in the literature from Matsumoto et al. [21] (white bars with diagonal lines pattern), Wessels et al. [23] (gray bars), Banka et al. [24] (white bars with dots), this paper (black bars). EEG electroencephalography, MRI magnetic resonance imaging
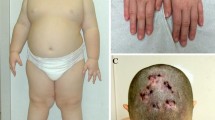
Facial fetaures in some of KS patients reported in this paper; the code is the same reported in Tables S1–S2. a P5. Long palpebral fissure, palpebral eversion, hypertelorism, arched eyebrow with thinning of lateral third, malformed and prominent ear, broad nasal root, short columella, thin lips, microretrognathia. b P11. Long palpebral fissure, palpebral eversion, epicanthus, thinning of lateral third of eyebrow, malformed and prominent ear, broad nasal root, thin lips, micrognathia. c P9. Long palpebral fissure, palpebral eversion, strabismus, ptosis, exophtalmos, epicanthus, arched eyebrow with thinning of lateral third, malformed and prominent ear, short columella, thin lips, high forehead. d P3. Long palpebral fissure, palpebral eversion, ptosis, strabismus (surgical correction), malformed ear, broad nasal root, anteverse nostrils, thin upper lip, low neck implant. e P15. Long palpebral fissure, eversion of third lateral, arched and thick eyebrow with thinning of lateral third, malformed and prominent ear, broad nasal root, short columella, depressed nasal tip, thin upper lip, down lip corners, micrognathia, high forehead. f P14. Long palpebral fissure, palpebral eversion, ptosis, arched eyebrow with thinning of lateral third, malformed and prominent ear, broad nasal root, short columella, thin lips with lip pit, micrognathia, high forehead. g P7 and his mother. Long palpebral fissure, lower palpebral eversion, epicanthus and prominent ear in a patient of our cohort (on the left) and his affected mother (on the right)
Characteristic facial features
Most of the typical facial features of KS, such as long palpebral fissures 15/15 (100%), lower palpebral eversion 13/15 (87%), and arched eyebrows 10/13 (77%) with thinning of the lateral third 12/15 (80%), were present in almost all patients. Ear anomalies, micrognathia, and broad nasal root were very common. Cleft lip or palate was reported in 3/11 (27%) whereas high-arched palate was frequent 9/11 (82%). None of the patients showed full lower lips, nodules, or pits, although this is a frequent feature in KS patients. Abnormal dentition was recorded in 6/6 adults and 3/3 children, specifically dental agenesis 5/9 (55.5%); 3 children presented, respectively, eruptive cyst, dysodontiasis, and oligodontia; an adult patient presented dysodontiasis and maxillary odontoma. Finally, 4/11 (36%) patients showed cutaneous haemangiomas: two patients in frontonasal region and two patients in sacral region (Table 1).
Neurological abnormalities
Intellectual disability (intellectual quotient, IQ < 70) was found in 87% of cases.
Mild (IQ 50–69) and moderate (IQ 35–49) ID was observed in 6/15 (40%) and in 3/15 (20%) patients, respectively. In 4/15 (27%), an unspecified degree was recorded. None had severe disability (IQ < 34) and 2 had normal intellective function.
Intellectual function does not change over time. Nevertheless, a patient showed an IQ improvement (from 43, with WPPSI scale at the age of 6 years, to 61, with WISC-III scale at the age of 7 years); this difference could be explained by the diffident behavior of the patient that probably influenced the first evaluation. No sufficient data were available for the evaluation of a progression of behavioral problems. Rare findings, present in three different patients, include speech delay (1/15), aggressive behavior (1/15), and severe posttraumatic stress disorder with psychotic episodes and visual hallucinations (1/15).
Hypotonia was reported in one adult patient; neonatal hypotonia has not been reported. Microcephaly was present in 5/15 (33%), with neonatal onset only in one patient.
Two patients presented seizures, one pharmacologically treated; three patients showed EEG anomalies without clinical manifestations.
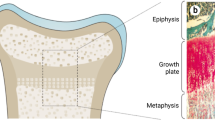
Brain MRI showed anomalies in 6/10 patients: modest increase of CNS liquoral spaces (2/10), upper parietal gyrus reduction, corpus callosum abnormalities, pituitary microadenoma, partial empty sella, and consequences of CNS ischemia in one patient, respectively (Table 2 and Fig. 1).
Skeletal abnormalities
Skeletal abnormalities were reported in 14/14 patients (100%): brachydactyly 7/13 (54%), fifth finger clinodactyly 7/13 (54%), scoliosis 7/10 (70 %), vertebral abnormalities 4/10 (40%) (2 cases of L3 vertebral cleft, one case of butterfly vertebra and one case of C7 apophysis malformation), fingertip pads 14/14 (100%). Skeletal alterations also interested hip, knee and feet (flat foot, hip dislocation, and valgus knee) (Table 3).
Growth and endocrine system involvement
Growth
Harmonic short stature (height less than − 2.0 SD) was present in 27% (4/15); in three patients, height corresponded to − 2.0 SD. Mean height in the 7 adult patients (5 female and 2 male) was 155.3 cm, in particular 153 cm (− 1.62 SD) in females and 161.1 cm (− 2.32 SD) in males. Short stature was present in both adult male patients; one of them was diagnosed for growth hormone (GH) deficiency but parents refused therapy; the other one showed a familiar short stature. Growth hormone deficiency was investigated, and GH deficit was detected in 3/10 patients. Parents of one patient refused GH therapy; his height was 157 cm at the age of 22 years (− 2.94 SD). Two of them, one male and one female, underwent recombinant growth hormone therapy: one had a good response and reached a normal stature, while the other still shows short stature. GH deficiency was diagnosed in the female patient when she was 6 years old (height 105.5 cm, − 2.02 SD). The patient underwent GH treatment from the age of 6 to the age of 15.75 years (height was 152 cm, − 1.6 SD). GH deficiency in the male patient was diagnosed when he was 13 years old (height 135.6 cm, SD − 2.79). GH therapy is still ongoing, and his height at the age of 15.67 years was 149.5 cm (− 2.9 SD). No adverse effect was reported for both patients. Intrauterine growth restriction was reported in two cases and polyhydramnios in five pregnancies. One patient was born small for gestational age and two late-preterm.
Endocrine system
The study of thyroid function showed high TSH levels in 2/8 and autoimmunity in 4/11, but only two of these presented hypothyroidism. Recurrent hypoglycaemia was reported in two patients, just in one case in neonatal period. Hyperinsulinism was present in one child, no patients showed diabetes mellitus. Obesity or overweight were reported in 4/14 patients (29%), all adults. Cryptorchidism was present in five patients, and one of them underwent orchidopexy at age 11 years. Hypogonadism and hypogenitalism are rarely reported (Table 4).
Immune system involvement
Autoimmune markers and/or diseases were detected in 6/11 cases: thyroid autoantibodies in 4 patients, vitiligo in one patient, and periodic fever and polyserositis in another patient.
Some patients with KS (2/11) also underwent recurrent ear and respiratory infections.
Low immunoglobulin levels were a frequent finding: decreased IgA were observed in 7/9; decreased IgG in 6/8; decreased IgM in 4/8; severe immunodeficiency with pan-hypogammaglobulinemia in 4/8 patients.
Lymphocyte class investigation was normal with the exception of one patient showing significantly reduced expression of CD8+ T cells (6% vs normal range 19–29%, average 23%), according with the trend of lymphocyte reduction described in the literature (Table 5).
Multisystem involvement
Ophthalmologic examination showed strabismus in four patients, exophthalmos in two, myopia in one, corneal leukoma in one, and fundus oculi abnormalities in two (optical disc atrophy and bulging in the retinal nasal area).
Hearing loss appears to be common (4/6): three patients showed conductive hearing impairment, and the other one mixed hearing loss. Chronic otitis was reported in 2/6 patients.
Congenital heart disease (CHD) was reported in 10/13 patients. The most common were septal defects: ventricular defects 6/13; atrial defects 2/13; patent foramen ovale 2/13. We also reported three children with aortic coarctation, two with persistent arterial duct, one with bicuspid aortic valve, one with aortic valve dysplasia and one with aortic dilatation.
Urogenital abnormalities were present in 60% of KS patients: pyelectasis (2/10), renal cysts (2/10), double kidney district (2/10), abnormal kidney position (2/10), renal hypoplasia or dysplasia (1/10), fused kidney (1/10), and vesicoureteral reflux (1/10) were observed (Table 6).
Discussion
Kabuki syndrome is a well-recognized multiple congenital anomaly/ID disorder, mainly characterized by dysmorphic facial features, dermatoglyphic abnormalities, postnatal growth deficiency, and ID; congenital malformations can also be present [20, 21].
Our observation shows that KS patients from Campania region of Italy have some peculiarity.
We detected high prevalence of specific facial features, such as micrognathia, hypertelorism, broad nasal bridge, tooth agenesis, cutaneous haemangiomas, and strabismus.
Tooth abnormalities were present in all patients of our cohort, in particular tooth agenesis, abnormal tooth shape, and size (pitted incisors and truncated tooth roots). KMT2D and KDM6A are expressed in the dental epithelium of human tooth germs, thus confirming their roles in tooth development [34,35,36].
Cutaneous hemangiomas in our cohort are present in 4/15 patients (26 %), while prevalence in general population is reported between 4.5 and 9.9% [37, 38]. Association between KS and cutaneous haemangiomas has never been reported in literature, whereas in our cohort, it is well represented.
Minor variants such as brachidactyly, clinodactyly, and joint laxity, included among diagnostic criteria, are actually quite nonspecific. On the other hand, persistent foetal fingertip (100% of present cases) is a very peculiar feature, even if not pathognomonic, since other syndromes share this feature (Pitt–Hopkins syndrome, FG Opitz–Kaveggia, 2q37 microdeletion, and fetal alcohol syndrome ) [39,40,41,42].
The most frequent ophthalmologic anomaly reported in literature is strabismus (36%) [20,21,22,23,24,25,26,27, 29], comparable to our cohort (31%). We also recorded a considerable presence of fundus oculi abnormalities (15%), outlining the importance of ophthalmological examination.
Middle ear infections occur in approximately 70% of patients and can lead to conductive hearing loss and speech delay [34]. Hearing impairment (mostly conductive) appears to be common in our cases (67%). Delayed speech was also reported in one patient with conductive hearing loss.
Urogenital abnormalities are reported in 30–40% of KS patients [24] and include hydronephrosis, abnormal kidney position, renal hypoplasia or dysplasia, and fusion defects [16]. These anomalies showed a high frequency (60%) in our patients.
Rare findings reported in two pediatric patients in this paper are as follows: bronchial isomerism and bronchiectasis in one; left pulmonary artery hypoplasia and thymic ectopia in another.
Scoliosis could also strengthen the diagnostic suspicion, in particular if associated with a vertebral malformation [43].
Several neurological involvements are reported in KS patients, including hypotonia, seizures, behavioral problems, and intellectual disability [44,45,46,47].
Several studies on epilepsy in KS reported that patients were likely to present with focal seizures and focal EEG abnormalities, generally with favorable outcome. High prevalence of epilepsy in KS patients without brain abnormalities was previously reported [44]. In agreement with the literature, in our cohort, 29% of patients presented seizures. A relevant data was the high prevalence of EEG anomalies, namely pointed waves, reported in 43% of cases and rarely described in literature. Interestingly, both patients (2/2) with KDM6A mutations showed sporadic pointed waves and epilepsy with paroxysm.
Most KS patients have normal CNS imaging, even if brain atrophy and organic structural lesions have been reported [45, 46]. On the other hand, MRI abnormalities were described with high frequency in our cohort (60%), in particular slight increase of CNS liquoral spaces (20%). Microcephaly resulted more common in our series, if compared with literature [21,22,23,24,25,26,27, 29].
Neurodevelopmental and behavioral problems have been extensively reported in KS [47]. Previous reports indicated a wide range of IQ, with specific deficits in motor abilities, in linguistic domains, in phonological and oromotor functions; behavioral skills seem to be fairly preserved. In the present cohort, ID (IQ < 70) was one of the primary characteristics of KS, in mild to moderate range, and behavior problems were reported in two patients.
Congenital heart disease is described in literature in 50–75% of the patients [48, 49]. Next-generation sequencing in fetuses with CHD showed pathogenic variants in MYH6 and KMT2D [48]. In the present report, CHD were described in all children and in 40% of adults.
Patients with KS are also vulnerable to infections, including those affecting middle ear and upper airway tract. Recurrent infections, mostly affecting the upper respiratory tract, were recorded in 18% of our patients. Immune impairment is a common finding in KS, since correct histone-3 methylation patterns are essential to achieve modifications in Ig genes required for B cell development and function [50,51,52,53]. Approximately half of the patients present with common variable immune deficiency (CVID)-like characteristics. Concerning to healthy individuals, the numbers of memory B cells are reduced, with difficulty to generate or maintain specific antibody responses and long-term immunological memory [31, 32, 54, 55].
Lower serum IgG, IgA, or/and IgM levels have been scored in 10–79% of KS patients [55, 56]. In the current cohort, we observed hypogammaglobulinemia in several patients and reduced CD8 levels in one patient.
Autoimmune diseases are rarely seen in patients with KS [57, 58] but were documented in 54.5% of our patients.
Mutations in KMT2D gene are highly recurrent and occur early during tumorigenesis in diffuse large B cell lymphoma and follicular lymphoma. These findings suggest that, in KS, loss of KMT2D function could lead to impairment of cell maturation [50]. A significant reduction in memory B and T cells has been documented in an entire cohort of 12 KS patients with KMT2D heterozygous variants [31, 32, 54]. Furthermore, a reduced generation of memory cells can be based on the lack of a delayed hypersensitivity response (including purified protein derivative PPD and candidin), as documented in a Brazilian cohort of KS patients [54]. These data can help us to explain the variable occurrence (interindividual and temporal) of dysgammaglobulinemia that can increase the risk of infections or autoimmune diseases. So, the study of lymphocytes can be considered a useful tool to identify asymptomatic subjects who can develop autoimmune disorders.
Regarding endocrinological disorders, postnatal GH deficiency is reported in KS patients, while rare findings include hypothyroidism, diabetes insipidus, primary ovary dysfunction, abnormal pituitary findings on magnetic resonance images, hyperinsulinism, and hypoglycemia [59,60,61,62,63,64,65]. In our cases, short stature (height < − 2SD) is reported in 4 patients and 3 patients showed height corresponding to − 2SD; GH deficiency was diagnosed in 3/10 patients. It is noteworthy that short stature was present in both adult male patients, one with GH deficit and the other with familial short stature. Considering that the prevalence of GH deficiency is only 1% in the general population and 2% in one of the major reviews, it seems very high in our series. GH replacement therapy has many beneficial effects on KS children, including a significant improvement in joint hypermobility, suggesting a direct effect of GH on connective tissue [60, 61].
High levels of TSH, with thyroid hormone deficiency were recorded in 2 patients. Similar data are described in a single case report [66].
In our series, 20% of the patients showed premature thelarche; rare findings included hypermenorrhea, micropolycystic ovary, ginecomastia, hypogonadism, and hypogenitalism. High prevalence of cryptorchidism has been recorded in our cases when compared to literature.
More than 50% of KS patients reported in the literature are overweight or obese, during childhood or adolescence [16, 20,21,22,23]. In our series, overweight or obesity was present only in adult patients and three adolescents, instead, presented generalized poor growth.
Patients with KS can present with hypoglycemia, which can be transient or persistent [63,64,65]. One of our patients presented with neonatal hypoglycemia; chronic hypoglycemia was detected in 20% of the patients and one of them had hyperinsulinemia. KS patients with KDM6A variants may be at higher risk for neonatal hyperinsulinemic hypoglycemia than those with KMT2D variants [63, 64]. As hyperinsulinemic hypoglycemia is one of the most common causes of persistent hypoglycemia in KS patients, a high degree of suspicion is needed for early diagnosis and appropriate management.
Regarding genotype-phenotype correlation, it has been reported that patients with KMT2D variants show a significantly higher frequency of short stature, typical facial features, persistent fetal finger pads, renal abnormalities, and feeding problems compared with patients with KDM6A variants [7, 10, 16, 67,68,69,70]; conversely, KDM6A variants are associated with variable phenotypes, ranging from typical KS to milder clinical presentations [11,12,13,14,15]. Patients with KDM6A variants seem to have hypotonia and feeding difficulties during infancy, poor postnatal growth, and short stature.
Developmental delay and learning disabilities are generally moderate to severe in boys and mild to moderate in girls with KDM6A mutations [15], as expected for X-linked disorders, but it has recently been described a female patient with KDM6A variant showing typical facial features, severe ID, short stature, CHD, recurrent infection, and Chiari malformation [13].
In our cohort we found that patients with KDM6A variants showed a more severe clinical presentation. We observed two patients carrying KDM6A de novo variants. The first one, a 26-year-old woman, showed short stature, tipical dysmorphic features, ogival palate, maxillary odontoma and dysodontiasis, moderate ID, EEG and MRI anomalies, polycystic ovary disorder with hypermenorrea, autoimmune hypothyroidism, mild dilatation of the renal pelvis, and scoliosis with C7 apophysis malformation. The second patient was a 21-year-old woman, showing peculiar features: long palpebral fissures with eversion of the lateral third of the lower eyelids, sparseness of eyebrows’ lateral sides, ptosis of the left eye, strabismus, hypodontia, fetal pads, malformed ears, micrognathia, brachidactyly, mild ID, behavior disorder, seizures, and anterior pituitary hypoplasia. In both cases, there was no CHD. Thus, our experience suggests that KDM6A phenotype has moderate-severe manifestations of disease that persist even in adulthood. In particular, we underline the predominantly neurological phenotype of KDM6A mutations, in which epilepsy, seizures, or EEG anomalies seem much more frequent.
Conclusion
In conclusion, we confirm that KS is characterized by a great heterogeneity of clinical manifestations and suggest to take into consideration further clinical diagnostic criteria as an aid to perform a correct and more precocious diagnosis. Some dysmorphic features very common in our series, such as hypertelorism, broad nasal bridge, micrognathia, tooth agenesis, cutaneous haemangiomas, and strabismus, could be added to the signs allowing a gestalt diagnosis.
We also outline the multisystem involvement of KS and the need of a multi disciplinary team involved in the follow-up program, in order to allow a precocious diagnosis and treatment:the team should include neurologist, endocrinologist, ophthalmologist, ENT specialist, orthopedic, immuno-rheumatologist, cardiologist, dentist, nephrologist, gastro-hepatologist, and surgeon. Indeed, disease-specific treatment is probably on the way.
Abbreviations
- CHD:
-
Congenital heart disease
- CNS:
-
Central nervous system
- EEG:
-
Electroencephalogram
- ID:
-
Intellectual disability
- IQ:
-
Intellectual quotient
- KS:
-
Kabuki syndrome
- MRI:
-
Magnetic resonance imaging
References
Niikawa N, Matsura N, Fukushima Y, Ohsawa T, Kajii T (1981) Kabuki make-up syndrome: a syndrome of mental retardation, unusual facies, large and protruding ears, and postnatal growth deficiency. J Pediatr 1981(99):565–569
Kuroki Y, Suzuki Y, Chyo H, Hata A, Matsui I (1981) A new malformation syndrome of long palpebral fissures, large ears, depressed nasal tip, and skeletal anomalies associated with postnatal dwarfism and mental retardation. J Pediatr 99:570–573
Niikawa N, Kuroki Y, Kajii T, Matsuura N, lshikiriyarna S, Tonoki H et al (1988) Kabuki make-up (Niikawa-Kuroki) syndrome: a study of 62 patients. Am J Med Genet 31:562–569
Wang Y, Xu N, Wang J, Wang XM (2019) Kabuki syndrome: review of the clinical features, diagnosis and epigenetic mechanisms. World J Pediatr 15:528–535
Ng SB, Bigham AW, Buckingham KJ, Hannibal MC, McMillin MJ, Gildersleeveet HI et al (2010) Exome sequencing identifies MLL2 mutations as a cause of Kabuki syndrome. Nat Genet 42:790–793
Paulussen AD, Stegmann AP, Blok MJ, Tserpelis D, Posma-Velter C, Detisch Y et al (2011) MLL2 mutation spectrum in 45 patients with Kabuki syndrome. Hum Mutat 32:E2018–E2025
Cocciadiferro D, Augello B, De Nittis P, Zhang J, Mandriani B, Malerba N et al (2018) Dissecting KMT2D missense mutations in Kabuki syndrome patients. Hum Mol Genet 27:3651–3668
Xin C, Wang C, Wang Y, Zhao J, Wang L, Li R, Liu J (2018) Identification of novel KMT2D mutations in two Chinese children with Kabuki syndrome: a case report and systematic literature review. BMC Med Genet 19:31
Lintas C, Persico AM (2018) Unraveling molecular pathways shared by Kabuki and Kabuki-like syndromes. Clin Genet 94:283–295
Lederer D, Grisart B, Digilio MC, Benoit V, Crespin M, Ghariani SC, Maystadt I, Dallapiccola B, Verellen-Dumoulin C (2012) Deletion of KDM6A, a histonedemethylase interacting with MLL2, in three patients with Kabuki syndrome. Am J Hum Genet 90:119–124
Miyake N, Mizuno S, Okamoto N, Ohashi H, Shiina M, Ogata K, Tsurusaki Y, Nakashima M, Saitsu H, Niikawa N, Matsumoto N (2013) KDM6A point mutations cause Kabuki syndrome. Hum Mutat 34:108–110
Banka S, Lederer D, Benoit V, Jenkins E, Howard E, Bunstone S, Kerr B, McKee S, Lloyd IC, Shears D, Stewart H, White SM, Savarirayan R, Mancini GMS, Beysen D, Cohn RD, Grisart B, Maystadt I, Donnai D (2015) Novel KDM6A (UTX) mutations and a clinical and molecular review of the X-linked Kabuki syndrome (KS2). Clin Genet 87:252–258
Cheon CK, Sohn YB, Ko JM, Lee YJ, Song JS, Moon JW, Yang BK, Ha IS, Bae EJ, Jin HS, Jeong SY (2014) Identification of KMT2D and KDM6A mutations by exome sequencing in Korean patients with Kabuki syndrome. J Hum Genet 59:321–325
Bögershausen N, Gatinois V, Riehmer V, Kayserili H, Becker J, Thoenes M et al (2016) Mutation update for Kabuki syndrome genes KMT2D and KDM6A and further delineation of X-Linked Kabuki syndrome subtype 2. Hum Mutat 37:847–864
Bjornsson HT, Benjamin JS, Zhang L, Weissman J, Gerber EE, Chen YC et al (2014) Histone deacetylase inhibition rescues structural and functional brain deficits in a mouse model of Kabuki syndrome. Sci Transl Med 6:256–279
Micale L, Augello B, Maffeo C, Selicorni A, Zucchetti F, Fusco C, de Nittis P, Pellico MT, Mandriani B, Fischetto R, Boccone L, Silengo M, Biamino E, Perria C, Sotgiu S, Serra G, Lapi E, Neri M, Ferlini A, Cavaliere ML, Chiurazzi P, Monica MD, Scarano G, Faravelli F, Ferrari P, Mazzanti L, Pilotta A, Patricelli MG, Bedeschi MF, Benedicenti F, Prontera P, Toschi B, Salviati L, Melis D, di Battista E, Vancini A, Garavelli L, Zelante L, Merla G (2014) Molecular analysis, pathogenic mechanisms, and readthrough therapy on a large cohort of Kabuki syndrome patients. Hum Mutat 35:841–850
Adam MP, Hudgins L, Hannibal M (1993-2021) In: Adam MP, Ardinger HH, Pagon RA et al (eds) (2011, Updated 2019) Kabuki Syndrome. GeneReviews® [Internet], Seattle (WA) Available from: https://www.ncbi.nlm.nih.gov/books/NBK62111/
Bjornsson HT (2015) The Mendelian disorders of the epigenetic machinery. Genome Res 25:1473–1481
Squeo GM, Augello B, Massa V, Milani D, Colombo EA, Mazza T, et al. (2020) Customised next-generation sequencing multigene panel to screen a large cohort of individuals with chromatin-related disorder. J Med Genet: jmedgenet-2019-106724.
Bogershausen N, Wollnik B (2013) Unmasking Kabuki syndrome. Clin Genet 83:201–211
Matsumoto N, Niikawa N (2003) Kabuki make-up syndrome: a review. Am J Med Genet C: Semin Med Genet 117C:57–65
Adam MP, Banka S, Bjornsson HT, Bodamer O, Chudley AE, Harris J, Kawame H, Lanpher BC, Lindsley AW, Merla G, Miyake N, Okamoto N, Stumpel CT, Niikawa N, Kabuki Syndrome Medical Advisory Board (2019) Kabuki Syndrome Medical Advisory Board. Kabuki syndrome: international consensus diagnostic criteria. J Med Genet 56:89–95
Wessels MW, Brooks AS, Hoogeboom J, Niermeijer MF, Willems PJ (2002) Kabuki syndrome: a review study of three hundred patients. Clin Dysmorphol 11:95–102
Banka S, Veeramachaneni R, Reardon W, Howard E, Bunstone S, Ragge N, Parker MJ, Crow YJ, Kerr B, Kingston H, Metcalfe K, Chandler K, Magee A, Stewart F, McConnell VPM, Donnelly DE, Berland S, Houge G, Morton JE, Oley C, Revencu N, Park SM, Davies SJ, Fry AE, Lynch SA, Gill H, Schweiger S, Lam WWK, Tolmie J, Mohammed SN, Hobson E, Smith A, Blyth M, Bennett C, Vasudevan PC, García-Miñaúr S, Henderson A, Goodship J, Wright MJ, Fisher R, Gibbons R, Price SM, C de Silva D, Temple IK, Collins AL, Lachlan K, Elmslie F, McEntagart M, Castle B, Clayton-Smith J, Black GC, Donnai D (2012) How genetically heterogeneousis Kabuki syndrome? : MLL2 testing in 116 patients, review and analyses of mutation and phenotypic spectrum. Eur J Hum Genet 20:381–388
Cheon CK, Ko JM (2015) Kabuki syndrome: clinical and molecular characteristics. Korean J Pediatr 58:317–324
Lindsley AW, Saal HM, Burrow TA, Hopkin RJ, Shchelochkov O, Khandelwal P, Xie C, Bleesing J, Filipovich L, Risma K, Assa'ad AH, Roehrs PA, Bernstein JA (2016) Defects of B-cell terminal differentiation in patients with type-1 Kabuki syndrome. J Allergy Clin Immunol 137:179–187
White SM, Thompson EM, Kidd A, Savarirayan R, Turner A, Amor D, Delatycki MB, Fahey M, Baxendale A, White S, Haan E, Gibson K, Halliday JL, Bankier A (2004) Growth, behavior, and clinical findings in 27 patients with Kabuki (Niikawa-Kuroki) syndrome. Am J Med Genet 127A:118–127
Schott DA, Gerver WJ, Stumpel CT (2016) Growth Hormone Stimulation Tests in Children with Kabuki Syndrome. Horm Res Paediatr 86:319–324
Schrander-Stumpel CT, Spruyt L, Curfs LM, Defloor T, Schrander JJ (2005) Kabuki syndrome: Clinical data in 20 patients, literature review, and further guidelines for preventive management. Am J Med Genet 132A:234–243
Stagi S, Gulino AV, Lapi E, Rigante D (2016) Epigenetic control of the immune system: a lesson from Kabuki syndrome. Immunol Res 64:345–359
Lin JL, Lee WI, Huang JL, Chen PK, Chan KC, Lo LJ et al (2014) Immunologic assessment and KMT2D mutation detection in Kabuki syndrome. Clin Genet 88:255–260
Hoffman JD, Ciprero KL, Sullivan KE, Kaplan PB, McDonald-McGinn DM, Zackai EH et al (2005) Immune abnormalities are a frequent manifestation of Kabuki syndrome. Am J Med Genet 135A:278–281
Micale L, Augello B, Fusco C, Selicorni A, Loviglio MN, Silengo MC et al (2011) Mutation spectrum of MLL2 in a cohort of Kabuki syndrome patients. Orphanet J Rare Dis 6:38
Peterson-Falzone SJ, Golabi M, Lalwani AK (1997) Otolaryngologic manifestations of Kabuki syndrome. Int J Pediatr Otorhinolaryngol 38:227–236
Cudzilo D, Czochrowska E (2018) Orthodontic Treatment of a Kabuki Syndrome Patient. Cleft Palate Craniofac J 55:1175–1180
Porntaveetus T, Abid MF, Theerapanon T, Srichomthong C, Ohazama A, Kawasaki K, Kawasaki M, Suphapeetiporn K, Sharpe PT, Shotelersuk V (2018) Expanding the Oro-Dental and Mutational Spectra of Kabuki Syndrome and Expression of KMT2D and KDM6A in Human Tooth Germs. Int J Biol Sci 14:381–389
Hoornweg MJ, Smeulders MJ, Ubbink DT, van der Horst CM (2012) The prevalence and risk factors of infantile haemangiomas: a case-control study in the Dutch population. Paediatr Perinat Epidemiol 26(2):156–162
Léauté-Labrèze C, Harper JI, Hoeger PH (2017) Infantile haemangioma. Lancet 390(10089):85–94
Lehalle D, Williams C, Siu VM, Clayton-Smith J (2011) Fetal pads as a clue to the diagnosis of Pitt-Hopkins syndrome. Am J Med Genet A 155A:1685–1689
Clark RD, Graham JM Jr, Friez MJ, Hoo JJ, Jones KL, McKeown C et al (2009) FG syndrome, an X-linked multiple congenital anomaly syndrome: the clinical phenotype and an algorithm for diagnostic testing. Genet Med 11:769–775
Cuscó I, del Campo M, Vilardell M, González E, Gener B, Galán E, Toledo L, Pérez-Jurado LA (2008) Array-CGH in patients with Kabuki-like phenotype: identification of two patients with complex rearrangements including 2q37 deletions and no other recurrent aberration. BMC Med Genet 9:27
Vorgias D, Bernstein B. (2020) Fetal Alcohol Syndrome. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 Jan
Atar M, Lee W, O'Donnell D (2006) Kabuki syndrome: oral and general features seen in a 2-year-old Chinese boy. Int J Paediatr Dent 16(3):222–226
Kurahashi N, Miyake N, Mizuno S, Koshimizu E, Kurahashi H, Yamada K, Natsume J, Aoki Y, Nakamura M, Taniai H, Maki Y, Abe-Hatano C, Matsumoto N, Maruyama K (2017) Characteristics of epilepsy in patients with Kabuki syndrome with KMT2D mutations. Brain and Development 39:672–677
Boisgontier J, Tacchella JM, Lemaître H, Lehman N, Saitovitch A, Gatinois V, Boursier G, Sanchez E, Rechtman E, Fillon L, Lyonnet S, le Quang Sang KH, Baujat G, Rio M, Boute O, Faivre L, Schaefer E, Sanlaville D, Zilbovicius M, Grévent D, Geneviève D, Boddaert N (2019) Anatomical and functional abnormalities on MRI in Kabuki syndrome. Neuroimage Clin 21:101610
Guo Z, Liu F, Li HJ (2018) Novel KDM6A splice-site mutation in Kabuki syndrome with congenital hydrocephalus: a case report. BMC Med Genet 19:206
Caciolo C, Alfieri P, Piccini G, Digilio MC, Lepri FR, Tartaglia M, Menghini D, Vicari S (2018) Neurobehavioral features in individuals with Kabuki syndrome. Mol Genet Genomic Med 6:322–331
Hu P, Qiao F, Wang Y, Meng L, Ji X, Luo C, Xu T, Zhou R, Zhang J, Yu B, Wang L, Wang T, Pan Q, Ma D, Liang D, Xu Z (2018) Clinical application of targeted next-generation sequencing in fetuses with congenital heart defect. Ultrasound Obstet Gynecol 52:205–211
Maffre I, Vincenti M, Dalla Vale F, Amouroux C, Werner O, Meilhac A et al (2019) Diazoxide Causality Assessment of a Pericardial Effusion in a Child with Kabuki Syndrome. J Clin Res Pediatr Endocrinol 11:218–219
Zhang J, Dominguez-Sola D, Hussein S, Lee JE, Holmes AB, Bansal M, Vlasevska S, Mo T, Tang H, Basso K, Ge K, Dalla-Favera R, Pasqualucci L (2015) Disruption of KMT2D perturbs germinal center B cell development and promotes lymphomagnesis. Nat Med 21:1190–1198
Kaiwar C, Kruisselbrink TM, Kudva YC, Klee EW, Pichurin P (2019) Exome sequencing confirms diagnosis of Kabuki syndrome in an-adult with hodgkin lymphoma and unusually severe multisystem phenotype. Clin Immunol 207:55–57
de Billy E, Strocchio L, Cacchione A, Agolini E, Gnazzo M, Novelli A et al (2019) Burkitt lymphoma in a patient with Kabuki syndrome carrying a novel KMT2D mutation. Am J Med Genet 179A:113–117
Marzollo A, Colavito D, Sartori S, Fanelli GN, Putti MC (2018) Cerebral Lymphoproliferation in a Patient with Kabuki Syndrome. J Clin Immunol 38:475–477
Frenk NE, Kim CA, Carneiro-Sampaio M, Orii NM, de MoraesVasconcelos D (2009) Basic evaluation of the immunocompetence of Brazilian patients with Kabuki syndrome. Pediatria (São Paulo) 31:170–177
Chrzanowska KH, Krajewska-Walasek M, Kus J, Michalkiewicz J, Maziarka D, Wolski JK et al (1998) Kabuki (Niikawa-Kuroki) syndrome associated with immunodeficiency. Clin Genet 53:308–312
Campos-Sanchez E, Martínez-Cano J, Del Pino ML, López-Granados E, Cobaleda C (2019) Epigenetic Deregulation in Human Primary Immunodeficiencies. Trends Immunol 40(1):49–65
Ming JE, Russell KL, McDonald-McGinn DM, Zackai EH (2005) Autoimmune disorders in Kabuki syndrome. Am J Med Genet 132A:260–262
Arsov T, Sestan M, Cekada N, Frkovic M, Andrews D, He Y et al (2019) Systemic lupus erythematosus: A new autoimmune disorder in Kabuki syndrome. Eur J Med Genet 62:103538
Moon JE, Lee SJ, Ko CW (2018) A de novo KMT2D mutation in a girl with Kabuki syndrome associated with endocrine symptoms: a case report. BMC Med Genet 19:102
Schott DA, Gerver WJM, Stumpel CTRM (2017) Growth hormone therapy in children with Kabuki syndrome: 1-year treatment results. Horm Res Paediatr 88(3-4):258–264
Schott DA, Stumpel CTRM, Klaassens M (2019) Hypermobility in individuals with Kabuki syndrome: The effect of growth hormone treatment. Am J Med Genet 179A:219–223
Kuroki Y, Katsumata N, Eguchi T, Fukushima Y, Suwa S, Kajii T (1987) Precocious puberty in Kabuki makeup syndrome. J Pediatr 110:750–752
Sumida Y, Kuwashima M, Mizumoto H, Sato K, Hara T (2017) Hyperinsulinemic hypoglycemia in Beckwith-Wiedemann, Sotos, and Kabuki syndromes: a nationwide survey in Japan. Am J Med Genet 173:360–367
Yap KL, Johnson AEK, Fischer D, Kandikatla P, Deml J, Nelakuditi V, Halbach S, Jeha GS, Burrage LC, Bodamer O, Benavides VC, Lewis AM, Ellard S, Shah P, Cody D, Diaz A, Devarajan A, Truong L, Greeley SAW, de Leó-Crutchlow DD, Edmondson AC, Das S, Thornton P, Waggoner D, del Gaudio D (2019) Congenital hyperinsulinism as the presenting feature of Kabuki syndrome: clinical and molecular characterization of affected individuals. Genet Med 21:233–242
Subbarayan A, Hussain K (2014) Hypoglycemia in Kabuki syndrome. Am J Med Genet 164A:467–471
Gürbüz F, Özalp Yüreğir Ö, Ceylaner S, Topaloğlu AK, Yüksel B (2016) Coexistence of Kabuki Syndrome and Autoimmune Thyroiditis. J Clin Res Pediatr Endocrinol 8:105–106
Teranishi H, Koga Y, Nakashima K, Morihana E, Ishii K, Sakai Y, Taguchi T, Oda Y, Miyake N, Matsumoto N, Ohga S (2018) Cancer management in Kabuki syndrome: the first case of Wilms tumor and a literature review. J Pediatr Hematol Oncol 40:391–394
Paderova J, Drabova J, Holubova A, Vlckova M, Havlovicova M, Gregorova A, Pourova R, Romankova V, Moslerova V, Geryk J, Norambuena P, Krulisova V, Krepelova A, Macek M Sr, Macek M Jr (2018) Under the mask of Kabuki syndrome: elucidation of genetic-and phenotypic heterogeneity in patients with Kabuki-like phenotype. Eur J Med Genet 61:315–321
Faundes V, Malone G, Newman WG, Banka S (2019) A comparative analysis of KMT2D missense variants in Kabuki syndrome, cancers and the general population. J Hum Genet 64:161–170
Wang HM, Wang XH, Wu HS, Wu Y, Zhuo XW (2018) Clinical and laboratory characteristics and genetic diagnosis of Kabuki syndrome. Zhonghua Er Ke Za Zhi 56:846–849
Acknowledgements
We are grateful to Prof. Pietro Vajro for his supportive attitude toward this project.
Availability of data and material
All data are available on request.
Code availability
N/A
Funding
Open access funding provided by Università degli Studi di Salerno within the CRUI-CARE Agreement.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Francesca Di Candia, Paolo Fontana, Mariateresa Falco, Carmen Rosano, Carmelo Piscopo, Gerarda Cappuccio, Maria Anna Siano, Daniele De Brasi, Claudia Mandato, Ilaria De Maggio, Matteo Della Monica, Gioacchino Scarano, Fortunato Lonardo, Daniela Melis.
Molecular analysis were performed by Giuseppe Merla and Gabriella Maria Squeo.
The first draft of the manuscript was written by Francesca Di Candia, Paolo Fontana, and Pamela Paglia, and all authors commented on previous versions of the manuscript.
Daniela Melis, Pietro Strisciuglio and Giuseppe Merla revised the final version.
All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the local Ethics Committee of University of Naples Federico II.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
The participants consented to the submission of their data.
Conflict of interest
The authors declare no competing interests.
Additional information
Responsible editor: Peter de Winter
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
ESM 1
Table S1-2. Individual data of KS patients reported in this paper (AGA, antigliadin antibodies; anti-tTG, transglutaminase antibodies; AoCa, aortic coarctation; ASD, atrial septal defect; IQ, intelligence quotient; IUGR intrauterine growth retardation; OFC, occipitofrontal circumference; PDA, persistent ductus arteriosus; PFO, patent foramen ovale; SD, standard deviation; VSD, ventricular septal defect; VUR, vesicoureteric reflux) (DOCX 37 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Di Candia, F., Fontana, P., Paglia, P. et al. Clinical heterogeneity of Kabuki syndrome in a cohort of Italian patients and review of the literature. Eur J Pediatr 181, 171–187 (2022). https://doi.org/10.1007/s00431-021-04108-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-021-04108-w