Abstract
Purpose
Magnetic anal sphincter (MAS) augmentation is a novel surgical option for the treatment of fecal incontinence. Current clinical evidence is conflicting. The purpose of this meta-analysis was to report the safety profile, potential benefits, and the functional efficacy of this device.
Methods
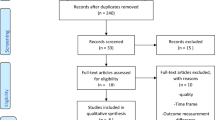
The study followed the PRISMA guidelines. Literature databases (Medline, Scopus, Web of Science, CENTRAL) were screened for eligible articles. The primary endpoint was the pooled effect of MAS in the Cleveland Clinic Incontinence Score (CCIS) score. Quality evaluation was based on the ROBINS-I and Risk of Bias 2 tool.
Results
Overall, 8 studies with 205 patients were included. MAS resulted in a significant reduction of CCIS values (p = 0.019), and improvement only in the embarrassment domain of FIQoL scores (p = 0.034). The overall morbidity rate was 61.8%. Postoperative adverse events included MAS explantation in 12%, infection in 5.1%, pain in 10% and obstructed defecation in 5.8% of patients.
Conclusion
The application of MAS in patients with fecal incontinence results in the improvement of some clinical parameters with a notable morbidity rate. Due to several study limitations, further, high-quality RCTs are required to delineate the efficacy and safety of MAS.
Similar content being viewed by others
Data availability
Data available upon request from the authors.
References
Bharucha AE, Knowles CH, Mack I et al (2022) Faecal incontinence in adults. Nat Rev Dis Prim 8:53. https://doi.org/10.1038/s41572-022-00381-7
Mack I, Hahn H, Gödel C et al (2023) Global Prevalence of Fecal Incontinence in Community-Dwelling Adults: A Systematic Review and Meta-analysis. Clin Gastroenterol Hepatol. https://doi.org/10.1016/j.cgh.2023.09.004
Group ES of C (ESCP) C, Dulskas A (2023) The 2022 European Society of Coloproctology (ESCP) global snapshot audit of faecal incontinence: Study protocol. Color Dis 25:1694–1697. https://doi.org/10.1111/codi.16633
Gallo G, Realis Luc A (2023) Epidemiology, anorectal anatomy, physiology and pathophysiology of continence. In: Docimo L (ed) Anal Incontinence, Updates in Surgery. Springer, Cham, pp 9–17
Knol ME, Bastiaannet E, DeRuiter MC et al (2023) Clinical characteristics of phenotypes of fecal incontinence. Tech Coloproctol 27:475–480. https://doi.org/10.1007/s10151-023-02778-2
Hayden DM, Weiss EG (2011) Fecal incontinence: Etiology, evaluation, and treatment. Clin Colon Rectal Surg 24:64–70. https://doi.org/10.1055/s-0031-1272825
Menees S, Chey WD (2022) Fecal Incontinence: Pathogenesis, Diagnosis, and Updated Treatment Strategies. Gastroenterol Clin North Am 51:71–91. https://doi.org/10.1016/j.gtc.2021.10.005
Lee YY (2014) What’s new in the toolbox for constipation and fecal incontinence? Front Med 1:1–9. https://doi.org/10.3389/fmed.2014.00005
Bortolotti M (2006) A novel antireflux device based on magnets. J Biomech 39:564–567. https://doi.org/10.1016/j.jbiomech.2004.10.035
Bortolotti M (2014) The “magnetic collar”: The ultimate solution for gastroesophageal reflux? Scand J Gastroenterol 49:511–512. https://doi.org/10.3109/00365521.2013.878383
Bortolotti M (2021) Magnetic challenge against gastroesophageal reflux. World J Gastroenterol 27:8227–8241. https://doi.org/10.3748/wjg.v27.i48.8227
Gagner M (2021) History of Magnets Used in Surgery BT - Magnetic Surgery. In: International S (ed) Gagner M. Publishing, Cham, pp 19–25
Mantoo S, Meurette G, Podevin J, Lehur PA (2012) The magnetic anal sphincter: A new device in the management of severe fecal incontinence. Expert Rev Med Devices 9:483–490. https://doi.org/10.1586/erd.12.38
Bortolotti M (2022) Magnetic sphincter for anal incontinence: an update. Mini-invasive Surg 6:45. https://doi.org/10.20517/2574-1225.2022.33
Lehur PA, Wyart V, Riche VP (2016) SaFaRI: sacral nerve stimulation versus the Fenix® magnetic sphincter augmentation for adult faecal incontinence: a randomised investigation. Int J Colorectal Dis 31:1505. https://doi.org/10.1007/s00384-016-2531-8
Williams AE, Croft J, Napp V et al (2016) SaFaRI: sacral nerve stimulation versus the FENIX™ magnetic sphincter augmentation for adult faecal incontinence: a randomised investigation. Int J Colorectal Dis 31:465–472. https://doi.org/10.1007/s00384-015-2492-3
Jayne DG, Williams AE, Corrigan N et al (2021) Sacral nerve stimulation versus the magnetic sphincter augmentation device for adult faecal incontinence: The SaFaRI RCT. Health Technol Assess (Rockv) 25:1–95. https://doi.org/10.3310/hta25180
Higgins JPT, Green S, Ben Van Den A (2020) Cochrane Handbook for Systematic Reviews of Interventions. https://doi.org/10.1002/9781119536604
Hutton B, Salanti G, Caldwell DM et al (2015) The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: Checklist and explanations. Ann Intern Med 162:777–784. https://doi.org/10.7326/M14-2385
Lehur PA, McNevin S, Buntzen S et al (2010) Magnetic anal sphincter augmentation for the treatment of fecal incontinence: A preliminary report from a feasibility study. Dis Colon Rectum 53:1604–1610. https://doi.org/10.1007/DCR.0b013e3181f5d5f7
Wong MTC, Meurette G, Wyart V, Lehur PA (2012) Does the magnetic anal sphincter device compare favourably with sacral nerve stimulation in the management of faecal incontinence? Color Dis 14:323–329. https://doi.org/10.1111/j.1463-1318.2012.02995.x
Barussaud ML, Mantoo S, Wyart V et al (2013) The magnetic anal sphincter in faecal incontinence: Is initial success sustained over time? Color Dis 15:1499–1503. https://doi.org/10.1111/codi.12423
Bridoux V, Gourcerol G, Leroi AM et al (2014) Response to barussaud et al.: The magnetic anal sphincter in faecal incontinence, is initial success sustained over time? Color Dis 16:145–146. https://doi.org/10.1111/codi.12519
Pakravan F, Helmes C (2015) Magnetic anal sphincter augmentation in patients with severe fecal incontinence. Dis Colon Rectum 58:109–114. https://doi.org/10.1097/DCR.0000000000000263
Sugrue J, Lehur PA, Madoff RD et al (2017) Long-term Experience of Magnetic Anal Sphincter Augmentation in Patients with Fecal Incontinence. Dis Colon Rectum 60:87–95. https://doi.org/10.1097/DCR.0000000000000709
Kim M, Meurette G, Ragu R et al (2019) Functional Results and Quality of Life Following Magnetic Anal Sphincter Augmentation in Severely Incontinent Patients. Ann Surg 269:310–314. https://doi.org/10.1097/SLA.0000000000002512
McGuinness LA, Higgins JPT (2020) Risk-of-bias VISualization (robvis): An R package and Shiny web app for visualizing risk-of-bias assessments. Res Synth Methods n/a. https://doi.org/10.1002/jrsm.1411
Hozo SP, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Med Res Methodol 5:1–10. https://doi.org/10.1186/1471-2288-5-13
Williams AE, Croft J, Napp V et al (2016) SaFaRI: sacral nerve stimulation versus the FENIX™ magnetic sphincter augmentation for adult faecal incontinence: a randomised investigation. Dis Colon Rectum 31:310–314. https://doi.org/10.1007/DCR.0b013e3181f5d5f7
Faucheron JL, Sage PY, Trilling B (2019) Erosion Rate of the Magnetic Sphincter Augmentation Device Is Much Higher for Anal Incontinence than for Antireflux. J Gastrointest Surg 23:389–390. https://doi.org/10.1007/s11605-018-4032-2
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
Conception and design of the study: Liapis, Perivoliotis.
Acquisition of data: Liapis, Moula.
Drafting the article: Liapis, Perivoliotis, Moula.
Critical revision: Baloyiannis, Lytras, Psarianos, Stavrou.
Final approval: Baloyiannis, Lytras.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
Not applicable.
Informed consent to participate
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Appendix
Appendix
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liapis, S.C., Perivoliotis, K., Moula, A.I. et al. Is magnetic anal sphincter augmentation still an option in fecal incontinence treatment: a systematic review and meta-analysis. Langenbecks Arch Surg 409, 98 (2024). https://doi.org/10.1007/s00423-024-03288-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00423-024-03288-x