Abstract
Purpose
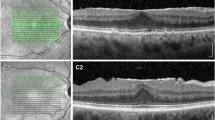
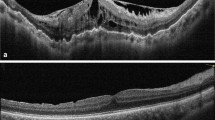
To assess epiretinal membrane (ERM) formation, severity, and the associated risk factors after scleral buckling using en face optical coherence tomography (OCT) images.
Methods
Medical records of 61 consecutive patients (66 eyes) with rhegmatogenous retinal detachment who underwent scleral buckling were retrospectively reviewed. Posterior vitreous detachment (PVD) was determined based on B-scan OCT images. En face OCT images were used to visualize the ERM and retinal folds. ERM formation was identified by comparing en face images pre- and post-surgery. The maximum depth of the retinal folds (MDRF) was measured using en face imaging to objectively assess traction strength.
Results
ERM formation occurred in 15 (22.7%) eyes at the final visit; the foveal pit was preserved in all cases. Parafoveal retinal folds were present in 5 (7.6%) eyes, with a mean MDRF of 21.8 ± 12.6 µm. No significant difference was observed in best-corrected visual acuity (logarithm of the minimal angle of resolution) between the ERM formation (-0.019 ± 0.128) and non-ERM formation (-0.001 ± 0.213) groups at the final visit (P = 0.593; Mann-Whitney U test). Multivariate logistic regression analysis revealed that older age and the presence of PVD were significant risk factors for ERM formation (odds ratio 1.07, 95% confidence interval 1.01–1.14, P = 0.032; odds ratio 5.26, 95% confidence interval 1.06–26.10, P = 0.042; respectively).
Conclusion
ERM occurred in 22.7% of cases but was mild and did not affect visual acuity. Older age and the presence of PVD are risk factors for ERM formation.



Similar content being viewed by others
Data availability
Data are available on request.
References
Matoba R, Morizane Y (2021) Surgical treatment of epiretinal membrane. Acta Med Okayama 75:403–413. https://doi.org/10.18926/AMO/62378
Lobes LA Jr, Burton TC (1978) The incidence of macular pucker after retinal detachment surgery. Am J Ophthalmol 85:72–77. https://doi.org/10.1016/s0002-9394(14)76668-1
Azad RV, Chanana B, Sharma YR, Vohra R (2007) Primary vitrectomy versus conventional retinal detachment surgery in phakic rhegmatogenous retinal detachment. Acta Ophthalmol Scand 85:540–545. https://doi.org/10.1111/j.1600-0420.2007.00888.x
Kobashi H, Takano M, Yanagita T et al (2014) Scleral buckling and pars plana vitrectomy for rhegmatogenous retinal detachment: an analysis of 542 eyes. Curr Eye Res 39:204–211. https://doi.org/10.3109/02713683.2013.838270
Shu I, Ishikawa H, Nishikawa H et al (2019) Scleral buckling versus vitrectomy for young japanese patients with rhegmatogenous retinal detachment in the era of microincision surgery: real-world evidence from a multicentre study in Japan. Acta Ophthalmol 97:e736–e741. https://doi.org/10.1111/aos.14050
Hirakata T, Hiratsuka Y, Yamamoto S et al (2021) Risk factors for macular pucker after rhegmatogenous retinal detachment surgery. Sci Rep 11:18276. https://doi.org/10.1038/s41598-021-97738-x
Koriyama M, Nishimura T, Matsubara T et al (2007) Prospective study comparing the effectiveness of scleral buckling to vitreous surgery for rhegmatogenous retinal detachment. Jpn J Ophthalmol 51:360–367. https://doi.org/10.1007/s10384-007-0463-0
Ahmadieh H, Moradian S, Faghihi H et al (2005) Anatomic and visual outcomes of scleral buckling versus primary vitrectomy in pseudophakic and aphakic retinal detachment: six-month follow-up results of a single operation–report no. 1. Ophthalmology 112:1421–1429. https://doi.org/10.1016/j.ophtha.2005.02.018
Huang C, Fu T, Zhang T et al (2013) Scleral buckling versus vitrectomy for macula-off rhegmatogenous retinal detachment as accessed with spectral-domain optical coherence tomography: a retrospective observational case series. BMC Ophthalmol 13:12. https://doi.org/10.1186/1471-2415-13-12
Uemura A, Ideta H, Nagasaki H et al (1992) Macular pucker after retinal detachment surgery. Ophthalmic Surg 23:116–119
Hirano M, Morizane Y, Kimura S et al (2018) Assessment of lamellar macular hole and macular pseudohole with a combination of En face and radial B-scan optical coherence tomography imaging. Am J Ophthalmol 188:29–40. https://doi.org/10.1016/j.ajo.2018.01.016PMID-29360459
Hirano M, Morizane Y, Kanzaki Y et al (2020) En face image-based analysis of retinal traction caused by epiretinal membrane and its relationship with visual functions. Retina 40:1262–1271. https://doi.org/10.1097/IAE.0000000000002569
Fujiwara A, Kanzaki Y, Kimura S et al (2021) En face image-based classification of diabetic macular edema using swept source optical coherence tomography. Sci Rep 11:7665. https://doi.org/10.1038/s41598-021-87440-3
Kanzaki S, Kanzaki Y, Doi S et al (2021) En face image-based analysis of epiretinal membrane formation after surgery for idiopathic epiretinal membrane. Ophthalmol Retina 5:815–823. https://doi.org/10.1016/j.oret.2020.10.017
Kanzaki Y, Doi S, Matoba R et al (2021) Objective and quantitative estimation of the optimal timing for epiretinal membrane surgery on the basis of metamorphopsia. Retina. https://doi.org/10.1097/IAE.0000000000003401
Kanzaki Y, Matoba R, Kimura S et al (2023) Epiretinal membrane impairs the inner retinal layer in a traction force-dependent manner. Ophthalmol Sci 3:100312. https://doi.org/10.1016/j.xops.2023.100312
Mino M, Matoba R, Kanzaki Y et al (2023) Quantitative analyses of retinal traction force and metamorphopsia in lamellar macular hole and related diseases. Ophthalmol Sci 3:100305. https://doi.org/10.1016/j.xops.2023.100305
Matoba R, Kanzaki Y, Kimura S et al (2023) A factor for predicting simultaneous internal limiting membrane peeling during epiretinal membrane removal: swept-source optical coherence tomography-based evaluation of epiretinal membrane adhesion to the retina. Jpn J Ophthalmol. https://doi.org/10.1007/s10384-023-00993-w
Matoba R, Kanzaki Y, Doi S et al (2021) Assessment of epiretinal membrane formation using en face optical coherence tomography after rhegmatogenous retinal detachment repair. Graefes Arch Clin Exp Ophthalmol 259:2503–2512. https://doi.org/10.1007/s00417-021-05118-y
Govetto A, Lalane RA 3rd, Sarraf D et al (2017) Insights into epiretinal membranes: presence of ectopic inner foveal layers and a new optical coherence tomography staging scheme. Am J Ophthalmol 175:99–113. https://doi.org/10.1016/j.ajo.2016.12.006
Moon SY, Park SP, Kim Y-K (2020) Evaluation of posterior vitreous detachment using ultrasonography and optical coherence tomography. Acta Ophthalmol 98:e29–e35. https://doi.org/10.1111/aos.14189
Pang CE, Freund KB, Engelbert M (2014) Enhanced vitreous imaging technique with spectral-domain optical coherence tomography for evaluation of posterior vitreous detachment. JAMA Ophthalmol 132:1148–1150. https://doi.org/10.1001/jamaophthalmol.2014.1037
Abraham JR, Ehlers JP (2020) Posterior vitreous detachment: methods for detection. Ophthalmol Retina 4:119–121
Clarkson JG, Green WR, Massof D (1977) A histopathologic review of 168 cases of preretinal membrane. Am J Ophthalmol 84:1–17. https://doi.org/10.1016/0002-9394(77)90317-8
Machemer R, van Horn D, Aaberg TM (1978) Pigment epithelial proliferation in human retinal detachment with massive periretinal proliferation. Am J Ophthalmol 85:181–191. https://doi.org/10.1016/s0002-9394(14)75946-x
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
R.M. designed the study; R.M., Y.K., and T.M. analyzed and interpreted the data; S.K., M.M.H., and Y.S. collected the data; R.M. wrote the manuscript; and Y.M. supervised the study. All the authors reviewed the manuscript.
Corresponding author
Ethics declarations
Ethics approval
All investigative procedures were conducted in accordance with the tenets of the Declaration of Helsinki, and the study was approved by the Ethics Committee of Okayama University Hospital, Okayama, Japan (K2205-010).
Informed consent
Informed consent was obtained from all study participants.
Conflict of interests
The authors have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Matoba, R., Kanzaki, Y., Morita, T. et al. Evaluation of epiretinal membrane formation after scleral buckling for treating rhegmatogenous retinal detachment: En face optical coherence tomography image-based study. Graefes Arch Clin Exp Ophthalmol 262, 469–476 (2024). https://doi.org/10.1007/s00417-023-06285-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00417-023-06285-w