Abstract
The implementation status of clinical guidelines is, despite their important role in connecting research with practice, frequently not satisfactory. This study aims to investigate the implementation status of the current German guideline for schizophrenia. Moreover, the attitude toward a living guideline has been explored for the first time by presenting screenshots of the German schizophrenia guideline transferred to a digital living guideline format called MAGICapp. A cross-sectional online survey was performed under the participation of 17 hospitals for psychiatry and psychosomatic medicine in Southern Germany and one professional association for German neurologists and psychiatrists. 439 participants supplied sufficient data for analysis. 309 provided complete data sets. Regarding the current guideline for schizophrenia and key recommendations, a large awareness-to-adherence gap was found. Group comparisons between different professions (caregivers, medical doctors, psychologists/psychotherapists, psychosocial therapists) detected differences in the implementation status showing higher awareness and agreement with the schizophrenia guideline and its key recommendations among medical doctors compared to psychosocial therapists and caregivers. Moreover, we detected differences in the implementation status of the guideline as a whole and its key recommendations between specialist and assistant doctors. The attitude toward an upcoming living guideline was mostly positive, especially among younger healthcare professionals. Our findings confirm an awareness-to-adherence gap, not only for the current schizophrenia guideline in general but also for its key recommendations with apparent differences between professions. Overall, our results show promising positive attitudes toward the living guideline for schizophrenia among healthcare providers, suggesting that a living guideline may be a supportive tool in everyday clinical practice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background
The implementation of practical guidelines in routine clinical practice is a challenge. It is a well-known problem that in spite of a multitude of existing clinical guidelines, the implementation in clinical practice remains insufficient worldwide [1,2,3,4]. For this reason, the focus of research has increasingly shifted from the development to the implementation of guidelines [5].
However, why is the implementation of clinical guidelines so important? Non-maleficence is one of the four basic principles in medical ethics. It is impossible in clinical practice to never do harm; however, decision-making in healthcare requires a thorough consideration of doing no net harm [6]. Evidence-based guidelines are intended to support clinicians in making decisions, not only by ensuring that harm is prevented, but also by providing optimal healthcare [6]. However, studies in different countries show that many patients receive care that is not needed or even potentially harmful [3, 7, 8]. Moreover, guidelines support optimizing health outcomes [5, 9,10,11,12,13]. This illustrates the importance of improving the implementation of guidelines in clinical practice.
In 2019, the German evidence- and consensus-based S3 guideline for schizophrenia [14, 15] was published. A recent preceding study conducted in the year of publication of the guideline showed that in spite of a high acceptance of this guideline, more than half of the participants did not use the guideline in everyday clinical care [16].
One reason for these results are the multifaceted barriers and facilitating factors in guideline adherence [5, 16,17,18]. Several frameworks exist allocating the barriers and facilitators to different categories. One of them is the in 1996 by Pathman and colleagues developed awareness-to-adherence model [19], a four-step model including awareness, agreement, adoption, and adherence. It postulates that a sequence of cognitive and behavioral processes is necessary so that guidelines can have an impact on physicians’ clinical behavior. Clinicians follow practical guidelines if they are aware of the guidelines, intellectually agree with them and then decide to follow them for some patients. Finally, the path to guideline adherence also requires regular adherence to it for most patients. A progressive drop off over the four steps is observed in general, which is described as a ‘pipeline’, with research evidence ‘leaks’ leading to a reduced guideline implementation [20].
A further reason is the fact that medical knowledge is increasing exponentially; consequently, many guidelines are already out of date when published [21,22,23,24,25]. Moreover, most clinicians cannot keep up with the amount of increasing knowledge [21, 26]. One strategy to address this problem is the development of so-called living guidelines. Living guidelines are an optimization of the guideline development process as individual recommendations can be updated as soon as relevant new evidence is available [22]. In that regard, the user’s perspective on the concept of living guidelines has not yet been investigated.
This study aims to explore the current implementation status of the German evidence-and consensus-based guideline for schizophrenia [14, 15] and its key recommendations as well as the attitude of users toward a future living guideline for schizophrenia.
Design and methods
Subjects and recruitment
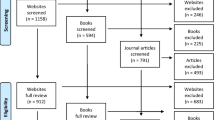
The cross-sectional online survey was performed from 01/2022 to 04/2022. In total, 17 hospitals for psychiatry, psychotherapy, and psychosomatic medicine in Southern Germany (see Supplementary Table 1) and one professional association for German neurologists and psychiatrists (BVDN: Berufsverband Deutscher Nervenärzte e. V.) participated in the study by forwarding the link to the survey to their clinical staff/members [27]. We recruited caregivers of the participating hospitals in the same manner as the other professions. After approximately three weeks, a reminder mail was sent. The licensed LimeSurveyR version 5.3.4+ (LMU hospital) was used to generate the questionnaire, conduct the survey, and to ensure an anonymous participation. Figure 1 displays the recruitment and study flow chart. The data protection officer of the University Hospital Munich reviewed the survey and the local ethical committee approved the project (reference number 21-0780). The trial has been performed according to the latest version of the Declaration of Helsinki [28]. If not stated otherwise, the term “schizophrenia guideline” refers to the current German evidence-and consensus-based guideline for schizophrenia (as of 2019) [14].
Survey structure
The survey aimed to identify the compliance (a) of the general guideline for schizophrenia and (b) of four-key recommendations (see Supplementary Table 2) using the concept of an adapted awareness-to-adherence questionnaire by Pathman et al. [19]. The four recommendations are listed in Supplementary Table 2 and were selected in advance by the editors of the German schizophrenia guideline based on their high-evidence and recommendation levels and practical importance (dose of antipsychotics, antipsychotics for relapse prevention, management of severe weight gain, and application of cognitive behavioral therapy).
Regarding the guideline as a whole and the four key recommendations, participants were asked if they were familiar, agreed with the guideline/recommendation, assessed it as appropriate and feasible and how high they estimated the percentage of patients receiving treatment according to the guideline/respective recommendation. In our analysis, we assigned Pathman’s four categories to these four questions, i.e., awareness, agreement, adoption, and adherence.
Respondents were classified as aware if they were “familiar” or “very familiar” (five-point Likert scale) with the guideline (question 13) or a specific recommendation (questions 17, 21, 25, 32), respectively. Agreement was assessed by participants indicating whether they agreed with the guideline (question 14)/recommendation (questions 18, 22, 26, 30), nominal scale: “yes” versus “no”. They were classified as (potential) adopters if they regarded the guideline (question 15)/recommendation (questions 19, 23, 27, 31) as appropriate and feasible (five-point Likert scale: “agree” and “fully agree”). Finally, those who indicated that 90% or greater of their patients received a treatment according to the guideline (question 16)/the specific recommendation (questions 20, 24, 28, 32) were considered as adherers. Additionally, the attitude toward the living guideline for schizophrenia was investigated on a five-point Likert scale (agreement: 1 = strongly disagree, 3 = neutral, 5 = strongly agree) by assessing user-friendliness (questions 33, 34, 36), the perceived practicability (questions 37, 38, 39) as well as preferences in the application and potential benefits as compared to the print version (questions 40, 41). At the time of the study, no living guideline for mental disorders was available [29]. Therefore, we introduced the concept of a living guideline by an explanatory text and presented screenshots of the digitally prepared guideline for schizophrenia within the MAGICapp system, which is an evidence ecosystem making the whole process of a living guideline possible [30].
With regard to the implementation status of the guideline for schizophrenia, we investigated contrasts between the different professions: medical doctors, psychologists/psychotherapists, psychosocial therapists, and caregivers. For medical doctors, we additionally explored contrasts between specialist doctors and assistant doctors. Concerning the attitude toward the living guideline, we had a closer look at age differences assuming difference in digital competence across age groups [31]. Please see the supplement for the provided text and examples as well as the whole questionnaire in the supplement. The questionnaire was provided in German language and translated in English by the authors for this publication (see supplement).
Statistical analysis
All analyses were carried out in IBM SPSS for Windows (version 28) with a significance level of α = 0.05. Descriptive statistics are displayed with frequency and percentage distributions for binary data. For continuous data, means and standard deviations are presented and additionally medians for categorical data. Intergroup differences were assessed using Chi2 tests in case of binary data. For categorical data (e.g., Likert scale), Mann–Whitney-U tests, Kruskal–Wallis tests for between group analyses (Dunn–Bonferroni tests for subgroup analyses in case of significant intergroup differences) or Wilcoxon signed-rank tests (in case of dependent samples within subjects) were used. For continuous data, we applied independent sample t-tests or one-way ANOVAs (Bonferroni tests for subgroup analyses in case of significant intergroup differences, Welch tests homogeneity of variance was violated). In addition to age groups [young (20–34 years old) vs. middle-aged (35–49 years old) vs. older mental healthcare professionals (50–66 years old)], professional groups were compared. Therefore, we conducted intergroup comparisons between medical doctors, psychotherapists/psychologists, psychosocial therapists as well as caregivers. See Table 1 for a detailed listing of the associated occupational profiles.
Results
Participants’ characteristics
309 respondents finalized the survey ultimately. Of the 524 participants who initially participated (response to at least one question) in the survey, 439 mental healthcare professionals provided sufficient data for analyses. 85 participants were excluded from analyses due to missing experience in the treatment of mental disorders (n = 22) or the absence of answering at least one content-related question (n = 63). Moreover, 130 respondents dropped out along the questionnaire, leaving 309 respondents who completed the survey, see Fig. 1. Demographic information is shown in Table 1. Comparisons on demographic information between excluded and included participants, professions, specialist and assistant doctors as well as age groups are shown in the Supplementary Results (Supplementary Tables 3–6).
Awareness, agreement, adoption, and adherence: implementation status of the guideline for schizophrenia and its key recommendations
In total, less than half of the participants were aware of (40%), agreed with (43%), and adopted (41%) the guideline for schizophrenia. Less than one-tenth (7%) of the surveyed mental healthcare professionals reported to adhere to the schizophrenia guideline as a whole. Regarding the specific recommendations, awareness ranged between 38% for recommendation 3 (severe weight gain) and 81% for recommendation 2 (relapse prevention). Likewise, recommendation 3 (severe weight gain) exhibited the lowest rates on agreement (36%), adoption (33%), and adherence (5%), whereas recommendation 2 (relapse prevention) received the highest rates on agreement (88%), adoption (74%), and adherence (40%). Throughout the recommendations, a large discrepancy between awareness and adherence as well as between agreement and adherence was found. The greatest awareness-to-adherence gap for all four professions together was detected for recommendation 4 (psychotherapy)—68% of the participants fell off the track from awareness to adherence and 74% agreed on the recommendation but did not adhere to it. For complete test statistics and an overview of the evaluated recommendations, see Table 2 and Supplementary Table 2, respectively.
Group comparisons—profession
Chi2 tests of independence indicate higher awareness and agreement rates of the current schizophrenia guideline as a whole as well as for all four recommendations among medical doctors compared to psychosocial therapists and caregivers (ps ≤ 0.036) (see Fig. 2). Additionally, psychologists/psychotherapists were more aware of and agreed more with recommendation 4 (psychotherapy) than psychosocial therapists and caregivers (ps ≤ 0.006). Moreover, psychologists/psychotherapists regarded recommendation 4 (psychotherapy) as more appropriate and feasible in the treatment of patients with schizophrenia (adoption) than any other profession (medical doctors, psychosocial therapists, caregivers), ps ≤ 0.018 (see Fig. 3). Regarding adherence, the estimated proportion of patients who receive a treatment according to the recommendation or the schizophrenia guideline as a whole, no significant differences between professions were found—except for recommendation 3 (relapse prevention): medical doctors reported a higher adherence rate compared to psychosocial therapists, p = 0.001. For complete test statistics, see Table 2.
The bar chart shows the implementation status of the guideline as a whole among different professions (medical doctors, psychologists/psychotherapists, psychosocial therapists, caregivers). An awareness-to-adherence gap can be seen throughout all professions. Higher awareness and agreement rates of the current schizophrenia guideline as a whole can be detected among medical doctors compared to psychosocial therapists, psychologists/psychotherapists and caregivers (ps <0.001). For complete test statistics, see Table 2
The bar chart depicts the implementation status of specific recommendations (A–D) among different professions (medical doctors, psychologists/psychotherapists, psychosocial therapists, caregivers). Throughout the recommendations, a large discrepancy between awareness and adherence as well as between agreement and adherence was found for all four professions (A–D). Higher awareness and agreement rates of all four recommendations can be detected among medical doctors compared to psychosocial therapists and caregivers (ps ≤ 0.036) (A–D). In A, the implementation status of the recommendation dose of antipsychotics and in B, the implementation status of the recommendation relapse prevention is shown. The recommendation weight gain (C) is the only one with significant differences among professions regarding adherence: medical doctors reported a higher adherence rate compared to psychosocial therapists, p = 0.001. In D, the implementation status of the recommendation psychotherapy is displayed. Psychologists/psychotherapists were more aware of and agreed more with the psychotherapy recommendation than psychosocial therapists and caregivers (ps ≤ 0.006). Moreover, psychologists/psychotherapists regarded the psychotherapy recommendation as more appropriate and feasible in the treatment of patients with schizophrenia (adoption) than any other profession (medical doctors, psychosocial therapists, caregivers), ps ≤ 0.018. For complete test statistics, see Table 2
Group comparisons—specialist versus assistant doctors
Chi2 tests of independence show higher awareness, agreement and adoption rates among specialist doctors for the schizophrenia guideline as a whole, ps ≤ 0.002 (see Supplementary Table 8). Moreover, specialist doctors stated to be more aware of recommendation 1 (dose of antipsychotics) and 4 (psychotherapy) and agreed more to recommendation 4 than assistant doctors, ps ≤ 0.022. Among assistant doctors, recommendation 3 (severe weight gain) exhibited higher agreement, adoption and adherence rates than among specialist doctors, ps ≤ 0.026.
Attitude toward the living guideline for schizophrenia
To explore the attitude toward the living guideline for schizophrenia, three screenshots of the unpublished digital layout of the planned living guideline were presented for illustration. To give a broad overview, the table of contents, two examples of recommendations (social skills training and cognitive remediation) as well as a graphical comparison of two treatment options (e.g., to use for shared decision-making) were shown (Please see supplement for more details). About two-thirds (64%) of the surveyed mental healthcare professionals would currently, in the absence of an available living guideline, prefer the living guideline to the printed format, and three-quarters (75%) expressed awareness about the advantages of the living guideline over the printed version. Based on the presented images of the living guideline for schizophrenia, more than half of the participants regarded the living guideline as user-friendly—68% find the layout appealing and the content clearly presented, 77% can imagine getting along well with the living format and for 52% the living guideline seemed to be clearer than the previous print version. Regarding clinical practicability/relevance, more than half of the respondents considered the living guideline as more practical than the print format (62%) and as a valuable tool in everyday clinical practice (80%). However, the presented concept of a living guideline seemed to be more informative than the print version for only 39% of the surveyed mental healthcare professionals. See Table 3 for further descriptive information and the supplement for the description and presented pictures of the living guideline.
Group comparisons—age
Kruskal–Wallis tests showed significant differences between age groups concerning the attitude toward the living guideline. Young mental healthcare professionals (20–34 years old) showed a more positive attitude throughout all categories of a potential living guideline (user-friendliness, clinical practicability, general, mean value) than older participants (50–66 years old), ps ≤ 0.006, and a higher mean positive attitude than middle-aged respondents (35–49 years old), p = 0.003. No significant differences were found in the mean positive attitude between middle-aged and older participants, p = 0.291. For complete test statistics, see Table 4.
Discussion
This study ascertained the current implementation of the German guideline for schizophrenia approximately three years after its publication in March 2019. It further provides an initial assessment of the attitude toward the German living guideline for schizophrenia (currently under development).
In a previous study, an insufficient implementation status of the guideline for schizophrenia was shown [16]. Beyond this, we investigated the implementation status of four key recommendations and differences in implementation between professions. As a living guideline for schizophrenia is currently under development, we examined the attitude toward a living guideline and discrepancies among different age groups.
Two-fifths of the participants were aware of, agreed with, and adopted [19] the guideline for schizophrenia, less than one-tenth of the surveyed mental healthcare professionals reported to adhere to the schizophrenia guideline as a whole, showing an awareness-, agreement-, as well as an adoption-to-adherence gap in guideline use. This result is consistent with findings of a study on the current German schizophrenia guideline conducted in 2019 directly after its publication [16], and other mental health or somatic guidelines [32, 33]. Similarly, a large discrepancy between awareness and adherence as well as between agreement and adherence was also shown for specific recommendations. The greatest awareness-to-adherence gap for all four professions together was detected for the psychotherapy recommendation—68% of the participants fell off the track from awareness to adherence and 74% agreed on the recommendation but did not adhere to it. A possible reason could be the lack of time [34] for psychotherapy in an inpatient setting due to work load and/or a lack of prioritization of psychotherapy compared to other treatment forms, e.g., pharmacological treatment. Moreover, recommendation 3 regarding severe weight gain exhibited the lowest rates on awareness, agreement, adoption, and adherence out of all recommendations in total. This may be the result of a lack of experience with prescribing the recommended metformin (Evidence level A) and concerns regarding side effects or interaction with other drugs. Another potential explanation is that the consequences of antipsychotic-induced weight gain are underestimated [35]. A close look regarding barriers and facilitators influencing the gap to adherence will, therefore, be of importance for further research.
Moreover, analyses showed significant differences between professions by showing higher awareness and agreement rates of the current schizophrenia guideline as a whole as well as for all four recommendations among medical doctors compared to psychosocial therapists and caregivers. Psychologists/psychotherapists were more aware and agreed more to the psychotherapy recommendation than psychosocial therapists and caregivers and regarded the recommendation as more appropriate and feasible in the treatment of patients with schizophrenia (adoption) than any other profession (medical doctors, psychosocial therapists, caregivers). Profession-specific differences in guideline implementation are in line with previously conducted studies in mental health as well as general health provision [16, 36] and highlight the need for greater attention to profession-specific barriers and facilitators in further research. The reasons for physicians’ higher awareness and agreement with the guideline may be that they usually represent the case-leading professional group in multiprofessional inpatient settings. Furthermore, these results could also be explained by the fact that the guideline as a whole contains a greater number of and more specific recommendations for medical doctors compared with other professional groups and that the majority of the experts involved in the development of the guideline are physicians [14].
The different curricula of the professions in Germany may play a substantial role. For example, medical doctors have a smaller proportion of psychotherapeutic content in their training compared to psychotherapists. Psychotherapists are taught various psychotherapeutic interventions during their studies, and this knowledge is expanded during three to five years of practical and theoretical training of psychotherapy. Medical doctors have far less modules on that topic, as psychotherapy is solely one component of a comprehensive specialist training program. It should be further investigated how the training/studies of various professions may differ regarding guidelines (e.g., guidelines are more used in training of medical doctors, and in training of psychotherapists, manuals are more predominant) and how this may influence the implementation of such.
Our results show higher awareness, agreement, and adoption rates among specialist doctors for the schizophrenia guideline as a whole compared to assistant doctors. Specialist doctors were not only more aware of the recommendation regarding dose of antipsychotics and psychotherapy but also agreed more to the latter recommendation than assistant doctors. This may be a reflection of the expertise associated with an increased professional experience.
On contrary, recommendation 3 (severe weight gain) exhibited higher agreement, adoption, and adherence rates among assistant doctors than specialist doctors showing further differences between the more experienced and usually older professionals and assistants. Further research is needed investigating whether a more recent education and/or the amount of experience influences the present results.
Our results indicate acceptance of the concept of a living guideline among the surveyed mental healthcare professionals—about two-thirds showed positive attitude toward the presented concept of a living guideline. More than half of the subjects evaluate the living guideline as clearer, more practical and generally preferable to the print version. However, less than half of the subjects regarded the living guideline as more informative than the print version. This implies an assumption among clinicians that the living format might not be an improvement regarding additional information content.
We detected significant differences between age groups on attitude toward the living guideline. Young mental healthcare professionals showed a more positive attitude throughout all categories than older participants did, and a higher mean positive attitude than middle-aged respondents did. An uncertainty dealing with new technology is very common in older professionals [31]. In addition, younger professionals tend to have a greater affinity for technology. Living guidelines are being increasingly used in practice [31] and could, therefore, be more incorporated into the training of younger practitioners. Further research should investigate if these findings are in agreement with perceived potential barriers and facilitating factors in the use of the upcoming living guideline for schizophrenia.
Limitations regarding the results of this study first include disadvantages related to online surveys, e.g., survey frauds, response bias, and lack of representativeness [37]. Due to data protection settings of the used software and the anonymous nature of our study, we did not implement tracking of IT addresses. Thus, we cannot exclude, e.g., that some participants participated more than one time. However, this scenario appears to be unlikely as our sample consisted of professionals from inpatient and outpatient settings of our model region and all participants were asked to answer the questionnaire only one time. Our setting differs significantly from, e.g., settings with recruitment from social media platforms where multiple participants are a relevant source of bias. However, our approach may have resulted in a sampling bias as specific clinics in the south of Germany were contacted to participate in the survey. Although the questionnaire is predominantly based on theoretical frameworks [19, 38], it was developed and adjusted for specific research questions, and thus be potentially biased by the researchers. Further, the reader should bear in mind that the living guideline is still under development and our participants received only a conceptual presentation. Moreover, significant differences in demographic information such as age, gender, work setting and experience with the treatment of schizophrenia between professions were detected. Additionally, significant differences between included and excluded participants could be identified concerning gender, profession (medical doctors and other professions), setting (public hospital, research, and other) as well as age (Supplementary Tables 3–6). Therefore, analyses should be interpreted with caution.
Conclusion
Overall, our findings show a high number of non-adherers to the current guideline of schizophrenia. More specifically, a discrepancy between awareness and adherence, not only for the current schizophrenia guideline as a whole, but also for selected four key recommendations was found. Differences between professions were detected—medical doctors showed higher awareness and agreement on the guideline for schizophrenia as well as on its key recommendations compared to caregivers and psychosocial therapists. Therefore, the role of different profession-specific curricula should be considered in the efforts to increase guideline knowledge and acceptance and, consequently, in the process of implementation. In addition to profession-specific differences, our results indicate a crucial role of clinician’s experience in guideline implementation—higher rates of awareness, agreement, and adoption of the overall schizophrenia guideline were found among specialists compared to assistant doctors.
Overall, our results show promising positive attitudes toward the living guideline for schizophrenia among healthcare providers, suggesting that a living guideline may be a supportive tool in everyday clinical practice. Nevertheless, the development of new guideline formats (e.g., living) cannot address all challenges in guideline implementation. Yet, living guidelines can be helpful to provide more versatile, responsive, and, thus, more user-oriented guidelines (e.g., adapted to profession, experience level, age).
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Girlanda F et al (2017) The evidence-practice gap in specialist mental healthcare: systematic review and meta-analysis of guideline implementation studies. Br J Psychiatry 210(1):24–30. https://doi.org/10.1192/bjp.bp.115.179093
Waldorff FB et al (2003) Implementation of a clinical dementia guideline. A controlled study on the effect of a multifaceted strategy. Scand J Prim Health Care 21(3):142–147. https://doi.org/10.1080/02813430310005136
Grol R (2001) Successes and failures in the implementation of evidence-based guidelines for clinical practice. Med Care 39:46–54
Pereira VC et al (2022) Strategies for the implementation of clinical practice guidelines in public health: an overview of systematic reviews. Health Res Policy Syst 20(1):13. https://doi.org/10.1186/s12961-022-00815-4
Fischer F et al (2016) Barriers and Strategies in Guideline Implementation—a scoping review. Healthcare (Basel). https://doi.org/10.3390/healthcare4030036
Schünemann HJ (2011) Guidelines 2.0: do no net harm-the future of practice guideline development in asthma and other diseases. Curr Allergy Asthma Rep 11(3):261–268. https://doi.org/10.1007/s11882-011-0185-8
Grol R, Grimshaw J (2003) From best evidence to best practice: effective implementation of change in patients’ care. The Lancet 362(9391):1225–1230. https://doi.org/10.1016/s0140-6736(03)14546-1
Schuster MA, McGlynn EA, Brook RH (1998) How good is the quality of health care in the United States? Milbank Q 76(4):517–563. https://doi.org/10.1111/1468-0009.00105
Miller ALea (2004) The Texas Medication Algorithm Project: clinical results for schizophrenia. Schizophrenia Bull 30:627–647
Weinmann S, Janssen B, Gaebel W (2005) Guideline adherence in medication management of psychotic disorders: an observational multisite hospital study. Acta Psychiatr Scand 112(1):18–25. https://doi.org/10.1111/j.1600-0447.2005.00547.x
Weinmann S et al (2008) Implementation of a schizophrenia practice guideline: clinical results. J Clin Psychiatry 69:1299–1306
Zimlichman E, Meilik-Weiss A (2004) Clinical guidelines as a tool for ensuring good clinical practice. IMAJ 6:626–627
Institute of Medicine Committee on Standards for Developing Trustworthy Clinical Practice, G., in Clinical Practice Guidelines We Can Trust, R. Graham, et al., Editors. 2011, National Academies Press (US) Copyright 2011 by the National Academy of Sciences. All rights reserved.: Washington (DC).
DGPPN. DGPPN, 2019. S3-Leitlinie Schizophrenie (WWW Document). Dtsch. Gesellschaft für Psychiatr. Psychother. Psychosom. und Nervenheilkd. 2019; Available from: https://www.awmf.org/leitlinien/detail/ll/038-009.html. Accessed 13 June 2022.
Hasan A et al (2020) Schizophrenia. Dtsch Arztebl Int 117(24):412–419. https://doi.org/10.3238/arztebl.2020.0412
Gaigl G et al (2021) Multifactorial barriers in the implementation of schizophrenia and psychosocial therapies guidelines: a quantitative study across different professions. Schizophr Res 228:425–434. https://doi.org/10.1016/j.schres.2021.01.010
Bighelli I et al (2016) Implementation of treatment guidelines for specialist mental health care. Cochrane Database Syst Rev 12:CD009780. https://doi.org/10.1002/14651858.CD009780.pub3
Forsner T et al (2010) Implementing clinical guidelines in psychiatry: a qualitative study of perceived facilitators and barriers. BMC Psychiatry 10:1–10. https://doi.org/10.1186/1471-244X-10-8
Pathman DE et al (1996) The awareness-to-adherence model of the steps to clinical guideline compliance. The case of pediatric vaccine recommendations. Med Care 34:873–889
Mickan S, Burls A, Glasziou P (2011) Patterns of ‘leakage’ in the utilisation of clinical guidelines: a systematic review. Postgrad Med J 87(1032):670–679. https://doi.org/10.1136/pgmj.2010.116012
Tendal B et al (2021) Weekly updates of national living evidence-based guidelines: methods for the Australian living guidelines for care of people with COVID-19. J Clin Epidemiol 131:11–21. https://doi.org/10.1016/j.jclinepi.2020.11.005
Akl EA et al (2017) Living systematic reviews: 4 Living guideline recommendations. J Clin Epidemiol 91:47–53. https://doi.org/10.1016/j.jclinepi.2017.08.009
Nature E (2021) Evidence-based medicine: how COVID can drive positive change. Nature 593(7858):168. https://doi.org/10.1038/d41586-021-01255-w
Paige E et al (2019) Living guidelines for absolute cardiovascular disease risk assessment and management. Heart Lung Circ 28(6):829–832. https://doi.org/10.1016/j.hlc.2019.01.014
Martínez García L et al (2014) The validity of recommendations from clinical guidelines: a survival analysis. CMAJ 186(16):1211–1219. https://doi.org/10.1503/cmaj.140547
Shaneyfelt TM (2001) Building bridges to quality. JAMA 286(20):2600–2601. https://doi.org/10.1001/jama.286.20.2600
BVDN. Berufsverband Deutscher Nervenärzte. Available from: https://www.berufsverband-nervenaerzte.de. Accessed 13 June 2022.
WMA Declaration of Helsinki. https://www.wma.net/policies-post/wma-declaration-of-helsinki-ethical-principles-for-medical-research-involving-human-subjects/. Accessed 14 Dec 2022.
Pielenz C et al (2022) From conventional to living guidelines—faster updates for better informed guidance? A scoping review. Z Evid Fortbild Qual Gesundhwes. https://doi.org/10.1016/j.zefq.2022.07.004
MAGICapp. MAGIC Evidence Ecosystem Foundation. Available from: https://magicevidence.org/approach/. Accessed 28 Nov 2022.
Wilson J et al (2021) Barriers and facilitators to the use of e-health by older adults: a scoping review. BMC Public Health 21(1):1556. https://doi.org/10.1186/s12889-021-11623-w
Batko B et al (2019) Physician adherence to treat-to-target and practice guidelines in rheumatoid arthritis. J Clin Med. https://doi.org/10.3390/jcm8091416
Yang J et al (2013) Experiences and barriers to implementation of clinical practice guideline for depression in Korea. BMC Psychiatry 13:150. https://doi.org/10.1186/1471-244x-13-150
Lugtenberg M et al (2016) Occupational physicians’ perceived barriers and suggested solutions to improve adherence to a guideline on mental health problems: analysis of a peer group training. BMC Health Serv Res 16:271. https://doi.org/10.1186/s12913-016-1530-3
Barton BB et al (2020) Update on weight-gain caused by antipsychotics: a systematic review and meta-analysis. Expert Opin Drug Saf 19(3):295–314. https://doi.org/10.1080/14740338.2020.1713091
Timen A et al (2010) Barriers to implementing infection prevention and control guidelines during crises: experiences of health care professionals. Am J Infect Control 38(9):726–733. https://doi.org/10.1016/j.ajic.2010.03.006
Andrade C (2020) The limitations of online surveys. Indian J Psychol Med 42(6):575–576. https://doi.org/10.1177/0253717620957496
Cabana MD et al (1999) Why Don't Physicians Follow Clinical Practice Guidelines? A Framework for Improvement. JAMA 282:1458–1465
Acknowledgements
We specifically thank all participants for their time and willingness to participate.
Funding
Open Access funding enabled and organized by Projekt DEAL. This research project is part of the G-BA (Gemeinsamer Bundesausschuss) funded project SISYPHOS—Strukturierte Implementierung digitaler, systematisch aktualisierter Leitlinienempfehlungen zur optimierten Therapeutenadhärenz bei Schizophrenie, funding reference number 01VSF20024.
Author information
Authors and Affiliations
Contributions
NKG, GG, DG, TH, AR, and AH: conceptualization, methodology, investigation, resources. AH: funding acquisition. GG and AH: project administration and supervision. GG, CL: formal analysis and data curation. NKG, CL, and GG: writing—original draft, visualization. All authors: review and editing.
Corresponding author
Ethics declarations
Conflict of interest
C. Lorenz, N. Khorikian-Ghazari, G. Gaigl, C. Pielenz, M. Schneider, E. Salveridou-Hof, M. Flick, D. Güler, T. Halms, A. Burschinski. A. Röh report no conflicts of interest. P. Falkai received research support/honoraria for lectures or advisory activities from: Abbott, Boehringer-Ingelheim, Janssen, Essex, Lundbeck, Otsuka, Recordati, Richter, Servier and Takeda. He holds a payed position as Chairman of the Psychiatric Department of the University Munich; is full professor at the Psychiatric Department of the University Munich. He has received and is currently receiving grants from several national and international foundations and institutions, e.g., from the “German Science Foundation”, the “German Ministry of Science” and the “German Ministry of Health”. S. Leucht reported personal fees from Alkermes, Angelini Pharma, Eisai, Gedeon Richter, Janssen Pharmaceuticals, Johnson & Johnson, Lundbeck, Medichem, Merck Sharp & Dohme, Otsuka Pharmaceutical, Casen Recordati, Rovi, Sandoz, Sanofi, Sunovion, Teva Pharmaceuticals, Boehringer Ingelheim, and LTS Lohmann. W. Gaebel is a member of the Lundbeck International Neuroscience Foundation. A.H. is editor of the German (DGPPN) Schizophrenia treatment guidelines and first-author of the WFSBP schizophrenia treatment guidelines. He has been on the advisory boards of Janssen, Lundbeck, Recordati, Rovi and Otsuka and received speaker fees from those companies and from AbbVie.E. Wagner has been invited to advisory boards from Recordati.
Ethical approval
The project (incl. protocol) was approved by the local ethics committees of the University Hospital Munich. The survey was reviewed by the data protection officer of the University Hospital Munich.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Khorikian-Ghazari, N., Lorenz, C., Güler, D. et al. Guideline for schizophrenia: implementation status and attitude toward an upcoming living guideline. Eur Arch Psychiatry Clin Neurosci 273, 1587–1598 (2023). https://doi.org/10.1007/s00406-023-01568-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00406-023-01568-z