Abstract
Purpose
To examine the influence of demographic, audiologic, and hearing-aid (HA)-related variables on HA outcomes.
Methods
In total, 235 adults with hearing loss (HL) who used HAs for at least 3 months were included in the study, and completed audiologic tests and the Chinese version of the International Outcome Inventory for Hearing Aids (IOI-HA). Spearman correlation analysis and Wilcoxon test were conducted to identify factors related to IOI-HA overall and subscales scores. Stepwise multiple linear regression analysis was subsequently performed to determine the influence of factors on HA outcomes.
Results
Age, daily use time, HA price, pure tone average (PTA) threshold, word recognition score (WRS), fitting (bilateral or unilateral), and HA style were associated with IOI-HA overall and subscales scores. However, only WRS, daily HA use time, HA price, and age entered the final regression model and were factors determining HA outcomes.
Conclusions
HA outcome is a multi-dimensional construct. In this study, WRS had the greatest influence on HA outcomes and seemed to be a primary predictor. Thus, HA owners with a higher WRS before HA fitting may indicate better satisfaction. Daily use time, HA price, and patient age also made significant contributions to HA outcomes and should be considered in clinical practice to facilitate auditory rehabilitation.

Similar content being viewed by others
Notes
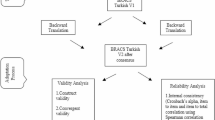
Details are shown in the legend of Fig. 1.
References
Laplante-Lévesque A, Hickson L, Worrall L (2010) Rehabilitation of older adults with hearing impairment: a critical review. J Aging Health 22:143–153. https://doi.org/10.1177/0898264309352731
Panza F, Solfrizzi V, Logroscino G (2015) Age-related hearing impairment-a risk factor and frailty marker for dementia and AD. Nat Rev Neurol 11:166–175. https://doi.org/10.1038/nrneurol.2015.12
Lopez-Poveda EA, Johannesen PT, Pérez-González P, Blanco JL, Kalluri S, Edwards B (2017) Predictors of hearing-aid outcomes. Trends Hear 21:1–28. https://doi.org/10.1177/2331216517730526
Davis A (2003) Population study of the ability to benefit from amplification and the provision of a hearing aid in 55–74-year-old first-time hearing aid users. Int J Audiol 42(Suppl 2:2s):39–52
Chang HP, Chou P (2007) Presbycusis among older Chinese people in Taipei, Taiwan: a community-based study. Int J Audiol 46:738–745. https://doi.org/10.1080/14992020701558529
Chien W, Lin FR (2012) Prevalence of hearing aid use among older adults in the United States. Arch Intern Med 172:292–293. https://doi.org/10.1001/archinternmed.2011.1408
Meister H, Rählmann S, Walger M, Margolf-Hackl S, Kießling J (2015) Hearing aid fitting in older persons with hearing impairment: the influence of cognitive function, age, and hearing loss on hearing aid benefit. Clin Interv Aging 10:435–443. https://doi.org/10.2147/cia.S77096
Moon IJ, Baek SY, Cho YS (2015) Hearing aid use and associated factors in South Korea. Medicine (Baltimore) 94:e1580. https://doi.org/10.1097/md.0000000000001580
Hartley D, Rochtchina E, Newall P, Golding M, Mitchell P (2010) Use of hearing AIDS and assistive listening devices in an older Australian population. J Am Acad Audiol 21:642–653. https://doi.org/10.3766/jaaa.21.10.4
Knudsen LV, Oberg M, Nielsen C, Naylor G, Kramer SE (2010) Factors influencing help seeking, hearing aid uptake, hearing aid use and satisfaction with hearing aids: a review of the literature. Trends Amplif 14:127–154. https://doi.org/10.1177/1084713810385712
Williams VA, Johnson CE, Danhauer JL (2009) Hearing aid outcomes: effects of gender and experience on patients’ use and satisfaction. J Am Acad Audiol 20:422–432. https://doi.org/10.3766/jaaa.20.7.4 (quiz 459–460)
Humes LE, Rogers SE, Quigley TM, Main AK, Kinney DL, Herring C (2017) The effects of service-delivery model and purchase price on hearing-aid outcomes in older adults: a randomized double-blind placebo-controlled clinical trial. Am J Audiol 26:53–79. https://doi.org/10.1044/2017_aja-16-0111
Kaplan-Neeman R, Muchnik C, Hildesheimer M, Henkin Y (2012) Hearing aid satisfaction and use in the advanced digital era. Laryngoscope 122:2029–2036. https://doi.org/10.1002/lary.23404
Korkmaz MH, Bayır Ö, Er S, Işık E, Saylam G, Tatar E, Özdek A (2016) Satisfaction and compliance of adult patients using hearing aid and evaluation of factors affecting them. Eur Arch Otorhinolaryngol 273:3723–3732. https://doi.org/10.1007/s00405-016-4046-x
Saunders GH, Jutai JW (2004) Hearing specific and generic measures of the psychosocial impact of hearing aids. J Am Acad Audiol 15:238–248. https://doi.org/10.3766/jaaa.15.3.6
Hickson L, Meyer C, Lovelock K, Lampert M, Khan A (2014) Factors associated with success with hearing aids in older adults. Int J Audiol 53(Suppl 1):S18-27. https://doi.org/10.3109/14992027.2013.860488
Hickson L, Clutterbuck S, Khan A (2010) Factors associated with hearing aid fitting outcomes on the IOI-HA. Int J Audiol 49:586–595. https://doi.org/10.3109/14992021003777259
Wu X, Ren Y, Wang Q, Li B, Wu H, Huang Z, Wang X (2019) Factors associated with the efficiency of hearing aids for patients with age-related hearing loss. Clin Interv Aging 14:485–492. https://doi.org/10.2147/cia.S190651
Wilson C, Stephens D (2003) Reasons for referral and attitudes toward hearing aids: do they affect outcome? Clin Otolaryngol Allied Sci 28:81–84. https://doi.org/10.1046/j.1365-2273.2003.00669.x
Chang YS, Choi J, Moon IJ, Hong SH, Chung WH, Cho YS (2016) Factors associated with self-reported outcome in adaptation of hearing aid. Acta Otolaryngol 136:905–911. https://doi.org/10.3109/00016489.2016.1170201
Chang WH, Tseng HC, Chao TK, Hsu CJ, Liu TC (2008) Measurement of hearing aid outcome in the elderly: comparison between young and old elderly. Otolaryngol Head Neck Surg 138:730–734. https://doi.org/10.1016/j.otohns.2008.02.012
Cox RM, Alexander GC (2002) The International Outcome Inventory for Hearing Aids (IOI-HA): psychometric properties of the English version. Int J Audiol 41:30–35. https://doi.org/10.3109/14992020209101309
Liu H, Zhang H, Liu S, Chen X, Han D, Zhang L (2011) International outcome inventory for hearing aids (IOI-HA): results from the Chinese version. Int J Audiol 50:673–678. https://doi.org/10.3109/14992027.2011.588966
Cox RM, Alexander GC, Gray GA (2007) Personality, hearing problems, and amplification characteristics: contributions to self-report hearing aid outcomes. Ear Hear 28:141–162. https://doi.org/10.1097/AUD.0b013e31803126a4
Bertoli S, Bodmer D, Probst R (2010) Survey on hearing aid outcome in Switzerland: associations with type of fitting (bilateral/unilateral), level of hearing aid signal processing, and hearing loss. Int J Audiol 49:333–346. https://doi.org/10.3109/14992020903473431
Gallagher NE, Woodside JV (2018) Factors affecting hearing aid adoption and use: a qualitative study. J Am Acad Audiol 29:300–312. https://doi.org/10.3766/jaaa.16148
Convery E, Hickson L, Meyer C, Keidser G (2019) Predictors of hearing loss self-management in older adults. Disabil Rehabil 41:2026–2035. https://doi.org/10.1080/09638288.2018.1457091
Picou EM (2020) MarkeTrak 10 (MT10) survey results demonstrate high satisfaction with and benefits from hearing aids. Semin Hear 41:21–36. https://doi.org/10.1055/s-0040-1701243
Baiduc RR, Poling GL, Hong O, Dhar S (2013) Clinical measures of auditory function: the cochlea and beyond. Dis Mon 59:147–156. https://doi.org/10.1016/j.disamonth.2013.01.005
Demeester K, van Wieringen A, Hendrickx JJ, Topsakal V, Fransen E, van Laer L, Van Camp G, Van de Heyning P (2009) Audiometric shape and presbycusis. Int J Audiol 48:222–232. https://doi.org/10.1080/14992020802441799
Leijon A, Dillon H, Hickson L, Kinkel M, Kramer SE, Nordqvist P (2021) Analysis of data from the International Outcome Inventory for Hearing Aids (IOI-HA) using Bayesian Item Response Theory. Int J Audiol 60:81–88. https://doi.org/10.1080/14992027.2020.1813338
Cohen J (1992) A power primer. Psychol Bull 112:155–159. https://doi.org/10.1037//0033-2909.112.1.155
Jerger J, Jerger S, Oliver T, Pirozzolo F (1989) Speech understanding in the elderly. Ear Hear 10:79–89. https://doi.org/10.1097/00003446-198904000-00001
Stach BA, Spretnjak ML, Jerger J (1990) The prevalence of central presbyacusis in a clinical population. J Am Acad Audiol 1:109–115
Dörfler C, Hocke T, Hast A, Hoppe U (2020) Speech recognition with hearing aids for 10 standard audiograms: English version. HNO 68:93–99. https://doi.org/10.1007/s00106-020-00843-y
Wong LL, Hickson L, McPherson B (2003) Hearing aid satisfaction: what does research from the past 20 years say? Trends Amplif 7:117–161. https://doi.org/10.1177/108471380300700402
Gilliver M, Hickson L (2011) Medical practitioners’ attitudes to hearing rehabilitation for older adults. Int J Audiol 50:850–856. https://doi.org/10.3109/14992027.2011.601468
Meyer C, Hickson L, Lovelock K, Lampert M, Khan A (2014) An investigation of factors that influence help-seeking for hearing impairment in older adults. Int J Audiol 53(Suppl 1):S3-17. https://doi.org/10.3109/14992027.2013.839888
Lupsakko TA, Kautiainen HJ, Sulkava R (2005) The non-use of hearing aids in people aged 75 years and over in the city of Kuopio in Finland. Eur Arch Otorhinolaryngol 262:165–169. https://doi.org/10.1007/s00405-004-0789-x
Funding
This study was supported by the Achievement Transformation Project of West China Hospital (No. HX20200680).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection were performed by JL, ZC, and ZL. Data analysis was completed by XW and YL. The first draft of the manuscript was written by XW and YZ commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare that are relevant to the content of this article.
Ethical approval
The study was approved by the Biomedical Ethics Committee of West China Hospital of Sichuan University (approval number: 2020(525)) and performed in line with the principles of the Declaration of Helsinki.
Informed consent
All participants provided written informed consent for their participation.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, X., Zheng, Y., Liu, Y. et al. Effects of demographic, audiologic, and hearing-aid-related variables on the outcomes of using hearing aids. Eur Arch Otorhinolaryngol 279, 3857–3865 (2022). https://doi.org/10.1007/s00405-021-07126-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-021-07126-4