Abstract
Purpose
To assess adverse pregnancy outcomes in patients complicated with mild or severe Hyperemesis Gravidarum (HG).
Methods
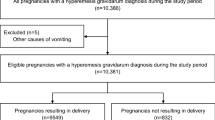
A retrospective cohort study of women aged 18–45 with a singleton pregnancy that were admitted to the gynecological ward at the Soroka University Medical Center due to HG between the years 2013–2016 and gave birth at the same hospital was conducted. During the study period 89 patients met the inclusion criteria and comprised the study group. Women without HG who gave birth at the same time period comprised the comparison group (n = 91). Univariate analysis was carried out using Chi square or Fisher's exact test for nominal variables, and T test for numeric variables. Significance was defined as a P value < 0.05.
Results
Women with HG were more likely to have experienced HG in a previous pregnancy. Rate of amniotic fluid abnormalities was significantly lower in the study group. However, rates of all other pregnancy complications were comparable between the groups. A sub-analysis of the HG group comparing mild and severe cases demonstrated no significant differences in rates of adverse pregnancy outcomes between the groups.
Conclusions
In this retrospective cohort study no association was demonstrated between HG and adverse pregnancy outcomes regardless of HG severity. Women with severe nausea and vomiting during pregnancy can be reassured that HG is not associated with unfavorable maternal and neonatal outcomes.
Similar content being viewed by others
References
Niebyl JR (2010) Clinical practice. Nausea and vomiting in pregnancy. N Engl J Med 363:1544–1550. https://doi.org/10.1056/NEJMcp1003896
Buyukkayaci Duman N, Ozcan O, Bostanci MÖ (2015) Hyperemesis gravidarum affects maternal sanity, thyroid hormones and fetal health: a prospective case control study. Arch Gynecol Obstet 292:307–312. https://doi.org/10.1007/s00404-015-3632-2
Fejzo MS, Sazonova OV, Sathirapongsasuti JF et al (2018) Placenta and appetite genes GDF15 and IGFBP7 are associated with hyperemesis gravidarum. Nat Commun 9:1178. https://doi.org/10.1038/s41467-018-03258-0
Fejzo MS, Myhre R, Colodro-Conde L et al (2017) Genetic analysis of hyperemesis gravidarum reveals association with intracellular calcium release channel (RYR2). Mol Cell Endocrinol 439:308–316. https://doi.org/10.1016/j.mce.2016.09.017
Erick M, Cox JT, Mogensen KM (2018) ACOG practice bulletin 189: nausea and vomiting of pregnancy. Obstet Gynecol 131:935. https://doi.org/10.1097/AOG.0000000000002604
Eliakim R, Abulafia O, Sherer DM (2000) Hyperemesis gravidarum: a current review. Am J Perinatol 17:207–218. https://doi.org/10.1055/s-2000-9424
Vikanes ÅV, Støer NC, Magnus P, Grjibovski AM (2013) Hyperemesis gravidarum and pregnancy outcomes in the Norwegian Mother and Child Cohort—a cohort study. BMC Pregnancy Childbirth 13:169. https://doi.org/10.1186/1471-2393-13-169
Dodds L, Fell DB, Joseph KS et al (2006) Outcomes of pregnancies complicated by hyperemesis gravidarum. Obstet Gynecol 107:285–292. https://doi.org/10.1097/01.AOG.0000195060.22832.cd
Morokuma S, Shimokawa M, Kato K et al (2016) Relationship between hyperemesis gravidarum and small-for-gestational-age in the Japanese population: the Japan Environment and Children’s Study (JECS). BMC Pregnancy Childbirth 16:247. https://doi.org/10.1186/s12884-016-1041-6
Koudijs HM, Savitri AI, Browne JL et al (2016) Hyperemesis gravidarum and placental dysfunction disorders. BMC Pregnancy Childbirth 16:374. https://doi.org/10.1186/s12884-016-1174-7
Peled Y, Melamed N, Hiersch L et al (2014) The impact of total parenteral nutrition support on pregnancy outcome in women with hyperemesis gravidarum. J Matern Fetal Neonatal Med 27:1146–1150. https://doi.org/10.3109/14767058.2013.851187
Matok I, Gorodischer R, Koren G et al (2009) The safety of metoclopramide use in the first trimester of pregnancy. N Engl J Med 360:2528–2535. https://doi.org/10.1056/NEJMoa0807154
Abu-Ghanem S, Sheiner E, Sherf M et al (2012) Lack of prenatal care in a traditional community: trends and perinatal outcomes. Arch Gynecol Obstet 285:1237–1242. https://doi.org/10.1007/s00404-011-2153-x
Fejzo MS, Magtira A, Schoenberg FP et al (2013) Antihistamines and other prognostic factors for adverse outcome in hyperemesis gravidarum. Eur J Obstet Gynecol Reprod Biol 170:71–76. https://doi.org/10.1016/j.ejogrb.2013.04.017
Acknowledgements
The authors report no sources of support for the work. This study was conducted as part of the requirements for MD degree from the Goldman Medical School at the Faculty of Health Sciences, Ben-Gurion University of the Negev.
Author information
Authors and Affiliations
Contributions
Niv Agmon: protocol development, data collection, data analysis, manuscript writing. Shanny Sade: protocol development, data collection, manuscript writing. Gali Pariente: protocol development, data collection, data analysis, manuscript editing. Reut Rotem: protocol development, data analysis, manuscript editing. Adi Yehuda Weintraub: protocol development, data collection, data analysis, manuscript editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Rights and permissions
About this article
Cite this article
Agmon, N., Sade, S., Pariente, G. et al. Hyperemesis gravidarum and adverse pregnancy outcomes. Arch Gynecol Obstet 300, 347–353 (2019). https://doi.org/10.1007/s00404-019-05192-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-019-05192-y