Abstract
Introduction
In spinal surgery, precise instrumentation is essential. This study aims to evaluate the accuracy of navigated, O-arm-controlled screw positioning in thoracic and lumbar spine instabilities.
Materials and methods
Posterior instrumentation procedures between 2010 and 2015 were retrospectively analyzed. Pedicle screws were placed using 3D rotational fluoroscopy and neuronavigation. Accuracy of screw placement was assessed using a 6-grade scoring system. In addition, screw length was analyzed in relation to the vertebral body diameter. Intra- and postoperative revision rates were recorded.
Results
Thoracic and lumbar spine surgery was performed in 285 patients. Of 1704 pedicle screws, 1621 (95.1%) showed excellent positioning in 3D rotational fluoroscopy imaging. The lateral rim of either pedicle or vertebral body was protruded in 25 (1.5%) and 28 screws (1.6%), while the midline of the vertebral body was crossed in 8 screws (0.5%). Furthermore, 11 screws each (0.6%) fulfilled the criteria of full lateral and medial displacement. The median relative screw length was 92.6%. Intraoperative revision resulted in excellent positioning in 58 of 71 screws. Follow-up surgery due to missed primary malposition had to be performed for two screws in the same patient. Postsurgical symptom relief was reported in 82.1% of patients, whereas neurological deterioration occurred in 8.9% of cases with neurological follow-up.
Conclusions
Combination of neuronavigation and 3D rotational fluoroscopy control ensures excellent accuracy in pedicle screw positioning. As misplaced screws can be detected reliably and revised intraoperatively, repeated surgery for screw malposition is rarely required.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The lifetime prevalence of back pain in Germany is 85.5%, with men and women over the age of 50 being particularly affected [1]. Due to the increasing proportion of older people and the longer life expectancy in our population, it must be assumed that the medical and socioeconomic relevance of back pain and degenerative diseases of the spine will further increase [2]. In addition to debilitating degeneration, various underlying conditions such as trauma, inflammation, or neoplasms can be causative agents of spinal instability and require surgical treatment. The main goal of spinal surgery is to restore the spinal column’s weight-bearing capabilities and motion range of the spine in order to improve patients’ quality of life. To ensure this, a high degree of intraoperative precision is required for spinal instrumentation in patients with instabilities as screw misplacement can lead to neurological and vascular complications [3, 4]. Conventional X-ray diagnostics (2D radiographs or biplanar fluoroscopy) are widely regarded as the reference standard for intraoperative imaging in general, and for spinal instrumentation in particular [5]. However, while spinal alignment and vertebral body shape are sufficiently assessable in the far majority of cases, exact screw placement may occasionally be difficult to evaluate [6]. The question of whether modern navigation techniques can improve the precision of spinal instrumentation compared with conventional methods has not yet been clearly answered. Particularly, the application of 3D rotational fluoroscopy in combination with neuronavigation appears promising for intraoperative screw position analysis, as it provides multiplanar image information comparable to multidetector CT imaging.
The purpose of this retrospective study was to evaluate the accuracy of pedicle screw positioning in navigated, O-arm-controlled posterior instrumentation for the thoracic und lumbar spine.
Material and methods
Retrospective data analysis was approved, and informed consent was waived by the local ethics committee. Information on patient history and surgical procedure was obtained from the clinical information system (SAP SE, Walldorf, Germany) and anonymized for further analysis. The evaluation of intraoperative imaging in terms of screw position and screw length was performed using an open-source DICOM viewer program (OsiriX Lite 8.0.1). For this study, we retrospectively analyzed data from patients who underwent dorsal spinal instrumentation with 3D fluoroscopic navigation (O-arm, Medtronic, Dublin, Ireland) at the local neurosurgical clinic between June 2010 to June 2015. Treatment indication was based on spinal instability due to degenerative, traumatic, inflammatory or tumor-related conditions. Inclusion criteria included surgical treatment via a dorsal approach (± additional fusion), surgery performed with an open or percutaneous technique and at least one rotational 3D fluoroscopy scan after dorsal instrumentation to evaluate the position of the screws. Patients who did not receive a rotational 3D scan were excluded from this study. Furthermore, screws that were not included in the field of view of the initial 3D fluoroscopy scan (n = 34) were also left out of the analysis.
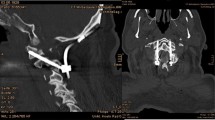
The O-arm represents a 3D rotational fluoroscopy device designed for intraoperative application. In addition to the rotor, the gantry-based scanner architecture contains the X-ray tube (B100, Varian Medical Systems, Palo Alto, USA) opposite a large flat-panel detector (PaxScan 4030D, Varex, Palo Alto, USA). In 3D mode, the O-arm creates a series of projection images during a complete 360° rotation. Gantry rotation speed can be set to 30° per second in standard mode or 15° per second in high-definition mode with up to 400 or 750 images generated during a full 360° rotation. By integrating the navigation system (StealthStation S7, Medtronic) into the scanner setup, intraoperative imaging can be used directly for neuronavigation. This approach enables periprocedural display of entry points as well as identification of important neighboring structures.
Qualitative evaluation of screw positioning for the thoracic and lumbar spine was performed using the 6-grade scoring system described by Zdichavsky et al., in which grade Ia represents an excellent position, whereas grades IIIa and IIIb are supposed to be surgically revised [7, 8]. The classification system is based on the relative position of the inserted screw to the pedicle and vertebral body (Fig. 1, Table 1). In addition, the length ratio between screw and vertebral body diameter was calculated, with any relative screw length between 85 and 100% classified as good [9].
All data were transferred to a standard spreadsheet (Microsoft Excel for Mac, version 15.22, Redmond, USA) for further processing. Statistical analysis was performed using dedicated software (IBM SPSS Statistics, version 24.0.0.1 for Mac, Armonk, USA). Normal distribution was assessed with Kolmogorov–Smirnov tests. For normally distributed continuous variables, we report mean values and standard deviation, whereas absolute values and percentage distribution are displayed otherwise. Chi-square tests were applied to compare categorical data. To measure the effect size of the chi-square-test, Cramer-V was computed. Student’s t-tests were conducted to determine whether two normally distributed samples differ significantly. P values ≤ 0.05 were considered to indicate statistical significance.
Results
Between June 2, 2010, and June 29, 2015, 285 patients (134 women, 47.0%) underwent 295 dorsal screw-rod instrumentations with 62 procedures performed on the thoracic and 233 on the lumbar spine. Lumbar vertebra 4 was stabilized most often (185 times) and thoracic vertebra 9 least often (14 times). Mean patient age at the time of surgery was 64.1 ± 12.6 years with almost 69% of patients over 60 years of age. Indication to perform surgical treatment was most frequently based on tumor-induced instability in the thoracic spine (46.8%) and degeneration-induced instability in the lumbar spine (76.8%). Table 2 summarizes the underlying conditions that led to surgical stabilization. Clinical follow-up was available in 238 patients (83.5%) with a mean time period of 14.3 ± 10.2 months.
Of 1704 included screws, 1621 (95.1%) showed an excellent position (Ia) in the initial intraoperative imaging. Of the remaining pedicle screws, 25 (1.5%) protruded the lateral rim of the pedicle (Ib), 28 (1.6%) protruded the lateral margin of the vertebral body (IIa), 8 (0.5%) crossed the vertebra’s midline (IIb). Furthermore, 11 screws each (0.6%) fulfilled the criteria of full lateral (IIIa) or medial displacement (IIIb). Median screw length was 92.6% of the maximum diameter of the vertebral body with 1224 screws (71.8%) displaying “good” length in the first scan.
After intraoperative revision, 58 of 71 screw positions were classified as Ia and one screw was classified as Ib. The other 12 revised screws were either not included in the field of view of the post-revision 3D scan or no further imaging was performed after intraoperative repositioning. Good relative length was ascertained in 1238 screws (72.7%). Screw position grading and relative length before and after intraoperative revision are summarized in Figs. 2 and 3, respectively. Repeated surgery was necessary in 11 patients (12 operations) with a total of 40 screws (2.3%) being repositioned. However, only two screws (0.1%) in one patient had to be revised due to primary malposition. The remaining screws had to be revised due to progressive loosening (20 screws [1.2%]), connection instability (15 screws [0.9%]) or inflammation-induced remodeling (3 screws [0.2%]).
At follow-up, 82.1% of patients declared total pain release or at least significant improvement of back and/or leg pain after surgery. No patient reported aggravating or new pain after surgery at the control examination. Neurological follow-up showed significant improvement or complete remission of symptoms in 70.8% of patients with neurological deficits. In contrast, 8.9% of patients with follow-up had new neurological symptoms that were not reported preoperatively.
Discussion
In this study, the accuracy of pedicle screw placement in the thoracic and lumbar spine was investigated using a combined approach of neuronavigation and intraoperative 3D rotational fluoroscopy. High precision of implant positioning was achieved in all spinal sections. With a total of 1738 screws placed, intraoperative revision was performed for 78 screws, whereas repeated surgery due to a missed malposition was necessary in just one patient.
The classification system of Zdichavsky et al. represents a validated concept for determining the accuracy of pedicle screw placement in the thoracic and lumbar spine [7, 8]. Our results for placement accuracy are superior compared to the literature on screw positioning with conventional fluoroscopy-guidance [9, 10]. However, many earlier studies with similar designs use other forms of graduation, e.g., deviation from the ideal position in millimeter, dichotomous assessment of pedicle wall penetration [11] or screw placement < 50% or > 50% outside the pedicle [12]. Other studies only report accurate screw positioning when the thread is entirely intraosseous [13,14,15,16,17], or state misplacement solely in patients with postoperative neurological deficit or screws that require postoperative revision [18]. A meta-analysis by Gelalis et al. evaluated screw positioning with 3D fluoroscopy-guided neuronavigation, reporting accurate positioning for completely transpedicular screws in 81–92% of patients [19]. Assumedly, the inferior performance in individual studies within the meta-analysis compared to the present work may be attributed to substantially smaller patient samples with different sociodemographic characteristics. Besides, various definitions of screw misalignment yielded different shares of “correct” positioning. Different surgical indications, the experience of the surgeon, as well as the complexity of the surgery and height of the instrumented spinal segment also contributed to the heterogeneity of the results.
Revision surgery frequencies of up to 5.2% have been described in various studies on neuronavigated spinal surgery [20,21,22], which is considerably higher than in the present work. In the series presented here, only one of 285 patients required repeated procedures because of screw misplacement that was not detected intraoperatively. We assume that the far lower frequency of repetitive surgery can be attributed to the superior screw assessability provided by the O-arm-navigated approach, which is in line with the findings of Beck et al. [6].
Perdomo-Pantoja et al. showed in a recent meta-analysis on the accuracy of pedicle screw placement with different techniques that the highest accuracy results from CT navigation [23]. Nevertheless, it must be stated that high precision can also be achieved with free-hand or fluoroscopy-assisted screw insertion, even in patients with pronounced spinal deformities such as degenerative scoliosis [24]. Although Chan et al. demonstrated that screw breach rates are lower with CT navigation compared to free-hand methods, complication rates remained low with either technique [25].
Several limitations have to be addressed for this study. Since we performed a retrospective analysis, data quality regarding long-term outcome, neurological status and pain relief was inconsistent. Intraoperative revision rates of 4.2% were slightly higher than in comparable studies [6, 26]. However, we believe that this finding can be attributed to the inclusion of data from the introductory phase of the 3D fluoroscopy system. As degenerative diseases were predominantly responsible for spinal surgery in this study, decompression of spinal stenosis and/or cage insertion was frequently performed in addition to dorsal stabilization with a screw-rod system, hence affecting the clinical outcome. While 8.9% of patients with adequate follow-up reported new neurological symptoms, no association could be ascertained with misplaced screws that were revised intraoperatively.
Conclusion
Combination of neuronavigation and 3D rotational fluoroscopy control ensures excellent accuracy in pedicle screw positioning. As misplaced screws can be detected reliably and revised intraoperatively, repeated surgery for screw malposition is rarely required.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
Abbreviations
- CT:
-
Computed tomography
- PS:
-
Pedicle screw
- PSD:
-
Pedicle screw diameter
References
Schmidt CO, Raspe H, Pfingsten M et al (2007) Back pain in the German adult population: prevalence, severity, and sociodemographic correlates in a multiregional survey. Spine (Phila Pa 1976) 32:2005–2011. https://doi.org/10.1097/BRS.0b013e318133fad8
Sobottke R, Csécsei G, Kaulhausen T et al (2008) Wirbelsäulenchirurgie bei patienten in höherem lebensalter. Sind operative eingriffe an der alternden wirbelsäule komplikationsträ chtig? Orthopade 37:367–373. https://doi.org/10.1007/s00132-008-1233-5
Ghasem A, Sharma A, Greif DN et al (2018) The Arrival of robotics in spine surgery. Spine (Phila Pa 1976) 43:1670–1677. https://doi.org/10.1097/BRS.0000000000002695
Kothe R, Richter M (2018) Relevanz der spinalen navigation in der rekonstruktiven halswirbelsäulenchirurgie. Orthopade 47:518–525. https://doi.org/10.1007/s00132-018-3568-x
von Rüden C, Trapp O, Augat P et al (2020) Evolution of imaging in surgical fracture management. Injury 51:S51–S56. https://doi.org/10.1016/j.injury.2019.10.080
Beck M, Mittlmeier T, Gierer P et al (2009) Benefit and accuracy of intraoperative 3D-imaging after pedicle screw placement: a prospective study in stabilizing thoracolumbar fractures. Eur Spine J 18:1469–1477. https://doi.org/10.1007/s00586-009-1050-5
Zdichavsky M, Blauth M, Knop C et al (2004) Accuracy of pedicle screw placement in thoracic spine fractures - part I: inter- and intraobserver reliability of the scoring system. Eur J Trauma 30:234–240. https://doi.org/10.1007/s00068-004-1422-9
Zdichavsky M, Blauth M, Knop C et al (2004) Accuracy of pedicle screw placement in thoracic spine fractures - part II: a retrospective analysis of 278 pedicle screws using computed tomographic scans. Eur J Trauma 30:241–247. https://doi.org/10.1007/s00068-004-1423-8
Heintel TM, Berglehner A, Meffert R (2013) Accuracy of percutaneous pedicle screws for thoracic and lumbar spine fractures: a prospective trial. Eur Spine J 22:495–502. https://doi.org/10.1007/s00586-012-2476-8
Marios T, Theologos T, Dimitrios Z et al (2017) Pedicle screw placement accuracy impact and comparison between grading systems. Surg Neurol Int. https://doi.org/10.4103/sni.sni_85_17
Kotani Y, Abumi K, Ito M, Minami A (2003) Improved accuracy of computer-assisted cervical pedicle screw insertion. J Neurosurg 99:257–263. https://doi.org/10.3171/spi.2003.99.3.0257
Nakashima H, Sato K, Ando T et al (2009) Comparison of the percutaneous screw placement precision of isocentric C-arm 3-dimensional fluoroscopy-navigated pedicle screw implantation and conventional fluoroscopy method with minimally invasive surgery. J Spinal Disord Tech 22:468–472. https://doi.org/10.1097/BSD.0b013e31819877c8
Silbermann J, Riese F, Allam Y et al (2011) Computer tomography assessment of pedicle screw placement in lumbar and sacral spine: comparison between free-hand and O-arm based navigation techniques. Eur Spine J 20:875–881. https://doi.org/10.1007/s00586-010-1683-4
Ishikawa Y, Kanemura T, Yoshida G et al (2010) Clinical accuracy of three-dimensional fluoroscopy-based computer-assisted cervical pedicle screw placement: a retrospective comparative study of conventional versus computer-assisted cervical pedicle screw placement - Clinical article. J Neurosurg Spine 13:606–611. https://doi.org/10.3171/2010.5.SPINE09993
Kim TT, Drazin D, Shweikeh F et al (2014) Clinical and radiographic outcomes of minimally invasive percutaneous pedicle screw placement with intraoperative CT (O-arm) image guidance navigation. Neurosurg Focus. https://doi.org/10.3171/2014.1.FOCUS13531
Nottmeier EW, Pirris SM (2013) Placement of thoracic transvertebral pedicle screws using 3D image guidance. J Neurosurg Spine 18:479–483. https://doi.org/10.3171/2013.2.SPINE12819
Shin BJ, James AR, Njoku IU, Härtl R (2012) Pedicle screw navigation: a systematic review and meta-analysis of perforation risk for computer-navigated versus freehand insertion. J Neurosurg Spine 17:113–122. https://doi.org/10.3171/2012.5.SPINE11399
Laudato PA, Pierzchala K, Schizas C (2018) Pedicle screw insertion accuracy using O-arm, robotic guidance, or freehand technique. Spine (Phila Pa 1976) 43:E373–E378. https://doi.org/10.1097/BRS.0000000000002449
Gelalis ID, Paschos NK, Pakos EE et al (2012) Accuracy of pedicle screw placement: a systematic review of prospective in vivo studies comparing free hand, fluoroscopy guidance and navigation techniques. Eur Spine J 21:247–255. https://doi.org/10.1007/s00586-011-2011-3
Luther N, Iorgulescu JB, Geannette C et al (2015) Comparison of navigated versus non-navigated pedicle screw placement in 260 patients and 1434 screws: Screw accuracy, screw size, and the complexity of surgery. J Spinal Disord Tech 28:E298–E303. https://doi.org/10.1097/BSD.0b013e31828af33e
Xiao R, Miller JA, Sabharwal NC et al (2017) Clinical outcomes following spinal fusion using an intraoperative computed tomographic 3D imaging system. J Neurosurg Spine 26:628–637. https://doi.org/10.3171/2016.10.SPINE16373
Amiot LP, Lang K, Putzier M et al (2000) Comparative results between conventional and computer-assisted pedicle screw installation in the thoracic, lumbar, and sacral spine. Spine (Phila Pa 1976) 25:606–614. https://doi.org/10.1097/00007632-200003010-00012
Perdomo-Pantoja A, Ishida W, Zygourakis C et al (2019) Accuracy of current techniques for placement of pedicle screws in the spine: a comprehensive systematic review and meta-analysis of 51,161 screws. World Neurosurg 126:664-678.e3. https://doi.org/10.1016/J.WNEU.2019.02.217
Yamada T, Hasegawa T, Yamato Y et al (2022) Characteristics of pedicle screw misplacement using freehand technique in degenerative scoliosis surgery. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-022-04380-x
Chan A, Parent E, Narvacan K et al (2017) Intraoperative image guidance compared with free-hand methods in adolescent idiopathic scoliosis posterior spinal surgery: a systematic review on screw-related complications and breach rates. Spine J 17:1215–1229. https://doi.org/10.1016/J.SPINEE.2017.04.001
Van de Kelft E, Costa F, Van der Planken D, Schils F (2012) A prospective multicenter registry on the accuracy of pedicle screw placement in the thoracic, lumbar, and sacral levels with the use of the O-arm imaging system and stealthstation navigation. Spine (Phila Pa 1976). 37:E1580–E1587. https://doi.org/10.1097/BRS.0b013e318271b1fa
Funding
Open Access funding enabled and organized by Projekt DEAL. The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Contributions
NC analyzed all data and prepared the manuscript. JPG and KSL supported the draft of the manuscript and revised it for style and language. KG and HH supported figure preparation and data analysis. PF provided quality control. SK and TW designed and supervised the study. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
The local institutional review board approved this retrospective study and waived the need for additional written informed consent (reference number 20160925 01). This work was carried out in accordance with the ethical standards of the institutional and national research committee and with the 1975 Declaration of Helsinki.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Conrads, N., Grunz, JP., Huflage, H. et al. Accuracy of pedicle screw placement using neuronavigation based on intraoperative 3D rotational fluoroscopy in the thoracic and lumbar spine. Arch Orthop Trauma Surg 143, 3007–3013 (2023). https://doi.org/10.1007/s00402-022-04514-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04514-1