Abstract
Introduction
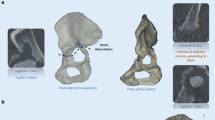
Classifying complex acetabular defects in revision total hip arthroplasty (THA) by means of conventional radiographs comes with significant limitations. Statistical shape modelling allows the virtual reconstruction of the native pelvic morphology, hereby enabling an analytic acetabular defect assessment. Our objective was to evaluate the effect of advanced imaging augmented with analytic representations of the defect on (1) intra- and inter-rater reliability, and (2) up- or downscaling of classification scores when evaluating acetabular defects in patients undergoing revision THA.
Materials and methods
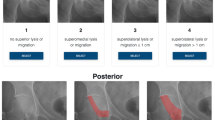
The acetabular defects of 50 patients undergoing revision THA were evaluated by three independent, fellowship-trained orthopaedic surgeons. Defects were classified according to the acetabular defect classification (ADC) using four different imaging-based representations, namely, standard radiographs, CT imaging, a virtual three-dimensional (3D) model and a quantitative analytic representation of the defect based on a statistical shape model reconstruction. Intra- and inter-rater reliabilities were quantified using Fleiss’ and Cohen’s kappa scores, respectively. Up- and downscaling of classification scores were compared for each of the imaging-based representations and differences were tested.
Results
Overall inter-rater agreement across all imaging-based representations for the classification was fair (κ 0.29 95% CI 0.28–0.30). Inter-rater agreement was lowest for radiographs (κ 0.21 95% CI 0.19–0.22) and increased for other representations with agreement being highest when using analytic defect models (κ 0.46 95% CI 0.43–0.48). Overall intra-rater agreement was moderate (κ 0.51 95% CI 0.42–0.60). Intra-rater agreement was lowest for radiographs (κ 0.40 95% CI 0.23–0.57), and highest for ratings including analytic defect models (κ 0.64:95% CI 0.46–0.82). Virtual 3D models with quantitative analytic defect representations upscaled acetabular defect scores in comparison to standard radiographs.
Conclusions
Using 3D CT imaging with statistical shape models doubles the intra- and inter-rater reliability and results in upscaling of acetabular defect classification when compared to standard radiographs. This method of evaluating defects will aid in planning surgical reconstruction and stimulate the development of new classification systems based on advanced imaging techniques.




Similar content being viewed by others
References
Barrack RL (2004) Preoperative planning for revision total hip arthroplasty. Clin Orthop Relat Res 420:32–38
Berend ME, Berend KR, Lombardi AV et al (2018) The patient-specific Triflange acetabular implant for revision total hip arthroplasty in patients with severe acetabular defects: planning, implantation, and results. Bone Jt J 100:50–54
Sheth NP, Nelson CL, Springer BD et al (2013) Acetabular bone loss in revision total hip arthroplasty: evaluation and management. J Am Acad Orthop Surg 21:128. https://doi.org/10.5435/JAAOS-21-03-128
Garcia-Rey E, Saldaña L, Garcia-Cimbrelo E (2021) Impaction bone grafting in hip re-revision surgery: bone stock restoration and radiological migration of the acetabular component. Bone Jt J 103:492–499
Jones CW, Choi DS, Sun P et al (2019) Clinical and design factors influence the survivorship of custom flange acetabular components. Bone Jt J 101-B:68–76. https://doi.org/10.1302/0301-620X.101B6.BJJ-2018-1455.R1
Löchel J, Janz V, Hipfl C et al (2019) Reconstruction of acetabular defects with porous tantalum shells and augments in revision total hip arthroplasty at ten-year follow-up. Bone Jt J 101-B:311–316. https://doi.org/10.1302/0301-620X.101B3.BJJ-2018-0959.R1
Claus AM, Totterman SM, Sychterz CJ et al (2004) Computed tomography to assess pelvic lysis after total hip replacement. Clin Orthop Relat Res 422:167–174
Garcia-Cimbrelo E, Tapia M, Martin-Hervas C (2007) Multislice computed tomography for evaluating acetabular defects in revision THA. Clin Orthop Relat Res 463:138–143. https://doi.org/10.1097/BLO.0b013e3181566320
Walde TA, Weiland DE, Leung SB et al (2005) Comparison of CT, MRI, and radiographs in assessing pelvic osteolysis: a cadaveric study. Clin Orthop Relat Res 437:138–144. https://doi.org/10.1097/01.blo.0000164028.14504.46
Marsh AG, Nisar A, El Refai M et al (2017) Can we predict which dysplastic hips will require acetabular augmentation during total hip arthroplasty based on pre-operative radiographs? Bone Jt J 99:445–450. https://doi.org/10.1302/0301-620X.99B4.BJJ-2016-0041.R1
Goodman GP, Engh CA Jr (2016) The custom triflange cup. Bone Jt J 98:68–72. https://doi.org/10.1302/0301-620X.98B.36354
Gelaude F, Clijmans T, Delport H (2011) Quantitative computerized assessment of the degree of acetabular bone deficiency: total radial acetabular bone loss (TrABL). Adv Orthop 2011:494382. https://doi.org/10.4061/2011/494382
Meynen A, Matthews H, Nauwelaers N, et al (2020) Accurate reconstructions of pelvic defects and discontinuities using statistical shape models. Comput Methods Biomech Biomed Eng Imaging Vis 1–8
Vanden Berghe P, Demol J, Gelaude F, Vander Sloten J (2017) Virtual anatomical reconstruction of large acetabular bone defects using a statistical shape model. Comput Methods Biomech Biomed Eng Imaging Vis 20:577–586. https://doi.org/10.1080/10255842.2016.1265110
Meynen A, Vles G, Zadpoor AA et al (2021) The morphological variation of acetabular defects in revision total hip arthroplasty—A statistical shape modeling approach. J Orthop Res. https://doi.org/10.1002/jor.24995
Donner A, Eliasziw M (1987) Sample size requirements for reliability studies. Stat Med 6:441–448
Wirtz DC, Jaenisch M, Osterhaus TA et al (2020) Acetabular defects in revision hip arthroplasty: a therapy-oriented classification. Arch Orthop Trauma Surg 140:815–825. https://doi.org/10.1007/s00402-020-03379-6
Altman DG (1990) Practical statistics for medical research. CRC Press
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174. https://doi.org/10.2307/2529310
Campbell DG, Garbuz DS, Masri BA, Duncan CP (2001) Reliability of acetabular bone defect classification systems in revision total hip arthroplasty. J Arthroplasty 16:83–86. https://doi.org/10.1054/arth.2001.19157
Martin JR, Barrett IJ, Sierra RJ et al (2016) Preoperative radiographic evaluation of patients with pelvic discontinuity. J Arthroplasty 31:1053–1056. https://doi.org/10.1016/j.arth.2015.11.024
Garbuz DS, Masri BA, Esdaile J, Duncan CP (2002) Classification systems in orthopaedics. J Am Acad Orthop Surg 10:290–297
Horas K, Arnholdt J, Steinert AF et al (2017) Acetabular defect classification in times of 3D imaging and patient-specific treatment protocols. Orthopäde 46:168–178. https://doi.org/10.1007/s00132-016-3378-y
Telleria JJM, Gee AO (2013) Classifications in brief: paprosky classification of acetabular bone loss. Clin Orthop Relat Res 471:3725–3730. https://doi.org/10.1007/s11999-013-3264-4
Jerosch J, Steinbeck J, Fuchs S, Kirchhoff C (1996) Radiologic evaluation of acetabular defects on acetabular loosening of hip alloarthroplasty. Unfallchirurg 99:727–733. https://doi.org/10.1007/s001130050048
Kavalerskiy GM, Murylev VY, Rukin YA et al (2018) Three-dimensional models in planning of revision hip arthroplasty with complex acetabular defects. Indian J Orthop 52:625–630
Li Q, Chen X, Lin B et al (2019) Three-dimensional technology assisted trabecular metal cup and augments positioning in revision total hip arthroplasty with complex acetabular defects. J Orthop Surg Res 14:431. https://doi.org/10.1186/s13018-019-1478-1
Sciberras N, Frame M, Bharadwaj RG, et al (2013) A novel technique for pre-operative planning of severe acetabular defects during revision hip arthroplasty. In: Orthopaedic proceedings. The British editorial society of bone & joint surgery, pp 63–63
Hettich G, Schierjott RA, Ramm H et al (2019) Method for quantitative assessment of acetabular bone defects. J Orthop Res 37:181–189
Trompeter AJ, Furness H, Kanakaris NK, Costa ML (2020) Classification of open fractures: the need to modernize. Bone Jt J 102-B:1431–1434. https://doi.org/10.1302/0301-620X.102B11.BJJ-2020-0947
Funding
The research for this paper was financially supported by the PROSPEROS project, funded by the Interreg VAFlanders—The Netherlands program, CCI Grant no. 2014TC16RFCB046; A.M. is a SB PhD fellow at FWO (Research Foundation—Flanders) Grant no. 1SB3819N.
Author information
Authors and Affiliations
Contributions
AM contributed to the image segmentation, development of the modeling approach, study design, data analysis, manuscript writing and preparation. GV contributed to the study design, data generation, manuscript writing and preparation. MR, AVE and HW contributed to the data generation, manuscript writing and preparation. MM supervised the research, contributed to the image segmentation, manuscript writing and preparation. LS supervised the research, contributed to the development of the modeling approach, study design, manuscript writing and preparation. All authors have read and approved the final submitted manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Meynen, A., Vles, G., Roussot, M. et al. Advanced quantitative 3D imaging improves the reliability of the classification of acetabular defects. Arch Orthop Trauma Surg 143, 1611–1617 (2023). https://doi.org/10.1007/s00402-022-04372-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04372-x