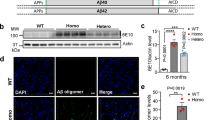
Abstract
Animal models aim to replicate the symptoms, the lesions or the cause(s) of Alzheimer disease. Numerous mouse transgenic lines have now succeeded in partially reproducing its lesions: the extracellular deposits of Aβ peptide and the intracellular accumulation of tau protein. Mutated human APP transgenes result in the deposition of Aβ peptide, similar but not identical to the Aβ peptide of human senile plaque. Amyloid angiopathy is common. Besides the deposition of Aβ, axon dystrophy and alteration of dendrites have been observed. All of the mutations cause an increase in Aβ 42 levels, except for the Arctic mutation, which alters the Aβ sequence itself. Overexpressing wild-type APP alone (as in the murine models of human trisomy 21) causes no Aβ deposition in most mouse lines. Doubly (APP × mutated PS1) transgenic mice develop the lesions earlier. Transgenic mice in which BACE1 has been knocked out or overexpressed have been produced, as well as lines with altered expression of neprilysin, the main degrading enzyme of Aβ. The APP transgenic mice have raised new questions concerning the mechanisms of neuronal loss, the accumulation of Aβ in the cell body of the neurons, inflammation and gliosis, and the dendritic alterations. They have allowed some insight to be gained into the kinetics of the changes. The connection between the symptoms, the lesions and the increase in Aβ oligomers has been found to be difficult to unravel. Neurofibrillary tangles are only found in mouse lines that overexpress mutated tau or human tau on a murine tau −/− background. A triply transgenic model (mutated APP, PS1 and tau) recapitulates the alterations seen in AD but its physiological relevance may be discussed. A number of modulators of Aβ or of tau accumulation have been tested. A transgenic model may be analyzed at three levels at least (symptoms, lesions, cause of the disease), and a reading key is proposed to summarize this analysis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The extracellular accumulation of Aβ peptide in the core of the senile plaque and the intracellular accumulation of tau protein as neurofibrillary tangles and neuropil threads are today considered the two molecular and morphologic signatures of Alzheimer disease (AD), mandatory for its diagnosis [16]. The neuronal loss does not belong to the diagnostic criteria, but has been also considered an important pathological component that should be replicated in a good model of AD. Aβ peptide, in its native state, is unstable in water solution (a third of its amino-acids -AA- sequence is hydrophobic); it forms dimers, trimers, and in general oligomers. It may finally aggregate. The aggregates of Aβ peptide may exhibit the properties of an amyloid substance, properties that are attributed to a high content of β-pleated sheet structures: it is stained by Congo red and thioflavin S, and is fibrillar at electron microscopy. The extracellular deposits of Aβ peptide may be diffuse or focal; some of the focal deposits are amyloid. Aβ peptide accumulates not only in the core of the senile plaque but also in the vessel walls (amyloid angiopathy).
Two successive cleavages are necessary to free the Aβ peptide from the amyloid precursor protein (APP)—for a review see [317]. The first one, the so-called β-cleavage, at the extracellular N-terminus of the Aβ peptide, is due to the beta-site APP-cleaving enzyme (BACE) [42]. It produces a terminal fragment of APP composed of 99 AA called C99. The second cleavage, taking place on APP C99, is performed within a lipid membrane by the γ-secretase complex (made of presenilin1 (PS1) or presenilin 2 (PS2), Pen 2, nicastrin and APH 1)—for a review see [340]. The α-cleavage occurring in the Aβ sequence of APP prevents the production of Aβ. Four isoforms of APP are expressed in the human, of 695, 714, 751, or 770 amino acid residues. APP 751 and 770 contain a protease inhibitor domain, homologous to the Kunitz type of serine protease inhibitors. In a few families, AD is transmitted as an autosomal dominant trait. The mutations that have been found to be responsible for these cases of familial Alzheimer disease (FAD) are localized on the APP, PS1 or PS2 genes.
The tau pathology is mainly intracellular: accumulation of tau may occur in the cell body (neurofibrillary tangle = NFT), in the dystrophic axons surrounding the amyloid core of the plaque, and in the neuropil threads, which are mainly dendrites. At electron microscopy, tau protein mainly accumulates as paired helical filaments (PHF).
Before analyzing in some detail the numerous models of AD that have been proposed in the literature, we would like to consider, in a general way, the aims that are pursued when trying to mimic a human disease—and more specifically a neurodegenerative disease in vivo.
Signs, lesions, cause: the SLC reading key
Animal models aim at replicating the symptoms, the lesions or the cause of a disease. A “reading key” relating Symptoms (S), Lesions (L) and Causes (C) with scores 0–1 is illustrated in Table 1. In neurology, the signs and symptoms (for instance, hemiplegia) are principally linked to the topography of the lesions (for instance motor cortex), and are only poorly correlated with their nature (for instance both cerebral infarct and tumor); in other words, similarity of clinical signs does not mean similarity in pathogenic mechanisms. Destroying the cholinergic system with ibotenic acid will lead to behavioral symptoms that may resemble those of AD and be amenable to treatments such as anticholinesterases [226]. It is clear, however, that at the symptomatic level (S), therapeutic research cannot pretend to reach an understanding of the pathological mechanisms. Such a model can aid our understanding of the symptoms (it can be termed “S1,” i.e., it reproduces signs and symptoms), but gives no information on the lesions occurring in AD (we will qualify it as “L0,” i.e., it gives no information on the way that lesions appear and interact) or on the cause of the disease (“C0”): it can therefore be classified as S1L0C0.
At the L level, the model attempts to mimic the lesions: for instance, amyloid peptide has been injected into the brains of living mice in an attempt to understand its neurotoxicity [262, 290]. The results of such an experiment will not provide any information on the reason(s) for Aβ accumulation in the extracellular space. The model is of the type S0L1C0. However, it has also been shown that the Aβ oligomers may impede the synaptic functions and be directly implied in the memory dysfunction [321]; it may therefore also explain the signs of the disease (S1L1C0). A more subtle example, as discussed later in this article, is the modelling of the NFTs of AD by transgenic mice overexpressing mutated tau. There is no tau mutation in AD, so the model is clearly not adequate to understand the cause of AD (it is therefore classified as C0). But, however the tangles are produced, it may be interesting to understand how they interact with Aβ peptide in transgenic mice which develop amyloid deposits (L1C0). When the tangles are located in the limbic system, then the symptoms may mimic those of AD (S1L1C0); in other mouse lines, the expression of tau in the motor neurones was responsible for paralyses [247]: such a model may help to elucidate how the tangles may cause neuronal dysfunction. It does not aid our understanding of the mechanisms responsible for NFT formation in AD nor of the clinical signs of dementia (S0L1C0).
Finally, at the C level, the model attempts to reconstruct the biological mechanisms responsible for the disease, starting from its cause(s). Transfecting a mutated human APP experimentally reproduces the cause of familial Alzheimer disease, APP mutation. Some lesions similar to those seen in humans are found in these mouse lines, which may therefore be classified as L1C1. The connection with the symptoms is far from simple, and it may happen that these mice do not show the typical clinical signs of AD (S0L1C1).
The three levels (S, L, and C) are independent: lesioning the cerebral cortex by an ischemic lesion may, for instance, mimic the symptoms of dementia; it will have little to do with both the lesions and the molecular mechanisms of AD: it is a S1L0C0 model. Introducing a mutated APP gene into the mouse may mimic familial Alzheimer disease (S1L1C1 for familial AD), but it could well be that the mechanism has nothing to do with the mechanism of sporadic AD (it is then classified as S1L1C0 or even S0L1C0 as far as sporadic AD is concerned). It should be stressed that the cellular mechanisms which lead to Aβ and tau accumulation, and eventually to neuronal death, could be replicated in neurons located outside the cerebral cortex: the pathology could for instance be fully reproduced in the motor neurone of the spinal cord. In such a hypothetical example, the mechanism would be elucidated although the animals would not exhibit the symptoms and signs of the disease (S0L1C1), and possibly not even exhibit the lesions that are presently considered to be the mandatory stigmata of the disease (S0L0C1)—see Table 1 for examples.
Scope of this review
Which animal models are to be reviewed here? Several procedures—some of which are listed below—have been devised in the past to mimic AD in the animal. Destruction has been used to produce the cortical or subcortical symptoms of AD. We will not deal with these models that clearly belong to the S level. The reproduction of the lesions by exogenous chemicals has been attempted: NFTs caused by aluminum have been shown to be actually an accumulation of neurofilaments (and not of tau) [185, 225]. Injection of Aβ peptide may induce some clinical signs [227, 289] or, under certain conditions, accelerate the pathological process in a transgenic mouse—see later and [111]—but it does not directly reproduce the lesions of the disease [99]. Spontaneous animal diseases, resembling AD, have been looked for: old monkeys [245] and old bears [66] for instance, develop plaques and tangles; plaques have been seen in numerous species, noticeably in old dogs [62, 69], old cats [68], and in mouse lemurs (Microcebus murinus) [78]. No model has appeared sufficiently practical to be of common use.
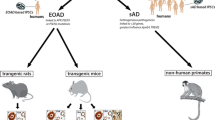
The real breakthrough came from the transgene technology. Transgenesis made it possible, probably for the first time, to reproduce specific neurodegenerative lesions. Mice have overwhelmingly been used and this review will principally deal with transgenic mice. Recently transgenic rats have been generated [96] with the aim of improving the behavioural analysis. Space is insufficient to deal with invertebrates models: transgenic drosophilae expressing beta-amyloid peptides have been devised to screen therapeutic targets [67]; the naturally lacking γ-secretase activity has been reconstituted in the yeast Saccharomyces cerevisiae [92]; the nematode Caenorhabditis elegans has also been used to elucidate the physiological role of AD molecular protagonists [134]. Flies, yeasts, and worms play the role of “gene factories,” which are particularly useful for studying protein interactions and unraveling molecular pathways. They are, however, too far from the neuropathology point of view, centered on the lesions, to be fully covered in this review.
In vitro models have been used to unravel the physiopathological mechanisms involved in AD. This is not the place to analyze the studies based on the hypothesis of a direct toxicity of Aβ peptide on the cell. In this paradigm, the effect of an experimental manipulation is usually tested by comparing neuronal death in control and experimental situations. Cell cultures have also been used to elucidate the subcellular topography of the secretase activities. BACE is located in endosomes and also at the cell membrane [142]; Presenilin 1 immunoreactivity is found in the endoplasmic reticulum, while the gamma-cleavage seems to take place downstream of the ER (the presenilin “spatial paradox”). The production of Aβ42 (but not of Aβ40) appears to take place in the endoplasmic reticulum/intermediate compartment [63] while Aβ40 is exclusively produced in the trans-Golgi network [114]. Primary cultures of hippocampal slices have been extensively used to study the impact of Aβ oligomers at the electrophysiological level (see later).
This paper is focused on transgenic mice. The literature has grown rapidly on this topic, and we have been forced, in many instances, to limit our subject and our analysis of the literature. The reader is referred to excellent reviews on the subject [102, 129, 214, 215, 285, 313]. We have deliberately not reviewed the effects of active or passive Aβ immunotherapy on transgenic (Tg) mice, since this subject is far too extensive for this review.
Specific problems raised by the pathology of transgenic mice
Transgenesis raises specific difficulties and questions. The number of transgenes that have been inserted and their sites of insertion are uncontrolled. The expression of the gene may reach high values that trigger cellular defence mechanisms that provide little information on the natural role of the transgene itself. The topography of the protein expression and its course during development largely depends on the promoter. Some defects may be related to anomaly of development and may be unrelated to the overexpression of the protein in the adult—a problem which can be solved through the use of inducible systems of expression (see later) or by the use of knock-down of gene expression by siRNA [274]. The genetic background may substantially modify the pathology [46], and uncontrolled results may be related to outbred lines. The transgenic animals should, if necessary, be back-crossed for multiple generations to obtain inbred lines. The incidence of gender has been mentioned in several studies: amyloid deposition has been found to be more extensive in female APP mice [323]. Pharmacological treatments with intended anti-Aβ effects have been found to have different (even opposed) effects in male and female transgenic mice, e.g., [240], reinforcing the contention that gender is a variable to take into account in the analysis of murine models.
The transgenic models of Aβ accumulation
After the identification of the Aβ peptide, initially in vessels of trisomy 21 patients and then in senile plaques of AD cases [105, 208, 341], several teams looked for “the” mutation responsible for the rare cases of familial Alzheimer disease (FAD)—only to realize that not one but numerous mutations were actually able to cause the disease. Mutations are indeed located not only in the APP gene [52, 106], from which the Aβ peptide is cleaved, but also in the genes of presenilin 1 or 2 [4, 259, 280] that are directly involved in Aβ production from APP.
It is now clear that there is not one but several Aβ peptides, with a C-terminal heterogeneity: some species end at the AA 40, and others at the AA 42 or even at AA 43, 45, 46 or 48 [248]; the cause of this heterogeneity is still unknown. Several Aβ species are N-truncated and were shown to be the main Aβ species in some APP mutations [173, 275]. All of the mutations that have been tested, when transfected in cellular models, induce an increase in the Aβ42/Aβ40 ratio [72], with the noticeable exception of the Arctic mutation directly involving the Aβ sequence itself [55]. All mutations induce an overproduction of Aβ except the mutation V715M, in which, however, the ratio Aβ42/Aβ40 is increased [6]. Transfecting the APP gene induces an overproduction of the protein, and APP overproduction may be sufficient to increase Aβ peptide secretion: both the β and the γ enzymatic activities do not appear to be rate-limiting. However, as we shall see, APP has generally to be mutated to produce a quantity of Aβ sufficient to cause visible changes.
Mutations of the gene of tau proteins are not associated with AD but with fronto-temporal dementia [284]. It is therefore logical to consider that AD pathogenesis is related to a change in APP rather than in tau metabolism. This conclusion is formalized as the “cascade hypothesis,” which states that the accumulation of Aβ peptide is the cause of a cascade of reactions that lead to tau pathology and neuronal death [116–119].
Various APP transgenic models
The three isoforms of human APP (hAPP) (695, 751, and 770 amino-acids) have been used as transgenes. The mutations of the APP gene that have been used most often are labeled by the place where they have been identified: Swedish (which is made of two contiguous mutations), London, and Indiana (K670N & M671L, V717I and V717F, respectively, with the numbering corresponding to the longest APP isoform). The hAPP gene has been driven by various promoters—PDGF, Thy-1 or Thy-1.2 (neuron-specific), and hamster PrP (not just neuronal)—which allows its exclusive or preferential expression in the central nervous system. A large but certainly incomplete list of the transgenic lines pertaining to AD can be found on the Alzforum website (http://www.alzforum.org/res/com/tra/).
The APP singly transgenic lines
Seventeen amino acids differ in mouse and human APP; three of them are located in the Aβ sequence (Arg 5 Gly, Tyr 10 Phe, His 13 Arg—the first AA is the human one). However, increasing the level of mouse APP does not cause Aβ deposition. Transfection of human APP is necessary [153], and the trisomy16 murine model (where no Aβ deposition is found) suggests that hAPP has to be mutated to obtain a reliable and abundant deposition.
Initial attempts
Now that numerous mouse lines with Aβ deposits have been produced, it is interesting to look back at the first, largely unsuccessful, attempts to develop an AD model mice [215]. After unconfirmed results of Alzheimer pathology in transgenics expressing the C-terminal part of APP [161] or the Aβ peptide under the promoter of APP [332], several lines were generated with various techniques. The sequence limited to the Aβ peptide itself, under the promoter of the light chain of neurofilament, was neurotoxic. Aβ remained intracellular and caused apoptotic cell death [179]. Since Aβ is partly hydrophobic, its cellular fate when synthesized outside a cell membrane was probably not physiological. These pathogenic effects of Aβ overproduction were probably not directly linked to the pathogenesis of AD. Several attempts were made to introduce wild-type hAPP into transgenic mice. Several transgenic lines were produced with a transgene that comprised the 100 AA of the C-terminal part of hAPP [160, 228]. A weak Aβ accumulation was found in the cell body and the neuropil; C100 was also found to aggregate in vesicular structures of the cytoplasm [160]. Long-term potentiation (LTP) was impaired [228], but the extracellular deposits of Aβ were limited or absent. In the APP-C99 (Tg 13592) mouse line, the signal sequence and the 99 amino-acids C terminal fragment (C99) of APP is overexpressed under a cytomegalovirus enhancer/β-actin promoter [97]. The expression is detected in many tissues, and Aβ deposits are detected only in the muscle in aged animals. The plasma concentration of Aβ peptide is increased 17-fold. There are no deposits in the brain. The mice exhibit hypoactivity and spatial learning deficit. This transgenic line indicates that the increase in plasma Aβ peptide concentration does not produce amyloid in the brain, and strongly suggests that the production of Aβ peptide takes place in the brain of FAD patients rather than at the periphery.
A yeast artificial chromosome (YAC) containing wild-type APP did not induce any visible changes. A YAC containing the hAPP gene encoding APP harboring the Swedish mutation, the London mutation or a combination of the two increased the Aβ42/Aβ40 ratio and decreased the concentration of α-secretase derivatives [184]. Aβ deposits and neuritic abnormalities were found in the olfactory cortex and olfactory bulb in 14 month-old animals which expressed a YAC containing APP with the Swedish mutation, mated to homozygosity [172]. A hAPP 695 transgene with the London mutation driven by the neuron-specific enolase (NSE) was not associated with any microscopical changes (probably because the levels of Aβ were not sufficient) [203]. These first attempts indicated that the Aβ sequence alone was inefficient; the whole sequence of APP had to be expressed, and only mutations were able to cause a significant increase in Aβ 42. The YAC technology was fruitful, but lesions were observed in limited amounts and only in old animals. The NSE promoter was not powerful enough to drive Aβ secretion to the threshold level necessary to cause lesions.
A large number of hAPP singly transgenic mice with significant changes have since been produced; only the singly transgenic mouse lines that have been most studied in the literature are listed below.
The PDAPP transgenic line
The transgene of the first mouse line with significant pathologic accumulation of Aβ peptide was a cDNA minigene bearing the sequence of hAPP carrying the Indiana mutation (V717F) with portions of APP introns 6–8. The presence of introns 7 and 8 allowed the alternative splicing of exons 7 and 8, and the expression of the 695, 751 and 770 APP isoforms. APP expression was driven by the PDGF promoter [98]. This PDAPP transgenic line has been extensively studied. From the age of six months, the heterozygous mouse develops visible extracellular deposits of Aβ peptide in the hippocampus, and at eight months in the isocortex [98, 146]. Some deposits are amyloid (Congo red and thioflavin S positive). Aβ peptide is also found in the vessel walls.
The Tg2576 mouse line
The Tg2576 mouse line [137] overexpresses the 695 isoform of hAPP with the Swedish double mutation (K670N/M671L) under the control of the hamster prion protein promoter. Aβ diffuse and focal deposits are found at 9–11 months of age in the heterozygous animal.
The APP23 mouse line
In the APP23 mouse line, developed by Novartis Pharma, the 751 isoform of hAPP with the double Swedish mutation is expressed under the control of a mouse Thy-1.2 promoter [292] (the same cDNA under the control of a human Thy-1 promoter had no pathology). There is diffuse and congophilic deposition of Aβ peptide in parenchyma and vessels from six months of age.
Line C3–3
This is also an APP bearing the Swedish double mutation, that is overexpressed in this mouse line. The chimeric mouse/human APP with the Swedish mutation K670N/M671L contains a humanized Aβ domain. The promoter is the mouse prion promoter. The mice do not develop plaques until 18 months of age [30, 31].
The Tg CRND8 mouse line
The Tg CRND8 mouse bearing both the Swedish double mutation and the Indiana mutation (hAPP695 K670N,M671L + V717F), under a hamster prion promoter, develops plaques at as soon as three months of age [57]. The high Aβ concentration and the highly increased Aβ42/Aβ40 ratio explain why this model is particularly aggressive.
The hAPP H6, J9 and J20 hAPP lines
Several Tg lines expressing, at various levels, wild-type or mutated hAPP were produced under a platelet-derived growth factor beta chain (PDGF) promoter. A summary of the most commonly used of these Tg animals is given in [222] (p. 4052). We just mention here the lines that we will consider later: the J9 and J20 lines, like the Tg CRND8 line, express hAPP with the Swedish and the Indiana mutation. In these lines, the human transgene is the isoform 770. The J9 line (“hAPPlow”) expresses a moderate level of neuronal APP and Aβ; the level of expression is high in the J20 line [56]. Line H6 also expresses hAPP with the Indiana mutation under the control of a PDGF promoter [344].
The APPDutch line
The E693Q mutation of APP induces a massive amyloid angiopathy, as described in Dutch patients. The disease has been replicated by generating a mouse line expressing hAPP751 with the E693Q mutation under a murine Thy1.2 promoter. Vascular accumulation of Aβ with hemorrhages and inflammation have been observed in these mice [128].
The ARC6 and ARC48 lines
The Arctic mutation (E22G) is located in the Aβ sequence; it stimulates Aβ fibrillization without changing the Aβ42/Aβ40 ratio. The transgene is a minigene containing APP with the Arctic mutation and also the Swedish and Indiana mutations, under the control of the PDGF promoter [54].
Data obtained from the comparison of different mouse lines indicate that the onset and the severity of the amyloid deposits are directly linked to the level of Aβ42 peptide. Sturchler–Pierrat et al., in parallel with the APP23, developed a line in which only a twofold overexpression of hAPP bearing the Swedish and the Indiana mutations was obtained. Aβ deposition was seen later than in the APP23 and there was little amyloid formation [292]. In a series of different mouse lines with a hAPP 751 transgene bearing the Swedish and the London mutations, the progression of the pathology appeared to be directly linked to the Aβ42 concentration [257], the level of Aβ(1–40) being higher in mice that did not show any amyloid deposits. A high level of Aβ42 is a necessary condition, but it is not sufficient: Mucke et al. generated different APP transgenic lines under the same promoter (PDGF); they noticed that the overexpression of wild-type hAPP, even if it increased the level of Aβ42, was insufficient to cause plaque formation—which was observed only when the APP transgene carried a pathogenic mutation known to be responsible for familial AD [222]. However, the late occurrence of Aβ deposits was mentioned in two lines (as briefly and incompletely described in the literature) in which hAPP, without mutation, was overexpressed under the control of a NSE [130] or a Thy-1 promoter [128]. Only the overexpression of APP751, not APP695, was able to induce Aβ deposition in the first model.
Trisomy 21 models
Chromosome 21, which is present in a triple dose in Down syndrome, contains the APP gene, which explains why AD lesions are almost constant at a relatively early age. An exceptional patient with a partial trisomy 21 that did not include the APP gene did not develop AD [244]. On the other hand, microduplication of the APP gene, inducing AD with prominent amyloid angiopathy, has recently been identified [261]. Models of trisomy 21 (trisomy 16 in the mouse) have been generated and provide information on the role not only of the APP gene but also of its contiguous genes in the pathology. Two segmental trisomy 16 models, Ts65Dn and Ts1Cje, have contrasted consequences. In the Ts65Dn mouse [251], a large segment of chromosome 16 including the APP gene is in three copies, while the segment in triplicate in the Ts1Cje mouse is smaller and does not include the APP gene nor the gene of the superoxide dismutase 1 (SOD1) [264]. Increased levels of APP mRNA and of the protein itself have been detected in the Ts65Dn mouse in the striatum by 6–8 months of age, and in the hippocampus and parietal cortex by 13–16 months of age. Aβ42 levels have been found to be increased at six months. At this age, the basal forebrain cholinergic neurons (BFCN) start degenerating [141], a degeneration that is related to impaired retrograde transport of NGF [64, 265]. Neither total tau nor tau phosporylated on the serine 199 are elevated in the Ts65Dn mice [140]. As expected, the level of Aβ42 is normal in the Ts1Cje mouse line (which has the normal two copies of the APP gene) and there is no degeneration of the BFCN. However, and quite unexpectedly, abnormal phosphorylation of tau has been detected in this mouse line without tangle formation [281]. In the “transchromosomic” 21 model (Tc1), an almost complete human chromosome 21 has been incorporated into the mouse genome [236]. Few data concerning APP metabolism are presently available.
Early endosomal alterations, the earliest known pathology detected in sporadic AD and DS, develop before Aβ is deposited and as soluble Aβ increases [50]. In the basal forebrain of Ts65Dn mice, neurons develop enlarged endosomes at two months. There is no enlargement of the endosomes in the Ts1Cje mice (no APP overexpression) or in transgenic mice overexpressing APP751 with the Swedish double mutation alone or in combination with the London mutation [49]. The cause of endosome enlargement is still to be fully elucidated.
Presenilin transgenic mice
Mutated human PS1 or PS2, when expressed alone, do not induce any detectable lesion, although they increase the level of Aβ peptide [211, 239, 268]. The behavioral impairment is modest [154, 183]. The mutated PS1 transgene, however, disturbs calcium homeostasis in the endoplasmic reticulum [211]. It has furthermore been recently shown that a mutated human PS1 transgene altered the fast axonal transport and induced tau hyperphosphorylation [189].
Doubly transgenic mice
The β- and γ-secretase pathway
APP and BACE (β-secretase)
APP plus BACE1
BACE1 cleaves APP at AA 1 of the Aβ peptide but also at AA 11, producing N-truncated Aβ. BACE1 transgenic mice (with the promoter of the Ca2+/calmodulin-dependent protein kinase II gene = CaMKII) have an increased turnover of serotonin and exhibit bolder behavior than control littermates [120]. hAPP mice have been crossed with mice overexpressing BACE1. The BACE transgene increased the level of Aβ but also that of the C-terminal fragments of APP [27]. The coexpression of BACE1 in a transgenic APP line increased the density of diffuse and focal deposits of Aβ peptide, but, unexpectedly, dramatically decreased the severity of amyloid angiopathy. This was considered a consequence of the abundance of N-truncated Aβ species. In this hypothesis, the N-truncated Aβ peptide accumulates preferentially in the parenchyma, while the full-length Aβ peptide may be drained and accumulates in the vessels [331]. In another study, BACE1 co-expression (murine Thy1 promoter) with hAPP decreased the level of Aβ and of APP, but worsened the severity of the neurodegeneration, which is possibly a consequence of the accumulation of APP C terminal fragments (CTF) [258].
APP minus BACE1
Mice knocked-out for BACE1 are viable and fertile and do not produce Aβ [199]. They are more anxious and less exploratory than the controls [120]. Mutation of the β-secretase cleavage site (M671I) on APP also eliminates the production of human Aβ [223]. Lowering BACE1 levels using lentiviral vectors expressing siRNAs that target BACE1 reduced amyloid production, and neurodegenerative and behavioral deficits in APP transgenic mice [282]. Crossing BACE1 KO mice with PDAPP mice [212] or TG2576 mice [199] prevented the pathology. Loss of BACE1 function rescued the behavioral alterations [212]. The effect was even spectacular in PDAPP mice heterozygous for BACE1, although the decrease in Aβ 42 was relatively modest (−12%) [212]. These results suggest that inhibition of BACE could be a therapeutic target. Unfortunately, other results indicate that BACE −/− × PDAPP mice have unexpected sensorimotor impairments, spatial memory deficits, and display seizures—a phenotype that could prevent the use of inhibitors of BACE [168].
APP and presenilins (γ-secretase)
APP plus presenilin
The co-transfection of human mutated (M146L or M146V) presenilin 1 significantly lowers the age at which the first plaques are detected [89, 131, 216], most probably by increasing the quantity of Aβ42 secreted. Wild-type PS1 or PS2 has no effect [89]. In C3-3 mice crossed with mice expressing a mutant PS1, the Aβ deposits are visible at nine months (instead of 18) [30, 31]. The PSAPP line has been obtained by crossing Tg2576 mice with mice expressing human PS1M146L. Amyloid deposits are present at six months (nine months in the Tg2576 mouse line). In a APPSLPS1M146L mouse model developed by Sanofi-Aventis, a hAPP751 gene carrying both the Swedish and the London mutations (K670N/M671L and V717I) under the control of the Thy-1 promoter is associated with a human mutant gene of presenilin-1 (PS-1 M146L) under the HMG-CoA reductase promoter (allowing a preferential cerebral expression). An intracellular accumulation of Aβ peptide is visible at two months, and Aβ plaques appear as early as three months [26, 186]. A similar mouse line with the M233T/L235P mutations knocked in the PS1 gene (APPSLPS1ki) develops a very aggressive form of the disease with a prominent neuronal loss in the CA1 sector [48].
The coexpression of hAPP with the Swedish double mutation (K670N/M671L) and of PS1 with the L166P mutation under the control of a neuron-specific Thy1 promoter element (APPPS1 mice) dramatically lowers the age at which the first lesions are visible: cerebral amyloidosis starts at 6–8 weeks, and the number of microglial cells increases threefold from one to eight months. Neuronal loss appears minimal [249].
The 5XFAD model was devised to accelerate Aβ deposition [231]; these APP/PS1 double transgenic mice coexpress five FAD mutations [APP K670N/M671L (Swedish) + I716V (Florida) + V717I (London) and PS1 M146L&L286V]. Intracellular accumulation of Aβ42 is seen at 1.5 months of age and amyloid deposition begins at two months.
The deletion of exon 9 in presenilin 1 increases, in man, the secretion of Aβ peptide and is associated with the occurrence of large and homogeneous senile plaques that are only weakly congophilic (the so-called “cotton wool plaques”). The occurrence of the lesions is accelerated in the mouse when a hPS1 gene with exon 9 deleted (line S9) is coexpressed with a hAPP gene with the APP Swedish mutation (line C3-3), yielding an APPswe/PS1dE9 line [100, 191]. The first Aβ deposits are detected at the age of 4–5 months. The E9 deletion of the PS1 gene, rather than inactivating the gene, induces a gain of function.
APP minus presenilin
The PS1 knockout (KO) mice are not viable. They have skeletal and CNS deficits (hemorrhages, deficient neurogenesis) which could partly be due to the role of the γ-secretase in Notch signaling [279]. Using a loxP/Cre-recombinase strategy, Dewachter et al. succeeded in generating a post-natal, neuron-specific, PS1 KO mouse. The absence of presenilin 1 prevented the formation of Aβ peptide deposits [77]. However, a cognitive deficit (object recognition test) was still present in the hAPP [V717I] × PS1 −/− mice, a deficit that the authors attributed to the increase in APP C99 (the product of the BACE cleavage of APP). The potential toxicity of C99 has been tested in the Tg 13592 line, in which spatial learning deficit has been observed in the absence of brain Aβ deposits.
The α-secretase pathway
The α-secretase cleaves APP in the Aβ sequence. ADAM10—A Disintegrin And Metalloproteinase—is presently the best candidate for the enzyme responsible for the α-secretase activity [170]. The wild-type human ADAM10 gene, in a mouse line carrying hAPP with the London mutation, increased the alpha-cleavage of APP, reduced the concentration of Aβ peptide, and prevented the formation of Aβ peptide deposits. In contrast, the expression of an inactive mutant of ADAM10 worsened the pathology [243].
Aβ degradation
Neprilysin
Neprilysin (or neutral endopeptidase 24.11 = NEP or CD10 or enkephalinase) is thought to be at least partly responsible for the degradation of Aβ peptide. This metalloendopeptidase is inhibited by phosphoramidon and thiorphan [149]. Transgenic expression of neprilysin improves the pathology and the behavior in an APP × PS1 mouse line with Swedish and Indiana mutations [242]. A lentiviral vector expressing human neprilysin decreases the density of plaques by half [205].
Chronic infusion of thiorphan in the rat induces Aβ deposition [149]. Increased concentration of Aβ peptide is observed in NEP−/− mice [91, 148]. Amyloid-like deposits and signs of neuronal degeneration have been observed in aged neprilysin-deficient mice [201]. Loss of NEP function in APP mice markedly increased hippocampal amyloid plaque burden, and led to the development of amyloid angiopathy. Even a 50% reduction in NEP activity was sufficient to increase amyloid neuropathology [95]. APP × NEP-KO mice have been shown to develop synaptic alterations and cognitive deficits, presumably in relation to increased levels of Aβ oligomers [138].
Inducible model
The difficulty involved in solubilizing amyloid, whatever its composition, meant that the question regarding the course of the disease if the Aβ accumulation is stopped but the amyloid stays in place remained open. An inducible model made it possible to study the evolution of the plaques after the hAPP695 Swedish/Indiana transgene had been inactivated. It appeared that the amyloid pathology did not progress, but it did not regress either. The amyloid core produced the same inflammation and was surrounded by dystrophic neurites [152].
Conclusions
The alterations observed in these various mouse models are compatible with a coherent view of APP metabolism: APP is cleaved by BACE1 and the γ-secretase complex to produce Aβ peptide. Higher Aβ levels are observed when either BACE or the γ-secretase activity is increased. When the concentration of Aβ is sufficient, deposits are observed in the mouse, but only if APP is mutated. Stimulating the α-secretase pathway (ADAM10 transgenic line) or the degradation of Aβ (NEP transgenic line) improves the pathology and the behavior.
In the next section we consider, from a pathological point of view, the lesions that are observed in the transgenic lines. We have distinguished the expected alterations, the alterations that are present in man and absent in the animal, and finally the lesions that raise new questions or suggest new points of view.
Pathological consequences of the accumulation of Aβ peptide
To simplify the terminology, the ambiguous term “senile plaque” will be avoided as much as possible. The term “diffuse” describes the nonamyloid (noncongophilic, nonfibrillar), large and irregular Aβ deposits; the term “focal” describes the small, spherical, intensely immunoreactive Aβ deposits; and the term “amyloid” is used for the deposits that are stained by thioflavin-S or Congo red.
Aspects for which the APP transgenic lines may serve as good models of AD
In many ways the APP transgenic mice mimic the amyloid aspect of AD pathology.
Aβ production and Aβ deposits
While APP overexpression remains roughly constant during the lives of the APP transgenic mice, the level of Aβ increases with age. In the PDAPP mouse line, for instance, Aβ concentrations increase 17-fold in the hippocampus between the ages of four and eight months, and by 18 months are over 500-fold that at four months [158]. From a given age on, the mice, which produce a large amount of Aβ42, develop visible deposits first in the hippocampus and isocortex and secondarily in some subcortical nuclei. Although the topography of the lesions depends on the transgene promoter, it should be stressed that the deposition exhibits a laminar pattern that suggests that Aβ42 is secreted in the terminal field of the neurons, probably just as occurs in humans. In some lines, this is particularly striking for the perforant path that links the neurons of layer II of the entorhinal cortex with the external molecular layer of the dentate gyrus [293]. Sectioning the perforant path prevents the formation of the amyloid deposits in the molecular layer of the dentate gyrus [188]. The deposits are Congo red and thioflavin S positive and are made of amyloid fibrils 9–11 nm in diameter, as in AD. The process by which the amyloid fibrils are formed is not a mechanical consequence of an increase in APP overexpression and Aβ peptide concentration. APP may be expressed at higher levels in regions devoid of plaques than in areas where they are abundant [158]. It has been shown that Aβ deposition can be dramatically accelerated by the injection of amyloid substances from older transgenic mice or even from human amyloid. Strangely enough, somewhat similarly to what has been observed in prion diseases, the fibrils obtained by simply having the synthetic peptides precipitated in solution are not efficient [218, 319].
Amyloid angiopathy
Amyloid angiopathy is common in APP transgenic mice [127]. It was a common belief that Aβ deposition in the vessel walls of perforating arteries and subarachnoid vessels was due to the secretion of Aβ peptide by the smooth vascular muscle cells [338]. Tg mice have demonstrated that this is far from always being true. In some transgenic lines, amyloid angiopathy appears particularly prominent—as in the line generated by Van Dorpe et al. (695 isoform of hAPP—London mutation V717I; murine Thy1 promoter) [315] and in the line APP23 (isoform 751 of APP with Swedish mutation; murine Thy-1.2 promoter) [43]. The role of the Aβ42/Aβ40 ratio is an important determinant of the distribution of Aβ in vessels or in parenchyma: the APPDutch mice (E693Q APP751) develop prominent amyloid angiopathy, associated with an increased level of Aβ40. However, the APPDutch mice crossed with PS1G384A Tg mice mainly develop parenchymal deposits, with an increased ratio of Aβ42 to Aβ40 [126]. Since the deposition is seen in transgenic lines in which Aβ peptide is expressed under a neuronal promoter, it is highly probable that the peptide produced by the neurons accumulates in the vessel walls [43, 315]. This is compatible with the theory put forward by Weller et al. that the Aβ peptide is drained with interstitial fluid through the perivascular space (in a direction opposite to the arterial blood flow) [328]. Recently, Aβ peptide was found in the perivascular space of APP23 mice and also, in small amounts, in wild-type aged animals. Aβ was colocalized with ApoE, suggesting that the drainage of Aβ could involve an interaction with ApoE [301].
Pathology of synapses
Synaptophysin immunoreactivity
Loss of synaptophysin immunoreactivity (IR) has been considered to be a hallmark of AD pathology and the best correlate of cognitive deficit [298], an opinion that has, however, been under discussion [79]. The results in the Tg mice have been contradictory. Some studies reported an absence of change: in the APP23 mouse line, for instance, no loss of synaptophysin IR has been detected despite robust Aβ deposition [28]. The loss may be subtle: in the TG2576 APP mouse line, no loss was initially observed, but rather an increase, correlated with a deficit in synaptic function [165]; a more exhaustive stereological and ultrastructural analysis in the same line found a decrease in the synaptic density of the external molecular layer of the dentate gyrus, in close relation to the Aβ deposits [87]. Some studies report a reproducible loss of synaptophysin IR. The decrease in density of presynaptic terminals precedes by several months the extracellular deposition of Aβ peptide in line H6 (see above) [136]. An age-dependent decrease in synaptophysin IR has been documented in the PDAPP mouse line [84]. Mucke et al. have generated several mouse lines expressing either wild-type or mutated human APP. At the same level of expression of hAPP, extracellular deposits of Aβ peptide are observed only when APP is mutated, even when the level of Aβ42 is high. The density of synaptophysin IR is even found to be decreased in mice expressing wild-type APP without Aβ deposits. It is inversely correlated with the level of Aβ42, but it is not necessarily associated with a high plaque load or with a high level of APP expression [222]. Synaptic alterations can thus be seen in the absence of extracellular deposit of Aβ peptide. Moreover, an age-related decrease in synaptophysin IR has been observed in PS1 singly transgenic mice [263]. Presynaptic markers synaptophysin and syntaxin as well postsynaptic density-95 decreased with age in the 5XFAD model [231].
The density of dendritic spines decreases in the CA1 sector of PDAPP and of Tg2576 before Aβ deposition [187]. It has been suggested that the loss of dendritic spines could be related to the toxicity of Aβ oligomers. The density of spines of rat pyramidal neurones in culture was decreased after exposure to picomolar levels of soluble oligomers of Aβ peptide. This effect is mediated by NMDA-type glutamate receptor and is reversible [278]. Aβ-derived oligomers (ADDLs) selectively bind to postsynaptic densities of presumably excitatory neurons (sparing the inhibitory GABAergic ones) in cultures of highly differentiated hippocampal neurons. This binding is associated with a decrease in membrane expression of NMDA and EphB2 receptors and with the appearance of abnormally long thin spines [177].
While the effect on spines is probably caused by Aβ-soluble oligomers, larger changes observed on dendritic trees seem to be more directly correlated with fibrillar amyloid deposits. In the Tg2576 transgenic line, the dendritic density is diminished within the boundaries of amyloid-beta plaques, with the greatest loss (about 80%) in the thioflavin S positive cores. The processes are abnormally curvy [190]. In the same line, in vivo imaging using multiphoton confocal microscopy reveals spine loss and shaft atrophy of dendrites near Aβ deposits [304].
In conclusion, the data in the literature indicate a regular drop in the presynaptic marker synaptophysin in the APP transgenic mice; this decrease may be seen in the absence of Aβ deposits (but with high concentrations of Aβ42), and has been also noticed in PS1 transgenic mice. The fibrillar deposits of Aβ peptide, on the other hand, alter the dendrites.
Long-term potentiation and Aβ oligomers
Long-term potentiation (LTP) is an enhanced synaptic transmission observed in synapses that have previously been stimulated. It is studied through electrophysiological means ex vivo (brain slices) or in vivo. LTP, which can be considered to be a mechanism that supports learning and memory functions, was shown to be severely impaired in old Tg2576 mice [51]. In the PDAPP mouse model, abnormal neurotransmission in hippocampal circuits can be detected before the formation of extracellular deposits of Aβ peptides [104]. Aβ peptide oligomers rapidly and significantly block LTP [320]. PS1 mutation alone can also induce anomalies in synaptic transmission that are similar to those observed after the application of Aβ42 peptide and are probably related to a decrease in the number of synapses [187] rather than to a modulation of their function [246].
In conclusion, the data in the literature suggest that synaptic alterations could be directly correlated with a high concentration of Aβ42, the amyloid conformation probably adding some supplementary detrimental constraints on the dendrites. They also suggest that electrophysiological alterations may be present in the absence of structural changes and that Aβ oligomers are responsible for these changes.
Synapses and connections
It has been known for a long time that neurites comprising the corona of the senile plaque contain synapses. The origin of the axons that contribute to this “innervation” of the plaque is unknown except in rare circumstances (for instance, the axons in the superficial part of the molecular layer of the dentate gyrus come from the entorhinal cortex; they probably heavily contribute to the plaques innervation in that region). It has been possible to track corticocortical connections with an anterograde tracer in APPxPS1 mice and to show that some of them came into contact with the plaque core, while thalamic connections for instance avoided the plaque by following a curvy trajectory (Fig. 1a, b) [74, 75]. Entorhinal axons form dystrophic boutons in contact with Aβ deposits located in the entorhinal projection area of the dentate gyrus [241]; aberrant boutons were found associated with amyloid in ectopic locations within the hippocampus, the thalamus, white matter tracts, as well as surrounding vascular amyloid [241]. These data show the presence of profound changes in neuronal connections that had been underestimated and probably contribute to dementia.
Connections of plaques. a The anterograde tracer biotinylated dextran amine (BDA) was injected into the mediodorsal nucleus of the thalamus. The prefrontal cortex was examined after Congo red staining. The anterogradely labeled fibers are shown in brown (long arrow). The normal connections are present and avoid the plaque, whose core is stained by Congo red (small arrow). b BDA was injected into the posterior cingulate cortex. Labeled fibers are visible in the visual cortex (black), which is normally connected with the posterior cingulate cortex. Several fibers (arrows) come into contact with the amyloid deposit (brown; immunolabeled by a polyclonal anti-Aβ42 antibody) and appear dystrophic. Bar = 10 μm for a and b. This experiment suggests that only a subset of the cortical connections “innervates” the plaque [75]
Pathology of neurites and axonopathy
The amyloid deposits induce massive changes in the neurites that surround them (the corona of the plaque). They are labeled by antineurofilament and anti-APP antibodies (PDAPP mouse line, 10–12 months of age) [207]. The tau immunoreactivity of the corona neurites has attracted much attention, since it may constitute the missing link between Aβ and tau pathology. Phosphorylated tau and ubiquitin epitopes generally appear late on, after 14 months of age in the PDAPP line [207]. No paired helical filaments (PHF) have ever been identified at electron microscopy [207] (with the noticeable exception of Kurt et al. [176]). The dystrophic neurites in the Tg2576 mouse are enriched in GSK3β, suggesting that this kinase is principally responsible for tau phosphorylation [303]. In a APPSwe/L × PS1 model, most Aβ peptide deposits are surrounded by a high number of degenerating neurites containing APP, ubiquitin, and manganese-dependent superoxide dismutase. Mitochondrial markers (cytochrome c, cytochrome oxidase 1, and Bax) are also present in these degenerating neurites. Phosphorylated tau immunoreactivity appears late and develops at a slow pace [25].
The accumulation of neurofilament, APP, tau and ubiquitin epitopes is associated with morphological changes of the neurites. The amyloid core of the plaques in PDAPP mice crossed with mice overexpressing yellow fluorescent protein (YFP) in a subset of neurons is surrounded by markedly enlarged YFP-labeled axonal and dendritic varicosities [36]. The geometry of the neurites in or near the amyloid core is modified [190]. The presence of abnormal axonal varicosities near fibrillar deposits has also been observed in vivo by transcranial two-photon imaging [304] (Tg2576). An alteration of axonal transport has been considered to be the possible cause of these changes: spheroids and myelin ovoids, axonal accumulation of APP, neurofilament and ubiquitin are observed in the white matter of the spinal cord [337] in the APP × PS1 and APP × PS1—Ki lines developed by Sanofi-Aventis [26, 336, 337]. Anterograde tracing of cortical connections has also revealed abnormal boutons in contact with the amyloid core [75, 241] (Fig. 1a, b). The tracing of connections by DiI, a lipophilic carbocyanine dye, has been used by Capetillo–Zarate et al. [45]. They found, in the APP23 mouse line, a selective vulnerability of commissural neurons.
Pathology of the cholinergic and other neurotransmitter systems
Cell loss affecting basal forebrain cholinergic areas (observed in patients with AD [330]) has not been reported in transgenic mice ([125]; reviewed in [102]) except in the trisomy 21 model (trisomy 16 in the mouse) [141, 265]. Dystrophic cholinergic neurites, in contrast, have been regularly observed in contact with congophilic plaques [38, 200, 292]. Several studies have demonstrated decreased cholinergic terminals in APP [103] or APP/PS1 [342] transgenic mice (see however, [81] for mixed results). The Tg2576 mouse shows a significant elevation in the density of cholinergic synapses in the frontal and parietal cortices, but in the double transgenic Tg2576 × PS1M146L the density of cholinergic synapses is significantly reduced in the frontal cortex. The size of these synapses is smaller than in wild-type animals in the frontal cortex and hippocampus [342]. A reorganization of cholinergic innervation (reduction of acetylcholinesterase-positive fibers in the subiculum; increased fiber density in CA1 and in the dentate gyrus) has also been mentioned [38]. Minor changes in acetylcholine release were measured by microdialysis [121]. Decreases in the enzymatic activity of the cholinergic, serotoninergic and noradrenergic systems were noticed only in the more aggressive models such as the APP23 [311]. These data indicate that the changes in neurotransmission are, as far as presently known, limited in APP Tg mice, which are therefore poorly adapted to testing therapeutics aimed at improving neurotransmission in AD.
Alterations that are lacking in the APP transgenic mouse models
Despite the many similarities between the pathology of AD and of its Tg models, the APP Tg mouse is not a perfect replica of AD. The most striking difference is the absence of NFTs. Even if hyperphosphorylated tau has been detected with immunohistochemical methods, as we have seen, PHF has, to our knowledge, never been found. The link that has been postulated in the cascade hypothesis between the alteration of APP metabolism and tau accumulation has not been reproduced, and the reason for this failure is still unknown. On the other hand, the large predominance of Aβ deposition on all other lesions in the Tg mice provides a new opportunity to study the effect of Aβ accumulation as if in isolation, not mixed with tau pathology.
Problems and questions
The transgenic animals, by allowing the exploration of uncharted territories, have revealed new pathogenic possibilities, although many of these cannot yet be proven in the human. There are, on the other hand, some discrepancies between the data obtained in the mice and in man, which remain unexplained. In this section we discuss the discrepancies and the open questions.
Atrophy
The atrophy of the medial part of the temporal lobe, including the entorhinal cortex, hippocampus and amygdala, is probably one of the best-established signs of AD. Atrophy has also been detected in the main APP transgenic lines, but with an unexpected time course. Most of the studies that have evaluated brain atrophy in transgenic mice have been carried out in the PDAPP model [84, 109, 250, 309, 327]. These investigations reported a reduction in hippocampal volume and a severe atrophy or agenesis of fiber tracts (fornix and corpus callosum). The alterations are already observed in young animals (three months) before the accumulation of Aβ and show no further deterioration in older mice [84, 109, 250, 309, 327]. They have to be considered in parallel with the difficulties met when searching for a significant neuronal loss in Tg animals (see the next section on “Neuronal loss”). Atrophy in Tg mice may therefore be the consequence of a developmental defect [124, 202] that could be amplified in strains with specific genetic backgrounds [202]. This observation suggests the possibility that some functional alterations observed in Tg mice are related to developmental changes rather than to the accumulation of Aβ peptide. Alternatively, the atrophy could be related to early alterations caused by the toxicity of Aβ oligomers before the formation of plaques.
The comparison, by in vivo MRI, of APP/PS1 Tg mice (Double Thy1 APP751 SL × HMG PS1 M146L developed by Sanofi-Aventis [26]) with plaque-free PS1 Tg mice did not reveal atrophy in young APP/PS1 animals. Hippocampal volumes are not affected by APP overexpression, regardless of age. However, an age-related atrophy occurs in APP/PS1 mice, involving posterior brain regions, including the midbrain and the internal capsule, the corpus callosum and the fornix. The pattern of atrophy, which involves white matter and largely spares the isocortex and hippocampus, is different from that reported in AD patients [76].
Neuronal loss
Contrarily to the popular belief that neuronal death is the essence of Alzheimer pathology, neuronal loss is particularly difficult to assess and opposite views have been expressed concerning its course and severity in AD (see for instance [108, 254]). Roughly speaking, two contrasting opinions have been expressed. For some, the neurotoxicity of Aβ peptide is directly responsible for the neuronal death [348]. Numerous cellular models have indeed shown, in vitro, the toxicity of the peptide (or even of part of the peptide) and have quantified the cell death that it induces. However, it is not yet clear how these results obtained outside living tissue can be transposed to the whole brain. In the human, for instance, large diffuse deposits are commonly seen in intellectually normal aging persons and in the absence of overt neuronal death; they may surround normal-looking neurons [73, 80]. On the other hand, the neurofibrillary pathology has often been incriminated as the direct cause of neuronal death. The “ghost tangles” (i.e., tangles left in the extracellular space after the death of the neurons that contained them) are a direct proof of the neuronal death caused by or at least associated with the NFTs [33]. Finally, other as yet unknown mechanisms have been incriminated [108].
Conflicting results have also been obtained for the transgenic mice, and a paradoxical increase in the number of neurons has even been noticed in young animals of the APP23 mouse line [29]. As a general rule, the neuronal loss has been mild or absent in singly transgenic lines: no significant neuronal loss has been found in the isocortex or hippocampus of PDAPP mice [146] except in the immediate vicinity of amyloid focal deposits [307], and in the Tg2576 mice [145]. Mild neuronal loss was described for instance in the APP23 mouse line [44] and in the CA3 sector of PDAPP mice [136]. By contrast, the neuronal loss was found to be moderate or severe in doubly transgenic mice (Tg2576 × PS1-M146L [307]; Swedish and London mutations ×PS1 (M146L) [271]; Swedish and London mutations × knock in PS1 (M146L) [48]; 5×FAD [231]). In the majority of the lines, the neuronal loss involves the hippocampus (with a few exceptions—cingulate cortex: PSAPP mice [307]; layer V of the isocortex [231]). The cause of the neuronal loss has been discussed: Aβ42 peptide at high concentration [231], amyloid Aβ deposits [307]; intracellular Aβ [48]. There is, however, some consensus that the possible toxic effect of Aβ peptide on the neurons is not direct, since the loss is not correlated with the amyloid burden, may be absent in regions rich in Aβ deposits and, in contrast, can be seen at some distance from them [271].
The nature of the precipitated amyloid peptide
The different isoforms of Aβ peptide are the main [260], and possibly the only [283], constituent of the core of the senile plaque observed in the human. These isoforms include full-size Aβ peptides 42 and 40 as well as N-truncated molecules that could represent up to 60% of all the Aβ species. The major truncated variants consist of Aβ peptide starting at AA 2–5 and 8–10 [275]. Post-translational modification leads to alteration of the Aβ molecule: isomerization, racemization, pyroglutamyl formation, oxidation, and covalent linkage of Aβ dimers [175]. As a consequence, the Aβ peptide of the human senile plaque appears particularly difficult to solubilize.
Aβ deposits observed in transgenic mice resemble those depicted in human patients, showing classical immunoreactivity with specific anti-Aβ antibodies and also amyloid characteristics following histochemical stainings (green fluorescence with thioflavine-S and Congo red birefringence under polarized light). The deposits of Aβ peptide in the APP Tg mice contain Aβ40 and Aβ42 as in the human [297], but have different physicochemical characteristics. At variance with what is observed in the human, in the APP23 Tg mice [175], as in Tg2576 mice [159], the Aβ peptide is fully soluble in buffers containing SDS. This is attributed to the lack of the post-translational modifications that are observed in man [175]. Quite intriguing is the weak affinity of the transgenic murine amyloid to the Pittsburgh compound-B (PIB) that is used in the human to visualize the senile plaques [167]. Changes in affinity might be caused by differences in the secondary structures of Aβ peptides deposited in human and mice brain tissues.
The topography of the Aβ deposits
The topography of the Aβ deposits follows, in man, a stereotyped progression that has been formalized by Thal et al. [302] (isocortex, hippocampus, basal ganglia, brainstem, cerebellum). This progression is not replicated in the Tg mice, where Aβ deposits often mainly affect the hippocampus, and where it largely depends on the promoter that is used.
Intracellular Aβ peptide
The abundance, the significance and even the presence of intraneuronal Aβ peptide (IAβ) in man are still under discussion. Since it is difficult to distinguish from lipofuscin, IAβ has probably been underestimated in human neuropathology. A technical factor altering the IR of Aβ peptide may have contributed to this underestimation: the use of heat enhances the visualisation of IAβ, but formic acid impedes it [70, 71, 238]. Formic acid is commonly used to enhance the IR of extracellular Aβ. The use of antibodies directed toward the N- and C-termini of the peptide has demonstrated that the IAβ is mainly made up of the 42 isoforms and is N-truncated (see for instance [113, 325]). IAβ could therefore be the cleavage product of α- and γ-secretases. There is some controversy concerning the abundance of intracellular Aβ peptide: Wegiel et al. detects it even in glia and at a young age. For them, it is unrelated to AD pathology, since it is observed in regions where Aβ deposition does not occur [325]. On the other hand, for others, intraneuronal Aβ accumulation, which takes place within the multivesicular bodies [294] (a specialized form of lysosomes) is an essential factor of the pathogenesis [18, 113, 178, 294, 334]. It has been seen in Down syndrome patients before the appearance of senile plaques [115, 221], and is said to be present in vulnerable regions before the development of full-blown pathology [113].
This point of view has been stimulated by the analysis of Tg mice. Large granules containing Aβ peptide immunoreactivity have indeed been seen within the cortical neurons of several transgenic lines, such as Tg2576 mice [113, 294], APPSLPS1M146L [186, 335], APPSLPS1 M146LKI [48] and 3 × Tg-AD mouse [233, 234]. In the transgenic models, intraneuronal Aβ accumulation is easy to identify and much simpler to distinguish from lipofuscin than in man. The density of intraneuronal Aβ peptide decreases while the density of extracellular Aβ deposits increases [186, 234, 335], suggesting that the secretion of intracellular Aβ is responsible for its extracellular accumulation (Fig. 2). The removal of extracellular Aβ deposits (by immunotherapy) is shortly followed by the clearance of intraneuronal Aβ, indicating that there is a dynamic balance between the two pools [234].
Comparison of extracellular deposition and intracellular accumulation of Aβ peptide in APPxPS1 Tg Mice. Five illustrative mice, taken at 2, 5, 9, 11, and 15 months of age, were studied. Sections, 25 μm in thickness, were immunostained with an anti-Aβ8–17 antibody (clone 6F/D3; Dako, Glostrup). The extracellular deposits of Aβ peptide are plotted on the left side in green; the intracellular granules of Aβ peptide are shown in red on the right side. Intracellular Aβ is visible after just two months, before the appearance of extracellular deposits. The density of intracellular Aβ decreases with the increase in the density of extracellular deposits of Aβ peptide. Scale bar = 1 mm. Modified from [186]
In conclusion, the frequency of intracellular Aβ peptide accumulation and its temporal relationship with the extracellular deposits in transgenic mice raise new questions: does the intracellular accumulation also constitute a constant stage in the neuropathology of AD? Should the cascade hypothesis be changed accordingly [334]? Is it, in contrast, due to the overproduction of Aβ peptide, observed only in a subset of AD (genetic cases)? Is its easy recognition in Tg animals the mere consequence of the artificial overexpression of APP? If the extracellular Aβ originates in the intracellular pool, why doesn’t the extracellular pool only consist of N-truncated species? No other example better illustrates the interplay between AD and its experimental models. The emphasis placed on intracellular Aβ is clearly a consequence of the scrutiny of the transgenic mice. On the other hand, its importance in Tg models has led to a reassessment of its role in the human.
Kinetics of the change
Multiphoton confocal microscopy, which does not induce the lesions caused by the high energy of the laser beam used in standard confocal microscopy, allows the examination of living tissue. This technique has been applied to living transgenic animals, so that the cortex can be visualized through a window made in the skull. Observations made over periods of months have provided new insight into the kinetics of the Aβ deposits in the parenchyma and in the vessel walls: focal amyloid deposits develop rapidly. They could be followed over periods of up to five months. Most of them remain stable in size and shape. Only a small population of the deposits grew or shrunk in Tg2576 mice [59]. The topical application of anti-Aβ antibodies cleared diffuse and focal deposits over a 3–8-day period [14].
Intracortical injections of adeno-associated virus (AAV) containing the gene for enhanced GFP in TG2576 allowed some neurons to be visualized, the processes of which could be followed over long distances. Around 14% of all the dystrophic processes in contact with the amyloid core were dendritic. Neurites did not penetrate the dense amyloid cores but curved around them. A severe deficit in spine density (−50%) was noticed within a distance of 20 μm from the plaque edge. A decrease (−25%) also occurred on dendrites not associated with plaques. Plaques and dendrites remained stable over the weeks of observation [286]. In a further study using the same methodology, a small subset of spines (around 5%) was found to appear at one-hour intervals in the control groups, counterbalanced by a similar percentage of spines that disappeared. In the Tg2576 mice, spine elimination increased, resulting in spine loss, especially in the near vicinity of the plaques [287]. In another experiment, the dystrophic neurites surrounding the amyloid core were visualized by their spontaneous fluorescence in the PDAPP/YFP model mentioned earlier, while the amyloid core was revealed by the in vivo fluorophore methoxy-X04, which has a high affinity for amyloid. Dystrophic neurites appeared stable over a three-day period. Antibodies applied at the surface of the brain partly cleared the Aβ deposits but also significantly improved the neuritic dystrophy within three days [35]. In Tg2576 mice, methoxy-X04 reveals that the first vascular amyloid deposits involve the leptomeningeal arteries as multifocal deposits of band-like Aβ. New observations made at weekly intervals showed an increase in the number of amyloid bands and a widening of those already present. Over time, the propagation of existing bands overtook the initiation of new ones [255]. In conclusion, these lesion kinetics observations indicate that the amyloid deposits are relatively stable, and that the amyloid angiopathy progresses initially by initiating new foci of deposition and later by increasing their size. The study of the dystrophic neurites suggests that they are relatively inert, while a small population of spines is continuously modified by plastic changes. An increase in the number of disappearing spines that is not balanced by a similar increase in the number of new spines explains the loss of spines that is found in the Tg2576 mouse line.
Inflammation and gliosis
The presence of microglia within the senile plaque and of astrocytes surrounding the amyloid core has been known for a long time and is mentioned in classical textbooks. These glial cells have been shown to express numerous inflammatory cytokines (reviewed in [2]). The presence of microglia and of astrocytes around the focal Aβ deposits has been abundantly documented in Tg mice. The first inflammatory changes are observed quite early, before any visible Aβ deposition. They are associated with increased BACE activity [123]. However, the cytokines whose expressions are induced by Aβ peptide, particularly the peptide in its fibrillar form, have been discussed and contradictory results have been published in the literature [20, 209, 217]. In the Tg2576 mouse line, for instance, IL-1β and TNF-α -immunopositive microglia as well as IL6 immunopositive astrocytes have been found in close contact with amyloid Aβ deposits [20]; the authors conclude that these changes are similar to those seen in man. Mehlhorn et al., in the same mouse line, only found an overexpression of IL-1β in the reactive astrocytes that surrounded the amyloid deposits, and concluded that the local immune response in transgenic Tg2576 mouse brain was different to that observed in brains from AD patients [217]. The microglial cells present in the plaque are partly derived from the bone marrow, as demonstrated by grafting bone marrow from mice expressing enhanced green fluorescent protein. Fluorescent microglia was detected around the amyloid deposits when the graft had been performed before the onset of pathology; they were less abundant when the graft was done in an old animal [204]. The presence of activated microglial cells in contact with the Aβ deposits has been explained in different ways: for Wegiel et al. [324, 326], the microglial cell is the “driving force” responsible for the transformation of nonfibrillar Aβ into congophilic amyloid deposits, while for others it is linked to the inflammation that is associated with the amyloid core [20, 295]. The effects of inflammation have also been discussed and captured through transgenic technology. It should be noted that several experimental data have uncovered the positive role of inflammation. TGF-β1 overexpression promoted the clearance of parenchymal Aβ by microglial cells but increased amyloid angiopathy [343]. The level of C3 complement factor was elevated in these mice. To inhibit C3, soluble complement receptor-related protein y, a complement inhibitor, was expressed with hAPP. The amyloid pathology was increased two- to threefold, suggesting that the activation of the complement that took place in the Tg mice was useful [345]. The inhibition of C1q (the recognition component of the classical complement activation pathway) had an opposite (although less marked) effect. The absence of its gene in Tg2576 mice and in APP/PS1 mice did not modify the amount of Aβ deposition and its amyloid transformation. However, it was associated with a lower level of glial activation around the Aβ deposits and improved the loss of synaptophysin and of MAP2 immunoreactivity. The Aβ deposits were reduced when double transgenic APPswe/PS1 delta E9 mice were crossed with mice overexpressing IL-1 β [277]. Injection of lipopolysaccharide into the hippocampus of APP/PS1 mice stimulated recruitment of microglia and reduced Aβ burden [204]. It is also clear that passive or active immunotherapy, which both bring anti-Aβ antibodies into contact with the amyloid deposits, produced spectacular results in the PDAPP mouse [269] and indicated that inflammation was not necessarily detrimental.
However, the benefits of inflammation must be contrasted with the deleterious effects observed after the overexpression of several inflammatory proteins. These data helped to advocate an anti-inflammatory strategy in AD: α1-anti-chymotrypsin, an acute-phase inflammatory protein, promoted amyloid pathology when coexpressed with hAPP in singly Tg mice [224, 230]. Coexpression of Cox2, an enzyme implicated in inflammation and inhibited by a class of anti-inflammatory drugs, with APPswe and PS1A246E did not modify Aβ pathology but induced an elevation in the number of phosphorylated retinoblastoma (pRb) tumor suppressor protein and active caspase-3 immunopositive neurons [346].
In conclusion, the presence of astrocytes and microglia around the amyloid core of the plaque is seen both in the human and in the Tg mice. The inflammation is, however, less severe in the latter [272]. The immunological mechanisms involved, the cytokines that are secreted, and even the effect (beneficial or detrimental) of inflammation remain the source of much discussion, with contradictory results published in the literature. The spectacular effect of immunotherapy has, however, demonstrated that the microglia, when correctly stimulated, are able to clear the extracellular Aβ deposits. This suggests that, on the whole, triggering an adequately oriented inflammation is a better strategy than attempting to silence it.
Alteration of neurogenesis in hAPP transgenic mice
Neurogenesis, restricted to the dentate gyrus and the subventricular zone in the adult, has been found to be enhanced in Alzheimer disease [157]. Largely divergent results have been obtained in different mouse lines expressing either mutated APP alone or mutated APP with mutated PS1. A two-fold increase in BrdU incorporation in the PDAPP mice was initially described by Jin et al. [156]. Several authors found that the proliferation of the neural progenitors was reduced [86, 88, 122], with a parallel reduction in their survival [122], in connection with the amyloid deposits [88] or even before their appearance [86]. Zhang et al. found the effect on neurogenesis to be linked to the presence of a mutant PS1 gene [351]. Finally, the proliferation was found to be increased by Verret et al., while the survival at four weeks of the newborn neurons was decreased in correlation with the Aβ deposits [318]. The effect could also depend on the ApoE genotype (see later).
Correlations between pathology and physiological alterations
Ideally, mimicking the lesions in a Tg mouse should induce clinical symptoms that are similar to those seen in man; as already mentioned, however, the signs depend largely on the topography of the changes. A L1C1 model could be S0 if the lesions, although a good replica of what is seen in man, do not occur at the correct place (see the “Signs, lesions, cause: the SLC reading key” above). We will have the opportunity to study such situations in tau mice. However, many attempts have been made to isolate specific signs that could be improved by the treatment and would allow a therapeutic screening.
Regulation of body weight, body temperature, sleep, increased lethality
Decreased thermoregulation and altered wake/sleep patterns have been described in PDAPP mice [139]. APP transgenic mice are occasionally reported to have reduced body weights and enhanced (premature) lethality [57, 164, 166, 174, 220]. These alterations depend on the genetic background and are still poorly understood: neurodevelopmental defects could be one of the factors; acute events (such as spontaneous epileptic seizures) might also play a role.
Behavioral changes in Tg mice
Anomalous anxiety-related behaviors are occasionally noted in APP transgenic mice, taking the form of either neophobia or, in contrast, hypo-anxiety and reduced inhibition [85, 101, 182, 237]. The anatomical correlates of these behavioral changes are unknown.
Neurological disorders
Signs of neurological impairments have been described in both single APP and double APP/PS1 transgenic mice from different lines (i.e., PDAPP, Tg2576, APP23, TgCRND8, APP/PS1 lines). Motor dysfunction and difficulties in coordinating movements are shown by reduced grip strength and altered behavior on a beam or an accelerated rotating device (rotarod) [12, 164, 166, 310]. The integrity of sensory functions has not been fully documented in APP transgenic mice. Enhanced acoustic (startle) reflex in TgCRND8 mice may indicate the abnormal processing of auditory stimuli [213]. Impairments in visually-guided navigation (swimming to a cued location in a spatial environment) could reflect compromised visual abilities [166]. A number of studies indicate that APP transgenic mice are hyperactive [12, 85, 132, 166, 182, 237], but locomotor activity has been shown to be decreased in the APP23 model that develops severe cerebral amyloid angiopathy in addition to parenchymal Aβ plaques [181, 310].
Cognitive dysfunctions
Based on the evidence of an amnesic syndrome and early medial temporal lobe pathology in AD patients, behavioral studies in APP transgenic mice have largely focused on learning abilities for tasks relying on the integrity of the hippocampus. For reviews, see [13, 83, 129, 169].
(1) Water maze
This test requires the animal to locate and swim towards an invisible platform in a water tank. During learning, the mouse is supposed to build a “cognitive map” of the environment, a representation that enables the animal to locate the platform, regardless of where it enters the pool. Rodents with damage to the hippocampus are severely impaired. Almost all APP transgenic models have, to date, been screened in the water maze task. The majority of these studies indicate defects in navigation behavior. The transgenic mice reach the goal later after having traveled a longer distance; they may have difficulties remembering the location of the platform when assessed during probe trials. These types of deficit, some of which exhibit very early onset [57, 310] have been observed in the PDAPP [53], Tg2576 [137, 329], APP23 [163, 181, 310], TgCRND8 [57], and crossed APP/PS1 [198] models. It is important to keep in mind, however, that some reports have failed to demonstrate significant or robust learning and retention deficits in the water maze task [132, 164, 166] in both APP and APP/PS1 transgenic mice. The reasons for such discrepancies are still unclear.
(2) Spatial alternation
The rodents have a natural propensity to alternate their visits from already-experienced locations to new ones. This behavior, that can either be analyzed spontaneously or conditioned by an explicit reinforced alternation rule, requires intact working memory abilities. Lesions of the hippocampus but also of the frontal cortex disrupt spatial alternation [180]. Spontaneous or reinforced spatial alternation has been extensively studied in the Tg2576 model, with several reports indicating decreased performances ([51, 65, 131, 137, 182, 237]; see however, [166] for mixed results). The deficit is said to be detectable at an early age before overt Aβ deposition, and to increase with age. The deficits were questionable in female APP23 mice [181]. Additional reports have illustrated reduced spatial alternation in double APPxPS1 transgenic mice ([131, 132, 333]; see, however, [197]).
(3) Object recognition
Visual recognition memory is also sensitive to hippocampal dysfuntion. Objects are shown to the mouse during an acquisition phase. Following a variable delay (from minutes to several hours), the mouse is placed back in the test arena, which now contains both familiar (previously shown) objects and new ones. The natural tendency of rodents is to explore the new objects (novelty attraction). Good performance in this test relies on the hippocampus, the perirhinal and entorhinal cortices, and on their interconnection. Impaired recognition memory has been demonstrated in both APP [77] and APPxPS1 transgenic mice [135]. As mentioned earlier, the knocking-out of PS1 did not rescue the cognitive deficit in the APP mouse [77]. Conflicting results have been obtained concerning the object recognition task in the PDAPP mice (deficit [85] which is possibly corrected by immunotherapy [82]; absence of deficit [53]).
(4) Sparing of “procedural memory”
The dichotomy between procedural memory (based on the acquisition of skills or of a sequence of procedures), which is relatively spared in AD, and declarative memory, which is affected at the initial stage, cannot be directly applied to animals. Some efforts have been made to test the ability to follow procedures in a stereotyped manner and to contrast it with the ability to build cognitive maps. The APP Tg mice are still able to apply at least some procedural strategies [85, 139], especially when given a choice between multiple strategies to solve problems [24, 219], thus suggesting selective alterations of different memory systems in these mice (sparing of procedural memory, while relational “declarative-like” memories are affected).
Is extracellular accumulation of Aβ peptide the cause of the deficit?
An inverse correlation between cognitive deficit and amyloid accumulation has been reported in several studies involving singly transgenic APP mice (e.g., [53, 84]) and doubly transgenic mice (e.g., [110, 267]). The good correlation between the areas where Aβ peptide accumulates and the type of cognitive deficit, and the efficiency of the immunotherapy in terms of the amyloid load and the behavioral symptoms also favor the hypothesis of a direct toxic effect of amyloid. However, some discrepancies are poorly compatible with this hypothesis: in some cases, the deficit is detectable without Aβ accumulation [131, 310]; sometimes it is observed after the Aβ accumulation has taken place [135]; while at other times there is no deficit despite a severe amyloid load [23, 24]. Cheng et al. [55], while working on mice bearing the Arctic mutation that alters the sequence of the Aβ peptide and makes it more prone to precipitate in fibrillar form (without altering the ratio Aβ42/Aβ40), demonstrated a striking dissociation between plaque formation and functional deficits. ARC6 mice had more plaques than J20 mice but essentially no behavioral deficits. Furthermore, ARC48 mice had markedly greater plaque loads than J20 mice but comparable or less severe functional deficits. This set of results, from different mouse lines, suggests that it is not the fibrillar Aβ peptide sequestred in the plaque that is responsible for the cognitive deficit, but rather some other diffusible Aβ species [329], or, as suggested more recently, intracellular Aβ peptide.
Pathogenicity of intracellular Aβ
In the previous section (“Intracellular Aβ peptide”) we mentioned the controversy over the role of intracellular Aβ peptide in the cascade of the pathogenetic events leading to neuronal dysfunction. Intracellular Aβ peptide has also been considered to be directly responsible for the clinical signs: in the 3×Tg-AD mouse, synaptic dysfunction is detected before the development of Aβ extracellular deposits and of NFTs, but in correlation with intracellular Aβ accumulation [233]. The deficit in long-term memory also appeared to be correlated with the accumulation of intracellular Aβ. Immunotherapy rescued the deficit and was associated with the clearance of intracellular Aβ that reappeared with the cognitive deficit when the effects of the immunotherapy waned [22]. However, since the density of neurons containing intracellular Aβ decreases with age, while cognitive deficits increase, intracellular Aβ cannot be the unique or even the crucial factor responsible for the neuronal dysfunction.
Pathogenicity of oligomers
Since insoluble fibrillar Aβ peptides do not diffuse and are thus unable to play a pathogenetic role, except by direct contiguity, other Aβ compounds that can be active at some distance from the plaques have been looked for. As already alluded to, Aβ peptides easily form dimers, trimers and, in general, oligomers that pre-exist in protofibrillar and aggregated Aβ deposits. In recent years, oligomers have repeatedly been found to play an important pathogenetic role, particularly in synapses (see above)—for a review see [322]. In several studies the presence of oligomers is thought to be necessary to explain the experimental observations. The total amount of cerebral Aβ, for instance, was not significantly altered by Aβ immunization, although cognitive dysfunction was improved in a TgCRND8 murine model of Alzheimer disease, suggesting that the antibodies acted on soluble Aβ species [155]. Dodart et al. [82] injected a monoclonal m266 anti-Aβ antibody into PDAPP mice. The memory deficits were reversed in less than 24 h by a single intraperitoneal injection (which could not modify amyloid burden). The antibodies were supposed to act directly on the oligomers.
In the Tg2576 mouse line, deficits in spatial alternation (Y-maze) were noticed at seven months of age, before Aβ deposits were seen in the brain, but at a time when the levels of soluble Aβ 40/42 were already elevated [237]. The memory loss detected at around six months coincided with the appearance of detergent-insoluble Aβ aggregates, but the inverse correlation between the aggregation of insoluble Aβ and memory was lost when age was taken into account. The authors concluded that the insoluble Aβ was a surrogate marker for small assemblies of Aβ peptide that disrupted cognition and occurred as intermediates during the formation of aggregates [329]. In the same mouse line, dimeric Aβ peptide was shown to accumulate in lipid rafts of cell membranes at six months of age, when the first memory alterations are observed. At that stage, Aβ dimers are fully soluble in SDS [162]. Lesné et al. looked for an Aβ species whose accumulation corresponded to the time course of the decline in spatial reference memory (appearing at six months and remaining stable for 7–8 months thereafter), again in the Tg2576 mouse line. They found that Aβ peptide forms stable molecular assemblies that are preferentially made of trimers. The dodecamers (four trimers) of molecular weight 56 (termed Aβ*56) were the best correlates of the memory deficit and the most likely candidates for the toxic species responsible for the memory deficit [192]. A direct test of the hypothesis of the Aβ-oligomers was achieved by injecting the conditioned medium of a cell culture producing large amounts of Aβ peptides and particularly of oligomers into the lateral ventricle of rats that had learned an alternation task. This injection caused a deficit in the learned task that was “rapid, potent and transient” [60].
The transgenic models of neurofibrillary pathology
The first part of this review was centered on Aβ pathology. Only dystrophic neurites of the corona of the plaque contain hyperphosphorylated tau epitopes; paired helical filaments are remarkably absent from these models. The neurofibrillary, tau part of the pathology is thus practically lacking in the Tg mice that we have considered up to now.
Normal and mutated tau transgene
Tau is a phosphoprotein that belongs to the family of the microtubule-associated proteins; it binds to tubulin and facilitates tubule polymerization [61]. It has an axonal subcellular localization in the normal adult brain. When phosphorylated it is detached from tubulin which depolymerizes—this depolymerization favors axonal growth and plasticity. Six isoforms of the protein are known [107], which differ in the presence or absence of exons 2, 3, or 10. An alternative splicing of exon 10 produces either tau with four repetitive motives (4R tau) or tau with only 3 (3R tau) [107]. Hyperphosphorylated tau is the main constituent of NFT of AD, which contains both 3R and 4R tau. The NFTs of progressive supranuclear palsy and corticobasal degeneration are principally or exclusively made of 4R tau [276], while Pick body contains exclusively or preferentially 3R tau [39, 40]. The presence of tau immunoreactivity in a somatodendritic distribution in the absence of true NFT defines the “pretangle” [17]. A somatodendritic distribution of tau is also found in argyrophilic grain disease. The subcellular distribution of tau (axonal or somatodendritic) depends on the distribution of its mRNA, not on signals included in the protein sequence [19]. No change in tau expression has been detected in AD, but intronic and exonic mutations of the tau gene are known to be the cause of frontotemporal dementia linked to chromosome 17 (FTDP-17).
The physiology of tau protein is different in adult mice and adult humans. Mouse brain contains the 4R tau isoforms exclusively, whereas levels of 3R and 4R are approximately equal in normal adult human brain. Although mouse and human tau sequences are similar, there are 14 amino acid differences in the N-terminal region [8].
The normal shortest 3R tau isoform (3R tau without N-terminal insert) has been introduced into the mouse genome under the promoter of the murine 3-hydroxy-methyl-glutaryl CoA reductase gene [37]. Tau immunoreactivity was present in the somatodendritic compartment. Several epitopes known to be phosphorylated in AD were also phosphorylated, but there were no NFTs. The shortest tau isoform was also expressed under a murine prion promoter [147]. Insoluble, hyperphosphorylated tau inclusions were present in cortical and brainstem neurons but were mostly abundant in spinal cord neurons. There were no paired helical filaments at electron microscopy. Lines expressing the longest four-repeat tau isoform under the murine thy-1 promoter (ALZ7 line) [112] developed a peripheral and central axonopathy [247, 288]. Dilated axons, spheroids, and pretangles were observed without true tangle formation.
Another approach consisted of expressing human genomic tau contained in P1-derived artificial chromosomes (PAC). In line 8c, a PAC containing all 14 exons, exon −1, and more than 7 kb of the 5’ flanking region, which includes the tau promoter, was overexpressed in mice. Tau was distributed in neurites and at synapses, but was absent from cell bodies. There were no significant pathological changes, while axonal spheroids and somatodendritic distributions were observed in mice overexpressing 4R cDNA [90]. Htau mice were obtained by crossing tau knock-out mice with 8c mice [8]. Neither tau knock-out mice nor 8c mice develop any evidence of tau pathology. Htau mice exclusively express the six normal human tau isoforms (without murine tau), the level of the 3R isoforms being significantly higher than that of the 4R isoform [8]. NFTs and extensive cell death were seen in the htau mice, although they express lower levels of human tau than the c8 mice [8]. This suggests that wild-type murine tau prevents the aggregation of overexpressed human tau. Cell death in htau mice does not seem to be directly caused by the NFTs but appears to be linked to reexpression of proteins involved in cell-cycle and DNA synthesis [7]. NFTs were observed at a young age in mouse lines in which the P301L mutation was introduced [111, 196] or the V337M mutation [296]. Nonapoptotic cell death and tau filaments were observed in transgenic mice with the P301S mutation of tau protein [3]. The expression of human four-repeat tau with G272V and P301S mutations under a Thy1.2-promoter induced neurofibrillary pathology in the brain with severe cognitive alteration and no sensorimotor deficit [270].
In conclusion, PHF and NFT are usually not observed when any form of wild-type human tau is expressed, except in the model developed by Andorfer et al. [8] in which mouse tau gene is knocked-out. In almost all of the models where cDNA wild-type tau is expressed, the distribution of tau is somatodendritic; only the construction of Duff et al. [90] using a minigene preserves a normal subcellular distribution of tau. Overexpression of mutated tau regularly produces NFT.
Interaction between tau and Aβ accumulation
The influence of Aβ hyperproduction on the neurofibrillary pathology was studied in different ways: injection of amyloid Aβ42 fibrils into the brains of P301L mutant tau transgenic mice caused a fivefold increase in the numbers of NFTs in cell bodies within the amygdala, from where neurons project to the injection sites [111]. In P301L mutant tau mice crossed with APP Tg2576 transgenic mice, the amyloid deposits occurred at the same age as in the Tg2576 simple transgenic progenitor, but the neurofibrillary pathology was substantially enhanced in the limbic system and olfactory cortex, suggesting a synergy between the two pathologies [195].
On the other hand, reducing endogenous tau ameliorates or even completely rescues amyloid beta-induced deficits (the hAPP Tau −/− mice had better results on cognitive test than hAPP Tau +/−, which, in turn, had better results than hAPP Tau +/+ mice). The presence of tau protein was also necessary to produce experimental excitotoxic lesions produced by the GABAA receptor antagonist pentylenetetrazole [256].
The triply transgenic tau model expressing 3R tau (without mutation), APP with the Swedish and the London mutation and PS1 with the M146L mutation, did not develop true NFTs; however, the human tau transgene and hyperphosphorylated tau epitopes were found in the neuritic component of the plaque [32].
Oddo et al., instead of crossing single transgenic mice, simultaneously injected a P301L mutant tau transgene and an APP transgene bearing the Swedish mutation, both under a Thy 1.2 murine promoter, into single-cell embryos from mutant homozygous PS1M146V knock-in mice. The two transgenes appeared to cointegrate at the same locus. These triple transgenic mice (=3×Tg-AD mice) finally bear a mutated knocked-in PS1 gene, as well as a mutated APP and a mutated tau gene. At the first stage, Aβ peptide accumulates intracellularly. Aβ then precipitates in the extracellular space. Intracellular tau accumulation is finally observed. As in the human, Aβ accumulation is first seen in the isocortex, while tau pathology first appears in the limbic system [233]. The electrophysiological alterations (most noticeably, the deficit in LTP) are seen before extracellular accumulation of Aβ peptide at a time when intracellular accumulation of Aβ is already seen. Moreover, the injection of antibodies directed against Aβ peptide first cleans the extracellular deposits before inducing the disappearance of intracellular accumulation [234]. Normalization of the electrophysiological alterations is correlated with the disappearance of intracellular Aβ peptide [233]. Increased tau levels and hyperphosphorylation have no effect on the onset and progression of Aβ pathology [232]. However, the cognitive deficit does not only appear to be linked with Aβ peptide; soluble tau species are also reduced after active and passive immunization and could be involved in the cognitive improvement caused by immunotherapy [235].
What is the physiological relevance of a triple transgenic mouse to explain sporadic AD or even familial AD (FAD), which has never been found to be associated with a tau gene mutation? It is clear that no human disease is provoked by a triple mutation on the PS1, APP and tau genes. The model can therefore not be considered to describe the cause of AD, and particularly of sporadic AD (C0). However, for the first time it integrates all of the lesions that have been described in the human (L1) in a topography that, in several ways, resembles the distribution of the lesions seen in man (S1). This model may therefore be considered, in our view, to belong to the S1L1C0 type. It is probably too early to draw from this model the conclusion that Aβ peptide deposition should precede tau pathology (it does in the model; this does not warrant that it occurs in this way in the human). In the same way, the conclusion that intracellular Aβ is crucial to human pathogenesis because intracellular Aβ is the best correlate of the electrophysiological signs in this triple transgenic model cannot be drawn, in our view, without a further and careful analysis of intracellular Aβ in man.
Persistence of the pathology in conditional KO mice
To analyze the mechanism of progression of the NFT, mice expressing a repressible human tau variant (rTg4510) were generated. The responder transgene consisted of a tetracycline operon-responsive element placed upstream of a cDNA encoding human tau with four microtubule binding repeats (4R tau) and the P301L mutation. Doxycycline, when introduced into the food and water, suppresses transgene expression. Before doxycycline administration, the mice developed progressive age-related NFTs, neuronal loss, and behavioral impairments; when the expression of human tau was repressed, the cognitive deficit recovered and the neuronal loss remained stable but the number of NFTs continued to increase. This observation suggested that, not unlike what was observed in Aβ pathology, the toxic effect of tau was not linked to the visible lesions (i.e., NFTs) but to another tau species, the production of which was prevented by the repression of the tau gene [266]. These tau assemblies appear to be, just as in Aβ pathology, multimers [21]. The toxic tau multimers of 140 and 170 kDa probably contain full-length tau [21]. The progression of NFT despite the silencing of the mutated tau gene could indicate that NFTs, once present in the human brain, will progress even if a putative treatment is targeted at their cause.
Modulation of APP transgene
The effects of overexpressing or knocking out various known or supposed modulators of Aβ secretion have been studied in the literature.
Modulation of Aβ secretion by APOE
Apolipoprotein E (ApoE) is a protein involved in cholesterol transport. Its main receptor, the low-density lipoprotein receptor-related protein (LRP), is widely expressed in the central nervous system. Moreover, ApoE [229, 305, 306] and LRP [10] appear to be bound with Aβ in a large subset of senile plaques. Much was expected of studies using Tg mice to elucidate the role of ApoE; the risk of developing AD is indeed increased in people bearing the epsilon 4 allele [291]. Actually, the expression of the various isoforms of human ApoE in Tg mice and the knock-out of the ApoE gene in the mouse brought conflicting results and somehow increased the complexity of the problem.
Effects on Aβ deposition
A comparative study of the time courses of Aβ42, Aβ40, and ApoE deposition in relation to astrogliosis in Tg2576 suggested that Aβ42 preceded ApoE in the plaque, followed by Aβ40, which occupied the center of the deposit in later stages. Moreover, the presence of ApoE was correlated with the astrogliosis [297]. The Aβ deposits were compared in heterozygous V717F APP Tg mice (APPV717F+/−) with graded expression of the mouse ApoE gene. The mice carried no (ApoE −/−), one (ApoE +/−) or two (ApoE +/+) alleles. Amyloid deposits as well as Aβ immunoreactivity were lacking in the cortex in the absence of ApoE expression in animals aged 22 months. Aβ deposition was observed—although at a lower level than in the ApoE +/+ mice—when only one allele (ApoE +/−) was present. ApoE immunoreactivity was found in all of the thioflavin S positive amyloid cores in the Tg mice with one or two ApoE alleles [15]. In a later study with homozygous V717F APP Tg mice (APPV717F+/+) on an ApoE null background, it was found that the cortical and dentate gyrus deposition of Aβ was dramatically reduced, but that the densities of the CA1 and CA3 diffuse deposits were increased even when there was no thioflavin S positive deposits [144]. The overexpression of ApoE4 in a hAPP mouse, knocked out for ApoE, increases the number of focal, amyloid deposits tenfold in comparison with the ApoE3 mice [133]. Since the dystrophic neurites that are found in the coronae of the plaques are only observed when the deposit is focal with amyloid, it is no wonder that no “neuritic plaques” are found in the ApoE −/− mice. The role of ApoE itself in the neuritic degeneration is discussed [133]. In heterozygous V717F APP Tg mice, Aβ deposition was compared in mice expressing no ApoE, murine ApoE, or the various human ApoE isoforms (ApoE2, E3, and E4). As previously shown, ApoE was not necessary but it enhanced the formation of fibrillar Aβ. Murine ApoE was the most efficient, then human ApoE4, E3 and E2. In other words, as in man, ApoE2 and ApoE3 delayed the formation of amyloid deposits when compared to murine ApoE and human ApoE4 [94]. In Tg mice bearing one allele of the Swedish mutation (APP sw+/−), the expression of the human ApoE4 (ApoE4+/−) (under the human transferrin promoter) accelerated Aβ deposition and amyloid formation [47]. However, in another study, the overexpression of human ApoE4 under a murine prion protein promoter (responsible for neuronal and glial expression) did not modify the amount and progression of Aβ deposition in Tg mice expressing human APPswe or APPswe and PS1 with the deletion of exon 9 [193]. Van Dooren et al. compared the effects of expressing human ApoE4 in neurons (thy1 gene promoter) or in glia (GFAP gene promoter) in hAPP V717I singly transgenic and APP-V717I × PS1-A246E doubly transgenic mice (thy1 gene promoter for both transgenes). All of the mice were female and hemizygous for the transgene. The thy1 gene promoter construct is practically unexpressed in the thalamus. The presence of the human ApoE4 allele had a differential effect on cortex and thalamus, which also depended on its production cells (neuronal or glial): in the cortex, neuronal ApoE4 increased the number of diffuse deposits of Aβ, while in the thalamus, the density of both diffuse and focal deposits increased with neuronal and with glial ApoE. Neuronal ApoE promoted cortical amyloid angiopathy, while both neuronal and glial ApoE had a similar effect on the thalamus. ApoE did not influence APP processing and was not associated with tau hyperphosphorylation (probably because the ApoE transgene was hemizygous) [314]. Since APP was not produced in the thalamus in these constructs, the accumulation of diffuse or focal Aβ in this topography was related to its migration.
Effects on tau
ApoE could have more widespread effects than suspected. Neuronal but not glial expression of ApoE4 resulted in hyperphosphorylation of protein tau and caused prominent axonopathy by disrupting axonal transport [299, 300]. In various transgenic lines in which human ApoE3 or ApoE4 was expressed under a GFAP or a neuron-specific enolase (NSE) promoter, C-terminal fragments of ApoE4 (and to a lesser degree of ApoE3) accumulated, and tau protein appeared to be hyperphosphorylated only in the NSE-ApoE Tg mice [34].
Effects on synapses
Buttini et al. found in hAPP mice that synaptophysin-immunoreactive presynaptic terminals, choline acetyltransferase (ChAT) activity, and ChAT-positive fibers were reduced in old apoE-deficient transgenic mice expressing human APP. This effect was prevented by the expression of the ApoE3 allele [41].
Conclusions
The effect of ApoE on Aβ metabolism and deposition is still controversial. The presence of murine or human ApoE does not directly modify the metabolism of APP, but increases the number of focal deposits, the number of their surrounding dystrophic neurites, and the level of vascular angiopathy. It could also be involved in the transport of Aβ, since lesions are seen in the thalamus under conditions in which Aβ is not produced by the thalamic neurons. The effects on the phosphorylation of tau are intriguing: they could provide a link between Aβ and tau alterations; alternatively, as tau hyperphosphorylation is only found when the neuronal expression of ApoE is high, they could be related to side effects of the transgenesis. The importance of ApoE to the trophicity of some synapses appears to be more firmly established, since it is revealed by knocking out the murine gene. Strangely enough, whereas ApoE is known to be mainly produced by glia, most of the effects are found with a neuronal expression [9], and this should prompt a re-evaluation of neuronal ApoE in human pathology.
Modulation of Aβ deposition by other proteins involved in cholesterol metabolism: liver X receptor, LRP and ABCA1
Besides the essential role of ApoE in Aβ deposition, a number of data suggest a link between cholesterol metabolism and AD pathology. In APP Tg mice (PSAPP line = TG2576 × PS1M146V), dietary cholesterol seems to accelerate Aβ deposition, whereas cholesterol-lowering drugs lower it [252, 253]. Inhibition of acyl-coenzyme A cholesterol acyltransferase (ACAT), an enzyme that controls the equilibrium between free cholesterol and cholesteryl esters, was shown to reduce amyloid pathology [143].
The liver X receptor (LXR) regulates cholesterol metabolism and also plays a role in inflammation: it inhibits the expression of genes involved in inflammation but promotes the phagocytosis of Aβ by microglia. Deletion of either LXRα or LXRβ in APPswe/PS1deltaE9 transgenic mice resulted in increased amyloid plaque load [349].
LRP is an endocytotic cell-surface receptor that is abundant in neurons (cell body and dendrites). It allows the internalization of several ligands such as ApoE, APP (with the Kunitz inhibitor) and α2-macroglobulin. LRP knock-out mice are not viable. van Uden et al. used mice deficient in receptor-associated protein (RAP) to reduce the level of LRP by 80%. They were crossed with the hAPP line J9. The amount of amyloid deposits was doubled on the RAP −/− background, while APP processing was not altered, suggesting that LRP does indeed help to clear Aβ42 [316]. On the other hand, overexpression of a functional mini LRP receptor (LRP2) in PDAPP mice produced a decrease in cerebal ApoE, a moderate but significant increase in insoluble, detergent soluble (probably membrane-bound) Aβ42, and a decrease in total Aβ in the CSF. The decrease in the ApoE level is explained by an accelerated internalization and degradation of ApoE when LRP is overexpressed. The effect on Aβ42 is abolished in ApoE −/− mice, suggesting that it is mediated through the binding of Aβ42 to ApoE. In cell culture, the cells overexpressing LRP2 clear the Aβ42 present in the culture medium more rapidly [350].
ABCA1 (ATP-binding cassette transporter A1) is a major regulator of cholesterol efflux and high-density lipoprotein (HDL) metabolism. The mutation of ABCA1 in the human causes severe hypercholesterolemia and marked deficits of high-density lipoprotein (HDL) and apoA-I. The level of ApoE is low in the brains of these patients. In APP23 Tg mice knocked out for ABCA1, the density of Aβ and Congo red positive deposits is increased. The amyloid angiopathy is more severe and associated with microhemorrhages. The level of soluble ApoE is decreased in the brain [171].
Modulation of Aβ secretion by α-synuclein
Lewy and AD pathologies are often associated in the human and could have a synergistic effect. On the other hand, some rare cases of familial Parkinson disease are linked to mutations on the α-synuclein gene. α-Synuclein-positive neurites have been mentioned in the aged TG2576 (APPswe) transgenic line [347]. Such a pathology in a mouse line without any known alteration of α-synuclein already hints at cooperation between amyloid and Lewy pathology. The human wild-type or mutated (A53T) α-synuclein gene has been expressed in mice under the control of the mouse Thy1 regulatory sequence [312]. Similar pathological changes were observed in the two mouse lines. The protein accumulated in the neurons and caused their degeneration. However, for unknown reasons, the pathology involved unexpected areas: brainstem neurons and motor neurons of the spinal cord appeared particularly vulnerable. There was no expression of the transgenes in the substantia nigra pars compacta. In other mouse lines in which the wild-type or the mutated α-synuclein gene was driven by the promoter of the tyrosine-hydroxylase [210] no degeneration was observed in the substantia nigra despite a high level of expression. Overexpression of wild-type and mutated α-synuclein in cultures of dopaminergic neurons, however, caused significant cell death. Cytoplasmic inclusions were observed only in the cultures where the mutant gene had been transfected.
Accumulation of α-synuclein occurred earlier in bigenic mice, hAPP (line J9) × wild-type α-synuclein. Some inclusions appeared fibrillar in the doubly transgenic animals, whereas they were always amorphous in the singly transgenic animals [206].
In conclusion, the effects of α-synuclein remain controversial: several reports indicate that even the wild-type form of the human protein may induce pathological changes. It is however surprising that, in contrast to what is observed in the human, the dopaminergic system appears resistant. Although still not well explained, α-synuclein and APP seem to interact in the transgenic lines just as they do in the human.
Modulation of the pathology by other proteins
Numerous doubly or triply transgenic lines (only some listed here) have been generated to elucidate the influence of a candidate protein on the secretion of Aβ peptide or on the pathology that it generates.
Transthyretin
Transthyretin (TTR) is a serum protein that precipitates in autosomal dominant familial amyloidotic polyneuropathy, in familial amyloidotic cardiomyopathy, and in sporadic senile systemic amyloidosis. It is also said to complex Aβ peptide that is physiologically present in the CSF of controls and of patients and could prevent amyloid formation [273]. Mouse strains transgenic for either wild-type or mutant (TTR L55P) human TTR genes have been produced and develop TTR deposits in heart and kidney, only some of which are congophilic. Hemizygous deletion of its gene favors Aβ deposition in APPswe/PS1deltaE9 mice [58].
Oxidative damage
The homozygous deletion of the superoxide dismutase 2 (SOD2), a mitochondrial enzyme implicated in the protection against oxidative damage, worsened the cognitive deficit and decreased the microtubule-associated protein 2 (MAP2) immunoreactivity, a sign of dendritic loss. Paradoxically, it lowered the density of Aβ deposits but increased amyloid angiopathy [93].
Fyn
Fyn, a tyrosine-kinase that is altered in AD brains, is located in the postsynaptic density of glutamatergic neurons. It could be involved in the signal transduction responsible for the toxic effect of Aβ on synapses. When overexpressed in hAPP mice lines J9 and J20, it induced impaired spatial memory retention and altered emotional behavior. It also caused changes in the expression of proteins, such as Fos and calbindin [56].
Modulation of the pathology by activity
The effects of environmental enrichment on Aβ deposition are contradictory. It was initially found to improve cognitive function but to exacerbate amyloid plaque formation in APPswe/PS1dE9 mice [150, 151]. In a later study, increasing cognitive, social, or physical activities protected the Tg mice from the cognitive impairment without affecting amyloid deposition [11]. Physical activity (running wheel: [1]) as well as an enriched environment [5] was found to reduce Aβ levels in the TgCRND8 line, while another study did not find any significant effect on Aβ deposition in the APP-23 mice [339]. In yet another study involving doubly transgenic mice TG2576 × PS1M671L, “complete” environmental enrichment (i.e., in terms of cognitive, social and physical activities) was shown to significantly reduce the amyloid load (−28% in hippocampus and −36 in entorhinal cortex). The contradictory results in the literature suggest that the effects of environmental enrichment and physical activity are related to additional, badly controlled factors. Recently, it has been suggested that the ApoE allele could play a role, since environmental enrichment stimulated apoptosis when the human ApoE4 was expressed on a murine ApoE deficient background, while it stimulated neurogenesis in ApoE3 mice [194].
Trauma
Repetitive mild traumatic injury of the brain increased the deposition of Aβ peptide in the Tg2576 mouse model. Single brain trauma had no effect [308].
Conclusions
The transgenic technology has, for the first time, allowed the production of some of the lesions observed in human neurodegenerative diseases. Its success proves, a contrario, how weak the other methods based on the use of destruction, toxic agents or observations of naturally occurring animal diseases were.
We have repeatedly seen in this review that the conclusion that may be drawn from a model depends on the joined analysis of the transgenic line and of the human disease. The renewed analysis of the lesions in the animal enlightens our view on the human pathology; ignorance of the human pathology will undoubtedly lead to erroneous interpretation. This crossed examination implies a double competence—in both human and animal pathology. The neuropathologist is a key scientist in the exploration of these new territories.
References
Adlard P, Perreau V, Pop V, Cotman CW (2005) Voluntary exercise decreases amyloid load in a transgenic model of Alzheimer’s disease. J Neurosci Res 25:4217–4221
Akiyama H, Barger S, Barnum S, Bradt B, Bauer J, Cole GM, Cooper NR, Eikelenboom P, Emmerling M, Fiebich BL, Finch CE, Frautschy S, Griffin WS, Hampel H, Hull M, Landreth G, Lue L, Mrak R, Mackenzie IR, McGeer PL, O’Banion MK, Pachter J, Pasinetti G, Plata-Salaman C, Rogers J, Rydel R, Shen Y, Streit W, Strohmeyer R, Tooyoma I, Van Muiswinkel FL, Veerhuis R, Walker D, Webster S, Wegrzyniak B, Wenk G, Wyss-Coray T (2000) Inflammation and Alzheimer’s disease. Neurobiol Aging 21:383–421
Allen B, Ingram E, Takao M, Smith MJ, Jakes R, Virdee K, Yoshida H, Holzer M, Craxton M, Emson PC, Atzori C, Migheli A, Crowther RA, Ghetti B, Spillantini MG, Goedert M (2002) Abundant tau filaments and nonapoptotic neurodegeneration in transgenic mice expressing human P301S tau protein. J Neurosci 22:9340–9351
Alzheimer’s disease collaborative group, Clark RP, Hutton M, Fuldner RA, Froelich S, Karran B, Talbot C, Crook R, Lendon C, Prihar G, He C, Korenblat K, Martinez A, Wragg M, Busfield F, Behrens MI, Myers A, Norton J, Morris J, Mehta N, Pearson C, Lincoln S, Baker M, Duff K, Zehr C, Perez-Tur J, Houlden H, Ruiz A, Ossa J, Lopera F, Arcos M, Madrigal M, Collinge J, Humphreys C, Ashworth T, Sarner S, Fox N, Harvey R, Kennedy A, Roques P, Cline RT, Philips L, Venter JC, Forsell L, Axelman K, Lilius L, Johnston J, Cowburn R, Vitanen N, Winblad D, Kosik K, Haltia M, Poyhonen M, Dickson D, Mann D, Neary D, Snowden J, Lantos P, Lannfeld L, Rossor M, Roberts GW, Adams MD, Hardy J, Goate A (1995) The structure of the Presenilin 1 (S182) gene and identification of six novel mutations in early onset AD families. Nat Genet 11:219–222
Ambree O, Leimer U, Herring A, Gortz N, Sachser N, Heneka MT, Paulus W, Keyvani K (2006) Reduction of amyloid angiopathy and Abeta plaque burden after enriched housing in TgCRND8 mice: involvement of multiple pathways. Am J Pathol 169:544–552
Ancolio K, Dumanchin C, Barelli H, Warter JM, Brice A, Campion D, Frebourg T, Checler F (1999) Unusual phenotypic alteration of beta amyloid precursor protein (betaAPP) maturation by a new Val-715 → Met betaAPP-770 mutation responsible for probable early-onset Alzheimer’s disease. Proc Natl Acad Sci USA 96:4119–4124
Andorfer C, Acker CM, Kress Y, Hof PR, Duff K, Davies P (2005) Cell-cycle re-entry and cell death in transgenic mice expressing nonmutant human tau isoforms. J Neurosci 25:5446–5454
Andorfer C, Kress Y, Espinoza M, de Silva R, Tucker KL, Barde YA, Duff K, Davies P (2003) Hyperphosphorylation and aggregation of tau in mice expressing normal human tau isoforms. J Neurochem 86:582–590
Aoki K, Uchihara T, Sanjo N, Nakamura A, Ikeda K, Tsuchiya K, Wakayama Y (2003) Increased expression of neuronal apolipoprotein E in human brain with cerebral infarction. Stroke 34:875–880
Arelin K, Kinoshita A, Whelan CM, Irizarry MC, Rebeck GW, Strickland DK, Hyman BT (2002) LRP and senile plaques in Alzheimer’s disease: colocalization with apolipoprotein E and with activated astrocytes. Mol Brain Res 104:38–46
Arendash G, Garcia M, Costa D, Cracchiolo J, Wefes I, Potter H (2004) Environmental enrichment improves cognition in aged Alzheimer’s transgenic mice despite stable beta-amyloid deposition. NeuroReport 15:1751–1754
Arendash GW, King DL, Gordon MN, Morgan D, Hatcher JM, Hope CE, Diamond DM (2001) Progressive, age-related behavioral impairments in transgenic mice carrying both mutant amyloid precursor protein and presenilin-1 transgenes. Brain Res 891:42–53
Ashe KH (2001) Learning and memory in transgenic mice modeling Alzheimer’s disease. Learn Mem 8:301–308
Bacskai BJ, Kajdasz ST, Christie RH, Carter C, Games D, Seubert P, Schenk D, Hyman BT (2001) Imaging of amyloid-beta deposits in brains of living mice permits direct observation of clearance of plaques with immunotherapy. Nat Med 7:369–372
Bales KR, Verina T, Cummins DJ, Du Y, Dodel RC, Saura J, Fishman CE, DeLong CA, Piccardo P, Petegnief V, Ghetti B, Paul SM (1999) Apolipoprotein E is essential for amyloid deposition in the APP(V717F) transgenic mouse model of Alzheimer’s disease. Proc Natl Acad Sci USA 96:15233–15238
Ball M, Braak H, Coleman P, Dickson D, Duyckaerts C, Gambetti P, Hansen L, Hyman B, Jellinger K, Markesbery W, Perl D, Powers J, Price J, Trojanowski JQ, Wisniewski H, Phelps C, Khachaturian Z (1997) Consensus recommendations for the postmortem diagnosis of Alzheimer’s disease. Neurobiol Aging 18:S1–S2
Bancher C, Brunner C, Lassmann H, Budka H, Jellinger K, Wiche G, Seitelberger F, Grundke-Iqbal I, Iqbal K, Wisniewski HM (1989) Accumulation of abnormally phosphorylated tau precedes the formation of neurofibrillary tangles in Alzheimer’s disease. Brain Res 477:90–99
Bayer TA, Wirths O, Majtenyi K, Hartmann T, Multhaup G, Beyreuther K, Czech C (2001) Key factors in Alzheimer’s disease: beta-amyloid precursor protein processing, metabolism and intraneuronal transport. Brain Pathol 11:1–11
Behar L, Marx R, Sadot E, Barg J, Ginzburg I (1995) Cis-acting signals and trans-acting proteins are involved in tau mRNA targeting into neurites of differentiating neuronal cells. Int J Dev Neurosci 13:113–127
Benzing WC, Wujek JR, Ward EK, Shaffer D, Ashe KH, Younkin SG, Brunden KR (1999) Evidence for glial-mediated inflammation in aged APP(SW) transgenic mice. Neurobiol Aging 20:581–589
Berger Z, Roder H, Hanna A, Carlson A, Rangachari V, Yue M, Wszolek Z, Ashe K, Knight J, Dickson D, Andorfer C, Rosenberry TL, Lewis J, Hutton M, Janus C (2007) Accumulation of pathological Tau species and memory loss in a conditional model of tauopathy. J Neurosci 27:3650–3662
Billings LM, Oddo S, Green KN, McGaugh JL, Laferla FM (2005) Intraneuronal Abeta causes the onset of early Alzheimer’s disease-related cognitive deficits in transgenic mice. Neuron 45:675–688
Bizon J, Prescott S, Nicolle MM (2007) Intact spatial learning in adult Tg2576 mice. Neurobiol Aging 28:440–446
Blanchard J, Martel G, Guillou JL, Nogues X, Micheau J (2007) Impairment of spatial memory consolidation in APP(751SL) mice results in cue-guided response. Neurobiol Aging. doi:10.1016/j.neurobiolaging.2007.02.010
Blanchard V, Czech C, Bonici B, Clavel N, Gohin M, Dalet K, Revah F, Pradier L, Imperato A, Moussaoui S (1997) Immunohistochemical analysis of presenilin 2 expression in the mouse brain: distribution pattern and co-localization with presenilin 1 protein. Brain Res 758:209–217
Blanchard V, Moussaoui S, Czech C, Touchet N, Bonici B, Planche M, Canton T, Jedidi I, Gohin M, Wirths O, Bayer TA, Langui D, Duyckaerts C, Tremp G, Pradier L (2003) Time sequence of maturation of dystrophic neurites associated with Abeta deposits in APP/PS1 transgenic mice. Exp Neurol 184:247–263
Bodendorf U, Danner S, Fischer F, Stefani M, Sturchler-Pierrat C, Wiederhold KH, Staufenbiel M, Paganetti P (2002) Expression of human beta-secretase in the mouse brain increases the steady-state level of beta-amyloid. J Neurochem 80:799–806
Boncristiano S, Calhoun ME, Howard V, Bondolfi L, Kaeser SA, Wiederhold KH, Staufenbiel M, Jucker M (2005) Neocortical synaptic bouton number is maintained despite robust amyloid deposition in APP23 transgenic mice. Neurobiol Aging 26:607–613
Bondolfi L, Calhoun M, Ermini F, Kuhn HG, Wiederhold KH, Walker L, Staufenbiel M, Jucker M (2002) Amyloid-associated neuron loss and gliogenesis in the neocortex of amyloid precursor protein transgenic mice. J Neurosci 22:515–522
Borchelt DR, Ratovitski T, van Lare J, Lee MK, Gonzales V, Jenkins NA, Copeland NG, Price DL, Sisodia SS (1997) Accelerated amyloid deposition in the brains of transgenic mice coexpressing mutant presenilin 1 and amyloid precursor proteins. Neuron 19:939–945
Borchelt DR, Thinakaran G, Eckman CB, Lee MK, Davenport F, Ratovitsky T, Prada CM, Kim G, Seekins S, Yager D, Slunt HH, Wang R, Seeger M, Levey AI, Gandy SE, Copeland NG, Jenkins NA, Price DL, Younkin SG, Sisodia SS (1996) Familial Alzheimer’s disease-linked presenilin 1 variants elevate Abeta1–42/1–40 ratio in vitro and in vivo. Neuron 17:1005–1013
Boutajangout A, Authelet M, Blanchard V, Touchet N, Tremp G, Pradier L, Brion JP (2004) Characterisation of cytoskeletal abnormalities in mice transgenic for wild type human tau and familial Alzheimer’s disease mutants of APP and presenilin-1. Neurobiol Dis 15:47–60
Braak H, Braak E (1991) Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol (Berl) 82:239–259
Brecht WJ, Faith MH, Chang S, Tesseur I, Yu GQ, Xu Q, Fish JD, Wyss-Coray T, Buttini M, Mucke L, Mahley RW, Huang Y (2004) Neuron-specific apolipoprotein E4 proteolysis is associated with increased tau phosphorylation in brains of transgenic mice. J Neurosci 24:2527–2534
Brendza RP, Bacskai BJ, Cirrito JR, Simmons KA, Skoch JM, Klunk WE, Mathis CA, Bales KR, Paul SM, Hyman BT, Holtzman DM (2005) Anti-Abeta antibody treatment promotes the rapid recovery of amyloid-associated neuritic dystrophy in PDAPP transgenic mice. J Clin Invest 115:428–433
Brendza RP, O’Brien C, Simmons K, McKeel DW, Bales KR, Paul SM, Olney JW, Sanes JR, Holtzman DM (2003) PDAPP; YFP double transgenic mice: a tool to study amyloid-beta associated changes in axonal, dendritic, and synaptic structures. J Comp Neurol 456:375–383
Brion JP, Tremp G, Octave JN (1999) Transgenic expression of the shortest human tau affects its compartmentalization and its phosphorylation as in the pretangle stage of Alzheimer’s disease. Am J Pathol 154:255–270
Bronfman FC, Moechars D, Van Leuven F (2000) Acetylcholinesterase-positive fiber deafferentation and cell shrinkage in the septohippocampal pathway of aged amyloid precursor protein London mutant transgenic mice. Neurobiol Dis 7:152–168
Buée L, Delacourte A (1999) Comparative biochemistry of tau in progressive supranuclear palsy, corticobasal degeneration, FTDP-17 and Pick’s disease. Brain Pathol 9:681–693
Buée-Scherrer V, Hof PR, Buée L, Leveugle B, Vermersch P, Perl DP, Olanow CW, Delacourte A (1996) Hyperphosphorylated tau proteins differentiate corticobasal degeneration and Pick’s disease. Acta Neuropathol (Berl) 91:351–359
Buttini M, Yu GQ, Shockley K, Huang Y, Jones B, Masliah E, Mallory M, Yeo T, Longo FM, Mucke L (2002) Modulation of Alzheimer-like synaptic and cholinergic deficits in transgenic mice by human apolipoprotein E depends on isoform, aging, and overexpression of amyloid beta peptides but not on plaque formation. J Neurosci 22:10539–10548
Cai H, Wang Y, McCarthy D, Wen H, Borchelt DR, Price DL, Wong PC (2001) BACE1 is the major beta-secretase for generation of Abeta peptides by neurons. Nat Neurosci 4:233–234
Calhoun ME, Burgermeister P, Phinney AL, Stalder M, Tolnay M, Wiederhold KH, Abramowski D, Sturchler-Pierrat C, Sommer B, Staufenbiel M, Jucker M (1999) Neuronal overexpression of mutant amyloid precursor protein results in prominent deposition of cerebrovascular amyloid. Proc Natl Acad Sci USA 96:14088–14093
Calhoun ME, Wiederhold KH, Abramowski D, Phinney AL, Probst A, Sturchler-Pierrat C, Staufenbiel M, Sommer B, Jucker M (1998) Neuron loss in APP transgenic mice. Nature 395:755–756
Capetillo-Zarate E, Staufenbiel M, Abramowski D, Haass C, Escher A, Stadelmann C, Yamaguchi H, Wiestler OD, Thal DR (2006) Selective vulnerability of different types of commissural neurons for amyloid beta-protein-induced neurodegeneration in APP23 mice correlates with dendritic tree morphology. Brain 129:2992–3005
Carlson GA, Borchelt DR, Dake A, Turner S, Danielson V, Coffin JD, Eckman C, Meiners J, Nilsen SP, Younkin SG, Hsiao KK (1997) Genetic modification of the phenotypes produced by amyloid precursor protein overexpression in transgenic mice. Hum Mol Genet 6:1951–1959
Carter DB, Dunn E, McKinley DD, Stratman NC, Boyle TP, Kuiper SL, Oostveen JA, Weaver RJ, Boller JA, Gurney ME (2001) Human apolipoprotein E4 accelerates beta-amyloid deposition in APPsw transgenic mouse brain. Ann Neurol 50:468–475
Casas C, Sergeant N, Itier JM, Blanchard V, Wirths O, van der Kolk N, Vingtdeux V, van de Steeg E, Ret G, Canton T, Drobecq H, Clark A, Bonici B, Delacourte A, Benavides J, Schmitz C, Tremp G, Bayer TA, Benoit P, Pradier L (2004) Massive CA1/2 neuronal loss with intraneuronal and N-terminal truncated Abeta42 accumulation in a novel Alzheimer transgenic model. Am J Pathol 165:1289–1300
Cataldo AM, Petanceska S, Peterhoff CM, Terio NB, Epstein CJ, Villar A, Carlson EJ, Staufenbiel M, Nixon RA (2003) APP gene dosage modulates endosomal abnormalities of Alzheimer’s disease in a segmental trisomy 16 mouse model of down syndrome. J Neurosci 23:6788–6792
Cataldo AM, Peterhoff CM, Troncoso JC, Gomez-Isla T, Hyman BT, Nixon RA (2000) Endocytic pathway abnormalities precede amyloid beta deposition in sporadic Alzheimer’s disease and Down syndrome: differential effects of APOE genotype and presenilin mutations. Am J Pathol 157:277–286
Chapman PF, White GL, Jones MW, Cooper-Blacketer D, Marshall VJ, Irizarry M, Younkin L, Good MA, Bliss TV, Hyman BT, Younkin SG, Hsiao KK (1999) Impaired synaptic plasticity and learning in aged amyloid precursor protein transgenic mice. Nat Neurosci 2:271–276
Chartier-Harlin MC, Crawford F, Houlden H, Warren A, Hughes D, Fidani L, Goate A, Rossor M, Roques P, Hardy J, Mullan M (1991) Early-onset Alzheimer’s disease caused by mutations at codon 717 of the β-amyloid precursor protein gene. Nature 353:844–846
Chen G, Chen KS, Knox J, Inglis J, Bernard A, Martin SJ, Justice A, McConlogue L, Games D, Freedman SB, Morris RG (2000) A learning deficit related to age and beta-amyloid plaques in a mouse model of Alzheimer’s disease. Nature 408:975–979
Cheng IH, Palop JJ, Esposito LA, Bien-Ly N, Yan F, Mucke L (2004) Aggressive amyloidosis in mice expressing human amyloid peptides with the Arctic mutation. Nat Med 10:1190–1192
Cheng IH, Scearce-Levie K, Legleiter J, Palop JJ, Gerstein H, Bien-Ly N, Puolivali J, Lesne S, Ashe KH, Muchowski PJ, Mucke L (2007) Accelerating amyloid-beta fibrillization reduces oligomer levels and functional deficits in Alzheimer disease mouse models. J Biol Chem 282:23818–23828
Chin J, Palop JJ, Puolivali J, Massaro C, Bien-Ly N, Gerstein H, Scearce-Levie K, Masliah E, Mucke L (2005) Fyn kinase induces synaptic and cognitive impairments in a transgenic mouse model of Alzheimer’s disease. J Neurosci 25:9694–9703
Chishti MA, Yang DS, Janus C, Phinney AL, Horne P, Pearson J, Strome R, Zuker N, Loukides J, French J, Turner S, Lozza G, Grilli M, Kunicki S, Morissette C, Paquette J, Gervais F, Bergeron C, Fraser PE, Carlson GA, St George-Hyslop P, Westaway D (2001) Early-onset amyloid deposition and cognitive deficits in transgenic mice expressing a double mutant form of amyloid precursor protein 695. J Biol Chem 276:21562–21570
Choi SH, Leight SN, Lee VM, Li T, Wong PC, Johnson JA, Saraiva MJ, Sisodia SS (2007) Accelerated Abeta deposition in APPswe/PS1deltaE9 mice with hemizygous deletions of TTR (transthyretin). J Neurosci 27:7006–7010
Christie RH, Bacskai BJ, Zipfel WR, Williams RM, Kajdasz ST, Webb WW, Hyman BT (2001) Growth arrest of individual senile plaques in a model of Alzheimer’s disease observed by in vivo multiphoton microscopy. J Neurosci 21:858–864
Cleary JP, Walsh DM, Hofmeister JJ, Shankar GM, Kuskowski MA, Selkoe DJ, Ashe KH (2005) Natural oligomers of the amyloid-beta protein specifically disrupt cognitive function. Nat Neurosci 8:79–84
Cleveland DW, Hwo SY, Kirschner MW (1977) Purification of tau, a microtubule-associated protein that induces assembly of microtubules from purified tubulin. J Mol Biol 116:207–225
Colle MA, Hauw J-J, Crespeau F, Uchihara T, Akiyama H, Checler F, Pageat P, Duyckaerts C (2000) Vascular and parenchymal A beta deposition in the aging dog: correlation with behavior. Neurobiol Aging 21:695–704
Cook DG, Forman MS, Sung JC, Leight S, Kolson DL, Iwatsubo T, Lee VM, Doms RW (1997) Alzheimer’s A beta(1–42) is generated in the endoplasmic reticulum/intermediate compartment of NT2N cells. Nat Med 3:1021–1023
Cooper JD, Salehi A, Delcroix JD, Howe CL, Belichenko PV, Chua-Couzens J, Kilbridge JF, Carlson EJ, Epstein CJ, Mobley WC (2001) Failed retrograde transport of NGF in a mouse model of Down’s syndrome: reversal of cholinergic neurodegenerative phenotypes following NGF infusion. Proc Natl Acad Sci USA 98:10439–10444
Corcoran KA, Lu Y, Turner RS, Maren S (2002) Overexpression of hAPPswe impairs rewarded alternation and contextual fear conditioning in a transgenic mouse model of Alzheimer’s disease. Learn Mem 9:243–252
Cork LC, Powers RE, Selkoe DJ, Davies P, Geyer JJ, Price DL (1988) Neurofibrillary tangles and senile plaques in aged bears. J Neuropathol Exp Neurol 47:629–641
Crowther DC, Kinghorn KJ, Page R, Lomas DA (2004) Therapeutic targets from a Drosophila model of Alzheimer’s disease. Curr Opin Pharmacol 4:513–516
Cummings BJ, Satou T, Head E, Milgram NW, Cole GM, Savage MJ, Podlisny MB, Selkoe DJ, Siman R, Greenberg BD, Cotman CW (1996) Diffuse plaques contain C-terminal A beta 42 and not A beta 40: evidence from cats and dogs. Neurobiol Aging 17:653–659
Cummings BJ, Su JH, Cotman CW, White R, Russell MJ (1993) Beta-amyloid accumulation in aged canine brain: a model of early plaque formation in Alzheimer’s disease. Neurobiol Aging 14:547–560
D’Andrea MR, Nagele RG, Gumula NA, Reiser PA, Polkovitch DA, Hertzog BM, Andrade-Gordon P (2002) Lipofuscin and Abeta42 exhibit distinct distribution patterns in normal and Alzheimer’s disease brains. Neurosci Lett 323:45–49
D’Andrea MR, Reiser PA, Polkovitch DA, Gumula NA, Branchide B, Hertzog BM, Schmidheiser D, Belkowski S, Gastard MC, Andrade-Gordon P (2003) The use of formic acid to embellish amyloid plaque detection in Alzheimer’s disease tissues misguides key observations. Neurosci Lett 342:114–118
De Jonghe C, Esselens C, Kumar-Singh S, Craessaerts K, Serneels S, Checler F, Annaert W, Van Broeckhoven C, De Strooper B (2001) Pathogenic APP mutations near the gamma-secretase cleavage site differentially affect Abeta secretion and APP C-terminal fragment stability. Hum Mol Genet 10:1665–1671
Delaère P, He Y, Fayet G, Duyckaerts C, Hauw JJ (1993) Beta A4 deposits are constant in the brain of the oldest old: an immunocytochemical study of 20 French centenarians. Neurobiol Aging 14:191–194
Delatour B, Blanchard V, Pradier L, Duyckaerts C (2003) The innervation of senile plaques: a link between amyloid and neurofibrillary pathology? In: Gauthier S, Scheltenset P, Cummings JL (eds) Alzheimer’s disease and related disorders: Annual 2004. Martin Dunitz, London, pp 1–19
Delatour B, Blanchard V, Pradier L, Duyckaerts C (2004) Alzheimer pathology disorganizes cortico-cortical circuitry: direct evidence from a transgenic animal model. Neurobiol Dis 16:41–47
Delatour B, Guegan M, Volk A, Dhenain M (2006) In vivo MRI and histological evaluation of brain atrophy in APP/PS1 transgenic mice. Neurobiol Aging 27:835–847
Dewachter I, Reverse D, Caluwaerts N, Ris L, Kuiperi C, Van den Haute C, Spittaels K, Umans L, Serneels L, Thiry E, Moechars D, Mercken M, Godaux E, Van Leuven F (2002) Neuronal deficiency of presenilin 1 inhibits amyloid plaque formation and corrects hippocampal long-term potentiation but not a cognitive defect of amyloid precursor protein [V717I] transgenic mice. J Neurosci 22:3445–3453
Dhenain M, Michot J-L, Privat N, Picq JL, Boller F, Duyckaerts C, Volk A (2000) MRI description of cerebral atrophy in mouse lemurs. Relation with amyloid deposition. Neurobiol Aging 21:81–88
Dickson DW, Crystal HA, Bevona C, Honer W, Vincent I, Davies P (1995) Correlations of synaptic and pathological markers with cognition of the elderly. Neurobiol Aging 16:285–304
Dickson DW, Crystal HA, Mattiace LA, Masur DM, Blau AD, Davies P, Yen SH, Aronson MK (1991) Identification of normal and pathological aging in prospectively studied nondemented elderly humans. Neurobiol Aging 13:179–189
Diez M, Koistinaho J, Kahn K, Games D, Hokfelt T (2000) Neuropeptides in hippocampus and cortex in transgenic mice overexpressing V717F beta-amyloid precursor protein—initial observations. Neuroscience 100:259–286
Dodart JC, Bales KR, Gannon KS, Greene SJ, DeMattos RB, Mathis C, DeLong CA, Wu S, Wu X, Holtzman DM, Paul SM (2002) Immunization reverses memory deficits without reducing brain Abeta burden in Alzheimer’s disease model. Nat Neurosci 5:452–457
Dodart JC, Mathis C, Bales KR, Paul SM (2002) Does my mouse have Alzheimer’s disease? Genes Brain Behav 1:1–16
Dodart JC, Mathis C, Saura J, Bales KR, Paul SM, Ungerer A (2000) Neuroanatomical abnormalities in behaviorally characterized APP(V717F) transgenic mice. Neurobiol Dis 7:71–85
Dodart JC, Meziane H, Mathis C, Bales KR, Paul SM, Ungerer A (1999) Behavioral disturbances in transgenic mice overexpressing the V717F beta-amyloid precursor protein. Behav Neurosci 113:982–990
Dong H, Goico B, Martin M, Csernansky CA, Bertchume A, Csernansky JG (2004) Modulation of hippocampal cell proliferation, memory, and amyloid plaque deposition in APPsw (Tg2576) mutant mice by isolation stress. Neuroscience 127:601–609
Dong H, Martin MV, Chambers S, Csernansky JG (2007) Spatial relationship between synapse loss and beta-amyloid deposition in Tg2576 mice. J Comp Neurol 500:311–321
Donovan MH, Yazdani U, Norris RD, Games D, German DC, Eisch AJ (2006) Decreased adult hippocampal neurogenesis in the PDAPP mouse model of Alzheimer’s disease. J Comp Neurol 495:70–83
Duff K, Eckman C, Zehr C, Yu X, Prada CM, Perez-Tur J, Hutton M, Buee L, Harigaya Y, Yager D, Morgan D, Gordon MN, Holcomb L, Refolo L, Zenk B, Hardy J, Younkin S (1996) Increased amyloid-beta42(43) in brains of mice expressing mutant presenilin 1. Nature 383:710–713
Duff K, Knight H, Refolo LM, Sanders S, Yu X, Picciano M, Malester B, Hutton M, Adamson J, Goedert M, Burki K, Davies P (2000) Characterization of pathology in transgenic mice over-expressing human genomic and cDNA tau transgenes. Neurobiol Dis 7:87–98
Eckman EA, Reed DK, Eckman CB (2001) Degradation of the Alzheimer’s amyloid beta peptide by endothelin-converting enzyme. J Biol Chem 276:24540–24548
Edbauer D, Winkler E, Regula JT, Pesold B, Steiner H, Haass C (2003) Reconstitution of gamma-secretase activity. Nat Cell Biol 5:486–488
Esposito L, Raber J, Kekonius L, Yan F, Yu GQ, Bien-Ly N, Puolivali J, Scearce-Levie K, Masliah E, Mucke L (2006) Reduction in mitochondrial superoxide dismutase modulates Alzheimer’s disease-like pathology and accelerates the onset of behavioral changes in human amyloid precursor protein transgenic mice. J Neurosci 26:5167–5179
Fagan AM, Watson M, Parsadanian M, Bales KR, Paul SM, Holtzman DM (2002) Human and murine ApoE markedly alters Abeta metabolism before and after plaque formation in a mouse model of Alzheimer’s disease. Neurobiol Dis 9:305–318
Farris W, Schutz SG, Cirrito JR, Shankar GM, Sun X, George A, Leissring MA, Walsh DM, Qiu WQ, Holtzman DM, Selkoe DJ (2007) Loss of neprilysin function promotes amyloid plaque formation and causes cerebral amyloid angiopathy. J Neurosci 27:2866–2875
Folkesson R, Malkiewicz K, Kloskowska E, Nilsson T, Popova E, Bogdanovic N, Ganten U, Ganten D, Bader M, Winblad B, Benedikz E (2007) A transgenic rat expressing human APP with the Swedish Alzheimer’s disease mutation. Biochem Biophys Res Commun 358:777–782
Fukuchi K, Ho L, Younkin SG, Kunkel DD, Ogburn CE, LeBoeuf RC, Furlong CE, Deeb SS, Nochlin D, Wegiel J, Wisniewski HM, Martin GM (1996) High levels of circulating beta-amyloid peptide do not cause cerebral beta-amyloidosis in transgenic mice. Am J Pathol 149:219–227
Games D, Adams D, Alessandrini R, Barbour R, Berthelette P, Blackwell C, Carr T, Clemens J, Donaldson T, Gillepsie F, Guido T, Hagopian S, Johnson-Wood K, Khan K, Lee M, Leibowitz P, Liberburg I, Little S, Masliah E, McColongue L, Montaya-Zavala M, Mucke L, Paganini L, Penniman E, Power M, Schenk D, Seubert P, Snyder B, Soriano F, Tan H, Vitale J, Wadsworth S, Wolozin B, Zhao J (1995) Alzheimer-type neuropathology in transgenic mice overexpressing V717F β-amyloid precursor protein. Nature 373:523–527
Games D, Khan KM, Soriano FG, Keim PS, Davis DL, Bryant K, Lieberburg I (1992) Lack of Alzheimer pathology after beta-amyloid protein injections in rat brain. Neurobiol Aging 13:569–576
Garcia-Alloza M, Robbins EM, Zhang-Nunes SX, Purcell SM, Betensky RA, Raju S, Prada C, Greenberg SM, Bacskai BJ, Frosch MP (2006) Characterization of amyloid deposition in the APPswe/PS1dE9 mouse model of Alzheimer disease. Neurobiol Dis 24:516–524
Gerlai R, Fitch T, Bales KR, Gitter BD (2002) Behavioral impairment of APP(V717F) mice in fear conditioning: is it only cognition? Behav Brain Res 136:503–509
German DC, Eisch AJ (2004) Mouse models of Alzheimer’s disease: insight into treatment. Rev Neurosci 15:353–369
German DC, Yazdani U, Speciale SG, Pasbakhsh P, Games D, Liang CL (2003) Cholinergic neuropathology in a mouse model of Alzheimer’s disease. J Comp Neurol 462:371–381
Giacchino J, Criado JR, Games D, Henriksen S (2000) In vivo synaptic transmission in young and aged amyloid precursor protein transgenic mice. Brain Res 876:185–190
Glenner GG, Wong CW (1984) Alzheimer’s disease: Initial report of the purification and characterization of a novel cerebrovascular amyloid protein. Biochem Biophys Res Commun 120:885–890
Goate A, Chartier-Harlin MC, Mullan M, Brown J, Crawford F, Fidani L, Giuffra L, Haynes A, Irving N, James L, Mant R, Newton P, Rooke K, Roques P, Talbot C, Pericak-Vance M, Roses A, Williamson R, Rossor M, Owen M, Hardy J (1991) Segregation of a missense mutation in the amyloid precursor protein gene with familial Alzheimer’s disease. Nature 349:704–706
Goedert M, Spillantini MG, Potier MC, Ulrich J, Crowther RA (1989) Cloning and sequencing of the cDNA encoding an isoform of microtubule-associated protein tau containing four tandem repeats: differential expression of tau protein mRNAs in human brain. EMBO J 8:393–399
Gomez-Isla T, Hollister R, West H, Mui S, Growdon JH, Petersen RC, Parisi JE, Hyman BT (1997) Neuronal loss correlates with but exceeds neurofibrillary tangles in Alzheimer’s disease. Ann Neurol 41:17–24
Gonzalez-Lima F, Berndt JD, Valla JE, Games D, Reiman EM (2001) Reduced corpus callosum, fornix and hippocampus in PDAPP transgenic mouse model of Alzheimer’s disease. Neuroreport 12:2375–2379
Gordon MN, King DL, Diamond DM, Jantzen PT, Boyett KV, Hope CE, Hatcher JM, DiCarlo G, Gottschall WP, Morgan D, Arendash GW (2001) Correlation between cognitive deficits and Abeta deposits in transgenic APP+PS1 mice. Neurobiol Aging 22:377–385
Götz J, Chen F, van Dorpe J, Nitsch RM (2001) Formation of neurofibrillary tangles in P301L tau transgenic mice induced by Abeta42 fibrils. Science 293:1491–1495
Götz J, Probst A, Spillantini MG, Schafer T, Jakes R, Burki K, Goedert M (1995) Somatodendritic localization and hyperphosphorylation of tau protein in transgenic mice expressing the longest human brain tau isoform. EMBO J 14:1304–1313
Gouras GK, Tsai J, Naslund J, Vincent B, Edgar M, Checler F, Greenfield JP, Haroutunian V, Buxbaum JD, Xu H, Greengard P, Relkin NR (2000) Intraneuronal Abeta42 accumulation in human brain. Am J Pathol 156:15–20
Greenfield JP, Tsai J, Gouras GK, Hai B, Thinakaran G, Checler F, Sisodia SS, Greengard P, Xu H (1999) Endoplasmic reticulum and trans-Golgi network generate distinct populations of Alzheimer beta-amyloid peptides. Proc Natl Acad Sci USA 96:742–747
Gyure KA, Durham R, Stewart WF, Smialek JE, Troncoso JC (2001) Intraneuronal abeta-amyloid precedes development of amyloid plaques in Down syndrome. Arch Pathol Lab Med 125:489–492
Hardy J (1999) The shorter amyloid cascade hypothesis. Neurobiol Aging 20:85
Hardy J (2002) Testing times for the “amyloid cascade hypothesis”. Neurobiol Aging 23:1073–1074
Hardy J, Allsop D (1991) Amyloid deposition as the central event in the aetiology of Alzheimer’s disease. Trends Pharmacol Sci 12:383–388
Hardy JA, Mann DMA, Wester P, Winblad B (1986) An integrative hypothesis concerning the pathogenesis and progression of Alzheimer’s disease. Neurobiol Aging 7:489
Harrison SM, Harper AJ, Hawkins J, Duddy G, Grau E, Pugh PL, Winter PH, Shilliam CS, Hughes ZA, Dawson LA, Gonzalez I, Upton N, Pangalos MN, Dingwallb C (2003) BACE1 (beta-secretase) transgenic and knockout mice: identification of neurochemical deficits and behavioral changes. Mol Cell Neurosci 24:646–655
Hartmann J, Erb C, Ebert U, Baumann KH, Popp A, König G, Klein J (2004) Central cholinergic functions in human amyloid precursor protein knock-in/presenilin-1 transgenic mice. Neuroscience 125:1009–1017
Haughey NJ, Nath A, Chan SL, Borchard AC, Rao MS, Mattson MP (2002) Disruption of neurogenesis by amyloid beta-peptide, and perturbed neural progenitor cell homeostasis, in models of Alzheimer’s disease. J Neurochem 83:1509–1524
Heneka MT, Sastre M, Dumitrescu-Ozimek L, Dewachter I, Walter J, Klockgether T, Van Leuven F (2005) Focal glial activation coincides with increased BACE1 activation and precedes amyloid plaque deposition in APP[V717I] transgenic mice. J Neuroinflam 2:22
Herms J, Anliker B, Heber S, Ring S, Fuhrmann M, Kretzschmar H, Sisodia S, Müller U (2004) Cortical dysplasia resembling human type 2 lissencephaly in mice lacking all three APP family members. EMBO J 23:4106–4115
Hernandez D, Sugaya K, Qu T, McGowan E, Duff K, McKinney M (2001) Survival and plasticity of basal forebrain cholinergic systems in mice transgenic for presenilin-1 and amyloid precursor protein mutant genes. Neuroreport 12:1377–1384
Herzig MC, Paganetti P, Staufenbiel M, Jucker M (2007) BACE1 and mutated presenilin-1 differently modulate Abeta40 and Abeta42 levels and cerebral amyloidosis in APPDutch transgenic mice. Neurodegener Dis 4:127–135
Herzig MC, Van Nostrand WE, Jucker M (2006) Mechanism of cerebral beta-amyloid angiopathy: murine and cellular models. Brain Pathol 16:40–54
Herzig MC, Winkler DT, Burgermeister P, Pfeifer M, Kohler E, Schmidt SD, Danner S, Abramowski D, Stürchler-Pierrat C, Bürki K, van Duinen SG, Maat-Schieman ML, Staufenbiel M, Mathews PM, Jucker M (2004) Abeta is targeted to the vasculature in a mouse model of hereditary cerebral hemorrhage with amyloidosis. Nat Neurosci 7:954–960
Higgins GA, Jacobsen H (2003) Transgenic mouse models of Alzheimer’s disease: phenotype and application. Behav Pharmacol 14:419–438
Higgins LS, Catalano R, Quon D, Cordell B (1993) Transgenic mice expressing human beta-APP751, but not mice expressing beta-APP695, display early Alzheimer’s disease-like histopathology. Ann N Y Acad Sci 695:224–227
Holcomb L, Gordon MN, McGowan E, Yu X, Benkovic S, Jantzen P, Wright K, Saad I, Mueller R, Morgan D, Sanders S, Zehr C, O’Campo K, Hardy J, Prada CM, Eckman C, Younkin S, Hsiao K, Duff K (1998) Accelerated Alzheimer-type phenotype in transgenic mice carrying both mutant amyloid precursor protein and presenilin 1 transgenes. Nat Med 4:97–100
Holcomb LA, Gordon MN, Jantzen P, Hsiao K, Duff K, Morgan D (1999) Behavioral changes in transgenic mice expressing both amyloid precursor protein and presenilin-1 mutations: lack of association with amyloid deposits. Behav Genet 29:177–185
Holtzman DM, Bales KR, Tenkovai T, Fagan AM, Parsadanian M, Sartorius LJ, Mackey B, Olneyi J, McKeel D, Wozniaki D, Paul S (2000) Apolipoprotein E isoform-dependent amyloid deposition and neuritic degeneration in a mouse model of Alzheimer’s disease. Proc Natl Acad Sci USA 97:2892–2897
Hornsten A, Lieberthal J, Fadia S, Malins R, Ha L, Xu X, Daigle I, Markowitz M, O’Connor G, Plasterk R, Li C (2007) APL-1, a Caenorhabditis elegans protein related to the human beta-amyloid precursor protein, is essential for viability. Proc Natl Acad Sci USA 104:1971–1976
Howlett DR, Richardson JC, Austin A, Parsons AA, Bate ST, Davies DC, Gonzalez MI (2004) Cognitive correlates of Abeta deposition in male and female mice bearing amyloid precursor protein and presenilin-1 mutant transgenes. Brain Res 1017:130–136
Hsia AY, Masliah E, McConlogue L, Yu GQ, Tatsuno G, Hu K, Kholodenko D, Malenka RC, Nicoll RA, Mucke L (1999) Plaque-independent disruption of neural circuits in Alzheimer’s disease mouse models. Proc Natl Acad Sci USA 96:3228–3233
Hsiao K, Chapman P, Nilsen S, Eckman C, Harigaya Y, YounKin S, Yang F, Cole G (1996) Correlative memory deficits, Abeta elevation, and amyloid plaques in trangenic mice. Science 274:99–102
Huang SM, Mouri A, Kokubo H, Nakajima R, Suemoto T, Higuchi M, Staufenbiel M, Noda Y, Yamaguchi H, Nabeshima T, Saido TC, Iwata N (2006) Neprilysin-sensitive synapse-associated amyloid-beta peptide oligomers impair neuronal plasticity and cognitive function. J Biol Chem 281:17941–17951
Huitron-Resendiz S, Sanchez-Alavez M, Gallegos R, Berg G, Crawford E, Giacchino JL, Games D, Henriksen SJ, Criado JR (2002) Age-independent and age-related deficits in visuospatial learning, sleep-wake states, thermoregulation and motor activity in PDAPP mice. Brain Res 928:126–137
Hunter CL, Bimonte-Nelson HA, Nelson M, Eckman CB, Granholm AC (2004) Behavioral and neurobiological markers of Alzheimer’s disease in Ts65Dn mice: effects of estrogen. Neurobiol Aging 25:873–884
Hunter CL, Isacson O, Nelson M, Bimonte-Nelson H, Seo H, Lin L, Ford K, Kindy MS, Granholm AC (2003) Regional alterations in amyloid precursor protein and nerve growth factor across age in a mouse model of Down’s syndrome. Neurosci Res 45:437–445
Huse JT, Pijak DS, Leslie GJ, Lee VM, Doms RW (2000) Maturation and endosomal targeting of beta-site amyloid precursor protein-cleaving enzyme. The Alzheimer’s disease beta-secretase. J Biol Chem 275:33729–33737
Hutter-Paier B, Huttunen HJ, Puglielli L, Eckman CB, Kim DY, Hofmeister A, Moir RD, Domnitz SB, Frosch MP, Windisch M, Kovacs DM (2004) The ACAT inhibitor CP-113,818 markedly reduces amyloid pathology in a mouse model of Alzheimer’s disease. Neuron 44:227–238
Irizarry MC, Cheung BS, Rebeck GW, Paul SM, Bales KR, Hyman BT (2000) Apolipoprotein E affects the amount, form, and anatomical distribution of amyloid beta-peptide deposition in homozygous APP(V717F) transgenic mice. Acta Neuropathol (Berl) 100:451–458
Irizarry MC, McNamara M, Fedorchak K, Hsiao K, Hyman BT (1997) APPSw transgenic mice develop age-related A beta deposits and neuropil abnormalities, but no neuronal loss in CA1. J Neuropathol Exp Neurol 56:965–973
Irizarry MC, Soriano F, McNamara M, Page KJ, Schenk D, Games D, Hyman BT (1997) Abeta deposition is associated with neuropil changes, but not with overt neuronal loss in the human amyloid precursor protein V717F (PDAPP) transgenic mouse. J Neurosci 17:7053–7059
Ishihara T, Hong M, Zhang B, Nakagawa Y, Lee MK, Trojanowski JQ, Lee VM (1999) Age-dependent emergence and progression of a tauopathy in transgenic mice overexpressing the shortest human tau isoform. Neuron 24:751–762
Iwata N, Tsubuki S, Takaki Y, Shirotani K, Lu B, Gerard NP, Gerard C, Hama E, Lee HJ, Saido TC (2001) Metabolic regulation of brain Abeta by neprilysin. Science 292:1550–1552
Iwata N, Tsubuki S, Takaki Y, Watanabe K, Sekiguchi M, Hosoki E, Kawashima-Morishima M, Lee HJ, Hama E, Sekine-Aizawa Y, Saido TC (2000) Identification of the major Abeta 1–42 degrading catabolic pathway in brain parenchyma: suppression leads to biochemical and pathological deposition. Nat Med 6:143–150
Jankowsky J, Zu G, Fromholt D, Gonzales V, Borchelt DR (2003) Environmental enrichment exacerbates amyloid plaque formation in a transgenic mouse model of Alzheimer disease. J Neuropathol Exp Neurol 62:1220–1227
Jankowsky JL, Melnikova T, Fadale DJ, Xu GM, Slunt HH, Gonzales V, Younkin LH, Younkin SG, Borchelt DR, Savonenko AV (2005) Environmental enrichment mitigates cognitive deficits in a mouse model of Alzheimer’s disease. J Neurosci 25:5217–5224
Jankowsky JL, Slunt HH, Gonzales V, Savonenko AV, Wen JC, Jenkins NA, Copeland NG, Younkin LH, Lester HA, Younkin SG, Borchelt DR (2005) Persistent amyloidosis following suppression of Abeta production in a transgenic model of Alzheimer disease. PLoS Med 2:e355
Jankowsky JL, Younkin LH, Gonzales V, Fadale DJ, Slunt HH, Lester HA, Younkin SG, Borchelt DR (2007) Rodent abeta modulates the solubility and distribution of amyloid deposits in transgenic mice. J Biol Chem 282:22707–22720
Janus C, D’Amelio S, Amitay O, Chishti MA, Strome R, Fraser P, Carlson GA, Roder JC, St George-Hyslop P, Westaway D (2000) Spatial learning in transgenic mice expressing human presenilin 1 (PS1) transgenes. Neurobiol Aging 21:541–549
Janus C, Pearson J, McLaurin J, Mathews PM, Jiang Y, Schmidt SD, Chishti MA, Horne P, Heslin D, French J, Mount HT, Nixon RA, Mercken M, Bergeron C, Fraser PE, St George-Hyslop P, Westaway D (2000) A beta peptide immunization reduces behavioural impairment and plaques in a model of Alzheimer’s disease. Nature 408:979–982
Jin K, Galvan V, Xie L, Mao XO, Gorostiza OF, Bredesen DE, Greenberg DA (2004) Enhanced neurogenesis in Alzheimer’s disease transgenic (PDGF-APPSw,Ind) mice. Proc Natl Acad Sci USA 101:13363–13367
Jin K, Peel AL, Mao XO, Xie L, Cottrell BA, Henshall DC, Greenberg DA (2004) Increased hippocampal neurogenesis in Alzheimer’s disease. Proc Natl Acad Sci USA 101:343–347
Johnson-Wood K, Lee M, Motter R, Hu K, Gordon G, Barbour R, Khan K, Gordon M, Tan H, Games D, Lieberburg I, Schenk D, Seubert P, McConlogue L (1997) Amyloid precursor protein processing and A beta42 deposition in a transgenic mouse model of Alzheimer disease. Proc Natl Acad Sci USA 94:1550–1555
Kalback W, Watson MD, Kokjohn TA, Kuo YM, Weiss N, Luehrs DC, Lopez J, Brune D, Sisodia SS, Staufenbiel M, Emmerling M, Roher AE (2002) APP transgenic mice Tg2576 accumulate Abeta peptides that are distinct from the chemically modified and insoluble peptides deposited in Alzheimer’s disease senile plaques. Biochemistry 41:922–928
Kammesheidt A, Boyce FM, Spanoyannis AF, Cummings BJ, Ortegon M, Cotman CW, Vaught JF, Neve RL (1992) Deposition of ß/A4 immunoreactivity and neuronal pathology in transgenic mice expressing the carboxyl-terminal fragment of the Alzheimer amyloid precursor in the brain. Proc Natl Acad Sci (USA) 89:10857–10861
Kawabata S, Higgins GA, Gordon JW (1991) Amyloid plaques, neurofibrillary tangles and neuronal loss in brains of transgenic mice overexpressing a C-terminal fragment of human amyloid precursor protein. Nature 354:476–478
Kawarabayashi T, Shoji M, Younkin LH, Wen-Lang L, Dickson DW, Murakami T, Matsubara E, Abe K, Ashe KH, Younkin SG (2004) Dimeric amyloid beta protein rapidly accumulates in lipid rafts followed by apolipoprotein E and phosphorylated tau accumulation in the Tg2576 mouse model of Alzheimer’s disease. J Neurosci 24:3801–3809
Kelly PH, Bondolfi L, Hunziker D, Schlecht HP, Carver K, Maguire E, Abramowski D, Wiederhold KH, Sturchler-Pierrat C, Jucker M, Bergmann R, Staufenbiel M, Sommer B (2003) Progressive age-related impairment of cognitive behavior in APP23 transgenic mice. Neurobiol Aging 24:365–378
King DL, Arendash GW (2002) Behavioral characterization of the Tg2576 transgenic model of Alzheimer’s disease through 19 months. Physiol Behav 75:627–642
King DL, Arendash GW (2002) Maintained synaptophysin immunoreactivity in Tg2576 transgenic mice during aging: correlations with cognitive impairment. Brain Res 926:58–68
King DL, Arendash GW, Crawford F, Sterk T, Menendez J, Mullan MJ (1999) Progressive and gender-dependent cognitive impairment in the APP(SW) transgenic mouse model for Alzheimer’s disease. Behav Brain Res 103:145–162
Klunk WE, Lopresti BJ, Ikonomovic MD, Lefterov IM, Koldamova RP, Abrahamson EE, Debnath ML, Holt DP, Huang GF, Shao L, DeKosky ST, Price JC, Mathis CA (2005) Binding of the positron emission tomography tracer Pittsburgh compound-B reflects the amount of amyloid-beta in Alzheimer’s disease brain but not in transgenic mouse brain. J Neurosci 25:10598–10606
Kobayashi D, Zeller M, Cole T, Buttini M, McConlogue L, Sinha S, Freedman S, Morris RG, Chen KS (2007) BACE1 gene deletion: Impact on behavioral function in a model of Alzheimer’s disease. Neurobiol Aging 26:134–145
Kobayashi DT, Chen KS (2005) Behavioral phenotypes of amyloid-based genetically modified mouse models of Alzheimer’s disease. Genes Brain Behav 4:173–196
Kojro E, Fahrenholz F (2005) The non-amyloidogenic pathway: structure and function of alpha-secretases. Subcell Biochem 38:105–127
Koldamova R, Staufenbiel M, Lefterov I (2005) Lack of ABCA1 considerably decreases brain ApoE level and increases amyloid deposition in APP23 mice. J Biol Chem 280:43224–43235
Kulnane LS, Lamb BT (2001) Neuropathological characterization of mutant amyloid precursor protein yeast artificial chromosome transgenic mice. Neurobiol Dis 8:982–992
Kumar-Singh S, De Jonghe C, Cruts M, Kleinert R, Wang R, Mercken M, De Strooper B, Vanderstichele H, Lofgren A, Vanderhoeven I, Backhovens H, Vanmechelen E, Kroisel PM, Van Broeckhoven C (2000) Nonfibrillar diffuse amyloid deposition due to a gamma(42)-secretase site mutation points to an essential role for N-truncated A beta(42) in Alzheimer’s disease. Hum Mol Genet 9:2589–2598
Kumar-Singh S, Dewachter I, Moechars D, Lübke U, De Jonghe C, Ceuterick C, Checler F, Naidu A, Cordell B, Cras P, Van Broeckhoven C, Van Leuven F (2000) Behavioral disturbances without amyloid deposits in mice overexpressing human amyloid precursor protein with Flemish (A692G) or Dutch (E693Q) mutation. Neurobiol Dis 7:9–22
Kuo YM, Kokjohn TA, Beach TG, Sue LI, Brune D, Lopez JC, Kalback WM, Abramowski D, Sturchler-Pierrat C, Staufenbiel M, Roher AE (2001) Comparative analysis of amyloid-beta chemical structure and amyloid plaque morphology of transgenic mouse and Alzheimer’s disease brains. J Biol Chem 276:12991–12998
Kurt MA, Davies DC, Kidd M, Duff K, Howlett DR (2003) Hyperphosphorylated tau and paired helical filament-like structures in the brains of mice carrying mutant amyloid precursor protein and mutant presenilin-1 transgenes. Neurobiol Dis 14:89–97
Lacor PN, Buniel MC, Furlow PW, Clemente AS, Velasco PT, Wood M, Viola KL, Klein WL (2007) Abeta oligomer-induced aberrations in synapse composition, shape, and density provide a molecular basis for loss of connectivity in Alzheimer’s disease. J Neurosci 27:796–807
LaFerla FM, Green KN, Oddo S (2007) Intracellular amyloid-beta in Alzheimer’s disease. Nat Rev Neurosci 8:499–509
LaFerla FM, Tinkle BT, Bieberich CJ, Haudenschild CC, Jay G (1993) The Alzheimer’s A beta peptide induces neurodegeneration and apoptotic cell death in transgenic mice. Nat Genet 5:22–30
Lalonde R (2002) The neurobiological basis of spontaneous alternation. Neurosci Biobehav Rev 26:91–104
Lalonde R, Dumont M, Staufenbiel M, Sturchler-Pierrat C, Strazielle C (2002) Spatial learning, exploration, anxiety, and motor coordination in female APP23 transgenic mice with the Swedish mutation. Brain Res 956:36–44
Lalonde R, Lewis TL, Strazielle C, Kim H, Fukuchi K (2003) Transgenic mice expressing the betaAPP695SWE mutation: effects on exploratory activity, anxiety, and motor coordination. Brain Res 977:38–45
Lalonde R, Qian S, Strazielle C (2003) Transgenic mice expressing the PS1-A246E mutation: effects on spatial learning, exploration, anxiety, and motor coordination. Behav Brain Res 138:71–79
Lamb BT, Call LM, Slunt HH, Bardel KA, Lawler AM, Eckman CB, Younkin SG, Holtz G, Wagner SL, Price DL, Sisodia SS, Gearhart JD (1997) Altered metabolism of familial Alzheimer’s disease-linked amyloid precursor protein variants in yeast artificial chromosome transgenic mice. Human Mol Genet 6:1535–1541
Langui D, Anderton BH, Brion JP, Ulrich J (1988) Effects of aluminium chloride on cultured cells from rat brain hemispheres. Brain Res 438:67–76
Langui D, Girardot N, El Hachimi H, Allinquant B, Blanchard V, Pradier L, Duyckaerts C (2004) Subcellular topography of neuronal A-beta peptide in APPxPS1 transgenic mice. Am J Pathol 165:1465–1477
Lanz TA, Carter DB, Merchant KM (2003) Dendritic spine loss in the hippocampus of young PDAPP and Tg2576 mice and its prevention by the ApoE2 genotype. Neurobiol Dis 13:246–253
Lazarov O, Lee M, Peterson DA, Sisodia SS (2002) Evidence that synaptically released beta-amyloid accumulates as extracellular deposits in the hippocampus of transgenic mice. J Neurosci 22:9785–9793
Lazarov O, Morfini GA, Pigino G, Gadadhar A, Chen X, Robinson J, Ho H, Brady ST, Sisodia SS (2007) Impairments in fast axonal transport and motor neuron deficits in transgenic mice expressing familial Alzheimer’s disease-linked mutant presenilin 1. J Neurosci 27:7011–7020
Le R, Cruz L, Urbanc B, Knowles RB, Hsiao-Ashe K, Duff K, Irizarry MC, Stanley HE, Hyman BT (2001) Plaque-induced abnormalities in neurite geometry in transgenic models of Alzheimer disease: implications for neural system disruption. J Neuropathol Exp Neurol 60:753–758
Lee MK, Borchelt DR, Kim G, Thinakaran G, Slunt HH, Ratovitski T, Martin LJ, Kittur A, Gandy S, Levey AI, Jenkins N, Copeland N, Price DL, Sisodia SS (1997) Hyperaccumulation of FAD-linked presenilin 1 variants in vivo. Nat Med 3:756–760
Lesné S, Teng Koh M, Kotilinek L, Kayed R, Glabe CG, Yang A, Gallagher M, Ashe KH (2006) A specific amyloid-beta protein assembly in the brain impairs memory. Nature 440:352–357
Lesuisse C, Xu G, Anderson J, Wong M, Jankowsky J, Holtz G, Gonzalez V, Wong PC, Price DL, Tang F, Wagner S, Borchelt DR (2001) Hyper-expression of human apolipoprotein E4 in astroglia and neurons does not enhance amyloid deposition in transgenic mice. Hum Mol Genet 10:2525–2537
Levi O, Michaelson DM (2007) Environmental enrichment stimulates neurogenesis in apolipoprotein E3 and neuronal apoptosis in apolipoprotein E4 transgenic mice. J Neurochem 100:202–210
Lewis J, Dickson DW, Lin WL, Chisholm L, Corral A, Jones G, Yen SH, Sahara N, Skipper L, Yager D, Eckman C, Hardy J, Hutton M, McGowan E (2001) Enhanced neurofibrillary degeneration in transgenic mice expressing mutant tau and APP. Science 293:1487–1491
Lewis J, McGowan E, Rockwood J, Melrose H, Nacharaju P, Van Slegtenhorst M, Gwinn-Hardy K, Paul Murphy M, Baker M, Yu X, Duff K, Hardy J, Corral A, Lin WL, Yen SH, Dickson DW, Davies P, Hutton M (2000) Neurofibrillary tangles, amyotrophy and progressive motor disturbance in mice expressing mutant (P301L) tau protein. Nat Genet 25:402–405
Liu L, Ikonen S, Heikkinen T, Heikkila M, Puolivali J, van Groen T, Tanila H (2002) Effects of fimbria-fornix lesion and amyloid pathology on spatial learning and memory in transgenic APP+PS1 mice. Behav Brain Res 134:433–445
Liu L, Tapiola T, Herukka SK, Heikkila M, Tanila H (2003) Abeta levels in serum, CSF and brain, and cognitive deficits in APP + PS1 transgenic mice. Neuroreport 14:163–166
Luo Y, Bolon B, Kahn S, Bennett BD, Babu-Khan S, Denis P, Fan W, Kha H, Zhang J, Gong Y, Martin L, Louis JC, Yan Q, Richards WG, Citron M, Vassar R (2001) Mice deficient in BACE1, the Alzheimer’s beta-secretase, have normal phenotype and abolished beta-amyloid generation. Nat Neurosci 4:231–232
Luth HJ, Apelt J, Ihunwo AO, Arendt T, Schliebs R (2003) Degeneration of beta-amyloid-associated cholinergic structures in transgenic APP SW mice. Brain Res 977:16–22
Madani R, Poirier R, Wolfer DP, Welzl H, Groscurth P, Lipp HP, Lu B, El Mouedden M, Mercken M, Nitsch RM, Mohajeri MH (2006) Lack of neprilysin suffices to generate murine amyloid-like deposits in the brain and behavioral deficit in vivo. J Neurosci Res 84:1871–1878
Magara F, Müller U, Li ZW, Lipp HP, Weissmann C, Stagljar M, Wolfer DP (1999) Genetic background changes the pattern of forebrain commissure defects in transgenic mice underexpressing the beta-amyloid-precursor protein. Proc Natl Acad Sci USA 96:4656–4661
Malherbe P, Richards JG, Martin JR, Bluethmann H, Maggio J, Huber G (1996) Lack of beta-amyloidosis in transgenic mice expressing low levels of familial Alzheimer’s disease missense mutations. Neurobiol Aging 17:205–214
Malm TM, Koistinaho M, Parepalo M, Vatanen T, Ooka A, Karlsson S, Koistinaho J (2005) Bone-marrow-derived cells contribute to the recruitment of microglial cells in response to beta-amyloid deposition in APP/PS1 double transgenic Alzheimer mice. Neurobiol Dis 18:134–142
Marr RA, Rockenstein E, Mukherjee A, Kindy MS, Hersh LB, Gage FH, Verma IM, Masliah E (2003) Neprilysin gene transfer reduces human amyloid pathology in transgenic mice. J Neurosci 23:1992–1996
Masliah E, Rockenstein E, Veinbergs I, Sagara Y, Mallory M, Hashimoto M, Mucke L (2001) Beta-amyloid peptides enhance alpha-synuclein accumulation and neuronal deficits in a transgenic mouse model linking Alzheimer’s disease and Parkinson’s disease. Proc Natl Acad Sci USA 98:12245–12250
Masliah E, Sisk A, Mallory M, Games D (2001) Neurofibrillary pathology in transgenic mice overexpressing V717F beta-amyloid precursor protein. J Neuropathol Exp Neurol 60:357–368
Masters CL, Simms G, Weinman NA, Multhaup G, McDonald BL, Beyreuther K (1985) Amyloid plaque core protein in Alzheimer disease and Down syndrome. Proc Natl Acad Sci USA 82:4245–4249
Matsuoka Y, Picciano M, Malester B, LaFrancois J, Zehr C, Daeschner JM, Olschowka JA, Fonseca MI, O’Banion MK, Tenner AJ, Lemere CA, Duff K (2001) Inflammatory responses to amyloidosis in a transgenic mouse model of Alzheimer’s disease. Am J Pathol 158:1345–1354
Matsuoka Y, Vila M, Lincoln S, McCormack A, Picciano M, LaFrancois J, Yu X, Dickson D, Langston WJ, McGowan E, Farrer M, Hardy J, Duff K, Przedborski S, Di Monte DA (2001) Lack of nigral pathology in transgenic mice expressing human alpha-synuclein driven by the tyrosine hydroxylase promoter. Neurobiol Dis 8:535–539
Mattson MP, Gary DS, Chan SL, Duan W (2001) Perturbed endoplasmic reticulum function, synaptic apoptosis and the pathogenesis of Alzheimer’s disease. Biochem Soc Symp 67:151–162
McConlogue L, Buttini M, Anderson JP, Brigham EF, Chen KS, Freedman SB, Games D, Johnson-Wood K, Lee M, Zeller M, Liu W, Motter R, Sinha S (2007) Partial reduction of BACE1 has dramatic effects on Alzheimer plaque and synaptic pathology in APP transgenic mice. J Biol Chem 282:26326–26334
McCool MF, Varty GB, Del Vecchio RA, Kazdoba TM, Parker EM, Hunter JC, Hyde LA (2003) Increased auditory startle response and reduced prepulse inhibition of startle in transgenic mice expressing a double mutant form of amyloid precursor protein. Brain Res 994:99–106
McGowan E, Eriksen J, Hutton M (2006) A decade of modeling Alzheimer’s disease in transgenic mice. Trends Genet 22:281–289
McGowan E, Pickford F, Dickson D (2003) Alzheimer animal models: models of Abeta deposition in transgenic mice. In: Dickson D (ed) Neurodegeneration: the molecular pathology of dementia and movement disorders. ISN Neuropath Press, Basel, pp 74–79
McGowan E, Sanders S, Iwatsubo T, Takeuchi A, Saido T, Zehr C, Yu X, Uljon S, Wang R, Mann D, Dickson D, Duff K (1999) Amyloid phenotype characterization of transgenic mice overexpressing both mutant amyloid precursor protein and mutant presenilin 1 transgenes. Neurobiol Dis 6:231–244
Mehlhorn G, Hollborn M, Schliebs R (2000) Induction of cytokines in glial cells surrounding cortical beta-amyloid plaques in transgenic Tg2576 mice with Alzheimer pathology. Int J Dev Neurosci 18:423–431
Meyer-Luehmann M, Coomaraswamy J, Bolmont T, Kaeser S, Schaefer C, Kilger E, Neuenschwander A, Abramowski D, Frey P, Jaton AL, Vigouret JM, Paganetti P, Walsh DM, Mathews PM, Ghiso J, Staufenbiel M, Walker LC, Jucker M (2006) Exogenous induction of cerebral beta-amyloidogenesis is governed by agent and host. Science 313:1781–1784
Middei S, Geracitano R, Caprioli A, Mercuri N, Ammassari-Teule M (2004) Preserved fronto-striatal plasticity and enhanced procedural learning in a transgenic mouse model of Alzheimer’s disease overexpressing mutant hAPPswe. Learn Mem 11:447–452
Moechars D, Lorent K, Van Leuven F (1999) Premature death in transgenic mice that overexpress a mutant amyloid precursor protein is preceded by severe neurodegeneration and apoptosis. Neuroscience 91:819–830
Mori C, Spooner ET, Wisniewsk KE, Wisniewski TM, Yamaguch H, Saido TC, Tolan DR, Selkoe DJ, Lemere CA (2002) Intraneuronal Abeta42 accumulation in Down syndrome brain. Amyloid 9:88–102
Mucke L, Masliah E, Yu GQ, Mallory M, Rockenstein EM, Tatsuno G, Hu K, Kholodenko D, Johnson-Wood K, McConlogue L (2000) High-level neuronal expression of abeta 1–42 in wild-type human amyloid protein precursor transgenic mice: synaptotoxicity without plaque formation. J Neurosci 20:4050–4058
Mucke L, Masliah E, Yu GQ, Mallory M, Rockenstein EM, Tatsuno G, Hu K, Kholodenko D, Johnson-Wood K, McConlogue L (2000) High-level neuronal expression of Abeta 1–42 in wild-type human amyloid protein precursor transgenic mice: synaptotoxicity without plaque formation. J Neurosci 20:4050–4058
Mucke L, Yu GQ, McConlogue L, Rockenstein EM, Abraham CR, Masliah E (2000) Astroglial expression of human alpha(1)-antichymotrypsin enhances alzheimer-like pathology in amyloid protein precursor transgenic mice. Am J Pathol 157:2003–2010
Munoz-Garcia D, Pendlebury WW, Kessler JB, Perl DP (1986) An immunocytochemical comparison of cytoskeletal proteins in aluminum-induced and Alzheimer-type neurofibrillary tangles. Acta Neuropathol (Berl) 70:243–248
Murray CL, Fibiger HC (1985) Learning and memory deficits after lesions of the nucleus basalis magnocellularis: reversal by physostigmine. Neuroscience 14:1025–1032
Nakamura S, Murayama N, Noshita T, Annoura H, Ohno T (2001) Progressive brain dysfunction following intracerebroventricular infusion of beta(1–42)-amyloid peptide. Brain Res 912:128–136
Nalbantoglu J, Tirado-Santiago G, Lahsaini A, Poirier J, Goncalves O, Verge G, Momoli F, Welner SA, Massicote G, Julien JP, Shapiro ML (1997) Impaired learning and LTP in mice expressing the carboxy terminus of the Alzheimer amyloid precursor protein. Nature 387:500–505
Namba Y, Tomonaga M, Kawasaki H, Otomo E, Ikeda K (1991) Apolipoprotein E immunoreactivity in cerebral amyloid deposits and neurofibrillary tangles in Alzheimer’s disease and kuru plaque amyloid in Creutzfeldt–Jakob disease. Brain Res 541:163–166
Nilsson LN, Bales KR, DiCarlo G, Gordon MN, Morgan D, Paul SM, Potter H (2001) Alpha-1-antichymotrypsin promotes beta-sheet amyloid plaque deposition in a transgenic mouse model of Alzheimer’s disease. J Neurosci 21:1444–1451
Oakley H, Cole SL, Logan S, Maus E, Shao P, Craft J, Guillozet-Bongaarts A, Ohno M, Disterhoft J, Van Eldik L, Berry R, Vassar R (2006) Intraneuronal beta-amyloid aggregates, neurodegeneration, and neuron loss in transgenic mice with five familial Alzheimer’s disease mutations: potential factors in amyloid plaque formation. J Neurosci 26:10129–10140
Oddo S, Caccamo A, Cheng D, Jouleh B, Torp R, Laferla FM (2007) Genetically augmenting tau levels does not modulate the onset or progression of Abeta pathology in transgenic mice. J Neurochem 102:1053–1063
Oddo S, Caccamo A, Shepherd JD, Murphy MP, Golde TE, Kayed R, Metherate R, Mattson MP, Akbari Y, LaFerla FM (2003) Triple-transgenic model of Alzheimer’s disease with plaques and tangles: intracellular Abeta and synaptic dysfunction. Neuron 39:409–421
Oddo S, Caccamo A, Smith IF, Green KN, LaFerla FM (2006) A dynamic relationship between intracellular and extracellular pools of Abeta. Am J Pathol 168:184–194
Oddo S, Vasilevko V, Caccamo A, Kitazawa M, Cribbs DH, LaFerla FM (2006) Reduction of soluble Abeta and tau, but not soluble Abeta alone, ameliorates cognitive decline in transgenic mice with plaques and tangles. J Biol Chem 281:39413–39423
O’Doherty A, Ruf S, Mulligan C, Hildreth V, Errington ML, Cooke S, Sesay A, Modino S, Vanes L, Hernandez D, Linehan JM, Sharpe PT, Brandner S, Bliss TV, Henderson DJ, Nizetic D, Tybulewicz VL, Fisher EM (2005) An aneuploid mouse strain carrying human chromosome 21 with Down syndrome phenotypes. Science 309:2033–2037
Ognibene E, Middei S, Daniele S, Adriani W, Ghirardi O, Caprioli A, Laviola G (2005) Aspects of spatial memory and behavioral disinhibition in Tg2576 transgenic mice as a model of Alzheimer’s disease. Behav Brain Res 156:225–232
Ohyagi Y, Tsuruta Y, Motomura K, Miyoshi K, Kikuchi H, Iwaki T, Taniwaki T, Kira J (2007) Intraneuronal amyloid beta42 enhanced by heating but counteracted by formic acid. J Neurosci Methods 159:134–138
Oyama F, Sawamura N, Kobayashi K, Morishima-Kawashima M, Kuramochi T, Ito M, Tomita T, Maruyama K, Saido TC, Iwatsubo T, Capell A, Walter J, Grunberg J, Ueyama Y, Haass C, Ihara Y (1998) Mutant presenilin 2 transgenic mouse: effect on an age-dependent increase of amyloid beta-protein 42 in the brain. J Neurochem 71:313–322
Park IH, Hwang EM, Hong HS, Boo JH, Oh SS, Lee J, Jung MW, Bang OY, Kim SU, Mook-Jung I (2003) Lovastatin enhances Abeta production and senile plaque deposition in female Tg2576 mice. Neurobiol Aging 24:637–643
Phinney AL, Deller T, Stalder M, Calhoun ME, Frotscher M, Sommer B, Staufenbiel M, Jucker M (1999) Cerebral amyloid induces aberrant axonal sprouting and ectopic terminal formation in amyloid precursor protein transgenic mice. J Neurosci 19:8552–8559
Poirier R, Wolfer DP, Welzl H, Tracy J, Galsworthy MJ, Nitsch RM, Mohajeri MH (2006) Neuronal neprilysin overexpression is associated with attenuation of Abeta-related spatial memory deficit. Neurobiol Dis 24:475–483
Postina R, Schroeder A, Dewachter I, Bohl J, Schmitt U, Kojro E, Prinzen C, Endres K, Hiemke C, Blessing M, Flamez P, Dequenne A, Godaux E, van Leuven F, Fahrenholz F (2004) A disintegrin-metalloproteinase prevents amyloid plaque formation and hippocampal defects in an Alzheimer disease mouse model. J Clin Invest 113:1456–1464
Prasher VP, Farrer MJ, Kessling AM, Fisher EM, West RJ, Barber PC, Butler AC (1998) Molecular mapping of Alzheimer-type dementia in Down’s syndrome. Ann Neurol 43:380–383
Price DL, Martin LJ, Sisodia SS, Wagster MV, Koo EH, Walker LC, Koliatsos VE, Cork LC (1991) Aged non-human primates: an animal model of age-associated neurodegenerative disease. Brain Pathol 1:287–296
Priller C, Dewachter I, Vassallo N, Paluch S, Pace C, Kretzschmar HA, Van Leuven F, Herms J (2007) Mutant presenilin 1 alters synaptic transmission in cultured hippocampal neurons. J Biol Chem 282:1119–1127
Probst A, Gotz J, Wiederhold KH, Tolnay M, Mistl C, Jaton AL, Hong M, Ishihara T, Lee VM, Trojanowski JQ, Jakes R, Crowther RA, Spillantini MG, Burki K, Goedert M (2000) Axonopathy and amyotrophy in mice transgenic for human four-repeat tau protein. Acta Neuropathol (Berl) 99:469–481
Qi-Takahara Y, Morishima-Kawashima M, Tanimura Y, Dolios G, Hirotani N, Horikoshi Y, Kametani F, Maeda M, Saido TC, Wang R, Ihara Y (2005) Longer forms of amyloid beta protein: implications for the mechanism of intramembrane cleavage by gamma-secretase. J Neurosci 25:436–445
Radde R, Bolmont T, Kaeser SA, Coomaraswamy J, Lindau D, Stoltze L, Calhoun ME, Jaggi F, Wolburg H, Gengler S, Haass C, Ghetti B, Czech C, Holscher C, Mathews PM, Jucker M (2006) Abeta42-driven cerebral amyloidosis in transgenic mice reveals early and robust pathology. EMBO Rep 7:940–946
Redwine JM, Kosofsky B, Jacobs RE, Games D, Reilly JF, Morrison JH, Young WG, Bloom FE (2003) Dentate gyrus volume is reduced before onset of plaque formation in PDAPP mice: a magnetic resonance microscopy and stereologic analysis. Proc Natl Acad Sci USA 100:1381–1386
Reeves RH, Irving NG, Moran TH, Wohn A, Kitt C, Sisodia SS, Schmidt C, Bronson RT, Davisson MT (1995) A mouse model for Down syndrome exhibits learning and behaviour deficits. Nat Genet 11:177–184
Refolo LM, Malester B, LaFrancois J, Bryant-Thomas T, Wang R, Tint G, Sambamurti K, Duff K, Pappolla M (2000) Hypercholesterolemia accelerates the Alzheimer’s amyloid pathology in a transgenic mouse model. Neurobiol Dis 7:321–331
Refolo LM, Pappolla MA, LaFrancois J, Malester B, Schmidt SD, Thomas-Bryant T, Tint GS, Wang R, Mercken M, Petanceska SS, Duff KE (2001) A cholesterol-lowering drug reduces beta-amyloid pathology in a transgenic mouse model of Alzheimer’s disease. Neurobiol Dis 8:890–899
Regeur L, Badsberg Jensen G, Pakkenberg H, Evans SM, Pakkenberg B (1994) No global neocortical nerve cell loss in brains from patients with senile dementia of Alzheimer’s type. Neurobiol Aging 15:347–352
Robbins EM, Betensky RA, Domnitz SB, Purcell SM, Garcia-Alloza M, Greenberg C, Rebeck GW, Hyman BT, Greenberg SM, Frosch MP, Bacskai BJ (2006) Kinetics of cerebral amyloid angiopathy progression in a transgenic mouse model of Alzheimer disease. J Neurosci 26:365–371
Roberson ED, Scearce-Levie K, Palop JJ, Yan F, Cheng IH, Wu T, Gerstein H, Yu G-Q, Mucke L (2007) Reducing endogenous Tau ameliorates amyloid beta-induced deficits in an Alzheimer’s disease mouse model. Science 316:750–754
Rockenstein E, Mallory M, Mante M, Sisk A, Masliaha E (2001) Early formation of mature amyloid-beta protein deposits in a mutant APP transgenic model depends on levels of Abeta(1–42). J Neurosci Res 66:573–582
Rockenstein E, Mante M, Alford M, Adame A, Crews L, Hashimoto M, Esposito L, Mucke L, Masliah E (2005) High beta-secretase activity elicits neurodegeneration in transgenic mice despite reductions in amyloid-beta levels: implications for the treatment of Alzheimer disease. J Biol Chem 280:32957–32967
Rogaev EI, Sherrington R, Rogaeva EA, Levesque G, Ikeda M, Lyang Y, Chi H, Lin C, Holman K, Tsuda T, Mar L, Sorbi S, Nacmias B, Piacentini S, Amaducci L, Chumakov I, Cohen D, Lannfelt L, Fraser PE, Rommens JM, St George-Hyslop P (1995) Familial Alzheimer’s disease in kindreds with missense mutations in a gene on chromosome 1 related to the Alzheimer’s type 3 gene. Nature 376:775–778
Roher AE, Palmer KC, Yurewicz EC, Ball MJ, Greenberg BD (1993) Morphological and biochemical analyses of amyloid plaque core proteins purified from Alzheimer disease brain tissue. J Neurochem 61:1916–1926
Rovelet-Lecrux A, Hannequin D, Raux G, Le Meur N, Laquerrière A, Vital A, Dumanchin C, Feuillette S, Brice A, Vercelletto M, Dubas F, Frebourg T, Campion D (2006) APP locus duplication causes autosomal dominant early-onset Alzheimer disease with cerebral amyloid angiopathy. Nat Genet 38:24–26
Rush DK, Aschmies S, Merriman MC (1992) Intracerebral beta-amyloid (25–35) produces tissue damage: is it neurotoxic? Neurobiol Aging 13:591–594
Rutten BP, Van der Kolk NM, Schafer S, van Zandvoort MA, Bayer TA, Steinbusch HW, Schmitz C (2005) Age-related loss of synaptophysin immunoreactive presynaptic boutons within the hippocampus of APP751SL, PS1M146L, and APP751SL/PS1M146L transgenic mice. Am J Pathol 167:161–173
Sago H, Carlson EJ, Smith DJ, Kilbridge J, Rubin EM, Mobley WC, Epstein CJ, Huang TT (1998) Ts1Cje, a partial trisomy 16 mouse model for Down syndrome, exhibits learning and behavioral abnormalities. Proc Natl Acad Sci USA 95:6256–6261
Salehi A, Delcroix JD, Belichenko PV, Zhan K, Wu C, Valletta JS, Takimoto-Kimura R, Kleschevnikov AM, Sambamurti K, Chung PP, Xia W, Villar A, Campbell WA, Kulnane LS, Nixon RA, Lamb BT, Epstein CJ, Stokin GB, Goldstein LS, Mobley WC (2006) Increased App expression in a mouse model of Down’s syndrome disrupts NGF transport and causes cholinergic neuron degeneration. Neuron 51:29–42
SantaCruz K, Lewis J, Spires T, Paulson J, Kotilinek L, Ingelsson M, Guimaraes A, DeTure M, Ramsden M, McGowan E, Forster C, Yue M, Orne J, Janus C, Mariash A, Kuskowski M, Hyman B, Hutton M, Ashe KH (2005) Tau suppression in a neurodegenerative mouse model improves memory function. Science 309:476–481
Savonenko A, Xu GM, Melnikova T, Morton JL, Gonzales V, Wong MP, Price DL, Tang F, Markowska AL, Borchelt DR (2005) Episodic-like memory deficits in the APPswe/PS1dE9 mouse model of Alzheimer’s disease: relationships to beta-amyloid deposition and neurotransmitter abnormalities. Neurobiol Dis 18:602–617
Sawamura N, Morishima-Kawashima M, Waki H, Kobayashi K, Kuramochi T, Frosch MP, Ding K, Ito M, Kim TW, Tanzi RE, Oyama F, Tabira T, Ando S, Ihara Y (2000) Mutant presenilin 2 transgenic mice. A large increase in the levels of Abeta 42 is presumably associated with the low density membrane domain that contains decreased levels of glycerophospholipids and sphingomyelin. J Biol Chem 275:27901–27908
Schenk D, Barbour R, Dunn W, Gordon G, Grajeda H, Guido T, Hu K, Huang J, Johnson-Wood K, Khan K, Kholodenko D, Lee M, Liao Z, Lieberburg I, Motter R, Mutter L, Soriano F, Shopp G, Vasquez N, Vandevert C, Walker S, Wogulis M, Yednock T, Games D, Seubert P (1999) Immunization with amyloid-beta attenuates Alzheimer-disease-like pathology in the PDAPP mouse. Nature 400:173–177
Schindowski K, Bretteville A, Leroy K, Begard S, Brion JP, Hamdane M, Buée L (2006) Alzheimer’s disease-like tau neuropathology leads to memory deficits and loss of functional synapses in a novel mutated tau transgenic mouse without any motor deficits. Am J Pathol 169:599–616
Schmitz C, Rutten BP, Pielen A, Schäfer S, Wirths O, Tremp G, Czech C, Blanchard V, Multhaup G, Rezaie P, Korr H, Steinbusch HW, Pradier L, Bayer TA (2004) Hippocampal neuron loss exceeds amyloid plaque load in a transgenic mouse model of Alzheimer’s disease. Am J Pathol 164:1495–1502
Schwab C, Hosokawa M, McGeer PL (2004) Transgenic mice overexpressing amyloid beta protein are an incomplete model of Alzheimer disease. Exp Neurol 188:52–64
Schwarzman AL, Gregori L, Vitek MP, Lyubski S, Strittmatter WJ, Enghilde JJ, Bhasin R, Silverman J, Weisgraber KH, Coyle PK, Zagorski MG, Talafous J, Eisenberg KH, Saunders AM, Roses AD, Goldgaber D (1994) Transthyretin sequesters amyloid ß protein and prevents amyloid formation. Proc Natl Acad Sci USA 91:8368–8372
Senechal Y, Larmet Y, Dev KK (2006) Unraveling in vivo functions of amyloid precursor protein: insights from knockout and knockdown studies. Neurodegener Dis 3:134–147
Sergeant N, Bombois S, Ghestem A, Drobecq H, Kostanjevecki V, Missiaen C, Wattez A, David JP, Vanmechelen E, Sergheraert C, Delacourte A (2003) Truncated beta-amyloid peptide species in pre-clinical Alzheimer’s disease as new targets for the vaccination approach. J Neurochem 85:1581–1591
Sergeant N, Wattez A, Delacourte A (1999) Neurofibrillary degeneration in progressive supranuclear palsy and corticobasal degeneration: tau pathologies with exclusively “exon 10” isoforms. J Neurochem 72:1243–1249
Shaftel SS, Kyrkanides S, Olschowka JA, Miller JN, Johnson RE, O’Banion MK (2007) Sustained hippocampal IL-1 beta overexpression mediates chronic neuroinflammation and ameliorates Alzheimer plaque pathology. J Clin Invest 117:1595–1604
Shankar GM, Bloodgood BL, Townsend M, Walsh DM, Selkoe DJ, Sabatini BL (2005) Natural oligomers of the Alzheimer amyloid-beta protein induce reversible synapse loss by modulating an NMDA-type glutamate receptor-dependent signaling pathway. Nat Neurosci 8:79–84
Shen J, Bronson RT, Chen DF, Xia W, Selkoe DJ, Tonegawa S (1997) Skeletal and CNS defects in Presenilin-1-deficient mice. Cell 89:629–639
Sherrington S, Rogaev EI, Liang Y, Rogaeva EA, Levesque G, Ikeda M, Chi H, Lin C, Li G, Holman K, Tsuda T, Mar L, Foncin JF, Bruni AC, Montesi MP, Sorbi S, Rainero I, Pinessi L, Nee L, Chumakov I, Pollen D, Brookes A, Sanseau P, Polinsky RJ, Wasco W, Da Silva HAR, Haines JL, Pericak-Vance MA, Tanzi RE, Roses AD, Fraser PE, Rommens JM, St George-Hyslop PH (1995) Cloning of a gene bearing missense mutations in early-onset familial Alzheimer’s disease. Nature 375:754–760
Shukkur EA, Shimohata A, Akagi T, Yu W, Yamaguchi M, Murayama M, Chui D, Takeuchi T, Amano K, Subramhanya KH, Hashikawa T, Sago H, Epstein CJ, Takashima A, Yamakawa K (2006) Mitochondrial dysfunction and tau hyperphosphorylation in Ts1Cje, a mouse model for Down syndrome. Hum Mol Genet 15:2752–2762
Singer O, Marr RA, Rockenstein E, Crews L, Coufal NG, Gage FH, Verma IM, Masliah E (2005) Targeting BACE1 with siRNAs ameliorates Alzheimer disease neuropathology in a transgenic model. Nat Neurosci 8:1343–1349
Soderberg L, Bogdanovic N, Axelsson B, Winblad B, Naslund J, Tjernberg LO (2006) Analysis of single Alzheimer solid plaque cores by laser capture microscopy and nanoelectrospray/tandem mass spectrometry. Biochemistry 45:9849–9856
Spillantini MG, Murrell JR, Goedert M, Farlow MR, Klug A, Ghetti B (1998) Mutation in the tau gene in familial multiple system tauopathy with presenile dementia. Proc Natl Acad Sci USA 95:7737–7741
Spires T, Hyman BT (2005) Transgenic models of Alzheimer’s disease: learning from animals. NeuroRx 2:423–437
Spires TL, Meyer-Luehmann M, Stern EA, McLean PJ, Skoch J, Nguyen PT, Bacskai BJ, Hyman BT (2005) Dendritic spine abnormalities in amyloid precursor protein transgenic mice demonstrated by gene transfer and intravital multiphoton microscopy. J Neurosci 25:7278–7287
Spires-Jones TL, Meyer-Luehmann M, Osetek JD, Jones PB, Stern EA, Bacskai BJ, Hyman BT (2007) Impaired spine stability underlies plaque-related spine loss in an Alzheimer’s disease mouse model. Am J Pathol 171:1304–1311
Spittaels K, Van den Haute C, Van Dorpe J, Bruynseels K, Vandezande K, Laenen I, Geerts H, Mercken M, Sciot R, Van Lommel A, Loos R, Van Leuven F (1999) Prominent axonopathy in the brain and spinal cord of transgenic mice overexpressing four-repeat human tau protein. Am J Pathol 155:2153–2165
Stephan A, Laroche S, Davis S (2001) Generation of aggregated beta-amyloid in the rat hippocampus impairs synaptic transmission and plasticity and causes memory deficits. J Neurosci 21:5703–5714
Stephan A, Phillips AG (2005) A case for a non-transgenic animal model of Alzheimer’s disease. Genes Brain Behav 4:157–172
Strittmatter WJ, Saunders AM, Schmechel D, Pericak-Vance M, Enghild J, Salvesen GS, Roses AD (1993) Apolipoprotein E: high avidity binding to β-amyloid and increased frequency of type 4 allele in late-onset familial Alzheimer disease. Proc Natl Acad Sci USA 90:1977–1981
Sturchler-Pierrat C, Abramowski D, Duke M, Wiederhold KH, Mistl C, Rothacher S, Ledermann B, Bürki K, Frey P, Paganetti PA, Waridel C, Calhoun ME, Jucker M, Probst A, Staufenbiel M, Sommer B (1997) Two amyloid precursor protein transgenic mouse models with Alzheimer disease-like pathology. Proc Natl Acad Sci USA 94:13287–13292
Su Y, Ni B (1998) Selective deposition of amyloid-beta protein in the entorhinal-dentate projection of a transgenic mouse model of Alzheimer’s disease. J Neurosci Res 53:177–186
Takahashi RH, Milner TA, Li F, Nam EE, Edgar MA, Yamaguchi H, Beal MF, Xu H, Greengard P, Gouras GK (2002) Intraneuronal Alzheimer abeta42 accumulates in multivesicular bodies and is associated with synaptic pathology. Am J Pathol 161:1869–1879
Tan J, Town T, Mori T, Wu Y, Saxe M, Crawford F, Mullan M (2000) CD45 opposes beta-amyloid peptide-induced microglial activation via inhibition of p44/42 mitogen-activated protein kinase. J Neurosci Res 20:7587–7594
Tanemura K, Murayama M, Akagi T, Hashikawa T, Tominaga T, Ichikawa M, Yamaguchi H, Takashima A (2002) Neurodegeneration with tau accumulation in a transgenic mouse expressing V337M human tau. J Neurosci 22:133–141
Terai K, Iwai A, Kawabata S, Tasaki Y, Watanabe T, Miyata K, Yamaguchi T (2001) beta-amyloid deposits in transgenic mice expressing human beta-amyloid precursor protein have the same characteristics as those in Alzheimer’s disease. Neuroscience 104:299–310
Terry RD, Masliah E, Salmon DP, Butters N, DeTeresa R, Hill R, Hansen LA, Katzman R (1991) Physical basis of cognitive alterations in Alzheimer’s disease: synapse loss is the major correlate of cognitive impairment. Ann Neurol 30:572–580
Tesseur I, Van Dorpe J, Bruynseels K, Bronfman F, Sciot R, Van Lommel A, Van Leuven F (2000) Prominent axonopathy and disruption of axonal transport in transgenic mice expressing human apolipoprotein E4 in neurons of brain and spinal cord. Am J Pathol 157:1495–1510
Tesseur I, Van Dorpe J, Spittaels K, Van den Haute C, Moechars D, Van Leuven F (2000) Expression of human apolipoprotein E4 in neurons causes hyperphosphorylation of protein tau in the brains of transgenic mice. Am J Pathol 156:951–964
Thal DR, Larionov S, Abramowski D, Wiederhold KH, Van Dooren T, Yamaguchi H, Haass C, Van Leuven F, Staufenbiel M, Capetillo-Zarate E (2007) Occurrence and co-localization of amyloid beta-protein and apolipoprotein E in perivascular drainage channels of wild-type and APP-transgenic mice. Neurobiol Aging 28:1221–1230
Thal DR, Rüb U, Orantes M, Braak H (2002) Phases of A beta-deposition in the human brain and its relevance for the development of AD. Neurology 58:1791–1800
Tomidokoro Y, Ishiguro K, Harigaya Y, Matsubara E, Ikeda M, Park JM, Yasutake K, Kawarabayashi T, Okamoto K, Shoji M (2001) Abeta amyloidosis induces the initial stage of tau accumulation in APP(Sw) mice. Neurosci Lett 299:169–172
Tsai J, Grutzendler J, Duff K, Gan WB (2004) Fibrillar amyloid deposition leads to local synaptic abnormalities and breakage of neuronal branches. Nat Neurosci 7:1181–1183
Uchihara T, Duyckaerts C, He Y, Kobayashi K, Seilhean D, Amouyel P, Hauw JJ (1995) ApoE immunoreactivity and microglial cells in Alzheimer’s disease brain. Neurosci Lett 195:5–8
Uchihara T, Duyckaerts C, Lazarini F, Mokhtari K, Seilhean D, Amouyel P, Hauw J-J (1996) Inconstant apolipoprotein E (ApoE)-like immunoreactivity in amyloid beta protein deposits: Relationship with APOE genotype in aging brain and Alzheimer’s disease. Acta Neuropathol (Berl) 92:180–185
Urbanc B, Cruz L, Le R, Sanders J, Ashe KH, Duff K, Stanley HE, Irizarry MC, Hyman BT (2002) Neurotoxic effects of thioflavin S-positive amyloid deposits in transgenic mice and Alzheimer’s disease. Proc Natl Acad Sci USA 99:13990–13995
Uryu K, Laurer H, McIntosh T, Pratico D, Martinez D, Leight S, Lee VM, Trojanowski JQ (2002) Repetitive mild brain trauma accelerates Abeta deposition, lipid peroxidation, and cognitive impairment in a transgenic mouse model of Alzheimer amyloidosis. J Neurosci 22:446–454
Valla J, Schneider LE, Gonzalez-Lima F, Reiman EM (2006) Nonprogressive transgene-related callosal and hippocampal changes in PDAPP mice. Neuroreport 17:829–832
Van Dam D, D’Hooge R, Staufenbiel M, Van Ginneken C, Van Meir F, De Deyn PP (2003) Age-dependent cognitive decline in the APP23 model precedes amyloid deposition. Eur J Neurosci 17:388–396
Van Dam D, Marescau B, Engelborghs S, Cremers T, Mulder J, Staufenbiel M, De Deyn PP (2005) Analysis of cholinergic markers, biogenic amines, and amino acids in the CNS of two APP overexpression mouse models. Neurochem Int 46:409–422
van der Putten H, Wiederhold KH, Probst A, Barbieri S, Mistl C, Danner S, Kauffmann S, Hofele K, Spooren WP, Ruegg MA, Lin S, Caroni P, Sommer B, Tolnay M, Bilbe G (2000) Neuropathology in mice expressing human alpha-synuclein. J Neurosci 20:6021–6029
Van Dooren T, Dewachter I, Borghgraef P, van Leuven F (2005) Transgenic mouse models for APP processing and Alzheimer’s disease: early and late defects. Subcell Biochem 38:45–63
Van Dooren T, Muyllaert D, Borghgraef P, Cresens A, Devijver H, Van der Auwera I, Wera S, Dewachter I, Van Leuven F (2006) Neuronal or glial expression of human apolipoprotein e4 affects parenchymal and vascular amyloid pathology differentially in different brain regions of double- and triple-transgenic mice. Am J Pathol 168:245–260
Van Dorpe J, Smeijers L, Dewachter I, Nuyens D, Spittaels K, Van Den Haute C, Mercken M, Moechars D, Laenen I, Kuiperi C, Bruynseels K, Tesseur I, Loos R, Vanderstichele H, Checler F, Sciot R, Van Leuven F (2000) Prominent cerebral amyloid angiopathy in transgenic mice overexpressing the London mutant of human APP in neurons. Am J Pathol 157:1283–1298
Van Uden E, Mallory M, Veinbergs I, Alford M, Rockenstein E, Masliah E (2002) Increased extracellular amyloid deposition and neurodegeneration in human amyloid precursor protein transgenic mice deficient in receptor-associated protein. J Neurosci 22:9298–9304
Vassar R, Citron M (2000) Abeta-generating enzymes: recent advances in beta- and gamma-secretase research. Neuron 27:419–422
Verret L, Jankowsky JL, Xu GM, Borchelt DR, Rampon C (2007) Alzheimer’s-type amyloidosis in transgenic mice impairs survival of newborn neurons derived from adult hippocampal neurogenesis. J Neurosci 27:6771–6780
Walker LC, Callahan MJ, Bian F, Durham RA, Roher AE, Lipinski WJ (2002) Exogenous induction of cerebral beta-amyloidosis in betaAPP-transgenic mice. Peptides 23:1241–1247
Walsh DM, Klyubin I, Fadeeva JV, Cullen WK, Anwyl R, Wolfe MS, Rowan MJ, Selkoe DJ (2002) Naturally secreted oligomers of amyloid beta protein potently inhibit hippocampal long-term potentiation in vivo. Nature 416:535–539
Walsh DM, Klyubin I, Shankar GM, Townsend M, Fadeeva JV, Betts V, Podlisny MB, Cleary JP, Ashe KH, Rowan MJ, Selkoe DJ (2005) The role of cell-derived oligomers of Abeta in Alzheimer’s disease and avenues for therapeutic intervention. Biochem Soc Trans 33:1087–1090
Walsh DM, Selkoe DJ (2007) A beta oligomers - a decade of discovery. J Neurochem 101:1172–1184
Wang J, Tanila H, Puolivali J, Kadish I, van Groen T (2003) Gender differences in the amount and deposition of amyloid beta in APPswe and PS1 double transgenic mice. Neurobiol Dis 14:318–327
Wegiel J, Imaki H, Wang KC, Rubenstein R (2004) Cells of monocyte/microglial lineage are involved in both microvessel amyloidosis and fibrillar plaque formation in APPsw tg mice. Brain Res 1022:19–29
Wegiel J, Kuchna I, Nowicki K, Frackowiak J, Mazur-Kolecka B, Imaki H, Mehta PD, Silverman WP, Reisberg B, Deleon M, Wisniewski T, Pirttilla T, Frey H, Lehtimaki T, Kivimaki T, Visser FE, Kamphorst W, Potempska A, Bolton D, Currie JR, Miller DL (2007) Intraneuronal Abeta immunoreactivity is not a predictor of brain amyloidosis-beta or neurofibrillary degeneration. Acta Neuropathol (Berl) 113:389–402
Wegiel J, Wang KC, Imaki H, Rubenstein R, Wronska A, Osuchowski M, Lipinski WJ, Walker LC, LeVine H (2001) The role of microglial cells and astrocytes in fibrillar plaque evolution in transgenic APP(SW) mice. Neurobiol Aging 22:49–61
Weiss C, Venkatasubramanian PN, Aguado AS, Power JM, Tom BC, Li L, Chen KS, Disterhoft JF, Wyrwicz AM (2002) Impaired eyeblink conditioning and decreased hippocampal volume in PDAPP V717F mice. Neurobiol Dis 11:425–433
Weller RO, Nicoll JA (2003) Cerebral amyloid angiopathy: pathogenesis and effects on the ageing and Alzheimer brain. Neurol Res 25:611–616
Westerman MA, Cooper-Blacketer D, Mariash A, Kotilinek L, Kawarabayashi T, Younkin LH, Carlson GA, Younkin SG, Ashe KH (2002) The relationship between Abeta and memory in the Tg2576 mouse model of Alzheimer’s disease. J Neurosci 22:1858–1867
Whitehouse PJ, Price DL, Clark AW, Coyle JT, DeLong MR (1981) Alzheimer disease: evidence for selective loss of cholinergic neurons in the nucleus basalis. Ann Neurol 13:243–248
Willem M, Dewachter I, Smyth N, Van Dooren T, Borghgraef P, Haass C, Van Leuven F (2004) beta-site amyloid precursor protein cleaving enzyme 1 increases amyloid deposition in brain parenchyma but reduces cerebrovascular amyloid angiopathy in aging BACE x APP[V717I] double-transgenic mice. Am J Pathol 165:1621–1631
Wirak DO, Bayney R, Ramambhadran TV, Fracasso RP, Hart JT, Hauer PE, Hsiau P, Pekar SK, Scangos GA, Trapp BD, Unterbeck AJ (1991) Deposits of amyloid ß protein in the central nervous system of transgenic mice. Science 253:323–325
Wirths O, Breyhan H, Schäfer S, Roth C, Bayer TA (2007) Deficits in working memory and motor performance in the APP/PS1ki mouse model for Alzheimer’s disease. Neurobiol Aging doi:10.1016/j.neurobiolaging.2006.12.004
Wirths O, Multhaup G, Bayer TA (2004) A modified beta-amyloid hypothesis: intraneuronal accumulation of the beta-amyloid peptide—the first step of a fatal cascade. J Neurochem 91:513–520
Wirths O, Multhaup G, Czech C, Blanchard V, Moussaoui S, Tremp G, Pradier L, Beyreuther K, Bayer TA (2001) Intraneuronal Abeta accumulation precedes plaque formation in beta- amyloid precursor protein and presenilin-1 double-transgenic mice. Neurosci Lett 306:116–120
Wirths O, Weis J, Kayed R, Saido TC, Bayer TA (2007) Age-dependent axonal degeneration in an Alzheimer mouse model. Neurobiol Aging 28(11):1689–99
Wirths O, Weis J, Szczygielski J, Multhaup G, Bayer TA (2006) Axonopathy in an APP/PS1 transgenic mouse model of Alzheimer’s disease. Acta Neuropathol (Berl) 111:312–329
Wisniewski HM, Frackowiak J, Mazur-Kolecka B (1995) In vitro production of ß-amyloid in smooth muscle cells isolated from amyloid angiopathy-affected vessels. Neurosci Lett 183:120–123
Wolf S, Kronenberg G, Lehmann K, Blankenship A, Overall R, Staufenbiel M, Kempermann G (2006) Cognitive and physical activity differently modulate disease progression in the amyloid precursor protein (APP)-23 model of Alzheimer’s disease. Biol Psychiatry 60:1314–1323
Wolfe MS (2006) The gamma-secretase complex: membrane-embedded proteolytic ensemble. Biochemistry 45:7931–7939
Wong CW, Quaranta V, Glenner GG (1985) Neuritic plaques and cerebrovascular amyloid in Alzheimer disease are antigenically related. Proc Natl Acad Sci USA 82:8729–8732
Wong TP, Debeir T, Duff K, Cuello AC (1999) Reorganization of cholinergic terminals in the cerebral cortex and hippocampus in transgenic mice carrying mutated presenilin-1 and amyloid precursor protein transgenes. J Neurosci 19:2706–2716
Wyss-Coray T, Lin C, Yan F, Yu GQ, Rohde M, McConlogue L, Masliah E, Mucke L (2001) TGF-beta1 promotes microglial amyloid-beta clearance and reduces plaque burden in transgenic mice. Nat Med 7:612–618
Wyss-Coray T, Masliah E, Mallory M, McConlogue L, Johnson-Wood K, Lin C, Mucke L (1997) Amyloidogenic role of cytokine TGF-beta1 in transgenic mice and Alzheimer’s disease. Nature 389:603–606
Wyss-Coray T, Yan F, Hsiu-Ti Lin A, Lambris JD, Alexander JJ, Quigg RJ, Masliah E (2002) Prominent neurodegeneration and increased plaque formation in complement-inhibited Alzheimer’s mice. Proc Natl Acad Sci USA 99:10837–10842
Xiang Z, Ho L, Yemul S, Zhao Z, Qing W, Pompl P, Kelley K, Dang A, Teplow D, Pasinetti GM (2002) Cyclooxygenase-2 promotes amyloid plaque deposition in a mouse model of Alzheimer’s disease neuropathology. Gene Exp 10:271–278
Yang F, Uéda K, Chen P, Ashe KH, Cole GM (2000) Plaque-associated alpha-synuclein (NACP) pathology in aged transgenic mice expressing amyloid precursor protein. Brain Res 853:381–383
Yankner BA (1996) Mechanisms of neuronal degeneration in Alzheimer’s disease. Neuron 16:921–932
Zelcer N, Khanlou N, Clare R, Jiang Q, Reed-Geaghan EG, Landreth GE, Vinters HV, Tontonoz P (2007) Attenuation of neuroinflammation and Alzheimer’s disease pathology by liver x receptors. Proc Natl Acad Sci USA 104:10601–10606
Zerbinatti CV, Wahrle SE, Kim H, Cam JA, Bales KR, Paul SM, Holtzman DM, Bu G (2006) Apolipoprotein E and low-density lipoprotein receptor-related protein facilitate intraneuronal Abeta 42 accumulation in amyloid model mice. J Biol Chem 281:36180–36186
Zhang C, McNeil E, Dressler L, Siman R (2007) Long-lasting impairment in hippocampal neurogenesis associated with amyloid deposition in a knock-in mouse model of familial Alzheimer’s disease. Exp Neurol 204:77–87
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License ( https://creativecommons.org/licenses/by-nc/2.0 ), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Duyckaerts, C., Potier, MC. & Delatour, B. Alzheimer disease models and human neuropathology: similarities and differences. Acta Neuropathol 115, 5–38 (2008). https://doi.org/10.1007/s00401-007-0312-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-007-0312-8