Abstract
Purpose
To assess the association between three different a priori dietary patterns adherence (17-item energy reduced-Mediterranean Diet (MedDiet), Trichopoulou-MedDiet and Dietary Approach to Stop Hypertension (DASH)), as well as the Protein Diet Score and kidney function decline after one year of follow-up in elderly individuals with overweight/obesity and metabolic syndrome (MetS).
Methods
We prospectively analyzed 5675 participants (55–75 years) from the PREDIMED-Plus study. At baseline and at one year, we evaluated the creatinine-based estimated glomerular filtration rate (eGFR) and food-frequency questionnaires-derived dietary scores. Associations between four categories (decrease/maintenance and tertiles of increase) of each dietary pattern and changes in eGFR (ml/min/1.73m2) or ≥ 10% eGFR decline were assessed by fitting multivariable linear or logistic regression models, as appropriate.
Results
Participants in the highest tertile of increase in 17-item erMedDiet Score showed higher upward changes in eGFR (β: 1.87 ml/min/1.73m2; 95% CI: 1.00–2.73) and had lower odds of ≥ 10% eGFR decline (OR: 0.62; 95% CI: 0.47–0.82) compared to individuals in the decrease/maintenance category, while Trichopoulou-MedDiet and DASH Scores were not associated with any renal outcomes. Those in the highest tertile of increase in Protein Diet Score had greater downward changes in eGFR (β: − 0.87 ml/min/1.73m2; 95% CI: − 1.73 to − 0.01) and 32% higher odds of eGFR decline (OR: 1.32; 95% CI: 1.00–1.75).
Conclusions
Among elderly individuals with overweight/obesity and MetS, only higher upward change in the 17-item erMedDiet score adherence was associated with better kidney function after one year. However, increasing Protein Diet Score appeared to have an adverse impact on kidney health. Trial Registration Number: ISRCTN89898870 (Data of registration: 2014).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic Kidney Disease (CKD) is an increasing global public health problem, which affects about 9.1% of the worldwide population and 35% of those over 70 years [1]. CKD is characterized by abnormalities in kidney structure and a decline in its function [2], often accompanied by several comorbidities, decreased quality of life and premature mortality [1,2,3]. In fact, this heterogeneous condition is accelerated at older ages when comorbidities such as obesity, diabetes, hypertension and/or cardiovascular disease are present [1, 4]. As this disease involves a huge health and economic burden, preserving renal function, especially in old people, it is essential to ensure the well-being and reduce adverse health outcomes [1]. Accordingly, effective strategies to deal with the spread of CKD and its harmful consequences are urgently needed.
Among the lifestyle risk factors of CKD, diet may play an important role as potential modulator of kidney function decline and CKD progression [5]. However, most of the investigations have been predominantly focused on single nutrients [6, 7] or food groups [5, 8] instead of dietary patterns, hence it is likely to not exhibit the synergistic effect between its dietary components. Thus, considering that meals are composed by a combination of foods and nutrients, analysis of diet as a whole could be a more all-inclusive approach not only to assess dietary exposure but also to examine its relationship with kidney health [3, 9, 10].
In this regard, results of a recent meta-analysis of prospective studies reported that a healthy dietary pattern characterized by a high consumption of plant-based food was associated with reduced incidence of CKD or albuminuria, but not with glomerular filtration rate (GFR) decline [11]. When studies are focused on particular dietary patterns such as the Mediterranean diet (MedDiet) or the Dietary Approach to Stop Hypertension (DASH), which are the most commonly investigated a priori dietary scores in the context of CKD [3, 12], there are inconsistent results. Whereas some studies reported a decrease in GFR decline [13], microalbuminuria or lower CKD risk [14], others failed to demonstrate any relationship between these dietary patterns and kidney outcomes [15, 16]. It is noteworthy that most of these epidemiologic studies were conducted in healthy young or middle-aged individuals, instead of high-risk participants such as elders or people with cardiometabolic comorbidities.
Furthermore, MedDiet and DASH diet are characterized by a high plant protein content and, even though protein intake has been previously associated with kidney function deterioration [17], this potential harmful effect could depend on the protein source. Accordingly, it may be of interest to investigate the association between not only the quantity but also the quality of dietary protein and renal function using specific tools as the recently developed Protein Diet Score [18].
Consequently, in view of the above, further research is required to clarify whether specific healthy dietary patterns could preserve kidney function and even prevent its decline in elderly population with underlying comorbid conditions. Therefore, the main aim of the present study was to prospectively evaluate the association between changes towards an increase in the adherence to three a priori dietary patterns (17-item erMedDiet Score, Trichopoulou-MedDiet and DASH) and kidney function decline after 1 year of follow-up in a large Spanish cohort of middle-aged individuals with overweight/obesity and metabolic syndrome (MetS). Secondarily, we evaluated the association between changes in the Protein Diet Score and kidney function.
Material and methods
Study design and participants
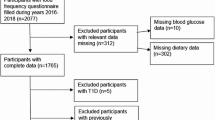
In the present study, data was analyzed using an observational prospective design conducted within the framework of the Prevención con Dieta Mediterránea (PREDIMED)-Plus trial, which included 6874 older adults enrolled between 2013 and 2016 by 23 Spanish centers working in collaboration with primary care clinics. The study design and protocol have been described in detail elsewhere [19], and are available at http://www.predimedplus.com. In brief, the PREDIMED-Plus study is an ongoing, 8-year, parallel-group, randomized and controlled clinical trial which combines dietary and physical activity intervention with behavioral support for primary cardiovascular prevention. Eligible participants were men (55–75 years) and women (60–75 years) with overweight or obesity (BMI ≥ 27 kg/m2 and < 40 kg/m2) and free from cardiovascular disease who satisfied at least 3 criteria for the MetS definition [20]. More specific details of inclusion/exclusion criteria have been previously reported [19]. All participants provided written informed consent and the Institutional Review Boards of each participating center approved the final study protocol and procedures, which followed the standards of the Declaration of Helsinki. The trial was registered in 2014 at the International Standard Randomized Controlled Trial registry (https://www.isrctn.com/ISRCTN89898870).
For the current analysis, we excluded 777 participants who did not complete food frequency questionnaires (FFQ) at baseline and after a 1 year of follow-up; 160 participants with extreme total energy intake (women < 500 and > 3500 kcal/day, and men < 800 and > 4000 kcal/day) [21]; and 262 participants with missing creatinine data at baseline and after 1 year of follow-up. Consequently, the final sample for the present study was 5675 participants. Supplementary table S3 depicts the baseline characteristics by included and excluded participants.
Dietary assessment
Dietary intake was evaluated at baseline and yearly during the follow-up using a 143-item semi-quantitative FFQ [22]. Trained dieticians asked the participants about their frequency consumption of each specific item during the preceding year in a face-to-face interview. There were nine possible answers ranging from never or almost never to more than six times per day. Each item answer was collected in standard portion sizes and then transformed to g/day. Total daily intake of energy, nutrients and food groups were estimated using Spanish food composition tables [23, 24].
Moreover, in order to assess the degree of adherence to an energy reduced-MedDiet of each participant, a recently validated 17-item test (17-items erMedDiet Score) [25] was filled in every visit. This questionnaire specifically asked about the frequency consumption of extra virgin olive oil, other fats (butter, margarine, or cream), fruits and fruit juices, vegetables, meat, legumes, fish, nuts, pastries, “sofrito”, non-caloric artificial sweeteners, refined grains, wholegrains, and wine. Each item of the questionnaire is scored with 1 or 0 points, when the criterion is met or not met respectively, ranging the overall score from 0 to 17 points, with 0 meaning no adherence and 17 meaning maximum adherence. Hence, this pre-defined questionnaire has the remarkable characteristic of being based on the scientific knowledge on what is a health level of intake and not on the study population distribution, unlike other indices that are calculated based on specific cut-off points (mean or quintiles) of the population included for each item of the score.
We also constructed the Trichopoulou-MedDiet Score and the DASH Score following previous detailed description in the scientific literature [26, 27]. Briefly, Trichopoulou-MedDiet Score, one of the most used MedDiet scores in nutritional epidemiological studies, is comprised of nine components and a sex-specific cutoff point, based on the median of each item consumption (g/day), is established. Components which consumption is highly recommended were 1 point scored when their consumption was equal to or greater than the median (vegetables, fruits and nuts, legumes, cereals and potatoes, fish and others, monounsaturated: saturated ratio) and zero otherwise. Non favourable components were scored with 0 when their intake was equal to or greater than the median (meat and meat products, dairy) and one otherwise. With regard to alcohol, it has been recommended a moderate consumption; therefore, the consumption of 10–50 g/day in men and 5–25 g/day in women was scored with 1 point. Alcohol consumption above or below these limits was assigned a score of 0. The total final score ranged from 0 to 9 points. For DASH Score, study population was classified into quintiles according to each score item (g/day). A progressive score from 1 to 5 was given to each quintile in case of highly recommended foods (fruits, vegetables, legumes and nuts, low-fat dairy, and whole grains). Nevertheless, an inverse score was assigned to components quintiles whose consumption is not recommended (sodium, red and processed meats, and sweetened-sugar beverages). Thus, the total score after summing up every single component ranged from 8 to 40 for DASH score.
We also included the pre-defined Protein Diet Score in our analyses [18]. The study population was divided in 11 strata according to total protein intake (E%) and in another 11 strata according to plant to animal protein ratio. Subjects in the highest stratum received 10 points and those in the lowest stratum received 0 points. Therefore, the overall score could range from 0 to 20 points, with 0 meaning the lowest total protein intake (E%) and lowest plant to animal protein ratio, and 20 meaning the highest total protein intake (E%) and the highest plant to animal protein ratio. Each component of the score was also considered separately.
Ascertainment of renal function
For the present study, we considered as main outcomes of interest, absolute changes in eGFR and ≥ 10% eGFR decline after 1 year of follow-up. For this purpose, eGFR was estimated indirectly from serum creatinine (SCr) at baseline and after a 1 year of follow-up using the Chronic Kidney Disease Epidemiology Collaboration equation for Caucasian individuals (CKD-EPI) [28]. Fasting blood samples were collected and SCr levels were determined by the enzymatic creatinine assay method (coefficient of variation < 4%). Decline in eGFR (≥ 10%) was estimated using the following formula: (one-year eGFR− baseline eGFR)/(baseline eGFR)*100. Participants were categorized in those with a ≥ 10% eGFR decline and those with < 10% eGFR decline [29].
Assessment of other covariates
At baseline and after 1 year of follow-up, socio-demographic (age, sex, educational level) and lifestyle (physical activity, smoking habits) information, medication use and history of disease were collected by PREDIMED-Plus-trained staff through several questionnaires or reviewing medical records. Anthropometric measurements as weight, height or waist circumference were assessed following the study protocol. Body Mass Index (BMI) was calculated by dividing the weight (in kg) by the square of the height (in meters). For weight change after 1 year of follow-up, we constructed a new covariate by subtracting weight at 1 year minus weight at baseline. Resting blood pressure was measured in triplicate by an automated digital device (Omron-HEM297705C).
Statistical analyses
Data were analyzed using the available PREDIMED-Plus database updated to December 2020. Participants were categorized in four categories according to changes in dietary pattern scores after 1 year of follow-up: decrease or maintenance of changes and tertiles of increasing changes. Baseline characteristics of the study population were compared among categories of dietary patterns changes by using one-way ANOVA and Chi-square, as appropriate. Values were presented as percentages and numbers for categorical variables and means ± standard deviations for continuous variables.
Multivariable linear regression models were fitted to evaluate associations between categories of changes in dietary patterns and changes in eGFR (ml/min/1.73m2); results were expressed as β-coefficients and their 95% confidence interval (CI). Besides, logistic regression models were used to assess the association between categories of changes in dietary patterns and eGFR decline (≥ 10%); results were expressed as odds ratios (OR) and their 95% CI. In both regression models, the first category (decrease or maintenance of changes) was used as reference. Changes in dietary pattern exposures were also modeled as continuous per 1-point increase. All regression models were adjusted for several potential confounders: Model 1 was adjusted for sex and age; model 2 was additionally adjusted for BMI (kg/m2), smoking habits (never, current or former smoker), educational level (primary, secondary education or graduate), leisure time physical activity (METS/min/week), diabetes prevalence (yes/no), hypertension prevalence (yes/no), hypercholesterolemia prevalence (yes/no), center (categorized into quartiles by number of participants), intervention group and energy intake (kcal/day); and model 3, additionally adjusted for each baseline dietary pattern score and 1-year changes in body weight. All linear regression models were further adjusted for baseline eGFR (ml/min/1.73m2).
We used the robust variance estimators to account for intra-cluster correlations in all regression models. The p for linear trend was calculated assigning the median value of each category and modelling it as a continuous variable.
We also evaluated whether the associations observed between categories of changes in dietary pattern scores and changes in eGFR could be modified by sex, age, diabetes, and intervention group. Interaction was tested with the likelihood ratio tests, which involved comparing models with and without cross-product terms.
An additional analysis was included to assess the importance of each individual item of the 17-item erMedDiet Score on changes in eGFR and ≥ 10% decline in eGFR. Following a previous described method [30], each item was consecutively removed one at a time from the total score. The exclusion of each item reduced the total score to 16 items. Therefore, to assure comparability with the original score, which could have a maximum punctuation of 17, we multiplied the estimated β-coefficients and the logarithm of the estimated odds ratios by 16/17. The latest was back-transformed to the original scale through exponentiation.
Statistical analyses were performed with Stata/SE software, version 14.0 (StataCorp, College Station, TX). All tests were considered significant at a 2-tailed p value < 0.05.
Results
Baseline characteristics of the study population according to 1-year changes categories (decrease/maintenance vs. tertile 3) of 17-item erMedDiet, Trichopoulou-MedDiet and DASH dietary pattern scores are presented in Table 1. Participants located in the highest tertile of increase in the 17-item erMedDiet score were less likely to be older, women and physically active, had less prevalence of diabetes, had more energy intake and consumed less proteins. Participants with higher increase in the Trichopoulou-MedDiet score adherence were more likely to exercise, had higher hypertension prevalence, less energy intake and consumed more proteins. Those individuals with higher increase in the DASH score were younger and mainly men. They had a higher energy intake and consumed less protein. Furthermore, differences in smoking status and education level were also observed. Regarding baseline scores of each dietary pattern, participants who most changed their adherence to the corresponding dietary pattern after one year of follow-up showed lower points at the beginning of the study. Baseline characteristics of the population under study according to the four categories of changes of each dietary pattern and Protein Diet Score are displayed in Supplementary Tables 1 and 2.
The mean eGFR of the study population at baseline was 84.2 mL/min/1.73 m2. Over the first year of follow-up, the mean eGFR change was -0.94 mL/min/1.73 m2. Multivariable linear regression analyses for the associations between categories of changes in the adherence to the different dietary patterns and changes in eGFR at one year are depicted in Table 2. In the fully adjusted model, one year 17-item erMedDiet score changes were directly associated with eGFR changes (β: 0.78; 95% CI: 0.12–1.44 for T1 vs. decrease/maintenance; β: 1.06; 95% CI: 0.31–1.82 for T2 vs. decrease/maintenance; and β: 1.87; 95% CI: 1.00–2.73 for T3 vs. decrease/maintenance). Similar results were observed when we modeled this dietary pattern as continuous variable (β: 0.23; 95% CI: 0.13–0.32 for each 1-point increment). Changes in the Trichopoulou-MedDiet and DASH scores were not associated with eGFR changes neither when analyzed as categories nor in continuous manner, in any of the adjusted models.
No statistically significant interactions were observed between sex, age, diabetes status or intervention group and the changes in the dietary patterns scores mentioned above in relation to changes in eGFR (data not shown).
Table 3 shows the association between changes in dietary patterns and ORs of ≥ 10% eGFR decline after 1 year of follow-up. Changes in the 17-item erMedDiet score showed a significant graded association with eGFR decline in the fully adjusted model (OR: 0.75; 95% CI: 0.61–0.92 for T1 of increase vs. decrease/maintenance; OR: 0.68; 95% CI: 0.53–0.87 for T2 of increase vs. decrease/maintenance; OR: 0.62; 95% CI: 0.47–0.82, for T3 of increase vs. decrease/maintenance). No significantly associations were observed between changes in the Trichopoulou-MedDiet neither in the DASH score and ≥ 10% eGFR decline after 1 year. When these dietary patterns were modeled as continuous variables, similar associations were obtained, being only the 17-item erMedDiet score associated with lower odds of ≥ 10% eGFR decline (OR: 0.95; 95%: CI 0.92–0.98 for 1-point increment). Similar results were observed after excluding 378 participants with CKD at baseline from the main analysis, which are depicted in Supplementary Table 4.
Figure 1 displays the association between changes in Protein Diet score and eGFR changes and ≥ 10% eGFR decline after one year of follow-up. We observed a significant association between this score and both renal outcomes. Compared to participants without changes or with a decrease in the Protein Diet score, those in the highest tertile of increase had greater downward changes in eGFR (β: − 0.87; 95% CI: − 1.73 to − 0.01) and a 32% higher odds of eGFR decline (OR: 1.32; 95% CI: 1.00–1.75) in the fully adjusted model. When each component of this score was examined separately, only the change in total protein intake (E%) score presented a significant inverse association with eGFR changes (β: − 1.04; 95% CI: − 1.88 to − 0.21; for T3 vs. decrease/maintenance) in the multivariate adjusted model.
Associations between changes in Protein Diet score and kidney function. A Multivariable adjusted β-coefficients and 95%CI for changes in eGFR (ml/min/1.73m2) across categories of changes to the protein diet score adherence after 1 year of follow-up. B Multivariable adjusted odd ratios and 95%CI for eGFR decline (> 10%) across categories of changes to the protein diet score adherence after 1 year of follow-up. Decr/Maint, Decrease/Maintenance; eGFR, Estimated glomerular filtration rate; Decr/Maint, Decrease/Maintenance. aMean changes in eGFR (ml/min/1.73m2): Decr/Maint (− 0.71; − 1.02 to − 0.41), tertile 1 of changes (− 1.05; − 1.52 to − 0.57), tertile 2 of changes (− 1.31; − 1.96 to − 0.65), tertile 3 of changes (− 1.61; − 2.38 to − 0.84). bPercentage of participants with eGFR decline(> 10%): Decr/Maint (n = 507; % = 15.54), tertile 1 of changes (n = 196; % = 16.27), tertile 2 of changes (n = 106; % = 15.57), tertile 3 of changes (n = 98; % = 18.60). All models were adjusted for baseline eGFR (except for eGFR decline > 10%), sex, age, BMI, smoking habits (never, current or former smoker), educational level (primary, secondary education, graduate), leisure time physical activity (METS/min/week), diabetes prevalence (yes/no), hypertension prevalence (yes/no), hypercholesterolemia prevalence (yes/no), center (categorized into quartiles by number of participants), intervention group and energy intake (kcal/day) and 1-year changes in body weight
Table 4 shows the additional analysis after the alternatively removal of each individual component of the 17-item erMedDiet score modeled as continuous in the regression models. The results remained consistent with those from the main analyses for both eGFR changes and ≥ 10% eGFR decline. We observed that the greatest contributors to the association between changes in 17-item erMedDiet score and eGFR changes after 1 year of follow-up were the consumption of ≥ 2 units/day of vegetables, ≥ 3 servings/week of legumes (13% reduction in the association after removing these items from the total score); the use of sofrito ≥ 2 times/week (17% reduction) and moderate consumption of wine (22% reduction). Similar results were obtained when we performed the same removing items procedures for ≥ 10% eGFR decline as an outcome variable.
Discussion
To the best of our knowledge, this is the first prospective study examining the association between different a priori defined dietary patterns adherence and kidney function in elderly individuals with overweight/obesity and MetS. We found that a higher upward change in the adherence to a 17-item erMedDiet score was associated with improvements in eGFR changes and with 38% lower odds of eGFR decline after controlling for potential confounders. However, changes in the adherence to the Trichopoulou-MedDiet and DASH Score were not associated with changes in eGFR, neither with a ≥ 10% eGFR decline. Regarding the Protein Diet Score, higher changes toward a greater adherence were associated with a worsening of eGFR.
Previous studies have reported that MedDiet adherence is inversely associated with eGFR decline [31], incidence of CKD [32, 33], and risk of end-stage of kidney disease (ESKD) [34] in populations of youth to middle-age with apparently preserved eGFR. Our results regarding the pre-specified 17-item Med Diet score are in line with two prior randomized clinical trials, the PREDIMED in Spain [35] and the DIRECT [36] in Israel, in which MedDiet improved levels of eGFR in participants with overweight/obesity, whereas the data-driven by the Trichopoulou score not. In the Lifelines cohort study conducted on apparently healthy middle-aged adults of Netherlands, an inverse association between the MedDiet adherence according to Trichopoulou and eGFR decline was reported in men, but not in women [31]. Besides, in the Uppsala Longitudinal Study of Adult Men cohort (ULSAM), conducted in middle-age men, it was observed that a greater adherence to the MedDiet according Trichopoulou was significantly associated with lower odds of having CKD when it was estimated by cystatine C, but not by creatinine estimation [33]. In our study, the analysis was performed in the whole study population because we did not observe any interaction with sex. However, considering that previous evidence has reported significant associations in men but not in women, future studies stratifying by sex are needed to shed new light on whether the MedDiet could have a different role in kidney function in men than women. In the Northern Manhattan Study (NOMAS), a prospective multiethnic cohort conducted in 3298 middle-age participants with no previous history of stroke, no significant association were observed across their four categories of Trichopoulou-MedDiet adherence and eGFR decline, neither change in eGFR [15]. The apparent disagreement between 17-MedDiet and Trichopoulou-MedDiet Scores in our study reveals the disparities between both tools concerning the items included. The inclusion of more food groups into the 17-MedDiet Score screener tool maybe would imply a more representative assessment of diet to observe changes in eGFR. Additionally, scoring criteria are quite different; while the 17-item erMedDiet uses absolute values derived from a predefined questionnaire, the Trichopoulou-MedDiet score is assigned according to gender-specific medians of food group consumption of the study population [26]. The later may hinder comparability with other publications where particular cultural and dietary habits are present. Likewise, these issues may explain the controversial results observed between both MedDiet scoring methods in our sample. Of note, this is the first study so far analyzing the association between the adherence to the MedDiet, using the 17-MedDiet score screener tool, and renal function. Further studies, considering both scores (Trichopoulou-MedDiet and 17-item erMedDiet) are needed to clarify and strengthen our results.
Although the DASH diet has been formerly associated with better kidney function outcomes such as rapid eGFR decline [13] or CKD incidence [37], a recent meta-analysis did not confirm such associations [11], which is partly agreed with our findings. In fact, in the Healthy Aging in Neighborhoods of Diversity across the Life Span (HANDLS) study [16], the authors not only reported a lack of association between this dietary pattern and eGFR decline or incident CKD but also even greater risk of rapid kidney function decline among the group of middle-age individuals with hypertension after 5 years of follow-up. Whether a plant-based diet like the DASH, which is apparently similar to the MedDiet, is not associated with a better kidney function, despite being protective against hypertension [38], which in turn is a well-known risk factor for kidney disease, needs to be further investigated.
The underlying biological mechanisms whereby changes toward a greater adherence to a plant-based diet as the MedDiet, but not the DASH diet, could preserve or improve kidney function are not entirely clear. When we analyzed individual components of the 17-item erMedDiet Score, vegetables, legumes, wine and the traditional Mediterranean tomato and olive oil sauce (sofrito) were associated with better renal function. These foods represent the main differences between the two dietary aforementioned patterns and are rich in some beneficial nutrients such as fiber, antioxidants and anti-inflammatory compounds that may play a protective role by reducing the levels of inflammatory biomarkers, improving endothelial function, plasma lipid profiles and insulin resistance, lowering high blood pressure, and preserving a low glycemic index and load [6, 39,40,41,42,43,44,45].
Both Mediterranean diet and DASH, which has been usually associated with better markers of kidney function, are rich in plant-protein. Despite some evidence has raised concerns about the detrimental effects of high-protein intake on kidney damage [46], it seems that besides the quantity, the source of protein intake might be considered when analyzing these associations. Likewise, its long-term effects in vulnerable elderly individuals are still unknown. Our results regarding the Protein Diet Score are not in line with those of a previous cross-sectional study based on three cohort [18], NQplus, Lifelines, and the Young Finns Study, where a positive association between the protein score and eGFR was repy, by assuming that participants with renal dysfunction have already changed their protein intake [18]. Besides, our results from each component of the Protein Diet Score suggest that increased protein total intake could be the major drive for the deleterious renal association observed. Further research with long duration is warranted using this score to clarify its potential implication in kidney function and damage.
Limitations of the current study must be considered when interpreting the results. Firstly, eGFR measurement was estimated using SCr, as in most of epidemiologic studies, but other more optimal biomarkers exist. However, the procedures of those biomarkers are expensive, time consuming and difficult to be used in large population studies. Secondly, although the FFQ is an appropriate tool to assess usual dietary intake when it is carefully administered by trained staff, recall bias could not be ruled out. Thirdly, this study was conducted in elderly Mediterranean individuals with overweight/obesity and MetS; consequently, our findings cannot be extrapolated to other study populations. Fourthly, PREDIMED-Plus study is a randomized controlled trial; therefore, the lifestyle advice in turn could affect our findings. Nevertheless, we adjusted our analyses by the intervention group. Finally, SCr has a well-known biological variability and as we only measured it at baseline and 1 year (at short term), some degree of misclassification could be present. The present study also has notable strengths, which deserve to be mentioned, such as its prospective design, the relatively large sample size and the inclusion of different dietary patterns in main analyses. Moreover, we adjusted our models for a substantial number of covariates which could affect renal function, to try to control for potential bias. Even so, as in any observational study, we cannot rule out the possibility of residual or unmeasured confounding.
Conclusion
In summary, changes towards a greater adherence in the 17-item erMedDiet score after 1 year of follow-up were associated with better eGFR and lower odds of ≥ 10% eGFR decline in an elderly population with MetS. Not significant results were observed with regards to the Trichopoulou-MedDiet and DASH Score. These discrepancies could be partially explained by their differences in the calculation of the score, which in contrast to the 17-item erMedDiet depends on cut-off points based on the study population distribution of each item. Future studies in the renal function field should consider including the 17-item erMedDiet score in their analyses to clarify and strengthen our findings. Besides, the Protein Diet Score was associated with changes towards a worse eGFR and higher odds of ≥ 10% eGFR decline. Our results provide further insights to the evidence concerning a priori dietary patterns associated with kidney function in populations at high cardiovascular risk and reinforce the role of a plant-protein-based healthy diet in preserving renal function, particularly among this vulnerable population group. Therefore, improving dietary habits following a MedDiet could lead to a better kidney function, and even it could be considered an appropriate and safe preventive strategy against the onset or progression of CKD. However, these findings should be confirmed by future long-term studies and randomized controlled trials before including this kind of diet in the prevention and management guidelines of CKD.
Abbreviations
- BMI:
-
Body mass index
- CKD:
-
Chronic kidney disease
- CI:
-
Confidence interval
- DASH:
-
Dietary approach to stop hypertension
- E:
-
Energy
- FFQ:
-
Food frequency questionnaire
- GFR:
-
Glomerular filtration rate
- MedDiet:
-
Mediterranean diet
- MetS:
-
Metabolic syndrome
- METS:
-
Metabolic equivalent task
- PREDIMED:
-
Prevención con dieta Mediterránea
- SCr:
-
Serum creatinine
- CKD-EPI:
-
Chronic kidney disease epidemiology collaboration equation for caucasian individuals
- OR:
-
Odds ratios
References
Bikbov B, Purcell CA, Levey AS et al (2020) Global, regional, and national burden of chronic kidney disease, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 395:709–733
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group (2013) KDIGO 2012 Clinical Practice Guideline for the evaluation and management of chronic kidney disease. Kidney Int 3:1–150
Ajjarapu AS, Hinkle SN, Li M, Francis EC, Zhang C (2019) Dietary patterns and renal health outcomes in thegeneral population: a review focusing on prospective studies. Nutrients. https://doi.org/10.3390/nu11081877
O’Sullivan ED, Hughes J, Ferenbach DA (2017) Renal aging: causes and consequences. J Am Soc Nephrol 28:407–420
van Westing AC, Küpers LK, Geleijnse JM (2020) Diet and kidney function: a literature review. Curr Hypertens Rep 22:1–9
Yuzbashian E, Asghari G, Mirmiran P, Hosseini FS, Azizi F (2015) Associations of dietary macronutrients with glomerular filtration rate and kidney dysfunction: Tehran lipid and glucose study. J Nephrol 28:173–180
Lin J, Hu FB, Curhan GC (2010) Associations of diet with albuminuria and kidney function decline. Clin J Am Soc Nephrol 5:836–843
Nettleton JA, Steffen LM, Palmas W, Burke GL, Jacobs DR (2008) Associations between microalbuminuria and animal foods, plant foods, and dietary patterns in the Multiethnic Study of Atherosclerosis. Am J Clin Nutr 87:1825–1836
Hu FB (2002) Dietary pattern analysis: a new direction in nutritional epidemiology. Curr Opin Lipidol 13:3–9
Xu SS, Hua J, Huang YQ, Shu L (2020) Association between dietary patterns and chronic kidney disease in a middle-aged Chinese population. Public Health Nutr 23:1058–1066
Bach KE, Kelly JT, Campbell KL, Palmer SC, Khalesi S, Strippoli GFM (2019) Healthy dietary patterns and incidence of CKD: a meta-analysis of cohort studies. Clin J Am Soc Nephrol 14:1441–1449
Quintela BCSF, Carioca AAF, de Oliveira JGR, Fraser SDS, da Silva Junior GB (2021) Dietary patterns and chronic kidney disease outcomes: a systematic review. Nephrology 26:603–612
Lin J, Fung TT, Hu FB, Curhan GC (2011) Association of dietary patterns with albuminuria and kidney function decline in older white women: a subgroup analysis from the nurses health study. Am J Kidney Dis 57:245–254
Hu EA, Coresh J, Anderson CAM et al (2021) Adherence to healthy dietary patterns and risk of CKD progression and all-cause mortality: findings from the CRIC (Chronic Renal Insufficiency Cohort) Study. Am J Kidney Dis 77:235–244
Khatri M, Moon YP, Scarmeas N, Gu Y, Gardener H, Cheung K, Wright CB, Sacco RL, Nickolas TL, Elkind MSV (2014) The association between a mediterranean-style diet and kidney function in the northern manhattan study cohort. Clin J Am Soc Nephrol 9:1868–1875
Liu Y, Kuczmarski MF, Miller ER, Nava MB, Zonderman AB, Evans MK, Powe NR, Crews DC (2017) Dietary habits and risk of kidney function decline in an urban population. J Ren Nutr 27:16–25
Jee Ko G, Obi Y, Tortorici AR, Kalantar-Zadeh K (2017) Dietary protein intake and chronic kidney disease. Curr Opin Clin Nutr Metab Care 20:77–85
Møller G, Sluik D, Ritz C et al (2017) A protein diet score, including plant and animal protein, investigating the association with hba1c and eGFR-The PREVIEW project. Nutrients 9:1–14
Martínez-González MA, Buil-Cosiales P, Corella D et al (2019) Cohort profile: design and methods of the PREDIMED-Plus randomized trial. Int J Epidemiol 48:387–388o
Alberti KGMM, Eckel RH, Grundy SM, Zimmet PZ, Cleeman JI, Donato KA, Fruchart JC, James WPT, Loria CM, Smith SC (2009) Harmonizing the metabolic syndrome: a joint interim statement of the international diabetes federation task force on epidemiology and prevention; National heart, lung, and blood institute; American heart association; World heart federation; International. Circulation 120:1640–1645
Willett WC, Howe R, Kushi LH (1997) Adjustment for total energy intake in epidemiologic studies. Am J Clin Nutr 65:1220S-S1228
Fernández-Ballart JD, Piñol JL, Zazpe I, Corella D, Carrasco P, Toledo E, Perez-Bauer M, Martínez-González MÁ, Salas-Salvadó J, Martín-Moreno JM (2010) Relative validity of a semi-quantitative food-frequency questionnaire in an elderly Mediterranean population of Spain. Br J Nutr 103:1808–1816
Mataix Verdú J (2003) Tabla de composición de alimentos [Food Composition Tables]. Granada, Spain
Moreiras O, Carvajal A, Cabrera L CC (2005) Tablas de composición de alimentos” Food Composition Tables” Pirámide, Madrid, Spain
Schröder H, Zomeño MD, Martínez-González MA et al (2021) Validity of the energy-restricted Mediterranean Diet Adherence Screener. Clin Nutr. https://doi.org/10.1016/J.CLNU.2021.06.030
Trichopoulou A, Costacou T, Bamia CTD (2003) Adherence to a Mediterranean diet and survival in a Greek population. N Engl J Med 348:2599–2608
Fung TT, Chiuve SE, McCullough ML, Rexrode KM, Logroscino G, Hu FB (2008) Adherence to a DASH-Style diet and risk of coronary heart disease and stroke in women. Arch Intern Med 168:713–720
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
Levey AS, Inker LA, Matsushita K, Greene T, Willis K, Lewis E, De Zeeuw D, Cheung AK, Coresh J (2014) GFR decline as an end point for clinical trials in CKD: a scientific workshop sponsored by the national kidney foundation and the US food and drug administration. Am J Kidney Dis 64:821–835
Trichopoulou A, Bamia C, Trichopoulos D (2009) Anatomy of health effects of Mediterranean diet: Greek EPIC prospective cohort study. BMJ 339:26–28
Cai Q, Dekker LH, Bakker SJL, de Borst MH, Navis GJ (2020) Dietary patterns based on estimated glomerular filtration rate and kidney function decline in the general population: the lifelines cohort study. Nutrients. https://doi.org/10.3390/nu12041099
Hu EA, Steffen LM, Grams ME, Crews DC, Coresh J, Appel LJ, Rebholz CM (2019) Dietary patterns and risk of incident chronic kidney disease: the Atherosclerosis Risk in Communities study. Am J Clin Nutr 110:713–721
Huang X, Jiménez-Molén JJ, Lindholm B, Cederholm T, Ärnlöv J, Risérus U, Sjögren P, Carrero JJ (2013) Mediterranean diet, kidney function, and mortality in men with CKD. Clin J Am Soc Nephrol 8:1548–1555
Geng T-T, Jafar TH, Neelakantan N, Yuan J-M, van Dam RM, Koh W-P (2021) Healthful dietary patterns and risk of end-stage kidney disease: the Singapore Chinese Health Study. Am J Clin Nutr 113:675–683
Díaz-López A, Bulló M, Martínez-González MÁ, Guasch-Ferré M, Ros E, Basora J, Covas MI, Del Carmen L-S, Salas-Salvadó J (2012) Effects of mediterranean diets on kidney function: a report from the PREDIMED trial. Am J Kidney Dis 60:380–389
Tirosh A, Golan R, Harman-Boehm I et al (2013) Renal function following three distinct weight loss dietary strategies during 2 years of a randomized controlled trial. Diabetes Care 36:2225–2232
Rebholz CM, Crews DC, Grams ME, Steffen LM, Levey AS, Miller ER, Appel LJ, Coresh J (2016) DASH (Dietary Approaches to Stop Hypertension) Diet and risk of subsequent kidney disease. Am J Kidney Dis 68:853–861
Appel LJ, Moore TJ, Obarzanek E et al (1997) A clinical trial of the effects of dietary patterns on blood pressure. N Engl J Med 336:1117–1124
Esposito K, Marfella R, Ciotola M, Di Palo C, Giugliano F, Giugliano G, D’Armiento M, D’Andrea F, Giugliano D (2004) Effect of a Mediterranean-style diet on endothelial dysfunction and markers of vascular inflammation in the metabolic syndrome: a randomized trial. J Am Med Assoc 292:1440–1446
Holt EM, Steffen LM, Moran A, Basu S, Steinberger J, Ross JA, Hong CP (2009) Fruit and vegetable consumption and its relation to markers of inflammation and oxidative stress in adolescents. J Am Diet Assoc 109:414–421
Farhadnejad H, Asghari G, Mirmiran P, Yuzbashian E, Azizi F (2016) Micronutrient intakes and incidence of chronic kidney disease in adults: Tehran Lipid and Glucose Study. Nutrients 8:1–10
Slavin J, Beate L (2012) Health benefits of fruits and vegetables. Adv Nutr 3:506–516
Letourneau P, Bataille S, Chauveau P, Fouque D, Koppe L (2020) Source and composition in amino acid of dietary proteins in the primary prevention and treatment of CKD. Nutrients 12:1–21
Apetrii M, Daniel Timofte LV, Covic A (2021) Nutrition in chronic kidney disease—the role of proteins and specific diets. Nutrients 13:956
Widmer RJ, Flammer AJ, Lerman LO, Lerman A (2015) The Mediterranean diet, its components, and cardiovascular disease. Am J Med 128:229–238
King AJ, Levey AS (1993) Dietary protein and renal function. J Am Soc Nephrol 3:1723–1737
Acknowledgements
The authors would especially like to thank the PREDIMED-Plus participants for their enthusiastic collaboration, the PREDIMED-Plus personnel for their outstanding support and the personnel of affiliated primary care centers for their exceptional effort. CIBEROBN, CIBERESP and CIBERDEM are initiatives of ISCIII, Madrid, Spain. We also thank the PREDIMED-Plus Biobank Network, part of the National Biobank Platform of the ISCIII for storing and managing the PREDIMED-Plus biological samples.
Funding
Open Access funding provided thanks to the CRUE-CSIC agreement with Springer Nature. This work was supported by the official Spanish Institutions for funding scientific biomedical research, CIBER Fisiopatología de la Obesidad y Nutrición (CIBEROBN) and Instituto de Salud Carlos III (ISCIII), through the Fondo de Investigación para la Salud (FIS), which is co-funded by the European Regional Development Fund (six coordinated FIS projects leaded by JS-S and JVi, including the following projects: PI13/00673, PI13/00492, PI13/00272, PI13/01123, PI13/00462, PI13/00233, PI13/02184, PI13/00728, PI13/01090, PI13/01056, PI14/01722, PI14/00636, PI14/00618, PI14/00696, PI14/01206, PI14/01919, PI14/00853, PI14/01374, PI14/00972, PI14/00728, PI14/01471, PI16/00473, PI16/00662, PI16/01873, PI16/01094, PI16/00501, PI16/00533, PI16/00381, PI16/00366, PI16/01522, PI16/01120, PI17/00764, PI17/01183, PI17/00855, PI17/01347, PI17/00525, PI17/01827, PI17/00532, PI17/00215, PI17/01441, PI17/00508, PI17/01732, PI17/00926, PI19/00957, PI19/00386, PI19/00309, PI19/01032, PI19/00576, PI19/00017, PI19/01226, PI19/00781, PI19/01560, PI19/01332, PI20/01802, PI20/00138, PI20/01532, PI20/00456, PI20/00339, PI20/00557, PI20/00886, PI20/01158); the Especial Action Project entitled: Implementación y evaluación de una intervención intensiva sobre la actividad física Cohorte PREDIMED-Plus grant to JS-S; the European Research Council (Advanced Research Grant 2014–2019; agreement #340918) granted to MÁM-G.; the Recercaixa (number 2013ACUP00194) grant to JS-S; grants from the Consejería de Salud de la Junta de Andalucía (PI0458/2013, PS0358/2016, PI0137/2018); the PROMETEO/2017/017 and the PROMETEO 21/2021 grant from the Generalitat Valenciana; the SEMERGEN grant; the Boosting young talent call grant program for the development of IISPV research projects 2019–2021 (Ref.: 2019/IISPV/03 grant to AD-L); the Societat Catalana d'Endocrinologia i Nutrició (SCEN) Clinical-Research Grant 2019 (IPs: JS-S and AD-L). Collaborative Nutrition and/or Obesity Project for Young Researchers 2019 supported by CIBEROBN entitled: Lifestyle Interventions and Chronic Kidney Disease: Inflammation, Oxidative Stress and Metabolomic Profile (LIKIDI study) grant to AD-L. Jordi Salas-Salvadó, gratefully acknowledges the financial support by ICREA under the ICREA Academia programme. M.R.-G., is supported by the Ministry of Education of Spain (FPU17/06488). None of the funding sources took part in the design, collection, analysis, interpretation of the data, or writing the report, or in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
CV-H, AD-L, NB-T, MAM-G, VR-G, DC, AG, JAM, AMA-G, JW, JV, DR, JLM, RE, FJT, JL, LS-M, NC-I, JAT, MR-G, XP, MD-R, PM-M, JV, SM-F, LD, ER, ET, JV-S, CR, IA, AM-R, EC-O, IC-G, MM, AG-R, RC, JCF-G, JMS-L, JD-E, CO-Z, MC, MAZ, CS-S, MR-C, MF, JS-S, and NB designed and conducted the research. CV-H, AD-L and NB-T- analysed the data. CV-H, AD-L, NB-T, and NB wrote the article. All authors revised the manuscript for important intellectual content and read and approved the final manuscript. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted. CV-H and NBT are the guarantors of this work and, as such, had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
JS-S reported receiving research support from the Instituto de Salud Carlos III (ISCIII), Ministerio de Educación y Ciencia, Departament de Salut Pública de la Generalitat de Catalunya, the European Commission, the California Walnut Commission, Patrimonio Comunal Olivarero, La Morella Nuts, and Borges S.A; receiving consulting fees or travel expenses from California Walnut Commission, Eroski Foundation, Instituto Danone, Abbott Laboratories and Mundifarma, receiving nonfinancial support from Hojiblanca, Patrimonio Comunal Olivarero, and Almond Board of California; serving on the board of and receiving grant support through his institution from the International Nut and Dried Foundation and the Eroski Foundation; and grants and personal fees from Instituto Danone. ER reported receiving grants, personal fees, and nonfinancial support from the California Walnut Commission during the conduct of the study and grants, personal fees, nonfinancial support from Alexion; personal fees from Amarin; and nonfinancial support from the International Nut Council outside the submitted work. RE reported receiving grants from Instituto de Salud Carlos III and olive oil for the trial from Fundacion Patrimonio Comunal Olivarero\during the conduct of the study and personal fees from Brewers of Europe, Fundación Cerveza y Salud, Interprofesional del Aceite de Oliva, Instituto Cervantes, Pernaud Richar, Fundación Dieta Mediterránea, Wine and Culinary International Forum; nonfinancial support from Sociedad Española de Nutrición and Fundación Bosch y Gimpera; and grants from Uriach Laboratories outside the submitted work. XP reported receiving grants from ISCIII during the conduct of the study; receiving consulting fees from Sanofi Aventis, Amgen, and Abbott laboratories; receiving lecture personal fees from Esteve, Lacer and Rubio laboratories. All other authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The study protocol and procedures were approved according to the ethical standards of the Declaration of Helsinki by the Institutional Review Boards (IRBs) of all the participating institutions.
Consent to participate
Written informed consent was obtained from all individual participants included in the study.
Consent for publication
All authors have approved this manuscript for publication.
Availability of the data and materials
There are restrictions on the availability of data for the PREDIMED-Plus trial, due to the signed consent agreements around data sharing, which only allow access to external researchers for studies following the project purposes. Requestors wishing to access the PREDIMED-Plus trial data used in this study can make a request to the PREDIMED-Plus trial Steering Committee chair: predimed_plus_scommitte@googlegroups.com. The request will then be passed to members of the PREDIMED-Plus Steering Committee for deliberation.
Code availability
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Valle-Hita, C., Díaz-López, A., Becerra-Tomás, N. et al. Prospective associations between a priori dietary patterns adherence and kidney function in an elderly Mediterranean population at high cardiovascular risk. Eur J Nutr 61, 3095–3108 (2022). https://doi.org/10.1007/s00394-022-02838-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-022-02838-7