Abstract
Introduction
A number of studies have evaluated the effects of subcutaneous drainage during digestive surgery. All of the previous studies assessed the usefulness of active-suctioning drain, including two randomized controlled studies which found no benefit for the placement of active-suctioning drains in digestive surgery. The utility of passive drainage has not been evaluated previously. The purpose of this study was to evaluate the efficacy of subcutaneous passive drainage system for preventing surgical site infections during major colorectal surgery.
Patients and methods
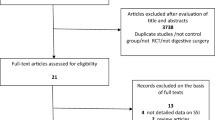
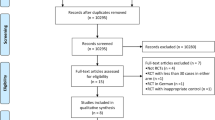
A total of 263 patients who underwent major colorectal surgery were enrolled in this study. Patients were randomly assigned to receive subcutaneous passive drainage or no drainage. The primary outcome measured was the incidence of superficial surgical site infections. The secondary outcomes measured were the development of hematomas, seromas, and wound dehiscence.
Results
Finally, a total of 246 patients (124 underwent passive drainage, and 122 underwent no drainage) were included in the analysis after randomization. There was a significant difference in the incidence of superficial surgical site infections between patients assigned to the passive drainage and no drainage groups (3.2 % vs 9.8 %, respectively, P = 0.041). There were no cases that developed a hematoma, seroma, or wound dehiscence in either group. A subgroup analysis revealed that male gender, age ≥75 years, diabetes mellitus, American Society of Anesthesiologists (ASA) status ≥2, blood loss ≥100 ml, and open access were factors that were associated with a beneficial effect of subcutaneous passive drainage.
Conclusions
Subcutaneous passive drainage provides benefits over no drainage in patients undergoing major colorectal surgery.

Similar content being viewed by others
References
Romy S, Eisenring MC, Bettschart V, Petignat C, Francioli P, Troillet N (2008) Laparoscope use and surgical site infections in digestive surgery. Ann Surg 247:627–632
Leaper DJ, van Goor H, Reilly J, Petrosillo N, Geiss HK, Torres AJ, Berger A (2004) Surgical site infection—a European perspective of incidence and economic burden. Int Wound J 1:247–273
Panici PB, Zullo MA, Casalino B, Angioli R, Muzii L (2003) Subcutaneous drainage versus no drainage after minilaparotomy in gynecologic benign conditions: a randomized study. Am J Obstet Gynecol 188:71–75
Baier PK, Gluck NC, Baumgartner U, Adam U, Fischer A, Hopt UT (2010) Subcutaneous Redon drains do not reduce the incidence of surgical site infections after laparotomy. A randomized controlled trial on 200 patients. Int J Color Dis 25:639–643
Kaya E, Paksoy E, Ozturk E, Sigirli D, Bilgel H (2010) Subcutaneous closed-suction drainage does not affect surgical site infection rate following elective abdominal operations: a prospective randomized clinical trial. Acta Chir Belg 110:457–462
Fujii T, Tabe Y, Yajima R, Yamaguchi S, Tsutsumi S, Asao T, Kuwano H (2011) Effects of subcutaneous drain for the prevention of incisional SSI in high-risk patients undergoing colorectal surgery. Int J Color Dis 26:1151–1155
Pocock SJ, Simon R (1975) Sequential treatment assignment with balancing for prognostic factors in the controlled clinical trial. Biometrics 31:103–115
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for prevention of surgical site infection, 1999. Centers for Disease Control and Prevention (CDC) Hospital Infection Control Practices Advisory Committee. Am J Infect Control 27:97–132, quiz 133–134; discussion 196
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET, Carbone PP (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Furukawa K, Onda M, Suzuki H, Maruyama H, Akiya Y, Ashikari M, Maezawa K, Tokunaga A, Tajiri T, Tanaka N, Yamasita K (1999) The usefulness of conducting investigations on intra-abdominal bacterial contamination in digestive tract operations. Surg Today 29:701–706
Chelmow D, Rodriguez EJ, Sabatini MM (2004) Suture closure of subcutaneous fat and wound disruption after cesarean delivery: a meta-analysis. Obstet Gynecol 103:974–980
Vermillion ST, Lamoutte C, Soper DE, Verdeja A (2000) Wound infection after cesarean: effect of subcutaneous tissue thickness. Obstet Gynecol 95:923–926
Gallup DC, Gallup DG, Nolan TE, Smith RP, Messing MF, Kline KL (1996) Use of a subcutaneous closed drainage system and antibiotics in obese gynecologic patients. Am J Obstet Gynecol 175:358–361, discussion 362
Al-Inany H, Youssef G, Abd ElMaguid A, Abdel Hamid M, Naguib A (2002) Value of subcutaneous drainage system in obese females undergoing cesarean section using Pfannenstiel incision. Gynecol Obstet Invest 53:75–78
Durai R, Mownah A, Ng PC (2009) Use of drains in surgery: a review. J Perioper Pract 19:180–186
Batstone MD, Lowe D, Shaw RJ, Brown JS, Vaughan ED, Rogers SN (2009) Passive versus active drainage following neck dissection: a non-randomised prospective study. Eur Arch Otorhinolaryngol 266:121–124
Razavi SM, Ibrahimpoor M, Sabouri Kashani A, Jafarian A (2005) Abdominal surgical site infections: incidence and risk factors at an Iranian teaching hospital. BMC Surg 5:2
Watanabe A, Kohnoe S, Shimabukuro R, Yamanaka T, Iso Y, Baba H, Higashi H, Orita H, Emi Y, Takahashi I, Korenaga D, Maehara Y (2008) Risk factors associated with surgical site infection in upper and lower gastrointestinal surgery. Surg Today 38:404–412
Biscione FM, Couto RC, Pedrosa TM, Neto MC (2007) Factors influencing the risk of surgical site infection following diagnostic exploration of the abdominal cavity. J Infect 55:317–323
Vaporciyan AA, Kies MS, Stevens CW (2003) Performance status. In: Kufe DW (ed) Holland-Frei cancer medicine, 6th edn. BC Decker, Ontario, p 302
Tsujita E, Yamashita Y, Takeishi K, Matsuyama A, Tsutsui S, Matsuda H, Taketomi A, Shirabe K, Ishida T, Maehara Y (2012) Subcuticular absorbable suture with subcutaneous drainage system prevents incisional SSI after hepatectomy for hepatocellular carcinoma. World J Surg 36:1651–1656
Acknowledgments
The authors would like to thank Y. Ishida, S. Shibuya, and T. Ishibashi for their secretarial assistance.
Conflicts of interest
We declare that there is no conflict of interest and that the trial was done independently of the producer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Numata, M., Godai, T., Shirai, J. et al. A prospective randomized controlled trial of subcutaneous passive drainage for the prevention of superficial surgical site infections in open and laparoscopic colorectal surgery. Int J Colorectal Dis 29, 353–358 (2014). https://doi.org/10.1007/s00384-013-1810-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-013-1810-x