Abstract
Understanding the molecular and cellular mechanisms driving pediatric low-grade glioma (pLGG)—the most prevalent brain tumor in children—is essential for the identification and evaluation of novel effective treatments. This review explores the intricate relationship between the mitogen-activated protein kinase (MAPK) pathway, oncogene-induced senescence (OIS), the senescence-associated secretory phenotype (SASP), and the tumor microenvironment (TME), integrating these elements into a unified framework termed the MAPK/OIS/SASP/TME (MOST) axis. This integrated approach seeks to deepen our understanding of pLGG and improve therapeutic interventions by examining the MOST axis’ critical influence on tumor biology and response to treatment. In this review, we assess the axis’ capacity to integrate various biological processes, highlighting new targets for pLGG treatment, and the need for characterized in vitro and in vivo preclinical models recapitulating pLGG’s complexity to test targets. The review underscores the need for a comprehensive strategy in pLGG research, positioning the MOST axis as a pivotal approach in understanding pLGG. This comprehensive framework will open promising avenues for patient care and guide future research towards inventive treatment options.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pediatric low-grade gliomas (pLGGs), the most frequent brain tumors in children [1], present a therapeutic conundrum of benign histology but significant clinical challenge due to their high risk of multiple progressions [2] and morbidity, making them a high-burden chronic disease. While the overall survival for these patients is excellent with a 10-year overall survival (OS) of 96% [2], 10-year progression-free survival (PFS) can be poor and is below 50% for partially resected tumors [3]. Patients are furthermore burdened with life-impeding morbidities related to the tumor location and/or treatment sequelae [4, 5].
Central to this disease is the mitogen-activated protein kinase (MAPK) pathway, a critical regulator of cell fate decisions including proliferation, differentiation, and apoptosis. Dysregulation of the MAPK pathway, resulting from various molecular alterations leading to activation, is a hallmark of pLGG [6,7,8].
The genetics and biology of the MAPK in pLGG is well understood and has led to the translation of preclinical concepts into the clinical reality of targeted MAPK inhibition. While the preclinical work has been focusing on the tumor compartment, the multiple aspects of the biology downstream, in particular of the oncogene-induced senescence (OIS), the senescence-associated secretory phenotype (SASP), and their interconnection with the tumor microenvironment (TME) are still incompletely understood. These components need to be investigated as interactive and not as separate entities in order to meet the clinical challenges of efficacious therapies, predictive stratification, rebound, and resistance in pLGG therapy.
In this review, we propose an integration of the MAPK pathway, OIS, SASP, and the TME into a MOST axis, a framework encapsulating the multifaceted biology of pLGG. Understanding and modeling this axis with adequate models will be crucial for unraveling the complexity of pLGG pathogenesis and identifying novel therapeutic targets.
MAPK pathway in pediatric low-grade gliomas
MAPK signaling pathways relay various extracellular signals, such as the presence of growth factors or stress, to cytoplasmic processes and transcriptional programs [9]. The RAS/RAF/MEK/ERK MAPK pathway plays not only a role in many physiological processes but is also dysregulated by somatic and germ-line mutations in tumor diseases and RASopathies, respectively [10]. pLGGs are a prime example for tumor diseases that are predominantly driven by aberrant ERK/MAPK activity due to mutations in core and accessory signaling elements of this pathway [6] (Fig. 1).
MAPK pathway in pediatric low-grade gliomas. RTK, receptor tyrosine kinase. Percentages from [7]
This signaling axis becomes activated by a plethora of cell surface receptors, with receptor tyrosine kinases (RTKs) being the most relevant in the context of this review. In pLGGs, alterations were identified in the RTKs NTRK2 and FGFR1/2 (< 1% and 12% of all pLGG, respectively) [7, 11]. RTKs are activated by growth factors inducing their dimerization, activation, and trans-phosphorylation resulting in the recruitment of effector protein complexes such as the Grb2/SOS complex promoting RAS-GTP loading [12].
The antagonistic reaction, the stimulation of GTP hydrolysis by RAS-GAPs such as neurofibromin 1 (NF1), is of particular interest from the pLGG perspective, as this tumor suppressor product is often lost or inactive in optic pathway glioma (OPG), which often occur in patients suffering from the RASopathy neurofibromatosis I (15% of all pLGG) [7, 13]. Albeit still mechanistically ill-defined, the proto-oncogene product SHP2/PTPN11 enhances RAS signaling, probably by multiple mechanisms [14]. Similar to NF1, gain-of-function SHP2 mutations are also found in LGG (< 2% of all pLGG) [7, 10]. Lastly, mutations affecting the intrinsic GTPase activity of RAS proteins are also found in pLGGs (< 1% of all pLGG) [7, 11].
Active RAS-GTP undergoes a conformational change resulting in the exposure of its effector loop and the recruitment of proteins with RAS binding domains such as the RAF proteins [15, 16].
pLGG is a tumor entity with a high frequency and diverse spectrum of RAF family kinase alterations [17]. Indeed, KIAA1549::BRAF fusion can be classified as the genetic signature alteration in pLGG (35% of all pLGG), and other BRAF fusions involving other genes have been reported [7, 18]. Almost all oncogenic BRAF fusion proteins reported so far share the inability to attain a closed inactive conformation as their pathomechanism [19]. As a result, these proteins bypass the need for the RAS-induced conformational change exposing the kinase domain and thus become strong MEK/ERK pathway activators due to their increased dimerization. Likewise, oncogenic RAF1 fusions have also been described in LGG, albeit at lower frequency (< 2% of all pLGG) [7, 18, 20,21,22]. However, RAF fusions are not completely uncoupled from regulatory layers [23, 24], unlike their BRAFV600E counterpart, the second most common RAF alteration in pLGG (15% of all pLGG) [7]. Mechanistically, the glutamic acid residue from the BRAFV600E mutation locks the BRAF kinase domain in an active conformation by mimicking the usual conformation change induced by its phosphorylation [25]. While most molecules form in fact stable homo-dimers as shown by complementary approaches [26,27,28], BRAFV600E also exists in monomeric state.
In turns, the MAPK ERK1 and ERK2 phosphorylate hundreds of substrates [29]. ERK is well known to influence transcription by phosphorylating transcription factors such as ELK1, in turn inducing the transcription of so-called immediate early genes such as FOS, which encodes another transcription factor that initiates the second wave of transcription. Among these target genes, we find genes involved in negative feedback loops (such as DUSPs and SPRY proteins) [30], allowing for fine tuning of the MAPK pathway’s activity.
Despite the diverse spectrum of alterations affecting the MAPK pathway and its excessive activation as the pathomechanism driving pLGG, these mechanistically different mutations generate distinct signaling outputs that can be further modulated by the position of the oncoprotein in the signaling network topology and its independence form positive and regulatory principles. For example, the high ERK pathway activity observed in BRAFV600E-driven tumors is explained by its independence from RAS-regulated events and its insensitivity against negative feedback loops [26, 31, 32], while these regulatory requirements still apply to RAF proteins in tumors driven by RTK alterations and probably by other upstream elements such as RAS or SHP2 [33]. Thus, depending on the molecular alteration, MAPK signaling output might be different. This highlights the need to appreciate a spectrum of aberrant MAPK activity that in turn address specific and sometimes contrasting gene expression programs such as proliferation, differentiation, or senescence that are demarcated by distinct quantitative and/or temporal thresholds. This concept was already discussed almost 30 years ago [34] and has been corroborated by studies showing how spatio-temporal and quantitative differences in MAPK activity contribute to cellular decision making [35]. Even within pLGGs, there appears to be a preference for BRAFV600E in supratentorial neoplasms, while cerebellar tumors are dominated by BRAF fusions [36]. This finding could also support the “goldilocks” hypothesis according to which certain pLGG precursor cells have different transformation thresholds, i.e. a critical amount of a “MAPK dose” that keeps the cells in cycle without causing either a resting state due to a too weak signal, or cell cycle arrest caused by a too high-dose triggering oncogene-induced senescence (OIS). Likewise, understanding the intrinsic factors, e.g. precise type of mutation or fusion partner, and extrinsic factors, e.g. the state of the intra- and intercellular signaling network, will be key to understanding the initiation of pLGG and their goldilocks principle driving tumor growth. Moreover, answering these questions will be key for a successful targeted therapy as an incomplete inhibition of a highly active BRAF oncoprotein triggering OIS instead of cell death in the majority of tumor cells might allow cell cycle re-entry and tumor expansion instead.
Oncogene-induced senescence (OIS) and senescence-associated secretory phenotype (SASP) in pLGG
Among the many cellular processes regulated by the MAPK pathway, OIS represents one of the most characteristic of pLGG. Cellular senescence is characterized by loss of proliferative capacity with preservation of viability and metabolic activity [37]. Continuous attrition of telomers triggering DNA damage response pathways was identified as the causative molecular correlate of the observed phenotype, corresponding to replicative senescence [38]. In more general terms, however, senescence can also be triggered by various other stimuli including overactivation of oncogenes in cells with intact tumor suppressor pathways, leading to OIS [39]. Both types of senescence share a number of features including cell cycle arrest, morphological transformation (large and flat phenotype), activation of tumor suppressor networks (p53/p21 and p16/RB pathways), SA-b-GAL activity, and senescence-associated heterochromatin foci (SAHF) [40] (Fig. 2). However, a key difference between replicative senescence and OIS is that OIS is independent of telomere shortening and therefore cannot be bypassed by expression of telomerase [41].
Pilocytic astrocytoma (PA), the most common pLGG subtype [2], shows typical features of senescence [42], and patient-derived PA cell lines exhibit a typical OIS and not replicative [43] senescent phenotype with upregulation of senescence gene-sets [43, 44]. In line with the observation that OIS can be induced by overactivation of an oncogene in the context of an otherwise intact genome, oncogenic MAPK signaling driven by PA-typical MAPK alterations (e.g. BRAF V600E mutation; KIAA1549::BRAF fusion) is able to induce senescence in normal astrocytes and human neural stem cells in vitro [42, 45]. The prominent role of intact tumor suppressor pathways for the execution of OIS in pLGG is underlined by two observations: firstly, pleomorphic xanthoastrocytoma cells that harbor a deletion of the tumor suppressor gene CDKN2A encoding p16 do not go into OIS [46]; second, senescence can be bypassed by expression of SV40 large T antigen, which inhibits p53/p21 as well as p16/RB pathways in PA cells [43, 44].
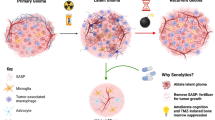
OIS requires the senescence-associated secretory phenotype (SASP), a complex inflammatory network composed of several chemokines and cytokines secreted by senescent cells [47]. These factors maintain growth arrest (human fibroblast models of OIS) and attract immune cells leading to clearance of growth-arrested genetically altered cells (hepatocellular carcinoma) [47, 48] or conversely execute proangiogenic effects leading to formation and growth of tumors (e.g. epithelial cells and breast cancer cells) [49, 50]. While it is not established whether SASP factor expression is under the control of the MAPK pathway in pLGG, they are upregulated in primary human pLGG tumors as well as in senescent patient-derived PA cells, with IL1B and IL6 being the most important cytokines, inducing and maintaining OIS via NFkB activation in an autocrine manner [51].
OIS, representing a powerful cell-intrinsic fail-safe mechanism, may explain why patients with PA tumors experience slow tumor growth, no progression to higher-grade astrocytomas, and excellent overall survival rates [42, 45]. High expression of OIS [43] and SASP [51] gene-signatures in primary PA tumors correlate with excellent event free survival, suggesting a tumor controlling role of OIS. However, non-proliferating tumor cells in OIS are likely not responsive to anti-proliferative treatments and may constitute a source of tumor progression after discontinuation of anti-proliferative treatments [52]. OIS is therefore a novel as well as clinically yet unexploited molecular target for the improved treatment of pLGG.
Tumor microenvironment (TME) in pLGG
While MAPK-driven pLGG cells characterized by OIS/SASP features represent an estimate of 50–60% of the bulk tumor, the remaining 40–50% are represented by microenvironmental cells [53]. Indeed, the TME is an important biological and clinical feature of brain tumors, plays critical roles in their development and progression, and has garnered clinical interest for therapeutic approaches [54]. Across brain tumors, the most common cell type found in the TME are myeloid cells (i.e. microglia and macrophages) [54,55,56,57,58,59,60,61,62]. In pediatric brain tumors, the amount and composition of the TME vary across tumor diagnoses. In particular, the proportions of immune infiltration tend to decrease with increasing WHO grade, making pLGG immune hot tumors compared to their cold and higher grade counterpart [59].
The composition of the TME in pLGG is diverse and comprises many subpopulations (Fig. 3). The main non-malignant cell type found in pLGG tumors are microglia (30–50%) [53, 63, 64], followed by macrophages (~ 5–10%) [53]. While the debate how to clearly discriminate between macrophages and microglia in gliomas [65, 66] is still ongoing, these monocytic populations are characterized by a high expression of the surface markers CD68 and IBA1 [63, 64]. Of particular interest, MAPK activity was found to be high in pLGG-associated microglia [67], while proliferating microglia have been found to be enriched in pilocytic astrocytomas compared to astrocytomas of higher grade (III–IV), suggesting a major role of these cells in pLGG biology [68]. For instance, microglia cells are essential for the initiation of NF1-driven OPGs in a mouse model [69], while PFS is inversely correlated with proportions of CD68 + cells in PA [70].
Lymphocytes were also identified in primary pLGG samples, including CD3 + , CD4 + , CD8 + , and NK and Tregs cells (~ 5–10%) [53, 59, 71]. In particular, CD8 + T cells were found in higher fractions in PAs (3.28%) compared to other types of brain tumors (1.3–0.1%) [72], while the proportion of CD3 + T cells was shown to vary across pLGG subtypes, with PXAs (4.7%) and GGs (4.8%) showing higher content compared to PAs (0.9%) [71]. They are also characterized by a low expression of immune checkpoint protein PD-1 in PA (16.6% and 23.3% of all CD8 + and CD4 + T cells, respectively) [53, 72]. T cells also play an important role in tumor initiation and progression, as CD4 + T cells may inhibit tumor formation [73], while CD8 + T cells may promote tumor cell survival [74]. Of note, B cells were also identified in pLGG from deconvolution of methylation profiles and scRNAseq studies, however in small proportions (< 1%) [59, 67], making this population rather understudied in pLGG.
In addition to immune cells, some studies demonstrated a potential tumor growth-promoting role of neurons in pLGG. An integrated proteogenomics study showed two subgroups in pLGG, one characterized by gene signatures associated with immune and microglia activity, the second by signatures related to neuronal activity [75]. These data are in concordance with another pLGG multi-omics study showing an “immune hot” group, enriched for microglia and macrophages signatures, and a “neuronal” group, enriched for neuronal signatures [76]. A recent study showed that pLGG tumors with reduced MAPKi sensitivity scores (MSS) were of a neuronal type, possibly suggesting a role for neuronal features in MAPKi treatment resistance [67]. While glioneuronal synapses were observed in adult LGGs [77], a study of such structures in their pediatric counter-part remains to be pursued.
Finally, pLGGs are invaded by endothelial cells [59] and highly vascularized [78]. Vascularization plays an important role in tumor biology, and high microvessel density was associated with decreased PFS in optic pathway and hypothalamic gliomas [79]. In addition, PA were shown to have a rather disrupted blood–brain barrier [80], evident in the clinical observation of contrast agent enhancement. In line with increased VEGF expression in PA, similar to glioblastoma [78, 81], anti-VEGF therapy using bevacizumab has shown radiological and functional efficacy in pLGG patients during treatment [82,83,84]. Beyond this, molecular mechanisms underlying the interactions between tumor cells and the vasculature in pLGGs remain to be investigated.
MAPK-OIS-SASP-TME axis: biology and potential clinical opportunities
While constitutive MAPK activation, induction of OIS/SASP and TME, represent more or less well-known key pLGG features on their own, their functional interconnection and cross-regulation has only recently become evident, and remains understudied. It has now become essential to envision these pLGG tumor components in an integrated manner, in what we propose to call the MAPK-OIS-SASP-TME (MOST) axis (Fig. 4).
The MAPK pathway plays in important intrinsic role in several brain TME cell populations. In microglia/macrophages, high MAPK activity was found to be associated with the polarization into a tumor promoting M2 phenotype, in adult glioblastoma (GBM) [85]. The MAPK pathway is also involved in the regulation of several processes in GBM-associated T cells, such as T cell proliferation, survival, activation, and aging [86,87,88], which can impair the anti-tumor immune response and favor tumor escape. The MAPK pathway is also highly involved in neo-vessel formation, as its effectors are found downstream of the main pro-angiogenic receptors VEGFR and FGFR [89], and can be activated during neo-angiogenesis in other tumor entities, such as renal and head and neck squamous cell carcinoma [90, 91]. Importantly, the MAPK pathway can promote an immunosuppressive environment in several preclinical models of colorectal cancer via the regulation of gene programs related to immune activity, such as interferon and inflammatory pathways, and reversible upon MAPK inhibition [87, 92, 93]. The MAPK pathway activity can also be dependent on the expression of the immune checkpoint protein TIM-3 in DIPGs, suggesting a role in the immuno-regulation of the TME [94]. While the MAPK pathway activity in the TME has been extensively studied in several entities, little is known about it in pLGG. Only recently a study found high MAPK pathway activity in microglia and macrophage populations in pLGG, associated with a high MSS [67]. Thus, these data indicate that the MAPK pathway plays a significant functional role in several populations of the TME of several tumor entities, including pLGG, possibly modulating the response to MAPKi treatment.
The OIS/SASP has a strong impact on the regulation of tumor development via its effect not only on the tumor cells, but also on the TME cells in pLGG. In a KIAA1549::BRAF fusion-driven neural stem cells (NSC) model, CCL2 secreted by the tumor cells, and under the control of the MAPK pathway, was necessary for the recruitment of microglia cells promoting tumor formation [95]. Increased secretion of cytokines by glioma cells upon MAPKi treatment and withdrawal was able to recruit microglia in an in vitro pLGG rebound model, highlighting the involvement of MAPKi signaling in the reshaping of pLGG TME via paracrine SASP factors (Kocher et al. in revision).
While SASP factors secreted by the tumor cells influence the pLGG TME, cytokines produced by TME cells can in turn influence the tumor cell compartment. For instance, CCL4 (secreted by CD8 + T cells) and CCL5 (secreted by microglia cells) were necessary to support OPG initiation via the induction of a neuronal-immune axis [74, 95]. Interestingly, CXCL10 produced by astrocytes was also important to prevent human-induced pluripotent stem cells (hiPSC)-LGG xenograft initiation via its activity on T cells [73].
SASP factors have been shown to be involved in the regulation of other TME populations in different tumor entities. VEGFA is generally involved in the induction of neo-angiogenesis [96]. The chemokine CXCL8 has been shown to be involved in the recruitment of neutrophils in colon carcinoma [97], while SASP gene expression signatures correlated with the expression of immune checkpoint proteins, such as PD-L1, in senescent fibroblast models [98]. It is important to note that senescent cells themselves can regulate their interaction with the immune system via reshaping their surface proteome and escape the clearance by the immune system, as has been shown in liver cancer [99]. Since these SASP factors are also produced by senescent pLGG cells, these mechanisms could be translated to pLGG.
All these findings, either demonstrated in pLGG or extrapolated from other entities and potentially transferable to pLGG biology, highlight the complexity of the MOST axis. All components influence each other forward and backward, in an auto- and paracrine manner, and in an extensive network of interactions and co-regulations. Therefore, an integrated analysis and understanding of pLGG and its TME can lead to new therapeutic strategies that target not only the tumor cells, but also the non-tumor cells and the interactions between these populations.
As an example, a combination of a MAPKi, potentially targeting the tumor cells and certain TME subpopulations, with an anti-angiogenic drug, such as bevacizumab, which on its own has already shown promising results in OPG in a retrospective study with regard to both tumor growth (at least stable disease was reached in 89% of patients) and visual function [82], could lead to a synergistic anti-tumor activity. Interestingly, similar progression patterns upon treatment withdrawal were observed in pLGG treated with either the VEGFRi bevacizumab [84] or MAPKi ([100], Kocher et al. in revision). Therefore, a sequential treatment regimen, with one treatment taking over when the other is withdrawn, could represent a way to prevent such progression upon treatment withdrawal.
As mentioned above, the MAPK pathway can promote an immunosuppressive microenvironment in other MAPK-driven entities [93]. Considering the importance of the MAPK pathway and immune cells in pLGG, a combination of MAPKi, inducing a more immunologically active TME, and immune checkpoint inhibitors, increasing immune cells’ activity, could potentiate the efficacy of the tumor cells’ clearance by the immune system. Such an approach, which already showed promising results in clinical trials in MAPK-driven CRC and melanoma [87, 93, 101], could be translated to pLGG.
Finally, senescent pLGG cells are dependent on pro-survival networks and can be targeted pharmacologically by senolytic drugs [44]. Senescent cells in pLGG, as well as other entities (melanoma, pancreatic carcinoma), can express PD-L1 [53, 98] or PD-L2 [53, 102]. These could be targeted by immune checkpoint inhibition facilitating the clearance of PD-L1/2 expressing senescent cells by the microenvironment, while inducing apoptosis in the remaining senescent cells with senolytic drugs. Preclinical data from lung adeno- and squamous cell carcinoma furthermore indicate that BCL-2 inhibitors such as APG-2575 were capable of reprogramming macrophages to a tumor suppressing M1 phenotype, thereby promoting the response to anti-PD-1 therapy [103]. This could represent a novel concept for pLGG treatment targeting the senescent compartment, with BCL-2 inhibitors both killing senescent tumor cells [44] as well as reprogramming the TME to promote PD-1 inhibitor response.
Taken together, the concept of the MOST axis illustrates the intricacies of pLGG tumors and opens the door to new therapeutic concepts to be investigated. While promising, a thorough pre-clinical evaluation of these treatment strategies will be necessary to support their future clinical investigations, highlighting the need for suitable preclinical models to model the MOST.
Modeling of the MOST in preclinical models
Preclinical pLGG research relies heavily on the use of in vitro and in vivo models, limiting the scope of potential discoveries to the constraints of the respective models used. The general challenges and opportunities of available pLGG models are discussed elsewhere [104]. With respect to the MOST, many models are limited in the coverage of the complete MOST axis, and the selection of the appropriate model therefore needs be guided by the questions to be studied.
Thus, the ideal model retains the genetics, signaling pathway activations (MAPK and beyond), tumor and TME cell population proportions, and the communications between as well as the interdependencies of these populations, in order to study the full MOST axis.
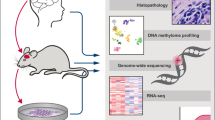
pLGG models currently available can be categorized in human primary tumor and hiPSC-derived in vitro cell lines and genetically engineered in vivo models [104]. pLGG in vitro cell line models derived from human primary tumors range from PA with a BRAF-fusion or -V600E mutation only (DKFZ-BT66, -BT308, -BT314, and -BT317) [43, 44] or NF1 loss (JHH-NF1-PA1) [105], to pleomorphic xanthoastrocytoma (PXA) with BRAFV600E mutation and CDKN2A/B deletion (BT40) [46]. hiPSC-derived pLGG cell lines harboring homozygous NF1 loss or ectopic KIAA1549::BRAF expression have been developed for studies of progenitor cell biology in vitro and gliomagenesis as well as preclinical drug development [73]. While these cell line models offer pragmatic and substantial advantages in terms of scalability, long-term usability, prompt availability, and relatively modest expense, by themselves they completely lack cell population heterogeneity and TME interaction (Fig. 5). However, basic MOST aspects such as MAPK in tumor cells, OIS, and SASP can be easily studied in a high-throughput manner in these systems. To leverage the advantages of cell line cultures for the investigation of circumscribed MOST functions, defined co-cultures may be of advantage, such as pLGG cell line—HMC3 microglia co-cultures (Kocher et al. in revision). Neural stem cell (NSC)-derived organoid-primary tumor tissue co-cultures, as described for high-grade gliomas [106] and if transferable to pLGG, may be a future intermediate pLGG in vitro culture system, maintaining the primary tumor cells and the primary immune cell populations as well as possibly the tumor-intrinsic architecture within the TME.
Beyond in vitro cell culture, the hiPSC pLGG models are usable in vivo in immunodeficient Rag1−/− mice [73]. While very well suited to study tumor cell-directed therapies in vivo, immunodeficient models lack intrinsic immune functions, limiting the scope of questions regarding the MOST axis. Immune-competent pLGG in vivo models comprise genetically engineered mouse models (GEMM) with NfF1 loss [107,108,109,110] or ectopic BRAFV600E kinase domain overexpression (BRAFV600E KD-RCAS-Ntv-a) [111], as well as genetically engineered minipigs with NFf1 loss [112]. Finally, GEMM to study specific TME populations exist, e.g. for microglia (i.e. tissue-resident macrophages) (HexbtdTomato mice) [113] and bone marrow-derived macrophages (BMDM) (Flt3:Cre; Rosa26:mTmG mice) [114, 115], opening the possibility to investigate consequences of MAPK inhibition on specific TME populations. In summary, immune competent pLGG GEMM, such as the BRAFV600E KD-RCAS-Ntv-a, modeling BRAFV600E mutated PA, or the Nf1neo/flox;GFAP-Cre, modeling NF1-deficient OPG, in particular represent an optimal overlap of prerequisites to study all aspects of the MOST axis, limited only by financial, infrastructural and expertise resources (Fig. 5).
It is thus dependent on the specific question to be studied, which model is optimally suited for MOST axis investigations. While genetically faithful models, true to pLGG biology, are becoming more widely available, the community is still very far away from full availability of models reflecting the wide range of genetically defined pLGG entities as recognized by the WHO [116], highlighting the need for further pLGG model development.
Conclusion and translational roadmap
In this exploration of pediatric low-grade glioma (pLGG) through the lens of the MOST axis, we present a complex network of interactions that drives tumor behavior and response to therapy. This integrated approach highlights not only the intricacies of pLGG tumor and TME biology, but also potential avenues for innovative therapeutic strategies. The dysregulation of the MAPK pathway, a cornerstone in pLGG initiation and development, represents a prime target for intervention. However, as the MAPK pathway is closely intertwined with all aspects of pLGG biology, it cannot be viewed in an isolated manner, and as such requires further investigation to elucidate its role in pLGG’s TME populations. Moreover, the dual roles of OIS and SASP in tumor control and progression underscore the necessity for treatments that can navigate the fine line between inhibiting tumor growth and avoiding the promotion of a tumor-supporting microenvironment. Finally, the immunomodulation of the TME represent a new therapeutic opportunity which remains to be investigated in pLGG.
The translation of these insights into clinical practice demands a refined development of preclinical models that accurately recapitulate the disease. Such models are crucial for testing novel therapeutic agents and combinations. The impact of the MOST on the natural course of disease, as well as on (conventional, novel, and future) treatment response (i.e. treatment efficacy), as well as treatment effects on the MOST axis itself, need to be studied pre-clinically to provide a rationale for translation in clinical trials. Finally, clinical trials need to encompass reverse-translation, to include tumor material collection at appropriate timepoints (e.g. before, and if the need for an operation arises for clinical reasons, ideally also during or after treatment) in clinical trial protocols to study the MOST in primary patient tumor material. Therefore, concerted collaborative studies in the pre-clinical, translational, and clinical space will be necessary for the development of therapies targeting the MOST that are both effective and minimize long-term sequelae for pLGG patients.
By embracing the intricacies of all aspects of pLGG biology and leveraging advanced preclinical models, the path is set for groundbreaking advancements in therapy and patient care, marking a new era in pediatric neuro-oncology.
Data availability
No datasets were generated or analysed during the current study.
References
Ostrom QT, Price M, Neff C et al (2022) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2015–2019. Neuro Oncol 24:v1–v95. https://doi.org/10.1093/NEUONC/NOAC202
Ostrom QT, De Blank PM, Kruchko C et al (2015) Alex’s lemonade stand foundation infant and childhood primary brain and central nervous system tumors diagnosed in the United States in 2007–2011. Neuro Oncol 16:x1. https://doi.org/10.1093/NEUONC/NOU327
Wisoff JH, Sanford RA, Heier LA et al (2011) Primary neurosurgery for pediatric low-grade gliomas: a prospective multi-institutional study from the children’s oncology group. Neurosurgery 68:1548–1554. https://doi.org/10.1227/NEU.0B013E318214A66E
Armstrong GT, Conklin HM, Huang S et al (2011) Survival and long-term health and cognitive outcomes after low-grade glioma. Neuro Oncol 13:223. https://doi.org/10.1093/NEUONC/NOQ178
Bandopadhayay P, Bergthold G, London WB et al (2014) Long-term outcome of 4,040 children diagnosed with pediatric low-grade gliomas: an analysis of the Surveillance Epidemiology and End Results (SEER) database. Pediatr Blood Cancer 61:1173. https://doi.org/10.1002/PBC.24958
Ryall S, Zapotocky M, Fukuoka K et al (2020) Integrated molecular and clinical analysis of 1,000 pediatric low-grade gliomas. Cancer Cell 37:569-583.e5. https://doi.org/10.1016/J.CCELL.2020.03.011
Ryall S, Tabori U (2020) Hawkins C (2020) Pediatric low-grade glioma in the era of molecular diagnostics. Acta Neuropathol Commun 81(8):1–22. https://doi.org/10.1186/S40478-020-00902-Z
Milde T, Rodriguez FJ, Barnholtz-Sloan JS et al (2021) Reimagining pilocytic astrocytomas in the context of pediatric low-grade gliomas. Neuro Oncol 23:1634–1646. https://doi.org/10.1093/NEUONC/NOAB138
Schaeffer HJ, Weber MJ (1999) Mitogen-activated protein kinases: specific messages from ubiquitous messengers. Mol Cell Biol 19:2435. https://doi.org/10.1128/MCB.19.4.2435
Hebron KE, Hernandez ER, Yohe ME (2022) The RASopathies: from pathogenetics to therapeutics. Dis Model Mech 15. https://doi.org/10.1242/DMM.049107
Jones DTW, Hutter B, Jäger N et al (2013) (2013) Recurrent somatic alterations of FGFR1 and NTRK2 in pilocytic astrocytoma. Nat Genet 458(45):927–932. https://doi.org/10.1038/ng.2682
Du Z, Lovly CM (2018) Mechanisms of receptor tyrosine kinase activation in cancer. Mol Cancer 17. https://doi.org/10.1186/S12943-018-0782-4
Anastasaki C, Orozco P, Gutmann DH (2022) RAS and beyond: the many faces of the neurofibromatosis type 1 protein. Dis Model Mech 15:. https://doi.org/10.1242/DMM.049362
Wei W, Geer MJ, Guo X et al (2023) Genome-wide CRISPR/Cas9 screens reveal shared and cell-specific mechanisms of resistance to SHP2 inhibition. J Exp Med 220. https://doi.org/10.1084/JEM.20221563
Jeon H, Tkacik E, Eck MJ (2024) Signaling from RAS to RAF: the molecules and their mechanisms. Annu Rev Biochem 93. https://doi.org/10.1146/ANNUREV-BIOCHEM-052521-040754
Martinez Fiesco JA, Durrant DE, Morrison DK, Zhang P (2022) Structural insights into the BRAF monomer-to-dimer transition mediated by RAS binding. Nat Commun 13. https://doi.org/10.1038/S41467-022-28084-3
Jones DTW, Gronych J, Lichter P et al (2012) MAPK pathway activation in pilocytic astrocytoma. Cell Mol Life Sci 69:1799. https://doi.org/10.1007/S00018-011-0898-9
Cin H, Meyer C, Herr R et al (2011) Oncogenic FAM131B-BRAF fusion resulting from 7q34 deletion comprises an alternative mechanism of MAPK pathway activation in pilocytic astrocytoma. Acta Neuropathol 121:763–774. https://doi.org/10.1007/S00401-011-0817-Z/TABLES/1
Weinberg F, Griffin R, Fröhlich M et al (2019) (2019) Identification and characterization of a BRAF fusion oncoprotein with retained autoinhibitory domains. Oncogene 394(39):814–832. https://doi.org/10.1038/s41388-019-1021-1
Jain P, Fierst TM, Han HJ et al (2017) CRAF gene fusions in pediatric low-grade gliomas define a distinct drug response based on dimerization profiles. Oncogene 36:6348. https://doi.org/10.1038/ONC.2017.276
Rankin A, Johnson A, Roos A et al (2021) Targetable BRAF and RAF1 alterations in advanced pediatric cancers. Oncologist 26:e153. https://doi.org/10.1002/ONCO.13519
Jones DTW, Kocialkowski S, Liu L et al (2009) Oncogenic RAF1 rearrangement and a novel BRAF mutation as alternatives to KIAA1549:BRAF fusion in activating the MAPK pathway in pilocytic astrocytoma. Oncogene 28:2119. https://doi.org/10.1038/ONC.2009.73
Sievert AJ, Lang S-S, Boucher KL et al (2013) Paradoxical activation and RAF inhibitor resistance of BRAF protein kinase fusions characterizing pediatric astrocytomas. Proc Natl Acad Sci 110:5957–5962. https://doi.org/10.1073/PNAS.1219232110
Köhler M, Röring M, Schorch B et al (2016) Activation loop phosphorylation regulates B‐Raf in vivo and transformation by B‐Raf mutants. EMBO J 35:143. https://doi.org/10.15252/EMBJ.201592097
Wan PTC, Garnett MJ, Roe SM et al (2004) Mechanism of activation of the RAF-ERK signaling pathway by oncogenic mutations of B-RAF. Cell 116:855–867. https://doi.org/10.1016/S0092-8674(04)00215-6
Röring M, Herr R, Fiala GJ et al (2012) Distinct requirement for an intact dimer interface in wild-type, V600E and kinase-dead B-Raf signalling. EMBO J 31:2629. https://doi.org/10.1038/EMBOJ.2012.100
Thevakumaran N, Lavoie H, Critton DA et al (2014) (2014) Crystal structure of a BRAF kinase domain monomer explains basis for allosteric regulation. Nat Struct Mol Biol 221(22):37–43. https://doi.org/10.1038/nsmb.2924
Rohrer L, Spohr C, Beha C et al (2023) Analysis of RAS and drug induced homo- and heterodimerization of RAF and KSR1 proteins in living cells using split Nanoluc luciferase. Cell Commun Signal 21:136. https://doi.org/10.1186/S12964-023-01146-9
Ünal EB, Uhlitz F, Blüthgen N (2017) A compendium of ERK targets. FEBS Lett 591:2607–2615. https://doi.org/10.1002/1873-3468.12740
Lavoie H, Gagnon J (2020) Therrien M (2020) ERK signalling: a master regulator of cell behaviour, life and fate. Nat Rev Mol Cell Biol 2110(21):607–632. https://doi.org/10.1038/s41580-020-0255-7
Brady SC, Coleman ML, Munro J et al (2009) Sprouty2 association with B-Raf is regulated by phosphorylation and kinase conformation. Cancer Res 69:6773–6781. https://doi.org/10.1158/0008-5472.CAN-08-4447
Friday BB, Yu C, Dy GK et al (2008) BRAF V600E disrupts AZD6244-induced abrogation of negative feedback pathways between extracellular signal-regulated kinase and Raf proteins. Cancer Res 68:6145–6153. https://doi.org/10.1158/0008-5472.CAN-08-1430
Pratilas CA, Taylor BS, Ye Q et al (2009) V600EBRAF is associated with disabled feedback inhibition of RAF–MEK signaling and elevated transcriptional output of the pathway. PNAS 106:4519–4524. https://doi.org/10.1073/PNAS.0900780106
Marshall CJ (1995) Specificity of receptor tyrosine kinase signaling: transient versus sustained extracellular signal-regulated kinase activation. Cell 80:179–185. https://doi.org/10.1016/0092-8674(95)90401-8
Murphy LO, Blenis J (2006) MAPK signal specificity: the right place at the right time. Trends Biochem Sci 31:268–275. https://doi.org/10.1016/J.TIBS.2006.03.009
Penman CL, Faulkner C, Lowis SP, Kurian KM (2015) Current understanding of BRAF alterations in diagnosis, prognosis, and therapeutic targeting in pediatric low-grade gliomas. Front Oncol 5. https://doi.org/10.3389/FONC.2015.00054
Hayflick L, Moorhead PS (1961) The serial cultivation of human diploid cell strains. Exp Cell Res 25:585–621. https://doi.org/10.1016/0014-4827(61)90192-6
D’Adda Di Fagagna F, Reaper PM, Clay-Farrace L et al (2003) A DNA damage checkpoint response in telomere-initiated senescence. Nature 426:194–198. https://doi.org/10.1038/NATURE02118
Serrano M, Lin AW, McCurrach ME et al (1997) Oncogenic ras provokes premature cell senescence associated with accumulation of p53 and p16INK4a. Cell 88:593–602. https://doi.org/10.1016/S0092-8674(00)81902-9
Kuilman T, Michaloglou C, Mooi WJ, Peeper DS (2010) The essence of senescence. Genes Dev 24:2463–2479. https://doi.org/10.1101/GAD.1971610
Wei S, Wei W, Sedivy JM (1999) Expression of catalytically active telomerase does not prevent premature senescence caused by overexpression of oncogenic Ha-Ras in normal human fibroblasts. Cancer Res 59:1539–1543
Jacob K, Quang-Khuong DA, Jones DTW et al (2011) Genetic aberrations leading to MAPK pathway activation mediate oncogene-induced senescence in sporadic pilocytic astrocytomas. Clin Cancer Res 17:4650–4660. https://doi.org/10.1158/1078-0432.CCR-11-0127/84269/AM/GENETIC-ABERRATIONS-LEADING-TO-MAPK-PATHWAY
Selt F, Hohloch J, Hielscher T et al (2017) Establishment and application of a novel patient-derived KIAA1549:BRAF-driven pediatric pilocytic astrocytoma model for preclinical drug testing. Oncotarget 8:11460. https://doi.org/10.18632/ONCOTARGET.14004
Selt F, Sigaud R, Valinciute G et al (2022) BH3 mimetics targeting BCL-XL impact the senescent compartment of pilocytic astrocytoma. Neuro Oncol. https://doi.org/10.1093/NEUONC/NOAC199
Raabe EH, Lim KS, Kim JM et al (2011) BRAF activation induces transformation and then senescence in human neural stem cells: a pilocytic astrocytoma model. Clin Cancer Res 17:3590. https://doi.org/10.1158/1078-0432.CCR-10-3349
Bid HK, Kibler A, Phelps DA et al (2013) Development, characterization, and reversal of acquired resistance to the MEK1 inhibitor selumetinib (AZD6244) in an in vivo model of childhood astrocytoma. Clin Cancer Res 19:6716–6729. https://doi.org/10.1158/1078-0432.CCR-13-0842
Kuilman T, Michaloglou C, Vredeveld LCW et al (2008) Oncogene-induced senescence relayed by an interleukin-dependent inflammatory network. Cell 133:1019–1031. https://doi.org/10.1016/j.cell.2008.03.039
Xue W, Zender L, Miething C et al (2007) Senescence and tumour clearance is triggered by p53 restoration in murine liver carcinomas. Nature 445. https://doi.org/10.1038/NATURE05529
Krtolica A, Parrinello S, Lockett S et al (2001) Senescent fibroblasts promote epithelial cell growth and tumorigenesis: a link between cancer and aging. Proc Natl Acad Sci U S A 98:12072–12077
Coppe JP, Kauser K, Campisi J, Beauséjour CM (2006) Secretion of vascular endothelial growth factor by primary human fibroblasts at senescence. J Biol Chem 281:29568–29574. https://doi.org/10.1074/jbc.M603307200
Buhl JL, Selt F, Hielscher T et al (2019) The senescence-associated secretory phenotype mediates oncogene-induced senescence in pediatric pilocytic astrocytoma. Clin Cancer Res 25:1851–1866. https://doi.org/10.1158/1078-0432.CCR-18-1965
Carreno G, Guiho R, Martinez-Barbera JP (2021) Cell senescence in neuropathology: a focus on neurodegeneration and tumours. Neuropathol Appl Neurobiol 47:359–378. https://doi.org/10.1111/NAN.12689
Reitman ZJ, Paolella BR, Bergthold G et al (2019) Mitogenic and progenitor gene programmes in single pilocytic astrocytoma cells. Nat Commun 10:1–17. https://doi.org/10.1038/s41467-019-11493-2
Pasqualini C, Kozaki T, Bruschi M et al (2020) Modeling the interaction between the microenvironment and tumor cells in brain tumors. Neuron 108:1025–1044. https://doi.org/10.1016/j.neuron.2020.09.018
González-Tablas Pimenta M, Otero Á, Arandia Guzman DA et al (2021) Tumor cell and immune cell profiles in primary human glioblastoma: impact on patient outcome. Brain Pathol 31:365–380. https://doi.org/10.1111/bpa.12927
Korin B, Ben-Shaanan TL, Schiller M et al (2017) High-dimensional, single-cell characterization of the brain’s immune compartment. Nat Neurosci 20:1300–1309. https://doi.org/10.1038/nn.4610
Zhong QY, Fan EX, Feng GY et al (2019) A gene expression-based study on immune cell subtypes and glioma prognosis. BMC Cancer 19. https://doi.org/10.1186/s12885-019-6324-7
Graeber MB, Scheithauer BW, Kreutzberg GW (2002) Microglia in brain tumors. John Wiley & Sons, Ltd
Grabovska Y, Mackay A, O’Hare P et al (2020) Pediatric pan-central nervous system tumor analysis of immune-cell infiltration identifies correlates of antitumor immunity. Nat Commun 11. https://doi.org/10.1038/S41467-020-18070-Y
Rossi ML, Hughes JT, Esiri MM et al (1987) Immunohistological study of mononuclear cell infiltrate in malignant gliomas. Acta Neuropathol 74:269–277. https://doi.org/10.1007/BF00688191
Morantz RA, Wood GW, Foster M et al (1979) Macrophages in experimental and human brain tumors. Part 2: Studies of the macrophage content of human brain tumors. J Neurosurg 50:305–311. https://doi.org/10.3171/jns.1979.50.3.0305
Sharma P, Aaroe A, Liang J, Puduvalli VK (2023) Tumor microenvironment in glioblastoma: current and emerging concepts. Neuro-Oncology Adv 5. https://doi.org/10.1093/noajnl/vdad009
Simmons GW, Pong WW, Emnett RJ et al (2011) Neurofibromatosis-1 heterozygosity increases microglia in a spatially and temporally restricted pattern relevant to mouse optic glioma formation and growth. J Neuropathol Exp Neurol 70:51–62. https://doi.org/10.1097/NEN.0b013e3182032d37
Gutmann DH, McLellan MD, Hussain I et al (2013) Somatic neurofibromatosis type 1 (NF1) inactivation characterizes NF1-associated pilocytic astrocytoma. Genome Res 23:431–439. https://doi.org/10.1101/gr.142604.112
Chen Z, Feng X, Herting CJ et al (2017) Cellular and molecular identity of tumor-associated macrophages in glioblastoma. Cancer Res 77:2266–2278. https://doi.org/10.1158/0008-5472.CAN-16-2310
Buonfiglioli A, Hambardzumyan D (2021) Macrophages and microglia: the cerberus of glioblastoma. Acta Neuropathol Commun 9. https://doi.org/10.1186/S40478-021-01156-Z
Sigaud R, Albert TK, Hess C et al (2023) MAPK inhibitor sensitivity scores predict sensitivity driven by the immune infiltration in pediatric low-grade gliomas. Nat Commun 14:1–21. https://doi.org/10.1038/s41467-023-40235-8
Klein R, Roggendorf W (2001) Increased microglia proliferation separates pilocytic astrocytomas from diffuse astrocytomas: a double labeling study. Acta Neuropathol 101:245–248. https://doi.org/10.1007/S004010000286
Pong WW, Higer SB, Gianino SM et al (2013) Reduced microglial CX3CR1 expression delays neurofibromatosis-1 glioma formation. Ann Neurol 73:303–308. https://doi.org/10.1002/ana.23813
Dorward IG, Luo J, Perry A et al (2010) Postoperative imaging surveillance in pediatric pilocytic astrocytomas. J Neurosurg Pediatr 6:346–352. https://doi.org/10.3171/2010.7.PEDS10129
Robinson MH, Vasquez J, Kaushal A et al (2020) Subtype and grade-dependent spatial heterogeneity of T-cell infiltration in pediatric glioma. J Immunother Cancer 8. https://doi.org/10.1136/jitc-2020-001066
Griesinger AM, Birks DK, Donson AM et al (2013) Characterization of distinct immunophenotypes across pediatric brain tumor types. J Immunol 191:4880–4888. https://doi.org/10.4049/JIMMUNOL.1301966
Anastasaki C, Chatterjee J, Cobb O et al (2022) Human induced pluripotent stem cell engineering establishes a humanized mouse platform for pediatric low-grade glioma modeling. Acta Neuropathol Commun 10:120. https://doi.org/10.1186/S40478-022-01428-2
Guo X, Pan Y, Xiong M et al (2020) (2020) Midkine activation of CD8+ T cells establishes a neuron–immune–cancer axis responsible for low-grade glioma growth. Nat Commun 111(11):1–15. https://doi.org/10.1038/s41467-020-15770-3
Picard D, Felsberg J, Langini M et al (2023) Integrative multi-omics reveals two biologically distinct groups of pilocytic astrocytoma. Acta Neuropathol 146:551. https://doi.org/10.1007/S00401-023-02626-5
Petralia F, Tignor N, Reva B et al (2020) Integrated proteogenomic characterization across major histological types of pediatric brain cancer. Cell 183:1962-1985.e31. https://doi.org/10.1016/J.CELL.2020.10.044
Venkataramani V, Tanev DI, Strahle C et al (2019) (2019) Glutamatergic synaptic input to glioma cells drives brain tumour progression. Nat 5737775(573):532–538. https://doi.org/10.1038/s41586-019-1564-x
Sie M, De Bont ESJM, Scherpen FJG et al (2010) Tumour vasculature and angiogenic profile of paediatric pilocytic astrocytoma; is it much different from glioblastoma? Neuropathol Appl Neurobiol 36:636–647. https://doi.org/10.1111/j.1365-2990.2010.01113.x
Bartels U, Hawkins C, Ma J et al (2006) Vascularity and angiogenesis as predictors of growth in optic pathway/hypothalamic gliomas. J Neurosurg 104:314–320. https://doi.org/10.3171/ped.2006.104.5.314
Hong C, Ho W, Piazza M et al (2016) Characterization of the blood brain barrier in pediatric central nervous system neoplasms. J Interdiscip Histopathol 4:29. https://doi.org/10.5455/JIHP.20160623053540
Mustafa D, Swagemakers S, French P et al (2013) Structural and expression differences between the vasculature of pilocytic astrocytomas and glioblastomas. J Neuropathol Exp Neurol 72:1171–1181. https://doi.org/10.1097/NEN.0000000000000015
Green K, Panagopoulou P, D’Arco F et al (2023) A nationwide evaluation of bevacizumab-based treatments in pediatric low-grade glioma in the UK: safety, efficacy, visual morbidity, and outcomes. Neuro Oncol 25:774–785. https://doi.org/10.1093/neuonc/noac223
Simão-Rafael M, Cruz O, Perez-Jaume S et al (2023) Use of bevacizumab in pediatric low-grade glioma: ten-year experience in a single center. EJC Paediatr Oncol 2:100115. https://doi.org/10.1016/j.ejcped.2023.100115
de Marcellus C, Tauziède-Espariat A, Cuinet A et al (2022) The role of irinotecan-bevacizumab as rescue regimen in children with low-grade gliomas: a retrospective nationwide study in 72 patients. J Neurooncol 157:355–364. https://doi.org/10.1007/s11060-022-03970-4
Fermi V, Warta R, Wöllner A et al (2023) Effective reprogramming of patient-derived M2-polarized glioblastoma-associated microglia/macrophages by treatment with GW2580. Clin Cancer Res 29:4685–4697. https://doi.org/10.1158/1078-0432.CCR-23-0576/728983/AM/EFFECTIVE-REPROGRAMMING-OF-PATIENT-DERIVED-M2
D’Souza WN, Chang C-F, Fischer AM et al (2008) The Erk2 MAPK regulates CD8 T cell proliferation and survival. J Immunol 181:7617. https://doi.org/10.4049/JIMMUNOL.181.11.7617
Ebert PJR, Cheung J, Yang Y et al (2016) MAP kinase inhibition promotes T cell and anti-tumor activity in combination with PD-L1 checkpoint blockade. Immunity 44:609–621. https://doi.org/10.1016/j.immuni.2016.01.024
Lanna A, Gomes DCO, Muller-Durovic B et al (2017) A sestrin-dependent Erk/Jnk/p38 MAPK activation complex inhibits immunity during ageing. Nat Immunol 18:354. https://doi.org/10.1038/NI.3665
Song M, Finley SD (2018) Mechanistic insight into activation of MAPK signaling by pro-angiogenic factors. BMC Syst Biol 12:1–17. https://doi.org/10.1186/S12918-018-0668-5/FIGURES/7
Huang D, Ding Y, Luo WM et al (2008) Inhibition of MAPK kinase signaling pathways suppressed renal cell carcinoma growth and angiogenesis in vivo. Cancer Res 68:81–88. https://doi.org/10.1158/0008-5472.CAN-07-5311
Zeng Q, Li S, Chepeha DB et al (2005) Crosstalk between tumor and endothelial cells promotes tumor angiogenesis by MAPK activation of Notch signaling. Cancer Cell 8:13–23. https://doi.org/10.1016/j.ccr.2005.06.004
Liu L, Mayes PA, Eastman S et al (2015) The BRAF and MEK inhibitors dabrafenib and trametinib: effects on immune function and in combination with immunomodulatory antibodies targeting PD-1, PD-L1, and CTLA-4. Clin Cancer Res 21:1639–1651. https://doi.org/10.1158/1078-0432.CCR-14-2339/175401/AM/THE-BRAF-AND-MEK-INHIBITORS-DABRAFENIB-AND
Tian J, Chen JH, Chao SX et al (2023) (2023) Combined PD-1, BRAF and MEK inhibition in BRAFV600E colorectal cancer: a phase 2 trial. Nat Med 292(29):458–466. https://doi.org/10.1038/s41591-022-02181-8
Ausejo-Mauleon I, Labiano S, de la Nava D et al (2023) TIM-3 blockade in diffuse intrinsic pontine glioma models promotes tumor regression and antitumor immune memory. Cancer Cell 41:1911-1926.e8. https://doi.org/10.1016/j.ccell.2023.09.001
Chen R, Keoni C, Waker CA et al (2019) KIAA1549-BRAF expression establishes a permissive tumor microenvironment through NFκB-mediated CCL2 production. Neoplasia 21:52. https://doi.org/10.1016/J.NEO.2018.11.007
Hicklin DJ, Ellis LM (2016) Role of the vascular endothelial growth factor pathway in tumor growth and angiogenesis. 23:1011–1027. https://doi.org/10.1200/JCO.2005.06.081
Kryczek I, Wang L, Wu K et al (2016) Inflammatory regulatory T cells in the microenvironments of ulcerative colitis and colon carcinoma. Oncoimmunology 5. https://doi.org/10.1080/2162402X.2015.1105430
Wang TW, Johmura Y, Suzuki N et al (2022) (2022) Blocking PD-L1–PD-1 improves senescence surveillance and ageing phenotypes. Nat 6117935(611):358–364. https://doi.org/10.1038/s41586-022-05388-4
Chen HA, Ho YJ, Mezzadra R et al (2023) Senescence rewires microenvironment sensing to facilitate antitumor immunity. Cancer Discov 13:433–453. https://doi.org/10.1158/2159-8290.CD-22-0528/710081/AM/SENESCENCE-REWIRES-MICROENVIRONMENT-SENSING-TO
Nobre L, Zapotocky M, Ramaswamy V et al (2020) Outcomes of BRAF V600E pediatric gliomas treated with targeted BRAF inhibition. 561–571. https://doi.org/10.1200/PO.19.00298
Sullivan RJ, Hamid O, Gonzalez R et al (2019) (2019) Atezolizumab plus cobimetinib and vemurafenib in BRAF-mutated melanoma patients. Nat Med 256(25):929–935. https://doi.org/10.1038/s41591-019-0474-7
Chaib S, López-Domínguez JA, Lalinde-Gutiérrez M et al (2024) The efficacy of chemotherapy is limited by intratumoral senescent cells expressing PD-L2. Nat Cancer 2024:1–15. https://doi.org/10.1038/s43018-023-00712-x
Luo F, Li H, Ma W et al (2024) The BCL-2 inhibitor APG-2575 resets tumor-associated macrophages toward the M1 phenotype, promoting a favorable response to anti-PD-1 therapy via NLRP3 activation. Cell Mol Immunol 21:60–79. https://doi.org/10.1038/S41423-023-01112-Y
Milde T, Fangusaro J, Fisher MJ et al (2023) Optimizing preclinical pediatric low-grade glioma models for meaningful clinical translation. Neuro Oncol 25:1920–1931. https://doi.org/10.1093/NEUONC/NOAD125
Yuan M, White D, Resar L et al (2021) Conditional reprogramming culture conditions facilitate growth of lower-grade glioma models. Neuro Oncol 23:770–782. https://doi.org/10.1093/NEUONC/NOAA263
Wang C, Sun M, Shao C et al (2024) A multidimensional atlas of human glioblastoma-like organoids reveals highly coordinated molecular networks and effective drugs. NPJ Precis Oncol 8. https://doi.org/10.1038/S41698-024-00500-5
Bajenaru ML, Hernandez MR, Perry A et al (2003) Optic nerve glioma in mice requires astrocyte Nf1 gene inactivation and Nf1 brain heterozygosity. Cancer Res 63:8573–8577
Zhu Y, Harada T, Liu L et al (2005) Inactivation of NF1 in CNS causes increased glial progenitor proliferation and optic glioma formation. Development 132:5577–5588. https://doi.org/10.1242/DEV.02162
Hegedus B, Dasgupta B, Shin JE et al (2007) Neurofibromatosis-1 regulates neuronal and glial cell differentiation from neuroglial progenitors in vivo by both cAMP- and Ras-dependent mechanisms. Cell Stem Cell 1:443–457. https://doi.org/10.1016/J.STEM.2007.07.008
Kaul A, Toonen JA, Gianino SM, Gutmann DH (2015) The impact of coexisting genetic mutations on murine optic glioma biology. Neuro Oncol 17:670–677. https://doi.org/10.1093/NEUONC/NOU287
Gronych J, Korshunov A, Bageritz J et al (2011) An activated mutant BRAF kinase domain is sufficient to induce pilocytic astrocytoma in mice. J Clin Invest 121. https://doi.org/10.1172/JCI44656
Isakson SH, Rizzardi AE, Coutts AW et al (2018) Genetically engineered minipigs model the major clinical features of human neurofibromatosis type 1. Commun Biol 1. https://doi.org/10.1038/S42003-018-0163-Y
Masuda T, Amann L, Sankowski R et al (2020) Novel Hexb-based tools for studying microglia in the CNS. Nat Immunol 21:802–815. https://doi.org/10.1038/S41590-020-0707-4
Boyer SW, Schroeder AV, Smith-Berdan S, Forsberg EC (2011) All hematopoietic cells develop from hematopoietic stem cells through Flk2/Flt3-positive progenitor cells. Cell Stem Cell 9:64–73. https://doi.org/10.1016/J.STEM.2011.04.021
Bowman RL, Klemm F, Akkari L et al (2016) Macrophage ontogeny underlies differences in tumor-specific education in brain malignancies. Cell Rep 17:2445–2459. https://doi.org/10.1016/J.CELREP.2016.10.052
Louis DN, Perry A, Wesseling P et al (2021) The 2021 WHO classification of tumors of the central nervous system: a summary. Neuro Oncol 23:1231–1251. https://doi.org/10.1093/NEUONC/NOAB106
Acknowledgements
T.M. is supported by The Everest Centre for Low-grade Pediatric Brain Tumours (GN-000707, The Brain Tumour Charity, UK). All figures were created with BioRender.com.
Funding
Open Access funding enabled and organized by Projekt DEAL. T.M. was supported by The Everest Centre for Low-grade Paediatric Brain Tumors (GN-000707, The Brain Tumour Charity, UK) and received research grants from BioMed Valley Discoveries, Inc., and Day One Biopharmaceuticals. TB is supported by the Deutsche Forschungsgemeinschaft, SFB-1479 – Project ID: 441891347 (P14).
Author information
Authors and Affiliations
Contributions
R.S., T.M. and F.S. conceived the idea for the article, R.S., T.B., D.K., T.M. and F.S. performed the literature search and data analysis, R.S. generated the figures, R.S., T.B., D.K., T.M. and F.S. drafted sections of and critically revised the manuscript. R.S. and F.S. edited, compiled, and organized this submission.
Corresponding authors
Ethics declarations
Conflict of interests
T.M. was supported by research grants from Biomed Valley Discoveries, Inc., and Day One Biopharmaceuticals.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Sigaud, R., Brummer, T., Kocher, D. et al. MOST wanted: navigating the MAPK-OIS-SASP-tumor microenvironment axis in primary pediatric low-grade glioma and preclinical models. Childs Nerv Syst (2024). https://doi.org/10.1007/s00381-024-06463-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00381-024-06463-z