Abstract
Objectives
Underestimation of concomitant patellofemoral instability in patients with anterior cruciate ligament (ACL) injury has aroused extensive attention. However, the characteristics of the combined injury is not well recognized. Hence, we aimed to characterize the features of the combined injury, and determine the radiographic risk factors.
Methods
Fifteen radiological parameters were identified after discussion and pilot-tested. Radiographic measurements were compared using the analysis of variance model with Tukey post hoc analysis. A stepwise binomial logistic regression was performed and a nomogram model combining the significant risk factors was created. The model performance was validated by C-index, calibration plot, and decision curve.
Results
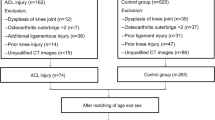
A total of 204 patients (mean [SD] age, 25.1 [6.7] years; 108 [52.9%] male) were included. The final model was updated through regression analysis using 4 parameters as significant risk factors: lateral femoral condyle ratio (OR (95% CI), 1.194 (1.023 to 1.409)), medial anterior tibial subluxation (mATS) (OR (95% CI), 1.234 (1.065 to 1.446)), medial posterior plateau tibial angle (mPPTA) (OR (95% CI), 1.266 (1.088 to 1.500)), and trochlear depth (OR (95% CI), 0.569 (0.397 to 0.784)). C-index for the nomogram was 0.802 (95% CI, 0.731 to 0.873) and was confirmed to be 0.784 through bootstrapping validation. Calibration plot established a good agreement between prediction and observation. Decision curve analysis showed that if threshold probability was over 10%, using the nomogram adds more benefit than either all or none scheme.
Conclusions
Lateral femoral condyle ratio, mATS, mPPTA, and trochlear depth are strong adverse predictors of patellofemoral instability in patients with ACL injury.
Clinical relevance
This study characterizes the radiological features of the combined injury. Patellofemoral instability should be noted when treating ACL injuries.
Key Points
• The radiological characteristics of the combined ACL injury and patellofemoral instability is not well recognized.
• Lateral femoral condyle ratio, mATS, mPPTA, and trochlear depth are predominant risk factors for patellofemoral instability in patients with ACL injury.
• Patellofemoral instability should be noted when treating ACL injuries.






Similar content being viewed by others
Abbreviations
- ACL:
-
Anterior cruciate ligament
- ACLI:
-
ACL injury
- ACLI + PI:
-
ACL injury and patellofemoral instability
- ANOVA:
-
Analysis of variance
- aNWI:
-
Axial notch width index
- CDI:
-
Caton-Deschamps index
- CI:
-
Confidence interval
- cNWI:
-
Coronal notch width index
- CT:
-
Computed tomography
- ICC:
-
Interclass correlation coefficient
- lATS:
-
Lateral anterior tibial subluxation
- lPPTA:
-
Lateral posterior plateau tibial angle
- LTI:
-
Lateral trochlear inclination
- mATS:
-
Medial anterior tibial subluxation
- mPPTA:
-
Medial posterior plateau tibial angle
- OR:
-
Odds ratio
- TGM:
-
Trochlear groove medialization
- TTL:
-
Tibial tubercle lateralization
- TT-TG:
-
Tibial tubercle–trochlear groove
References
Kaeding CC, Leger-St-Jean B, Magnussen RA (2017) Epidemiology and diagnosis of anterior cruciate ligament injuries. Clin Sports Med 36:1–8
Gornitzky AL, Lott A, Yellin JL, Fabricant PD, Lawrence JT, Ganley TJ (2016) Sport-specific yearly risk and incidence of anterior cruciate ligament tears in high school athletes: a systematic review and meta-analysis. Am J Sports Med 44:2716–2723
Musahl V, Karlsson J (2019) Anterior cruciate ligament tear. N Engl J Med 380:2341–2348
Schilaty ND, Nagelli C, Bates NA et al (2017) Incidence of second anterior cruciate ligament tears and identification of associated risk factors from 2001 to 2010 using a geographic database. Orthop J Sports Med 5:2325967117724196
Huang W, Ong TY, Fu SC, Yung SH (2020) Prevalence of patellofemoral joint osteoarthritis after anterior cruciate ligament injury and associated risk factors: a systematic review. J Orthop Translat 22:14–25
Weber AE, Nathani A, Dines JS et al (2016) An algorithmic approach to the management of recurrent lateral patellar dislocation. J Bone Joint Surg Am 98:417–427
Macura M, Veselko M (2010) Simultaneous reconstruction of ruptured anterior cruciate ligament and medial patellofemoral ligament with ipsilateral quadriceps grafts. Arthroscopy 26:1258–1262
Hiemstra LA, Kerslake S, Heard M, Buchko G, Lafave M (2016) Outcomes of surgical stabilization in patients with combined ACL deficiency and patellofemoral instability - a case series. Knee 23:1106–1111
Shankar V, Natiq Hussain S, Sahanand S, Rajan D (2020) Concurrent anterior cruciate ligament and medial patellofemoral ligament reconstruction: a case report and literature review. Cureus 12:e7717
Liao TC, Pedoia V, Majumdar S, Souza RB (2021) Longitudinal changes of patellar alignment before and after anterior cruciate ligament reconstruction with hamstring autograft. Am J Sports Med 49:2908–2915
Macri EM, Patterson BE, Crossley KM et al (2019) Does patellar alignment or trochlear morphology predict worsening of patellofemoral disease within the first 5 years after anterior cruciate ligament reconstruction? Eur J Radiol 113:32–38
Lin Z, Tang Y, Tan H, Cai D (2019) Patellofemoral kinematic characteristics in anterior cruciate ligament deficiency and reconstruction. BMC Musculoskelet Disord 20:82
Liao TC, Martinez AGM, Pedoia V et al (2020) Patellar malalignment is associated with patellofemoral lesions and cartilage relaxation times after hamstring autograft anterior cruciate ligament reconstruction. Am J Sports Med 48:2242–2251
Van de Velde SK, Gill TJ, DeFrate LE, Papannagari R, Li G (2008) The effect of anterior cruciate ligament deficiency and reconstruction on the patellofemoral joint. Am J Sports Med 36:1150–1159
Maniar N, Verhagen E, Bryant AL, Opar DA (2022) Trends in Australian knee injury rates: an epidemiological analysis of 228,344 knee injuries over 20 years. Lancet Reg Health West Pac 21:100409
Moons KG, Altman DG, Reitsma JB et al (2015) Transparent Reporting of a multivariable prediction model for Individual Prognosis or Diagnosis (TRIPOD): explanation and elaboration. Ann Intern Med 162:W1-73
Manske RC, Davies GJ (2016) Examination of the patellofemoral joint. Int J Sports Phys Ther 11:831–853
Chen J, Wu C, Ye Z, Zhao J, Xie G (2022) Tibial tuberosity-trochlear groove distance and its components in patients with and without episodic patellar dislocation: a study of 781 knees. J Bone Joint Surg Am 104:504–511
Zhang C, Zhang X, Fang Z et al (2019) The correlation between common 2D femoral notch parameters and 3D notch volume: a retrospective MRI study. BMC Musculoskelet Disord 20:146
Pfeiffer TR, Burnham JM, Hughes JD et al (2018) An increased lateral femoral condyle ratio is a risk factor for anterior cruciate ligament injury. J Bone Joint Surg Am 100:857–864
Ho CP, James EW, Surowiec RK et al (2015) Systematic technique-dependent differences in CT versus MRI measurement of the tibial tubercle-trochlear groove distance. Am J Sports Med 43:675–682
Tensho K, Akaoka Y, Shimodaira H et al (2015) What components comprise the measurement of the tibial tuberosity-trochlear groove distance in a patellar dislocation population? J Bone Joint Surg Am 97:1441–1448
Tensho K, Shimodaira H, Akaoka Y et al (2018) Lateralization of the tibial tubercle in recurrent patellar dislocation: verification using multiple methods to evaluate the tibial tubercle. J Bone Joint Surg Am 100:e58
Tanaka MJ, Elias JJ, Williams AA, Carrino JA, Cosgarea AJ (2015) Correlation between changes in tibial tuberosity-trochlear groove distance and patellar position during active knee extension on dynamic kinematic computed tomographic imaging. Arthroscopy 31:1748–1755
Dejour H, Walch G, Nove-Josserand L, Guier C (1994) Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc 2:19–26
Charles MD, Haloman S, Chen L, Ward SR, Fithian D, Afra R (2013) Magnetic resonance imaging-based topographical differences between control and recurrent patellofemoral instability patients. Am J Sports Med 41:374–384
Fick CN, Grant C, Sheehan FT (2020) Patellofemoral pain in adolescents: understanding patellofemoral morphology and its relationship to maltracking. Am J Sports Med 48:341–350
Carrillon Y, Abidi H, Dejour D, Fantino O, Moyen B, Tran-Minh VA (2000) Patellar instability: assessment on MR images by measuring the lateral trochlear inclination-initial experience. Radiology 216:582–585
Hashemi J, Chandrashekar N, Gill B et al (2008) The geometry of the tibial plateau and its influence on the biomechanics of the tibiofemoral joint. J Bone Joint Surg Am 90:2724–2734
Naendrup JH, Drouven SF, Shaikh HS et al (2020) High variability of tibial slope measurement methods in daily clinical practice: comparisons between measurements on lateral radiograph, magnetic resonance imaging, and computed tomography. Knee 27:923–929
Ye Z, Xu J, Chen J et al (2022) Steep lateral tibial slope measured on magnetic resonance imaging is the best radiological predictor of anterior cruciate ligament reconstruction failure. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-06923-6
McDonald LS, van der List JP, Jones KJ et al (2017) Passive anterior tibial subluxation in the setting of anterior cruciate ligament injuries: a comparative analysis of ligament-deficient states. Am J Sports Med 45:1537–1546
Narkbunnam R, Chareancholvanich K (2015) Effect of patient position on measurement of patellar height ratio. Arch Orthop Trauma Surg 135:1151–1156
Chen J, Ye Z, Wu C, Zhang X, Zhao J, Xie G (2022) Sulcus depth, congruence angle, Wiberg index, TT-TG distance, and CDI are strong predictors of recurrent patellar dislocation. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-07245-3
Goutallier D, Bernageau J, Lecudonnec B (1978) The measurement of the tibial tuberosity. Patella groove distanced technique and results (author’s transl). Rev Chir Orthop Reparatrice Appar Mot 64:423–428
Rodriguez IV, Cisa PM, Monuszko K et al (2022) Development and validation of a model for opioid prescribing following gynecological surgery. JAMA Netw Open 5:e2222973
Iasonos A, Schrag D, Raj GV, Panageas KS (2008) How to build and interpret a nomogram for cancer prognosis. J Clin Oncol 26:1364–1370
Liu W, Sun Z, Xiong H et al (2022) Development and validation of a prognostic nomogram for open elbow arthrolysis : the Shanghai Prediction model for Elbow Stiffness Surgical Outcome. Bone Joint J 104-B:486–494
Steyerberg EW, Harrell FE (2016) Prediction models need appropriate internal, internal-external, and external validation. J Clin Epidemiol 69:245–247
Vickers AJ, Cronin AM, Elkin EB, Gonen M (2008) Extensions to decision curve analysis, a novel method for evaluating diagnostic tests, prediction models and molecular markers. BMC Med Inform Decis Mak 8:53
Vickers AJ, Elkin EB (2006) Decision curve analysis: a novel method for evaluating prediction models. Med Decis Making 26:565–574
Zhang Z, Rousson V, Lee WC et al (2018) Decision curve analysis: a technical note. Ann Transl Med 6:308
Fitzgerald M, Saville BR, Lewis RJ (2015) Decision curve analysis Jama 313:409–410
Botchu R, Obaid H, Rennie WJ (2013) Correlation between trochlear dysplasia and anterior cruciate ligament injury. J Orthop Surg (Hong Kong) 21:185–188
Ntagiopoulos PG, Bonin N, Sonnery-Cottet B, Badet R, Dejour D (2014) The incidence of trochlear dysplasia in anterior cruciate ligament tears. Int Orthop 38:1269–1275
Chen M, Qin L, Li M, Shen J (2020) Correlation analysis between femoral trochlear dysplasia and anterior cruciate ligament injury based on CT measurement. Quant Imaging Med Surg 10:847–852
Akgün AS, Agirman M (2021) Associations between anterior cruciate ligament injuries and patella alta and trochlear dysplasia in adults using magnetic resonance imaging. J Knee Surg 34:1220–1226
Isiklar S, Ozdemir ST, Gokalp G (2021) An association between femoral trochlear morphology and non-contact anterior cruciate ligament total rupture: a retrospective MRI study. Skeletal Radiol 50:1441–1454
Kwak YH, Nam JH, Koh YG, Kang KT (2021) Correlation of femoral trochlear dysplasia with anterior cruciate ligament injury in skeletally immature patients. Orthop J Sports Med 9:23259671211022690
Paiva M, Blond L, Holmich P et al (2018) Quality assessment of radiological measurements of trochlear dysplasia; a literature review. Knee Surg Sports Traumatol Arthrosc 26:746–755
Prakash J, Seon JK, Woo SH, Jin C, Song EK (2016) Comparison of radiological parameters between normal and patellar dislocation groups in Korean population: a rotational profile CT-based study. Knee Surg Relat Res 28:302–311
Arendt EA, England K, Agel J, Tompkins MA (2017) An analysis of knee anatomic imaging factors associated with primary lateral patellar dislocations. Knee Surg Sports Traumatol Arthrosc 25:3099–3107
Hashemi J, Chandrashekar N, Mansouri H et al (2010) Shallow medial tibial plateau and steep medial and lateral tibial slopes: new risk factors for anterior cruciate ligament injuries. Am J Sports Med 38:54–62
Song GY, Zhang H, Zhang J, Zhang ZJ, Zheng T, Feng H (2020) Excessive preoperative anterior tibial subluxation in extension is associated with inferior knee stability after anatomic anterior cruciate ligament reconstruction. Am J Sports Med 48:573–580
Ziegler CG, DePhillipo NN, Kennedy MI, Dekker TJ, Dornan GJ, LaPrade RF (2021) Beighton Score, tibial slope, tibial subluxation, quadriceps circumference difference, and family history are risk factors for anterior cruciate ligament graft failure: a retrospective comparison of primary and revision anterior cruciate ligament reconstructions. Arthroscopy 37:195–205
Gobbi RG, Videira LD, Dos Santos AA et al (2022) Anatomical risk factors for anterior cruciate ligament injury are not important as patellar instability risk factors in patients with acute knee injury. J Knee Surg 35:676–683
Foos J, Amakoutou K, Cooperman DR, Liu RW (2021) A cadaveric anatomical study of the relationship between proximal tibial slope and coronal plane deformity. J Knee Surg. https://doi.org/10.1055/s-0041-1728816
Hermans K, Claes S, Bellemans J (2013) Valgus instability as a cause for recurrent lateral patellar dislocation: a new mechanism for patellofemoral instability? Acta Orthop Belg 79:495–501
Flury A, Jud L, Hoch A, Camenzind RS, Fucentese SF (2021) Linear influence of distal femur osteotomy on the Q-angle: one degree of varization alters the Q-angle by one degree. Knee Surg Sports Traumatol Arthrosc 29:540–545
Grassi A, Macchiarola L, Urrizola Barrientos F et al (2019) Steep posterior tibial slope, anterior tibial subluxation, deep posterior lateral femoral condyle, and meniscal deficiency are common findings in multiple anterior cruciate ligament failures: an MRI case-control study. Am J Sports Med 47:285–295
Pfeiffer TR, Burnham JM, Kanakamedala AC et al (2019) Distal femur morphology affects rotatory knee instability in patients with anterior cruciate ligament ruptures. Knee Surg Sports Traumatol Arthrosc 27:1514–1519
Li K, Zheng X, Li J et al (2021) Increased lateral femoral condyle ratio is associated with greater risk of ALC injury in non-contact anterior cruciate ligament injury. Knee Surg Sports Traumatol Arthrosc 29:3077–3084
Zhang LK, Wang XM, Niu YZ, Liu HX, Wang F (2016) Relationship between patellar tracking and the “screw-home” mechanism of tibiofemoral joint. Orthop Surg 8:490–495
Funding
This study has received funding by Shanghai Municipal Health Commission key priority discipline project; Shanghai Spinal Disease and Trauma Orthopedics Research Center, Grant No. 2022ZZ01014; Exploratory Research Program of Shanghai Sixth People’s Hospital, Grant No. YNTS202001; and Shanghai Municipal Hospital Orthopedic Specialist Alliance.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Jinzhong Zhao.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors (Jingyi Guo) has significant statistical expertise.
Informed consent
Written informed consent was not required for this study because it was a retrospective study, all patients could not be identified, only basic and imaging data were collected, and the extracted data did not contain patient names.
Ethical approval
Institutional Review Board approval was obtained.
Study subjects or cohorts overlap
Not available.
Methodology
-
retrospective
-
diagnostic study
-
performed at one institution
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chen, J., Wu, X., Guo, J. et al. Characterization of the CT-based risk factors for concomitant patellofemoral instability in patients with anterior cruciate ligament injury. Eur Radiol 34, 250–259 (2024). https://doi.org/10.1007/s00330-023-10028-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-10028-0