Abstract
Extracellular vesicles such as exosomes, microvesicles, apoptotic bodies, and large oncosomes have been shown to participate in a wide variety of biological processes and are currently under intense investigation in many different fields of biomedicine. One of the key features of extracellular vesicles is that they have relatively large surface compared to their volume. Some extracellular vesicle surface molecules are shared with those of the plasma membrane of the releasing cell, while other molecules are characteristic for extracellular vesicular surfaces. Besides proteins, lipids, glycans, and nucleic acids are also players of extracellular vesicle surface interactions. Being secreted and present in high number in biological samples, collectively extracellular vesicles represent a uniquely large interactive surface area which can establish contacts both with cells and with molecules in the extracellular microenvironment. Here, we provide a brief overview of known components of the extracellular vesicle surface interactome and highlight some already established roles of the extracellular vesicle surface interactions in different biological processes in health and disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Extracellular vesicles (EVs) are membrane-enclosed heterogeneous structures that are secreted by all cells [1] and have many different physiological and pathophysiological roles [2]. They include small EVs of endosomal origin (exosomes) as well as plasma membrane-derived intermediate-sized (100–1000 nm) microvesicles, and large sized (> 1 μm) apoptotic bodies and large oncosomes [3, 4]. In the past few years, EVs attracted rapidly growing scientific interest from various fields of biomedicine.
Surface molecules of EVs are of critical functional significance as they (i) establish connections with the surrounding micro milieu and with cells, (ii) determine EV mobility, (iii) mediate cellular uptake, (iv) affect immune recognition of EVs (also via posttranslational modifications) by the innate and adaptive immune systems, and (v) may represent effector molecules (such as FasL). On the other hand, from a researcher’s perspective, they enable identification, affinity isolation, and molecular classification of EVs and EV subtypes, and enable the use of EVs as biomarkers.
Here, we overview EV surface interactions with the surrounding microenvironment (extracellular matrix (ECM) molecules or components of the blood plasma) and with cells and provide examples for the functional relevance of the surface interactions of EVs.
Evidences for exofacial localization of EV proteins as partners in EV surface interactions
When considering EV surface interactions, it is of crucial importance to define EV molecules with exofacial topology that can serve as interaction partners. EV surface molecules are identified by immunolabeling (immunogold electron microscopy, flow cytometry or immunochemistry using confocal or super resolution microscopy). These widely used approaches enabled identification of “canonical” EV surface proteins including tetraspanins (CD9, CD63, and CD81), integrins (ITG), cell adhesion molecules (CAM), and growth factor receptors [5]. The presence of these molecules has been confirmed by many different laboratories.
Mass spectrometry (MS)-based proteomic characterization has proven to be a very efficient and widely used tool to characterize EVs. This approach was first used by Thery et al. [6] for the characterization of exosomes followed by many other studies over the years. These proteomic data are also publicly available from databases (Exocarta, EVpedia, and Vesiclepedia) (http://student4.postech.ac.kr/evpedia2_xe/xe/, http://www.exocarta.org/, http://www.microvesicles.org/). However, MS does not enable identification of the precise topology of EV proteins. Possible membrane defects due to centrifuge-based EV isolation procedures or the occurrence of inverted vesicles may enable labeled antibodies to recognize internal cargo molecules of EVs making the distinction between EV surfaces and internal cargo proteins challenging. This possibility cannot be completely excluded even when using, e.g., antibody-coated EV arrays [7].
Recently, a combination of proteinase treatment and subsequent biotinylation, a strategy known from studying cellular membrane proteins, has been suggested for the study of luminal and surface-accessible EV cargo [8]. Even with this approach, it cannot be determined whether the surface-accessible EV proteins were present already at the time of EV production or they were subsequently acquired from conditioned media or biological fluids.
Strong evidence for EV surface localization of certain molecules comes from the ability to target the putative protein (or other molecule) for affinity isolation of EVs. Anti-EpCAM and anti-A33 antibodies were used for immunocapture of colon cancer-derived exosomes [9]. Similarly, anti-tetraspanin (antiCD63, CD9 and CD81) antibodies can be used for immunoisolation of EVs [3]. Immune electron microscopy revealed that hsp70 is localized on the surface of exosomes [10], and a synthetic peptide (Vn96) with high affinity for heat shock proteins has proven useful for affinity enrichment of cancer EVs [11,12,13]. Furthermore, EVs can be isolated by heparin affinity purification. Suggested heparin-binding proteins on EVs include histones, heat shock proteins, and annexin; however, definite interacting ligand(s) have not been determined yet [14]. Of note, not only proteins but also other surface molecules are targeted for EV affinity capture. As an example, the recently identified phosphatidyl serine (PS) receptor TIM4 [15] was found efficient in capturing PS-exposing EVs [16].
For immunodetection of EV surface molecules, dot scan (antibody microarray) has been used recently. It showed moderate/high levels of CD19, CD5, CD31, CD44, CD55, CD62Lm, CD82, HLA-A, B, and C and low levels of CD21, CD49c, and CD63 on EVs. The authors proposed these EV surface molecules as a diagnostic signature for chronic lymphocytic leukemia [17]. Furthermore, surface plasmon resonance (SPR) has been used recently for the simultaneous detection of both EV and cancer markers on exosomes from breast cancer cells [18]. Moreover, exosome “surfaceome” profiling was carried out by an initial MS testing EVs secreted by 13 pancreatic ductal adenocarcinoma cell lines and 2 non-neoplastic cell lines. MS was followed by identification of candidate biomarkers and validation by an immunocapture pulldown assay. In this assay, a multiplexed panel of antibodies was used that included anti-CLDN4, EPCAM, CD151, LGALS3BP, HIST2H2BE, and HIST2H2BF antibodies for the enrichment of tumor-specific exosomes for subsequent studies [19].
Numerous pieces of evidence suggest that surface molecules on EVs determine the uptake and biological functions of EVs. As one example, blockade of exosome surface SIRPα (CD47) was shown to be effective in increasing cancer cell phagocytosis [20].
Interaction of EVs with the plasma membrane of cells
Surface interactions of EVs with the plasma membrane are of outstanding importance since such interactions mediate binding of EVs to cells resulting in signal transduction or uptake of EVs by cells. It is now established that EV-target cell interactions involve tetraspanins, integrins, ECM proteins, immunoglobulin superfamily members, proteoglycans, and lectins [21, 22]. Details of EV docking and entry to cells are not in the focus of this review, as these interactions have recently been reviewed elsewhere [21, 22]. To illustrate the outstanding functional significance of the interaction of EV surface molecules with those of the plasma membrane, here, we only refer to the plethora of EV-immune cell interactions including cell-free antigen presentation by EVs [23], Fas ligand or TRAIL-mediated cell death induction by EVs [24,25,26], or the transfer of immune checkpoint molecules (PD1, PDL-1) by EVs [27].
Here, we also point out the significance of externalization (translocation to the outer leaflet of a phospholipid bilayer) of phosphatidyl serine (PS), a characteristic feature of many EVs. The negatively charged, surface-exposed phospholipid PS is recognized by numerous plasma membrane receptors either directly or indirectly, via bridging proteins. Direct PS sensing receptors include the previously mentioned TIM4 [15], the receptor for advanced glycation end products, RAGE [28], brain-specific angiogenesis inhibitor 1 Bai-1 [29], and stabilin-2 [30]. Indirect PS recognition and subsequent uptake is mediated by milk fat globule-EGF factor 8, MFGE8 [31] which forms a molecular bridge between PS and plasma membrane integrins (such as αvβ3) [31] (Fig. 1a).Of note, MFGE8 is not only detectable on the surface of exosomes [32], but it is also secreted by cells as an EV-MFGE8 complex [33]. This EV-protein complex secretion is similar to secretion EV-integrin-FN and EV-C3b complexes (Fig. 1b).
Examples for EV surface interactions with the plasma membrane and components of the extracellular matrix. a One of the best characterized interactions between the plasma membrane and the surface of EVs is mediated by proteins that recognize externalized phosphatidyl serine (PS) on EVs. Direct interactions with PS include those with TIM4, stabilin-2, RAGE, or BAI-1. Indirect interactions include those between the PS-binding MFGE-8 and αvβ3 integrin as well as the PS-binder GAS-6 and the MER tyrosine kinase on the cell. b Endocytosis of fibronectin (FN) or C3b complement protein is followed by an association of these molecules with intraluminal vesicles within MVBs followed by secretion of exosomes with surface-associated FN or C3b. c Interaction of EVs with ECM is mediated by integrins or CD44. d FN forms a bridge between HSPGs present on both EV surface and plasma membrane, and mediates EV uptake by cells
Of note, similar indirect recognition of PS is also described in the case of PS recognized by the growth arrest-specific protein 6, Gas6. The PS-Gas6 complex was shown to activate TAM family member MER tyrosine kinases on the surface of macrophages triggering uptake and inducing an anti-inflammatory phenotype [34].
Until now, most studies investigated PS–plasma membrane receptor interactions focusing on the uptake of apoptotic cell-derived vesicles. This is explained by the fact that apoptosis has been long known to be accompanied by PS externalization. However, given that externalized PS is characteristic for many EV surfaces, and annexin V is used broadly to detect EVs, it seems plausible that PS-mediated interactions with the plasma membrane govern the binding and uptake of non-apoptotic EVs as well. Indeed, there are accumulating pieces of evidence that show PS-mediated EV uptake or signaling in the case of non-apoptotic vesicles also [35, 36].
Interaction of EV surfaces with the extracellular matrix: extracellular binding or re-cycling?
It is an important question whether EVs secreted by cells of tissues rich in extracellular matrix (ECM) such as connective tissue, interact with matrix molecules. Accumulating pieces of evidence suggest that indeed such interactions exist and their significance is increasingly recognized. It may seem intuitive that EV surfaces interact with the ECM components upon secretion, once being surrounded by the macromolecular ECM milieu. This may predict that EV membrane deposition of matrix molecules results from binding of these molecules onto EV surfaces extracellularly. Although newly secreted EVs evidently establish interactions with ECM molecules in tissues and body fluids (Fig. 1c), there seems to be another mechanism, which may explain the presence of certain ECM molecules on the surface of EVs. It has been proposed recently that cells endocytose ECM molecules and re-secrete them on the exofacial surface of EVs (exosomes) [37] (Fig. 1b). This continuous endocytosis and re-secretion of ECM components guarantees an abundant source of ECM-carrying EVs, which may play an important role in cell migration. Such endocytosis and EV-associated re-secretions has been recently demonstrated in the case of fibronectin (FN)–integrin complexes. FN is endocytosed in association with integrins, it is then targeted to MVB, where it binds to the surface of intraluminal vesicles in correct topology to interact with both the cell surface and other ECM molecules (e.g. collagen fibers) [37].
Kowal et al. used immuno-isolated EVs by CD9, CD63, and CD81-specific antibodies. The authors have demonstrated the existence of a subtype of small EVs (sEVs) that the authors referred to as “dense sEVs” which carried FN, complement, prothrombin, and serum albumin, while another subpopulation of sEVs (“light sEVs”) did not carry any of these molecules on its surface [3]. Whether dense sEVs acquired their ECM coat from the conditioned medium of the cells upon secretion or were secreted with surface-bound ECM molecules, was not investigated in this study.
Fibronectin
One of the most extensively studied ECM molecules with respect to surface interaction with EVs is FN. FN binds multiple integrins. It has been shown that reticulocyte maturation is accompanied by release of EVs carrying α4β1 integrin (Very Late Antigen-4, VLA4) by which EVs were shown to bind to FN [38]. Myeloma-derived EVs (exosomes) were found to carry FN on their surface [39]. This exofacially bound FN could interact with cell surface heparan sulfate (through its Hep-II domain). The authors showed that FN could simultaneously bind to heparan sulfate proteoglycans both on the exosomal and the plasma membrane surfaces thereby facilitating cellular uptake of EVs [39] (Fig. 1d).
There are multiple evidences that beyond facilitating cell binding and cellular uptake, there are other functional consequences of EV-association of FN. A striking function of FN on EVs is related to cellular motility. As described above, FN bound to integrins on exosomes was shown to promote directional cancer cell movement by reinforcing transient polarization states and adhesion assembly [37]. Furthermore, exosomal FN was shown to induce IL-1β expression by macrophages [40]. We have shown recently that DNA present on the surface of small EVs secreted by stressed cells facilitated interaction of EVs with FN [41]. Finally, FN on circulating EVs in liquid biopsy samples of breast cancer patients samples was suggested to be a promising cancer biomarker [42].
Glycosaminoglycans (GAGs) and proteoglycans
Heparan sulfate proteoglycans (HSPGs) are abundant glycoproteins having a core protein to which one or more heparan sulfate (HS) glycosaminoglycan (GAG) chains are attached covalently. Membrane-bound HSPGs include syndecans and glypicans. Interestingly, syndecans and glypicans are present both on the plasma membrane of the EV-releasing cells and the membrane of EVs. Cancer cell-surface HSPGs of the syndecan and glypican types were shown to mediate internalization of EVs [43]. This process was readily inhibited by free heparan sulfate. Importantly, the same study demonstrated sorting of HSPGs to EVs (exosomes) [43]. As we mentioned earlier, by forming a bridge between EV and plasma membrane HSPGs, FN was shown to mediate EV uptake [39].
Recently, the presence of glypican 1 associated with exosomes was demonstrated by different groups [44,45,46]. Its proposed exploitation as a biomarker of pancreatic cancer is currently under investigation.
Among other ECM molecules, hyaluronan (HA) synthesis was shown to be associated with the shedding of HA-coated EVs by human mesenchymal stem cells (Fig. 1d). HA coating on EVs was proposed to (i) contribute to HA-mediated tissue regeneration, (ii) regulate interactions of EVs with target cells, and (iii) play a role in ECM remodeling [47]. Not only HA but also the HA receptor CD44 is associated with EV surfaces. Ovarian cancer cell invasion was shown to be supported by exosomal transfer of CD44 to peritoneal mesothelial cells [48]. CD44 was also identified as a component of the cancer cell-derived circulating EV-specific diagnostic signature [17] and was recently shown to serve as one of the diagnostic and prognostic exosomal biomarkers of breast cancer [49]. Interestingly, transcripts of CD44 are also carried horizontally as internal cargo in human mesenchymal stem cell-derived HA-coated EVs [47].
The role of integrins in EV-ECM interactions
Integrins represent a group of transmembrane receptors that play a role in cell-ECM adhesion. Known integrin ligands in the ECM include molecules such as fibronectin, collagen, vitronectin, and laminin. Numerous pieces of evidence support that among EV surface adhesion molecules, integrins play a distinguished role. Tumor EVs (exosomes) can promote cancer progression by transferring integrin transcripts horizontally and by selecting metastatic sites as reviewed recently [50]. Tumor-derived EV (exosome) integrins α6β4 and α6β1 correlated with the development of lung metastasis, while exosomal integrin αvβ5 was associated with liver metastasis [51]. This important observation suggests that there is a potential of EVs to predict metastatic sites of tumors based on their surface integrins.
EVs and the blood plasma
Immunoglobulins
The association of EVs with plasma factors, notably immunoglobulins and complement factors (Fig. 2a, b), is best described concerning the spectrum of autoimmune rheumatological diseases. Systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) are autoimmune diseases with a significant type III hypersensitivity component meaning that immune complexes and complement activation contribute to the disease pathology.
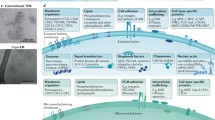
Examples for EV surface-associated molecules. a Antibody binding to EVs has been demonstrated, e.g., in numerous autoimmune diseases. b Both complement factors and complement regulatory proteins have been shown to associate with EV surfaces. c On EVs from blood plasma, different coagulation factors are also identified. d EV-associated cytokines include TNF bound to TNF receptor as well as TGFβ bound to TGFβR3 (betaglycan) on EV surfaces. e Both bacterial and mammalian EVs have been demonstrated to carry surface-associated DNA and DNA-binding proteins. In the case of mammalian EVs, both mitochondrial and nuclear DNA were found on EV surfaces. f A surprisingly large variety of EV surface enzymes were identified that can bind and cleave protein or glycan substrates of the EV microenvironment
EVs have been known to associate with autoantibodies in several autoimmune diseases, forming pro-inflammatory immune complexes contributing to disease pathology as we reviewed recently [52]. In RA synovial fluid, platelet EVs display autoantigens and form immune complexes, which potently activate neutrophils thereby perpetuating inflammation [53]. SLE is an immune complex disease where disease symptoms arise due to the reduced clearance of immune complexes, which leads to complement-mediated inflammation. EVs also associate with immunoglobulins and enhance the formation of such pathological immune complexes in SLE [54]. A recent study showed that distinct subpopulations of EVs harboring immunoglobulins were associated with distinct clinical characteristics of SLE and may therefore serve as biomarkers in future [55].
Autoimmune phenomena can also arise due to autoantibodies produced against nucleic acids. EV-associated chromatin is normally digested off by DNAse1L3. The loss of this mechanism can lead to the formation of autoantibodies which in turn can cause autoimmunity [56].
Complement
It was demonstrated that complement activation occurs on platelet-derived microvesicles (also referred to as microparticles). Complement proteins (C3b and C5b-9) were shown to deposit on the surface of platelet-derived EVs exposed to blood plasma. Of note, not only complement proteins but also complement regulatory proteins (C1-INH, CD55, and CD59) were present on platelet EVs. The authors proposed that these EVs may present concentrated activated complement components to targets in the blood vessels [57].
Complement components have a major role in the clearance of apoptotic cells. In SLE, the mechanism of apoptotic cell clearance is damaged which leads to the disease symptoms of widespread inflammation due to chronic complement activation. Complement components associated with EVs and an altered binding of C3 components to EVs were observed in SLE even though there was no difference in the concentration of EVs between SLE patients and healthy subjects. SLE patients had higher levels of C3d-positive EVs and lower levels of C3b and C3ib-positive EVs. Since the latter components opsonize cells and EVs for phagocytosis, this difference could also contribute to chronic inflammation [58]. Association of complement factors with EVs in different types of renal disease has been extensively reviewed in [59].
It appears that in autoimmune and renal diseases, binding of different complement factors to EVs is preferential. Similarly, the attachment of complement factors, immunoglobulins, and other serum components to artificial particles depends on the particles’ surface chemistry. Differential binding of such plasma components has an influence on the adjuvant properties of the particles and thus has an influence on the use of these particles in vaccine delivery. Importantly, complement factors were necessary for the uptake of the artificial particles by antigen presenting cells via complement receptor 3 in mice [60].
EV-associated complement proteins may not only directly attach onto EVs upon exposure to blood plasma. C3 fragments were detected by immune electron microscopy in MVBs on the surface of intraluminal vesicles [60]. This may represent another example for endocytic uptake and exosomal re-secretion of an extracellular protein. These C3b-coated EVs were suggested to have an immunomodulatory role by enhancing the antigen presentation [60] (Fig. 2b).
Association of coagulation factors with EVs
Early evidence for procoagulant surfaces in platelet-free blood plasma was published by Wolf and collegues and was described as “platelet dust” back in 1967 [61]. Since then, a high number of studies confirmed that platelet-derived EVs, highly abundant in blood plasma, indeed have procoagulant properties. Furthermore, non-platelet EVs such as tumor derived vesicles [62] proved to affect hemostasis partially by assembling factors of coagulation on their surface in the blood plasma. The most extensively studied two components of EVs in coagulation are phosphatidylserine (PS) and tissue factor (TF) (Fig. 2c).
As a high percentage of platelet-derived MVs bear the anionic phospholipid PS on their outer membrane, they facilitate the assembly of several proteins of the coagulation cascade. These proteins contain positively charged γ-carboxyglutamic acid domains to which PS can bind with electrostatic interaction. These factors include VII, IX, X, and prothrombin [63]. Underlining the importance of PS-positive EV formation in hemostasis, patients suffering from a rare bleeding disorder (Scott syndrome) were found to have reduced floppase activity resulting in faulty PS externalization and reduced microparticle shedding [64].
Also, TF, a transmembrane receptor of factor VII/VIIa, can be present on MVs (vesicles often referred to as microparticles, MPs in coagulation studies). The elevated activity levels of this protein have been detected in various diseases (such as in acute liver injury, cirrhosis, urinary tract infection, endotoxemia, influenza, cancer, and related thromboembolism [65]). The platelet origin of TF on platelet MVs and the overall relevance of TF-bearing platelet MVs have been questioned by several authors [66,67,68]. However, the role of TF positive EVs irrespective whether they originate form platelets, tumor cells, endothelial cells, or leukocytes is clear in various hemostatic diseases and diseases tipically presenting with thrombembolic complications (as detailed in the comprehensive review by Owens and Mackman [63]). The presence of TF on EVs makes the presence of its specific inhibitor molecule, tissue factor pathway inhibitor (TFPI), also probable [63].
In addition to assembling factors that initiate the coagulation cascade, platelets and their MPs also can present specific binding sites for factors V, IX, and VIII [69,70,71]. Indeed, these binding sites can be found concentrated on MPs relative to platelets. In the case of factor Va and VIIIa, a 10-fold, while in the case of factor IXa, a 2-fold concentration of factor binding sites was observed in the above mentioned studies [69,70,71]. Another factor, von Willebrand Factor (vWF), an interaction partner of both glycoproteins GPIb and GPIIbIIIa, was found to be attached to platelet- and also to endothelial cell-derived EVs [72, 73]. Together, the accumulation of PS and of other coagulation factor binding sites enables the surface of platelet MPs to enhance coagulation approximately 50–100-fold as compared to platelets [74].
Interestingly, depending on what stimuli the parent cell recieved, MPs may bear different surface molecules resulting in different binding features. For instance, platelets activated with thrombin or collagen were found to shed MPs exposing GPIIbIIIa complexes binding fibrinogen, while those activated with C5b-9 shed non-GPIIbIIIa-exposing MPs [70].
Although the effect of platelet-derived microvesicles has been studied most widely, it is important to note that activated platelets also secrete exosomes [75]. However, their association with coagulation factors in plasma is questionable, as they, if at all, bear very low levels of PS [76]. Also, it is controversial whether plasma exosomes of different cellular origin bear TF [77].
Association of EVs with lipoproteins
Isolation of EVs from human blood plasma or serum is often confounded by the co-isolated lipoproteins [78,79,80,81]. Moreover, antibody-mediated depletion of lipoproteins [82] and lipoprotein apheresis [83] both resulted in loss of EV content as well. On the other hand, MS analysis of VLDL and LDL particles purified from human blood plasma revealed the presence of EV proteins (CD14, LDL-receptor, HLA class I molecules, and protein S100-A8) in these isolates [84]. Taken together, these data suggest that beyond the shared physiological parameters, there might be an association between lipoproteins and EVs as well. In vitro association has already been demonstrated by transmission electron microscopy [80]. However, experimental data are not available yet in support of an in vivo association of EVs and lipoproteins. Exchange of the protein and lipid content between lipoproteins is an established phenomenon [85,86,87,88]. Exchange of ApoE between lipoproteins and hepatitis C virus lipoviral particles has been also described [89]. Moreover, in vitro SR-B1-dependent transfer of a fluorescent phospholipid from engineered HDL nanoparticles to exosomes was also reported [90]. Finally, ApoE has been implicated in amyloid formation of pigment cells [91], and it has been shown that in these cells, ApoE associates with intraluminal vesicles and is secreted on the surface of exosomes [92].
Further blood plasma proteins associated with the surface of circulating EVs
Beside the known role of EVs as carriers of luminal cargo, EVs may also carry a significant surface cargo. Technically challenging to investigate, so far, very little is known about the externally adsorbed proteins. It is likely that the external cargo of EVs is at least partly acquired in body liquids after the EVs have been shed. As an example, blood plasma-derived EVs commonly carry substantial amounts of albumin [93]. In line with this, proteomics data in EV databases (http://student4.postech.ac.kr/evpedia2_xe/xe/, http://www.exocarta.org/, http://www.microvesicles.org/), [94,95,96] show that blood plasma-derived EVs co-isolate with numerous blood plasma proteins. Given the known presence of integrins and HSPGs on EVs, integrin ligands and heparin binding proteins are evident potential partners to establish interactions on the surface of circulating EVs. Furthermore, phosphatidyl serine binding proteins (such as MFGE8) and glycan binding galectins are obvious interaction partners of EVs in the circulation. Systemic analysis of EVs surface interactions with blood plasma proteins is still lacking.
Association of EVs with cytokines/chemokines
An increasing number of data support that EVs are capable of carrying various cytokines [2]. In most instances, these cytokines are carried in EVs as part of the internal cargo. However, it was shown that EVs carry a full-length 55-kDa tumor necrosis factor receptor 1 (TNFR1). Importantly, it was demonstrated by the authors that HUVEC-derived exosomes carried bound TNF [97] (Fig. 2d).
In addition, TGF beta was shown to be associated with the cell-surface chondroitin sulfate/heparan sulfate proteoglycan betaglycan (also referred to as transforming growth factor beta receptor III, TGFBR3) on the surface of cancer cell-derived exosomes. Although the authors found that the kinetics and magnitude of biological response were similar irrespective if they used soluble or EV-associated TGF beta, there were some qualitative differences in the elicited cellular responses [98] (Fig. 2d). Although it is tempting to hypothesize that additional cytokines (including chemokines) may be carried on the surface of EVs in association with EV surface proteoglycans, a systemic analysis of this question has not been performed yet.
DNA associated with the surfaces of EVs
In bacteria, outer membrane vesicle (OMV)-associated DNA has been shown to mediate inter- and intra-species horizontal gene transfer by carrying antibiotic resistance genes and virulence factor [99,100,101], and participating in the establishment of bacterial biofilms [102, 103]. Recently, it was also reported that OMV-associated DNA was found predominantly on the outer surface of OMVs [104].
In mammalian systems, most studies so far focused on DNA encapsulated in EVs as an internal cargo, and only very few reports investigated the EV surface-associated DNase-sensitive DNA. Of note, these studies drew attention towards the potential of EV surface-associated DNA in horizontal gene transfer [105], induction of autoimmunity [56], and cellular uptake [106]. Recently, we have shown that antibiotic-exposed cells undergoing genotoxic shock secreted small EVs (exosomes) with surface-associated DNA which was predominantly mitochondrial DNA [41]. The amount of this DNA was not enhanced by induction of apoptosis of the EV-releasing cells. As mentioned earlier, exosome surface-associated DNA was capable of mediating EV binding to FN [41] (Fig. 2e).
Enzymes associated with EV surfaces
Several pieces of evidence support the presence and activity of EV-associated enzymes as reviewed recently [107]. Thus, enzymes do not only represent components of the EV internal cargo but are also characterized by active exofacial enzymes. These include both proteases MT1-MMP (MMP-14) [108], ADAM17 [109], insulin-degrading enzyme (IDE) (insulin-like), and EV surface-associated glycosidases such as sialidase NEU3 [110, 111] and heparanase [112]. Importantly, EV surface-associated proteases and glycosidases may exert their function in concert with one another in matrix degradation. In addition, flow cytometry of isolated EVs bound to latex beads demonstrated the presence of multiple other enzymes (MMPs-2, -3, -9, -13, -14, ADAM-10, ADAM-17, ADAMTS-5, ADAMTS-8, uPAR, and hyaluronidase) [113]. EV-associated enzymes may (i) facilitate cell and EV mobility by degrading ECM macromolecules as substrates, (ii) release bound growth factors or chemokines, and (iii) destruct amyloid β plaques [114] (Fig. 2f).
EV surface-associated thiols
Thiol interactions are relevant both in the release and uptake of EVs, and it is highly likely that the content and composition of exofacial thiols has a vast influence on the interactions of EVs with their environment including macromolecules. The total surface thiol content of EVs can also be utilized for labeling purposes [115]. Plasma-derived and tissue culture-derived EVs can equally be labeled by thiol-reactive fluorescent reagents. However, it is important to be aware that contaminating plasma proteins interfere with such labeling and therefore, a dual labeling protocol of EV thiols is preferable from plasma samples [115]. Certain plasma proteins, like albumin, have a reactive thiol moiety [116], and interactions with EVs may take place via thiol interactions. In particular, in the case of albumin, it seems feasible that EVs form part of the “albuminome” potentially extending their half-life in the circulation via interacting with albumin. Albumin certainly appears among the molecules associated with EVs as discussed above. Redox regulation of cellular surface molecules is an emerging factor affecting cellular functions. Importantly, adhesion molecules such as integrins underlie redox regulation. Reducing the α4-integrin by N-acetyl-cysteine leads to increased FN adhesion and cellular aggregation of Jurkat cells [117]. Similar redox regulation may be relevant in EV biology. EV-associated integrin regulation is of particular interest, since distinct expression pattern of integrins on EVs is responsible for organotropism in cancer metastasis [51]. Therefore, redox regulation of exofacial molecules on EVs is likely to affect their functions.
Several thiol-reactive antioxidants are present in the plasma, notably certain members of the thioredoxin family such as peroxiredoxins 1, 2, and 4 and different forms of thioredoxin [118]. These thiol-reactive antioxidants are also known to appear on the surface of cells [118, 119]. Therefore, it is to be expected that these molecules also appear on the surface of EVs either as membrane proteins or plasma proteins associating with the EVs. Indeed, peroxiredoxin 2 was present on the surface of EVs [120, 121], and peroxiredoxin1 (Prdx1)-positive EVs were elevated in rheumatoid arthritis (RA) patient plasma compared with healthy controls which may be a marker of inflammation [115]. Since Prdx 1 is also present as a free protein in plasma, it may be released together with EVs or it associates with EVs after release, in the plasma. Protein disulfide isomerase is thought to be responsible for regulating cell surface thiols [122] and associated with EV surface, and it also seems to activate platelets [123].
Conclusions
The relatively large surface to volume ratio of EVs enables highly efficient surface interactions of these structures with cells and extracellular molecules. Such surface interactions have outstanding importance since they determine the fate of EVs by targeting them to the plasma membrane of cells or to certain tissues. One of the most exciting aspects of EV surface interactions is that they can be tailored by engineering the EV-releasing cells [124, 125]. This way, by having the designed EV-producing cells, one may achieve to produce EVs with specific targeting molecules on their surface and thus may be able to alter the biodistribution of EVs used as drug delivery systems. Feasibility of this approach was first demonstrated when siRNA was successfully delivered to murine brain upon systemic administration of exosomes carrying a brain-targeting peptide [126]. This initial proof-of-concept study has been followed by several subsequent works in which designer EVs were specifically targeted to tissues or cells [125]. The potential of designing targeted EVs for drug delivery, and the known ability of exosomes to cross blood tissue barriers such as blood brain barrier, underlies the significance in emerging EV-based therapies including gene therapy.
Another aspect of EV surface interactions is that due to technical limitations, it is not feasible to perform comprehensive analysis of EVs in situ in living tissues. Considering the interactions of EVs both with cells and with molecules of the microenvironment, there is an urgent need for much more complex systems to model EV surface interactions.
Recognizing the complexity of EV surface interactions, we should change our way of thinking about EVs as “pure” membrane vesicles. We should rather consider EV surface interactome in our experimental design since EV surface-associated molecules can hinder those already present on the EV surface, resulting in unexpected outcomes of both analysis and isolation of EVs.
Grant support
This work was supported by the National Research, Development and Innovation Office NKFIH, Hungary, OTKA11958, OTKA120237, NVKP_16-1-2016-0017, Ministry for National Economy of Hungary VEKOP-2.3.2-16-2016-00002, and VEKOP-2.3.315201600016.
References
Gyorgy B, Szabo TG, Pasztoi M, Pal Z, Misjak P, Aradi B, Laszlo V, Pallinger E, Pap E, Kittel A, Nagy G, Falus A, Buzas EI (2011) Membrane vesicles, current state-of-the-art: emerging role of extracellular vesicles. Cell Mol Life Sci 68:2667–2688
Yanez-Mo M, Siljander PR, Andreu Z, Zavec AB, Borras FE, Buzas EI, Buzas K, Casal E, Cappello F, Carvalho J, Colas E, Cordeiro-da Silva A, Fais S, Falcon-Perez JM, Ghobrial IM, Giebel B, Gimona M, Graner M, Gursel I, Gursel M, Heegaard NH, Hendrix A, Kierulf P, Kokubun K, Kosanovic M, Kralj-Iglic V, Kramer-Albers EM, Laitinen S, Lasser C, Lener T, Ligeti E, Line A, Lipps G, Llorente A, Lotvall J, Mancek-Keber M, Marcilla A, Mittelbrunn M, Nazarenko I, Nolte-'t Hoen EN, Nyman TA, O'Driscoll L, Olivan M, Oliveira C, Pallinger E, Del Portillo HA, Reventos J, Rigau M, Rohde E, Sammar M, Sanchez-Madrid F, Santarem N, Schallmoser K, Ostenfeld MS, Stoorvogel W, Stukelj R, Van der Grein SG, Vasconcelos MH, Wauben MH, De Wever O (2015) Biological properties of extracellular vesicles and their physiological functions. J Extracell Vesicles 4:27066
Kowal J, Arras G, Colombo M, Jouve M, Morath JP, Primdal-Bengtson B, Dingli F, Loew D, Tkach M, Thery C (2016) Proteomic comparison defines novel markers to characterize heterogeneous populations of extracellular vesicle subtypes. Proc Natl Acad Sci U S A 113:E968–E977
Di Vizio D, Morello M, Dudley AC, Schow PW, Adam RM, Morley S, Mulholland D, Rotinen M, Hager MH, Insabato L, Moses MA, Demichelis F, Lisanti MP, Wu H, Klagsbrun M, Bhowmick NA, Rubin MA, D'Souza-Schorey C, Freeman MR (2012) Large oncosomes in human prostate cancer tissues and in the circulation of mice with metastatic disease. Am J Pathol 181:1573–1584
Lotvall J, Hill AF, Hochberg F, Buzas EI, Di Vizio D, Gardiner C, Gho YS, Kurochkin IV, Mathivanan S, Quesenberry P, Sahoo S, Tahara H, Wauben MH, Witwer KW, Thery C (2014) Minimal experimental requirements for definition of extracellular vesicles and their functions: a position statement from the International Society for Extracellular Vesicles. J Extracell Vesicles 3:26913
Théry C, Regnault A, Garin J, Wolfers J, Zitvogel L, Ricciardi-Castagnoli P, Raposo G, Amigorena S (1999) Molecular characterization of dendritic cell-derived exosomes: selective accumulation of the heat shock protein hsc73. J Cell Biol 147:599–610
Jørgensen MM, Bæk R, Varming K (2015) Potentials and capabilities of the extracellular vesicle (EV) array. J Ext Vesicles 4:26048
Cvjetkovic A, Jang SC, Konečná B, Höög JL, Sihlbom C, Lässer C, Lötvall J (2016) Detailed analysis of protein topology of extracellular vesicles—evidence of unconventional membrane protein orientation. Sci Rep 6:36338
Tauro BJ, Greening DW, Mathias RA, Mathivanan S, Ji H, Simpson RJ (2013) Two distinct populations of exosomes are released from LIM1863 colon carcinoma cell-derived organoids. Mol Cell Proteomics 12:587–598
Radons J, Multhoff G (2005) Immunostimulatory functions of membrane-bound and exported heat shock protein 70. Exerc Immunol Rev 11:17–33
Ghosh A, Davey M, Chute IC, Griffiths SG, Lewis S, Chacko S, Barnett D, Crapoulet N, Fournier S, Joy A (2014) Rapid isolation of extracellular vesicles from cell culture and biological fluids using a synthetic peptide with specific affinity for heat shock proteins. PLoS One 9:e110443
Griffiths SG, Lewis SE (2015) Polypeptides with affinity for heat shock proteins (HSPs) and HSP associated complexes (HACS) and their use in diagnosis and therapy
Griffiths SG, Cormier MT, Clayton A, Doucette AA (2017) Differential proteome analysis of extracellular vesicles from breast cancer cell lines by chaperone affinity enrichment. Proteomes 5:25
Balaj L, Atai NA, Chen W, Mu D, Tannous BA, Breakefield XO, Skog J, Maguire CA (2015) Heparin affinity purification of extracellular vesicles. Sci Rep 5:10266
Tietjen GT, Gong Z, Chen CH, Vargas E, Crooks JE, Cao KD, Heffern CT, Henderson JM, Meron M, Lin B, Roux B, Schlossman ML, Steck TL, Lee KY, Adams EJ (2014) Molecular mechanism for differential recognition of membrane phosphatidylserine by the immune regulatory receptor Tim4. Proc Natl Acad Sci USA 111(15):E1463–E1E72
Nakai W, Yoshida T, Diez D, Miyatake Y, Nishibu T, Imawaka N, Naruse K, Sadamura Y, Hanayama R (2016) A novel affinity-based method for the isolation of highly purified extracellular vesicles. Sci Rep 6:33935
Belov L, Matic KJ, Hallal S, Best OG, Mulligan SP, Christopherson RI (2016) Extensive surface protein profiles of extracellular vesicles from cancer cells may provide diagnostic signatures from blood samples. J Ext Vesicles 5:25355
Grasso L, Wyss R, Weidenauer L, Thampi A, Demurtas D, Prudent M, Lion N, Vogel H (2015) Molecular screening of cancer-derived exosomes by surface plasmon resonance spectroscopy. Anal Bioanal Chem 407:5425–5432
Castillo J, Bernard V, San Lucas F, Allenson K, Capello M, Kim D, Gascoyne P, Mulu F, Stephens B, Huang J (2017) Surfaceome profiling enables isolation of cancer-specific exosomal cargo in liquid biopsies from pancreatic cancer patients. Ann Oncol 29:223–229
Koh E, Lee EJ, Nam G-H, Hong Y, Cho E, Yang Y, Kim I-S (2017) Exosome-SIRPα, a CD47 blockade increases cancer cell phagocytosis. Biomaterials 121:121–129
Mulcahy LA, Pink RC, Carter DRF (2014) Routes and mechanisms of extracellular vesicle uptake. J Ext Vesicles 3:24641
French KC, Antonyak MA, Cerione RA (2017) Extracellular vesicle docking at the cellular port: extracellular vesicle binding and uptake. Presented at Seminars in cell & developmental biology
Raposo G, Nijman HW, Stoorvogel W, Liejendekker R, Harding CV, Melief CJ, Geuze HJ (1996) B lymphocytes secrete antigen-presenting vesicles. J Exp Med 183:1161–1172
Martínez-Lorenzo MJ, Anel A, Gamen S, Monleón I, Lasierra P, Larrad L, Piñeiro A, Alava MA, Naval J (1999) Activated human T cells release bioactive Fas ligand and APO2 ligand in microvesicles. J Immunol 163:1274–1281
Monleón I, Martínez-Lorenzo MJ, Monteagudo L, Lasierra P, Taulés M, Iturralde M, Piñeiro A, Larrad L, Alava MA, Naval J, Anel A (2001) Differential secretion of Fas ligand- or APO2 ligand/TNF-related apoptosis-inducing ligand-carrying microvesicles during activation-induced death of human T cells. J Immunol 167(12):6736–6744
Rivoltini L, Chiodoni C, Squarcina P, Tortoreto M, Villa A, Vergani B, Bürdek M, Botti L, Arioli I, Cova A (2016) TNF-related apoptosis-inducing ligand (TRAIL)—armed exosomes deliver proapoptotic signals to tumor site. Clin Cancer Res 22:3499–3512
Theodoraki M-N, Yerneni S, Hoffmann TK, Gooding WE, Whiteside TL (2017) Clinical significance of PD-L1+ exosomes in plasma of head and neck cancer patients. Clin Cancer Res pp. clincanres 2664.017
He M, Kubo H, Morimoto K, Fujino N, Suzuki T, Takahasi T, Yamada M, Yamaya M, Maekawa T, Yamamoto Y (2011) Receptor for advanced glycation end products binds to phosphatidylserine and assists in the clearance of apoptotic cells. EMBO Rep 12:358–364
Park D, Tosello-Trampont A-C, Elliott MR, Lu M, Haney LB, Ma Z, Klibanov AL, Mandell JW, Ravichandran KS (2007) BAI1 is an engulfment receptor for apoptotic cells upstream of the ELMO/Dock180/Rac module. Nature 450:430–434
Park SY, Jung MY, Kim HJ, Lee SJ, Kim SY, Lee BH, Kwon TH, Park RW, Kim IS (2008) Rapid cell corpse clearance by stabilin-2, a membrane phosphatidylserine receptor. Cell Death Differ 15(1):192–201
Hanayama R, Tanaka M, Miwa K, Shinohara A, Iwamatsu A, Nagata S (2002) Identification of a factor that links apoptotic cells to phagocytes. Nature 417:182–187
Véron P, Segura E, Sugano G, Amigorena S, Théry C (2005) Accumulation of MFG-E8/lactadherin on exosomes from immature dendritic cells. Blood Cell Mol Dis 35:81–88
Oshima K, Aoki N, Kato T, Kitajima K, Matsuda T (2002) Secretion of a peripheral membrane protein, MFG-E8, as a complex with membrane vesicles. FEBS J 269:1209–1218
Graham DK, DeRyckere D, Davies KD, Earp HS (2014) The TAM family: phosphatidylserine-sensing receptor tyrosine kinases gone awry in cancer. Nat Rev Cancer 14:769–785
Zakharova L, Svetlova M, Fomina AF (2007) T cell exosomes induce cholesterol accumulation in human monocytes via phosphatidylserine receptor. J Cell Physiol 212:174–181
Wei X, Liu C, Wang H, Wang L, Xiao F, Guo Z, Zhang H (2016) Surface phosphatidylserine is responsible for the internalization on microvesicles derived from hypoxia-induced human bone marrow mesenchymal stem cells into human endothelial cells. PLoS One 11:e0147360
Sung BH, Ketova T, Hoshino D, Zijlstra A, Weaver AM (2015) Directional cell movement through tissues is controlled by exosome secretion. Nat Commun 6:7164
Rieu S, Géminard C, Rabesandratana H, Sainte-Marie J, Vidal M (2000) Exosomes released during reticulocyte maturation bind to fibronectin via integrin α4β1. FEBS J 267:583–590
Purushothaman A, Bandari SK, Liu J, Mobley JA, Brown EE, Sanderson RD (2016) Fibronectin on the surface of myeloma cell-derived exosomes mediates exosome-cell interactions. J Biol Chem 291:1652–1663
Atay S, Gercel-Taylor C, Taylor DD (2011) Human trophoblast-derived Exosomal fibronectin induces pro-inflammatory Il-1β production by macrophages. Am J Reprod Immunol 66:259–269
Németh A, Orgovan N, Sódar BW, Osteikoetxea X, Pálóczi K, Szabó-Taylor KÉ, Vukman KV, Kittel Á, Turiák L, Wiener Z (2017) Antibiotic-induced release of small extracellular vesicles (exosomes) with surface-associated DNA. Sci Rep 7:8202
Moon P-G, Lee J-E, Cho Y-E, Lee SJ, Chae YS, Jung JH, Kim I-S, Park HY, Baek M-C (2016) Fibronectin on circulating extracellular vesicles as a liquid biopsy to detect breast cancer. Oncotarget 7:40189
Christianson HC, Svensson KJ, van Kuppevelt TH, Li J-P, Belting M (2013) Cancer cell exosomes depend on cell-surface heparan sulfate proteoglycans for their internalization and functional activity. Proc Natl Acad Sci 110:17380–17385
Lai X, Wang M, McElyea SD, Sherman S, House M, Korc M (2017) A microRNA signature in circulating exosomes is superior to exosomal glypican-1 levels for diagnosing pancreatic cancer. Cancer Lett 393:86–93
Melo SA, Luecke LB, Kahlert C, Fernandez AF, Gammon ST, Kaye J, LeBleu VS, Mittendorf EA, Weitz J, Rahbari N (2015) Glypican-1 identifies cancer exosomes and detects early pancreatic cancer. Nature 523:177–182
Liang K, Liu F, Fan J, Sun D, Liu C, Lyon CJ, Bernard DW, Li Y, Yokoi K, Katz MH (2017) Nanoplasmonic quantification of tumour-derived extracellular vesicles in plasma microsamples for diagnosis and treatment monitoring. Nat Biomed Eng 1:0021
Arasu UT, Kärnä R, Härkönen K, Oikari S, Koistinen A, Kröger H, Qu C, Lammi MJ, Rilla K (2017) Human mesenchymal stem cells secrete hyaluronan-coated extracellular vesicles. Matrix Biol 64:54–68
Nakamura K, Sawada K, Kinose Y, Yoshimura A, Toda A, Nakatsuka E, Hashimoto K, Mabuchi S, Morishige K-I, Kurachi H (2016) Exosomes promote ovarian cancer cell invasion through transfer of CD44 to peritoneal mesothelial cells. Mol Cancer Res pp. molcanres 0191.2016
Wang M, Ji S, Shao G, Zhang J, Zhao K, Wang Z, Wu A (2017) Effect of exosome biomarkers for diagnosis and prognosis of breast cancer patients. Clin Transl Oncol 1–6
Paolillo M, Schinelli S (2017) Integrins and exosomes, a dangerous liaison in cancer progression. Cancers 9:95
Hoshino A, Costa-Silva B, Shen TL, Rodrigues G, Hashimoto A, Tesic Mark M, Molina H, Kohsaka S, Di Giannatale A, Ceder S, Singh S, Williams C, Soplop N, Uryu K, Pharmer L, King T, Bojmar L, Davies AE, Ararso Y, Zhang T, Zhang H, Hernandez J, Weiss JM, Dumont-Cole VD, Kramer K, Wexler LH, Narendran A, Schwartz GK, Healey JH, Sandstrom P, Labori KJ, Kure EH, Grandgenett PM, Hollingsworth MA, de Sousa M, Kaur S, Jain M, Mallya K, Batra SK, Jarnagin WR, Brady MS, Fodstad O, Muller V, Pantel K, Minn AJ, Bissell MJ, Garcia BA, Kang Y, Rajasekhar VK, Ghajar CM, Matei I, Peinado H, Bromberg J, Lyden D (2015) Tumour exosome integrins determine organotropic metastasis. Nature 527(7578):329–335
Buzas EI, György B, Nagy G, Falus A, Gay S (2014) Emerging role of extracellular vesicles in inflammatory diseases. Nat Rev Rheumatol 10(6):356–364
Cloutier N, Tan S, Boudreau LH, Cramb C, Subbaiah R, Lahey L, Albert A, Shnayder R, Gobezie R, Nigrovic PA (2013) The exposure of autoantigens by microparticles underlies the formation of potent inflammatory components: the microparticle-associated immune complexes. EMBO Mol Med 5:235–249
Perez-Hernandez J, Redon J, Cortes R (2017) Extracellular vesicles as therapeutic agents in systemic lupus erythematosus. Int J Mol Sci 18:717
Fortin PR, Cloutier N, Bissonnette V, Aghdassi E, Eder L, Simonyan D, Laflamme N, Boilard E (2016) Distinct subtypes of microparticle-containing immune complexes are associated with disease activity, damage, and carotid intima-media thickness in systemic lupus erythematosus. J Rheumatol pp. jrheum. 160050
Sisirak V, Sally B, D’Agati V, Martinez-Ortiz W, Özçakar ZB, David J, Rashidfarrokhi A, Yeste A, Panea C, Chida AS (2016) Digestion of chromatin in apoptotic cell microparticles prevents autoimmunity. Cell 166:88–101
Yin W, Ghebrehiwet B, Peerschke EI (2008) Expression of complement components and inhibitors on platelet microparticles. Platelets 19:225–233
Winberg LK, Nielsen CH, Jacobsen S (2017) Surface complement C3 fragments and cellular binding of microparticles in patients with SLE. Lupus Sci Med 4(1):e000193
Karpman D, Ståhl A-L, Arvidsson I (2017) Extracellular vesicles in renal disease. Nat Rev Nephrol 13:545–562
Carrillo-Conde BR, Ramer-Tait AE, Wannemuehler MJ, Narasimhan B (2012) Chemistry-dependent adsorption of serum proteins onto polyanhydride microparticles differentially influences dendritic cell uptake and activation. Acta Biomater 8:3618–3628
Wolf P (1967) The nature and significance of platelet products in human plasma. Br J Haematol 13:269–288
Zwicker JI, Liebman HA, Neuberg D, Lacroix R, Bauer KA, Furie BC, Furie B (2009) Tumor-derived tissue factor–bearing microparticles are associated with venous thromboembolic events in malignancy. Clin Cancer Res 15:6830–6840
Owens AP, Mackman N (2011) Microparticles in hemostasis and thrombosis. Circ Res 108:1284–1297
Toti F, Satta N, Fressinaud E, Meyer D, Freyssinet J-M (1996) Scott syndrome, characterized by impaired transmembrane migration of procoagulant phosphatidylserine and hemorrhagic complications, is an inherited disorder. Blood 87:1409–1415
Hisada Y, Auriemma AC, Alexander W, Ay C, Mackman N (2017) Detection of tissue factor-positive extracellular vesicles by laser scanning confocal microscopy. Thromb Res 150:65–72
Cointe S, Lacroix R, Dignat-George F (2017) Platelet-derived microparticles. In: Platelets in thrombotic and non-thrombotic disorders. Springer, p 379–92
Lacroix R, Dubois C, Leroyer A, Sabatier F, Dignat-George F (2013) Revisited role of microparticles in arterial and venous thrombosis. J Thromb Haemost 11:24–35
Van Der Meijden P, Van Schilfgaarde M, Van Oerle R, Renne T, Ten Cate H, Spronk H (2012) Platelet-and erythrocyte-derived microparticles trigger thrombin generation via factor XIIa. J Thromb Haemost 10:1355–1362
Gilbert GE, Sims PJ, Wiedmer T, Furie B, Furie BC, Shattil SJ (1991) Platelet-derived microparticles express high affinity receptors for factor VIII. J Biol Chem 266(26):17261–17268
Sims PJ, Wiedmer T, Esmon CT, Weiss HJ, Shattil S (1989) Assembly of the platelet prothrombinase complex is linked to vesiculation of the platelet plasma membrane. Studies in Scott syndrome: an isolated defect in platelet procoagulant activity. J Biol Chem 264:17049–17057
Hoffman M, Monroe DM, Roberts HR (1992) Coagulation factor IXa binding to activated platelets and platelet-derived microparticles: a flow cytometric study. Thromb Haemost 68:74–78
Thom SR, Bennett M, Banham ND, Chin W, Blake DF, Rosen A, Pollock NW, Madden D, Barak O, Marroni A (2015) Association of microparticles and neutrophil activation with decompression sickness. J Appl Physiol 119:427–434
Jy W, Jimenez J, Mauro L, Horstman L, Cheng P, Ahn E, Bidot C, Ahn Y (2005) Endothelial microparticles induce formation of platelet aggregates via a von Willebrand factor/ristocetin dependent pathway, rendering them resistant to dissociation. J Thromb Haemost 3:1301–1308
Sinauridze EI, Kireev DA, Popenko NY, Pichugin AV, Panteleev MA, Krymskaya OV, Ataullakhanov FI (2007) Platelet microparticle membranes have 50-to 100-fold higher specific procoagulant activity than activated platelets. Thromb Haemost 98:425–434
Théry C, Zitvogel L, Amigorena S (2002) Exosomes: composition, biogenesis and function. Nat Rev Immunol 2:569–579
Heijnen HF, Schiel AE, Fijnheer R, Geuze HJ, Sixma JJ (1999) Activated platelets release two types of membrane vesicles: microvesicles by surface shedding and exosomes derived from exocytosis of multivesicular bodies and-granules. Blood 94:3791–3799
van der Pol E, Böing AN, Harrison P, Sturk A, Nieuwland R (2012) Classification, functions, and clinical relevance of extracellular vesicles. Pharmacol Rev 64:676–705
Yuana Y, Levels J, Grootemaat A, Sturk A, Nieuwland R (2014) Co-isolation of extracellular vesicles and high-density lipoproteins using density gradient ultracentrifugation. J Ext Vesicles 3:23262
Deregibus MC, Figliolini F, D'antico S, Manzini PM, Pasquino C, De Lena M, Tetta C, Brizzi MF, Camussi G (2016) Charge-based precipitation of extracellular vesicles. Int J Mol Med 38:1359–1366
Sódar BW, Kittel Á, Pálóczi K, Vukman KV, Osteikoetxea X, Szabó-Taylor K, Németh A, Sperlágh B, Baranyai T, Giricz Z (2016) Low-density lipoprotein mimics blood plasma-derived exosomes and microvesicles during isolation and detection. Sci Rep 6:24316
Grigor’eva A, Dyrkheeva N, Bryzgunova O, Tamkovich S, Chelobanov B, Ryabchikova E (2017) Contamination of exosome preparations, isolated from biological fluids. Biochem (Moscow), Suppl Ser B: Biomed Chem 11:265–271
Mørk M, Handberg A, Pedersen S, Jørgensen MM, Bæk R, Nielsen MK, Kristensen SR (2017) Prospects and limitations of antibody-mediated clearing of lipoproteins from blood plasma prior to nanoparticle tracking analysis of extracellular vesicles. J Ext Vesicles 6:1308779
Connolly KD, Willis GR, Datta DB, Ellins EA, Ladell K, Price DA, Guschina IA, Rees DA, James PE (2014) Lipoprotein-apheresis reduces circulating microparticles in individuals with familial hypercholesterolemia. J Lipid Res 55:2064–2072
Dashty M, Motazacker MM, Levels J, de Vries M, Mahmoudi M, Peppelenbosch MP, Rezaee F (2014) Proteome of human plasma very low-density lipoprotein and low-density lipoprotein exhibits a link with coagulation and lipid metabolism. Thromb Haemost 112:518–530
Illingworth DR, Portman OW (1972) Independence of phospholipid and protein exchange between plasma lipoproteins in vivo and in vitro. Biochim Biophys Acta (BBA)-Lipids Lipid Metab 280:281–289
Barr SI, Kottke B, Mao S (1981) Postprandial exchange of apolipoprotein C-III between plasma lipoproteins. Am J Clin Nutr 34:191–198
Liu X, Bagdade J (1995) Neutral lipid mass transfer among lipoproteins in plasma from normolipidemic subjects is not an equimolar heteroexchange. J Lipid Res 36:2574–2579
Ooi EM, Barrett PHR, Chan DC, Watts GF (2008) Apolipoprotein C-III: understanding an emerging cardiovascular risk factor. Clin Sci (Lond) 114:611–624
Yang Z, Wang X, Chi X, Zhao F, Guo J, Ma P, Zhong J, Niu J, Pan X, Long G (2016) Neglected but important role of apolipoprotein E exchange in hepatitis C virus infection. J Virol 90:9632–9643
Angeloni NL, McMahon KM, Swaminathan S, Plebanek MP, Osman I, Volpert OV, Thaxton CS (2016) Pathways for modulating exosome lipids identified by high-density lipoprotein-like nanoparticle binding to scavenger receptor type B-1. Sci Rep 6:22915
Van Niel G, Bergam P, Di Cicco A, Hurbain I, Cicero AL, Dingli F, Palmulli R, Fort C, Potier MC, Schurgers LJ (2015) Apolipoprotein E regulates amyloid formation within endosomes of pigment cells. Cell Rep 13:43–51
van Niel G (2016) Study of exosomes shed new light on physiology of amyloidogenesis. Cell Mol Neurobiol 36:327–342
Baranyai T, Herczeg K, Onódi Z, Voszka I, Módos K, Marton N, Nagy G, Mäger I, Wood MJ, El Andaloussi S (2015) Isolation of exosomes from blood plasma: qualitative and quantitative comparison of ultracentrifugation and size exclusion chromatography methods. PLoS One 10:e0145686
Keerthikumar S, Chisanga D, Ariyaratne D, Al Saffar H, Anand S, Zhao K, Samuel M, Pathan M, Jois M, Chilamkurti N (2016) ExoCarta: a web-based compendium of exosomal cargo. J Mol Biol 428:688–692
Mathivanan S, Simpson RJ (2009) ExoCarta: a compendium of exosomal proteins and RNA. Proteomics 9:4997–5000
Kim D-K, Kang B, Kim OY, Choi D-S, Lee J, Kim SR, Go G, Yoon YJ, Kim JH, Jang SC (2013) EVpedia: an integrated database of high-throughput data for systemic analyses of extracellular vesicles. J Ext Vesicles 2:20384
Hawari FI, Rouhani FN, Cui X, Yu Z-X, Buckley C, Kaler M, Levine SJ (2004) Release of full-length 55-kDa TNF receptor 1 in exosome-like vesicles: a mechanism for generation of soluble cytokine receptors. Proc Natl Acad Sci U S A 101:1297–1302
Webber J, Steadman R, Mason MD, Tabi Z, Clayton A (2010) Cancer exosomes trigger fibroblast to myofibroblast differentiation. Cancer Res 70:9621–9630
Rumbo C, Fernández-Moreira E, Merino M, Poza M, Mendez JA, Soares NC, Mosquera A, Chaves F, Bou G (2011) Horizontal transfer of the OXA-24 carbapenemase gene via outer membrane vesicles: a new mechanism of dissemination of carbapenem resistance genes in Acinetobacter baumannii. Antimicrob Agents Chemother 55:3084–3090
Fulsundar S, Harms K, Flaten GE, Johnsen PJ, Chopade BA, Nielsen KM (2014) Gene transfer potential of outer membrane vesicles of Acinetobacter baylyi and effects of stress on vesiculation. Appl Environ Microbiol 80:3469–3483
Yaron S, Kolling GL, Simon L, Matthews KR (2000) Vesicle-mediated transfer of virulence genes from Escherichia coli O157: H7 to other enteric bacteria. Appl Environ Microbiol 66:4414–4420
Liao S, Klein MI, Heim KP, Fan Y, Bitoun JP, Ahn S-J, Burne RA, Koo H, Brady LJ, Wen ZT (2014) Streptococcus mutans extracellular DNA is upregulated during growth in biofilms, actively released via membrane vesicles, and influenced by components of the protein secretion machinery. J Bacteriol 196:2355–2366
Gloag ES, Turnbull L, Huang A, Vallotton P, Wang H, Nolan LM, Mililli L, Hunt C, Lu J, Osvath SR (2013) Self-organization of bacterial biofilms is facilitated by extracellular DNA. Proc Natl Acad Sci 110:11541–11546
Bitto NJ, Chapman R, Pidot S, Costin A, Lo C, Choi J, D’cruze T, Reynolds EC, Dashper SG, Turnbull L (2017) Bacterial membrane vesicles transport their DNA cargo into host cells. Sci Rep 7:7072
Fischer S, Cornils K, Speiseder T, Badbaran A, Reimer R, Indenbirken D, Grundhoff A, Brunswig-Spickenheier B, Alawi M, Lange C (2016) Indication of horizontal DNA gene transfer by extracellular vesicles. PLoS One 11:e0163665
Shelke GV, Jang SC, Yin Y, Lässer C, Lötvall J (2016) Human mast cells release extracellular vesicle-associated DNA. Matters 2:e201602000034
Sanderson RD, Bandari SK, Vlodavsky I (2017) Proteases and glycosidases on the surface of exosomes: newly discovered mechanisms for extracellular remodeling. Matrix Biol
Hakulinen J, Sankkila L, Sugiyama N, Lehti K, Keski-Oja J (2008) Secretion of active membrane type 1 matrix metalloproteinase (MMP-14) into extracellular space in microvesicular exosomes. J Cell Biochem 105:1211–1218
Groth E, Pruessmeyer J, Babendreyer A, Schumacher J, Pasqualon T, Dreymueller D, Higashiyama S, Lorenzen I, Grötzinger J, Cataldo D (2016) Stimulated release and functional activity of surface expressed metalloproteinase ADAM17 in exosomes. Biochim Biophys Acta (BBA)-Mol Cell Res 1863:2795–2808
Sumida M, Hane M, Yabe U, Shimoda Y, Pearce OM, Kiso M, Miyagi T, Sawada M, Varki A, Kitajima K, Sato C (2015) Rapid trimming of cell surface polysialic acid (PolySia) by exovesicular sialidase triggers release of preexisting surface neurotrophin. J Biol Chem 290(21):13202–13214
Paolini L, Orizio F, Busatto S, Radeghieri A, Bresciani R, Bergese P, Monti E (2017) Exosomes secreted by HeLa cells shuttle on their surface the plasma membrane-associated sialidase NEU3. Biochemistry 56:6401–6408
Bandari SK, Purushothaman A, Ramani VC, Brinkley GJ, Chandrashekar DS, Varambally S, Mobley JA, Zhang Y, Brown EE, Vlodavsky I (2017) Chemotherapy induces secretion of exosomes loaded with heparanase that degrades extracellular matrix and impacts tumor and host cell behavior. Mat Biol
Mu W, Rana S, Zöller M (2013) Host matrix modulation by tumor exosomes promotes motility and invasiveness. Neoplasia 15:875–IN4
Shimoda M, Khokha R (2017) Metalloproteinases in extracellular vesicles. Biochim Biophys Acta (BBA)-Mol Cell Res 1864:1989–2000
Szabó-Taylor KÉ, Tóth EÁ, Balogh AM, Sódar BW, Kádár L, Pálóczi K, Fekete N, Németh A, Osteikoetxea X, Vukman KV, Holub M, Pállinger É, Nagy G, Winyard PG, Buzás EI (2017) Monocyte activation drives preservation of membrane thiols by promoting release of oxidised membrane moieties via extracellular vesicles. Free Radic Biol Med 108:56–65
Turell L, Radi R, Alvarez B (2013) The thiol pool in human plasma: the central contribution of albumin to redox processes. Free Radic Biol Med 65:244–253
Laragione T, Bonetto V, Casoni F, Massignan T, Bianchi G, Gianazza E, Ghezzi P (2003) Redox regulation of surface protein thiols: identification of integrin α-4 as a molecular target by using redox proteomics. Proc Natl Acad Sci 100:14737–14741
Szabó KÉ, Line K, Eggleton P, Littlechild JA, Winyard PG (2009) Structure and function of the human peroxiredoxin-based antioxidant system: the interplay between peroxiredoxins, thioredoxins, thioredoxin reductases, sulfiredoxins and sestrins. Redox Sign Regul Biol Med 143–79
Szabó-Taylor KÉ, Eggleton P, Turner CA, Faro MLL, Tarr JM, Tóth S, Whiteman M, Haigh RC, Littlechild JA, Winyard PG (2012) Lymphocytes from rheumatoid arthritis patients have elevated levels of intracellular peroxiredoxin 2, and a greater frequency of cells with exofacial peroxiredoxin 2, compared with healthy human lymphocytes. Int J Biochem Cell Biol 44:1223–1231
Théry C, Boussac M, Véron P, Ricciardi-Castagnoli P, Raposo G, Garin J, Amigorena S (2001) Proteomic analysis of dendritic cell-derived exosomes: a secreted subcellular compartment distinct from apoptotic vesicles. J Immunol 166:7309–7318
Żmigrodzka M, Guzera M, Miśkiewicz A, Jagielski D, Winnicka A (2016) The biology of extracellular vesicles with focus on platelet microparticles and their role in cancer development and progression. Tumour Biol 37(11):14391–14401
Jiang X-M, Fitzgerald M, Grant CM, Hogg PJ (1999) Redox control of exofacial protein thiols/disulfides by protein disulfide isomerase. J Biol Chem 274:2416–2423
Fan G-Q, Qin R-R, Li Y-H, Song D-J, Chen T-S, Zhang W, Zhong M, Zhang Y, Xing Y-Q, Wang Z-H (2016) Endothelial cells microparticle-associated protein disulfide isomerase promotes platelet activation in metabolic syndrome. Oncotarget 7:83231
György B, Hung ME, Breakefield XO, Leonard JN (2015) Therapeutic applications of extracellular vesicles: clinical promise and open questions. Annu Rev Pharmacol Toxicol 55:439–464
Kim S-M, Kim H-S (2017) Engineering of extracellular vesicles as drug delivery vehicles. Stem Cell Investig 4:74
Alvarez-Erviti L, Seow Y, Yin H, Betts C, Lakhal S, Wood MJ (2011) Delivery of siRNA to the mouse brain by systemic injection of targeted exosomes. Nat Biotechnol 29:341–345
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is a contribution to the special issue on Extracellular Vesicles - Guest Editor: Esther Nolte-’t Hoen
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Buzás, E.I., Tóth, E.Á., Sódar, B.W. et al. Molecular interactions at the surface of extracellular vesicles. Semin Immunopathol 40, 453–464 (2018). https://doi.org/10.1007/s00281-018-0682-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00281-018-0682-0