Abstract
Introduction
Blunt liver injury is common and is associated with a high morbidity and mortality. More severe injuries often require either angioembolization or open operative repair, depending on patient factors and facility capacity. We sought to describe patient outcomes based on intervention type.
Methods
We analyzed the National Trauma Data Bank (2017–2019) using ICD-10 codes to identify adult patients with blunt liver injury and their interventions. AIS (Abbreviated Injury Scale) scores were used to group patients based on liver injury severity (AIS 2–6). Logistic regression modeling was used to estimate the adjusted odds ratio of death based on intervention type, excluding patients with severe injury.
Results
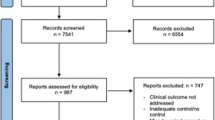
Of 2,848,592 trauma patients, 50,250 patients had a blunt liver injury. Among patients with AIS 3/4/5 injury, 1,140 had angioembolization, 1,529 had an open repair, and 188 had both angioembolization and open repair. In comparison with no intervention and adjusted for age, sex, shock index, ISS, and transfusion total (first four hours), angioembolization was associated with a significant decrease in the odds of mortality for patients with an AIS 4 (OR 0.68, 95% CI 0.47, 0.99) and AIS 5 injury (OR 0.39, 95% CI 0.24, 0.64). In patients with an AIS 5 injury, open repair had an increased odds of mortality at OR 1.99 (95% CI 1.47, 2.69).
Conclusion
In an analysis of a national trauma database, patients with a moderate to severe injury (AIS 4 or 5), angioembolization was associated with a significant reduction in the adjusted odds of mortality compared to open repair and should be considered when clinically appropriate.



Similar content being viewed by others
References
Tinkoff G, Esposito TJ, Reed J et al (2008) American association for the surgery of trauma organ injury scale I: spleen, liver, and kidney, validation based on the National Trauma Data Bank. J Am Coll Surg 207:646–655
Scollay JM, Beard D, Smith R et al (2005) Eleven years of liver trauma: the Scottish experience. World J Surg 29:744–749
David Richardson J, Franklin GA, Lukan JK et al (2000) Evolution in the management of hepatic trauma: a 25-year perspective. Ann Surg 232:324–330
Parks R, Chrysos E, Diamond T (1999) Management of liver trauma. Br J Surg 86:1121–1135
Matthes G, Stengel D, Seifert J et al (2003) Blunt liver injuries in polytrauma: results from a cohort study with the regular use of whole-body helical computed tomography. World J Surg 27:1124–1130
Matthes G, Stengel D, Bauwens K et al (2006) Predictive factors of liver injury in blunt multiple trauma. Langenbecks Arch Surg 391:350–354
Chien L-C, Lo S-S, Yeh S-Y (2013) Incidence of liver trauma and relative risk factors for mortality: a population-based study. J Chin Med Assoc 76:576–582
Chmatal P, Kupka P, Fuksa Z et al (2008) Liver trauma usually means management of multiple injuries: analysis of 78 patients. Int Surg 93:72–77
Malhotra AK, Fabian TC, Croce MA et al (2000) Blunt hepatic injury: a paradigm shift from operative to nonoperative management in the 1990s. Ann Surg 231:804–813
Croce MA, Fabian TC, Menke PG et al (1995) Nonoperative management of blunt hepatic trauma is the treatment of choice for hemodynamically stable patients. Results of a prospective trial. Ann Surg 221:744–753 (discussion 753–745)
Pachter HL, Knudson MM, Esrig B et al (1996) Status of nonoperative management of blunt hepatic injuries in 1995: a multicenter experience with 404 patients. J Trauma 40:31–38
Goan YG, Huang MS, Lin JM (1998) Nonoperative management for extensive hepatic and splenic injuries with significant hemoperitoneum in adults. J Trauma 45:360–364 (discussion 365)
Cadili A, Gates J (2021) The role of angioembolization in hepatic trauma. Am Surg 87:1793–1801
Green CS, Bulger EM, Kwan SW (2016) Outcomes and complications of angioembolization for hepatic trauma: a systematic review of the literature. J Trauma Acute Care Surg 80:529–537
Charlson M, Szatrowski TP, Peterson J et al (1994) Validation of a combined comorbidity index. J Clin Epidemiol 47:1245–1251
Samuel AM, Grant RA, Bohl DD et al (2015) Delayed surgery after acute traumatic central cord syndrome is associated with reduced mortality. Spine (Phila Pa 1976) 40:349–356
Carrillo EH, Platz A, Miller FB et al (1998) Non-operative management of blunt hepatic trauma. Br J Surg 85:461–468
Suen K, Skandarajah AR, Knowles B et al (2016) Changes in the management of liver trauma leading to reduced mortality: 15-year experience in a major trauma centre. ANZ J Surg 86:894–899
Saltzherr TP, van der Vlies CH, van Lienden KP et al (2011) Improved outcomes in the non-operative management of liver injuries. HPB 13:350–355
Gaarder C, Naess PA, Eken T et al (2007) Liver injuries–improved results with a formal protocol including angiography. Injury 38:1075–1083
Asensio JA, Roldán G, Petrone P et al (2003) Operative management and outcomes in 103 AAST-OIS grades IV and V complex hepatic injuries: trauma surgeons still need to operate, but angioembolization helps. J Trauma Acute Care Surg 54:647–654
Stassen NA, Bhullar I, Cheng JD et al (2012) Nonoperative management of blunt hepatic injury: an Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg 73:S288–S293
Ahmed N, Kassavin D, Kuo Y-H et al (2013) Sensitivity and specificity of CT scan and angiogram for ongoing internal bleeding following torso trauma. Emerg Med J 30:e14–e14
Cadili A, Gates J (2021) The role of angioembolization in hepatic trauma. Am Surg 87(11):1793–1801
Matsumoto S, Cantrell E, Jung K et al (2018) Influence of postoperative hepatic angiography on mortality after laparotomy in Grade IV/V hepatic injuries. J Trauma Acute Care Surg 85:290–297
Matsushima K, Hogen R, Piccinini A et al (2020) Adjunctive use of hepatic angioembolization following hemorrhage control laparotomy. J Trauma Acute Care Surg 88:636–643
Kutcher ME, Weis JJ, Siada SS et al (2015) The role of computed tomographic scan in ongoing triage of operative hepatic trauma: a western trauma association multicenter retrospective study. J Trauma Acute Care Surg 79:951–956
van der Wilden GM, Velmahos GC, Emhoff T et al (2012) Successful nonoperative management of the most severe blunt liver injuries: a multicenter study of the research consortium of New England centers for trauma. Arch Surg 147:423–428
Duane TM, Como JJ, Bochicchio GV et al (2004) Reevaluating the management and outcomes of severe blunt liver injury. J Trauma Acute Care Surg 57:494–500
Misselbeck TS, Teicher EJ, Cipolle MD et al (2009) Hepatic angioembolization in trauma patients: indications and complications. J Trauma 67:769–773
Mohr AM, Lavery RF, Barone A et al (2003) Angiographic embolization for liver injuries: low mortality, high morbidity. J Trauma 55:1077–1081 (discussion 1081-1072)
Dabbs DN, Stein DM, Scalea TM (2009) Major hepatic necrosis: a common complication after angioembolization for treatment of high-grade liver injuries. J Trauma 66:621–627 (discussion 627-629)
Samuels JM, Urban S, Peltz E et al (2020) A modern, multicenter evaluation of hepatic angioembolization–complications and readmissions persist. Am J Surg 219:117–122
Samuels JM, Carmichael H, Kovar A et al (2020) Reevaluation of hepatic angioembolization for trauma in stable patients: weighing the risk. J Am Coll Surg 231(123–131):e123
Tignanelli CJ, Joseph B, Jakubus JL et al (2018) Variability in management of blunt liver trauma and contribution of level of American College of Surgeons Committee on Trauma verification status on mortality. J Trauma Acute Care Surg 84:273–279
Funding
Financial support was provided by the Department of Surgery at the University of North Carolina.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to disclose. The authors have no financial relationships to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gallaher, J., Burton, V., Schneider, A.B. et al. The Effect of Angioembolization Versus Open Exploration for Moderate to Severe Blunt Liver Injuries on Mortality. World J Surg 47, 1271–1281 (2023). https://doi.org/10.1007/s00268-023-06926-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-023-06926-5