Abstract
Background
Whether surgical resection for recurrent biliary tract carcinoma (BTC) prolongs survival and the patients who are most likely to benefit from such treatment remain unclear.
Methods
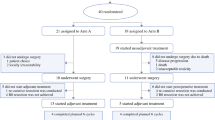
Among 251 patients with recurrences after the initial resection of BTC, a total of 21 patients (8.4%) underwent surgical resection for the recurrence, with a zero mortality rate. The clinicopathological features of these patients were compared with those of patients who did not undergo surgery.
Results
The median survival time (MST) after the first recurrence and the 5-year post-recurrent survival (PRS) rate were 19.8 months and 32.8%, respectively, for patients who underwent re-resection. Fourteen patients (66.7%) experienced second recurrences; however, none of these patients underwent further surgical resection. Surgical resection for recurrence was identified as an independent prognostic factor for survival after recurrence (hazard ratio of 0.33, 95% CI of 0.17–0.58, p < 0.001). Patients with less than three liver metastases had a significantly better PRS after surgical resection than after chemotherapy (p = 0.015). Among the patients with an isolated solitary liver metastasis, patients who underwent resection had a significantly longer MST after the first recurrence than patients receiving chemotherapy (22.8 vs. 10.9 months, p = 0.025), whereas the PRS was similar between the two groups among patients with two liver lesions.
Conclusions
Surgical resection for recurrent BTC may prolong survival in highly selected patients. A hepatectomy might offer a survival benefit for patients with a solitary liver metastasis.



Similar content being viewed by others
Abbreviations
- BTC:
-
Biliary tract carcinoma
- ICC:
-
Intrahepatic cholangiocarcinoma
- PCC:
-
Perihilar cholangiocarcinoma
- DCC:
-
Distal cholangiocarcinoma
- GBC:
-
Gallbladder carcinoma
- CAV:
-
Carcinomas of the ampulla of Vater
- PD:
-
Pancreaticoduodenectomy
- DFI:
-
Disease-free interval
- TNM:
-
Tumor, node, metastasis
- AJCC:
-
American Joint Committee on Cancer
- OS:
-
Overall survival
- MST:
-
Median survival time
References
Razumilava N, Gores GJ (2014) Cholangiocarcinoma. Lancet 383:2168–2179
Takao S, Shinchi H, Uchikura K et al (1999) Liver metastases after curative resection in patients with distal bile duct cancer. Br J Surg 86:327–331
Todoroki T, Kawamoto T, Koike N et al (2001) Treatment strategy for patients with middle and lower third bile duct cancer. Br J Surg 88:364–370
Kobayashi A, Miwa S, Nakata T et al (2010) Disease recurrence patterns after R0 resection of hilar cholangiocarcinoma. Br J Surg 97:56–64
Gruenberger B, Schueller J, Heubrandtner U et al (2010) Cetuximab, gemcitabine, and oxaliplatin in patients with unresectable advanced or metastatic biliary tract cancer: a phase 2 study. Lancet Oncol 11:1142–1148
Valle J, Wasan H, Palmer DH et al (2010) Cisplatin plus gemcitabine versus gemcitabine for biliary tract cancer. N Engl J Med 362:1273–1281
Lee J, Park SH, Chang HM et al (2012) Gemcitabine and oxaliplatin with or without erlotinib in advanced biliary-tract cancer: a multicentre, open-label, randomised, phase 3 study. Lancet Oncol 13:181–188
Malka D, Cervera P, Foulon S et al (2014) Gemcitabine and oxaliplatin with or without cetuximab in advanced biliary-tract cancer (BINGO): a randomised, open-label, non-comparative phase 2 trial. Lancet Oncol 15:819–828
Eckel F, Schmid RM (2014) Chemotherapy and targeted therapy in advanced biliary tract carcinoma: a pooled analysis of clinical trials. Chemotherapy 60:13–23
Valle JW, Wasan H, Lopes A et al (2015) Cediranib or placebo in combination with cisplatin and gemcitabine chemotherapy for patients with advanced biliary tract cancer (ABC-03): a randomised phase 2 trial. Lancet Oncol 16:967–978
Yamamoto M, Takasaki K, Otsubo T et al (2001) Recurrence after surgical resection of intrahepatic cholangiocarcinoma. J Hepatobiliary Pancreat Surg 8:154–157
Ohtsuka M, Kimura F, Shimizu H et al (2009) Significance of repeated resection for recurrent intrahepatic cholangiocarcinoma. Hepatogastroenterology 56:1–5
Ercolani G, Vetrone G, Grazi GL et al (2010) Intrahepatic cholangiocarcinoma: primary liver resection and aggressive multimodal treatment of recurrence significantly prolong survival. Ann Surg 252:107–114
Kamphues C, Seehofer D, Eisele RM et al (2010) Recurrent intrahepatic cholangiocarcinoma: single-center experience using repeated hepatectomy and radiofrequency ablation. J Hepatobiliary Pancreat Sci 17:509–515
Saiura A, Yamamoto J, Kokudo N et al (2011) Intrahepatic cholangiocarcinoma: analysis of 44 consecutive resected cases including 5 cases with repeat resections. Am J Surg 201:203–208
Song SC, Heo JS, Choi DW et al (2011) Survival benefits of surgical resection in recurrent cholangiocarcinoma. J Korean Surg Soc 81:187–194
Sulpice L, Rayar M, Boucher E et al (2012) Treatment of recurrent intrahepatic cholangiocarcinoma. Br J Surg 99:1711–1717
Takahashi Y, Ebata T, Yokoyama Y et al (2015) Surgery for recurrent biliary tract cancer: a single-center experience with 74 consecutive resections. Ann Surg 262:121–129
Souche R, Addeo P, Oussoultzoglou E et al (2016) First and repeat liver resection for primary and recurrent intrahepatic cholangiocarcinoma. Am J Surg 212:221–229
Digestive system. In: Edge SBBD, Compton CC, Fritz AG, Greene FL, Trotti A (ed) AJCC cancer staging manual seventh edition, 7th edn. Springer, New York, pp 201–240 (2010)
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Neoptolemos JP, Moore MJ, Cox TF et al (2012) Effect of adjuvant chemotherapy with fluorouracil plus folinic acid or gemcitabine vs observation on survival in patients with resected periampullary adenocarcinoma: the ESPAC-3 periampullary cancer randomized trial. JAMA 308:147–156
Oettle H, Neuhaus P, Hochhaus A et al (2013) Adjuvant chemotherapy with gemcitabine and long-term outcomes among patients with resected pancreatic cancer: the CONKO-001 randomized trial. JAMA 310:1473–1481
Uesaka K, Boku N, Fukutomi A et al (2016) Adjuvant chemotherapy of S-1 versus gemcitabine for resected pancreatic cancer: a phase 3, open-label, randomised, non-inferiority trial (JASPAC 01). Lancet 388:248–257
Weitz J, Blumgart LH, Fong Y et al (2005) Partial hepatectomy for metastases from noncolorectal, nonneuroendocrine carcinoma. Ann Surg 241:269–276
Adam R, Chiche L, Aloia T et al (2006) Hepatic resection for noncolorectal nonendocrine liver metastases: analysis of 1,452 patients and development of a prognostic model. Ann Surg 244:524–535
Earle SA, Perez EA, Gutierrez JC et al (2006) Hepatectomy enables prolonged survival in select patients with isolated noncolorectal liver metastasis. J Am Coll Surg 203:436–446
Lendoire J, Moro M, Andriani O et al (2007) Liver resection for non-colorectal, non-neuroendocrine metastases: analysis of a multicenter study from Argentina. HPB (Oxford) 9:435–439
Reddy SK, Barbas AS, Marroquin CE et al (2007) Resection of noncolorectal nonneuroendocrine liver metastases: a comparative analysis. J Am Coll Surg 204:372–382
O’Rourke TR, Tekkis P, Yeung S et al (2008) Long-term results of liver resection for non-colorectal, non-neuroendocrine metastases. Ann Surg Oncol 15:207–218
Ercolani G, Vetrone G, Grazi GL et al (2009) The role of liver surgery in the treatment of non-colorectal non-neuroendocrine metastases (NCRNNE). Analysis of 134 resected patients. Minerva Chir 64:551–558
Berney T, Mentha G, Roth AD et al (1998) Results of surgical resection of liver metastases from non-colorectal primaries. Br J Surg 85:1423–1427
Elias D, Cavalcanti de Albuquerque A, Eggenspieler P et al (1998) Resection of liver metastases from a noncolorectal primary: indications and results based on 147 monocentric patients. J Am Coll Surg 187:487–493
Hemming AW, Sielaff TD, Gallinger S et al (2000) Hepatic resection of noncolorectal nonneuroendocrine metastases. Liver Transpl 6:97–101
Laurent C, Rullier E, Feyler A et al (2001) Resection of noncolorectal and nonneuroendocrine liver metastases: late metastases are the only chance of cure. World J Surg 25:1532–1536
Ercolani G, Grazi GL, Ravaioli M et al (2005) The role of liver resections for noncolorectal, nonneuroendocrine metastases: experience with 142 observed cases. Ann Surg Oncol 12:459–466
Yedibela S, Gohl J, Graz V et al (2005) Changes in indication and results after resection of hepatic metastases from noncolorectal primary tumors: a single-institutional review. Ann Surg Oncol 12:778–785
Schmelzle M, Eisenberger CF, am Esch JS 2nd et al (2010) Non-colorectal, non-neuroendocrine, and non-sarcoma metastases of the liver: resection as a promising tool in the palliative management. Langenbecks Arch Surg 395:227–234
Marudanayagam R, Sandhu B, Perera MT et al (2011) Hepatic resection for non-colorectal, non-neuroendocrine, non-sarcoma metastasis: a single-centre experience. HPB (Oxford) 13:286–292
Kleeff J, Reiser C, Hinz U et al (2007) Surgery for recurrent pancreatic ductal adenocarcinoma. Ann Surg 245:566–572
Thomas RM, Truty MJ, Nogueras-Gonzalez GM et al (2012) Selective reoperation for locally recurrent or metastatic pancreatic ductal adenocarcinoma following primary pancreatic resection. J Gastrointest Surg 16:1696–1704
Fong Y (2013) Chemotherapy and resection for colorectal metastases. Lancet Oncol 14:1148–1149
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors have nothing to disclose.
Rights and permissions
About this article
Cite this article
Motoyama, H., Kobayashi, A., Yokoyama, T. et al. Survival Benefits of Surgical Resection in Patients with Recurrent Biliary Tract Carcinoma. World J Surg 41, 2817–2829 (2017). https://doi.org/10.1007/s00268-017-4107-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4107-3