Abstract
Background
Radical antegrade modular pancreatosplenectomy (RAMPS) is a modification of standard retrograde pancreatosplenectomy (SRPS) used to achieve the dissection of N1 lymph nodes, early vascular control, and negative posterior margins. However, there have been few comparative studies regarding the clinical outcomes of the RAMPS and SRPS procedures.
Methods
Ninety-three patients underwent distal pancreatectomy for the treatment of pancreas body and tail adenocarcinoma between 2000 and 2014. Clinicopathologic data were retrospectively analyzed in this study. We compared short- and long-term outcomes between RAMPS and SRPS. In addition, we investigated the significance of clinicopathologic factors in left-sided pancreatic cancers.
Results
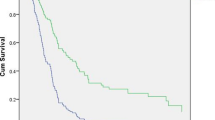
Fifty-three patients underwent RAMPS and 40 patients underwent SRPS. RAMPS revealed a larger number of retrieved lymph nodes [28.4 ± 11.6 vs 20.7 ± 10.1; P = 0.0016], more frequent R0 resection [90.5 vs 67.5 %; P = 0.0053], less intraoperative bleeding than SRPS [485.4 ± 63.3 vs 682.3 ± 72.8 ml; P = 0.0444], and shorter operating time (267.3 ± 11.5 vs 339.4 ± 13.2 min; P < 0.0001) as compared with SRPS. In comparing RAMPS and SRPS, RAMPS showed a tendency for improvement of the median survival times than SRPS (47 vs 34 months) (P = 0.1920). In the multivariate analysis, R1 resection, histologic grade, and vascular invasion for overall survival (OS) were found to be independent factors.
Conclusions
There were a decrease of intraoperative bleeding and an increase in the number of retrieved lymph nodes and the R0 resection rate using RAMPS as compared with SRPS.




Similar content being viewed by others
Abbreviations
- RAMPS:
-
radical antegrade modular pancreatosplenectomy
- SRPS:
-
standard retrograde pancreatosplenectomy
- DP:
-
distal pancreatectomy
- CEA:
-
carcinoembryonic antigen
- CA19-9:
-
carbohydrate antigen 19-9
- CY:
-
intraoperative peritoneal washing cytology
- OS:
-
overall survival
- DFS:
-
disease-free survival
- ROC:
-
receiver operating characteristic
- AUC:
-
area under the curve
- CRT:
-
chemoradiotherapy
References
Brennan MF, Moccia RD, Klimstra D (1996) Management of adenocarcinoma of the body and tail of the pancreas. Ann Surg 223:506–512
Strasberg SM, Drebin JA, Linehan D (2003) Radical antegrade modular pancreatosplenectomy. Surgery 133:521–527
Strasberg SM, Linehan DC, Hawkins WG et al (2007) Radical antegrade modular pancreatosplenectomy procedure for adenocarcinoma of the body and tail of the pancreas: ability to obtain negative tangential margins. J Am Coll Surg 204:244–249
Mitchem JB, Hamilton N, Gao F et al (2012) Long-term results of resection of adenocarcinoma of the body and tail of the pancreas using radical antegrade modular pancreatosplenectomy procedure. J Am Coll Surg 214:46–52
Park HJ, You DD, Choi SH et al (2014) Role of radical antegrade modular pancreatosplenectomy for adenocarcinoma of the body and tail of the pancreas. World J Surg 38:186–193
Latorre M, Ziparo V, Nigri G et al (2013) Standard retrograde pancreatosplenectomy versus radical antegrade modular pancreatosplenectomy for body and tail pancreatic adenocarcinoma. Am Surg 79:1154–1158
Trottman P, Swett K, Shen P et al (2014) Comparison of standard distal pancreatectomy and splenectomy with radical antegrade modular pancreatosplenectomy. Am Surg 80:295–300
Yamamoto J, Saiura A, Koga R et al (2010) Improved survival of left-sided pancreas cancer after surgery. Jpn J Clin Oncol 40:530–536
Shimada K, Sakamoto Y, Sano T et al (2006) Prognostic factors after distal pancreatectomy with extended lymphadenectomy for invasive pancreatic adenocarcinoma of the body and tail. Surgery 139:288–295
Fujita T, Nakagohri T, Gotohda N et al (2010) Evaluation of the prognostic factors and significance of lymph node status in in-vasive ductal carcinoma of the body or tail of the pancreas. Pancreas 39:e48–e54
Kanda M, Fujii T, Sahin TT et al (2010) Invasion of the splenic artery is a crucial prognostic factor in carcinoma of the body and tail of the pancreas. Ann Surg 251:483–487
O’Morchoe CC (1997) Lymphatic system of the pancreas. Microsc Res Tech 37:456–477
Edge SB, Compton CC (2010) The American Joint Committee On Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol 17:1471–1474
Sobin LH, Gospodarowicz MK, Wittekind C (2010) TNM classification of malignant tumors, 7th edn. Wiley, New York
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Bassi C, Dervenis C, Butturini G et al (2005) Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 138:8–13
Wente MN, Bassi C, Dervenis C et al (2007) Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery 142:761e–768e
Chang YR, Han SS, Park SJ et al (2012) Surgical outcome of pancreatic cancer using radical antegrade modular pancreatosplenectomy procedure. World J Gastroenterol 18:5595–5600
Kang CM, Kim DH, Lee WJ (2010) Ten years of experience with resection of left-sided pancreatic ductal adenocarcinoma: evolution and initial experience to a laparoscopic approach. Surg Endosc 24:1533–1541
Jang JY, Kang MJ, Heo JS et al (2014) A prospective randomized controlled study comparing outcomes of standard resection and extended resection, including dissection of the nerve plexus and various lymph nodes, in patients with pancreatic head cancer. Ann Surg 259:656–664
Satoi S, Murakami Y, Motoi F et al (2015) Reappraisal of peritoneal washing cytology in 984 patients with pancreatic ductal adenocarcinoma who underwent margin-negative resection. J Gastrointest Surg 19:6–14
Acknowledgments
This work was supported in part by a Japan Society for the Promotion of Science Grant-in-Aid for Scientific Research (B) and (C) and Scientific Research on Innovative Areas (Grant Number: 26108010).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest directly relevant to the content of this article.
Rights and permissions
About this article
Cite this article
Abe, T., Ohuchida, K., Miyasaka, Y. et al. Comparison of Surgical Outcomes Between Radical Antegrade Modular Pancreatosplenectomy (RAMPS) and Standard Retrograde Pancreatosplenectomy (SPRS) for Left-Sided Pancreatic Cancer. World J Surg 40, 2267–2275 (2016). https://doi.org/10.1007/s00268-016-3526-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3526-x