Abstract
Background
Due to the evolving nature of the applications of adipose tissue-derived stem cells (ADSCs) and the rapidly growing body of scientific literature, it is difficult to generate a manual compilation and systematic review of ADSCs in plastic and reconstructive surgery.
Methods
Bibliographic records were retrieved from the Web of Science Core Collection and analyzed with CiteSpace.
Results
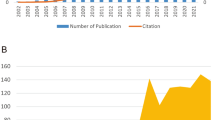
We retrieved 691 publications and their references. We identified 52 research categories. Interdisciplinary studies were common. The journals clustered into 13 subnetworks. The top institutions were Stanford University; University of Pittsburgh; University of Tokyo; University of California, Los Angeles; University of California, Davis; New York University; Tulane University; and University of Michigan. National Institutes of Health and National Natural Science Foundation of China provided the most generous financial support. Studies clustered into 22 topics. Emerging trends may include improvement of fat grafting, and application of ADSCs in wound healing, scleroderma, and facial rejuvenation.
Conclusion
The present study provides a panoramic view of ADSCs in plastic and reconstructive surgery. Analysis of journals, institutions, and grants could help researchers in different ways. Researchers may consider the emerging trends when deciding the direction of their study.
Level of Evidence III
This journal requires that authors assign a level of evidence to each article. For a full description of these Evidence-Based Medicine ratings, please refer to the Table of Contents or the online Instructions to Authors www.springer.com/00266.




Similar content being viewed by others
Change history
06 May 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00266-024-04100-3
References
Xiong B-J, Tan Q-W, Chen Y-J et al (2018) The effects of platelet-rich plasma and adipose-derived stem cells on neovascularization and fat graft survival. Aesthetic Plast Surg 42(1):1–8. https://doi.org/10.1007/s00266-017-1062-1
Harris WM, Plastini M, Kappy N et al (2019) Endothelial differentiated adipose-derived stem cells improvement of survival and neovascularization in fat transplantation. Aesthetic Surg J 39(2):220–232. https://doi.org/10.1093/asj/sjy130
Deng J, Shi Y, Gao Z et al (2018) Inhibition of pathological phenotype of hypertrophic scar fibroblasts via coculture with adipose-derived stem cells. Tissue Eng Part A 24(5–6):382–393. https://doi.org/10.1089/ten.tea.2016.0550
Hsu M-F, Yu S-H, Chuang S-J et al (2018) Can mesenchymal stem cell lysate reverse aging? Aging (Albany NY) 10(10):2900–2910. https://doi.org/10.18632/aging.101595
Ullah M, Sun Z (2018) Stem cells and anti-aging genes: double-edged sword—do the same job of life extension. Stem Cell Res Ther 9(1):3. https://doi.org/10.1186/s13287-017-0746-4
Toyserkani NM, Christensen ML, Sheikh SP, Sørensen JA (2015) Adipose-derived stem cells: new treatment for wound healing? Ann Plast Surg 75(1):117–123. https://doi.org/10.1097/SAP.0000000000000083
McCarthy ME, Brown TA, Bukowska J et al (2018) Therapeutic applications for adipose-derived stem cells in wound healing and tissue engineering. Curr Stem Cell Rep 4(2):127–137. https://doi.org/10.1007/s40778-018-0125-9
Di Summa PG, Schiraldi L, Cherubino M et al (2018) Adipose derived stem cells reduce fibrosis and promote nerve regeneration in rats. Anat Rec 301(10):1714–1721. https://doi.org/10.1002/ar.23841
Zarei F, Negahdari B (2017) Recent progresses in plastic surgery using adipose-derived stem cells, biomaterials and growth factors. J Microencapsul 34(7):699–706. https://doi.org/10.1080/02652048.2017.1370027
Kim Y-J, Jeong J-H (2014) Clinical application of adipose stem cells in plastic surgery. J Korean Med Sci 29(4):462. https://doi.org/10.3346/jkms.2014.29.4.462
Banyard DA, Salibian AA, Widgerow AD, Evans GRD (2015) Implications for human adipose-derived stem cells in plastic surgery. J Cell Mol Med 19(1):21–30. https://doi.org/10.1111/jcmm.12425
Cobo MJ, López-Herrera AG, Herrera-Viedma E, Herrera F (2011) Science mapping software tools: review, analysis, and cooperative study among tools. J Am Soc Inf Sci Technol 62(7):1382–1402. https://doi.org/10.1002/asi.21525
Pan X, Yan E, Cui M, Hua W (2018) Examining the usage, citation, and diffusion patterns of bibliometric mapping software: a comparative study of three tools. J Informetr 12(2):481–493. https://doi.org/10.1016/j.joi.2018.03.005
Chen C, Dubin R, Kim MC (2014) Orphan drugs and rare diseases: a scientometric review (2000–2014). Expert Opin Orphan Drugs 2(7):709–724. https://doi.org/10.1517/21678707.2014.920251
Jehangir S, Barnes EH, McDowell D, Holland AJA (2019) Publishing trends in journal of paediatric surgery, pediatric surgery international and European journal of pediatric surgery over the past three decades. Pediatr Surg Int 35(4):413–418. https://doi.org/10.1007/s00383-019-04445-w
Baek S, Yoon DY, Lim KJ, Cho YK, Seo YL, Yun EJ (2018) The most downloaded and most cited articles in radiology journals: a comparative bibliometric analysis. Eur Radiol 28(11):4832–4838. https://doi.org/10.1007/s00330-018-5423-1
Gutiérrez-Salcedo M, Martínez MÁ, Moral-Munoz JA, Herrera-Viedma E, Cobo MJ (2018) Some bibliometric procedures for analyzing and evaluating research fields. Appl Intell. 48(5):1275–1287. https://doi.org/10.1007/s10489-017-1105-y
Liu Z, Yin Y, Liu W, Dunford M (2015) Visualizing the intellectual structure and evolution of innovation systems research: a bibliometric analysis. Scientometrics 103(1):135–158. https://doi.org/10.1007/s11192-014-1517-y
Muslu Ü (2018) The evolution of breast reduction publications: a bibliometric analysis. Aesthetic Plast Surg 42(3):679–691. https://doi.org/10.1007/s00266-018-1080-7
Lalezari S, Daar DA, Mathew PJ, Mowlds DS, Paydar KZ, Wirth GA (2018) Trends in rhinoplasty research: a 20-Year bibliometric analysis. Aesthetic Plast Surg 42(4):1071–1084. https://doi.org/10.1007/s00266-018-1130-1
Trevatt AEJ, Thomson DR, Miller R, Colquhoun M, Idowu AI, Rahman S (2019) A comparison of the academic impact of plastic surgery units in the United Kingdom and Ireland using bibliometric analysis. J Plast Surg Hand Surg 53(2):97–104. https://doi.org/10.1080/2000656X.2018.1556669
Ruan QZ, Cohen JB, Baek Y et al (2018) Does industry funding mean more publications for subspecialty academic plastic surgeons? J Surg Res 224:185–192. https://doi.org/10.1016/j.jss.2017.12.025
Chen C (2006) CiteSpace II: detecting and visualizing emerging trends and transient patterns in scientific literature. J Am Soc Inf Sci Technol 57(3):359–377. https://doi.org/10.1002/asi.20317
Chen C, Hu Z, Liu S, Tseng H (2012) Emerging trends in regenerative medicine: a scientometric analysis in CiteSpace. Expert Opin Biol Ther 12(5):593–608. https://doi.org/10.1517/14712598.2012.674507
Schvaneveldt RW, Durso FT, Dearholt DW (1989) Network structures in proximity data. Psychol Learn Motiv 24:249–284. https://doi.org/10.1016/S0079-7421(08)60539-3
Rigotti G, Marchi A, Galiè M et al (2007) Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg 119(5):1409–1422. https://doi.org/10.1097/01.prs.0000256047.47909.71
Yoshimura K, Sato K, Aoi N, Kurita M, Hirohi T, Harii K (2008) Cell-assisted lipotransfer for cosmetic breast augmentation: supportive use of adipose-derived stem/stromal cells. Aesthetic Plast Surg 32(1):48–55. https://doi.org/10.1007/s00266-007-9019-4
Coleman SR (2006) Structural fat grafting: more than a permanent filler. Plast Reconstr Surg 118(3 SUPPL.):108S–120S. https://doi.org/10.1097/01.prs.0000234610.81672.e7
Atef A, Shaker AAEM, Sadek EY, Boughdadi NS, Atalla SS, Abu Zahra F (2018) The optimal timing of adipose derived stem cells injection to improve skin flap survival in a rat model. Eur J Plast Surg 41(4):387–394. https://doi.org/10.1007/s00238-018-1400-9
Yang Y, Qu R, Fan T et al (2018) Cross-talk between microtubules and the linker of nucleoskeleton complex plays a critical role in the adipogenesis of human adipose-derived stem cells. Stem Cell Res Ther 9(1):125. https://doi.org/10.1186/s13287-018-0836-y
Cho KH, Uthaman S, Park IK, Cho CS (2018) Injectable biomaterials in plastic and reconstructive surgery: a Review of the Current Status. Tissue Eng Regen Med 15(5):559–574. https://doi.org/10.1007/s13770-018-0158-2
de Gast H, Torrensma B, Fitzgerald E, Stevens H (2016) The treatment of chronic neuropathic pain: bio (regenerative) pain treatment through lipofilling. A short communication case series. Pain Physician 19(3):E495–E498
Ichim TE, Harman RJ, Min WP et al (2010) Autologous stromal vascular fraction cells: a tool for facilitating tolerance in rheumatic disease. Cell Immunol 264(1):7–17. https://doi.org/10.1016/j.cellimm.2010.04.002
Tabit CJ, Slack GC, Fan K, Wan DC, Bradley JP (2012) Fat grafting versus adipose-derived stem cell therapy: distinguishing indications, techniques, and outcomes. Aesthetic Plast Surg 36(3):704–713. https://doi.org/10.1007/s00266-011-9835-4
Schipper BM, Marra KG, Zhang W, Donnenberg AD, Rubin JP (2008) Regional anatomic and age effects on cell function of human adipose-derived stem cells. Ann Plast Surg 60:538–544. https://doi.org/10.1097/sap.0b013e3181723bbe
Shin H, Perdue RR (2018) Self-service technology research: a bibliometric co-citation visualization analysis. Int J Hosp Manag 2019(80):101–112. https://doi.org/10.1016/j.ijhm.2019.01.012
He Y, Lu F (2016) Development of synthetic and natural materials for tissue engineering applications using adipose stem cells. Stem Cells Int. https://doi.org/10.1155/2016/5786257
Cai J, Li B, Wang J et al (2017) tamoxifen prefabricated beige adipose tissue improves fat graft survival in Mice. Plast Reconstr Surg 141(4):1. https://doi.org/10.1097/PRS.0000000000004220
Levi B, Nelson ER, Hyun JS et al (2012) Enhancement of human adipose-derived stromal cell angiogenesis through knockdown of a BMP-2 inhibitor. Plast Reconstr Surg 129(1):53–66. https://doi.org/10.1097/PRS.0b013e3182361ff5
Wu I, Nahas Z, Kimmerling KA, Rosson GD, Elisseeff JH (2012) An injectable adipose matrix for soft-tissue reconstruction. Plast Reconstr Surg 129(6):1247–1257. https://doi.org/10.1097/PRS.0b013e31824ec3dc
Zuk PA, Zhu M, Mizuno H et al (2001) Multilineage cells from human adipose tissue: implications for cell-based therapies. Tissue Eng 7(2):211–228. https://doi.org/10.1089/107632701300062859
Lee JA, Parrett BM, Conejero JA et al (2003) Biological alchemy: engineering bone and fat from fat-derived stem cells. Ann Plast Surg 50(6):610–617. https://doi.org/10.1097/01.SAP.0000069069.23266.35
Cowan CM, Shi Y-Y, Aalami OO et al (2004) Adipose-derived adult stromal cells heal critical-size mouse calvarial defects. Nat Biotechnol 22(5):560–567. https://doi.org/10.1038/nbt958
Dragoo JL, Choi JY, Lieberman JR et al (2003) Bone induction byBMP-2 transduced stem cells derived from human fat. J Orthop Res 21(4):622–629. https://doi.org/10.1016/S0736-0266(02)00238-3
Gentile P, De Angelis B, Pasin M et al (2014) Adipose-derived stromal vascular fraction cells and platelet-rich plasma: basic and clinical evaluation for cell-based therapies in patients with scars on the face. J Craniofac Surg 25(1):267–272. https://doi.org/10.1097/01.scs.0000436746.21031.ba
Coleman SR, Katzel EB (2015) Fat grafting for facial filling and regeneration. Clin Plast Surg 42(3):289–300. https://doi.org/10.1016/j.cps.2015.04.001
Cleveland EC, Albano NJ, Hazen A (2015) Roll, spin, wash, or filter? Processing of lipoaspirate for autologous fat grafting: an updated, evidence-based review of the literature. Plast Reconstr Surg 136(4):706–713. https://doi.org/10.1097/PRS.0000000000001581
Pu LLQ (2012) Towards more rationalized approach to autologous fat grafting. J Plast Reconstr Aesthetic Surg 65(4):413–419. https://doi.org/10.1016/j.bjps.2011.09.033
Li F, Guo W, Li K et al (2015) Improved fat graft survi val by different volume fractions of platelet-rich plasma and adipose-derived stem cells. Aesthetic Surg J 35(3):319–333. https://doi.org/10.1093/asj/sju046
Cervelli V, Gentile P, De Angelis B et al (2011) Application of enhanced stromal vascular fraction and fat grafting mixed with PRP in post-traumatic lower extremity ulcers. Stem Cell Res 6(2):103–111. https://doi.org/10.1016/j.scr.2010.11.003
Raposio E, Bertozzi N, Bonomini S et al (2016) Adipose-derived stem cells added to platelet-rich plasma for chronic skin ulcer therapy. Wounds a Compend Clin Res Pract 28(4):126–131
Hassan WU, Greiser U, Wang W (2014) Role of adipose-derived stem cells in wound healing. Wound Repair Regen 22(3):313–325. https://doi.org/10.1111/wrr.12173
Magalon G, Daumas A, Sautereau N, Magalon J, Sabatier F, Granel B (2015) Regenerative Approach to Scleroderma with Fat Grafting. Clin Plast Surg 42(3):353–364. https://doi.org/10.1016/j.cps.2015.03.009
Rigotti G, Charles-De-Sá L, Gontijo-De-Amorim NF et al (2016) Expanded stem cells, Stromal-vascular fraction, and platelet-rich plasma enriched fat: comparing results of different facial rejuvenation approaches in a clinical trial. Aesthetic Surg J 36(3):261–270. https://doi.org/10.1093/asj/sjv231
Salgado AJBOG, Reis RLG, Sousa NJC, Gimble JM (2010) Adipose tissue derived stem cells secretome: soluble factors and their roles in regenerative medicine. Curr Stem Cell Res Ther 5(2):103–110
Khouri RK, Smit JM, Cardoso E et al (2013) Percutaneous aponeurotomy and lipofilling: a regenerative alternative to flap reconstruction? Plast Reconstr Surg 132(5):1280–1290. https://doi.org/10.1097/PRS.0b013e3182a4c3a9
Borovikova AA, Ziegler ME, Banyard DA et al (2018) Adipose-derived tissue in the treatment of dermal fibrosis: antifibrotic effects of adipose-derived stem cells. Ann Plast Surg 80(3):297–307. https://doi.org/10.1097/SAP.0000000000001278
Acknowledgments
This work was supported by the Scientific Research Team Construction Foundation of Henan Province (TD2011010).
Author information
Authors and Affiliations
Contributions
GSL and LBL designed this study; WHL and KS analyzed and interpreted the data, and were major contributors in writing the manuscript. XRZ, HYZ, HZ and AJ analyzed and interpreted the data. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to disclose.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
For this type of study informed consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Wenhui Liu and Ke Shi are co-first authors of this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, W., Shi, K., Zhu, X. et al. Adipose Tissue-derived Stem cells in Plastic and Reconstructive Surgery: A Bibliometric Study. Aesth Plast Surg 45, 679–689 (2021). https://doi.org/10.1007/s00266-020-01615-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00266-020-01615-3