Abstract
Objective
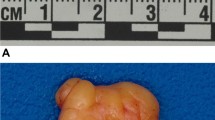
The purpose of this study was to describe the imaging characteristics of subcutaneous amyloid deposits occurring at sites of insulin injection, commonly known as “insulin balls,” in diabetic patients on ultrasound, CT, and MRI with pathologic correlation.
Materials and methods
We retrospectively reviewed the radiographic findings of 14 lesions in 9 patients diagnosed with subcutaneous amyloid deposits at our institution between 2005–2015. Three board-certified radiologists analyzed the following: (1) the shape, size, margin, morphologic characteristics, and blood flow on US using the color Doppler signal, (2) shape, size, margin, attenuation, and presence or absence of contrast enhancement on CT, and (3) shape, size, margin, signal intensity, and presence or absence of contrast enhancement on MRI.
Results
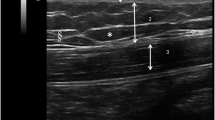
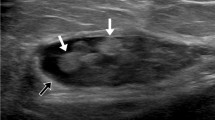
All lesions showed ill-defined hypovascular subcutaneous nodules with irregular margins. The median diameter of lesions was 50.4 mm on US, 46.8 mm on CT, and 51.4 mm on MRI. The internal echogenicity of subcutaneous amyloid deposits was hypoechoic and heterogeneous on US. All lesions showed isodensity compared to muscle with irregular margins and minimal contrast enhancement on CT. Both T1- and T2-weighted MR images showed low signal intensity compared with subcutaneous fat. Normal diffusion and minimal contrast enhancement were seen.
Conclusions
Subcutaneous amyloid deposits which cause insulin resistance are typically ill-defined and heterogeneous hypovascular subcutaneous nodules with irregular margins on imaging that correspond to insulin injection sites. It is also characteristic that T2WI shows low intensity compared with fat on MRI, reflective of the amyloid content.




Similar content being viewed by others
References
Storkel S, Schneider HM, Muntefering H, Kashiwagi S. Iatrogenic, insulin-dependent, local amyloidosis. Lab Investig. 1983;48(1):108–11.
Dische FE, Wernstedt C, Westermark GT, Westermark P, Pepys MB, Rennie JA, et al. Insulin as an amyloid-fibril protein at sites of repeated insulin injections in a diabetic patient. Diabetologia. 1988;31(3):158–61.
Swift B. Examination of insulin injection sites: an unexpected finding of localized amyloidosis. Diabet Med. 2002;19(10):881–2.
Sahoo S, Reeves W, DeMay RM. Amyloid tumor: a clinical and cytomorphologic study. Diagn Cytopathol. 2003;28(6):325–8.
Albert SG, Obadiah J, Parseghian SA, Yadira Hurley M, Mooradian AD. Severe insulin resistance associated with subcutaneous amyloid deposition. Diabetes Res Clin Pract. 2007;75(3):374–6.
Yumlu S, Barany R, Eriksson M, Rocken C. Localized insulin-derived amyloidosis in patients with diabetes mellitus: a case report. Hum Pathol. 2009;40(11):1655–60.
Nagase T, Katsura Y, Iwaki Y, Nemoto K, Sekine H, Miwa K, et al. The insulin ball. Lancet. 2009;373(9658):184.
Lonsdale-Eccles AA, Gonda P, Gilbertson JA, Haworth AE. Localized cutaneous amyloid at an insulin injection site. Clin Exp Dermatol. 2009;34(8):e1027–8.
Shikama Y, Kitazawa J, Yagihashi N, Uehara O, Murata Y, Yajima N, et al. Localized amyloidosis at the site of repeated insulin injection in a diabetic patient. Intern Med. 2010;49(5):397–401.
Sie MP, van der Wiel HE, Smedts FM, de Boer AC. Human recombinant insulin and amyloidosis: an unexpected association. Neth J Med. 2010;68(3):138–40.
Endo JO, Rocken C, Lamb S, Harris RM, Bowen AR. Nodular amyloidosis in a diabetic patient with frequent hypoglycemia: sequelae of repeatedly injecting insulin without site rotation. J Am Acad Dermatol. 2010;63(6):e113–4.
Kudo-Watanuki S, Kurihara E, Yamamoto K, Mukai K, Chen KR. Coexistence of insulin-derived amyloidosis and an overlying acanthosis nigricans-like lesion at the site of insulin injection. Clin Exp Dermatol. 2013;38(1):25–9.
Okamura S, Hayashino Y, Kore-Eda S, Tsujii S. Localized amyloidosis at the site of repeated insulin injection in a patient with type 2 diabetes. Diabetes Care. 2013;36(12):e200.
Giovagnorio F, Andreoli C, De Cicco ML. Color Doppler sonography of focal lesions of the skin and subcutaneous tissue. J Ultrasound Med. 1999;18(2):89–93.
Kiss E, Keusch G, Zanetti M, Jung T, Schwarz A, Schocke M, et al. Dialysis-related amyloidosis revisited. AJR Am J Roentgenol. 2005;185(6):1460–7.
Gean-Marton AD, Kirsch CF, Vezina LG, Weber AL. Focal amyloidosis of the head and neck: evaluation with CT and MR imaging. Radiology. 1991;181(2):521–5.
Vanhoenacker FM, Eyselbergs M, Van Hul E, Van Dyck P, De Schepper AM. Pseudotumoural soft tissue lesions of the hand and wrist: a pictorial review. Insights Imaging. 2011;2(3):319–33.
Morten IJ, Gosal WS, Radford SE, Hewitt EW. Investigation into the role of macrophages in the formation and degradation of beta 2-microglobulin amyloid fibrils. J Biol Chem. 2007;282(40):29691–700.
Yoshizaki T, Honda M. Insulin absorption in a patient with local subcutaneous amyloid deposition. J Japan Diab Soc. 2012;55(10):786–92.
Hauner H, Stockamp B, Haastert B. Prevalence of lipohypertrophy in insulin-treated diabetic patients and predisposing factors. Exp Clin Endocrinol Diabetes. 1996;104(2):106–10.
McNally PG, Jowett NI, Kurinczuk JJ, Peck RW, Hearnshaw JR. Lipohypertrophy and lipoatrophy complicating treatment with highly purified bovine and porcine insulins. Postgrad Med J. 1988;64(757):850–3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Tanio, N., Nozaki, T., Matsusako, M. et al. Imaging characteristics of subcutaneous amyloid deposits in diabetic patients: the “insulin ball”. Skeletal Radiol 47, 85–92 (2018). https://doi.org/10.1007/s00256-017-2749-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-017-2749-8