Abstract
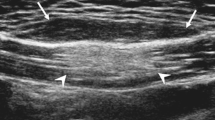
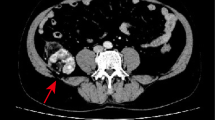
We report the case of a 34-year-old female who was evaluated for a right lower extremity soft-tissue mass, found to be a large cystic lesion bound by fibrous tissue containing innumerable, freely mobile nodules of fat. Her presentation suggested the diagnosis of nodular cystic fat necrosis (NCFN), a rare entity that likely represents a morphological subset of fat necrosis potentially caused by vascular insufficiency secondary to local trauma. Her lesion was best visualized using MRI, which revealed characteristic imaging features of NCFN including nodular lipid-signal foci that suppress on fat-saturated sequences, intralesional fluid with high signal intensity on T2-weighted imaging, and a contrast-enhancing outer capsule with low signal intensity on T1-weighted imaging. Ultrasound imaging offered the advantage of showing mobile hyperechogenic foci within the anechoic cystic structure, and the lesion was otherwise visualized on radiography as a nonspecific soft-tissue radiopacity. She was managed with complete surgical excision with pathologic evaluation demonstrating, similar to the radiologic features, innumerable free-floating, 1–5 mm, smooth, nearly uniform spherical nodules of mature fat with widespread necrosis contained within a thick fibrous pseudocapsule. Follow-up imaging revealed no evidence of remaining or recurrent disease on postoperative follow-up MRI. The differential diagnosis includes lipoma with fat necrosis, lipoma variant, atypical lipomatous tumor, and a Morel-Lavallée lesion. There is overlap in the imaging features between fat necrosis and both benign and malignant adipocytic tumors, occasionally making this distinction based solely on imaging findings challenging. To our knowledge, this is the largest example of NCFN ever reported.





Similar content being viewed by others
References
Hurt MA, Santa Cruz DJ. Nodular-cystic fat necrosis: A reevaluation of the so-called mobile encapsulated lipoma. J Am Acad Dermatol. 1989;21:493–8.
Przyjemski CJ, Schuster SR. Nodular-cystic fat necrosis. J Pediatr. 1977;91:605–7.
Ban M. Nodular-cystic fat necrosis-A review of 147 Japanese patients. J Dermatol Res. 2016;1:65–8.
Kiryu H, Rikihisa W, Furue M. Encapsulated fat necrosis – A clinicopathological study of 8 cases and a literature review. J Cutan Pathol. 2000;27:19–23.
Oh C-W, Kim K-H. A case of nodular cystic fat necrosis: The end stage lesion showing calcification and lipomembranous changes. J Dermatol. 1998;25:616–21.
Pujol RM, Wang C-Y, Gibson LE, Daniel Su WP. Lipomembranous changes in nodular-cystic fat necrosis. J Cutan Pathol. 1995;22:551–5.
Weaver J, Downs-Kelly E, Goldblum JR, Turner S, Kulkarni S, Tubbs RR, et al. Fluorescence in situ hybridization for MDM2 gene amplification as a diagnostic tool in lipomatous neoplasms. Mod Pathol. 2008;21:943–9.
De Wilde R, Hautekiet A, Geers S, Bossche LV, De Muynck M. Ultrasonographic presentation of nodular cystic fat necrosis after a low-velocity trauma: A case report. J Rehabil Med-Clin Commun. 2022;5:jrmcc00083.
Nakamura Y, Ishizuki S, Ishitsuka Y, Watanabe R, Saito A, Furuta J, et al. Multiple, lipid-containing, subcutaneous cysts suspected of end-stage nodular cystic fat necrosis. J Dermatol. 2020;47:e85–7.
Yi-Hsin H, Ya-Wen H, Yi-Chin S. Multiple floating fat balls on the right lower leg. Indian J Dermatol Venereol Leprol. 2011;77:731.
Gocmen R, Kerimoglu U. An unusual appearance of traumatic fat necrosis: Floating fat balls. European Journal of Radiology Extra. 2008;66:e43–5.
Burkholz KJ, Roberts CC, Lidner TK. Posttraumatic pseudolipoma (fat necrosis) mimicking atypical lipoma or liposarcoma on MRI. Radiol Case Rep. 2007;2:56–60.
Kransdorf MJ, Murphey MD. Radiologic evaluation of soft-tissue masses. AJR Am J Roentgenol. 2000;175:575–87.
Einarsdottir H, Söderlund V, Larson O, Jenner G, Bauer HCF. MR imaging of lipoma and liposarcoma. Acta Radiol SAGE Publications. 1999;40:64–8.
Sundaram M, McLeod RA. MR imaging of tumor and tumorlike lesions of bone and soft tissue. AJR Am J Roentgenol Ray Soc. 1990;155:817–24.
Bancroft LW, Kransdorf MJ, Peterson JJ, O’Connor MI. Benign fatty tumors: Classification, clinical course, imaging appearance, and treatment. Skelet Radiol. 2006;35:719–33.
López JA, Saez F, Alejandro Larena J, Capelastegui A, Martín JI, Canteli B. MRI diagnosis and follow-up of subcutaneous fat necrosis. J Magn Reson Imaging. 1997;7:929–32.
Galant J, Martí-Bonmatí L, Sáez F, Soler R, Alcalá-Santaella R, Navarro M. The value of fat-suppressed T2 or STIR sequences in distinguishing lipoma from well-differentiated liposarcoma. Eur Radiol. 2003;13:337–43.
Canteli B, Saez F, de los Ríos A, Alvarez C. Fat necrosis. Skeletal Radiol. 1996;25:305–7.
Tsai TS, Evans HA, Donnelly LF, Bisset GS, Emery KH. Fat necrosis after trauma: A benign cause of palpable lumps in children. AJR Am J Roentgenol Ray Soc. 1997;169:1623–6.
Chan LP, Gee R, Keogh C, Munk PL. Imaging features of fat necrosis. AJR Am J Roentgenol Ray Soc. 2003;181:955–9.
Drevelegas A, Pilavaki M, Chourmouzi D. Lipomatous tumors of soft tissue: MR appearance with histological correlation. Eur J Radiol. 2004;50:257–67.
Gupta P, Potti TA, Wuertzer SD, Lenchik L, Pacholke DA. Spectrum of fat-containing soft-tissue masses at MR imaging: The common, the uncommon, the characteristic, and the sometimes confusing. Radio Graphics. 2016;36:753–66.
Ahlawat S, Fritz J, Morris CD, Fayad LM. Magnetic resonance imaging biomarkers in musculoskeletal soft tissue tumors: Review of conventional features and focus on nonmorphologic imaging. J Magn Reson Imaging. 2019;50:11–27.
Yee EJ, Stewart CL, Clay MR, McCarter MM. Lipoma and its doppelganger: The atypical lipomatous tumor/well-differentiated liposarcoma. Surg Clin N Am. 2022;102:637–56.
Shannon BA, Ahlawat S, Morris CD, Levin AS, Fayad LM. Do contrast-enhanced and advanced MRI sequences improve diagnostic accuracy for indeterminate lipomatous tumors? Radiol Med. 2022;127:90–9.
Andaç N, Baltacıoǧlu F, Çimşit NÇ, Tüney D, Aktan Ö. Fat necrosis mimicking liposarcoma in a patient with pelvic lipomatosis: CT findings. Clin Imaging. 2003;27:109–11.
Diviti S, Gupta N, Hooda K, Sharma K, Lo L. Morel-Lavallee lesions-Review of pathophysiology, clinical findings, imaging findings and management. J Clin Diagn Res. 2017;11:TE01–4.
Vanhegan IS, Dala-Ali B, Verhelst L, Mallucci P, Haddad FS. The Morel-Lavallée lesion as a rare differential diagnosis for recalcitrant bursitis of the knee: Case report and literature review. Case Rep Orthop. 2012;2012:593193.
Bonilla-Yoon I, Masih S, Patel DB, White EA, Levine BD, Chow K, et al. The Morel-Lavallée lesion: Pathophysiology, clinical presentation, imaging features, and treatment options. Emerg Radiol. 2014;21:35–43.
Mellado JM, Bencardino JT. Morel-Lavallée lesion: Review with emphasis on MR imaging. Magn Reson Imaging Clin N Am. 2005;13:775–82.
Mellado JM, del Palomar LP, Díaz L, Ramos A, Saurí A. Long-standing Morel-Lavallée lesions of the trochanteric region and proximal thigh: MRI features in five patients. AJR Am J Roentgenol Ray Soc. 2004;182:1289–94.
Masarapu V, Wang PS, Gorbachova T. Slow-growing buttock mass after failure of incorporation of autologous fat transfer for gluteal augmentation: Ultrasound and MRI features. Skelet Radiol. 2020;49:1669–75.
Kontoes P, Gounnaris G. Complications of fat transfer for breast augmentation. Aesthet Plast Surg. 2017;41:1078–82.
Lin DJ, Wong TT, Ciavarra GA, Kazam JK. Adventures and misadventures in plastic surgery and soft-tissue implants. RadioGraphics Radiol Soc North Am. 2017;37:2145–63.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Shivani Ahlawat: Neurofibromatosis Therapeutic Acceleration Program. Laura M. Fayad: NIH R61, Neurofibromatosis Therapeutic Acceleration Program, Johns Hopkins University. Minsoo Kim, John M. Gross, and Adam S. Levin declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kim, M., Gross, J.M., Ahlawat, S. et al. Nodular cystic fat necrosis: a distinctive rare soft-tissue mass. Skeletal Radiol 53, 583–588 (2024). https://doi.org/10.1007/s00256-023-04426-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-023-04426-0