Abstract
Background
Potentially false-positive findings on radioiodine scans in children with differentiated thyroid carcinoma can mimic functioning thyroid tissue and functioning thyroid carcinomatous tissue. Such false-positive findings comprise variants and pitfalls that can vary slightly in children as compared with adults.
Objective
To determine the patterns and frequency of these potential false-positive findings on radioiodine scans in children with differentiated thyroid carcinoma.
Materials and methods
We reviewed a total of 223 radioiodine scans from 53 pediatric patients (mean age 13.3 years, 37 girls) with differentiated thyroid carcinoma. Focal or regional activity that likely did not represent functioning thyroid tissue or functioning thyroid carcinomatous tissue were categorized as variants or pitfalls. The final diagnosis was confirmed by reviewing the concurrent and follow-up clinical data, correlative ultrasonography, CT scanning, serum thyroglobulin and antithyroglobulin antibody levels. We calculated the frequency of these variants and pitfalls from diagnostic and post-therapy radioiodine scans.
Results
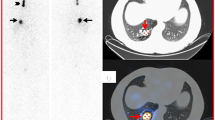
The most common variant on the radioiodine scans was the thymic activity (24/223, 10.8%) followed by the cardiac activity (8/223, 3.6%). Salivary contamination and star artifact, caused by prominent thyroid remnant, were the most important observed pitfalls.
Conclusion
Variants and pitfalls that mimic functioning thyroid tissue or functioning thyroid carcinomatous tissue on radioiodine scan in children with differentiated thyroid carcinoma are not infrequent, but they decrease in frequency on successive radioiodine scans. Potential false-positive findings can be minimized with proper knowledge of the common variants and pitfalls in children and correlation with clinical, laboratory and imaging data.









Similar content being viewed by others
References
Shapiro B, Rufini V, Jarwan A et al (2000) Artifacts, anatomical, and physiological variants, and unrelated diseases that might cause false-positive whole-body 131-I scans in patients with thyroid cancer. Semin Nucl Med 30:115–132
Intenzo CM, Jabbour S, Dam HQ et al (2005) Changing concepts in the management of differentiated thyroid cancer. Semin Nucl Med 35:257–265
Glazer DI, Brown RKJ, Wong KK et al (2013) SPECT/CT evaluation of unusual physiologic radioiodine biodistributions: pearls and pitfalls in image interpretations. Radiographics 33:397–418
Buton L, Morel O, Gault P et al (2013) False-positive iodine-131 whole-body scan findings in patients with differentiated thyroid carcinoma: report of 11 cases and review of literature. Ann Endocrinol 74:221–230
Choi HS, Kim SH, Park SY et al (2014) Clinical significance of diffuse intrathoracic uptake on post-therapy I-131 scans in thyroid cancer patients. Nucl Med Mol Imaging 48:63–71
Ozguven M, Ilgan S, Arslan N et al (2004) Unusual patterns of I-131 contamination. Ann Nucl Med 18:271–274
Omur O, Akgun A, Ozcan Z et al (2009) Clinical implications of diffuse hepatic uptake observed in postablative and post therapeutic I-131 scans. Clin Nucl Med 34:11–14
Biyi A, Oufroukhi Y, Doudouh A (2008) False-positive whole-body I-131 scan in thyroid carcinoma caused by gastrooesophageal reflux disease. Internet J Nucl Med. https://nucleus.iaea.org/HHW/NuclearMedicine/Radioguided_Surgery_and_Radionuclide_Therapy/RadionuclideTherapy/Thyroidmalignant/TeachingCases/ThryoidTeacCases/For_Thyroid_Malig-_ATLAS_I131_False_Positives_.pdf. Accessed 10 May 2016
Blum M, Tiu S, Chu M et al (2011) I-131 SPECT/CT elucidates cryptic findings on planar whole-body scans and can reduce needless therapy with I-131 in post-thyroidectomy thyroid cancer patients. Thyroid 21:1035–1048
Francis GL, Waguespack SG, Bauer AJ et al (2015) Management guidelines for children with thyroid nodules and differentiated thyroid cancer. The American Thyroid Association Guidelines Task Force on Pediatric Thyroid Cancer. Thyroid 25:716–759
Shea KM (2009) Children and radiation. Children’s health and the environment: WHO training package for the health sector. World Health Organization. http://www.who.int/ceh/capacity/radiation.pdf. Accessed 10 May 2016
Brenner DJ, Elliston CD, Hall EJ et al (2001) Estimated risk of radiation-induced fatal cancer from pediatric CT. AJR Am J Roentgenol 176:289–296
Van Nostrand D, Aiken M, Atkins F et al (2009) The utility of radioiodine scans prior to iodine 131 ablation in patients with well-differentiated thyroid cancer. Thyroid 19:849–855
Byeong-Cheol A (2011) Physiologic and false positive pathologic uptakes on radioiodine whole body scan. In: Gholamrezanezhad A (ed) 12 chapters on nuclear medicine. In Tech, Rijeka, pp 1–25
Chung JK (2002) Sodium iodide symporter: its role in nuclear medicine. J Nucl Med 43:1188–1200
Oh J-R, Ahn B-C (2012) False-positive uptake on radioiodine whole-body scintigraphy: physiologic and pathologic variants unrelated to thyroid cancer. Am J Nucl Med Mol Imaging 2:362–385
Michigishi T, Mizukami Y, Shuke NK et al (1993) Visualization of the thymus with therapeutic doses of radioiodine in patients with thyroid cancer. Eur J Nucl Med 20:75–79
Vermiglio F, Baudin E, Travagli JP et al (1996) Iodine concentration by the thymus in thyroid carcinoma. J Nucl Med 37:1830–1831
Wilson LM, Barrington SF, Morrison ID et al (1998) Therapeutic implications of thymic uptake of radioiodine in thyroid carcinoma. Eur J Nucl Med 25:622–628
Mello ME, Flamini RC, Corbo R et al (2009) Radioiodine concentration by the thymus in differentiated thyroid carcinoma: report of five cases. Arq Bras Endocrinol Metabol 53:874–879
Davidson J, McDougall IR (2000) How frequently is the thymus seen on whole-body iodine-131 diagnostic and post-treatment scans? Eur J Nucl Med 27:425–430
Steinmann GG (1986) Changes in the human thymus during aging. Curr Top Pathol 75:43–88
Meller J, Becker W (2000) The human sodium iodine symporter (NIS) as a key for specific thymic iodine-131 uptake. Eur J Nucl Med 27:473–474
Connolly LP, Connolly SA (2003) Thymic uptake of radiopharmaceuticals. Clin Nucl Med 28:648–651
Riesco-Eizaguirre G, Santisteban P (2006) A perspective view of sodium iodide symporter research and its clinical implications. Eur J Endocrinol 155:495–512
Aktas A, Kocabas B, Erhamamcı S et al (2015) Cardiac blood pool activity on postablation radioiodine imaging. Ann Nucl Med 29:170–176
Jong I, Taubman K, Schlicht S (2005) Bronchiectasis simulating pulmonary metastases on iodine-131 scintigraphy in well-differentiated thyroid carcinoma. Clin Nucl Med 30:688–689
Tsai D-H, Hsiao H-C, Tu S-T et al (2007) Concomitant false-positive and false-negative iodine-131 scintigraphy secondary to bronchiectasis and cervical lymph node metastasis in a patient with thyroid cancer: the usefulness of FDG-PET/CT. Ann Nucl Med Sci 20:217–221
Klebanoff SJ, Hamon CB (1972) Role of myeloperoxidase-mediated antimicrobial systems in intact leukocytes. J Reticuloendothel Soc 12:170–196
Regalbuto C, Buscema M, Arena S et al (2002) False-positive findings on (131)I whole-body scans because of posttraumatic superficial scabs. J Nucl Med 43:207–209
Brucker-Davis F, Reynolds JC, Skarulis MC et al (1996) False-positive iodine-131 whole-body scans due to cholecystitis and sebaceous cyst. J Nucl Med 37:1690–1693
Wartofsky L, Van Nostrand D (2006) Thyroid cancer: a comprehensive guide to clinical management, 2nd edn. Humana Press, Totowa
Raza H, Khan AU, Hameed A et al (2006) Quantitative evaluation of salivary gland dysfunction after radioiodine therapy using salivary gland scintigraphy. Nucl Med Commun 27:495–499
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Mostafa, M., Vali, R., Chan, J. et al. Variants and pitfalls on radioiodine scans in pediatric patients with differentiated thyroid carcinoma. Pediatr Radiol 46, 1579–1589 (2016). https://doi.org/10.1007/s00247-016-3655-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-016-3655-2