Abstract
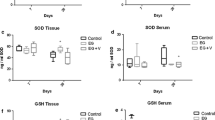
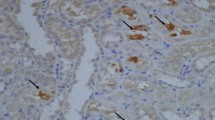
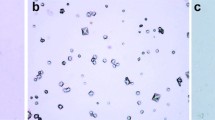
Hyperoxaluria and cell injury are key factors in urolithiasis. Oxalate metabolism may be altered by renal dysfunction and therefore, impact the deposition of calcium oxalate (CaOx) crystals. We investigated the relationship of renal function, oxalate metabolism and CaOx crystal deposition in renal ischemia. One hundred male Sprague–Dawley rats were randomly divided into four groups. Hyperoxaluria model (Group A and B) was established by feeding rats with 0.75 % ethylene glycol (EG). The left renal pedicle was clamped for 30 min to establish renal ischemia Groups (B and C), while Groups A and D underwent sham operation. Then, serum and urine oxalate (Ox), creatinine (Cr) and urea nitrogen (UN) levels were evaluated by liquid chromatography mass spectrometry (LCMS) and ion mass spectrum (IMS) at days 0, 2, 4, 7, and 14. CaOx crystallization was assessed by transmission electron microscope (TEM). A temporal and significant increase of serum Cr and UN levels was observed in Groups B and C compared to values obtained for Groups A and D (P < 0.05). Ox levels in serum and urine were significantly higher in Groups A and B than in the other two groups from day 7 (P < 0.05). In addition, CaOx crystallization was observed in both Groups A and B, but Group B showed earlier and more pronounced crystal deposition in the renal tissue. Our results indicated that renal tubular injury induced by renal ischemia might not affect Ox levels but could promote CaOx crystal retention under hyperoxaluria.








Similar content being viewed by others
References
Mehmet NM, Ender O (2015) Effect of urinary stone disease and its treatment on renal function. World J Nephrol 4(2):271–276
Tsujihata M (2008) Mechanism of calcium oxalate renal stone formation and renal tubular cell injury. Int J Urol 15:115–120
Lieske J, Deganello S (1999) Nucleation, adhesion, and internalization of calcium-containing urinary crystals by renal cells. JAm Soc Nephrol 10:S422–429
Coe FL, Evan A, Worcester E (2005) Kidney stone disease. J Clin Invest 115:2598–2608
Pak CY (1991) Etiology and treatment of urolithiasis. Am J Kidney Dis 18:624–637
Sasikumar P, Gomathi S, Anbazhagan K, Abhishek A, Paul E, Vasudevan V, Sasikumar S, Selvam GS (2014) Recombinant Lactobacillus plantarum expressing and secreting heterologous oxalate decarboxylase prevents renal calcium oxalate stone deposition in experimental rats. J Biomed Sci 30(21):86. doi:10.1186/s12929-014-0086-y
Letavernier E, Vandermeersch S, Traxer O, Tligui M, Baud L, Ronco P, Haymann JP, Daudon M (2015) Demographics and characterization of 10,282 Randall plaque-related kidney stones: a new epidemic? Medicine (Baltimore) 94(10):e566. doi:10.1097/MD.0000000000000566
Verkoelen C, Romijn J (1996) Oxalate transport and calcium oxalate renal stone disease. Urol Res 24(4):183–191
Robertson W (1986) Pathophysiology of stone formation. Urol Int 41(5):329–333
Heilberg IP, Schor N (2006) Renal stone disease: causes, evaluation and medical treatment. Arq Bras Endocrinol Metabol 50(4):823–831
Ferraro PM, Taylor EN, Eisner BH, Gambaro G, Rimm EB, Mukamal KJ, Curhan GC (2013) History of kidney stones and the risk of coronary heart disease. JAMA 310(4):408–415
Fasano JM, Khan SR (2001) Intratubular crystallization of calcium oxalate in the presence of membrane vesicles: an in vitro study. Kidney int 59(1):169–178
Stoller ML, Meng MV, Abrahams HM, Kane JP (2004) The primary stone event: a new hypothesis involving a vascular etiology. J Urol 171(5):1920–1924
Liu Y, Zeng Z, Wang J, Xie L, Li T, He Y, Qin X, Zhao J (2014) Kidney stones and cardiovascular risk: a meta-analysis of cohort studies. Am J Kidney Dis 64(3):402–410
Impellizzeri D, Bruschetta G, Ahmad A, Crupi R, Siracusa R, Di Paola R, Paterniti I, Prosdocimi M, Esposito E, Cuzzocrea S (2015) Effects of palmitoylethanolamide and silymarin combination treatment in an animal model of kidney ischemia and reperfusion. Eur J Pharmacol 762:136–149
Li CY, Deng YL, Sun BH (2009) Taurine protected kidney from oxidative injury through mitochondrial-linked pathway in a rat model of nephrolithiasis. Urol Res 37:211–220
Saw NK, Rao PN, Kavanagh JP (2008) A nidus, crystalluria and aggregation: key ingredients for stone enlargement. Urol Res 36(1):11–15
Hirose M, Tozawa K, Okada A, Hamamoto S, Shimizu H, Kubota Y, Itoh Y, Yasui T, Kohri K (2008) Glyoxylate induces renal tubular cell injury and microstructural changes in experimental mouse. Urol Res 36(3–4):139–147
Vervaet BA, Verhulst A, D’Haese PC, De Broe ME (2009) Nephrocalcinosis: new insights into mechanisms and consequences. Nephrol Dial Transplant 24(7):2030–2035
De Water R, Boevé ER, van Miert PP, Deng G, Cao LC, Stijnen T, de Bruijn WC, Schröder FH (1996) Experimental nephrolithiasis in rats: the effect of ethylene glycol and vitamin D3 on the induction of renal calcium oxalate crystals. Scanning Microsc 10(2):591–601
Khan S (1997) Animal models of kidney stone formation: an analysis. World J Urol 15(4):236–243
Anderson LC, English AM, Wang W, Bai DL, Shabanowitz J, Hunt DF (2015) Protein derivatization and sequential ion/ion reactions to enhance sequence coverage produced by electron transfer dissociation mass spectrometry. Int J Mass Spectrom 377:617–624
De Water R, Noordermeer C, Houtsmuller AB, Nigg AL, Stijnen T, Schröder FH, Kok DJ (2000) Role of macrophages in nephrolithiasis in rats: an analysis of the renal interstitium. Am J Kidney Dis 36(3):615–625
Khan SR (2004) Role of renal epithelial cells in the initiation of calcium oxalate stones. Nephron Exp Nephrol 98(2):e55–60
Yamanobe T, Okada F, Iuchi Y, Onuma K, Tomita Y, Fujii J (2007) Deterioration of ischemia/reperfusion-induced acute renal failure in SOD1-deficient mice. Free Radic Res 41(2):200–207
Rashed T, Menon M, Thamilselvan S (2004) Molecular mechanism of oxalate-induced free radical production and glutathione redox imbalance in renal epithelial cells: effect of antioxidants. Am J Nephrol 24(5):557–568
Thamilselvan S, Khan SR, Menon M (2003) Oxalate and calcium oxalate mediated free radical toxicity in renal epithelial cells: effect of antioxidants. Urol Res 31(1):3–9
Umekawa T, Byer K, Uemura H, Khan SR (2005) Diphenyleneiodium (DPI) reduces oxalate ion-and calcium oxalate monohydrate and brushite crystal-induced upregulation of MCP-1 in NRK 52E cells. Nephrol Dial Transplant 20(5):870–878
Acknowledgments
This work was supported by Chinese Shandong Province Natural Foundation No. ZR1014HM059.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guidelines of Qingdao University for the care and use of animals were followed
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Y. Cao and W. Liu equally contributed to this work.
Rights and permissions
About this article
Cite this article
Cao, Y., Liu, W., Hui, L. et al. Renal tubular injury induced by ischemia promotes the formation of calcium oxalate crystals in rats with hyperoxaluria. Urolithiasis 44, 389–397 (2016). https://doi.org/10.1007/s00240-016-0876-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-016-0876-7