Abstract
Introduction
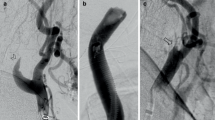
Cerebral hyperperfusion syndrome (HPS) is an uncommon but serious complication of carotid artery stenting (CAS). The purpose of this study was to investigate the efficacy of CT perfusion imaging (CTP) with acetazolamide challenge to identify patients at risk for HPS after CAS.
Methods
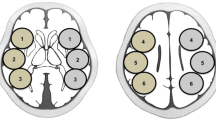
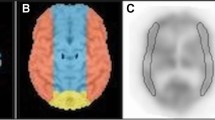
We retrospectively analyzed 113 patients who underwent CTP with rest and acetazolamide challenge before CAS. CTP maps were assessed for absolute and relative cerebral blood flow (CBF), cerebral blood volume (CBV), mean transit time (MTT), and change of each parameter before and after acetazolamide challenge. Patients were divided into two groups according to the HPS after the CAS. Receiver-operating characteristic (ROC) curve analysis was performed to determine the most accurate CTP parameter for the prediction of HPS.
Results
Nine of 113 patients had HPS. There were significant differences for absolute and relative values of resting CBF (p = 0.001 and p = 0.026), resting MTT (p < 0.001 and p = 0.004), post-acetazolamide CBF (p < 0.001 and p = 0.001), post-acetazolamide MTT (p < 0.001 and p = 0.002), and %changes of CBF (p = 0.009) between the HPS and non-HPS groups. ROC curve analysis showed that the CTP parameters with the maximal area under the receiver-operating characteristic curve (AUC) for HPS was the absolute value of post-acetazolamide MTT (AUC 0.909) and the absolute value of resting MTT (AUC 0.896).
Conclusion
Pretreatment CTP with acetazolamide challenge could identify patients at risk for HPS after CAS. Although the CTP parameter that most accurately identified patients at risk for HPS was the absolute value of post-acetazolamide MTT, resting MTT was sufficiently accurate.


Similar content being viewed by others
References
Eskey CJ, Sanelli PC (2005) Perfusion imaging of cerebrovascular reserve. Neuroimaging Clin N Am 15:367–381
Moulakakis KG, Mylonas SN, Sfyroeras GS, Andrikopoulos V (2009) Hyperperfusion syndrome after carotid revascularization. J Vasc Surg 49:1060–1068
Vagal AS, Leach JL, Fernandez-Ulloa M, Zuccarello M (2009) The acetazolamide challenge: techniques and applications in the evaluation of chronic cerebral ischemia. AJNR Am J Neuroradiol 30:876–884
Hosoda K, Kawaguchi T, Shibata Y, Kamei M, Kidoguchi K, Koyama J et al (2001) Cerebral vasoreactivity and internal carotid artery flow help to identify patients at risk for hyperperfusion after carotid endarterectomy. Stroke 32:1567–1573
North American Symptomatic Carotid Endarterectomy Trial Collaborators (1991) Beneficial effect of carotid endarterectomy in symptomatic patients with high-grade carotid stenosis. N Engl J Med 325:445–453
Tseng YC, Hsu HL, Lee TH, Hsieh IC, Chen CJ (2009) Prediction of cerebral hyperperfusion syndrome after carotid stenting: a cerebral perfusion computed tomography study. J Comput Assist Tomogr 33:540–545
van Mook WN, Rennenberg RJ, Schurink GW, van Oostenbrugge RJ, Mess WH, Hofman PA et al (2005) Cerebral hyperperfusion syndrome. Lancet Neurol 4:877–888
Kaku Y, Yoshimura S, Kokuzawa J (2004) Factors predictive of cerebral hyperperfusion after carotid angioplasty and stent placement. AJNR Am J Neuroradiol 25:1403–1408
Grunwald IQ, Politi M, Reith W, Krick C, Karp K, Zimmer A et al (2009) Hyperperfusion syndrome after carotid stent angioplasty. Neuroradiology 51:169–174
Chang CH, Chang TY, Chang YJ, Huang KL, Chin SC, Ryu SJ et al (2011) The role of perfusion computed tomography in the prediction of cerebral hyperperfusion syndrome. PLoS One 6:e19886
Fukuda T, Ogasawara K, Kobayashi M, Komoribayashi N, Endo H, Inoue T et al (2007) Prediction of cerebral hyperperfusion after carotid endarterectomy using cerebral blood volume measured by perfusion-weighted MR imaging compared with single-photon emission CT. AJNR Am J Neuroradiol 28:737–742
Moulakakis KG, Mylonas SN, Sfyroeras GS, Andrikopoulos V (2009) Hyperperfusion syndrome after carotid revascularization. J Vasc Surg 49(4):1060–1068
Bisdas S, Nemitz O, Berding G, Weissenborn K, Ahl B, Becker H et al (2006) Correlative assessment of cerebral blood flow obtained with perfusion CT and positron emission tomography in symptomatic stenotic carotid disease. Eur Radiol 16:2220–2228
Furukawa M, Kashiwagi S, Matsunaga N, Suzuki M, Kishimoto K, Shirao S (2002) Evaluation of cerebral perfusion parameters measured by perfusion CT in chronic cerebral ischemia: comparison with xenon CT. J Comput Assist Tomogr 26:272–278
Chen A, Shyr MH, Chen TY, Lai HY, Lin CC, Yen PS (2006) Dynamic CT perfusion imaging with acetazolamide challenge for evaluation of patients with unilateral cerebrovascular steno-occlusive disease. AJNR Am J Neuroradiol 27:1876–1881
Smith LM, Elkins JS, Dillon WP, Schaeffer S, Wintermark M (2008) Perfusion-CT assessment of the cerebrovascular reserve: a revisit to the acetazolamide challenges. J Neuroradiol 35:157–164
Kikuchi K, Murase K, Miki H, Yasuhara Y, Sugawara Y, Mochizuki T et al (2002) Quantitative evaluation of mean transit times obtained with dynamic susceptibility contrast-enhanced MR imaging and with (133)Xe SPECT in occlusive cerebrovascular disease. AJR Am J Roentgenol 179:229–235
Kang KH, Kim HS, Kim SY (2008) Quantitative cerebrovascular reserve measured by acetazolamide-challenged dynamic CT perfusion in ischemic adult moyamoya disease: initial experience with angiographic correlation. AJNR Am J Neuroradiol 29:1487–1493
Rim NJ, Kim HS, Shin YS, Kim SY (2008) Which CT perfusion parameter best reflects cerebrovascular reserve?: correlation of acetazolamide-challenged CT perfusion with single-photon emission CT in moyamoya patients. AJNR Am J Neuroradiol 29:1658–1663
Yamada K, Wu O, Gonzalez RG, Bakker D, Østergaard L, Copen WA et al (2002) Magnetic resonance perfusion-weighted imaging of acute cerebral infarction: effect of the calculation methods and underlying vasculopathy. Stroke 33:87–94
Calamante F, Gadian DG, Connelly A (2002) Quantification of perfusion using bolus tracking magnetic resonance imaging in stroke: assumptions, limitations, and potential implications for clinical use. Stroke 33:1146–1151
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
We declare that all human and animal studies have been approved by our institutional Ethics Committee and have therefore been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments. We declare that all patients gave informed consent prior to inclusion in this study.
Conflict of interest
We declare that we have no conflict of interest.
Rights and permissions
About this article
Cite this article
Yoshie, T., Ueda, T., Takada, T. et al. Prediction of cerebral hyperperfusion syndrome after carotid artery stenting by CT perfusion imaging with acetazolamide challenge. Neuroradiology 58, 253–259 (2016). https://doi.org/10.1007/s00234-015-1623-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-015-1623-4