Abstract
Purpose
Cerebral hyperperfusion syndrome (CHS) is a critical complication after carotid artery stenting (CAS). However, few CAS studies have evaluated immediate and temporary changes in ipsilateral cerebral blood flow (CBF) quantitatively. The study was performed to evaluate immediate changes in CBF after CAS and subsequent CBF changes in patients with cerebral hyperperfusion (HP) using 123I-IMP SPECT.
Methods
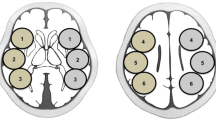
The subjects were 223 patients with chronic extracranial carotid artery stenosis who underwent CAS in our department between March 2010 and March 2020. Quantitative CBF and cerebrovascular reactivity to acetazolamide in the middle cerebral artery were assessed before CAS by 123I-IMP SPECT. CBF was also measured immediately after CAS by 123I-IMP SPECT. When HP was detected, CBF was measured again 3 and 7 days after CAS.
Results
The median (interquartile range) ipsilateral quantitative CBF change after CAS was − 0.1% (− 9.5–8.2%), and the upper value of the 95% CI of the quantitative CBF change was 48.2%. Thus, we defined HP after CAS as an increase in quantitative CBF of > 48.2% compared with the preoperative value. Of 223 patients, 5 (2.2%) had HP, and 4 of these patients (80%) developed CHS. In the CHS patients, HP was maintained for about 3 days and improved after about 7 days.
Conclusion
An immediate CBF increase of > 48.2% after CAS may lead to development of CHS. In CHS after CAS, HP persisted for about 1 week and postoperative management may be required for at least 1 week.






Similar content being viewed by others
Availability of data and material
Data will be made available on request.
Code availability
Not applicable.
References
Huibers AE, Westerink J, de Vries EE et al (2018) Cerebral hyperperfusion syndrome after carotid artery stenting: a systematic review and meta-analysis. Eur J Vasc Endovasc Surg 56:322–333
Piepgras DG, Morgan MK, Sundt TM Jr et al (1988) Intracerebral hemorrhage after carotid endarterectomy. J Neurosurg 68:532–536
Ogasawara K, Sakai N, Kuroiwa T et al (2007) Intracranial hemorrhage associated with cerebral hyperperfusion syndrome following carotid endarterectomy and carotid artery stenting: retrospective review of 4494 patients. J Neurosurg 107:1130–1136
van Mook WN, Rennenberg RJ, Schurink GW et al (2005) Cerebral hyperperfusion syndrome. Lancet Neurol 4:877–888
Ogasawara K, Yukawa H, Kobayashi M et al (2003) Prediction and monitoring of cerebral hyperperfusion after carotid endarterectomy by using single-photon emission computerized tomography scanning. J Neurosurg 99:504–510
Kuhl DE, Barrio JR, Huang SC et al (1982) Quantifying local cerebral blood flow by N-isopropyl-p-[123I]iodoamphetamine (IMP) tomography. Nucl Med 23:196–203
Matsubara S, Moroi J, Suzuki A et al (2009) Analysis of cerebral perfusion and metabolism assessed with positron emission tomography before and after carotid artery stenting. J Neurosurg 11:28–36
Nishizawa S, Tanada S, Yonekura Y et al (1989) Regional dynamics of N-isopropyl-(123I)p-iodoamphetamine in human brain. Nucl Med 30:150–156
North American Symptomatic Carotid Endarterectomy Trial (1991) Methods, patient characteristics, and progress. Stroke 22:711–720
Abou-Chebl A, Reginelli J, Bajzer CT et al (2007) Intensive treatment of hypertension decreases the risk of hyperperfusion and intracerebral hemorrhage following carotid artery stenting. Catheter Cardiovasc Interv 69:690–696
Oka F, Ishihara H, Kato S et al (2013) Cerebral hemodynamic benefits after contralateral carotid artery stenting in patients with internal carotid artery occlusion. AJNR Am J Neuroradiol 34:616–621
Yamada S, Kobayashi M, Watanabe Y et al (2014) Quantitative measurement of blood flow volume in the major intracranial arteries by using 123i-iodoamphetamine SPECT. Clin Nucl Med 39:868–873
Kim KM, Watabe H, Hayashi T et al (2006) Quantitative mapping of basal and vasareactive cerebral blood flow using split-dose 123I-iodoamphetamine and single photon emission computed tomography. Neuroimage 33:1126–1135
Minoshima S, Frey KA, Koeppe RA et al (1995) A diagnostic approach in Alzheimer’s disease using three-dimensional stereotactic surface projections of fluorine-18-FDG PET. J Nucl Med 36:1238–1248
Mizumura S, Nakagawara J, Takahashi M et al (2004) Three-dimensional display in staging hemodynamic brain ischemia for JET study: objective evaluation using SEE analysis and 3D-SSP display. Ann Nucl Med 18:13–21
Ogura T, Hida K, Masuzuka T et al (2009) An automated ROI setting method using Neurostat on cerebral blood flow SPECT images. Ann Nucl Med 23:33–41
Minoshima S, Koeppe RA, Frey KA et al (1994) Anatomic standardization: linear scaling and nonlinear warping of functional brain images. J Nucl Med 35:1528–1537
Iwata T, Mori T, Tajiri H et al (2011) Predictors of hyperperfusion syndrome before and immediately after carotid artery stenting in single-photon emission computed tomography and transcranial color-coded real-time sonography studies. Neurosurgery 68:649–655
Wang S, Han J, Cheng L et al (2017) Risk factors and preventive measures of cerebral hyperperfusion syndrome after carotid artery interventional therapy. Exp Ther Med 14:2517–2520
Bouri S, Thapar A, Shalhoub J et al (2011) Hypertension and the post-carotid endarterectomy cerebral hyperperfusion syndrome. Eur J Vasc Endovasc Surg 41:229–237
Komoribayashi N, Ogasawara K, Kobayashi M et al (2006) Cerebral hyperperfusion after carotid endarterectomy is associated with preoperative hemodynamic impairment and intraoperative cerebral ischemia. J Cereb Blood Flow Metab 26:878–884
Suga Y, Ogasawara K, Saito H et al (2007) Preoperative cerebral hemodynamic impairment and reactive oxygen species produced during carotid endarterectomy correlate with development of postoperative cerebral hyperperfusion. Stroke 38:2712–2717
Horie N, Kitagawa N, Morikawa M et al (2005) Monitoring of regional cerebral oxygenation by near-infrared spectroscopy in carotid arterial stenting: preliminary study. Neuroradiology 47:375–379
Schluter M, Tubler T, Mathey DG et al (2002) Feasibility and efficacy of balloon-based neuroprotection during carotid artery stenting in a single-center setting. J Am Coll Cardiol 40:890–895
Kuroda H, Ogasawara K, Hirooka R et al (2009) Prediction of cerebral hyperperfusion after carotid endarterectomy using middle cerebral artery signal intensity in preoperative single-slab 3-dimensional time-of-flight magnetic resonance angiography. Neurosurgery 64:1065–1071
Timmers HJLM, Wieling W, Karemaker JM et al (2004) Baroreflex failure: a neglected type of secondary hypertension. Neth J Med 62:151–155
Barry MC, Hendriks JM, Alberts G et al (2004) Comparison of catecholamine hormone release in patients undergoing carotid artery stenting or carotid endarterectomy. Endovasc Ther 11:240–250
Dangas G, Laird JR, Satler LF et al (2000) Postprocedural hypotension after carotid artery stent placement: predictors and short- and long-term clinical outcomes. Radiology 215:677–683
Lim S, Javorski MJ, Nassoiy SP et al (2019) Long-term hemodynamic effects after carotid artery revascularization. Vasc Endovascular Surg 53:297–302
McKevitt FM, Sivaguru A, Venables GS et al (2003) Effect of treatment of carotid artery stenosis on blood pressure: a comparison of hemodynamic disturbances after carotid endarterectomy and endovascular treatment. Stroke 34:2576–2581
Bladin CF, Chambers BR (1994) Frequency and pathogenesis of hemodynamic stroke. Stroke 25(2):2179–2182
Orlandi G, Fanucchi S, Fioretti C et al (2001) Characteristics of cerebral microembolism during carotid stenting and angioplasty alone. Arch Neurol 58:1410–1413
Author information
Authors and Affiliations
Contributions
T.N. studied the concept and design and helped in the analysis and interpretation and preparation of the article. F.O. helped in the interpretation of data and critical revision of the article for important intellectual content. K.O. carried out data analysis and interpretation and helped in the preparation of the article. H.I. helped to draft the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no financial or non-financial interests to disclose.
Ethical approval
This study was conducted retrospectively from data obtained for clinical purposes. The study was approved by the IRB of Yamaguchi University School of Medicine.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nishimoto, T., Oka, F., Okazaki, K. et al. Relationship between cerebral hyperperfusion syndrome and the immediate change of cerebral blood flow after carotid artery stenting evaluated by single-photon emission computed tomography. Neuroradiology 64, 1157–1164 (2022). https://doi.org/10.1007/s00234-021-02822-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-021-02822-8