Abstract
Urinary tract infections (UTIs) make up a significant proportion of the global burden of disease in vulnerable groups and tend to substantially impair the quality of life of those affected, making timely detection of UTIs a priority for public health. However, economic and societal barriers drastically reduce accessibility of traditional lab-based testing methods for critical patient groups in low-resource areas, negatively affecting their overall healthcare outcomes. As a result, cellulose-based materials such as paper and thread have garnered significant interest among researchers as substrates for so-called frugal analytical devices which leverage the material’s portability and adaptability for facile and reproducible diagnoses of UTIs. Although the field may be only in its infancy, strategies aimed at commercial penetration can appreciably increase access to more healthcare options for at-risk people. In this review, we catalogue recent advances in devices that use cellulose-based materials as the primary housing or medium for UTI detection and chart out trends in the field. We also explore different modalities employed for detection, with particular emphasis on their ability to be ported onto discreet casings such as sanitary products.
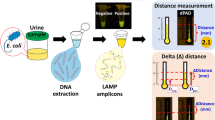
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Urinary tract infections (UTIs) are the most prevalent type of infection observed in women and the elderly. A large proportion of the female population has endured this at least once in their lifetime, and this risk increases as women age [1]. The presence and growth of microorganisms such as bacteria and fungi in the urinary tract is the main cause of UTIs. Bacteria that reside in the urethra, vagina, and digestive tract can inadvertently lead to a UTI and can also affect areas of the body such as the lower urinary tract or the bladder [2]. The bacteria from these regions travel through the urethra and then migrate to the kidneys and the bladder [3]. Pregnant women are more highly susceptible to UTIs than men, due to many anatomical variations such as shorter urethras, relatively easy contamination of the urinary tract by bacteria from the digestive system, i.e. fecal microbiota, and many other causes [4,5,6,7]. UTIs are more frequently caused by Gram-negative organisms than their Gram-positive counterparts. Gram-negative bacteria such as Escherichia coli, Klebsiella, Proteus, and Pseudomonas spp. have been identified in UTI cases, with E. coli being the most common. Additionally, Gram-positive bacteria including Streptococcus, Staphylococcus, and Enterococcus species are know to cause UTIs [7,8,9,10].
In addition to bacteria, fungi can also be pathogenic agents of UTI [11]. Studies have revealed a decline in the percentage of UTIs caused by the commonly responsible Gram-negative organisms and a growing percentage of UTIs caused by fungi, such as Candida species, particularly in the case of critically immunocompromised patients [11,12,13]. The pervasive risk of Candida-based UTIs is well studied and acknowledged, including in infants, the elderly, females, patients on immunosuppressant or antiseizure medication, and those with diabetes mellitus, prolonged hospitalization, recent consumption of broad-spectrum antibiotics, past surgeries irrespective of being urological in nature, abnormalities of the urinary tract, and catheterization, among many more [14,15,16]. In the elderly, upper UTI can cause fever, abdominal tenderness, nausea, and vomiting. The gastrointestinal and respiratory systems of these patients can also be affected. The elderly and postmenopausal women can develop urinary urgency, painful voiding, and low-back pain, among other symptoms. Premenopausal women may also experience a burning sensation with urination [17, 18]. These clinical presentations, which illustrate the distress caused by UTIs afflicting women and the elderly, highlight the need for further research in point-of-care diagnostics for UTI detection.
The urine-based culture method is the most reliable test for determining the presence of UTI. This conventional method requires trained personnel and 48 h to confirm the presence of pathogens (bacteria or fungi) and is also labor-intensive [19] (Fig. 1). Along with urine samples, blood has also been explored as a way to ascertain the presence of pathogens [20]. In addition to culture-based methods, rapid tests using a dipstick have been investigated, where the urine was tested for analytes such as leukocyte esterase, blood, protein, and nitrites [21]. These are also efficient because they can be performed quickly and easily. Among such methods, enzymatic tests are widely used to detect bacteria in urine, or pyuria, including catalase, glucose oxidase, nitrate reductase (Greiss test), and leukocyte esterase. These tests can also be performed at home, as they are noninvasive, easy to administer, and economical, and provide rapid results. However, dipstick-based tests also have considerable trade-offs, most notable of which is their low sensitivity (<90%) [22]. Moreover, dipstick-based tests are prone to contamination by the presence of commensal bacteria picked up when passing through the distal urethra. The reactions on the dipsticks can also be complicated and may be altered by complicated analytical chemistry which may be disrupted by oxidization, reduction, and discoloring agents in the urine, making dipstick-based tests further prone to false-negative and false-positive results [19].
Enzyme-based assays can also be utilized for detecting UTIs [23] by leveraging the catalase enzyme produced by most UTI-presenting pathogens as an indicator. A catalase test can be used for detecting UTIs, but false positives can occur if the catalase is detected due to erythrocytes, white blood cells, or kidney cells. Bacteria also normally metabolize glucose in urine, so a positive glucose oxidase test could be assumed to indicate infection. However, this method is highly sensitive and hence could easily produce false-positive results as well as false negatives when performed on patients with diabetes. Nitrite present in urine has been used as an indicator of UTIs, which can be detected using the Greiss test. This test, however, has low sensitivity [24]. Microscopic examination of urine has been utilized for detecting UTI-causing pathogens via Gram staining. The collected sample is spread on a slide, air-dried, dyed using Gram stain, and then observed under a microscope. However, a notable disadvantage is that the characteristics of the test results tend to be ill-defined, since various criteria are used to determine a positive test result. It is also quite an insensitive test, showing positive results only if the bacterial concentration in the urine is ≥105colony-forming units (CFU)/mL. In addition, it requires a significant amount of labor [20]. Various colorimetric [25, 26] and bioluminescence [27, 28] tests are also available; however, they are quite labor-intensive and were found to provide several false-negative and false-positive results [24].
The detection modalities discussed above present myriad testing paradigms that may be pursued for detecting UTIs. Critically, however, their utility is greatly diminished in the Global South, where they are needed the most. Therefore, the call for a more frugal design and portable porting medium has led scientists to consider readily available cellulose-based substances as potential housing candidates. For over a decade, cellulose substrates such as paper- and thread-based analytical devices (μPADs/μTADs) have been extensively developed and investigated for a wide range of applications including food and water analysis and other environmental applications [29,30,31,32,33,34]. Additionally, the biological relevance of μPADs and μTADs in blood separation and analysis, immunoassay, analyte testing, and usage of smartphones for biosensing have been studied for point-of-care diagnosis [29, 35,36,37]. Papers and threads are made of natural cellulose or synthesized polymer fibers. The manufacturing process allows them to be porous, with capillary gaps that facilitate the flow of liquid. Due to their low cost, portability, biocompatibility, biodegradability, and easy incorporation with other materials, these cellulose-based devices demonstrate a vast application field for fabrication of point-of-care μPADs/μTADs.
It can also be noted that there have been a significantly larger number of studies performed on paper than on thread devices [35, 36, 38]. Various detection methods including colorimetry, fluorometry, and electrochemistry have been utilized for these devices, making them ideal candidates for housing diagnostically relevant assays for easy use [39,40,41]. Along with paper, other cellulose-based substrates have also been combined with regular paper-based devices, such as introducing hemp paper alongside the commonly used filter paper. This device was explored for its potential in potassium detection in urine samples [42]. In this review, we will highlight various studies and developments which have leveraged cellulose-based substrates (paper and thread) and signal transduction methods for the detection of UTIs by targeting a range of biomarkers and pathogens in body fluids via invasive and noninvasive approaches (Fig. 2). We also discuss the possibility of integrating paper- and thread-based devices with hygiene products such as napkins, tampons, and diapers for discreet detection of UTIs.
Detection of urinary tract infection
Cellulose substrates as microfluidic analytical devices
Cellulose substrates, including paper and thread, have been gaining momentum as testing media in health systems, food safety, and environmental monitoring applications in light of their multifaceted properties which are conducive for low-cost fabrication and device portability. Microfluidic paper-based and thread-based analytical devices, commonly known as “μPADs” and “μTADs,” respectively, are reliable and can be widely used in performing assays and diagnostic tests without requiring large quantities of analytes, making them great candidates for remote detection of infections in humans. The use of paper, being highly flexible, porous, biodegradable, easily portable, and disposable, makes the integration of different signal transduction methods highly feasible. The efficiency by which hydrophobic barriers can be imprinted onto the PADs is a large determining factor in the overall manufacturing process. Since they are facile and economical to use, PADs can also be highly customized for a particular use case. Initially, PADs could only be used to identify one specific analyte at a time. To improve the device in this respect, multiple isolated test zones can be created on the device to allow the detection of multiple substances at once. A mechanical or chemical barrier can be used to prevent mixing to some degree. Methods for generating such barriers include photolithography, stamping, origami, and chemical modification. One method for imprinting a hydrophobic barrier on a PAD to prevent leakage of the analytes is discussed later in this section [38, 43,44,45].
While μPADs were developed as an alternative to overcome the limitations of conventional methods, they too are susceptible to limitations. The need for a hydrophobic barrier and their low mechanical strength and low surface tension can limit their wider application to a broad array of microfluidic analytical devices [46,47,48,49]. This led to the exploration of thread as a possible substrate for microfluidic device applications. Features such as their wide utility, high accessibility, low cost, general hydrophilic nature, and biodegradability have promoted wide interest in their potential use [50,51,52,53,54,55]. Thread-based microfluidic devices employ threads as a means for fluid retention and transport, similar to the fluid channels in μPADs, which can execute a variety of analytical assays. Commercial thread consists of thin strands of cotton, nylon, or other fibers which, when twisted together, facilitate the wicking property, or the flow of fluid without an external pumping system. Furthermore, threads tend to display superior tensile and overall mechanical strength when compared to paper, even when wet. Other advantages of μTADs include the ability of surface modulation via immobilization or inclusion of chemicals to fabricate reaction and detection zones [50] and reduce loss of solution volume due to the improved confinement of fluids [36].
Biocompatible substrates such as paper and threads of cotton and lignocellulose have recently been used increasingly frequently in the field of biosensor research as a result of their multiple beneficial use cases and low economic cost. They have already been employed in a variety of colorimetric assays for qualitative and quantitative analyses of nitrates and nitrites. Since these substances are by-products of bacterial metabolism, they can be used as analytes in samples such as urine and saliva to identify the presence of bacterial infection. One such device was utilized for environmental monitoring, where it was used to culture and identify bacteria based on T4 bacteriophage infection of E. coli and to confirm the presence of the enzyme β-galactosidase [56].
A marked advantage of using cellulose, particularly paper, is that researchers are able to design testing solutions that can operate in multiple functional directions [57]. The flexibility of the 3D matrix also allows complex multiplexing to be implemented rather easily by leveraging simple origami procedures [58]. The potential to test for multiple biomarkers on a single platform is particularly beneficial for UTI detection, as it enables researchers to gain more accurate analytical insight into the nature of the disease in question without having to perform multiple tests separately [59]. Furthermore, the current absence of a test that can accurately account for all UTI test cases calls for the use of a multipronged testing regime which can help build confidence in the final diagnosis [60]. Every testing scenario requires its own “best fit” morphology, which can range from lateral flow assays (LFAs) to complex 3D origami structures, each of which is discussed in detail in the sections that follow.
Detecting UTIs using paper- and thread-based cellulose substrates
Colorimetric detection
Colorimetric detection owes a large portion of its appeal to its facile use and visibly differentiable endpoint. However, it can also suffer from disadvantages such as high detection limits and small linear ranges, as well as limited sensitivity [61]. Furthermore, saturation may be reached in color formation, which may also affect the accuracy of cellulose substrates like paper. Colorimetric reactions are frequently difficult to detect at low concentrations, and some sample matrices may produce a background color on the paper [62]. Despite these drawbacks, however, the many advantages and potential for improvement have led to increased research on this technique.
An example of the viability of colorimetric detection in paper-based biosensors is demonstrated by Shafiee et al. [63], who developed a method that integrated cellulose paper and polyester films for use as biosensors. The device employed various detection methods using electrical/optical mechanisms incorporating antibodies and peptides for the detection of viruses and bacterial species from blood or plasma. Other analytes or by-products besides antibodies of pathogens can also be used for the detection of pathogens (Fig. 3a). Chen and Dong present a paper-based device that was fabricated using wax which was melted onto a filter paper, upon which a pattern was transferred. This micro-PAD was then leveraged for detecting nitrite, with a sensitivity range of 0.5 ppm to 100 ppm in urine samples collected in adult diapers. This could be a great low-cost, disposable UTI detection kit in remote areas [64].
(a) Concept of nanoparticle aggregation for detecting bacteria using cellulose paper and smartphone [63]. (b) Design of a paper-based analytical device (PAD) for nitrite quantification, nitrite determination, bacterial cultivation, and identification with dimensions [65]. (c) Schematic illustrating the working procedure for measuring the cation concentration in samples [66]
Another effort in using diapers to detect biomarkers in urine was undertaken by Couto and Dong [67]. An eight-layer device was produced which can utilize a self-locking technique to close the sample inlet within 5 min. This device was able to retain test results for 8 h, which is economical and highly effective, making it a potential candidate for analysis of samples in the future.
Apart from these techniques, DNA-based detection has also been explored extensively. A signal-producing electrochemical aptamer-based sensor was reported to detect ampicillin. The signal was based on target binding changes in the methylene probe which allowed the sensor response to be given within 200 s [68]. Another study reported a device capable of cultivating and identifying bacteria in situ [65]. This method in particular was quicker than the usual methods for UTI detection (Fig. 3b). The cultivation-based detection method relied on β-glucuronidase detection to indirectly determine whether E. coli was present in the sample. The interpretation of results is fundamental for accurate diagnostic results in tests, especially when they are self-administered. Therefore, in order to increase the objectivity and user-friendliness of the devices in question, the integration of smartphones for analysis of results can also be pursued. An example of this was demonstrated in 2020 by Ghaderinezhad et al., who created a smartphone-linked device for detecting the volume of various electrolytes in urine. A colorimetric method was used to detect anions such as NO2− and Cl−(Fig. 3c). This method was also shown to be potentially useful for diagnosing various kidney and-urine related disorders and has the ability to sense the daily concentration of ions, which can help identify disease in the case of abnormal numbers or spikes [66].
That same year, in 2020, an assay was reported that utilized arrays of nanoparticles to detect various bacterial species which could potentially detect UTIs. This system worked by monitoring the reaction between bacterial metabolites and the nanoparticles on a paper-based substrate. The color changes were unique to different strains of bacteria, and even very low concentrations could be detected in minutes, which is extremely fast. Additionally, thread has been leveraged as a detection device used for pathogen identification and quantification. A study by our lab used multifilament cotton thread in a microbial detection assay with smartphone imaging for quick pathogen detection. The detection was based on the by-products released by the pathogens as a result of the metabolic breakdown of the different sugars in the media in question. This method was highly scalable and could potentially differentiate between different attacking pathogens [69] (Table 1).
A method demonstrating paper-based enzyme-linked immunosorbent assay (ELISA) for rapid detection of E. coli was also reported. While this method does have several steps in the procedure, it was successfully used to detect E. coli when it was present at a concentration of under 105 CFU/mL. If improved upon, these could potentially be used for at-home detection kits [70]. In another study, a soaking-drying method was implemented on a resazurin-deposited PAD for the rapid detection of bacterial species and their biotoxicity. A color change occurred due to the reduction of the resazurin by the metabolic processes of Enterococcus faecalis. This could also be recorded and analyzed by smartphones [73].
Fluorometric detection
Fluorometric methods are frequently reported and generally have benefits over traditional biochemical assays, including lower cost and high sensitivity and reproducibility, which are further supplemented by the introduction of smartphone-based analysis [86, 87]. Conventional methods for conducting fluorescence assays in point-of-care diagnostics often use specialized electronic devices such as fluorescence microscopes, scanners, and other equipment that may be too resource-intensive for use in the field or low-resource environments [88].
Therefore, fluorometric detection which can be performed on paper-based devices is essential for the detection of UTIs in the Global South. To this end, a polydimethylsiloxane(PDMS)/paper/glass hybrid microfluidic device was developed with aptamer-functionalized graphene oxide (GO)nano-biosensors [80] for the detection of various pathogens [80]. Paper was utilized as a substrate to avoid complex surface treatment, and the aptamer was adsorbed on the GO surface in order to quench the fluorescence. The presence of the pathogens aided in the release of the aptamer, thus restoring its fluorescence signal. The pathogens that were used for detection were Staphylococcus aureus and Salmonella enterica. However, Lactobacillus acidophilus was the bacterium employed to determine the detection limit of 11.0 CFU.
Antibody-based fluorometric detection methods have also been utilized in UTI pathogen detection. For example, a paper-based device was reported for identifying UTIs, with E. coli as the pathogen, as well as for identifying sexually transmitted diseases (STDs) such as gonorrhea from human urine samples [77]. Anti-E. coli or anti-Neisseria gonorrhoeae antibodies were conjugated onto submicron particles, then pre-loaded and dried on the center of a paper microfluidic channel, which was then used for the pathogen detection (Fig. 4a). An additional benefit of the paper housing was the filtration of possible false-positive signal-causing agent urobilin, responsible for the yellow appearance of urine, along with green fluorescence emission by the paper-based device. Additionally, immunoagglutination of antibody-conjugated particles such as anti-E. coli were formed and quantified via smartphone camera detection. The limit of detection established was 10 CFU/mL. In addition to paper-based devices, thread-based devices have also been employed in pathogen or pathogen-biomarker isolation. An interesting thread-based device on a 3D printed platform was designed and fabricated by Cabot et al. to separate charged solutes, biomolecules, and intact bacterial cells [81]. Threads of different types of fibers were knotted onto each other and used electrophoretically to isolate target solutes or biomolecules, after which various fluorescence reagents were utilized for signal detection of the target particles. Escherichia coli was used as a pathogen to test the application of live bacteria detection from spiked urine samples.
(a) Schematic for the smartphone-based, sensitive μPAD detection of UTI gonorrhea. Reprinted with permission from Ref. [77]. Copyright 2015 Elsevier. (b) Schematic representation of a paper-based device for performing loop-mediated isothermal amplification (LAMP) with real-time simultaneous detection of multiple DNA targets [79]. (c) Loop-mediated isothermal amplification of methicillin-resistantStaphylococcus aureus using paper devices and further validated with clinical samples. Reprinted with permission from Ref. [78]. Copyright 2021 American Chemical Society
Just as in colorimetric methods, DNA-based detection has also been a useful technique for pathogen identification when integrated with fluorescence-based detection. A paper-based device capable of detecting multiple DNA targets through loop-mediated isothermal amplification (LAMP) was reported [79]. Hydroxynaphthol blue fluorescence was employed to analyze real-time LAMP signals in the paper device. Streptococcus agalactiae, Streptococcus pneumoniae, and S. aureus were simultaneously detected using this device, with 4.1 × 102 copies of extracted DNA being the limit of detection (Fig. 4b). Other analytes or biomarkers of pathogens were also used for fluorometric analysis in a study by Ghaderinezhad et al., where a paper-based sensor was devised and created for measuring the concentration of sodium, potassium, and calcium in urine, quantified using fluorescent probes and a smartphone, for image capture and analysis [66], resulting in detection limits of 1.26 mM, 0.85 mM, and 1.2 Mm for sodium, potassium, and calcium, respectively.
More recently, Choopara et al. produced a fluorometric paper-based LAMP on a cellulose membrane paper that demonstrated accuracy similar to quantitative polymerase chain reaction (qPCR) methods (Fig. 4c). The device enabled instant detection of methicillin-resistantS. aureus(MRSA) from clinical blood samples using a paper strip method, in which the lowest recorded detection of the MRSA gene mecA was 10 ag, which is equivalent to one copy of the gene [78] (Table 1).
Electrochemical detection
Colorimetric approaches are effective at intuitively indicating the presence of pathogens both qualitatively and quantitatively [57]. However, colorimetric detection can be rendered less effective when dealing with certain molecules and lower concentrations. As a means to rectify this shortcoming, an appropriate electrochemical technique can be deployed to significantly improve the specificity and accuracy of an assay [89]. In this vein, Prof. Henry’s group proposed electrochemical detection as an alternative to colorimetric detection on paper-based devices [89], which can produce results with superior sensitivity and specificity. This quantitative detection was accomplished through appropriate selection of the electrochemical technique, electrode material, and electrode potential [90], while also facilitating the development of reagent-free detection applications [91]. Moreover, electrochemical methods allow for high-throughput testing, which is especially useful when analyzing large samples in point-of-care diagnostics [61]. While the need for a reference electrode and its sensitivity to pH might be potential drawbacks, various other advantages make this method appealing in the diagnostic space.
A paper-based analytical device that used electrochemical methods to detect the biomarker leukocyte was reported by Ho et al., which could indicate the presence of UTI from urine [82]. Various reagents were deposited onto a silver conducting film on which the leukocyte esterase from the urine reacts with the reagents, leading to a change in resistivity which is then correlated with the quantification of the target (Fig. 5). The device showed promising results regarding UTI diagnosis, demonstrating its reliability by boasting a limit of detection of 1.91 x (5.1 U mg−1 mL−1). Another team of researchers created an electrochemical paper-based device (ePAD) for the detection of Pseudomonas aeruginosa in human saliva. A major advantage was the lack of any sample preparation or separation procedures, which would be of great importance if ported onto a potential UTI test. Pyocyanin was the biomarker virulence factor that was used to detect the pathogen, with a detection limit of 10 nmol L−1 [83] (Table 1).
Schematic representation of leukocyte esterase-PADs for leukocyte esterase detection [82]
Other methods: cell counting and microscopy
Cellulose-based materials not only provide great utility as substrates for microfluidic testing, but also provide considerable advantages as housing for other, more traditional auxiliary testing modalities. A most relevant example of this is demonstrated by the use of filter paper as a solid-phase dilution device [84]. Filtration dilutes and spreads the inoculum onto a solid culture surface, which is optimized to ascertain microbial permeability through filter papers, inoculum size, and ability to exclude vaginal epithelial cells. The pathogens were inoculated and incubated on a grid to aid in colony counting. This technique was devised as a better alternative to the streak plate method. Escherichia coli, S. aureus, Staphylococcus epidermidis, Enterococcus faecalis, Candida albicans, Klebsiella pneumonia, and Enterobacter cloacae were among the numerous pathogens tested from urine samples that could be detected through this technique. The lowest number of cells that could form enough colonies to be considered as testing positive for infection caused by Gram-negative bacteria was ≥104 CFU/mL.
A much more rudimentary yet fundamental application of paper is its use for providing structural support for microscopy implements. Perhaps the most acclaimed demonstration of paper versatility is the Foldscope. The Foldscope is an innovative low-cost and simple paper-based microscope that can be attached to a smartphone camera for viewing. Leveraging this low-cost yet powerful analytical tool, researchers have assessed the ability of the Foldscope in the clinical diagnosis of oral and urinary tract infections [85]. Twenty-five urine samples of patients aged 11–62 years were analyzed using the Foldscope, providing a clear distinction between those who tested positive for UTIs and those who tested negative. This technique can be considered a highly valuable and inexpensive method for detecting UTIs as well as kidney stones in urine samples (Table 1).
The detection methods described provide adequate utility individually but can be specifically tailored to their required application for maximized accuracy. Colorimetric approaches, in general, tend to be the most facile and economical diagnostic approach in all cellulose-based media, as they require minimal training and equipment. Fluorometric approaches have similarly unique applications but with added complexity, as they require specialized equipment for endpoint detection. However, thread-based detection devices in particular need to implement additional calibration when used in fluorescence detection methodologies, as the natural fluorescence of the thread may induce error in the final results [92]. Electrochemical approaches, if applicable, can be adopted as an addition to the previous testing regimes in instances of lower concentration, albeit with increased operational complexity. Other modalities, similar to those previously discussed, have particular use cases but are nevertheless still more economical than most traditional methods.
Lateral flow assay for detecting UTIs
The introduction of lateral flow assays (LFAs) to the market dates back to the early 1990s [93]. Although not directly related to cellulose-based μPADs and μTADs, their contribution to point-of-care diagnostics is especially noteworthy. The inception of the “dipstick” was revolutionary for women’s reproductive health due to its various applications such as pregnancy tests [94, 95], UTI tests [96, 97], and a multitude of other urinalysis techniques including, more broadly, diabetes/ketosis tests [98]. Their ease of use, portability, and low cost make such devices an accessible and frugal alternative to conventional diagnostic methods. Conventional lateral flow assays consist of a multifunctional array of components that overlap with one another. These components are installed onto a backing card/paper for support and fixed in place by an adhesive substance. Testing zones are constructed by creating segments of different materials such that when the urine is drawn through by capillary action, it encounters immobilized conjugates that aid in the detection of the analyte through a colorimetric readout [93].
UTIs in particular have been extensively diagnosed using devices employing lateral flow assays. While earlier studies on urine dipsticks indicated optimistic results [99], subsequent studies demonstrated their limitations such as their general low sensitivity [20, 100], and particular inaccuracies in cases of uncomplicated UTIs [101] and catheterized patients [102]. Similar results were found in a study of UTIs among pregnant women in Tanzania, where it was determined that the dipstick alone was not sufficiently reliable for accurate diagnosis [103]. These limitations motivated efforts for enhanced sensitivity. In 2015, an improvement was made in the sensitivity of an existing rapid urine-based circulating anodic antigen (CAA) test for diagnosing schistosomiasis, by increasing sample input. For many years, the preferred method had been the detection of eggs in urine. However, the detection of a worm-regurgitated antigen (circulating cathodic antigen, CCA) was observed to be comparable or even superior to the egg counting method, thus leading to this study, which was successful in improving sensitivity [104] . That same year, the rapid detection of bacteriuria was studied using an antibody-based lateral flow assay (RapidBac). Rigorous tests were conducted to determine the sensitivity and specificity of the device, ultimately concluding that the RapidBac test for bacteriuria may be valuable in emergency and primary care settings as UTI point-of-care diagnostics [105].
More recently, LFAs and dipstick testing have also been used in combination with flow cytometry for prediction models, such as deducing a probability prediction formula to diagnose a specific pathogenic strain responsible for UTIs in real time [106]. Developments in LFA technology and the subsequent commercialization of the technique [96, 97, 107] have greatly increased the accessibility to accurate UTI testing in point-of-care applications. Therefore, the development of market-ready LFA products which are leveraged towards UTI detection will remain relevant in the women’s health space (Table 2).
Future trends and challenges
Accessible and discreet UTI detection provides tremendous self-reliance to groups that are unable to access critical resources for traditional methods. As a result, the development of techniques that can advance personal capability in the detection of clinically relevant diseases is seeing significant momentum [109, 110]. In particular, the use of cellulose-based substrates for solving structural and sample manipulation problems is generating considerable interest, as it allows for much easier and more economical fabrication of devices [111]. The frugality of cellulose-based diagnostic media is most clearly seen in their ability to serve as an effective base onto which existing assays can be ported. The devices can house multiple stages involved in the detection process, from pathogen sampling to biomarker analysis, and their ability to operate with lower volumes of analyte greatly increases the viability of the method, as it caters to regions with less developed infrastructure, something generally absent in traditional methods. Additionally, cellulose-based materials, when used to structurally support essential equipment such as microscopes, further facilitates frugal innovation in the diagnosis of UTIs. The cost of operation can also be lowered by ensuring significant penetration of these techniques into general commercial use through incorporation into industrial and academic general practice fabrication routines. Mass adoption of the technique as previously described can be achieved by supplementing growth through the implementation of our proposed dual-pronged approach.
The first part of such approach would be focused on improving the base utility of the fabrication substrates by enhancing their technical robustness. In laboratory settings, progressive improvement in the performance efficiency of cellulose devices can be realized by improving the structural integrity and wicking ability of the substrate. This can be done, for example, by developing mercerization techniques geared towards increasing the water absorption and tensile strength of thread-based devices [112]. Traditional mercerization techniques typically use caustic substances such as hydrogen peroxide [113] and hydrochloric acid [114], which tend to leave residues on the substrate and can therefore interfere with the results of a thread-based test which may be sensitive to pH [115]. Additionally, traditional mercerization, in general, is a very cumbersome process that requires numerous resource-intensive treatment steps. As a result, developing long-term solutions and alternatives to these methods is essential for their utility to bear fruit. A viable alternative to this would be using heptane as a mercerizing agent, which can show similar effectiveness without adding extra heating steps and leaving any residue on the thread [76]. These methods when scaled can help produce a more suitable raw product that can be integrated into analytical devices (Fig. 6).
Another development that can contribute to achieving the proliferation of general production is the availability of a standardized manufacturing toolkit. Standardizing production on an industrial scale will require new techniques for facile fabrication which can be automated to boost the production of devices so that they are widely available to people in low-resource areas [116,117,118]. Standardizing an industrial toolkit can also help prevent issues with assay adaptation to the cellulose medium. Due to the complexity of the different methods and approaches for manufacturing cellulose-based analytical devices, their wider-scale adoption and use in industrial settings have been difficult [111]. If a standard toolkit is developed, a modular processing approach can be achieved, where preprocessing or postprocessing steps can be added according to the application. This method can also help in standardizing the equipment one might use for scale-up and automation, further increasing the method’s market penetration. Both these improvements can spur the development of numerous multiplexed detection devices which can detect multiple relevant diseases on a single substrate and sample, significantly increasing the efficiency of the medium [111, 119]. Facile fabrication can also possibly extend to localizing the production of analytical devices in the communities in which they are needed the most, by focusing on the do-it-yourself(DIY) aspect of fabrication [43, 120, 121]. This can be facilitated by developing techniques that use off-the-shelf materials such as pens [122], stamps [123], and general-purpose stationery [124, 125] for fabrication which can be easily done by hand or easily automated.
The second approach towards increasing the potential of cellulose-based substrates would be by lowering the barrier of entry into the use of the technology for all major stakeholders, particularly women (Fig. 6). Keeping the sustainable development goals of gender equality and reducing inequality as benchmarks [126], one can work towards increasing access to UTI detection technologies by enhancing the testing capabilities of paper-based devices and by lowering the cost of manufacturing each testing unit. As mentioned previously in this review, integrating testing devices into hygiene products can greatly increase the number of people the technology can reach and enhance its testing capabilities [76]. This can be built upon by developing additional wearable technologies which allow for continuous monitoring of relevant biomarkers, adding to the amount of data available to make informed clinical decisions [55, 127, 128]. Potential hurdles to the widespread use of wearable technology, namely the limited biocompatibility of the testing reagents and the inability of the device to be disposed of without pretreatment [129], could both be solved by using materials and chemicals that are designed with human contact in mind. Lack of particular preprocessing steps could also be a potential setback in the development of wearable cellulose-based devices [129], although further research into integrating electrochemical methods can work towards ameliorating the issue [130].
Although the current literature has limited if any examples of wearable UTI detection devices [76, 131, 132], wearable systems which use urine [133,134,135,136] or saliva [137,138,139] for testing can be adapted for similar use. The current boom in computing can also be exploited to greatly improve the sensitivity and specificity of testing by using smartphones for DIY image processing of the final result [66, 77]. The widespread availability and viability of smartphones allow for the development of specific applications geared towards testing socially relevant diseases [140]. Particularly important is their utility in eliminating subjectivity in the final results of an assay and their ability to directly parse electrical signals into readable data. Integrating cellulose-based devices into a smartphone-based testing regime can enable reusable and economical test sample collection which can be sourced individually for use.
Moreover, applying artificial intelligence (AI)-enabled technologies could not only increase the accuracy of the final diagnosis, but could also provide quick access to relevant medical records for future medical consultations [127]. This bridging between the digital and analog also spurs the development of personalized treatment for each patient which can be availed from anywhere around the world [141]. Testing capabilities can also be increased by incorporating multiple testing modalities on a single device, facilitating the creating of a veritable “one-stop shop” which can test numerous relevant biomarkers for multiple UTIs at the same time [110, 119, 142]. This personal testing method will favor quick and personal testing akin to pregnancy tests, which can significantly reduce the logistical hurdles individuals face in accessing testing for UTIs (Fig. 6).
Cellulose-based systems offer unique pathways towards multimodal detection of UTI infections and can supplement current diagnostic systems greatly. Nevertheless, it is prudent to note that cellulose-based diagnostic devices are also subject to complications inherent in UTI detection. Given the relatively rudimentary nature of the diagnostic devices, most of the devices discussed in the literature rely on the presence of pathogens in urine as a means of diagnosis. Detection in this manner has low diagnostic accuracy and clinical utility, as the data might change according to the stage of infection and can also often be conflated with results present in asymptomatic bacteriuria, which in most cases does not require intervention [60, 143, 144]. Another sizable part of the literature focuses on using conventional biomarkers such as urine nitrite and leukocyte esterase. These biomarkers have been shown to be effective in most clinical settings and can be used to diagnose UTIs in different stages of infection, but generally also have low sensitivity and specificity for predicting or differentiating UTIs [60, 144, 145]. Novel and more accurate biomarkers like interleukins [60] and lactoferrin [146] are yet to be explored in this medium. Additionally, complex detection methods such as spectrometry [147] are harder to port onto a cellulose-based medium. However, the absence of a biomarker that can be independently used to check for UTIs can be uniquely dealt with using multiplexed cellulose-based devices, as they can help significantly with the cost-effective testing of multiple biomarkers simultaneously.
In this review, we have highlighted the many developments in the field of cellulose-based substrate testing of UTIs and the utility they find in many clinical applications. Through review, one can see that the technology, although still in its infancy regarding commercial use, has tremendous potential as a medium to bridge the gap between the development of testing techniques in the lab and their introduction in the general market. Despite their many advantages, we envisage these testing methods not as a way to eclipse the use of standard testing but as a supplement to laboratory testing, offering multiple testing modalities for UTI diagnoses. These methods should command more attention, as they push the limit of what is considered feasible to achieve when leveraging low-cost materials towards high-level diagnostics and can pave the way towards many new exciting developments in the field of analytical devices.
References
Medina M, Castillo-Pino E. An introduction to the epidemiology and burden of urinary tract infections. Vol. 11, Therapeutic Advances in Urology. SAGE Publications Inc.; 2019.
de Vasconcelos-Pereira EF, Figueiró-Filho EA, de Oliveira VM, Fernandes ACO, Fé CSM de, Coelho LR, et al. Urinary tract infection in high risk pregnant women. Rev Patol Trop. 2013;42(1).
Al-Haddad AM. Urinary tract infection among pregnant women in Al-Mukalla district, Yemen. East Mediterr Heal J. 2005;11(3).
Parveen K, Momen A, Arzumath A, Begum, Begum M. Prevalence Of Urinary Tract Infection During Pregnancy. J Dhaka Natl Med Coll Hosp. 2012;17.
Tamalli M, Sangar B, Alghazal MA. Urinary tract infection during pregnancy at Al-khoms. Int J Med Med Sci. 2013;3:455–9.
Mcdermott S, Callaghan W, Szwejbka L, Mann H, Daguise V. Urinary Tract Infections During Pregnancy and Mental Retardation and Developmental Delay. Obstet Gynecol. 2000;96:113–9.
Stk S, Ranjan A. Prevalence of UTI among Pregnant Women and Its Complications in Newborns. Indian J Pharm Pract. 2018;10.
Amiri M, Lavasani Z, Norouzirad R, Najibpour R, Mohamadpour M, Amin, et al. Prevalence of Urinary Tract Infection Among Pregnant Women and its Complications in Their Newborns During the Birth in the Hospitals of Dezful City, Iran, 2012–2013. Iran Red Crescent Med J. 2015;17.
Obiora C, Dim C, Ezegwui H, Asimadu E, Okeudo C. Asymptomatic bacteriuria among pregnant women with sickle cell trait in Enugu, South Eastern Nigeria. Niger J Clin Pract. 2014;17:95–9.
Alemu A, Moges F, Anteneh Y, Tulu K, Kassu A, Anagaw B, et al. Bacterial profile and drug susceptibility pattern of urinary tract infection in pregnant women at University of Gondar Teaching Hospital, Northwest Ethiopia. BMC Res Notes. 2012;5:197.
Bongomin F, Gago S, Oladele R, Denning D. Global and Multi-National Prevalence of Fungal Diseases—Estimate Precision. J Fungi. 2017;3:57.
Fisher J, Sobel J, Kauffman C, Newman C. Candida Urinary Tract Infections--Treatment. Clin Infect Dis. 2011;52(Suppl 6):S457–66.
Gharanfoli A, Mahmoudi E, Torabizadeh R, Katiraee F, Faraji S. Isolation, characterization, and molecular identification of Candida species from urinary tract infections. Curr Med Mycol. 2019;5.
Sobel J, Fisher J, Kauffman C, Newman C. Candida Urinary Tract Infections--Epidemiology. Clin Infect Dis. 2011;52(Suppl 6):S433–6.
Hollenbach E. To treat or not to treat - Critically ill patients with candiduria. Mycoses. 2008;51(Suppl 2):12–24.
Heidemann J, Schmitz B, Kostev K. Association between antiseizure medication use and risk of urinary tract infection: A case–control study. Epilepsy Behav. 2021;115:107502.
Baldassarre J, Kaye D. Special Problems of Urinary Tract Infection in the Elderly. Med Clin North Am. 1991;75:375–90.
Raz R. Urinary tract infection in postmenopausal women. Korean J Urol. 2011;52(12):801–8.
Whiting P, Westwood M, Watt I, Cooper J. Kleijnen J. Rapid tests and urine sampling techniques for the diagnosis of systematic review. 2005;13:1–13.
Wilson ML, Gaido L. Laboratory Diagnosis of Urinary Tract Infections in Adult Patients. 2004;38(table 1).
Pels RJ, Bor DH, Woolhandler S, Himmelstein DU, Lawrence RS. Dipstick Urinalysis Screening of Asymptomatic Adults for Urinary Tract Disorders: II. Bacteriuria. JAMA. 1989;262(9):1220–4.
Ransohoff DF, Feinstein AR. Problems of Spectrum and Bias in Evaluating the Efficacy of Diagnostic Tests. N Engl J Med. 1978;299(17):926–30.
Hagay Z, Levy R, Miskin A, Milman D, Sharabi H, Insler V. Uriscreen, a rapid enzymatic urine screening test: useful predictor of significant bacteriuria in pregnancy. Obstet Gynecol. 1996;87(3):410–3.
Pezzlo M. of UTI by RM. Detection of Urinary Tract Infections by Rapid Method. 1988;1(2):268–80.
Murray PR, Smith TB, McKinney TC Jr. Clinical evaluation of three urine screening tests. J Clin Microbiol. 1987;25(3):467–70.
Pezzlo MT, Wetkowski MA, Peterson EM, de la Maza LM. Detection of bacteriuria and pyuria within two minutes. J Clin Microbiol. 1985;21(4):578–81.
Thore A, Anséhn S, Lundin A, Bergman S. Detection of bacteriuria by luciferase assay of adenosine triphosphate. J Clin Microbiol. 1975;1(1):1–8.
Thore A, Lundin A, Anséhn S. Firefly luciferase ATP assay as a screening method for bacteriuria. J Clin Microbiol. 1983;17(2):218–24.
Trofimchuk E, Hu Y, Nilghaz A, Hua MZ, Sun S, Lu X. Development of paper-based microfluidic device for the determination of nitrite in meat. Food Chem. 2020;316:126396.
Shrivas K, Monisha, Kant T, Karbhal I, Kurrey R, Sahu B, et al. Smartphone coupled with paper-based chemical sensor for on-site determination of iron(III) in environmental and biological samples. Anal Bioanal Chem. 2020;412(7):1573–83.
da Silva VAOP, de Freitas RC, de Oliveira PR, Moreira RC, Marcolino-Júnior LH, Bergamini MF, et al. Microfluidic paper-based device integrated with smartphone for point-of-use colorimetric monitoring of water quality index. Measurement. 2020;164:108085.
Mani NK, Prabhu A, Biswas SK, Chakraborty S. Fabricating Paper Based Devices Using Correction Pens. Sci Rep [Internet]. 2019 Dec 11 [cited 2019 Mar 17];9(1):1752. Available from: http://www.nature.com/articles/s41598-018-38308-6
Mani NK, Das SS, Dawn S, Chakraborty S. Electro-kinetically driven route for highly sensitive blood pathology on a paper-based device. Electrophoresis. 2020;41(7–8):615–20.
Mani NK, Rudiuk S, Baigl D. Spatially controlled DNA unzipping by microfluidic interface positioning on a molecule perpendicular to a multicomponent flow. Chem Commun [Internet]. 2013 Jul 4 [cited 2019 Mar 17];49(61):6858. Available from: http://xlink.rsc.org/?DOI=c3cc44016h
Tan W, Powles E, Zhang L, Shen W. Go with the capillary flow. Simple thread-based microfluidics. Sensors Actuators B Chem. 2021;334:129670.
Weng X, Kang Y, Guo Q, Peng B, Jiang H. Recent advances in thread-based microfluidics for diagnostic applications. Biosens Bioelectron [Internet]. 2019;132(January):171–85. Available from: https://doi.org/10.1016/j.bios.2019.03.009
Hua MZ, Lu X. Development of a Microfluidic Paper-Based Immunoassay for Rapid Detection of Allergic Protein in Foods. ACS Sensors. 2020;5(12):4048–56.
Ozer T, McMahon C, Henry CS. Advances in Paper-Based Analytical Devices. Annual Review of Analytical Chemistry. 2020.
Gutiérrez-Capitán M, Baldi A, Fernández-Sánchez C. Electrochemical Paper-Based Biosensor Devices for Rapid Detection of Biomarkers. Vol. 20, Sensors . 2020.
Y-Q LI, FENG L. Progress in Paper-based Colorimetric Sensor Array. Chinese J Anal Chem. 2020;48(11):1448–57.
Shih C-I, Chou Y-C, Chen H-Y, Chen K-H, Wang I-H, Yeh Y-C. Colorimetric and Fluorometric Paper-Based Assay for Cu2+ Detection Based on Green Synthesis of 2-Aminoterephthalic Acid-Derived Pigments. ACS Appl Bio Mater. 2020;3(4):2516–21.
Temirel M, Dabbagh SR, Tasoglu S. Hemp-Based Microfluidics. Vol. 12, Micromachines . 2021.
Singhal HR, Prabhu A, Giri Nandagopal MS, Dheivasigamani T, Mani NK. One-dollar microfluidic paper-based analytical devices: Do-It-Yourself approaches. Vol. 165, Microchemical Journal. Elsevier Inc.; 2021. p. 106126.
Shen L-L, Zhang G-R, Etzold BJM. Paper-Based Microfluidics for Electrochemical Applications. ChemElectroChem. 2020;7(1):10–30.
Chen C-A, Yeh W-S, Tsai T-T, Li Y-D, Chen C-F. Three-dimensional origami paper-based device for portable immunoassay applications. Lab Chip. 2019;19(4):598–607.
Agustini D, Bergamini MF, Marcolino-Junior LH. Low cost microfluidic device based on cotton threads for electroanalytical application. Lab Chip. 2016;16(2):345–52.
Akyazi T, Basabe-Desmonts L, Benito-Lopez F. Review on microfluidic paper-based analytical devices towards commercialisation. Anal Chim Acta [Internet]. 2018 Feb 25 [cited 2018 Apr 22];1001:1–17. Available from: http://linkinghub.elsevier.com/retrieve/pii/S000326701731262X
Dou M, Sanjay ST, Benhabib M, Xu F, Li XJ. Low-cost bioanalysis on paper-based and its hybrid microfluidic platforms. Talanta. 2015;145:43–54.
Zhang Y, Li T, Ren T, Fang D, He J. Hydrophobic/lipophobic barrier capable of confining aggressive liquids for paper-based assay. Colloids Surfaces A Physicochem Eng Asp. 2017;520:544–9.
Agustini D, Fedalto L, Bergamini MF, Marcolino-Junior LH. Microfluidic thread based electroanalytical system for green chromatographic separations. Lab Chip. 2018;18(4):670–8.
Gaines M, Gonzalez-Guerrero MJ, Uchida K, Gomez FA. A microfluidic glucose sensor incorporating a novel thread-based electrode system. Electrophoresis. 2018;39(16):2131–5.
Gaines RA, O’Hara M. Introduction: Shaw in Performance. Shaw. 2018;38(1):1–5.
Kabariya R, Ramani V. Exploration of Thread for their Possible use in Fabrication of Low Cost Diagnostic Microfluidic Device. Mater Sci Res India. 2018;15:179–84.
Ochiai LM, Agustini D, Figueiredo-Filho LCS, Banks CE, Marcolino-Junior LH, Bergamini MF. Electroanalytical thread-device for estriol determination using screen-printed carbon electrodes modified with carbon nanotubes. Sensors Actuators B Chem. 2017;241:978–84.
Yeo JC, Kenry, Lim CT. Emergence of microfluidic wearable technologies. Lab Chip. 2016;16(21):4082–90.
Burnham S, Hu J, Anany H, Brovko L, Deiss F, Derda R, et al. Towards rapid on-site phage-mediated detection of generic Escherichia coli in water using luminescent and visual readout. Anal Bioanal Chem 2014 40623 [Internet]. 2014 Jun 27 [cited 2021 Jul 15];406(23):5685–93. Available from: https://link.springer.com/article/10.1007/s00216-014-7985-3
Whitesides GM. The origins and the future of microfluidics. Nature [Internet]. 2006 Jul 26 [cited 2019 Apr 20];442(7101):368–73. Available from: http://www.nature.com/articles/nature05058
Whitesides GM, Stroock AD. Flexible methods for microfluidics. Phys Today. 2001;54(6):42.
Reches M, Mirica KA, Dasgupta R, Dickey MD, Butte MJ, Whitesides GM. Thread as a Matrix for Biomedical Assays. ACS Appl Mater Interfaces [Internet]. 2010 Jun 23 [cited 2020 Jul 10];2(6):1722–8. Available from: https://pubs.acs.org/doi/abs/10.1021/am1002266
Horváth J, Wullt B, Naber KG, Köves B. Biomarkers in urinary tract infections – which ones are suitable for diagnostics and follow-up? GMS Infect Dis. 2020;8:Doc24.
Noviana E, McCord C, Clark K, Jang I, Henry C. Electrochemical Paper-Based Devices: Sensing Approaches and Progress Toward Practical Applications. Lab Chip. 2019;20.
Morbioli GG, Mazzu-Nascimento T, Stockton AM, Carrilho E. Technical aspects and challenges of colorimetric detection with microfluidic paper-based analytical devices (μPADs)- A review. Vol. 970, Analytica Chimica Acta. Elsevier B.V.; 2017. p. 1–22.
Shafiee H, Asghar W, Inci F, Yuksekkaya M, Jahangir M, Zhang MH, et al. Paper and Flexible Substrates as Materials for Biosensing Platforms to Detect Multiple Biotargets. Sci Reports 2015 51 [Internet]. 2015 Mar 6 [cited 2021 Sep 2];5(1):1–9. Available from: https://www.nature.com/articles/srep08719
Chen C, Dong T. Microfluidic paper-based analytical devices for colorimetric detection of urinary tract infection biomarkers on adult diapers. Annu Int Conf IEEE Eng Med Biol Soc IEEE Eng Med Biol Soc Annu Int Conf. 2015;2015:5892–5.
Noiphung J, Laiwattanapaisal W. Multifunctional Paper-Based Analytical Device for In Situ Cultivation and Screening of Escherichia coli Infections. Sci Rep. 2019;9(1):1–10.
Ghaderinezhad F, Ceylan Koydemir H, Tseng D, Karinca D, Liang K, Ozcan A, et al. Sensing of electrolytes in urine using a miniaturized paper-based device. Sci Rep. 2020;10(1):13620.
Couto A, Dong T. Design of a microfluidic paper-based device for analysis of biomarkers from urine samples on diapers. Annu Int Conf IEEE Eng Med Biol Soc IEEE Eng Med Biol Soc Annu Int Conf. 2017;2017:181–4.
Yu Z, Lai RY. A reagentless and reusable electrochemical aptamer-based sensor for rapid detection of ampicillin in complex samples. Talanta. 2018;176:619–24.
Prabhu A, Nandagopal M. S. G, Peralam Yegneswaran P, Prabhu V, Verma U, Mani NK. Thread integrated smart-phone imaging facilitates early turning point colorimetric assay for microbes. RSC Adv [Internet]. 2020 Jul 13 [cited 2021 Jun 2];10(45):26853–61. Available from: https://pubs.rsc.org/en/content/articlehtml/2020/ra/d0ra05190j
Wang YC, Tsai YH, Shen CF, He MY, Fu YC, Sang CY, et al. Turntable paper-based device to detect Escherichia coli. Micromachines. 2021;12(2).
Bagheri Pebdeni A, Hosseini M. Fast and selective whole cell detection of Staphylococcus aureus bacteria in food samples by paper based colorimetric nanobiosensor using peroxidase-like catalytic activity of DNA-Au/Pt bimetallic nanoclusters. Microchem J. 2020;159:105475.
Prabhu A, Giri Nandagopal MS, Peralam Yegneswaran P, Singhal HR, Mani NK. Inkjet printing of paraffin on paper allowslow-costpoint-of-care diagnostics for pathogenic fungi. Cellulose. 2020;27(13):7691–701.
Sun Q, Tam NFY, Han J, Yung-Kang Peng W, Zhu Z, Chen JL. A simple paper-based colorimetric analytical device for rapid detection of Enterococcus faecalis under the stress of chlorophenols. Talanta. 2021;225:121966.
Wang C-H, Wu J-J, Lee G-B. Screening of highly-specific aptamers and their applications in paper-based microfluidic chips for rapid diagnosis of multiple bacteria. Sensors Actuators B Chem. 2019;284:395–402.
Shafiee H, Asghar W, Inci F, Yuksekkaya M, Jahangir M, Zhang MH, et al. Paper and flexible substrates as materials for biosensing platforms to detect multiple biotargets. Sci Rep. 2015;5(i):1–9.
Prabhu A, Singhal H, Giri Nandagopal MS, Kulal R, Peralam Yegneswaran P, Mani NK. Knitting Thread Devices: Detecting Candida albicans Using Napkins and Tampons . ACS Omega [Internet]. 2021 May 18 [cited 2021 Jun 2];6(19):12667–75. Available from: https://doi.org/10.1021/acsomega.1c00806
Cho S, Park TS, Nahapetian TG, Yoon JY. Smartphone-based, sensitive μPAD detection of urinary tract infection and gonorrhea. Biosens Bioelectron. 2015;74:601–11.
Choopara I, Suea-Ngam A, Teethaisong Y, Howes PD, Schmelcher M, Leelahavanichkul A, et al. Fluorometric Paper-Based, Loop-Mediated Isothermal Amplification Devices for Quantitative Point-of-Care Detection of Methicillin-ResistantStaphylococcus aureus (MRSA). ACS Sensors. 2021;6(3):742–51.
Seok Y, Joung HA, Byun JY, Jeon HS, Shin SJ, Kim S, et al. A paper-based device for performing loop-mediated isothermal amplification with real-time simultaneous detection of multiple DNA targets. Theranostics. 2017;7(8):2220–30.
Zuo P, Li X, Dominguez DC, Ye B-C. A PDMS/paper/glass hybrid microfluidic biochip integrated with aptamer-functionalized graphene oxide nano-biosensors for one-step multiplexed pathogen detection. Lab Chip. 2013;13(19):3921–8.
Cabot JM, Macdonald NP, Phung SC, Breadmore MC, Paull B. Fibre-based electrofluidics on low cost versatile 3D printed platforms for solute delivery, separations and diagnostics; from small molecules to intact cells. Analyst. 2016;141(23):6422–31.
Ho M-L, Liu W-F, Tseng H-Y, Yeh Y-T, Tseng W-T, Chou Y-Y, et al. Quantitative determination of leukocyte esterase with a paper-based device. RSC Adv. 2020;10(45):27042–9.
e Silva RF, Longo Cesar Paixão TR, Der Torossian Torres M, de Araujo WR. Simple and inexpensive electrochemical paper-based analytical device for sensitive detection of Pseudomonas aeruginosa. Sensors Actuators, B Chem. 2020;308.
Kunin CM, Buesching WJ. Novel screening method for urine cultures using a filter paper dilution system. J Clin Microbiol. 2000;38(3):1187–90.
Kaur T, Dahiya S, Satija SH, Nawal SJ, Kshetrimayum N, Ningthoujam J, et al. Foldscope as a primary diagnostic tool for oral and urinary tract infections and its effectiveness in oral health education. J Microsc. 2020;279(1):39–51.
Moczko E, Mirkes EM, Cáceres C, Gorban AN, Piletsky S. Fluorescence-based assay as a new screening tool for toxic chemicals. Sci Rep. 2016;6:33922.
Thom N, Lewis G, Yeung K, Phillips S. Quantitative Fluorescence Assays Using a Self-Powered Paper-Based Microfluidic Device and a Camera-Equipped Cellular Phone. RSC Adv. 2014;4:1334–40.
Nishi K, Isobe S, Zhu Y, Kiyama R. Fluorescence-Based Bioassays for the Detection and Evaluation of Food Materials. Sensors (Basel). 2015;15:25831–67.
Dungchai W, Chailapakul O, Henry CS. Electrochemical Detection for Paper-Based Microfluidics. Anal Chem. 2009;81(14):5821–6.
Adkins J, Boehle K, Henry C. Electrochemical paper-based microfluidic devices. Vol. 36, Electrophoresis. Wiley-VCH Verlag; 2015. p. 1811–24.
Rozenblum G, Pollitzer R. Challenges in Electrochemical Aptasensors and Current Sensing Architectures Using Flat Gold Surfaces. Chemosensors. 2019;7:57.
Nilghaz A, Ballerini DR, Guan L, Li L, Shen W. Red blood cell transport mechanisms in polyester thread-based blood typing devices. Anal Bioanal Chem. 2016;408(5):1365–71.
O’Farrell B. Evolution in Lateral Flow–Based Immunoassay Systems. Wong R, Tse H, editors. Lateral Flow Immunoass. 2008;1–33.
First response [Internet]. Available from: https://www.firstresponse.com/
Clearblue [Internet]. Available from: https://www.clearblue.com/pregnancy-tests
MOLOGIC [Internet]. Available from: https://mologic.co.uk/
AZO Test Strips [Internet]. Available from: https://www.azoproducts.com/products/uti-medications/azo-test-strips
Nurse Hatty [Internet]. Available from: https://nursehatty.com/
Sawyer KP, Stone LL. Evaluation of a leukocyte dip-stick test used for screening urine cultures. J Clin Microbiol. 1984;20(4):820–1.
Lammers RL, Gibson S, Kovacs D, Sears W, Strachan G. Comparison of test characteristics of urine dipstick and urinalysis at various test cutoff points. Ann Emerg Med. 2001;38(5):505–12.
Semeniuk H, Church D. Evaluation of the leukocyte esterase and nitrite urine dipstick screening tests for detection of bacteriuria in women with suspected uncomplicated urinary tract infections. J Clin Microbiol. 1999;37(9):3051–2.
Mimoz O, Bouchet E, Edouard A, Costa Y, Samii K. Limited usefulness of urinary dipsticks to screen out catheter-associated bacteriuria in ICU patients. Anaesth Intensive Care. 1995;23(6):706–7.
Masinde A, Gumodoka B, Kilonzo A, Mshana SE. Prevalence of urinary tract infection among pregnant women at Bugando Medical Centre, Mwanza. Tanzania. Tanzan J Health Res. 2009;11(3):154–9.
Corstjens PLAM, Nyakundi RK, de Dood CJ, Kariuki TM, Ochola EA, Karanja DMS, et al. Improved sensitivity of the urine CAA lateral-flow assay for diagnosing active Schistosoma infections by using larger sample volumes. Parasit Vectors. 2015;8(1):241.
Stapleton AE, Cox ME, DiNello RK, Geisberg M, Abbott A, Roberts PL, et al. Performance of a New Rapid Immunoassay Test Kit for Point-of-Care Diagnosis of Significant Bacteriuria. J Clin Microbiol. 2015;53(9):2805–9.
Nakamura A, Kohno A, Noguchi N, Kawa K, Ohno Y, Komatsu M, et al. Prediction of Uropathogens by Flow Cytometry and Dip-stick Test Results of Urine Through Multivariable Logistic Regression Analysis. PLoS One. 2020;15(1):e0227257.
Dip UTI.
Baral R, Nepal SK. Rapid Nitrite Dip Stick Vs Urine culture for diagnosis of Urinary tract Infections (UTI): Laboratory prospective. Int J Biomed Res. 2017;8(4):204–9.
Marx V. Putting microfluidics in other people’s hands. Nat Methods. 2018;15(3):167–70.
Sharma S, Zapatero-Rodríguez J, Estrela P, O’Kennedy R. Point-of-Care diagnostics in low resource settings: Present status and future role of microfluidics. Vol. 5, Biosensors. MDPI AG; 2015. p. 577–601.
Martinez AW, Phillips ST, Butte MJ, Whitesides GM. Patterned paper as a platform for inexpensive, low-volume, portable bioassays. Angew Chemie - Int Ed. 2007;46(8):1318–20.
Essays RG-SR and, 2010 undefined. Examining the effects of mercerization process applied under different conditions to dimensional stability. academicjournals.org.
Modibbo UU, Aliyu BA, Nkafamiya II. The effect of mercerization media on the physical properties of local plant bast fibres From the forgoing. Vol. 4, International Journal of Physical Sciences. Academic Journals; 2009.
Nilghaz A, Ballerini DR, Shen W. Exploration of microfluidic devices based on multi-filament threads and textiles: A review. Biomicrofluidics. 2013;7(5):051501.
Okano T, Sarko A. Mercerization of cellulose. II. Alkali–cellulose intermediates and a possible mercerization mechanism. J Appl Polym Sci. 1985;30(1):325–32.
Yetisen AK, Akram MS, Lowe CR. Paper-based microfluidic point-of-care diagnostic devices. Lab Chip [Internet]. 2013 May 21 [cited 2019 Aug 26];13(12):2210. Available from: http://xlink.rsc.org/?DOI=c3lc50169h
Martinez AW, Phillips ST, Whitesides GM, Carrilho E. Diagnostics for the Developing World: Microfluidic Paper-Based Analytical Devices. Anal Chem [Internet]. 2010 Jan [cited 2018 Apr 22];82(1):3–10. Available from: http://pubs.acs.org/doi/abs/10.1021/ac9013989
Urdea M, Penny LA, Olmsted SS, Giovanni MY, Kaspar P, Shepherd A, et al. Requirements for high impact diagnostics in the developing world. Nature. 2006;444(Suppl):73–9.
Carrell C, Kava A, Nguyen M, Menger R, Munshi Z, Call Z, et al. Beyond the lateral flow assay: A review of paper-based microfluidics. Microelectron Eng. 2019;206(December 2018):45–54.
Ravindran S. How DIY technologies are democratizing science. Vol. 587, Nature. NLM (Medline); 2020. p. 509–11.
Whitesides G. The frugal way. 2012.
Li Z, Liu H, He X, Xu F, Li F. Pen-on-paper strategies for point-of-care testing of human health. Vol. 108, TrAC - Trends in Analytical Chemistry. Elsevier B.V.; 2018. p. 50–64.
Dornelas KL, Dossi N, Piccin E. A simple method for patterning poly(dimethylsiloxane) barriers in paper using contact-printing with low-cost rubber stamps. Anal Chim Acta [Internet]. 2015;858(1):82–90. Available from:. https://doi.org/10.1016/j.aca.2014.11.025.
Hasandka A, Prabhu A, Prabhu A, Singhal HR, Nandagopal MSG, Shenoy R, et al. “Scratch it out”: carbon copy based paper devices for microbial assays and liver disease diagnosis. Anal Methods. 2021;13(28):3172–80.
Oyola-Reynoso S, Heim AP, Halbertsma-Black J, Zhao C, Tevis ID, Çinar S, et al. Draw your assay: Fabrication of low-cost paper-based diagnostic and multi-well test zones by drawing on a paper. Talanta. 2015;144:289–93.
Sustainable Development Goals | UNDP.
Mejía-Salazar JR, Cruz KR, Vásques EMM, de Oliveira ON. Microfluidic point-of-care devices: New trends and future prospects for ehealth diagnostics. Sensors (Switzerland). 2020;20(7).
Xu K, Lu Y, Takei K. Flexible Hybrid Sensor Systems with Feedback Functions. Advanced Functional Materials. Wiley-VCH Verlag; 2020. p. 2007436.
Pandey M, Shahare K, Srivastava M, Bhattacharya S. Paper-Based Devices for Wearable Diagnostic Applications. In Springer, Singapore; 2019. p. 193–208.
Liu L, Yang D, Liu G. Signal amplification strategies for paper-based analytical devices. Biosens Bioelectron. 2019;136(March):60–75.
Chen C, … TD-37th AIC of the 2015 undefined. Microfluidic paper-based analytical devices for colorimetric detection of urinary tract infection biomarkers on adult diapers. ieeexplore.ieee.org.
Chen C, Wu Y, Dong T. Dipsticks integrated on smart diapers for colorimetric analysis of urinary tract infections in the field. ieeexplore.ieee.org.
Couto A, … TD-39th AIC of the 2017 undefined. Design of a microfluidic paper-based device for analysis of biomarkers from urine samples on diapers. ieeexplore.ieee.org.
Zhang J, Liu J, Su H, Sun F, Lu Z, B AS-S and A, et al. A wearable self-powered biosensor system integrated with diaper for detecting the urine glucose of diabetic patients. Elsevier.
Zhao J, Nyein HYY, Hou L, Lin Y, Bariya M, Ahn CH, et al. A Wearable Nutrition Tracker. Adv Mater. 2021;33(1).
Carreiro S, Smelson D, Ranney M, Horvath KJ, Picard RW, Boudreaux ED, et al. Real-Time Mobile Detection of Drug Use with Wearable Biosensors: A Pilot Study. Springer.
de Castro LF, de Freitas SV, Duarte LC, de Souza JAC, Paixão TRLC, Coltro WKT. Salivary diagnostics on paper microfluidic devices and their use as wearable sensors for glucose monitoring. Anal Bioanal Chem. 2019;411(19):4919–28.
Salehipour Masooleh H, Ghavami-Lahiji M, Ciancio A, Tayebi L. Microfluidic Technologies Using Oral Factors: Saliva-Based Studies. In: Applications of Biomedical Engineering in Dentistry. Springer International Publishing; 2020. p. 339–58.
Kim J, Imani S, Araujo W de, … JW-B and, 2015 undefined. Wearable salivary uric acid mouthguard biosensor with integrated wireless electronics. Elsevier.
Xu X, Akay A, Wei H, Wang S, Pingguan-Murphy B, Erlandsson BE, et al. Advances in Smartphone-BasedPoint-of-Care Diagnostics. Proc IEEE. 2015;103(2):236–47.
Rivet C, Lee H, Hirsch A, Hamilton S, Lu H. Microfluidics for medical diagnostics and biosensors. Chem Eng Sci. 2011;66(7):1490–507.
Cui P, Wang S. Application of microfluidic chip technology in pharmaceutical analysis: A review. J Pharm Anal. 2019;9(4):238–47.
Colgan R, Nicolle LE, McGlone A, Hooton TM. Asymptomatic Bacteriuria in Adults. Am Fam Physician. 2006;74(6):985–90.
Averbeck MA, Rantell A, Ford A, Kirschner-Hermanns R, Khullar V, Wagg A, et al. Current controversies in urinary tract infections: ICI-RS 2017. Neurourol Urodyn. 2018;37:S86–92.
Kupelian AS, Horsley H, Khasriya R, Amussah RT, Badiani R, Courtney AM, et al. Discrediting microscopic pyuria and leucocyte esterase as diagnostic surrogates for infection in patients with lower urinary tract symptoms: Results from a clinical and laboratory evaluation. BJU Int. 2013;112(2):231–8.
Arao S, Matsuura S, Nonomura M, Miki K, Kabasawa K, Nakanishi H. Measurement of urinary lactoferrin as a marker of urinary tract infection. J Clin Microbiol. 1999;37(3):553–7.
Lussu M, Camboni T, Piras C, Serra C, Del Carratore F, Griffin J, et al. 1H NMR spectroscopy-based metabolomics analysis for the diagnosis of symptomatic E. coli-associated urinary tract infection (UTI). BMC Microbiol. 2017;17(1).
Acknowledgements
The work was partially funded by Manipal-McGill Center for Infectious Diseases [Seed Grant Award Number: MAC ID/SGA/2017/21]. NKM and AP acknowledge the financial support from the Vision Group on Science and Technology, Government of Karnataka, under SMYSR and RGS/F Scheme [Sanction Letter no.: KSTePS/VGST/SMYSR-2016–17/GRD-595/2017–18, KSTePS/VGSTRGS/F/GRD No.711/2017–18]. AP acknowledges the Indian Council of Medical Research (ICMR) for providing a Senior Research Fellowship [File no: 5/3/8/91/ITR-F/2020]. NKM acknowledges the financial support received from the Science and Engineering Research Board (SERB), Department of Science and Technology, Govt of India, under Core Research Grant (CRG) Scheme (File number CRG/2020/003060). We extend our special thanks to the Department of Biotechnology, Manipal Institute of Technology. GN acknowledges the Science and Engineering Research Board (SERB), Department of Science and Technology, Govt of India, for a National Post-Doctoral Fellowship [Sanction No.: PDF/2018/001486]. NKM acknowledges Dr. Praveen Kumar, Dr. Vijendra Prabhu, and Dr. Peralam Prakash for their fruitful discussions.
Funding
Open access funding provided by Manipal Academy of Higher Education, Manipal.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hasandka, A., Singh, A.R., Prabhu, A. et al. Paper and thread as media for the frugal detection of urinary tract infections (UTIs). Anal Bioanal Chem 414, 847–865 (2022). https://doi.org/10.1007/s00216-021-03671-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00216-021-03671-3