Abstract
Rationale
Corticotropin-releasing factor (CRF), the apical stress-inducing hormone, exacerbates stress and addictive behaviors. TCAP-1 is a peptide that directly inhibits both CRF-mediated stress and addiction-related behaviors; however, the direct action of TCAP-1 on morphine withdrawal-associated behaviors has not previously been examined.
Objective
To determine whether TCAP-1 administration attenuates behavioral and physiological consequences of morphine withdrawal in mice.
Methods
Mice were administered via subcutaneous route TCAP-1 either before or after initial morphine exposure, after which jumping behavior was quantified to assess the effects of TCAP-1 on naloxone-precipitated morphine withdrawal. As a comparison, mice were treated with nonpeptide CRF1 receptor antagonist CP-154,526. In one experiment, plasma corticosterone (CORT) was also measured as a physiological stress indicator.
Results
Pretreatment with TCAP-1 (10–250 nmol/kg) before morphine treatment significantly inhibited the development of naloxone-precipitated withdrawal. TCAP-1 (250–500 nmol/kg) treatment administered after morphine treatment attenuated the behavioral expression of naloxone-precipitated withdrawal. TCAP-1 (250 nmol/kg) treatment during morphine treatment was more effective than the optimal dosing of CP-154,526 (20 mg/kg) at suppressing the behavioral expression of naloxone-precipitated withdrawal, despite similar reduction of withdrawal-induced plasma CORT level increases.
Conclusions
These findings establish TCAP-1 as a potential therapeutic candidate for the prevention and treatment of morphine withdrawal.
Similar content being viewed by others

Introduction
Although opioids such as hydrocodone, oxycodone, and tramadol are extremely effective analgesics, their over-prescription fueled the rise of a large drug abuse epidemic due to the rewarding properties they also possess (Meldrum 2020; National Academies of Sciences et al., 2017). Due to public health initiatives, opioid prescription for pain management has been moderated in recent years (Alsultan and Guo 2022; Ball et al. 2021; Dowell et al. 2016; Flanagan et al. 2020), accompanied by a corresponding drop in prescription opioid overdose deaths (NIDA 2023). However, a non-prescription opioid epidemic continues in its wake, with synthetic opioid use now coming to the forefront (Friedman et al. 2022; NIDA 2023). One well-established consequence of opioid use is dependence, which includes a reluctance to discontinue opioids and the presentation of withdrawal symptoms when opioid use is halted. The magnitude of opioid withdrawal typically correlates with the duration and degree of opioid exposure, lasting for days or weeks in long-term heavy opioid users (Dydyk et al. 2023; WHO 2009). However, even short-term opioid exposure can result in acute, albeit less severe, withdrawal, that may nonetheless be sufficient to motivate subsequent use (Abdelhamid et al. 1991; Elhabazi et al. 2012; Gold et al. 1994; Heishman et al. 1989; Kest et al. 2001; Seth et al. 2011; Wilson et al. 2021; Yano and Takemori 1977). In rodents (Kamei et al. 1973; Kest et al. 2001, 2002) and humans (Bickel et al. 1988; Jones et al. 2020), withdrawal from opioids can be precipitated by administration of the opioid antagonist, naloxone. A behavioral hallmark of naloxone-precipitated opioid withdrawal in rodents is the induction of jumping behavior (Kamei et al. 1973; Kest et al. 2001, 2002; Singh et al. 2015; Wei et al. 2023).
Endogenous opioids like endorphins, dynorphins, and enkephalins act as part of the CRF-associated stressor response (Houshyar et al. 2003). Briefly, following a stressful sensory input, an increase in hypothalamic CRF initiates the hypothalamus-pituitary-adrenal (HPA) response, a cascade of events eventually resulting in the release of glucocorticoids from the adrenal cortex. One such glucocorticoid is corticosterone (CORT) in rodents, or cortisol in humans, a mediator of both behavioral and physiological stress responses (Vale et al. 1981). Withdrawal from drugs of abuse increases CRF levels both within the hypothalamus and other brain regions (Buckingham 1982; Funk et al. 2006; George et al. 2007; Merlo Pich et al. 1995; Richter and Weiss 1999; Roberto et al. 2010; Weiss et al. 2001; Zorrilla et al. 2001), indicating that withdrawal is a stressful experience. Accordingly, pre-treatment with CRF receptor antagonists reduce behavioral manifestations of withdrawal (Brugger et al. 1998; Funada et al. 2001; Iredale et al. 2000; Lu et al. 2000; McNally and Akil 2002; Skelton et al. 2007) and CRF1 receptor knockout mice demonstrate reduced withdrawal-associated behaviors (Contarino and Papaleo 2005). Together, these findings suggest a role for CRF in mediating withdrawal from drugs of abuse.
Teneurin C-terminal Associated Peptide (TCAP)-1 has been identified as a stress response regulator, likely acting through an HPA-independent CRF-related mechanism (Al Chawaf et al. 2007; Chen et al. 2013; Tan et al. 2009; Wang et al. 2005). In situ hybridization studies showed that TCAP-1 mRNA is highly expressed in brain regions that express CRF receptors and are important for the regulation of stress, such as the hypothalamus, cerebellum, and limbic system (Chen et al. 2013; Wang et al. 2005). Administration of TCAP-1 before CRF decreased CRF-induced c-Fos expression in these regions (Tan et al. 2009), suggesting that TCAP-1 blocks stress-related CRF activity. Using two behavioral assays commonly employed to study anxiolytics, administration of TCAP-1 attenuated the CRF-associated acoustic startle response and increased time spent in the open arm on an elevated plus-maze (Tan et al. 2011; Wang et al. 2005). More relevant to the present study, TCAP-1 has been directly implicated in aspects of substance use disorder (SUD), with repeated treatment attenuating both CRF-induced reinstatement of cocaine seeking and cocaine-sensitized CRF-induced locomotion (Kupferschmidt et al. 2011). These studies establish that TCAP-1 inhibits both CRF stress and addiction-related behaviors, but these attenuating effects on behavior associated with cocaine – a psychostimulant – may not necessarily generalize to other classes of psychoactive drugs, such as opioids. However, because the opioid-associated neurological circuit encompasses both stress- and addiction-related behaviors (Crowley and Kash 2015; Haun et al. 2022; Leconte et al. 2022; Rysztak and Jutkiewicz 2022; Simmons et al. 2020; Tkaczynski et al. 2022; Zhang et al. 2022), and because opioid cessation results in withdrawal which is itself as stressor, it is possible that TCAP-1 could have utility in facilitating opioid abstinence.
Therefore, the effects of TCAP-1 on the behavioral actions of morphine withdrawal were examined, together with a pharmacological comparison of the behavioral and physiological effects of TCAP-1 and nonpeptide CRF1 receptor antagonist CP-154,526. First, a naloxone-precipitated morphine withdrawal assay was utilized (Kamei et al. 1973; Kest et al. 2002; Tanganelli et al. 1991), to examine whether administration of TCAP-1 either before or after morphine treatment influenced withdrawal-related jumping behavior. Using a similar design, the efficacy of TCAP-1 and CP-154,526 were compared in attenuating the naloxone-induced jumping response and CORT level increase in morphine-treated mice.
Methods
Drugs
Naloxone hydrochloride dihydrate and CP-154,526 [N-butyl-N-ethyl-2,5-dimethyl-7-(2,4,6-trimethylphenyl)pyrrolo[3,2-e]pyrimidin-4-amine] hydrochloride was purchased from Sigma (St. Louis, MO). Morphine sulfate was purchased from Spectrum Chemical (New Brunswick, NJ). Synthetic mouse TCAP-1 (TCAP-1) was synthesized and purchased from Chinese Peptide Company, Incorporated (Hangzhou, China). (+)-MK-801 was obtained through Tocris Bioscience (Bristol, UK). Naloxone and MK-801 were dissolved in 0.9% sterile saline. Morphine hydrochloride was first dissolved in distilled water and then diluted using saline. TCAP-1 was first suspended in distilled water with ammonium hydroxide and vortexed and further diluted using saline. CP-154,526 was dissolved in 10% DMSO and 10% Cremophor EL in saline. Drug doses are expressed in terms of their salt form. Naloxone (2.5 and 10 mg/kg), morphine (32 mg/kg), and MK-801 (0.5 mg/kg) were administered i.p., while TCAP-1 (10–500 nmol/kg) and CP-154,526 (5–50 mg/kg) were given subcutaneously (s.c.).
Animals
Male Swiss Webster mice (Charles River Laboratories, Kingston, NY) six weeks of age and weighing 20–30 g at experiment onset were group housed on a 12/12-hour light/dark cycle with behavior conducted during the light period. Mice had free access to water and food, except during behavioral test sessions. All housing and experimental conditions complied with Institutional Animal Care and Use Committee guidelines of NeoSome Life Sciences, LLC (Lexington, MA). The number of animals used for each experiment is given in the corresponding figure legend.
Experimental design
Three studies were conducted to evaluate the effects of TCAP-1 on naloxone-precipitated jumping behavior in morphine-treated mice and the accompanying physiological stress response. First, a dose-range finding study was conducted to establish optimal doses of TCAP-1 to attenuate naloxone-precipitated jumping behavior when TCAP-1 was given prophylactically prior to morphine treatment. Next, the ability of TCAP-1 to attenuate naloxone-precipitated jumping behavior as an intervention was evaluated, after morphine treatment had already commenced. Finally, the ability of TCAP-1 to attenuate both jumping behavior and decrease physiological stress response as reflected by plasma corticosterone concentration was assessed along with a small molecule CRF1 receptor antagonist CP-154,526.
Naloxone-precipitated morphine withdrawal test
Seven intraperitoneal (i.p.) injections of morphine (32 mg/kg) were spread across two days, with the first three injections occurring in one-hour intervals and the last two injections occurring in two-hour intervals on the first day, and a two-hour interval on the second day. Two hours following the last injection of morphine, mice received one i.p. injection of naloxone (2.5 or 10 mg/kg) and were placed into individual Plexiglas observation cylinders (20 cm H x 12 cm W) where behavior was captured for 20 min. In some experiments, an additional control group of mice were treated with saline instead of morphine and treated with naloxone prior to the observation period (groups denoted ‘S’ in figures). Multiple blinded, independent scorers quantified the number of jumps, defined as the simultaneous removal of all paws, made by each mouse. In the experiment related to Fig. 1, TCAP-1 was administered at doses of 10–250 nmol/kg, and three daily injections were given one day prior to the initiation of morphine. In the experiment related to Fig. 2, TCAP-1 was administered at doses of 250 or 500 nmol/kg one hour following the last morphine injection. In the experiment related to Fig. 3, TCAP-1 was administered at a dose of 250 nmol/kg and CP-154,526 was administered at doses of 5–50 mg/kg; these treatments were administered one hour before and one hour after the last morphine injection.
Effects of TCAP-1 pretreatment on naloxone-precipitated morphine withdrawal. a Experimental procedure of drug treatment and behavioral measurement. TCAP-1 (10–250 nmol/kg, s.c.) was administered daily for three days prior to morphine treatment. Naloxone (10 mg/kg, i.p.) was administered to induce a behavioral manifestation of withdrawal after the morphine treatment regimen. MK-801 (0.5 mg/kg, i.p.) was administered 30 min prior to naloxone treatment. b Number of jumps during a 20 min period after naloxone injection. Data are represented as mean \(\pm\) SEM. S = saline, n = 9; V = vehicle, n = 9; 10–250 nmol/kg TCAP-1, n = 9 for each group; MK = MK-801, n = 4. *** P < 0.001; ** p < 0.01
Effects of TCAP-1 treatment post morphine on naloxone-precipitated withdrawal. a Experimental procedure of drug treatment and behavioral measurement. TCAP-1 (250–500 nmol/kg, s.c.) was administered once after morphine. Naloxone (10 mg/kg, i.p.) was administered to induce a behavioral manifestation of withdrawal after the morphine treatment regimen. b Number of jumps during a 20 min period after naloxone injection. Data are represented as mean \(\pm\) SEM. S = saline, n = 7; V = vehicle, n = 5; 250 nmol/kg TCAP-1, n = 6; 500 nmol/kg TCAP-1, n = 7. **** P < 0.0001; ** p < 0.01
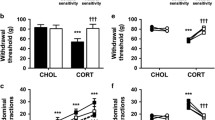
Effects of TCAP-1 or CP-154,526 administration at the end of morphine treatment on naloxone-precipitated withdrawal and plasma corticosterone levels. a Experimental procedure of drug treatment and behavioral measurement. TCAP-1 (250 nmol/kg, s.c.) or a dose range of CP-154,526 (5–50 mg/kg, s.c.) was administered in an interleaved fashion one hour before and after the last morphine treatment. Naloxone (2.5 mg/kg, i.p.) was administered to induce a behavioral manifestation of morphine withdrawal. b Number of jumps during a 20 min period after naloxone injection. V = vehicle, n = 11; 5 and 50 mg/kg CP-154,526, n = 11 for each group; 20 mg/kg CP-154,526, n = 12; T = 250 nmol/kg TCAP-1, n = 12. c Plasma corticosterone levels measured from blood taken immediately after jumping. V = vehicle, n = 6; 5–20 mg/kg CP-154,526, n = 6; 50 mg/kg CP-154,526, n = 9; T = 250 nmol/kg TCAP-1, n = 6. d Comparison of the number of jumps during a 20 min period after naloxone injection between an optimal dose of CP-154,526 and TCAP-1. S = saline, n = 4; V = vehicle, n = 12; CP-154,526 = 20 mg/kg, n = 8; T = 250 nmol/kg TCAP-1, n = 12. All data are expressed as mean \(\pm\) SEM. *** P < 0.001; ** p < 0.01
Plasma corticosterone assessment
In the experiment related to Fig. 3b, immediately following behavioral sessions, 0.15–0.3 mL of blood was collected and used to detect plasma CORT levels. Briefly, using a 5 mm lancet to prick the submandibular vein, blood was collected into heparin separator mini collect tubes (Greiner Bio-One, Monroe, North Carolina) and placed on ice. Samples were then spun in a refrigerated microcentrifuge at 2,000 x g for eight minutes, after which plasma was extracted. Finally, plasma CORT levels were quantified using a rodent CORT enzyme-linked immunosorbent assay (ELISA, Cayman Chemical Company, Ann Arbor, MI). The process was executed as per the manufacturer’s instruction, with absorbance measured at 420 nm using a microplate reader (Molecular Devices, San Jose, CA).
Data analysis
All statistical analyses and graphs were performed using Prism 9 (GraphPad Software, San Diego, CA). Values are expressed as mean ± SEM. Statistics were performed on behavioral and ELISA data using one-way analysis of variance (ANOVA) with follow-up Tukey’s tests for multiple comparisons to determine significance. An a priori level of significance of p < 0.05 was considered significant in these studies.
Results
Pretreatment with TCAP-1 attenuates the development of morphine withdrawal
Mice were treated daily with either TCAP-1 across a broad dose range (10–250 nmol/kg) or the control vehicle for three days. On the next day, mice began a morphine treatment assay, receiving a total of seven treatments over days four and five of the paradigm. One group of control mice that did not receive TCAP-1 were given saline injections in place of morphine. Naloxone was administered two hours after the last morphine or saline injection and jumping behavior was quantified immediately after (Fig. 1a). To validate our assay with a positive treatment control group, we included mice treated with MK-801, an N-methyl-D-aspartate (NMDA) receptor antagonist known to reduce the behavioral manifestation of precipitated withdrawal, 30 min prior to naloxone treatment (Cappendijk et al. 1993; Higgins et al. 1992; Koyuncuoğlu et al. 1992; Rasmussen et al. 1991; Trujillo and Akil 1991). There was a significant effect of treatment across groups on morphine-induced jumping behavior (one-way ANOVA, F7, 59 = 5.404, p < 0.0001, Fig. 1b). These data indicated that, first, the number of jumps in morphine-treated mice was significantly increased compared to saline-treated mice (‘S’ vs. ‘V’, p = 0.0001; Tukey’s Test). In contrast, the number of jumps in morphine-treated mice with 250 nmol/kg TCAP-1 treatment was significantly decreased by 78.4% as compared to morphine-treated mice with no TCAP-1 treatment (‘V’ vs. ‘250’, p = 0.0045; Tukey’s Test). Finally, as expected, MK-801 completely abolished naloxone-precipitated jumping (‘V’ vs. ‘MK’, p = 0.004; Tukey’s Test), supporting the validity of the experimental and scoring protocols. Altogether, these results show that TCAP-1 treatment prior to morphine treatment attenuated the development of naloxone-precipitated jumping.
Administration of TCAP-1 following morphine treatment attenuates the behavior of the expression of morphine withdrawal
Using the same morphine treatment regimen as the previous experiment, mice were first treated with morphine or saline over two days. One hour following the last injection, mice received one treatment of TCAP-1 or vehicle as the control. Naloxone was administered one hour later, and jumping was quantified (Fig. 2a). There was a significant treatment effect (one-way ANOVA, F3, 21 = 17.34, p < 0.0001, Fig. 2b). The number of jumps in morphine-treated mice was significantly increased compared to saline-treated mice (‘S’ vs. ‘V’, p < 0.0001; Tukey’s Test). Moreover, the number of jumps in morphine-treated mice with 500 nmol/kg TCAP-1 treatment was significantly decreased by 57.5% as compared to morphine-treated mice with no TCAP-1 treatment (‘V’ vs. ‘500’, p = 0.0058; Tukey’s Test). These results show that a single administration of TCAP-1 post morphine treatment attenuated the behavioral expression of naloxone-precipitated morphine withdrawal.
Comparison of the effects of TCAP-1 and CP-154,526 in attenuating the behavioral and physiological expression of morphine withdrawal
We next compared the efficacy of TCAP-1 with a dose range of nonpeptide corticotropin-releasing factor receptor 1 (CRF1) antagonist CP-154,526, an agent known to reduce behavioral (Lu et al. 2000) and physiological effects of morphine withdrawal (Navarro-Zaragoza et al. 2021). For this modified treatment design, all mice were treated with morphine over two days, with either TCAP-1 (250 nmol/kg), CP-154,526 (5–50 mg/kg), or vehicle being administered one hour before and one hour after the last morphine injection, to ensure that test compound remained on board before the naloxone-precipitated withdrawal test commenced. Naloxone was administered one hour after the last injection of TCAP-1, CP-154,526, or vehicle, jumping was recorded for 20 min, and blood was collected to measure plasma levels of CORT (Fig. 3a).
There was no significant effect of treatment on naloxone-precipitated jumping, due in part to the biphasic, U-shaped dose-effect produced by CP-154,526 (one-way ANOVA, F4,52 = 1.745, p = 0.1542, Fig. 3b). Sampled blood was used to measure CORT plasma levels as a biomarker for stress. Unlike the lack of effect observed on behavior, there was a significant treatment effect on CORT plasma levels (one-way ANOVA, F4,28 = 7.993, p = 0.0002, Fig. 3c). CORT levels in morphine-treated mice with either CP-154,526 (50 mg/kg) or TCAP-1 (250 nmol/kg) treatment were significantly lower by 71.0% and 64.9%, respectively, compared to morphine controls (‘V’ vs. ‘50’, p = 0.0008; ‘V’ vs. ‘T’, p = 0.0058; Tukey’s Test). Second, concentrations in morphine-treated mice with CP-154,526 (50 mg/kg) treatment were not significantly different from those treated with TCAP-1 (250 nmol/kg; ’CP 50 mg/kg’ vs. ‘T’, p = 0.9947; Tukey’s Test), despite the behavioral discrepancy between these treatments noted above.
Though treatments in this cohort did not elicit significant behavioral differences, which was not surprising due to known biphasic curves of CRF1 receptor antagonists (Millan et al. 2001; Vasconcelos et al. 2019; Walker et al. 2009a, b), it did establish 20 mg/kg as an optimal dose at which to test the inhibitory effects of CP-154,526 on naloxone-precipitated jumping. Using this established optimal dose of the antagonist we ran a second cohort using the same experimental design to directly compare 20 mg/kg CP-154,526 and 250 nmol/kg TCAP-1 (Fig. 3a). There was a significant effect of treatment on naloxone-precipitated jumping (one-way ANOVA, F3,32 = 9.587, p = 0.0001, Fig. 3d). The number of jumps in morphine-treated mice was significantly increased compared to saline-treated mice (‘S’ vs. ‘V’, p = 0.001; Tukey’s Test). Further, while the number of jumps in morphine-treated mice with 250 nmol/kg TCAP-1 treatment was significantly decreased by 75.1% as compared to morphine-treated mice with no treatment (‘V’ vs. ‘T’, p = 0.0005; Tukey’s Test), mice administered with 20 mg/kg CP-154,526 did not demonstrate a significant decrease in jumping behavior compared to controls (‘V’ vs. ‘CP’, p = 0.2813; Tukey’s Test). Taken together, these results suggest that TCAP-1 appears to better inhibit the behavioral and physiological expression of naloxone-precipitate morphine withdrawal than CP-154,526.
Discussion
For the first time the effects of TCAP-1 were investigated on both development and expression of the behavioral manifestation of naloxone-precipitated morphine withdrawal. As demonstrated in previous studies, a single naloxone injection reliably increased jumping behavior in morphine-treated mice. Administration of TCAP-1 either before or after initial morphine treatment attenuated naloxone-induced jumping, indicating the suppression of morphine withdrawal by TCAP-1. Comparison of TCAP-1 with the nonpeptide CRF1 receptor antagonist CP-154,526, which was previously shown to reduce the manifestation of withdrawal in the lab setting (Millan et al. 2001; Navarro-Zaragoza et al. 2010), revealed that TCAP-1 better attenuated the behavioral expression compared to the optimal dose of the antagonist. More specifically, whereas CP-154,526 paradoxically achieves maximum attenuating effects on naloxone-precipitated jumping and plasma CORT levels at the different doses of 20 mg/kg and 50 mg/kg, respectively, TCAP-1 achieved significant suppression of both endpoints at the same dose, providing compelling evidence for its role in the mechanisms that manifest opioid withdrawal. It should be noted that only male subjects were included in this study to clearly characterize the effects of TCAP-1 without the potential introduction of estrous cycle-related plasma CORT variability previously observed (Nichols and Chevins 1981). Moreover, male and female rodents exhibit developmental differences in opioid withdrawal-induced behavioral responses, which would have further complicated the characterization of TCAP-1 (Bravo et al. 2020). Nonetheless, future studies that include female subjects are warranted to more accurately characterize the broader potential clinical utility of TCAP-1.
This study supports literature implicating a role for TCAP-1 in aspects of the addiction cycle, specifically, opioid-associated withdrawal, functioning through a CRF-related mechanism for attenuating stress. The finding that the TCAP-1 peptide has profound effects on an evolutionarily novel phenomenon such as withdrawal from drugs of abuse is striking, and likely indicates that the primary influence of TCAP-1 is to reduce withdrawal-associated stress to ameliorate withdrawal. Previous work found that following cocaine self-administration, chronic but not acute pretreatment with TCAP-1 blocked both CRF-induced reinstatement and cocaine-sensitized locomotor stimulation by CRF in rats (Kupferschmidt et al. 2011). In another study, rats underwent either short- or long-access cocaine self-administration and the effect of TCAP-1 on CRF-mediated drug reinstatement was examined. Consistent with the previous findings, the study found that rats treated with TCAP-1 after self-administration but before reinstatement demonstrated less CRF-induced lever pressing compared to controls, suggesting that TCAP-1 suppressed CRF-induced cocaine seeking (Erb et al. 2014). Importantly, these findings did not necessarily predict the results of the current study, since the neural underpinnings of addiction of psychostimulants like cocaine are different from those from other classes of drugs, such as opioids in this case. Chronic TCAP-1 pretreatment has also been shown to attenuate other aspects of neuropsychiatric disorders including stress and anxiety. Chronic TCAP-1 pretreatment decreased acoustic startle responses (Wang et al. 2005) and attenuated CRF-induced anxiety-related behavior in the elevated plus maze and open field tests (Al Chawaf et al. 2007). Therefore, one key finding of the present study is that TCAP-1 was effective in attenuating naloxone-precipitated withdrawal-associated behavior either when given prophylactically (i.e., before morphine treatment began), or as an intervention (i.e., after morphine treatment had initiated but prior to precipitated withdrawal). There is great clinical benefit to treatment which can be given as an intervention, since only in certain scenarios (e.g., planned surgeries) will opioid use be predictable, and a therapeutic drug be able to be administered beforehand.
Though morphine is an effective drug for pain management, its use can lead to physiological dependence, after which discontinuation of the drug elicits symptoms of withdrawal syndrome including anxiety, muscle pain, insomnia, vomiting, and sweating. These unpleasant symptoms can drive individuals to continue using morphine via negative reinforcement, potentially leading to drug misuse and abuse. To mitigate morphine withdrawal, TCAP-1 could be administered at the end of morphine treatment to suppress morphine withdrawal. Unlike current treatments for opioid withdrawal including methadone, buprenorphine, and clonidine that also have a high abuse potential, preliminary studies with TCAP-1 suggest that it is not reinforcing and has low abuse potential (unpublished data).
In addition to the aforementioned studies that examined the effects of TCAP-1 on behavior, studies using CRF antagonists have found that these treatments influence stress- and anxiety-related behavior, which provides a strong rationale for the continued investigation of TCAP-1 as a therapeutic for these indications. Most relevant to our current work, treatment with a variety of CRF antagonists have been shown to attenuate behavioral manifestations of withdrawal from drugs of abuse (Roberto et al. 2017). Specifically, pretreatment with the nonpeptide CRF1 receptor antagonist CP-154,526 was previously shown to reduce jumping, teeth chattering, writhing, shaking, and weight loss induced by naloxone injection in morphine treated subjects (Almela et al. 2012; Lu et al. 2000). While these studies found that CP-154,526 was able to attenuate morphine withdrawal-induced jumping, these studies were different from the present study in that they used rats as opposed to mice, and used longer morphine treatment regimens to induce dependence (Iredale et al. 2000; Lu et al. 2000). Therefore, the weaker attenuating effect of CP-154,526 in the present study may result from a species difference or the extent of opioid withdrawal generated over the two days of morphine treatment. Treatment with CP-154,526 has also been shown to attenuate anxiety- and depression-related behaviors (Kehne and Cain 2010), with chronic treatment decreasing immobility time in a forced swim test (Overstreet et al. 2004), and acute treatment increasing the amount of time spent in open arms on an elevated plus maze (Griebel et al. 1998; Lundkvist et al. 1996) and decreasing separation-induced vocalizations in pups (Kehne and Cain 2010). However, despite a vast amount of preclinical data suggesting the utility of CRF antagonists to improve behaviors associated with stress and neuropsychiatric disorders at large, many were translational failures in the clinic due to factors such as poor drug safety, efficacy, and specificity, short duration of preclinical screens, and effects on other components of the CRF system that maintain normal physiology (Shaham and de Wit 2016; Spierling and Zorrilla 2017). The paradoxical biphasic dose-response curve elicited with CP-154,526 treatment found in the present study and other antagonists in previous studies may reflect some of these issues (Millan et al. 2001; Walker et al. 2009a, b).
Specifically, in one human trial it was shown that despite receptor antagonism made evident by decreased cortisol levels, a CRF1 receptor antagonist had no behavioral effect on major depressive disorder (Binneman et al. 2008). An additional cross-species study found that while a CRF1 receptor antagonist blocked HPA axis activation in rats and reduced cortisol levels in anxious alcohol-dependent women, the ratings for alcohol craving in the women were unaffected (Schwandt et al. 2016). The reasons for this dissociation between efficacy in attenuating circulating stress hormones and lack of efficacy in behavior are still uncertain but may be explained by the theory that CRF1 receptors in extrahypothalamic sites of action better predict behavioral efficacy. Several studies have implicated areas such as the amygdala as a critical site of action for the CRF1 receptor on behavior (Zorrilla et al. 2014), and sufficient CRF1 receptor antagonism in this area perhaps does not occur at the same systemic doses as those that effectively suppress circulating CORT. In addition, it is possible that at the doses of CRF1 receptor antagonists that effectively suppress CORT, poor selectivity, which may cause these antagonists to engage other receptors, or poor distribution, which may prevent these antagonists from blocking CRF in important target structures (e.g., the amygdala), can explain this lack of efficacy on behavior.
Accordingly, the reasons why TCAP-1 appears to better impact both the HPA axis response and provide behavioral efficacy at a comparable dose are likely complex. One reason may be that whereas CRF1 receptor antagonists like CP-154,526 target the receptor directly, TCAP-1 produces a similar net result to inhibit this pathway but via a different mechanism. Some currently documented mechanisms by which TCAP-1 functions include modulating synaptic plasticity and cytoskeletal dynamics via binding to the G-protein coupled receptor latrophilin (Husić et al. 2019; Woelfle et al. 2015), and by modulating intracellular calcium levels via actions on both the mitochondria and plasma membranes (Hogg et al. 2022). Moreover, some of these functions have been shown to attenuate CRF-induced cellular effects (Hogg et al. 2022). Thus, it is possible that this alternative mechanism for attenuating the downstream mechanisms of CRF1 receptor activation can account for the better matching behavioral and physiological endpoints determined by the current study. Furthermore, future pharmacokinetic/pharmacodynamic and selectivity data for TCAP-1 may further support its advantage over CRF1 receptor antagonists, either due to enhanced selectivity for the CRF1 receptor pathway, or better distribution to central sites of action important for behavior, such as the amygdala. The continued investigation of TCAP-1 in drug abuse contexts is warranted and may provide better clinical efficacy in the CRF-targeted class of treatments than direct CRF1 receptor antagonists.
Lastly, it is worthwhile to briefly note that the dosing regimen for naloxone was slightly altered across studies. The first two experiments were carried out using a naloxone dose of 10 mg/kg established in initial naloxone-precipitated morphine withdrawal studies to induce jumping in mice (Siegel et al. 1975). However, since more recent work has shown in fact more robust jumping behavior elicited at lower doses of naloxone, the naloxone dose for later studies was adjusted to 2.5 mg/kg to increase the magnitude of the jumping response to thus better compare efficacy between TCAP-1 and CP-154,526 (el-Kadi and Sharif 1994). Moreover, while we did not formally test the potential locomotor-suppressing effects of TCAP-1 in this study, which may have had a confounding effect on jumping behavior, several studies have demonstrated that either centrally or systemically administered TCAP-1 does not suppress general motor behavior (Al Chawaf et al. 2007; Kupferschmidt et al. 2011). It was also observed in the video recordings that TCAP-1-treated mice were able to move freely around the test cylinder, indicating no reduction of locomotor activity, in contrast to the MK-801-treated mice, which demonstrated a more generalized suppression of locomotion. Therefore, it is unlikely that the results of the current study are attributable to general motor suppression or sedation. Finally, when evaluating novel treatments for withdrawal in animals, it is important to not only consider their effects on stereotyped motor actions and autonomic responses as we have done in the present study, but also on measures of the withdrawal-associated negative affective state anhedonia, anxiety, and avoidance, which were not examined here. As such, while the current data suggest that TCAP-1 suppresses the positive symptoms associated withdrawal, further work will be needed to indicate whether negative affective symptoms may be expected clinically.
In summary, this study found that TCAP-1 treatment significantly attenuated both the development and expression of the behavioral manifestation of withdrawal in morphine-treated mice. Furthermore, TCAP-1 administration at the end of morphine treatment was better able to decrease the jumping behavior compared to nonpeptide CRF1 receptor antagonist CP-154,526. Continued investigation of the function and utility of TCAP-1 in the context of withdrawal and other stress-related neuropsychiatric disorders will potentially lead to the development of new and better therapies in the clinic.
References
Abdelhamid EE, Sultana M, Portoghese PS, Takemori AE (1991) Selective blockage of delta opioid receptors prevents the development of morphine tolerance and dependence in mice. J Pharmacol Exp Ther 258:299–303
Al Chawaf A, Xu K, Tan L, Vaccarino FJ, Lovejoy DA, Rotzinger S (2007) Corticotropin-releasing factor (CRF)-induced behaviors are modulated by intravenous administration of teneurin C-terminal associated peptide-1 (TCAP-1). Peptides 28:1406–1415. https://doi.org/10.1016/j.peptides.2007.05.014
Almela P, Navarro-Zaragoza J, García-Carmona JA, Mora L, Hidalgo J, Milanés MV, Laorden ML (2012) Role of corticotropin-releasing factor (CRF) receptor-1 on the catecholaminergic response to morphine withdrawal in the nucleus accumbens (NAc). PLoS ONE 7:e47089. https://doi.org/10.1371/journal.pone.0047089
Alsultan MM, Guo JJ (2022) Utilization, spending, and price of opioid medications in the US Medicaid Programs between 1991 and 2019. Am Health Drug Benefits 15:31–37
Ball SJ, Simpson K, Zhang J, Marsden J, Heidari K, Moran WP, Mauldin PD, McCauley JL (2021) J Public Health Manag Pract 27:379–384. https://doi.org/10.1097/phh.0000000000001203. High-Risk Opioid Prescribing Trends: Prescription Drug Monitoring Program Data From 2010 to 2018
Bickel WK, Stitzer ML, Liebson IA, Bigelow GE (1988) Acute physical dependence in man: effects of naloxone after brief morphine exposure. J Pharmacol Exp Ther 244:126–132
Binneman B, Feltner D, Kolluri S, Shi Y, Qiu R, Stiger T (2008) A 6-week randomized, placebo-controlled trial of CP-316,311 (a selective CRH1 antagonist) in the treatment of major depression. Am J Psychiatry 165:617–620. https://doi.org/10.1176/appi.ajp.2008.07071199
Bravo IM, Luster BR, Flanigan ME, Perez PJ, Cogan ES, Schmidt KT, McElligott ZA (2020) Divergent behavioral responses in protracted opioid withdrawal in male and female C57BL/6J mice. Eur J Neurosci 51:742–754. https://doi.org/10.1111/ejn.14580
Brugger S, Sánchez R, Brugger AJ, Martinez JA (1998) ICV administration of CRF blocker (CRF9-41 delta helical) reduces morphine withdrawal in rats. Prog Neuropsychopharmacol Biol Psychiatry 22:775–785. https://doi.org/10.1016/s0278-5846(98)00039 – 6
Buckingham JC (1982) Secretion of corticotrophin and its hypothalamic releasing factor in response to morphine and opioid peptides. Neuroendocrinology 35:111–116. https://doi.org/10.1159/000123364
Cappendijk SL, de Vries R, Dzoljic MR (1993) Excitatory amino acid receptor antagonists and naloxone-precipitated withdrawal syndrome in morphine-dependent mice. Eur Neuropsychopharmacol 3:111–116. https://doi.org/10.1016/0924-977x(93)90262-k
Chen Y, Xu M, De Almeida R, Lovejoy DA (2013) Teneurin C-terminal associated peptides (TCAP): modulators of corticotropin-releasing factor (CRF) physiology and behavior. Front Neurosci 7:166. https://doi.org/10.3389/fnins.2013.00166
Contarino A, Papaleo F (2005) The corticotropin-releasing factor receptor-1 pathway mediates the negative affective states of opiate withdrawal. Proc Natl Acad Sci U S A 102:18649–18654. https://doi.org/10.1073/pnas.0506999102
Crowley NA, Kash TL (2015) Kappa opioid receptor signaling in the brain: circuitry and implications for treatment. Prog Neuropsychopharmacol Biol Psychiatry 62:51–60. https://doi.org/10.1016/j.pnpbp.2015.01.001
Dowell D, Haegerich TM, Chou R (2016) CDC Guideline for Prescribing opioids for Chronic Pain–United States, 2016. JAMA 315:1624–1645. https://doi.org/10.1001/jama.2016.1464
Dydyk AM, Jain NK, Guptam M (2023) Opioid use disorder. StatPearls, Treasure Island (FL)
el-Kadi AO, Sharif SI (1994) The influence of various experimental conditions on the expression of naloxone-induced withdrawal symptoms in mice. Gen Pharmacol 25:1505–1510. https://doi.org/10.1016/0306-3623(94)90181-3
Elhabazi K, Trigo JM, Mollereau C, Moulédous L, Zajac JM, Bihel F, Schmitt M, Bourguignon JJ, Meziane H, Petit-demoulière B, Bockel F, Maldonado R, Simonin F (2012) Involvement of neuropeptide FF receptors in neuroadaptive responses to acute and chronic opiate treatments. Br J Pharmacol 165:424–435. https://doi.org/10.1111/j.1476-5381.2011.01563.x
Erb S, McPhee M, Brown ZJ, Kupferschmidt DA, Song L, Lovejoy DA (2014) Repeated intravenous administrations of teneurin-C terminal associated peptide (TCAP)-1 attenuates reinstatement of cocaine seeking by corticotropin-releasing factor (CRF) in rats. Behav Brain Res 269:1–5. https://doi.org/10.1016/j.bbr.2014.04.013
Flanagan CD, Joseph NM, Benedick A, Vallier HA (2020) Five-year trends in Opioid Prescribing following Orthopaedic Trauma. J Am Acad Orthop Surg Glob Res Rev 4. e20.00134
Friedman J, Godvin M, Shover CL, Gone JP, Hansen H, Schriger DL (2022) Trends in Drug Overdose deaths among US adolescents, January 2010 to June 2021. JAMA 327:1398–1400. https://doi.org/10.1001/jama.2022.2847
Funada M, Hara C, Wada K (2001) Involvement of corticotropin-releasing factor receptor subtype 1 in morphine withdrawal regulation of the brain noradrenergic system. Eur J Pharmacol 430:277–281. https://doi.org/10.1016/s0014-2999(01)01402-9
Funk CK, O’Dell LE, Crawford EF, Koob GF (2006) Corticotropin-releasing factor within the central nucleus of the amygdala mediates enhanced ethanol self-administration in withdrawn, ethanol-dependent rats. J Neurosci 26:11324–11332. https://doi.org/10.1523/jneurosci.3096-06.2006
George O, Ghozland S, Azar MR, Cottone P, Zorrilla EP, Parsons LH, O’Dell LE, Richardson HN, Koob GF (2007) CRF-CRF1 system activation mediates withdrawal-induced increases in nicotine self-administration in nicotine-dependent rats. Proc Natl Acad Sci U S A 104:17198–17203. https://doi.org/10.1073/pnas.0707585104
Gold LH, Stinus L, Inturrisi CE, Koob GF (1994) Prolonged tolerance, dependence and abstinence following subcutaneous morphine pellet implantation in the rat. Eur J Pharmacol 253:45–51. https://doi.org/10.1016/0014-2999(94)90755-2
Griebel G, Perrault G, Sanger DJ (1998) Characterization of the behavioral profile of the non-peptide CRF receptor antagonist CP-154,526 in anxiety models in rodents. Comparison with diazepam and buspirone. Psychopharmacology 138:55–66. https://doi.org/10.1007/s002130050645
Haun HL, Lebonville CL, Solomon MG, Griffin WC, Lopez MF, Becker HC (2022) Dynorphin/Kappa Opioid receptor activity within the extended amygdala contributes to stress-enhanced Alcohol drinking in mice. Biol Psychiatry 91:1019–1028. https://doi.org/10.1016/j.biopsych.2022.01.002
Heishman SJ, Stitzer ML, Bigelow GE, Liebson IA (1989) Acute opioid physical dependence in humans: effect of varying the morphine-naloxone interval. I. J Pharmacol Exp Ther 250:485–491
Higgins GA, Nguyen P, Sellers EM (1992) The NMDA antagonist dizocilpine (MK801) attenuates motivational as well as somatic aspects of naloxone precipitated opioid withdrawal. Life Sci 50: Pl167-72. https://doi.org/10.1016/0024-3205(92)90452-u
Hogg DW, Casatti CC, Belsham DD, Baršytė-Lovejoy D, Lovejoy DA (2022) Distal extracellular teneurin region (teneurin C-terminal associated peptide; TCAP) possesses independent intracellular calcium regulating actions, in vitro: a potential antagonist of corticotropin-releasing factor (CRF). Biochem Biophys Rep 32:101397. https://doi.org/10.1016/j.bbrep.2022.101397
Houshyar H, Gomez F, Manalo S, Bhargava A, Dallman MF (2003) Intermittent morphine administration induces dependence and is a chronic stressor in rats. Neuropsychopharmacology 28:1960–1972. https://doi.org/10.1038/sj.npp.1300271
Husić M, Barsyte-Lovejoy D, Lovejoy DA (2019) Teneurin C-Terminal Associated peptide (TCAP)-1 and Latrophilin Interaction in HEK293 cells: evidence for modulation of intercellular adhesion. Front Endocrinol (Lausanne) 10:22. https://doi.org/10.3389/fendo.2019.00022
Iredale PA, Alvaro JD, Lee Y, Terwilliger R, Chen YL, Duman RS (2000) Role of corticotropin-releasing factor receptor-1 in opiate withdrawal. J Neurochem 74:199–208. https://doi.org/10.1046/j.1471-4159.2000.0740199.x
Jones JD, Sherwin E, Martinez S, Comer SD (2020) Naloxone-Induced Withdrawal in individuals with and without fentanyl-positive urine samples. Am J Addict 29:51–56. https://doi.org/10.1111/ajad.12979
Kamei C, Shimomura K, Ueki S (1973) Significance of withdrawal jumping response in predicting physical dependence in mice. Jpn J Pharmacol 23:421–426. https://doi.org/10.1254/jjp.23.421
Kehne JH, Cain CK (2010) Therapeutic utility of non-peptidic CRF1 receptor antagonists in anxiety, depression, and stress-related disorders: evidence from animal models. Pharmacol Ther 128:460–487. https://doi.org/10.1016/j.pharmthera.2010.08.011
Kest B, Palmese CA, Hopkins E, Adler M, Juni A (2001) Assessment of acute and chronic morphine dependence in male and female mice. Pharmacol Biochem Behav 70:149–156. https://doi.org/10.1016/s0091-3057(01)00600-1
Kest B, Palmese CA, Hopkins E, Adler M, Juni A, Mogil JS (2002) Naloxone-precipitated withdrawal jumping in 11 inbred mouse strains: evidence for common genetic mechanisms in acute and chronic morphine physical dependence. Neuroscience 115:463–469. https://doi.org/10.1016/s0306-4522(02)00458-x
Koyuncuoğlu H, Dizdar Y, Aricioğlu F, Sayin U (1992) Effects of MK 801 on morphine physical dependence: attenuation and intensification. Pharmacol Biochem Behav 43:487–490. https://doi.org/10.1016/0091-3057(92)90181-e
Kupferschmidt DA, Lovejoy DA, Rotzinger S, Erb S (2011) Teneurin C-terminal associated peptide-1 blocks the effects of corticotropin-releasing factor on reinstatement of cocaine seeking and on cocaine-induced behavioural sensitization. Br J Pharmacol 162:574–583. https://doi.org/10.1111/j.1476-5381.2010.01055.x
Leconte C, Mongeau R, Noble F (2022) Traumatic stress-Induced vulnerability to addiction: critical role of the Dynorphin/Kappa opioid receptor system. Front Pharmacol 13:856672. https://doi.org/10.3389/fphar.2022.856672
Lu L, Liu D, Ceng X, Ma L (2000) Differential roles of corticotropin-releasing factor receptor subtypes 1 and 2 in opiate withdrawal and in relapse to opiate dependence. Eur J Neurosci 12:4398–4404
Lundkvist J, Chai Z, Teheranian R, Hasanvan H, Bartfai T, Jenck F, Widmer U, Moreau JL (1996) A non peptidic corticotropin releasing factor receptor antagonist attenuates fever and exhibits anxiolytic-like activity. Eur J Pharmacol 309:195–200. https://doi.org/10.1016/0014-2999(96)00337-8
McNally GP, Akil H (2002) Role of corticotropin-releasing hormone in the amygdala and bed nucleus of the stria terminalis in the behavioral, pain modulatory, and endocrine consequences of opiate withdrawal. Neuroscience 112:605–617. https://doi.org/10.1016/s0306-4522(02)00105-7
Meldrum M (2020) Opioids’ Long Shadow. AMA J Ethics 22:E729–734. https://doi.org/10.1001/amajethics.2020.729
Merlo Pich E, Lorang M, Yeganeh M, Rodriguez de Fonseca F, Raber J, Koob GF, Weiss F (1995) Increase of extracellular corticotropin-releasing factor-like immunoreactivity levels in the amygdala of awake rats during restraint stress and ethanol withdrawal as measured by microdialysis. J Neurosci 15:5439–5447. https://doi.org/10.1523/jneurosci.15-08-05439.1995
Millan MJ, Brocco M, Gobert A, Dorey G, Casara P, Dekeyne A (2001) Anxiolytic properties of the selective, non-peptidergic CRF(1) antagonists, CP154,526 and DMP695: a comparison to other classes of anxiolytic agent. Neuropsychopharmacology 25:585–600. https://doi.org/10.1016/s0893-133x(01)00244-5
National Academies of Sciences E, Medicine, Health, Medicine D, Board on Health Sciences P, Committee on Pain M Regulatory Strategies to address prescription opioid A (2017). In: Phillips JK, Ford MA, Bonnie RJ (eds) Pain Management and the opioid epidemic: balancing societal and individual benefits and risks of prescription opioid use. National Academies Press (US). Copyright 2017 by the National Academy of Sciences All rights reserved., Washington (DC)
Navarro-Zaragoza J, Núñez C, Laorden ML, Milanés MV (2010) Effects of corticotropin-releasing factor receptor-1 antagonists on the brain stress system responses to morphine withdrawal. Mol Pharmacol 77:864–873. https://doi.org/10.1124/mol.109.062463
Navarro-Zaragoza J, Martínez-Laorden E, Teruel-Fernández FJ, Gómez-Murcia V, Cánovas A, Milanés MV, Laorden ML, Almela P (2021) Naloxone-induced conditioned place aversion score and extinction period are higher in C57BL/6J morphine-dependent mice than in Swiss: role of HPA axis. Pharmacol Biochem Behav 201:173106. https://doi.org/10.1016/j.pbb.2021.173106
Nichols DJ, Chevins PF (1981) Plasma corticosterone fluctuations during the oestrous cycle of the house mouse. Experientia 37:319–320. https://doi.org/10.1007/bf01991678
NIDA (2023) Drug overdose death rates. Trends & Statistics
Overstreet DH, Keeney A, Hogg S (2004) Antidepressant effects of Citalopram and CRF receptor antagonist CP-154,526 in a rat model of depression. Eur J Pharmacol 492:195–201. https://doi.org/10.1016/j.ejphar.2004.04.010
Rasmussen K, Fuller RW, Stockton ME, Perry KW, Swinford RM, Ornstein PL (1991) NMDA receptor antagonists suppress behaviors but not norepinephrine turnover or locus coeruleus unit activity induced by opiate withdrawal. Eur J Pharmacol 197:9–16. https://doi.org/10.1016/0014-2999(91)90358-w
Richter RM, Weiss F (1999) In vivo CRF release in rat amygdala is increased during cocaine withdrawal in self-administering rats. Synapse 32:254–261
Roberto M, Cruz MT, Gilpin NW, Sabino V, Schweitzer P, Bajo M, Cottone P, Madamba SG, Stouffer DG, Zorrilla EP, Koob GF, Siggins GR, Parsons LH (2010) Corticotropin releasing factor-induced amygdala gamma-aminobutyric acid release plays a key role in alcohol dependence. Biol Psychiatry 67:831–839. https://doi.org/10.1016/j.biopsych.2009.11.007
Roberto M, Spierling SR, Kirson D, Zorrilla EP (2017) Corticotropin-releasing factor (CRF) and addictive behaviors. Int Rev Neurobiol 136:5–51. https://doi.org/10.1016/bs.irn.2017.06.004
Rysztak LG, Jutkiewicz EM (2022) The role of enkephalinergic systems in substance use disorders. Front Syst Neurosci 16:932546. https://doi.org/10.3389/fnsys.2022.932546
Schwandt ML, Cortes CR, Kwako LE, George DT, Momenan R, Sinha R, Grigoriadis DE, Pich EM, Leggio L, Heilig M (2016) The CRF1 antagonist verucerfont in anxious alcohol-dependent women: translation of neuroendocrine, but not of Anti-craving effects. Neuropsychopharmacology 41:2818–2829. https://doi.org/10.1038/npp.2016.61
Seth V, Upadhyaya P, Moghe V, Ahmad M (2011) Role of calcium in morphine dependence and naloxone-precipitated withdrawal in mice. J Exp Pharmacol 3:7–12. https://doi.org/10.2147/jep.S15240
Shaham Y, de Wit H (2016) Lost in translation: CRF1 receptor antagonists and addiction treatment. Neuropsychopharmacology 41:2795–2797. https://doi.org/10.1038/npp.2016.94
Siegel RK, Gusewelle BE, Jarvik ME (1975) Naloxone-induced jumping in morphine dependent mice: stimulus control and motivation. Int Pharmacopsychiatry 10:17–23. https://doi.org/10.1159/000468164
Simmons SC, Shepard RD, Gouty S, Langlois LD, Flerlage WJ, Cox BM, Nugent FS (2020) Early life stress dysregulates kappa opioid receptor signaling within the lateral habenula. Neurobiol Stress 13:100267. https://doi.org/10.1016/j.ynstr.2020.100267
Singh P, Sharma B, Gupta S, Sharma BM (2015) In vivo and in vitro attenuation of naloxone-precipitated experimental opioid withdrawal syndrome by insulin and selective KATP channel modulator. Psychopharmacology 232:465–475. https://doi.org/10.1007/s00213-014-3680-5
Skelton KH, Gutman DA, Thrivikraman KV, Nemeroff CB, Owens MJ (2007) The CRF1 receptor antagonist R121919 attenuates the neuroendocrine and behavioral effects of precipitated lorazepam withdrawal. Psychopharmacology 192:385–396. https://doi.org/10.1007/s00213-007-0713-3
Spierling SR, Zorrilla EP (2017) Don’t stress about CRF: assessing the translational failures of CRF(1)antagonists. Psychopharmacology 234:1467–1481. https://doi.org/10.1007/s00213-017-4556-2
Tan LA, Xu K, Vaccarino FJ, Lovejoy DA, Rotzinger S (2009) Teneurin C-terminal associated peptide (TCAP)-1 attenuates corticotropin-releasing factor (CRF)-induced c-Fos expression in the limbic system and modulates anxiety behavior in male Wistar rats. Behav Brain Res 201:198–206. https://doi.org/10.1016/j.bbr.2009.02.013
Tan LA, Al Chawaf A, Vaccarino FJ, Boutros PC, Lovejoy DA (2011) Teneurin C-terminal associated peptide (TCAP)-1 modulates dendritic morphology in hippocampal neurons and decreases anxiety-like behaviors in rats. Physiol Behav 104:199–204. https://doi.org/10.1016/j.physbeh.2011.03.015
Tanganelli S, Antonelli T, Morari M, Bianchi C, Beani L (1991) Glutamate antagonists prevent morphine withdrawal in mice and guinea pigs. Neurosci Lett 122:270–272. https://doi.org/10.1016/0304-3940(91)90875-t
Tkaczynski JA, Borodovitsyna O, Chandler DJ (2022) Delta Opioid receptors and Enkephalinergic Signaling within Locus Coeruleus promote stress resilience. Brain Sci 12. https://doi.org/10.3390/brainsci12070860
Trujillo KA, Akil H (1991) Inhibition of morphine tolerance and dependence by the NMDA receptor antagonist MK-801. Science 251:85–87. https://doi.org/10.1126/science.1824728
Vale W, Spiess J, Rivier C, Rivier J (1981) Characterization of a 41-residue ovine hypothalamic peptide that stimulates secretion of corticotropin and beta-endorphin. Science 213:1394–1397. https://doi.org/10.1126/science.6267699
Vasconcelos M, Stein DJ, Gallas-Lopes M, Landau L, Behrens L, Albrechet-Souza L, Miczek KA, de Almeida RMM (2019) Role of CRF receptor 1 antagonism in the bed nucleus of the stria terminalis of male rats after intermittent social defeat stress. bioRxiv 784488. https://doi.org/10.1101/784488
Walker D, Yang Y, Ratti E, Corsi M, Trist D, Davis M (2009a) Differential effects of the CRF-R1 antagonist GSK876008 on fear-potentiated, light- and CRF-enhanced startle suggest preferential involvement in sustained vs phasic threat responses. Neuropsychopharmacology 34:1533–1542. https://doi.org/10.1038/npp.2008.210
Walker DL, Miles LA, Davis M (2009b) Selective participation of the bed nucleus of the stria terminalis and CRF in sustained anxiety-like versus phasic fear-like responses. Prog Neuropsychopharmacol Biol Psychiatry 33:1291–1308. https://doi.org/10.1016/j.pnpbp.2009.06.022
Wang L, Rotzinger S, Al Chawaf A, Elias CF, Barsyte-Lovejoy D, Qian X, Wang NC, De Cristofaro A, Belsham D, Bittencourt JC, Vaccarino F, Lovejoy DA (2005) Teneurin proteins possess a carboxy terminal sequence with neuromodulatory activity. Brain Res Mol Brain Res 133:253–265. https://doi.org/10.1016/j.molbrainres.2004.10.019
Wei J, Lai M, Li F, Chen Y, Li X, Qiu Y, Shen H, Xu P, Di B (2023) Assessment of abuse potential of carfentanil. Addict Biol 28:e13265. https://doi.org/10.1111/adb.13265
Weiss F, Ciccocioppo R, Parsons LH, Katner S, Liu X, Zorrilla EP, Valdez GR, Ben-Shahar O, Angeletti S, Richter RR (2001) Compulsive drug-seeking behavior and relapse. Neuroadaptation, stress, and conditioning factors. Ann N Y Acad Sci 937:1–26. https://doi.org/10.1111/j.1749-6632.2001.tb03556.x
WHO (2009) WHO Guidelines approved by the Guidelines Review Committee Clinical Guidelines for Withdrawal Management and Treatment of Drug Dependence in Closed Settings. World Health Organization. Copyright (2009) © World Health Organization Geneva
Wilson JD, Abebe KZ, Kraemer K, Liebschutz J, Merlin J, Miller E, Kelley D, Donohue J (2021) Trajectories of opioid use following first opioid prescription in opioid-naive youths and young adults. JAMA Netw Open 4:e214552–e214552. https://doi.org/10.1001/jamanetworkopen.2021.4552
Woelfle R, D’Aquila AL, Pavlović T, Husić M, Lovejoy DA (2015) Ancient interaction between the teneurin C-terminal associated peptides (TCAP) and latrophilin ligand-receptor coupling: a role in behavior. Front Neurosci 9:146. https://doi.org/10.3389/fnins.2015.00146
Yano I, Takemori AE (1977) Inhibition by naloxone of tolerance and dependence in mice treated acutely and chronically with morphine. Res Commun Chem Pathol Pharmacol 16:721–734
Zhang JJ, Song CG, Dai JM, Li L, Yang XM, Chen ZN (2022) Mechanism of opioid addiction and its intervention therapy: Focusing on the reward circuitry and mu-opioid receptor. MedComm (2020) 3: e148. https://doi.org/10.1002/mco2.148
Zorrilla EP, Valdez GR, Weiss F (2001) Changes in levels of regional CRF-like-immunoreactivity and plasma corticosterone during protracted drug withdrawal in dependent rats. Psychopharmacology 158:374–381. https://doi.org/10.1007/s002130100773
Zorrilla EP, Logrip ML, Koob GF (2014) Corticotropin releasing factor: a key role in the neurobiology of addiction. Front Neuroendocrinol 35:234–244. https://doi.org/10.1016/j.yfrne.2014.01.001
Funding
The work described in this manuscript was supported by Protagenic Therapeutics. LEM, RSW, DAL, RBS, AMS are employees or consultants of Protagenic Therapeutics and receive compensation from Protagenic Therapeutics.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mueller, L.E., Wexler, R.S., Lovejoy, D.A. et al. Teneurin C-terminal associated peptide (TCAP)-1 attenuates the development and expression of naloxone-precipitated morphine withdrawal in male Swiss Webster mice. Psychopharmacology (2024). https://doi.org/10.1007/s00213-024-06582-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00213-024-06582-0