Abstract
Summary
Differential osteogenic potential and responsiveness to 17β-estradiol (E2) of mesenchymal stem cells (MSCs) were found between postmenopausal women with osteoporosis (OP) and osteoarthritis (OA). These results suggest differential biological mechanisms of estrogen deficiency in regulation of bone remodeling between OP and OA.
Introduction
OP and OA are two common disorders in postmenopausal women. The inverse relationship has been suggested between OP and OA, but their mechanisms that relate to estrogen deficiency are not fully understood. The aim of this study was to compare the differential responsiveness to E2 of MSCs from osteoporotic versus osteoarthritic donors.
Methods
Twenty postmenopausal patients, ten with osteoporotic hip fractures and ten with hip osteoarthritis, were included into this study. MSCs were derived from cancellous bones of femoral heads from OA and OP donors and cultured in osteogenic and adipogenic medium with or without E2 added. The alkaline phosphatase (ALP) activity, calcium content, calcified nodules, lipid droplets, messenger RNA (mRNA) expression of ALP, osteocalcin (OC), collagen 1α (COL1α), peroxisome proliferators-activated receptor γ2 (PPARγ2) and lipoprotein lipase (LPL) were measured and compared between two groups with OP and OA.
Results
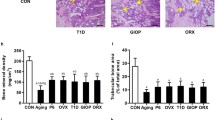
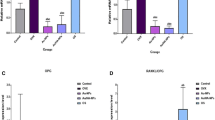
In osteogenic medium, ALP activity, calcium content and mRNA expression of OC and COL1α in MSCs from OA were significantly higher than those from OP group. In adipogenic condition, there was no significant difference in lipid droplets formation and mRNA expression of PPARγ2 and LPL between OP and OA groups. With E2 added in osteogenic medium, ALP activity, calcium content and OC mRNA were significantly higher in OP group than in OA group, whereas E2 had no significant effect on lipid droplet formation and mRNA expression of PPARγ2 and LPL.
Conclusion
Differential osteogenic potential and responsiveness to E2 of MSCs were found between postmenopausal women with OP and OA. These results may provide information for clinical application of MSCs in the differential setting of estrogen deficiency.





Similar content being viewed by others
References
Brandt KD, Dieppe P, Radin EL (2008) Etiopathogenesis of osteoarthritis. Rheum Dis Clin North Am 34:531–559
Hayami T, Pickarski M, Wesolowski GA, McLane J, Bone A, Destefano J, Rodan GA, Duong LT (2004) The role of subchondral bone remodeling in osteoarthritis: reduction of cartilage degeneration and prevention of osteophyte formation by alendronate in the rat anterior cruciate ligament transection model. Arthritis Rheum 50:1193–1206
Bellido M, Lugo L, Roman-Blas JA, Castañeda S, Caeiro JR, Dapia S, Calvo E, Largo R, Herrero-Beaumont G (2010) Subchondral bone microstructural damage by increased remodelling aggravates experimental osteoarthritis preceded by osteoporosis. Arthritis Res Ther 12:R152
Dequeker J, Aerssens J, Luyten FP (2003) Osteoarthritis and osteoporosis: clinical and research evidence of inverse relationship. Aging Clin Exp Res 15:426–439
Avci D, Bachmann GA (2004) Osteoarthritis and osteoporosis in postmenopausal women: clinical similarities and differences. Menopause 11:615–621
Roux C, Fechtenbaum J, Briot K, Cropet C, Liu-Leage S, Marcelli C (2008) Inverse relationship between vertebral fractures and spine osteoarthritis in postmenopausal women with osteoporosis. Ann Rheum Dis 67:224–228
Zhang ZM, Li ZC, Jiang LS, Jiang SD, Dai LY (2010) Micro-CT and mechanical evaluation of subchondral trabecular bone structure between postmenopausal women with osteoarthritis and osteoporosis. Osteoporos Int 21:1383–1390
Lancianese SL, Kwok E, Beck CA, Lerner AL (2008) Predicting regional variations in trabecular bone mechanical properties within the human proximal tibia using MR imaging. Bone 43:1039–1046
Li B, Aspden RM (1997) Mechanical and material properties of the subchondral bone plate from the femoral head of patients with osteoarthritis or osteoporosis. Ann Rheum Dis 56:247–254
Li B, Marshall D, Roe M, Aspden RM (1999) The electron microscope appearance of the subchondral bone plate in the human femoral head in osteoarthritis and osteoporosis. J Anat 195:101–110
Sun SS, Ma HL, Liu CL, Huang CH, Cheng CK, Wei HW (2008) Difference in femoral head and neck material properties between osteoarthritis and osteoporosis. Clin Biomech 23(Suppl 1):S39–S47
Riggs BL, Khosla S, Melton LJ III (2002) Sex steroids and the construction and conservation of the adult skeleton. Endocr Rev 23:279–302
Sniekers YH, Weinans H, Bierma-Zeinstra SM, van Leeuwen JP, van Osch GJ (2008) Animal models for osteoarthritis: the effect of ovariectomy and estrogen treatment: a systematic approach. Osteoarthr Cartil 16:533–541
Roman-Blas JA, Castaneda S, Largo R, Herrero-Beaumont G (2009) Osteoarthritis associated with estrogen deficiency. Arthritis Res Ther 11:241
Wlucka AE, Cicuttini F, Spector TD (2000) Menopause, oestrogens and arthritis. Maturitas 35:183–199
Murphy JM, Dixon K, Beck S, Fabian D, Feldman A, Barry F (2002) Reduced chondrogenic and adipogenic activity of mesenchymal stem cells from patients with advanced osteoarthritis. Arthritis Rheum 46:704–713
Dudics V, Kunstár A, Kovács J, Lakatos T, Géher P, Gömör B, Monostori E, Uher F (2009) Chondrogenic potential of mesenchymal stem cells from patients with rheumatoid arthritis and osteoarthritis: measurements in a microculture system. Cells Tissues Organs 189:307–316
Scharstuhl A, Schewe B, Benz K, Gaissmaier C, Bühring HJ, Stoop R (2007) Chondrogenic potential of human adult mesenchymal stem cells is independent of age or osteoarthritis etiology. Stem Cells 25:3244–3251
Astudillo P, Ríos S, Pastenes L, Pino AM, Rodríguez JP (2008) Increased adipogenesis of osteoporotic human-mesenchymal stem cells (MSCs) characterizes by impaired leptin action. J Cell Biochem 103:1054–1065
Rodríguez JP, Ríos S, Fernandez M, Santibanez JF (2004) Differential activation of ERK1, 2 MAP kinase signaling pathway in mesenchymal stem cell from control and osteoporotic postmenopausal women. J Cell Biochem 92:745–754
Zhang ZM, Jiang LS, Jiang SD, Dai LY (2009) Osteogenic potential and responsiveness to leptin of mesenchymal stem cells between postmenopausal women with osteoarthritis and osteoporosis. J Orthop Res 27:1067–1073
Hess R, Pino AM, Ríos S, Fernández M, Rodríguez JP (2005) High affinity leptin receptors are present in human mesenchymal stem cells (MSCs) derived from control and osteoporotic donors. J Cell Biochem 94:50–57
Ogita M, Rached MT, Dworakowski E, Bilezikian JP, Kousteni S (2008) Differentiation and proliferation of periosteal osteoblast progenitors are differentially regulated by estrogens and intermittent parathyroid hormone administration. Endocrinology 149:5713–5723
Hong L, Sultana H, Paulius K, Zhang G (2009) Steroid regulation of proliferation and osteogenic differentiation of bone marrow stromal cells: a gender difference. J Steroid Biochem Mol Biol 114:180–185
Hong L, Colpan A, Peptan IA (2006) Modulations of 17-β estradiol on osteogenic and adipogenic differentiations of human mesenchymal stem cells. Tissue Eng 12:2747–2753
Jenei-Lanzl Z, Straub RH, Dienstknecht T, Huber M, Hager M, Grässel S, Kujat R, Angele MK, Nerlich M, Angele P (2010) Estradiol inhibits chondrogenic differentiation of mesenchymal stem cells via nonclassic signaling. Arthritis Rheum 62:1088–1096
Dai Z, Li Y, Quarles LD, Song T, Pan W, Zhou H, Xiao Z (2007) Resveratrol enhances proliferation and osteoblastic differentiation in human mesenchymal stem cells via ER-dependent ERK1/2 activation. Phytomedicine 14:806–814
Zhou S, Zilberman Y, Wassermann K, Bain SD, Sadovsky Y, Gazit D (2001) Estrogen modulates estrogen receptor α and β expression, osteogenic activity, and apoptosis in mesenchymal stem cells (MSCs) of osteoporotic mice. J Cell Biochem Suppl 36:144–155
Jiang LS, Zhang ZM, Jiang SD, Chen WH, Dai LY (2008) Differential bone metabolism between postmenopausal women with osteoarthritis and osteoporosis. J Bone Miner Res 23:475–483
Dai LY (1996) The relationship between osteoarthritis and osteoporosis in the hip. J Orthop Rheumatol 9:214–216
Justesen J, Stenderup K, Ebbesen EN, Mosekilde L, Steiniche T, Kassem M (2001) Adipocyte tissue volume in bone marrow is increased with aging and in patients with osteoporosis. Biogerontology 2:165–171
Parfitt AM, Villanueva AR, Foldes J, Rao DS (1995) Relations between histologic indices of bone formation: implications for the pathogenesis of spinal osteoporosis. J Bone Miner Res 10:466–473
Martínez J, Silva S, Santibanez JF (1996) Prostate-derived soluble factors block osteoblast differentiation in culture. J Cell Biochem 61:18–25
Leskela HV, Olkku A, Lehtonen S, Mahonen A, Koivunen J, Turpeinen M, Uusitalo J, Pelkonen O, Kangas L, Selander K, Lehenkari P (2006) Estrogen receptor α genotype confers interindividual variability of response to estrogen and testosterone in mesenchymal-stem-cell-derived osteoblasts. Bone 39:1026–1034
Logar DB, Komadina R, Prezelj J, Ostanek B, Trost Z, Marc J (2007) Expression of bone resorption genes in osteoarthritis and in osteoporosis. J Bone Miner Metab 25:219–225
Bergman RJ, Gazit D, Kahn AJ, Gruber H, McDougall S, Hahn TJ (1996) Age-related changes in osteogenic stem cells in mice. J Bone Miner Res 11:568–577
Zhou S, Greenberger JS, Epperly MW, Goff JP, Adler C, LeBoff MS, Glowacki J (2008) Age-related intrinsic changes in human bone-marrow derived mesenchymal stem cells and their differentiation to osteoblasts. Aging Cell 7:335–343
Rodriguez JP, Garat S, Gajardo H, Pino AM, Seitz G (1999) Abnormal osteogenesis in osteoporotic patients is reflected by altered mesenchymal stem cells dynamics. J Cell Biochem 75:414–423
Herrero-Beaumont G, Roman-Blas JA, Largo R, Berenbaum F, Castaneda S (2011) Bone mineral density and joint cartilage: four clinical settings of a complex relationship in osteoarthritis. Ann Rheum Dis 70:1523–1525
Acknowledgment
This study was supported by the National Natural Science Foundation of China (No. U1032001).
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jin, WJ., Jiang, SD., Jiang, LS. et al. Differential responsiveness to 17β-estradiol of mesenchymal stem cells from postmenopausal women between osteoporosis and osteoarthritis. Osteoporos Int 23, 2469–2478 (2012). https://doi.org/10.1007/s00198-011-1859-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-011-1859-8