Abstract
Purpose
To analyse the effects of bicruciate-retaining total knee arthroplasty (BCR-TKA) on the tensile force of the collateral ligaments during two deep knee flexion activities, cross-leg sitting and squatting.
Methods
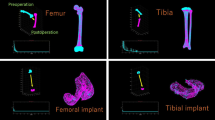
Thirteen patients (15 knees) treated using bicruciate-retaining total knee arthroplasty (BCR-TKA) for knee joint osteoarthritis were analysed. Knee joint kinematics during cross-leg sitting (open-chain flexion) and squatting (closed-chain flexion) were evaluated through fluoroscopy. The tensile force was calculated in vivo based on the change in the distance between the femoral and tibial attachment areas for the anterior, middle, and posterior components of the superficial (sMCL) and deep (dMCL) medial collateral ligament and the lateral collateral ligament (LCL). Differences in the calculated tensile forces of the collateral ligaments were evaluated using repeated measures of analysis of variance, with post hoc pairwise comparison (Bonferroni test). Statistical significance was set at P ≤ 0.05.
Results
The correction of the coronal alignment was related to the surgical technique, not to the implant design. No significant change in the tensile force in all three components of the sMCL from pre- to post-TKA (n.s.) was observed. For dMCL, a pre- to post-TKA change in the tensile force was observed only for the anterior dMCL component (p = 0.03). No change was observed in the tensile force of the anterior LCL with increasing flexion, with no difference in pre- to post-TKA and between activities (n.s.). In contrast, tensile force in the middle LCL slightly decreased with increasing flexion during squatting, pre- and post-TKA. After surgery, lower forces were generated at 40° of flexion (p = 0.04). Tensile force in the posterior LCL was higher in extension than flexion, which remained high in the extension post-TKA. However, after surgery, lower tensile forces were generated at 10° (p = 0.04) and 40° (p = 0.04) of flexion.
Conclusions
The in vivo change in tensile forces of the collateral ligaments of the knee before and after BCR-TKA can inform the development of appropriate ligament balancing strategies to facilitate recovery of deep knee flexion activities after TKA, as well as for continued improvement of BCR-TKA designs.
Level of evidence
III







Similar content being viewed by others
Data availability
The data that support the findings of the current study are available from the corresponding author [HI] upon reasonable request. The data are not publicly available.
References
Angerame MR, Holst DC, Jennings JM, Komistek RD, Dennis DA (2019) Total knee arthroplasty kinematics. J Arthroplasty 34:2502–2510
Blankevoort L, Huiskes R (1991) Ligament-bone interaction in a three-dimensional model of the knee. J Biomech Eng 113:263–269
Faul F, Erdfelder E, Buchner A, Lang AG (2009) Statistical power analyses using G*Power 3.1: tests for correlation and regression analyses. Behav Res Method 41:1149–1160
Halewood C, Traynor A, Bellemans J, Victor J, Amis AA (2015) Anteroposterior laxity after bicruciate-retaining total knee arthroplasty is closer to the native knee than ACL-resecting TKA: A biomechanical cadaver study. J Arthroplasty 30:2315–2319
Heyse TJ, Slane J, Peersman G, Dirckx M, van de Vyver A, Dworschak P et al (2017) Kinematics of a bicruciate-retaining total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 25:1784–1791
Hosseini Nasab SH, Smith CR, Schutz P, Postolka B, List R, Taylor WR (2019) Elongation patterns of the collateral ligaments after total knee arthroplasty are dominated by the knee flexion angle. Front Bioeng Biotechnol 7:323
Innocenti B, Bori E, Paszicsnyek T (2022) Functional stability: an experimental knee joint cadaveric study on collateral ligaments tension. Arch Orthop Trauma Surg 142:1213–1220
Jenny JY, Jenny G (1998) Preservation of anterior cruciate ligament in total knee arthroplasty. Arch Orthop Trauma Surg 118:145–148
Kittl C, Robinson J, Raschke MJ, Olbrich A, Frank A, Glasbrenner J et al (2021) Medial collateral ligament reconstruction graft isometry is effected by femoral position more than tibial position. Knee Surg Sports Traumatol Arthrosc 29:3800–3808
Kono K, Inui H, Tomita T, Yamazaki T, Konda S, Taketomi S et al (2021) In vivo kinematics and cruciate ligament forces in bicruciate-retaining total knee arthroplasty. Sci Rep 11:5645
Kono K, Inui H, Tomita T, Yamazaki T, Taketomi S, Tanaka S (2020) Bicruciate-retaining total knee arthroplasty reproduces in vivo kinematics of normal knees to a lower extent than unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 28:3007–3015
Kono K, Inui H, Tomita T, Yamazaki T, Taketomi S, Tanaka S (2021) In vivo kinematics of bicruciate-retaining total knee arthroplasty with anatomical articular surface under high-flexion conditions. J Knee Surg 34:452–459
Kono K, Konda S, Yamazaki T, Tanaka S, Sugamoto K, Tomita T (2020) In vivo length change of ligaments of normal knees during dynamic high flexion. BMC Musculoskelet Disord 21:552
Kono K, Tomita T, Futai K, Yamazaki T, Tanaka S, Yoshikawa H et al (2018) In vivo three-dimensional kinematics of normal knees during different high-flexion activities. Bone Joint J. 100:50–55
Kuriyama S, Ishikawa M, Furu M, Ito H, Matsuda S (2014) Malrotated tibial component increases medial collateral ligament tension in total knee arthroplasty. J Orthop Res 32:1658–1666
Lavoie F, Denis A, Chergui S, Al-Shakfa F, Sabouret P (2022) Bicruciate-retaining total knee arthroplasty non-inferior to posterior-stabilized prostheses after 5 years: a randomized, controlled trial. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-022-07210-0
Lee YS, Seon JK, Shin VI, Kim GH, Jeon M (2008) Anatomical evaluation of CT-MRI combined femoral model. Biomed Eng Online 7:6
Migaud H, De Ladoucette A, Dohin B, Cloutier JM, Gougeon F, Duquennoy A (1996) Influence of the tibial slope on tibial translation and mobility of non-constrained total knee prosthesis. Rev Chir Orthop Reparatrice Appar Mot 82:7–13
Moro-oka TA, Muenchinger M, Canciani JP, Banks SA (2007) Comparing in vivo kinematics of anterior cruciate-retaining and posterior cruciate-retaining total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 15:93–99
Nagai K, Muratsu H, Takeoka Y, Tsubosaka M, Kuroda R, Matsumoto T (2017) The influence of joint distraction force on the soft-tissue balance using modified gap-balancing technique in posterior-stabilized total knee arthroplasty. J Arthroplasty 32:2995–2999
Nakahara H, Okazaki K, Mizu-Uchi H, Hamai S, Tashiro Y, Matsuda S et al (2015) Correlations between patient satisfaction and ability to perform daily activities after total knee arthroplasty: why aren’t patients satisfied? J Orthop Sci 20:87–92
Nakamura N, Takeuchi R, Sawaguchi T, Ishikawa H, Saito T, Goldhahn S (2011) Cross-cultural adaptation and validation of the Japanese Knee Injury and Osteoarthritis Outcome Score (KOOS). J Orthop Sci 16:516–523
Noble PC, Conditt MA, Cook KF, Mathis KB (2006) The John Insall Award: Patient expectations affect satisfaction with total knee arthroplasty. Clin Orthop Relat Res 452:35–43
Okada Y, Teramoto A, Takagi T, Yamakawa S, Sakakibara Y, Shoji H et al (2018) ACL function in bicruciate-retaining total knee arthroplasty. J Bone Joint Surg Am 100:e114
Pandy MG, Sasaki K, Kim S (1998) A three-dimensional musculoskeletal model of the human knee joint. part 1: theoretical construct. Comput Methods Biomech Biomed Engin 1:87–108
Park KK, Hosseini A, Tsai TY, Kwon YM, Li G (2015) Elongation of the collateral ligaments after cruciate retaining total knee arthroplasty and the maximum flexion of the knee. J Biomech 48:418–424
Pritchett JW (1996) Anterior cruciate-retaining total knee arthroplasty. J Arthroplasty 11:194–197
Pritchett JW (2015) Bicruciate-retaining total knee replacement provides satisfactory function and implant survivorship at 23 Years. Clin Orthop Relat Res 473:2327–2333
Pritchett JW (2011) Patients prefer a bicruciate-retaining or the medial pivot total knee prosthesis. J Arthroplasty 26:224–228
Ritter MA, Harty LD, Davis KE, Meding JB, Berend ME (2003) Predicting range of motion after total knee arthroplasty. Clustering, log-linear regression, and regression tree analysis. J Bone Joint Surg Am 85:1278–1285
Ritter MA, Lutgring JD, Davis KE, Berend ME (2008) The effect of postoperative range of motion on functional activities after posterior cruciate-retaining total knee arthroplasty. J Bone Joint Surg Am 90:777–784
Shelburne KB, Kim HJ, Sterett WI, Pandy MG (2011) Effect of posterior tibial slope on knee biomechanics during functional activity. J Orthop Res 29:223–231
Shelburne KB, Pandy MG (1997) A musculoskeletal model of the knee for evaluating ligament forces during isometric contractions. J Biomech 30:163–176
Stiehl JB, Komistek RD, Cloutier JM, Dennis DA (2000) The cruciate ligaments in total knee arthroplasty: a kinematic analysis of 2 total knee arthroplasties. J Arthroplasty 15:545–550
Tsai TY, Liow M, Li G, Arauz P, Peng Y, Klemt C et al (2019) Bi-cruciate retaining total knee arthroplasty does not restore native tibiofemoral articular contact kinematics during Gait. J Orthop Res 37:1929–1937
Yamazaki T, Watanabe T, Nakajima Y, Sugamoto K, Tomita T, Yoshikawa H et al (2004) Improvement of depth position in 2-D/3-D registration of knee implants using single-plane fluoroscopy. IEEE Trans Med Imaging 23:602–612
Acknowledgements
The authors thank Ryota Yamagami, Kohei Kawaguchi, Tomofumi Kage and Takahiro Arakawa for their assistance in this study.
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
KK contributed to the formal analysis, investigation, and writing of the manuscript. HI and SK carried out data curation and conceived the study. TY provided technical assistance. TT, ST, RY, KK, ST, and DD provided general support. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article. The authors declare that they have no conflicts of interest.
Ethical approval
All participants provided informed consent for the surgery and our evaluation of the tensile force for the collateral ligaments after BCR TKA.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kono, K., Inui, H., Tomita, T. et al. Bicruciate-retaining total knee arthroplasty procedure reduced tensile force in the middle and posterior components of lateral collateral ligament during deep knee flexion activities with no effect on tensile force of the medial collateral ligament. Knee Surg Sports Traumatol Arthrosc 31, 3889–3897 (2023). https://doi.org/10.1007/s00167-023-07342-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-023-07342-x