Abstract
Purpose
The aim of this study was to compare the posterior tibial translation after ultracongruent (UC) and posterior-stabilized (PS) total knee arthroplasty (TKA) with two different UC with different heights in the anterior lip, and two different PS designs. This study also aimed to compare the range of motion (ROM) and outcomes scores after the use of these TKA models. It was hypothesised less posterior tibial translation after PS than after UC TKA, and less posterior tibial translation with a higher anterior lip in the UC insert than with a lower one.
Methods
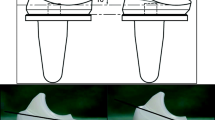
It was designed as a prospective randomized study of a group of 120 patients operated with a cemented TKA. To clarify the main purpose of the study, four groups were analysed using different polyethylene designs: Triathlon PS insert in group one, Triathlon UC insert in group two, U2 PS insert in group three and U2 UC insert in group four. One year after surgery, a forced posterior drawer with a Telos Stress applying 15 kg of force posteriorly on the proximal tibia at 90° of knee flexion was analysed in the lateral radiograph. Limb alignment, tibial posterior slope and posterior condylar offset were also studied.
Results
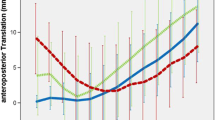
30 patients were included in each group. The average age was 73 years. There were 72.2% female and 27.8% male patients. There were no significant differences in any demographic or radiographic studied variables, preoperative range of motion (ROM) or preoperative Knee Society Scores (KSS) among the different groups. One year after surgery, the average postoperative ROM and the postoperative KSS Knee and KSS Function scores improved in respect of the preoperative values in all the groups. There were no significant differences in the postoperative outcome scores among the different groups (p = n.s.). Postoperative alignment of the limb, tibial posterior slope and posterior condylar offset were similar in the 4 study groups (p = n.s.). The postoperative posterior tibial translation was different between groups: the PS groups (groups 1 and 3) showed significant inferior values (p < 0.001) in respect of the UC groups (groups 2 and 4). There were no differences between both groups of PS models, but there was a significant increase in the posterior tibial translation of the Triathlon UC insert (11.2 mm SD 3.2) in respect of the U2 UC insert (6.1 mm SD 4.5) (p = 0.004).
Conclusions
UC inserts restrict the posterior tibial translation after TKA less than PS inserts, but a design with a high anterior lip in the polyethylene UC insert can better control the posterior tibial translation than an insert with a small anterior lip.
Level of evidence
Level I. Randomised controlled trial.



Similar content being viewed by others
References
Akti S, Karakus D, Sezgin EA, Cankaya D (2020) No differences in clinical outcomes or isokinetic performance between cruciate-substituting ultra-congruent and posterior stabilized total knee arthroplasties: a randomised controlled trial. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06275-z
Appy Fedida B, Krief E, Havet E, Massin P, Mertl P (2015) Cruciate-sacrificing total knee arthroplasty and insert design: A radiologic study of sagittal laxity. Orthop Traumatol Surg Res 101:941–945
Ares O, Castellet E, Maculé F, León V, Montañez E, Freire A, Hinarejos P, Montserrat F, Amillo JR (2013) Translation and validation of “The Knee Society Clinical Rating System” into Spanish. Knee Surg Sports Traumatol Arthrosc 21:2618–2624
Bae JH, Yoon JR, Sung JH, Shin YS (2018) Posterior-stabilized inserts are preferable to cruciate-substituting ultracongruent inserts due to more favourable kinematics and stability. Knee Surg Sports Traumatol Arthrosc 26:3300–3310
Bignozzi S, Zaffagnini S, Akkawi I, Marko T, Bruni D, Neri MP, Colle F, Marcacci M (2014) Three different cruciate-sacrificing TKA designs: minor intraoperative kinematic differences and negligible clinical differences. Knee Surg Sports Traumatol Arthrosc 22:3113–3120
Can A, Erdogan F, Erdogan AO (2017) Tibiofemoral instability after primary total knee arthroplasty: posterior-stabilized implants for obese patients. Orthopedics 40(5):e812–e819
Costanzo JA, Aynardi MC, Peters JD, Kopolovich DM, Purtill JJ (2014) Patellar clunk syndrome after total knee arthroplasty; risk factors and functional outcomes of arthroscopic treatment. J Arthroplasty 29(9 Suppl):201–204
Fritzsche H, Beyer F, Postler A, Lützner J (2018) Different intraoperative kinematics, stability, and range of motion between cruciate-substituting ultracongruent and posterior-stabilized total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26:1465–1470
Han HS, Kang SB (2020) Anterior-stabilized TKA is inferior to posterior-stabilized TKA in terms of postoperative posterior stability and knee flexion in osteoarthritic knees: a prospective randomized controlled trial with bilateral TKA. Knee Surg Sports Traumatol Arthrosc 28:3217–3225
Hofmann AA, Tkach TK, Evanich CJ, Camargo MP (2000) Posterior stabilization in total knee arthroplasty with use of an ultracongruent polyethylene insert. J Arthroplasty 15:576–583
Ishii Y, Noguchi H, Sato J, Sakurai T, Toyabe SI (2017) Anteroposterior translation and range of motion after total knee arthroplasty using posterior cruciate ligament-retaining versus posterior cruciate ligament-substituting prostheses. Knee Surg Sports Traumatol Arthrosc 25:3536–3542
Jones DP, Locke C, Pennington J, Theis JC (2006) The effect of sagittal laxity on function after posterior cruciate-retaining total knee replacement. J Arthroplasty 21:719–723
Kim MS, Koh IJ, Kim CK, Choi KY, Jeon JH, In Y (2021) Comparison of joint perception between posterior-stabilized and ultracongruent total knee arthroplasty in the same patient. J Bone Joint Surg Am 103:44–52
Kim TW, Lee SM, Seong SC, Lee S, Jang J, Lee MC (2016) Different intraoperative kinematics with comparable clinical outcomes of ultracongruent and posterior stabilized mobile-bearing total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 24:3036–3043
Ko YB, Jang EC, Park SM, Kim SH, Kwak YH, Lee HJ (2015) No difference in clinical and radiologic outcomes after total knee arthroplasty with a new ultra-congruent mobile bearing system and rotating platform mobile bearing systems after minimum 5-year follow-up. J Arthroplasty 30:379–383
Lee SS, Yeom J, Lee DH, Moon YW (2020) Similar outcomes between ultracongruent and posterior-stabilized insert in total knee arthroplasty: a propensity score-matched analysis. J Orthop Surg (Hong Kong) 28(1):2309499019893515
Lützner J, Beyer F, Dexel J, Fritzsche H, Lützner C, Kirschner S (2017) No difference in range of motion between ultracongruent and posterior stabilized design in total knee arthroplasty: a randomized controlled trial. Knee Surg Sports Traumatol Arthrosc 25:3515–3521
Lützner J, Beyer F, Lützner C, Riedel R, Tille E (2021) Ultracongruent insert design is a safe alternative to posterior cruciate-substituting total knee arthroplasty: 5-year results of a randomized controlled trial. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06545-4. Online ahead of print
Machhindra MV, Kang JY, Kang YG, Chowdhry M, Kim TK (2015) Functional outcomes of a new mobile-bearing ultra-congruent TKA system: comparison with the posterior stabilized system. J Arthroplasty 30:2137–2142
Mazzucchelli L, Deledda D, Rosso F, Ratto N, Bruzzone M, Bonasia DE, Rossi R (2016) Cruciate retaining and cruciate substituting ultra-congruent insert. Ann Transl Med 4(1):2
Ng JWG, Bloch BV, James PJ (2019) Sagittal radius of curvature, trochlea design and ultracongruent insert in total knee arthroplasty. EFORT Open Rev 4(8):519–524
Sherman WF, Mansour A, Sanchez FL, Wu VJ (2020) Increased intercondylar femoral box cut-to-femur size ratio during posterior-stabilized total knee arthroplasty increases risk for intraoperative fracture. Arthroplast Today 6:180–185
Song SJ, Bae DK, Kim KI (2016) Jeong HY (2016) Changes in femoral posterior condylar offset, tibial posterior slope angle, and joint line height after cruciate-retaining total knee arthroplasty. Knee Surg Relat Res 28(1):27–33
Sur YJ, Koh IJ, Park SW, Kim HJ, In Y (2015) Condylar-stabilizing tibial inserts do not restore anteroposterior stability after total knee arthroplasty. J Arthroplasty 30:587–591
Verra WC, van den Boom LG, Jacobs W, Clement DJ, Wymenga AA (2013) Nelissen RG (2013) Retention versus sacrifice of the posterior cruciate ligament in total knee arthroplasty for treating osteoarthritis. Cochrane Database Syst Rev 10:CD004803
Wajsfisz A, Biau D, Boisrenoult P, Beaufils P (2010) Comparative study of intraoperative knee flexion with three different TKR designs. Orthop Traumatol Surg Res 96:242–248
Acknowledgements
The authors would like to thank Xavier Duran from Institut Hospital del Mar d’Investigacions Mèdiques (IMIM) of Barcelona for his help in the methodological advice and statistical analysis.
Funding
No funding has received related to this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Hinarejos and Dr. Leal-Blanquet have perceived fees as scientific consultants by Medcomtech. Dr. Hinarejos has perceived fees for scientific presentations by Stryker.
Ethical approval
The present study received IRB approval by the Parc de Salut Mar Ethical Committee (2017/7170/I).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hinarejos, P., Leal-Blanquet, J., Fraile-Suari, A. et al. Increased posterior translation but similar clinical outcomes using ultracongruent instead of posterior stabilized total knee arthroplasties in a prospective randomized trial. Knee Surg Sports Traumatol Arthrosc 30, 3041–3048 (2022). https://doi.org/10.1007/s00167-021-06710-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06710-9