Abstract
Aims/hypothesis
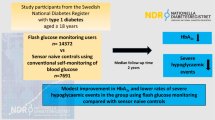
We assessed the real-world effect of flash monitor (FM) usage on HbA1c levels and diabetic ketoacidosis (DKA) and severe hospitalised hypoglycaemia (SHH) rates among people with type 1 diabetes in Scotland and across sociodemographic strata within this population.
Methods
This study was retrospective, observational and registry based. Using the national diabetes registry, 14,682 individuals using an FM at any point between 2014 and mid-2020 were identified. Within-person change from baseline in HbA1c following FM initiation was modelled using linear mixed models accounting for within-person pre-exposure trajectory. DKA and SHH events were captured through linkage to hospital admission and mortality data. The difference in DKA and SHH rates between FM-exposed and -unexposed person-time was assessed among users, using generalised linear mixed models with a Poisson likelihood. In a sensitivity analysis, we tested whether changes in these outcomes were seen in an age-, sex- and baseline HbA1c-matched sample of non-users over the same time period.
Results
Prevalence of ever-FM use was 45.9% by mid-2020, with large variations by age and socioeconomic status: 64.3% among children aged <13 years vs 32.7% among those aged ≥65 years; and 54.4% vs 36.2% in the least-deprived vs most-deprived quintile. Overall, the median (IQR) within-person change in HbA1c in the year following FM initiation was −2.5 (−9.0, 2.5) mmol/mol (−0.2 [−0.8, 0.2]%). The change varied widely by pre-usage HbA1c: −15.5 (−31.0, −4.0) mmol/mol (−1.4 [−2.8, −0.4]%) in those with HbA1c > 84 mmol/mol [9.8%] and 1.0 (−2.0, 5.5) mmol/mol (0.1 [−0.2, 0.5]%) in those with HbA1c < 54 mmol/mol (7.1%); the corresponding estimated fold change (95% CI) was 0.77 (0.76, 0.78) and 1.08 (1.07, 1.09). Significant reductions in HbA1c were found in all age bands, sexes and socioeconomic strata, and regardless of prior/current pump use, completion of a diabetes education programme or early FM adoption. Variation between the strata of these factors beyond that driven by differing HbA1c at baseline was slight. No change in HbA1c in matched non-users was observed in the same time period (median [IQR] within-person change = 0.5 [−5.0, 5.5] mmol/mol [0.0 (−0.5, 0.5)%]). DKA rates decreased after FM initiation overall and in all strata apart from the adolescents. Estimated overall reduction in DKA event rates (rate ratio) was 0.59 [95% credible interval (CrI) 0.53, 0.64]) after FM vs before FM initiation, accounting for pre-exposure trend. Finally, among those at higher risk for SHH, estimated reduction in event rates was rate ratio 0.25 (95%CrI 0.20, 0.32) after FM vs before FM initiation.
Conclusions/interpretation
FM initiation is associated with clinically important reductions in HbA1c and striking reduction in DKA rate. Increasing uptake among the socioeconomically disadvantaged offers considerable potential for tightening the current socioeconomic disparities in glycaemia-related outcomes.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
In type 1 diabetes, there has been a shift from traditional methods of self-monitoring of blood glucose using fingerpricks and glucometers (compliance can be poor with <50% adherence to guidelines among people with type 1 diabetes in Sweden [1]) to using new technologies that allow for more frequent measurements with less discomfort. These new technologies enable real-time or intermittently scanned continuous glucose monitoring [2]. The latter is known as flash monitoring, with the only system currently available for use in the National Health Service (NHS) in the UK (including Scotland) being Abbott’s Freestyle Libre. Flash monitors (FMs) have been available in the UK since late 2014 [3]. They became freely available in Scotland from the NHS in 2018, having been only self-funded previously. Eligibility for FM use follows a mixture of criteria defined by each of the Scottish Health boards.
The largest RCT of FMs (N = 328), IMPACT, demonstrated a significant effect of FM use on hypoglycaemia without any significant change in HbA1c. However IMPACT was restricted to adults with good glycaemic control (HbA1c ≤ 58 mmol/mol [7.5%]) [4], and is therefore not representative of the range of current recipients of this technology from the NHS. Observational studies have shown reductions in HbA1c, diabetic ketoacidosis (DKA) and hypoglycaemia with use of FMs [5,6,7,8,9,10,11,12,13,14]. Greater effects on HbA1c have been found in individuals with high initial HbA1c but, apart from this, study of variation in effectiveness across different subgroups of recipients has been limited, particularly for DKA, where there is a gap in the literature. It is important to determine whether any groups benefit less from FMs, as this may indicate a need for measures to improve efficacy.
In this paper, we aimed to describe the contemporary prevalence of FM use among all those with type 1 diabetes in Scotland and to examine the association of FM initiation with glycaemic outcomes (HbA1c, DKA and hypoglycaemia) across the full range of recipients and within age, sex and socioeconomic groups, as well as by prior glycaemic control, insulin pump usage and completed diabetes education programme. We also examined outcomes among the early adopters, who self-funded the device before it became NHS-funded.
Methods
Data sources
We used anonymised data from the Scottish Care Information - Diabetes Collaboration (SCI-DC) database, a registry with extensive electronic health records for all those with diabetes in Scotland. These routinely collected data include start and end dates for FM use, as well as prescription data. These data are also linked to hospital admissions data SMR01 from Information Services Division Scotland and mortality data from National Records of Scotland (NRS). The database and linkage procedure have been described in detail elsewhere [15, 16].
Study population
Among all those alive with type 1 diabetes, observable at any point between 2014 and mid-2020, we included for glycaemic outcome analyses those who started using an FM between 2014 and 31 October 2019 to limit the number of recipients with no post-initiation HbA1c by the end of study date. The type of diabetes was ascertained based on a validated algorithm [15]. FM start and stop dates were assessed from SCI-DC device dates and from encashed prescription data for Libre sensors. Individuals contributed person-time from the latest of either date of diabetes diagnosis or start of observability in the Scottish diabetes registry, to the earliest of date of death, last date of observability, first stop-date of FM use or 30 June 2020 (end of study). Glycaemic measures were assessed up to a maximum of 5 years prior to FM initiation, hence individual person-time was left-censored 5 years before FM initiation date. To disentangle the effect of FM initiation from that of other devices, person-time was right-censored at the first start date of insulin pump/continuous glucose monitoring (CGM) device if these started after FM initiation.
Exposure, outcomes and covariates
The exposure of interest was FM usage. Individual person-time was partitioned into intervals of 1 year centred on the date of FM initiation [17]. HbA1c records were obtained from the SCI-DC data. Individuals’ median HbA1c over time slices was used for analyses. Baseline value was defined as median over the 2 years prior to FM initiation for continuous covariates, and most severe state over this time window for discrete covariates.
Baseline HbA1c was categorised to reflect different levels of glycaemic control (in mmol/mol [%]: <54 [7.1]; ≥54 [7.1] to ≤63 [7.9]; ≥64 [8.0] to ≤74 [8.9]; ≥75 [9.0] to ≤84 [9.8]; >84 [9.8]). Data on hospitalisations and deaths for DKA and severe hypoglycaemia from up to 5 years pre-FM initiation were obtained using the ICD-10 codes (http://apps.who.int/classifications/icd10/browse/2016/en) detailed in electronic supplementary material (ESM) Methods, anywhere on the discharge summary or cause of death.
Area-level deprivation was measured by the Scottish Index of Multiple Deprivation (SIMD) 2016 definition [18], which is based on the postcode of residence. SIMD quintiles were used for analyses, Q1 being the most deprived. Insulin pump/CGM exposure and completed diabetes education programme status were ascertained from SCI-DC. Prior pump usage was defined as any usage of insulin pump preceding the initiation of FM, regardless of whether usage continued post-FM. An early adopter was defined as anyone who started FM before 2018.
Statistical analyses
Comparison of outcomes between users and non-users of FM may be subject to allocation bias or confounding by indication. Therefore, our analyses focused on changes within users over time in outcomes from pre- to post-initiation of FM. All analyses were conducted using R version 3.6.0–64 bit [19] and at significance level 0.05. No imputation of missing data was performed.
HbA1c
Absolute within-person change from baseline HbA1c was described over time, overall and among the groups of interest listed above. The significance of reductions was assessed using a one-sided (difference < 0) Wilcoxon signed-rank test with a Bonferroni correction for multiple comparisons of various time points vs baseline.
To account for any background trend over time occurring in HbA1c prior to FM initiation and for repeated measurements within individuals, we used mixed models adjusted for time, age, diabetes duration at initiation, sex and baseline HbA1c [20] (see ESM Methods). Specifically, log-transformed HbA1c was modelled using linear mixed models, with a random intercept and time slope on the individual, with categorical FM exposure time as a covariate, implemented in nlme 3.1-143 [21]. Model estimates represent change in HbA1c compared with what the levels would have been had any pre-exposure trend continued (i.e. the counterfactual). To examine whether the association of FM with HbA1c varied across groups of interest, we compared models with and without the FM × group interaction term using likelihood ratio tests (LRTs). Further, to examine whether any such interactions were explained by variation in baseline HbA1c across strata, we tested whether interactions remained significant when models were adjusted for the interaction term FM × baseline HbA1c.
DKA and SHH
Crude DKA and severe hospitalised hypoglycaemia (SHH) rates were described in pre- and post-FM person-time. Due to their discrete and rare nature, DKA and SHH event rates were modelled using generalised linear mixed models with a Poisson likelihood and a random intercept on the individual, with FM exposure as a binary time-varying covariate and adjusting for pre-FM time trend. To avoid reliance on approximations of intractable integrals, these models were implemented in a Bayesian Framework using rstan 2.19.3, with results expressed as rate ratios with 95% credible intervals (CrIs).
Stratified analyses of DKA rates were conducted across the groups of interest. Due to the sparser nature of SHH events, we focused on high risk groups for this outcome: those with a prior history of SHH in the 5 years pre-FM and those with baseline HbA1c < 54 mmol/mol (7.1%).
Sensitivity analyses
To ensure that any changes in outcomes attributed to FM use were not confounded by the occurrence of some more general phenomena coinciding with FM introduction, we performed crude sensitivity analyses of changes over a similar time period in a sample of non-users, matched 1:1 by sex, baseline HbA1c band and age band at FM initiation date (ESM Methods). Non-users were defined as individuals who had never used a device by the user’s date of FM initiation and for at least 6 months thereafter. The significance of differences in HbA1c was assessed using a one-sided Wilcoxon signed-rank test with a Bonferroni correction for multiple comparison. Comparisons of event rates were made using crude rate ratios.
Results
The study sample-size flowchart is shown in ESM Fig. 1.
Prevalence of FM use
The crude prevalence of ever-FM users among those alive with type 1 diabetes increased rapidly after reimbursement began, from 3.1% in 2017 to 45.9% (n = 14,682) by mid-2020. Usage was higher in female vs male individuals and in younger vs older age bands (Table 1). Quarterly prevalence by year and age band is detailed in ESM Fig. 2. Prevalence of use decreased with HbA1c band, was higher among those with vs without prior pump usage, those with prior SHH history, and in those from least vs most-deprived areas. These disparities were present across age bands and sex, although differences were smaller in younger vs older age bands (63.7% vs 52.8% in <13 years band; 22.3% vs 43.8% in ≥65 years band).
Baseline characteristics of ever-users of FM
We included for analyses of glycaemic outcomes 12,256 FM users who started using the device before 31 October 2019. Their baseline characteristics are described in ESM Table 1 alongside those of matched non-users. The median FM initiation date was 16 November 2018. The median (IQR) post-FM initiation follow-up time was 1.5 (1.0, 2.0) years. Among the FM users, 23.4% had initiated a pump prior to FM, and 0.5% (n = 60) had stepped down from a CGM; 29.2% had a record of any completed diabetes education and 7.6% were early adopters.
Changes in HbA1c
Overall
Among all users combined there was a median (IQR) reduction in HbA1c of −2.5 (−9.0, 2.5) mmol/mol (−0.2 [−0.8, 0.2]%) (n = 10,761; p < 0.01) within the first year post-exposure and −2.5 (−9.0, 3.5) mmol/mol (−0.2 [−0.8, 0.3]%) (n = 758; p < 0.01) for ≥2 years of exposure (Table 2). Over similar time periods, there was no change in HbA1c in the matched non-users, as illustrated in Fig. 1 (median [IQR] within-person change = 0.5 [−5.0, 5.5] mmol/mol [0.0 (−0.5, 0.5)%]). Taking into consideration the slight downward trend occurring in HbA1c among users prior to FM initiation, modelled estimates revealed a fold change in HbA1c of 0.94 (0.94, 0.95) at 1 year post-initiation and 0.99 (0.98, 1.00) at ≥2 years (ESM Table 2).
Stratified analyses
Since approximately half the FM users had more than 1 year of follow-up post-exposure, results for stratified analyses focus on the year following FM exposure. Results beyond that time period are given in the tables for informative purposes. We did not perform analyses stratified by prior CGM usage due to the low number of prior CGM users.
By baseline HbA1c
Among FM users, change in HbA1c was strongly dependent on HbA1c at baseline, ranging from a median (IQR) reduction of −15.5 (−31.0, −4.0) mmol/mol (−1.4 [−2.8, −0.4]%) during the first year following FM initiation in those with HbA1c > 84 mmol/mol (9.8%) at baseline to a slight median (IQR) increase of 1.0 (−2.0, 5.5) mmol/mol (0.1 [−0.2, 0.5]%) in those with HbA1c < 54 mmol/mol (7.1%) at baseline (Table 2). Taking into consideration trends occurring in HbA1c among users prior to FM initiation, the modelled estimates ranged from a fold change (95% CI) of 0.77 (0.76, 0.78) in those with HbA1c > 84 mmol/mol (9.8%) at baseline to 1.08 (1.07, 1.09) in those with HbA1c < 54 mmol/mol at baseline (ESM Table 2).
By age band
FM initiation was associated with a reduction in HbA1c in all age bands (Fig. 2a), with smaller estimated changes in the >64 years band. There was significant variation in HbA1c at initiation by age (ESM Table 3), with HbA1c being lowest in those aged <13 years and highest in those aged 19–24 years. As expected from this, reductions in HbA1c were greatest among the 19–24 years age band. Among those aged 13–18 years, the median observed within-person change was 0.0 (−7.0, 7.0) mmol/mol (0.0 [−0.6, 0.6]%) (ESM Table 4). However, the modelled estimate, accounting for increase in HbA1c pre-FM exposure, suggested a reduction compared with the counterfactual, with a 0.95 (95% CI 0.94, 0.96) fold change (ESM Table 5). Within any age band, in those with high HbA1c (≥75 mmol/mol [9.0%]) at FM initiation, clear reductions were observed in HbA1c. These were most pronounced in children (<13 years), with a median (IQR) within-person fall of −30.5 (−50.0, −12.0) mmol/mol (−2.8 [−4.6, −1.1]%) (ESM Table 6). Allowing for differences in initial HbA1c, there was evidence of some variation in the fold change by age band (p for age group × FM interaction <0.01).
Estimated fold changes (95% CI) in HbA1c within the first year post FM initiation, compared with pre-exposure levels, adjusted for pre-exposure trend, baseline HbA1c, age, sex and diabetes duration and stratified by age band at FM initiation (a), sex (b), SIMD quintile (c), prior pump usage (d), prior completed diabetes education programme status (e) and early adopter status (f)
By sex
FM initiation was associated with a similar reduction in HbA1c in men and women respectively (pinteraction = 0.18; Fig. 2b).
By SIMD
FM initiation was associated with a reduction in HbA1c in all SIMD quintiles. The magnitude of reduction was similar across quintiles (pinteraction = 0.10; Fig. 2c), despite those from more-deprived quintiles presenting with higher baseline HbA1c (ESM Tables 3, 7, 8).
By prior pump usage
FM initiation was associated with a reduction in HbA1c regardless of prior pump use, although reductions were smaller in prior pump users (Fig. 2d and ESM Tables 9, 10), as expected from their lower HbA1c at baseline compared with those with no prior pump use (ESM Table 3). However, when allowing for differences in baseline HbA1c, there was still evidence of some variation in effect by prior pump usage (p < 0.01 for FM × pump interaction).
By prior completed diabetes education programme
FM initiation was associated with a reduction in HbA1c regardless of prior education status (Fig. 2e and ESM Tables 11, 12). Reductions were higher in those without completed education, while both groups had similar baseline HbA1c (ESM Table 3).
By early adopter status
FM initiation was associated with similar reductions in HbA1c regardless of early FM adoption (Fig. 2f and ESM Tables 13, 14).
Changes in DKA rates
There were 53,046 person-years observable for DKA/SHH events before FM initiation and 19,001 afterwards. DKA rates pre-FM initiation varied considerably across the strata of interest (Fig. 3). Pre-FM rates were higher in those with high baseline HbA1c, young adults, those from more-deprived areas, those with no prior pump use, those with no completed diabetes education programme and in the non-early-adopters.
Crude DKA event rates (95% CI) in FM users, after and before FM initiation, stratified by baseline HbA1c at initiation (a), age at FM initiation (b), sex (c), SIMD quintile (d), prior pump usage (e), prior completed diabetes education programme status (f) and early adopter status (g). PY, person-years
DKA rates significantly decreased overall after FM initiation (estimated rate ratio from the Bayesian models was 0.59 [95% CrI 0.53, 0.64], see Table 3). At the same time, rates across non-users decreased slightly but to a much lesser magnitude: crude rate ratio (95% CI) for post- vs pre-index time 0.90 (0.85, 0.96) vs 0.67 (0.63, 0.72) in users.
Crude DKA rates decreased in pre- vs posts-FM person-time among all subgroups examined (Fig. 3), apart from the adolescent group, where an increase was observed (Fig. 3b). All reductions were significant apart for those with prior pump use and those with baseline HbA1c 64–74 mmol/mol (8.0–8.9%) (Fig. 3a,e).
The Bayesian models adjusting for prior trends showed reductions in all subgroups apart from those with prior pump use and those with baseline HbA1c 54–63 mmol/mol (7.1–7.9%), where there was uncertainty around the result (ESM Fig. 3). Estimated reduction in rates was most marked among those with baseline HbA1c ≥ 75 mmol/mol (9.0%) and those with HbA1c < 54 mmol/mol (7.1%), though the credible interval was extremely wide in this subgroup due to the low number of events (ESM Fig. 3a).
Estimated reductions were most substantial in children (ESM Fig. 3b). Model results also indicated that, accounting for increase in DKA rate in pre-FM years, FM was associated with a reduction in DKA rate among adolescents, compared with the counterfactual. The magnitude of estimated reduction was higher in male vs female participants (ESM Fig. 3c), in those from least- vs most-deprived areas (ESM Fig. 3d) and in those without vs with prior pump use (ESM Fig. 3.e). Model results also suggested a higher reduction in those without vs with prior completed diabetes education programme (ESM Fig. 3f) and early adopters of FM (ESM Fig. 3g), although CrIs were wide and overlapped.
Changes in SHH rates
SHH rates slightly decreased overall post-FM (Table 3) Among those with a prior SHH history, the crude event-rate was significantly lower during FM-exposed person-time. Bayesian model estimates supported this finding (estimated rate ratio 0.25 [95% CrI 0.20, 0.32], see Table 3). We did not have enough statistical power to analyse pre–post differences among those with starting HbA1c < 54 mmol/mol (7.1%), who will probably have been prescribed FM due to recurrent hypoglycaemia. There were only 109 events observed pre-FM (crude rate 15.4 [12.7, 18.6] per 1000 person-years) and 26 post-FM (crude rate 9.3 [6.1, 13.7] per 1000 person-years).
Discussion
This study showed that prevalence of FM use increased rapidly among individuals with type 1 diabetes in Scotland after FMs became free of charge but disparities remain across deprivation levels. FM initiation was associated with a significant decrease in HbA1c overall among users. HbA1c reductions were most pronounced in those with high baseline HbA1c. HbA1c reductions occurred in all SIMD quintiles and age groups, and regardless of sex, prior pump use, early adopter status or prior completed diabetes education programme. FM use was associated with marked reductions in DKA overall and generally within all subgroups examined. FM initiation was also associated with a decrease in SHH among those with a prior history of SHH.
To our knowledge, our large nationwide study is the first to examine disparities in the prevalence of FM use in Scotland. We have confirmed and extended previous glycaemic outcome findings of small-scale studies in Scotland [6, 22] by providing generalisable results. We have also augmented the scope of recent large-scale studies [13, 14] by extensively exploring variations in HbA1c and DKA outcomes following the initiation of FM use across sociodemographic strata, which has not been done before and provides novel information crucial to clinical practice.
Efforts made by the Scottish Government, clinical teams, charities such as Diabetes UK, and people with diabetes to widen the usage of FMs in Scotland have been successful, with a tenfold increase in use over the past couple of years. However, the gap between most- and least-deprived quintiles persists, although it is smaller than the 4% vs 60% observed in the most- vs least-deprived quintiles in an Edinburgh diabetes centre in 2017 prior to NHS funding [3]. This gap highlights the existence of healthcare inequalities in access to technology. The extent to which this relates to user preference or to failure of the devices being recommended by clinicians is unclear. Prevalence of use is highest among the paediatric population but gaps across deprivation levels exist even in this group.
Our overall findings on HbA1c reductions are in keeping with previous findings such as those from a single-centre Edinburgh study (−4 mmol/mol [−0.4%]) [22], meta-analyses performed on FM and HbA1c, mean −4.5 mmol/mol [−0.4%] in uncontrolled studies [7], and a registry-study from the Netherlands (mean −3.3 mmol/mol [−0.3%]) [11]. Less than half of the FM users were followed-up for more than 1 year post-initiation, therefore more longitudinal follow-up is needed to establish the long-term persistence of the improvements in HbA1c.
Only a few studies have looked at FM use and DKA so far. Our findings regarding DKA overall are in keeping with those of other nationwide studies regarding DKA hospitalisation rates [9, 14]. In a French nationwide database, Roussel et al. [14] reported that DKA hospitalisation rates fell by 56.2% in the year after vs before FM initiation. This reduction is beneficial in terms of individuals’ wellbeing and reductions in healthcare costs, as DKA is expensive to treat [23].
Stratified analyses of DKA rates following FM initiation are lacking in the literature. The variations in HbA1c changes from baseline across starting HbA1c were in keeping with those reported in previous studies: slight increase among those with optimally controlled baseline HbA1c [6, 24]; and substantial decrease among those with high baseline HbA1c [6, 7, 10, 13, 22]. We also found that reductions in DKA rates post- vs pre-FM were most marked in those with high baseline HbA1c. These improvements are extremely promising and likely to translate into a reduction in healthcare costs as those with high HbA1c levels are most at risk of complications [25].
We found that FM use was associated with improvements in HbA1c in all SIMD quintiles, showing that this technology benefits all, including those from more-deprived areas. Tsur et al. [9] also reported significant improvements in HbA1c among those with lower socioeconomic status. Although the magnitude of reduction in DKA rates was higher among those from least-deprived areas, there were marked improvements in all SIMD quintiles. Unequal distribution of, or access to, this technology may further widen existing inequalities in healthcare, especially since those from more-deprived areas have historically higher HbA1c [26] and thus stand to benefit most from FM.
Existing paediatric studies have had small sample sizes [7, 8] with heterogeneous findings. For example, Campbell et al. [27] reported a significant decrease in HbA1c among children aged 4–17 years, while Messaaoui et al. [28] reported no change in HbA1c among their sample of children/young people aged 4–20 years. In our study, HbA1c reduction appeared to be smaller among the paediatric group, although this was expected considering the well-controlled baseline HbA1c. Conversely, reduction in DKA rates was substantial in children. Among those with high baseline HbA1c, marked reductions in HbA1c were observed in all age groups.
Despite minimal observed reduction in HbA1c and observed increase in crude DKA rate among adolescents, model results accounting for prior trends suggested improvement in both areas. Longer post-FM follow-up is needed among adolescents to better understand how or whether FM use mitigates the usual deterioration in HbA1c among this age group. It is also important to consider factors other than blood glucose outcomes when evaluating the benefits of FM in this group, such as quality of life. Indeed, qualitative studies [29, 30] have suggested such improvements in this demographic. Al Hayek et al. [31] also found a significant reduction in diabetes distress in a sample of 187 adolescents. However, we do not have access to such data and additional work needs to be done to examine whether FM usage among adolescents could be improved further.
The smaller reductions observed among those with prior pump use was consistent with their lower baseline HbA1c, and was in keeping with other findings [9]. Individuals using insulin pumps in Scotland attend a structured education programme prior to pump initiation and receive substantial input from diabetes support services. Therefore, gains in terms of HbA1c are expected to be marginal in this group. The non-significant decrease in DKA is likely due to significant improvements already occurring following pump initiation [32]. Improvements in this group are expected in terms of quality of life or hypoglycaemia but we did not possess data to assess this.
DKA and HbA1c improved regardless of completion of a diabetes education programme but individual education levels were not available to assess their influence on outcomes.
Interestingly, disparities in DKA rates between strata before FM initiation generally persisted even after the post-FM reductions. This highlights the need to better understand drivers of elevated DKA rates. Indeed, O’Reilly et al. [33] showed that factors beyond structured education, use of pump and HbA1c likely contributed to elevated rates among most-deprived quintiles.
Our findings suggest that FM use is associated with a reduction in SHH among those at risk of this complication. Results on FM usage and hypoglycaemia in the literature vary. The IMPACT study [4] showed a reduction in hypoglycaemia in those with well-controlled HbA1c. Observational studies reported a significant decrease in severe hypoglycaemia [5, 9, 13, 14], while Campbell et al. [27] found time in hypoglycaemia to be unaffected in their paediatric sample. Differences in results are likely due to a combination of differing hypoglycaemia definitions and cohort characteristics/behaviour. It is nonetheless important to understand whether there is any over-adjustment of insulin dose following readings of FM data.
Strengths and limitations
Our study is one of the largest contemporary real-world-setting studies examining the association of FM initiation with glycaemic outcomes combining data from nationwide electronic health records with extensive subgroup analyses, in particular filling a gap in the literature with regards to FM use and DKA. Using data from all individuals with type 1 diabetes in Scotland, we were able to capture current disparities in usage in the country and had enough power to explore a large number of sociodemographic group-specific outcomes.
For comparison, a recent large-scale UK-based voluntary audit [10] possessed post-FM follow-up HbA1c measures for only one-third of the users included (3182 out of 9968), while recent national Swedish and French studies [13, 14] did not examine variations across sociodemographic groups.
We were limited in our analyses of hypoglycaemia by only being able to analyse hospital admissions, which represent a tiny fraction of hypoglycaemic events [34]. We did not have access to granular glucose data from the Libre devices; this would have allowed better understanding of glycaemic variability and analysis of hypoglycaemia with more precision. Our study suffers from the usual biases linked to observational studies, such as unmeasured confounding or measurement error. Since this study was observational, observed changes were not attributable to FM use in the clear-cut manner of an RCT. However, timing of changes and crude comparisons to non-users support the findings in relation to FM initiation.
Since the end of our study, newer FM models such as the Libre 2 have become available (since January 2021). Our findings pertaining to marked improvements even with first-generation Libre devices herald positive outcomes with more updated Libre versions.
Due to the criteria of eligibility for FM use, our results might not be generalisable to all those with type 1 diabetes. These criteria are less restrictive than eligibility to insulin pumps, which were also found to be associated with improved glycaemic outcomes among people with type 1 diabetes in Scotland [32]. It is nonetheless crucial to understand the determinants of good response to FMs to optimise a more widespread roll-out. For example, Riveline et al. [35], among others, showed that scanning frequency is associated with better glycaemic outcomes; however, we did not have access to such data.
Conclusions
Flash glucose monitoring use in Scotland has been associated with clinically important improvements in HbA1c, especially in individuals with high baseline HbA1c who have the most to gain in reducing the risk of diabetes complications. Historically, reducing rates of DKA has proven to be an extremely difficult task and uptake of effective interventions (such as structured education) has often been relatively low. The striking reduction in DKA across the sociodemographic spectrum following FM use is of major clinical importance. More research is needed to better understand how to increase the uptake of FM use and the drivers and features of its effect in order to tighten the existing socioeconomic gaps. Results will need to be updated when longer-term follow-up is available and to keep pace with newer technologies and systems such as newer Libre models, DIY closed-loop systems or officially licensed hybrid-loop systems.
Data availability
We do not have governance permissions to share individual-level data on which these analyses were conducted. However, bona fide researchers can apply to the Scottish Public Benefits and Privacy Protection Committee for access to these data. This research was conducted with approval from the Public Benefit Privacy Protection Panel (PBPP ref. 1617- 0147). All datasets were de-identified before analysis.
Abbreviations
- CGM:
-
Continuous glucose monitoring
- CrI:
-
Credible interval
- DKA:
-
Diabetic ketoacidosis
- FM:
-
Flash monitor
- NHS:
-
National Health Service
- SCI-DC:
-
Scottish Care Information - Diabetes Collaboration
- SHH:
-
Severe hospitalised hypoglycaemia
- SIMD:
-
Scottish Index of Multiple Deprivation
References
Moström P, Ahlén E, Imberg H, Hansson P-O, Lind M (2017) Adherence of self-monitoring of blood glucose in persons with type 1 diabetes in Sweden. BMJ Open Diabetes Res Care 5(1):e000342. https://doi.org/10.1136/bmjdrc-2016-000342
Edelman SV, Argento NB, Pettus J, Hirsch IB (2018) Clinical implications of real-time and intermittently scanned continuous glucose monitoring. Diabetes Care 41(11):2265–2274. https://doi.org/10.2337/dc18-1150
McKnight JA, Gibb FW (2017) Flash glucose monitoring is associated with improved glycaemic control but use is largely limited to more affluent people in a UK diabetes centre. Diabet Med 34(5):732–732. https://doi.org/10.1111/dme.13315
Bolinder J, Antuna R, Geelhoed-Duijvestijn P, Kröger J, Weitgasser R (2016) Novel glucose-sensing technology and hypoglycaemia in type 1 diabetes: a multicentre, non-masked, randomised controlled trial. Lancet 388(10057):2254–2263. https://doi.org/10.1016/S0140-6736(16)31535-5
Charleer S, De Block C, Van Huffel L et al (2020) Quality of life and glucose control after 1 year of nationwide reimbursement of intermittently scanned continuous glucose monitoring in adults living with type 1 diabetes (FUTURE): a prospective observational real-world cohort study. Diabetes Care 43(2):389–397. https://doi.org/10.2337/dc19-1610
Stimson RH, Dover AR, Ritchie SA et al (2020) HbA1c response and hospital admissions following commencement of flash glucose monitoring in adults with type 1 diabetes. BMJ Open Diabetes Res Care 8:e001292. https://doi.org/10.1136/bmjdrc-2020-001292
Gordon I, Rutherford C, Makarounas-Kirchmann K, Kirchmann M (2020) Meta-analysis of average change in laboratory-measured HbA1c among people with type 1 diabetes mellitus using the 14 day flash glucose monitoring system. Diabetes Res Clin Pract 164:108158. https://doi.org/10.1016/j.diabres.2020.108158
Evans M, Welsh Z, Ells S, Seibold A (2020) The impact of flash glucose monitoring on glycaemic control as measured by HbA1c: a meta-analysis of clinical trials and real-world observational studies. Diabetes Ther 11(1):83–95. https://doi.org/10.1007/s13300-019-00720-0
Tsur A, Cahn A, Israel M, Feldhamer I, Hammerman A, Pollack R (2021) Impact of flash glucose monitoring on glucose control and hospitalization in type 1 diabetes: a nationwide cohort study. Diabetes Metab Res Rev 37(1):e3355. https://doi.org/10.1002/dmrr.3355
Deshmukh H, Wilmot EG, Gregory R et al (2020) Effect of flash glucose monitoring on glycemic control, hypoglycemia, diabetes-related distress, and resource utilization in the Association of British Clinical Diabetologists (ABCD) Nationwide Audit. Diabetes Care 43(9):2153–2160. https://doi.org/10.2337/dc20-0738
Fokkert M, van Dijk P, Edens M et al (2019) Improved well-being and decreased disease burden after 1-year use of flash glucose monitoring (FLARE-NL4). BMJ Open Diabetes Res Care 7(1):e000809. https://doi.org/10.1136/bmjdrc-2019-000809
Gernay M-M, Philips J-C, Radermecker R, Paquot N (2018) L’apport du système FreeStyle Libre® dans la prise en charge du patient diabétique: expérience au CHU de Liège. Rev Médicale Liège 73(11):562–569
Nathanson D, Svensson A-M, Miftaraj M, Franzén S, Bolinder J, Eeg-Olofsson K (2021) Effect of flash glucose monitoring in adults with type 1 diabetes: a nationwide, longitudinal observational study of 14,372 flash users compared with 7691 glucose sensor naive controls. Diabetologia 64(7):1595–1603. https://doi.org/10.1007/s00125-021-05437-z
Roussel R, Riveline J-P, Vicaut E et al (2021) Important drop rate of acute diabetes complications in people with type 1 or type 2 diabetes after initiation of flash glucose monitoring in France: the RELIEF study. Diabetes Care 44:1368–1376. https://doi.org/10.2337/dc20-1690
Walker J, Colhoun H, Livingstone S et al (2018) Type 2 diabetes, socioeconomic status and life expectancy in Scotland (2012–2014): a population-based observational study. Diabetologia 61(1):108–116. https://doi.org/10.1007/s00125-017-4478-x
Livingstone SJ, Looker HC, Hothersall EJ et al (2012) Risk of cardiovascular disease and total mortality in adults with type 1 diabetes: Scottish registry linkage study. PLoS Med 9(10):e1001321. https://doi.org/10.1371/journal.pmed.1001321
McKnight JA, Ochs A, Mair C et al (2020) The effect of DAFNE education, continuous subcutaneous insulin infusion, or both in a population with type 1 diabetes in Scotland. Diabet Med 37(6):1016–1022. https://doi.org/10.1111/dme.14223
SIMD (Scottish Index of Multiple Deprivation). https://simd.scot/#/simd2016/BTTTFTT/9/-4.0000/55.9000/. Accessed 15 Mar 2021
R Core Team (2019) R: a language and environment for statistical computing. https://www.R-project.org/. Accessed 10 Feb 2021
McGurnaghan SJ, Brierley L, Caparrotta TM et al (2019) The effect of dapagliflozin on glycaemic control and other cardiovascular disease risk factors in type 2 diabetes mellitus: a real-world observational study. Diabetologia 62(4):621–632. https://doi.org/10.1007/s00125-018-4806-9
Pinheiro J, Bates D, DebRoy S, Sarkar D, R Core Team (2019) nlme: linear and nonlinear mixed effects models. https://CRAN.R-project.org/package=nlme. Accessed 10 Feb 2021
Tyndall V, Stimson RH, Zammitt NN et al (2019) Marked improvement in HbA1c following commencement of flash glucose monitoring in people with type 1 diabetes. Diabetologia 62(8):1349–1356. https://doi.org/10.1007/s00125-019-4894-1
Dhatariya KK, Glaser NS, Codner E, Umpierrez GE (2020) Diabetic ketoacidosis. Nat Rev Dis Primer 6(1):1–20
Paris I, Henry C, Pirard F, Gérard A-C, Colin IM (2018) The new FreeStyle libre flash glucose monitoring system improves the glycaemic control in a cohort of people with type 1 diabetes followed in real-life conditions over a period of one year. Endocrinol Diabetes Metab 1(3):e00023. https://doi.org/10.1002/edm2.23
Govan L, Wu O, Briggs A et al (2011) Achieved levels of HbA1c and likelihood of hospital admission in people with type 1 diabetes in the Scottish population: a study from the Scottish Diabetes Research Network Epidemiology Group. Diabetes Care 34(9):1992–1997. https://doi.org/10.2337/dc10-2099
Mair C, Wulaningsih W, Jeyam A et al (2019) Glycaemic control trends in people with type 1 diabetes in Scotland 2004–2016. Diabetologia 62(8):1375–1384. https://doi.org/10.1007/s00125-019-4900-7
Campbell FM, Murphy NP, Stewart C, Biester T, Kordonouri O (2018) Outcomes of using flash glucose monitoring technology by children and young people with type 1 diabetes in a single arm study. Pediatr Diabetes 19(7):1294–1301. https://doi.org/10.1111/pedi.12735
Messaaoui A, Tenoutasse S, Crenier L (2019) Flash glucose monitoring accepted in daily life of children and adolescents with type 1 diabetes and reduction of severe hypoglycemia in real-life use. Diabetes Technol Ther 21(6):329–335. https://doi.org/10.1089/dia.2018.0339
Al Hayek AA, Robert AA, Al Dawish MA (2020) Acceptability of the FreeStyle libre flash glucose monitoring system: the experience of young patients with type 1 diabetes. Clin Med Insights Endocrinol Diabetes 13:1179551420910122. https://doi.org/10.1177/1179551420910122
Boucher SE, Aum SH, Crocket HR et al (2020) Exploring parental perspectives after commencement of flash glucose monitoring for type 1 diabetes in adolescents and young adults not meeting glycaemic targets: a qualitative study. Diabet Med J Br Diabet Assoc 37(4):657–664. https://doi.org/10.1111/dme.14188
Al Hayek AA, Robert AA, Al Dawish MA (2020) Effectiveness of the Freestyle Libre Flash Glucose Monitoring System on diabetes distress among individuals with type 1 diabetes: a prospective study. Diabetes Ther 11(4):927–937. https://doi.org/10.1007/s13300-020-00793-2
Jeyam A, Gibb FW, McKnight JA et al (2021) Marked improvements in glycaemic outcomes following insulin pump therapy initiation in people with type 1 diabetes: a nationwide observational study in Scotland. Diabetologia 64(6):1320–1331. https://doi.org/10.1007/s00125-021-05413-7
O’Reilly JE, Jeyam A, Caparrotta TM et al (2021) Rising rates and widening socio-economic disparities in diabetic ketoacidosis in type 1 diabetes in Scotland: a nationwide retrospective cohort observational study. Diabetes Care 44:1–8. https://doi.org/10.2337/dc21-0689
McCoy RG, Lipska KJ, Van Houten HK, Shah ND (2020) Association of cumulative multimorbidity, glycemic control, and medication use with hypoglycemia-related emergency department visits and hospitalizations among adults with diabetes. JAMA Netw Open 3(1):e1919099–e1919099. https://doi.org/10.1001/jamanetworkopen.2019.19099
Riveline J-P, Guerci B, Wojtusciszyn A, Dunn TC (2020) La fréquence des scans du capteur de glucose FreeStyle Libre réalisés par le patient diabétique au quotidien est associée à de meilleurs paramètres de suivi de son profil glucosé : analyse de 312 millions d’heures de suivi en vraie vie en France. Médecine Mal Métaboliques 14(7):585–593. https://doi.org/10.1016/j.mmm.2020.08.001
Acknowledgements
We thank the SDRN Epidemiology Group: J. Chalmers (Diabetes Centre, Victoria Hospital, UK), C. Fischbacher (Information Services Division, NHS National Services Scotland, Edinburgh, UK), B. Kennon (Queen Elizabeth University Hospital, Glasgow, UK), G. Leese (Ninewells, Hospital, Dundee, UK), R. Lindsay (British Heart Foundation Glasgow Cardiovascular Research Centre, University of Glasgow, UK), J. McKnight (Western General Hospital, NHS, UK), J. Petrie (Institute of Cardiovascular & Medical Sciences, University of Glasgow, UK), R. McCrimmon (Division of Molecular and Clinical Medicine, University of Dundee, Dundee, UK), S. Philip (Grampian Diabetes research unit, Diabetes Centre, Aberdeen Royal Infirmary, Aberdeen, UK), D. Mcallister (Institute of Health & Wellbeing, University of Glasgow, Glasgow, UK), E. Pearson (population Health and Genomics, School of Medicine, University of Dundee, Dundee, UK), S. Wild (Usher Institute, University of Edinburgh, Edinburgh, UK) and F. Gibb (Royal Infirmary of Edinburgh, Edinburgh, UK). The SDRN Epidemiology Group resource was originally set up with approval from the Scottish A research ethics committee (ref 11/AL/0225), Caldicott Guardians and the Privacy Advisory Committee (PAC ref. 33/11), now running with approval from the Public Benefit and Privacy Panel for Health and Social Care (PBPP ref. 1617-0147). TMC is a Diabetes UK ‘Sir George Alberti Clinical Research Fellow’ (Grant number: 18/0005786).
Authors’ relationships and activities
FWG reports speaker fees and honorarium from Abbott Diabetes Care. JAM reports personal fees from Napp pharmaceuticals and institutional fees for trial participation from Novo Nordisk, Eli Lilly, Boehringer, MedImmune Ltd and GlaxoSmithKline during the conduct of this study. TMC is a Diabetes UK ‘Sir George Alberti Clinical Research Fellow’ and reports grant no.18/0005786 from Diabetes UK, outside the submitted work. RJM reports personal fees from Sanofi and Novo Nordisk, outside the submitted work. NS reports advisory board and speaker honoraria from Amgen, Astra Zeneca, Eli Lilly, Merck Sharp & Dohme, Novartis, Novo Nordisk, Pfizer and Sanofi, and grants and advisory board and speaker honoraria from Boehringer Ingelheim, outside the submitted work. HMC reports grants and personal fees from Eli Lilly and Company during the conduct of the study, grants and personal fees from Novo Nordisk, grants from AstraZeneca LP, Regeneron and Pfizer, institutional fees from Novartis Pharmaceuticals and Sanofi Aventis, and being a shareholder with Roche Pharmaceuticals, outside the submitted work. All other authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Funding
This study was supported by funding from the Diabetes UK (17/0005627) and the Chief Scientist Office (Ref. ETM/47).
Author information
Authors and Affiliations
Consortia
Contributions
AJ, JAM, FWG, HMC and PMM conceived and designed the analyses. AJ performed the analyses. AJ and HMC drafted the initial manuscript. SJM, LAKB and SH were involved in the cleaning, harmonisation, quality control and databasing of data and contributed to critical revision of the manuscript. BK, JAM, RJM, GL, SP and NS contributed to data acquisition and critical revision of the manuscript. PMM was involved in critical revision of the manuscript. FWG, JEOR, TMC and AH were involved in the interpretation of the data and critically revising and editing the manuscript. All authors approved the manuscript for publication. HMC is the guarantor and, as such, is responsible for the integrity of the work as a whole.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 653 kb)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jeyam, A., Gibb, F.W., McKnight, J.A. et al. Flash monitor initiation is associated with improvements in HbA1c levels and DKA rates among people with type 1 diabetes in Scotland: a retrospective nationwide observational study. Diabetologia 65, 159–172 (2022). https://doi.org/10.1007/s00125-021-05578-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-021-05578-1