Abstract
Aims/hypothesis
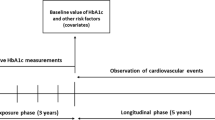
HbA1c variability has been shown to be an independent risk factor for nephropathy in patients with type 1 diabetes. In this study, we aimed to explore the association between HbA1c variability and microalbuminuria development in patients with type 2 diabetes. We also intended to test the applicability of serially measured HbA1c over 2 years for this risk assessment.
Methods
Between 2003 and 2005, we recruited 821 middle-aged normoalbuminuric individuals with type 2 diabetes and followed them through to the end of 2010. The average follow-up time was 6.2 years. We defined microalbuminuria as a urine albumin to creatinine ratio of 30 mg/g (3.4 mg/mmol) or higher. HbA1c variability was calculated by the SD of serially measured HbA1c. The Cox proportional hazards model was used to evaluate the association between HbA1c SD quartile and development of microalbuminuria.
Results
The incidence of microalbuminuria for the overall population was 58.4, 58.6, 60.8 and 91.9 per 1,000 person-years for Q1- to Q4-adjusted HbA1c SD, respectively (p for trend = 0.042). Compared with patients in Q1, those in Q4 were about 37% more likely to develop microalbuminuria. The HR derived from a series of 2 year HbA1c measurements was similar to that from data collection for longer than 4 years.
Conclusions/interpretation
In addition to mean HbA1c values, HbA1c variability, even measured as early as 2 years, is independently associated with the development of microalbuminuria in patients with type 2 diabetes.
Similar content being viewed by others
Introduction
The DCCT in type 1 diabetes and the UK Prospective Diabetes Study in type 2 diabetes both concluded that a rise in HbA1c can increase the development of microvascular complications [1–3]. Recently, glycaemic variability has also been demonstrated to affect the risk of micro- and macrovascular consequences in diabetes [4–7]; however, its association with diabetic complications has not been consistently confirmed [8–12].
Data from the Finnish Diabetic Nephropathy (FinnDiane) study indicated that HbA1c variability in type 1 diabetes patients is predictive of incident microalbuminuria and progression of renal disease [13]. In type 1 diabetes, HbA1c variability was similarly shown to be an independent risk factor for microalbuminuria development, even among the young, who are highly vulnerable to vascular complications [14]. Until now, however, the relationship between HbA1c variability and the development of nephropathy has not been investigated in type 2 diabetes.
Currently, there is no clear consensus as to how long HbA1c should be measured for to unwaveringly reflect the clinical impacts of HbA1c variability. The DCCT and the FinnDiane study undertook 9 and 5.7 year serial HbA1c measurements, respectively, to examine HbA1c variability [13, 15]. However, the follow-up study of the UK Prospective Diabetes Study demonstrated the important role of early strict glycaemic control in preventing vascular complications [16], implying that an indicator that needs to track HbA1c measurements for more than 5 years to correlate its clinical implications may be late for a prompt intervention.
The primary aim of this study was to explore the relationship between HbA1c variability and microalbuminuria development in patients with type 2 diabetes. Furthermore, in order to emphasise the importance of early stabilisation in glycaemic control, we also intended to determine whether HbA1c variability derived from 2 year measurements is an early indicator independently associated with diabetic nephropathy in type 2 diabetes.
Methods
Participants
The study participants were type 2 diabetes patients who were enrolled for the Diabetes Management through an Integrated Delivery System (DMIDS) project (ClinicalTrials.gov NCT00288678) [17]. The detailed inclusion and exclusion criteria for the DMIDS project are described elsewhere [18]. Briefly, 1,209 participants with type 2 diabetes were recruited from 2003 to 2005 and followed through to the end of 2010. Of these enrolees, 143 with fewer than three eligible urine albumin to creatinine ratio (ACR) tests and 245 with microalbuminuria at baseline (ACR ≥3.4 mg/mmol in two consecutive urine tests) were excluded from the analysis. The remaining 821 participants were selected for further investigation. Written informed consent was obtained from all enrolees. The institutional review board at the National Health Research Institutes reviewed and approved this study.
Laboratory tests
Fasting (overnight for ≥8 h) venous blood and morning spot urine specimens were collected every 6 months. HbA1c was measured by high-performance liquid chromatography (Variant II; Bio-Rad Laboratories, Hercules, CA, USA). Triacylglycerol and HDL-cholesterol levels were measured by an automatic analyser (Hitachi 7060; Hitachi High Technologies Co., Tokyo, Japan). Urinary albumin was measured by the immunoturbidimetric method (Hitachi 7060). All blood and urine samples were kept at 2–8°C and measured within 8 h at a central laboratory.
Definition of outcome, HbA1c variability and covariates
Participants who had an ACR of 3.4 mg/mmol or higher in two consecutive urine tests were defined as having developed microalbuminuria. Urine samples were excluded from analysis if microscopic urinalysis showed erythrocytes, white blood cells or epithelial cells of more than five per high-power field, or the appearance of casts or bacteria.
HbA1c variability was defined as the SD of serial HbA1c measurements, the CV of HbA1c to correct for the mean or the adjusted HbA1c SD—in which SD was divided by the square root of k / (k − 1), where k stands for the number of HbA1c measurements—to control for the effects of variation in the number of HbA1c measurements [15]. Because of similar results derived from all three SD definitions, we used the adjusted HbA1c SD to account for HbA1c variability in multivariable survival analysis.
Waist circumference was measured at the level of the midpoint between the lowest rib and the iliac crest. Blood pressure was measured three times separated by 1 min; the mean of these three measurements was recorded. Smoking status was categorised into three groups: current smokers, ex-smokers (having stopped smoking for ≥1 month) and non-smokers (having smoked <100 cigarettes in a lifetime). Those who had ever chewed betel nuts were defined as chewers. Those who had not performed any leisure-time physical activity in the past 2 weeks were defined as the sedentary group.
Statistical analysis
Data are expressed as mean ± SD for continuous variables, or as counts and proportions for categorical variables. Student’s t tests and χ 2 analyses were used for continuous and categorical variables, respectively, to compare characteristics between non-progressors and progressors (with microalbuminuria development). The incidence of microalbuminuria was estimated by the number of observed new microalbuminuria cases per 1,000 person-years. Person-years were calculated as the time elapsed from the date of recruitment until the date of death, loss to follow-up, microalbuminuria development or the end of follow-up, whichever came first. The calculation of a 95% CI for the incidence rate was based on the assumption that the observed incident cases followed a Poisson distribution. We estimated the incidence of microalbuminuria in different quartiles of adjusted HbA1c SD for overall participants and also for different subgroups according to their number of HbA1c measurements and baseline HbA1c. In order to test the predictability of HbA1c variability for microalbuminuria development in different subgroups, we calculated the mean HbA1c and adjusted HbA1c SD for three or four measurements (all HbA1c from recruitment to the end of year 2), and for those with baseline HbA1c ≤8% or >8% (64 mmol/mol), respectively, for subgroup analysis.
Kaplan–Meier analyses and univariate Cox proportional hazard models were used to explore the association between quartiles of adjusted HbA1c SD and microalbuminuria development. The covariates used in Cox proportional hazard models included baseline demographic and metabolic profiles (age at diabetes onset, sex, education, diabetes duration, smoking status, waist circumference, triacylglycerol and HDL-cholesterol levels, mean HbA1c and BP). Multivariable Cox proportional hazards modelling was used to determine the independent effects of HbA1c variability on microalbuminuria development. Study entry was defined as the date of enrolment. Observations were censored at the end of the study or the date that patients died or dropped out of the study, whichever occurred first. Results are expressed as HR compared with the group in the lowest quartile of adjusted HbA1c SD.
The proportional hazard assumption, the constant HR over time, was evaluated by comparing estimated log–log survival curves for all covariates. All assessed log–log survival plots graphically showed two parallel lines, indicating no violation of the assumption. A test for trend was conducted by treating quartiles of adjusted HbA1c SD as a continuous variable.
Analyses were performed with SAS software, version 9.1 (SAS Institute, Cary, NC, USA). A two-sided p value of <0.05 was considered statistically significant.
Results
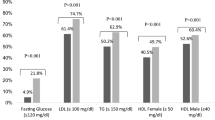
Table 1 shows that progressors were more likely to have lower education, longer diabetes duration and poorer metabolic profiles, including higher baseline urine ACR and poorer control of BP and glucose, compared with non-progressors. Those who developed microalbuminuria also had higher HbA1c variability during the follow-up period. With regard to characteristics in different quartiles of adjusted HbA1c SD (Table 2), those who had higher HbA1c variability tended to have earlier diabetes onset, use more glucose-lowering drugs and have poorer glycaemic control at baseline and during follow-up. Patients in the highest quartile (Q4) of HbA1c SD were also more likely to be smokers (32.4% vs 23.6% for Q1–Q3 combined, p < 0.001), betel nuts chewers (15.1% vs 10.9%, p = 0.031) and physically inactive (35.7% vs 27.5%, p = 0.011).
As shown in Table 3, both mean and adjusted SD of HbA1c were significantly related to microalbuminuria development in univariate analysis as well as in separate multivariable regressions (model 1, HR 1.10, p < 0.05 for mean of HbA1c; model 2, p for trend = 0.001 for adjusted SD of HbA1c); however, the effect of mean of HbA1c was attenuated (HR 1.04, non-significant) when these two variables were put together in the same model (model 3). Compared with those in the lowest quartile of adjusted HbA1c SD, as shown in Table 3, the patients in the Q4 were 48% more likely to develop microalbuminuria (p < 0.05 for Q4 and p for trend = 0.043 in model 3). With regard to other covariates, the impact of lower education was persistent in both univariate and multivariable models; furthermore, diabetes duration, high BP and the subsequent use of ACE inhibitors or angiotensin receptor blockers were also revealed to have marginal effects on the development of microalbuminuria (Table 3) after controlling for other covariates.
As shown in Table 4, the incidences of microalbuminuria for participants overall were 58.4, 58.6, 60.8 and 91.9 per 1,000 person-years for Q1–Q4 adjusted HbA1c SD, respectively (p for trend = 0.001). The graded association (p for trend) between the quartile of adjusted HbA1c SD and risk of microalbuminuria was consistent and little affected by the HbA1c follow-up time (2 vs ≤7 years) or baseline HbA1c (≤8% vs >8% [64 mmol/mol]) (Fig. 1 and Table 4). In contrast, the established effects of mean HbA1c were not significant in those with baseline HbA1c of 8% (64 mmol/mol) or less or for 2 years of follow-up (Table 4). We also used a sex-specific cut-off point [19] to define microalbuminuria and conducted a sensitivity analysis, with similar results (data not shown).
Probability of remaining in normoalbuminuria status, by quartile of adjusted HbA1c SD. (a) Adjusted HbA1c SD was calculated using all HbA1c measurements during the follow-up period. Logrank tests Q2 vs Q1 p = 0.415, Q3 vs Q1 p = 0.107; Q4 vs Q1 p < 0.001 (b) Adjusted HbA1c SD was calculated using the first three or four HbA1c measurements (from recruitment to the end of year 2). Logrank tests Q2 vs Q1 p = 0.335; Q3 vs Q1 p = 0.397; Q4 vs Q1 p < 0.001
Discussion
Intrapersonal HbA1c variability, as expressed by SD of serially measured HbA1c, is a reliable and stable indicator to predict microalbuminuria development in type 2 diabetes patients. Our findings not only enrich previous knowledge about the impact of HbA1c variability on type 1 diabetes [13–15], but also provide the first empirical evidence for a possible association of HbA1c variability with the development of microalbuminuria in patients with type 2 diabetes. Furthermore, the current study also demonstrates that a 2 year estimate of HbA1c variability can be used as a short-term monitoring indicator for the progression of diabetic nephropathy. This prospective cohort study may provide useful guidance for clinical applications.
In addition to the mean value of serially measured HbA1c, HbA1c variability has been frequently shown to be associated with diabetic complications in patients with type 1 diabetes. Adult patients with higher HbA1c variability are more likely to develop cardiovascular events and albuminuria, as shown in the FinnDiane Study [13]. A similar association has also been observed in young type 1 diabetes patients. The Oxford Regional Prospective Study [14] and the Pittsburgh Epidemiology of Diabetes Complications Study [20] demonstrated that higher SD of HbA1c could predict microalbuminuria and coronary artery disease in type 1 diabetes patients younger than 17 years of age. Although the DCCT data [21, 22] could not associate microvascular complications with acute glucose variability derived from the intra-day 7-point blood glucose profile, they revealed a significant link between long-term glycaemic stability and the development of retinopathy and nephropathy by using the 9 year adjusted SD of HbA1c as an indicator [15].
To the best of our knowledge, HbA1c variability has never been used to predict clinical outcomes in patients with type 2 diabetes. Instability of the fasting glucose level has been reported as a risk factor for the development of complications in type 2 diabetes, but the results have been inconsistent. Intra-day glucose variability was shown to be associated with coronary artery disease in type 2 diabetes in a cross-sectional study [7]; however, it could not predict recurrent cardiovascular outcomes in the prospective HEART2D study [23]. The predictability of all-cause and cardiovascular mortality from 3-year fasting glucose variability in type 2 diabetes patients was shown in the Verona Diabetes Study [24, 25], but is still controversial with regard to an association between glucose variability and microvascular outcomes. A small-scale study (n = 130) conducted in Spain found that fasting glucose variability was an independent risk factor for retinopathy in patients with type 2 diabetes in a 5.2 year follow-up [26]; however, another Italian study (n = 746) could not confirm this association [4]. The inconsistency in the results of the aforementioned studies may be attributable to the influence of food intake on serial glucose measurements. A sporadically measured acute glucose profile may also not be able to reflect a long-term dynamic pattern of glycaemic variability. Moreover, the standard measurement of acute glucose fluctuation using continuous glucose monitoring or intra-day 7-point glucose profile to calculate SD or the mean amplitude of glycaemic excursion [27] is not clinically applicable for most non-insulin-using type 2 diabetes patients.
In this study, we used HbA1c, an indicator reflecting glycaemic control over 2–3 months [28], to detect microalbuminuria development. The mean and SD derived from three or four HbA1c measurements in 2 years were adequate to predict microalbuminuria. This differs from most previous studies, which used HbA1c variability from long-term observations, varying from 5 to 16 years [13, 15, 20], to delineate its impacts on diabetic complications in type 1 diabetes. A series of HbA1c measurements is able to reveal a general pattern of glycaemic control during a certain period for risk assessment. However, it is difficult to apply in clinical practice if the required data collection period for a reliable indicator is too long; clinicians usually need to be aware of their patients’ risks at the earliest possible time to make prompt clinical decisions. Apart from the fact that the long-term follow-up of serial HbA1c levels is essential for better diabetes care, our findings indicate the use of 2-year variability and mean of HbA1c to correlate microalbuminuria development is a clinically responsive indicator, which emphasises the importance of optimising an unfluctuating HbA1c early to prevent diabetic nephropathy.
High variability of HbA1c implies that poor glycaemic control does exist, at least temporarily, although the average HbA1c may be desirable in our patients. According to ‘metabolic memory’ theory [29], poor glycaemic control, even if it lasts only a short time, can be ‘memorised’ and still cause detrimental effects later on. Glucose fluctuations have been demonstrated to cause oxidant overproduction and endothelial dysfunction, and this effect is even stronger in stable higher glucose status in type 2 diabetic patients [30, 31]. The overproduction of reactive oxygen species is the common mediator of several hyperglycaemia-activated pathways in the pathogenesis of diabetic nephropathy. Patients with high HbA1c variability often live unhealthier lifestyles and, as shown in this study, may also intensify their vulnerability to the development of diabetic nephropathy. Furthermore, persistent epigenetic changes could be induced by transient hyperglycaemia [32], although other mechanisms of nephropathy caused by higher HbA1c variability are still unknown.
We have to be cautious when interpreting the results of this study because we may not be able to fully control all confounding factors in an observational study. To clarify the possibility of reverse causation, which is often suspected in observational cohort design, a randomised clinical trial is needed to further validate the effects of the proposed 2-year HbA1c variability on diabetic nephropathy. Other limitations of this study are the measurement issues. We checked HbA1c every 6 months, from which the glycaemic variability was derived; however, HbA1c is an indicator reflecting glycaemic control over 2–3 months. Therefore, the HbA1c variability in the current study may be an underestimate, owing to the inadequate monitoring period. Furthermore, for practical reasons, instead of measuring 24 h albumin excretion or early-morning first voiding urine, ACR was measured using morning spot urine in this study. This is acceptable according to the Kidney Disease Outcome Quality Initiative Clinical Practice Guideline [33], but may overestimate the incidence of microalbuminuria.
In conclusion, the current study is the first prospective study showing that higher HbA1c variability is associated with the development of microalbuminuria in type 2 diabetes patients. The predictability of the 2 year HbA1c SD for development of microalbuminuria conveys a clinical message that sustaining glycaemic control at the early stage is crucial for the management of type 2 diabetes.
Abbreviations
- ACR:
-
Albumin to creatinine ratio
- DMIDS:
-
Diabetes Management through an Integrated Delivery System project
- FinnDiane:
-
Finnish Diabetic Nephropathy study
References
The Diabetes Control and Complications Trial Research Group (1993) The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329:977–986
The Diabetes Control and Complications Trial Research Group (1995) The relationship of glycemic exposure (HbA1c) to the risk of development and progression of retinopathy in the diabetes control and complications trial. Diabetes 44:968–983
Stratton IM, Adler AI, Neil HA et al (2000) Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ 321:405–412
Zoppini G, Verlato G, Targher G et al (2009) Is fasting glucose variability a risk factor for retinopathy in people with type 2 diabetes? Nutr Metab Cardiovasc Dis 19:334–339
Snell-Bergeon JK, Roman R, Rodbard D et al (2010) Glycaemic variability is associated with coronary artery calcium in men with type 1 diabetes: the Coronary Artery Calcification in Type 1 Diabetes study. Diabet Med 27:1436–1442
Takao T, Ide T, Yanagisawa H et al (2011) The effects of fasting plasma glucose variability and time-dependent glycemic control on the long-term risk of retinopathy in type 2 diabetic patients. Diabetes Res Clin Pract 91:e40–42
Su G, Mi S, Tao H et al (2011) Association of glycemic variability and the presence and severity of coronary artery disease in patients with type 2 diabetes. Cardiovasc Diabetol 10:19
Zaccardi F, Pitocco D, Ghirlanda G (2009) Glycemic risk factors of diabetic vascular complications: the role of glycemic variability. Diabetes Metab Res Rev 25:199–207
Ceriello A, Ihnat MA (2010) ‘Glycaemic variability’: a new therapeutic challenge in diabetes and the critical care setting. Diabet Med 27:862–867
Kilpatrick ES, Rigby AS, Atkin SL (2010) For debate. Glucose variability and diabetes complication risk: we need to know the answer. Diabet Med 27:868–871
Siegelaar SE, Holleman F, Hoekstra JBL, DeVries JH (2010) Glucose variability; does it matter? Endocr Rev 31:171–182
Nalysnyk L, Hernandez-Medina M, Krishnarajah G (2010) Glycaemic variability and complications in patients with diabetes mellitus: evidence from a systematic review of the literature. Diabetes Obes Metab 12:288–298
Waden J, Forsblom C, Thorn LM et al (2009) A1C variability predicts incident cardiovascular events, microalbuminuria, and overt diabetic nephropathy in patients with type 1 diabetes. Diabetes 58:2649–2655
Marcovecchio ML, Dalton RN, Chiarelli F, Dunger DB (2011) A1C variability as an independent risk factor for microalbuminuria in young people with type 1 diabetes. Diabetes Care 34:1011–1013
Kilpatrick ES, Rigby AS, Atkin SL (2008) A1C variability and the risk of microvascular complications in type 1 diabetes: data from the Diabetes Control and Complications Trial. Diabetes Care 31:2198–2202
Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HA (2008) 10-year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med 359:1577–1589
Huang MC, Hsu CC, Wang HS, Shin SJ (2010) Prospective randomized controlled trial to evaluate effectiveness of registered dietitian-led diabetes management on glycemic and diet control in a primary care setting in Taiwan. Diabetes Care 33:233–239
Hsu CC, Chang HY, Huang MC et al (2011) Association between insulin resistance and development of microalbuminuria in type 2 diabetes: a prospective cohort study. Diabetes Care 34:982–987
Haller H, Ito S, Izzo JL Jr et al (2011) Olmesartan for the delay or prevention of microalbuminuria in type 2 diabetes. N Engl J Med 364:907–917
Prince CT, Becker DJ, Costacou T, Miller RG, Orchard TJ (2007) Changes in glycaemic control and risk of coronary artery disease in type 1 diabetes mellitus: findings from the Pittsburgh Epidemiology of Diabetes Complications Study (EDC). Diabetologia 50:2280–2288
Siegelaar SE, Kilpatrick ES, Rigby AS et al (2009) Glucose variability does not contribute to the development of peripheral and autonomic neuropathy in type 1 diabetes: data from the DCCT. Diabetologia 52:2229–2232
Kilpatrick ES, Rigby AS, Atkin SL (2006) The effect of glucose variability on the risk of microvascular complications in type 1 diabetes. Diabetes Care 29:1486–1490
Siegelaar SE, Kerr L, Jacober SJ, Devries JH (2011) A decrease in glucose variability does not reduce cardiovascular event rates in type 2 diabetic patients after acute myocardial infarction: a reanalysis of the HEART2D study. Diabetes Care 34:855–857
Muggeo M, Verlato G, Bonora E et al (1997) Long-term instability of fasting plasma glucose, a novel predictor of cardiovascular mortality in elderly patients with non-insulin-dependent diabetes mellitus: the Verona Diabetes Study. Circulation 96:1750–1754
Muggeo M, Zoppini G, Bonora E et al (2000) Fasting plasma glucose variability predicts 10-year survival of type 2 diabetic patients: the Verona Diabetes Study. Diabetes Care 23:45–50
Gimeno-Orna JA, Castro-Alonso FJ, Boned-Juliani B, Lou-Arnal LM (2003) Fasting plasma glucose variability as a risk factor of retinopathy in type 2 diabetic patients. J Diabetes Complications 17:78–81
Monnier L, Colette C, Owens DR (2008) Glycemic variability: the third component of the dysglycemia in diabetes. Is it important? How to measure it? J Diabetes Sci Technol 2:1094–1100
Nathan DM, Turgeon H, Regan S (2007) Relationship between glycated haemoglobin levels and mean glucose levels over time. Diabetologia 50:2239–2244
Nathan DM, Cleary PA, Backlund J-YC et al (2005) Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N Engl J Med 353:2643–2653
Monnier L, Mas E, Ginet C et al (2006) Activation of oxidative stress by acute glucose fluctuations compared with sustained chronic hyperglycemia in patients with type 2 diabetes. JAMA 295:1681–1687
Ceriello A, Esposito K, Piconi L et al (2008) Oscillating glucose is more deleterious to endothelial function and oxidative stress than mean glucose in normal and type 2 diabetic patients. Diabetes 57:1349–1354
El-Osta A, Brasacchio D, Yao D et al (2008) Transient high glucose causes persistent epigenetic changes and altered gene expression during subsequent normoglycemia. J Exp Med 205:2409–2417
National Kidney Foundation KDOQI Clinical Practice Guidelines. Available from http://www.kidney.org/professionals/kdoqi/guidelines_ckd/p5_lab_g5.htm. Accessed 5 May 2012
Funding
This study was supported by the National Health Research Institutes, which had no role in the study design, data analysis, data interpretation or writing of the manuscript.
Contribution statement
CCH and SJS designed the study and conceived the idea. CCH, HYC SJH, TYT, and YSL analysed data and interpreted results. MCH and YCY collected and maintained the research data. CCH and SJS drafted the article. HYC, MCH, SJH, YCY YSL, and TYT critically revised the article for important intellectual content. All authors reviewed the manuscript and had final responsibility for the decision to submit for publication.
Duality of interest
All authors declare that there is no duality of interest associated with this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hsu, C.C., Chang, H.Y., Huang, M.C. et al. HbA1c variability is associated with microalbuminuria development in type 2 diabetes: a 7-year prospective cohort study. Diabetologia 55, 3163–3172 (2012). https://doi.org/10.1007/s00125-012-2700-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-012-2700-4