Abstract
Aims/hypothesis
The purpose of this study was to examine the association between urbanisation-related factors and diabetes prevalence in China.
Methods
Anthropometry, fasting blood glucose (FBG) and community-level data were collected for 7,741 adults (18–90 years) across 217 communities and nine provinces in the 2009 China Health and Nutrition Survey to examine diabetes (FBG ≥7.0 mmol/l or doctor diagnosis). Sex-stratified multilevel models, clustered at the community and province levels and controlling for individual-level age and household income were used to examine the association between diabetes and: (1) a multicomponent urbanisation measure reflecting overall modernisation and (2) 12 separate components of urbanisation (e.g., population density, employment, markets, infrastructure and social factors).
Results
Prevalent diabetes was higher in more-urbanised (men 12%; women 9%) vs less-urbanised (men 6%; women 5%) areas. In sex-stratified multilevel models adjusting for residential community and province, age and household income, there was a twofold higher diabetes prevalence in urban vs rural areas (men OR 2.02, 95% CI 1.47, 2.78; women, OR 1.94, 95% CI 1.35, 2.79). All urbanisation components were positively associated with diabetes, with variation across components (e.g. men, economic and income diversity, OR 1.42, 95% CI 1.20, 1.66; women, transportation infrastructure, OR 1.18, 95% CI 1.06, 1.32). Community-level variation in diabetes was comparatively greater for women (intraclass correlation [ICC] 0.03–0.05) vs men (ICC ≤0.01); province-level variation was greater for men (men 0.03–0.04; women 0.02).
Conclusions/interpretation
Diabetes prevention and treatment efforts are needed particularly in urbanised areas of China. Community economic factors, modern markets, communications and transportation infrastructure might present opportunities for such efforts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Over the past decade, the prevalence of type 2 diabetes in China has more than doubled from approximately 3% in 1994 to 7–10% in 2008 [1, 2], which is of concern as China is home to more than 1.3 billion people and comprises one-fifth of the world's population. Rapid urbanisation, economic growth and economic and healthcare reforms have been implicated in the increased diabetes prevalence [3–6]. Urbanisation may influence diabetes prevalence through increased time engaged in sedentary lifestyle behaviours and greater consumption of animal products, high-fat foods and highly processed foods [7, 8]. Yet, little is known about which specific elements of urbanisation are most associated with diabetes.
Most of the published literature relies on dichotomous contrasts between rural and urban areas. However, in China there is complexity and heterogeneity between and within urban and rural communities [9]. For example, in China's uneven economic transition, some rural areas became larger than small cities, while other urban areas lost services and physical infrastructure with development [9]. Provincial and regional differences in services and infrastructure due to decentralised healthcare and economic systems are exacerbated because of the urbanisation process [5, 6]. Research in China suggests that a dichotomous classification of urban and rural areas inadequately captures this heterogeneity, whereas a multidimensional measure that encompasses healthcare, economic systems, services and infrastructure adequately characterises variation across the spectrum of urbanicity [9]. While it is important to understand the association between overall urbanisation and diabetes prevalence, understanding the elements of urbanisation most associated with diabetes can inform community-level diabetes prevention and treatment efforts.
In this paper, we capitalise upon unique population-based, community- and individual-level data from the China Health and Nutrition Survey (CHNS) [10] to examine the association between urbanisation and diabetes using a validated, multidimensional urbanisation index [9]. This urbanisation index includes a total score as well as 12 component measures (reflecting a diverse range of factors such as healthcare, economic systems, services and infrastructure) that improve with urbanisation. In addition, we use multilevel modelling to account for the inherent interdependence between community-level factors and individual health outcomes among members of the same community or province [11]. We hypothesise that: (1) total urbanisation is positively associated with diabetes prevalence and (2) each of the 12 components of urbanisation is separately and differentially associated with diabetes prevalence.
Methods
CHNS
The CHNS collected health data in 228 communities in nine diverse provinces (Guangxi, Guizhou, Heilongjiang, Henan, Hubei, Hunan, Jiangsu, Liaoning and Shandong) throughout China from 1989 to 2009 in eight rounds of surveys. The 2009 survey included fasting blood collection for the first time. Using multistage, random-cluster sampling, counties in the nine provinces were stratified by income and weighted sampling was used to randomly select four counties in each province. Villages and small towns within counties and urban and suburban neighbourhoods within cities were selected randomly into primary sampling units defined politically and geographically based on State Statistical Office definitions [12]. The surveyed provinces represent 56% of the Chinese population. Survey procedures have been described elsewhere [10]. The study was approved by the Institutional Review Board at the University of North Carolina at Chapel Hill, the China–Japan Friendship Hospital, Ministry of Health and the Institute of Nutrition and Food Safety, China Centers for Disease Control. Individuals gave informed consent for participation.
Analysis sample
The 2009 examination surveyed a total of 8,597 adult respondents aged 18 or older; 402 were not fasting before blood withdrawal and 58 were pregnant, resulting in a total of 8,137 individuals with fasting blood. Of these, 221 were missing anthropometry data, 44 were missing laboratory results and 130 were missing household income data, resulting in 7,742 with anthropometry and clinical examination information. One person was excluded from the analysis because he was the only person in his community, resulting in an analytical sample of 7,741. There were no statistically significant differences in the total 2009 sample vs the analytical sample in sex, urbanisation or BMI, although the individuals in the analytical sample had a higher age and a larger household income.
Dependent variables
After an overnight fast, blood was collected by venipuncture (12 ml). Whole blood was immediately centrifuged and the serum was tested for glucose. Glucose was measured with a Hitachi 7600 analyser using a glucose oxidase phenol 4-aminoantipyrine peroxidase kit (GOD-PAP; Randox, Crumlin, UK). Self-report questionnaires were used to elicit information regarding medical history and current medication use. Diabetes was defined according to the WHO 2006 guidelines as having a fasting blood glucose (FBG) measurement ≥7.0 mmol/l (n = 364) or answering ‘yes’ to the question ‘has a doctor ever told you that you suffer from diabetes?’ (n = 229) [13].
Main exposure: urbanisation index and its components
Urbanisation was measured using an urbanisation index based on household- and community-level data representing 12 features of the community environment. Components related to healthcare, economic systems, services and infrastructure were chosen on conceptual and empirical grounds that the 12 components defined and distinguished levels of urbanicity (Table 1). The multicomponent scale is particularly relevant in areas such as China where rapid urbanisation has occurred with spatial and temporal variation in the types of changes occurring across regions. Jones-Smith et al [9] created the multicomponent urbanisation index for China using established scaling procedures from the psychometric literature to measure urban features on a continuum. Each urbanisation component was comprised of several variables. Scoring for each component was based upon data distribution to maintain adequate spread through the range of possible values and to set each component's median value at half of the total possible points. Points were allocated on the basis of: presence (or number) of infrastructure or facilities within communities; the percentage of households within communities with specific amenities or the average proportion of individuals (or households) at specific education (or household income) levels. Once points were aggregated, each component was rescaled so that the highest possible value a community could attain was ten points. Scoring of the overall index was based on a maximum of ten points for each of 12 equally weighted components.
The selection of variables and the scoring strategy were examined for content validity [9]. In addition, Jones-Smith et al [9] assessed unidimensionality and multidimensionality using exploratory factor analysis and assessed test–retest reliability (α = 0.85–0.89 across all study years) and temporal stability (r = 0.90–0.94 between study years). The authors assessed criterion-related validity (κ = 69–77% across study years) using official administratively based government classification of urban/rural and construct validity using regression analysis, finding a highly statistically significant association between the urbanisation index and household per capita income. Findings from this evaluation suggest that the multicomponent measure performs better than the dichotomous administrative classification of urban and rural in models predicting health outcomes [9].
In the first stage of analysis, we were primarily interested in whether the overall multicomponent measure of urbanisation was associated with diabetes prevalence. Given that the 12 components comprising the urbanisation index interact synergistically to reflect urbanisation, a continuous measure does not adequately capture overall urbanisation. Thus, we categorised total urbanisation (range 30.4–106.6) into tertiles representing low (<59.0), medium (59.0–82.2) and high (≥82.3) levels. In the second stage of analysis, we examined whether diabetes prevalence varied across the 12 urbanisation components. The components were scored separately; one point represents a higher level of urbanisation for each component. To facilitate comparison across the components, we present ORs comparing high (75th percentile) vs low (25th percentile) levels of each of the 12 distinct and equally weighted urbanisation index components (Table 1).
Individual- and community-level factors
Age and sex were self-reported. Income was reported at the household level. Height was measured without shoes to the nearest 0.2 cm using a portable SECA stadiometer and weight was measured without shoes and in light clothing to the nearest 0.1 kg on a calibrated beam scale. Overweight and obesity were reported according to WHO classifications (25–30 kg/m2 and ≥30 kg/m2, respectively) [14] and the Chinese classifications (24–28 kg/m2 and ≥28 kg/m2, respectively) [15]. Both sets of criteria are presented: the WHO classification for comparison across published studies and the Chinese classification for an internal reference.
Statistical analysis
All analyses were conducted in Stata 12 (Stata, College Station, TX, USA). In descriptive analyses, we examined individual-level characteristics, total urbanisation level and each of the 12 urbanisation components across the nine CHNS provinces. We tested sex-specific differences in individual-level characteristics across low, medium and high urbanisation and across the nine CHNS provinces by ANOVA for continuous outcomes and χ2 tests for categorical outcomes. In addition, we tested differences in medians (due to the skewed distributions of the urbanisation index components) using the K-sample equality of medians test. The significance level for all descriptive statistics was set at p < 0.05.
Given the high prevalence of undiagnosed diabetes in China [2], we examined the prevalence of undiagnosed and diagnosed diabetes by province and urbanisation levels. Using the question ‘Has a doctor ever told you that you suffer from diabetes?’, a ‘yes’ response was coded as diagnosed diabetes and a ‘no’ response plus an FBG ≥7.0 mmol/l was coded as undiagnosed diabetes. The two mutually exclusive categories together represent total diabetes used for the central analyses.
To examine diabetes prevalence across urbanisation levels, we used multilevel logistic regression models, with individual-level age and household income as fixed effects and with the community and province of residence as random effects. Given differences across regions of China in lifestyle, climate and economic factors, we assessed whether northern (Lianoning, Heilongjiang, Shandong and Henan) and southern (Jiangso, Jubei, Hunan, Guangxi and Guizho) region confounded the association between urbanisation and diabetes prevalence. Geographic region did not meet the 10% change-in-estimate criterion of confounding, so it was not included in the final models. However, variation due to geographic region was captured by the province random effect, which accounted for clustering in lifestyle, climate and economic factors across China.
We did not include BMI in the final models on the basis that it is a causal intermediate on the pathway from urbanisation to diabetes and, as such, could potentially bias results [16]. However, in a secondary analysis we assessed the confounding by BMI of the association between urbanisation and diabetes. Findings indicated that BMI did not meet the 10% change-in-estimate criterion of confounding, thus BMI was not included in the final models (see electronic supplementary material [ESM] Table 1).
Likelihood ratio tests showed a statistically significant sex difference in the association between the education and income diversity urbanisation component with diabetes prevalence (p < 0.05), thus all models were stratified by sex. When age was categorised as <50 or ≥50 years, there was no evidence for effect modification by age in the association between urbanisation and diabetes prevalence (men χ 2 = 5.11, p = 0.08; women χ 2 = 0.64, p = 0.73). Tests for the interaction between age and the 12 separate urbanisation index components yielded similar results (p > 0.05), showing no empirical basis for effect modification by age, thus analyses were not age-stratified.
First, we examined prevalence of diabetes across low, medium and high urbanisation to assess whether levels of the overall multicomponent urbanisation measure was significantly associated with diabetes (statistical significance set at p < 0.05). Second, using the individual component measures as mean-centred continuous variables, we examined whether each of the 12 components of urbanisation was separately associated with diabetes. Given colinearity between the 12 urbanisation index components (correlation ranging from 0.2 to 0.7) and interest in assessing the associations across urbanisation components, we constructed 12 separate models per sex for each of the 12 urbanisation index components, resulting in a total of 24 models. We used the Bonferroni correction for multiple comparisons with a type 1 error rate of 0.05 and 24 models (p value set at 0.002). Half of the components were linearly related to diabetes prevalence on the logit scale; thus, all components were retained as linear variables for consistency and comparability across models. The components are scored independently and vary in their distribution across provinces and in the total sample. To facilitate comparison across the components and for comparability with the total urbanisation measure, we present ORs with 95% CIs comparing the 75th (high) vs the 25th (low) percentile for each of the 12 urbanisation components. Variance and SE of the random effects are presented to characterise community- and province-level variation in diabetes prevalence. We calculated the intraclass correlation coefficients (ICCs) at the community and province levels to examine the relative contribution of province, community and individual levels to diabetes prevalence.
Sensitivity analysis
First, we replicated our analyses comparing two alternative diabetes diagnostic criteria ([1] HbA1c ≥6.5% [48 mmol/mol] and [2] a combination of HbA1c ≥6.5% [48 mmol/mol] and FBG ≥7.0 mmol/l) with the diabetes diagnostic criterion used in the primary analyses (FBG ≥7.0 mmol/l) (see ESM Tables 2 and 3).
Second, because diabetes prevalence across levels of the urbanisation index has not been compared with a traditional urban/rural dichotomy, we examined differences in diabetes according to the administratively defined urban/rural classification from the CHNS.
Results
Diabetes prevalence differed across low, medium and high areas of urbanisation, with highest prevalence in highly urbanised areas (Table 2). In addition, diabetes prevalence differed by sex (p = 0.001, χ2 test), with a higher mean prevalence across all levels of urbanisation in men (8.7% [SE 0.5]) vs women (6.7% [0.4]).
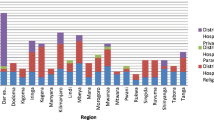
Across provinces, diabetes prevalence ranged from 4.8% to 12.1% (Table 3). Total urbanisation and the 12 urbanisation components varied across provinces, indicating a differential degree of urbanisation across the provinces.
Over half of the individuals with diabetes in this study were not previously diagnosed by a doctor (ESM Table 4). The proportion of the sample with undiagnosed and diagnosed diabetes differed across urbanisation level and province.
High vs low urbanisation was associated with an approximate twofold higher diabetes prevalence (men OR 2.02, 95% CI 1.47, 2.78; women OR 1.94, 95% CI 1.35, 2.79) after controlling for individual-level factors and accounting for clustering at the community and province levels (Table 4). In general, higher urbanisation across the 12 components was positively associated with diabetes prevalence, albeit with variation in statistical significance (ESM Figs 1 and 2). Comparatively stronger associations were observed for men.
Low variance and ICC at the community level for men suggests low variation in diabetes across communities (Table 4). In contrast, community-level variance was larger in women than men, and women had a higher ICC at the community level than at the province level. Thus, for women, variation in diabetes prevalence across communities remained even after urbanisation components were taken into account.
Although BMI was not an empirical confounder of the association between urbanisation and diabetes prevalence, findings from models with adjustment for BMI are shown in ESM Table 2. With BMI in the model, ORs were somewhat attenuated, but in general showed the same pattern of direction and statistical significance.
While models for total diabetes prevalence are presented in Table 4, we also considered associations with urbanisation for diagnosed and undiagnosed diabetes (ESM Table 5). We observed a similar pattern of association for diagnosed diabetes at high vs low urbanisation (men OR 5.86, 95% CI 3.08, 11.15; women OR 4.03, 95% CI 2.09, 7.78) after controlling for individual-level factors and accounting for clustering at the community and province levels. In contrast, the prevalence of undiagnosed diabetes did not differ by high vs low urbanisation level (men OR 1.25, 95% CI 0.84, 1.85; women OR 1.38, 95% CI 0.88, 2.17).
Sensitivity analyses related to diagnostic criteria for diabetes suggest that the use of HbA1c alone (ESM Table 4), a combination of high HbA1c and/or FBG (ESM Table 5), and FBG alone (Table 4) yielded findings similar in direction and magnitude.
In sensitivity analyses, we also compared an administratively defined classification of urban vs rural communities to the multidimensional urbanisation measure used in the central analysis. ORs for diabetes prevalence suggest a similar direction and magnitude for high vs low urbanisation using the traditional (men OR 1.54, 95% CI 1.21, 1.97; women OR 1.38, 95% CI 1.04, 1.84) vs multidimensional (men OR 2.02, 95% CI 1.47, 2.78; women OR 1.94; 95% CI 1.35, 2.79) measure.
Discussion
Our findings suggest that diabetes prevalence is elevated across areas of low and high urbanisation in China. However, using a detailed and multidimensional measure of urbanisation, we found that individuals living in more-urbanised areas had a twofold higher diabetes prevalence than individuals living in less-urbanised areas, even after community and province of residence, age, sex and household income were accounted for. These findings are concerning given the vast number of affected individuals. China is home to the world's largest population and approximately 80% of diabetes deaths occur in low- and middle-income countries [17]. Although we observed higher diabetes prevalence in more-urbanised areas, the relatively high level of diabetes in less-urbanised areas suggests that these areas are still in need of attention. We also observed variation in diabetes prevalence across specific components of urbanisation. Our findings suggest that community economic factors, modern markets, communications and transportation infrastructure might be areas deserving of further research and could potentially be the focus of community-level diabetes prevention efforts.
Although others have examined disparities in diabetes [4, 18, 19] and other have examined noncommunicable diseases [2, 20, 21] across regions of China using traditional measures of urbanisation, our analysis improves on these studies in three key ways. First, the CHNS intentionally sampled the capital city and rural areas within each province to span the breadth of economic development within provinces and thus provides substantial variation across more- and less-urbanised areas. Second, our multidimensional measure of urbanisation, which has been tested for reliability and validity [9], captures heterogeneity in a variety of services and infrastructure within and between high- and low-urbanised areas. This multidimensional measure is particularly relevant in China or other countries undergoing rapid and asymmetric urbanisation, which is inadequately captured by dichotomous classification of urbanicity [22–24]. Having observed the separate associations between the 12 urbanisation index components and diabetes prevalence, we suggest that some potentially modifiable factors, namely community economic factors, modern markets, communications and transportation infrastructure, might be foci for further research and community-level policy.
Third, we used multilevel modelling to account for the clustering of individuals at the community and province levels. This technique is critical given our research question, as well as the nature of the sampling method, and the fact that the main exposures of interest are measured at the community level [11]. Indeed, descriptive statistics suggested differences in the distribution of urbanisation components and diabetes prevalence across provinces. Accounting for these dependencies via random-effects modelling did not attenuate associations between urbanisation and diabetes. Therefore, although community and province of residence were associated with differential diabetes prevalence in China, unmeasured factors remain that might influence diabetes.
We observed variation in the level of urbanisation and prevalence of diabetes across provinces of China. The total measure of urbanisation captures synergies among its components across low-, medium- and high-urbanisation levels, and we observed higher prevalence of diabetes in high- vs low-urbanised areas of China. Our findings across the 12 urbanisation components provide additional information not captured in the overall measure. For example, we observed substantial variation in economy-related factors across provinces and increased diabetes prevalence in communities with high vs low economic activity, education, and education and income diversity. Together, these findings might be attributed to limited/regional free trade agreements, economic development that has favoured eastern China and port cities [25], and a decentralised healthcare system that determines health regulation and infrastructure at community and province levels [5, 6]. Modern markets (which in our study included supermarkets and fast-food restaurants) have also increased in number with economic development [26] and were positively associated with diabetes prevalence. Our findings, namely that multiple economy-related factors are positively associated with diabetes prevalence, suggest that the largest disease burden may be found in wealthier and more modernised areas of China.
Given inter-correlation across the 12 urbanisation components, combining them into a single model was not possible. Furthermore, we were explicitly interested in the net effect of each individual component. Looking at the associations between high vs low levels of the 12 urbanisation components with diabetes prevalence highlights modifiable factors with potential for community-level efforts to prevent and treat diabetes. While our findings are suggestive, further research on these community-level factors is needed before incorporating such factors into policy and programmes. Nonetheless, community-level factors, such as transportation and communication, which were positively associated with diabetes, have been useful for addressing chronic diseases in other developing-country contexts. For example, in Brazil, changes in transportation infrastructure have had an impact on population-level physical activity [27, 28]. In Pakistan, a communications-oriented health education campaign has positively affected nutrition-related chronic disease awareness [29]. Increased alcohol taxes in Thailand have been associated with reductions in alcohol-related mortality [30]. In China, community-level tobacco cessation efforts have been associated with reductions in smoking [31]. Thus, community-level strategies offer promise in deterring lifestyle-related diseases such as diabetes.
In general, associations between the 12 urbanisation index components and diabetes prevalence appeared to be stronger in men. The extent to which this difference represents a differential relationship between community-level factors and diabetes by sex or whether other factors (e.g. educational and economic opportunities for men vs women) drive this difference is unknown. In the CHNS, a comparatively stronger association between urbanisation and BMI for men has been shown [32]; therefore, it is possible that lifestyle in urban vs rural areas differs by sex.
In contrast, we did not find differences in the association between urbanisation and diabetes prevalence by age. Cumulative exposure to the urban environment has been shown to be related to increased prevalence of overweight and noncommunicable diseases [33]; however, because urbanisation is a relatively recent and ongoing phenomenon in China, cumulative exposure to the urban environment may not be greater in older people, so differential associations between urbanisation and diabetes by age may not be apparent.
There are limitations to the current study that should be noted: (1) the main exposure variables are based on community-level data and while our urbanisation index measure includes diverse and detailed components of urbanisation, elements such as local food prices and individual-level exposures are not captured; (2) our cross-sectional analysis does not take into account changes in urbanisation over time; (3) diabetes prevalence is influenced by a number of factors in addition to incidence; thus, differential mortality among individuals with diagnosed or undiagnosed diabetes may influence prevalence of diabetes (e.g. diabetes prevalence may be artificially lower in areas with higher mortality rates [34]). However, our findings do provide insight related to province- and community-level factors that might be targets for policy in China and other recently urbanised countries. Although we used just one FBG measure to classify individuals with diabetes, this is standard epidemiological practice for population-based studies. While FBG and HbA1c capture different populations of people with diabetes [35, 36], we found consistency in results using HbA1c and FBG in terms of the effect size and direction of association with overall urbanisation and its components, albeit with some differences by sex. Researchers in Korea found a greater proportion of women with diabetes when using HbA1c vs FBG as the diagnosis criterion [37]; however, the reasons why HbA1c would capture more women with diabetes are unknown. We are not able to distinguish type 1 from type 2 diabetes in our sample, but the incidence of type 1 diabetes in China is among the lowest in the world, with an estimate of 0.1 per 100,000 each year [38]. Due to differences between the WHO and Chinese BMI cut-off points for overweight and obesity, both were included in Table 2. While the internationally recognised WHO cut-off points facilitate comparison across studies and nations, the lower BMI Chinese cut-off points [15] reflect the higher noncommunicable disease risk at lower BMI in Chinese populations [14].
Conclusion
Diabetes is becoming a major public health concern across China. Using a multidimensional measure of urbanisation, which captures healthcare, economic systems, services and infrastructure, we observed a twofold higher prevalence of diabetes in more- vs less-urban areas, even after community and province of residence, age, sex and household income were accounted for. We also observed that high (i.e. more urbanised) values for some components of urbanisation, particularly community economic factors, modern markets, communications and transportation infrastructure, were separately and positively associated with diabetes. As such, these factors might present opportunities for community-level diabetes prevention efforts.
Abbreviations
- CHNS:
-
China Health and Nutrition Survey
- FBG:
-
Fasting blood glucose
- ICC:
-
Intraclass correlation coefficient
References
Yoon K-H, Lee J-H, Kim J-W et al (2006) Epidemic obesity and type 2 diabetes in Asia. Lancet 368:1681–1688
Yang W, Lu J, Weng J et al (2010) Prevalence of diabetes among men and women in China. N Engl J Med 362:1090–1101
Popkin BM, Horton S, Kim S, Mahal A, Shuigao J (2001) Trends in diet, nutritional status, and diet-related noncommunicable diseases in China and India: the economic costs of the nutrition transition. Nutr Rev 59:379–390
Tang S, Meng Q, Chen L, Bekedam H, Evans T, Whitehead M (2008) Tackling the challenges to health equity in China. Lancet 372:1493–1501
Blumenthal D, Hsiao W (2005) Privatization and its discontents—the evolving Chinese health care system. N Engl J Med 353:1165–1170
Liu S, Griffiths SM (2011) From economic development to public health improvement: China faces equity challenges. Public Health 125:669–674
Popkin BM (1999) Urbanization, lifestyle changes and the nutrition transition. World Dev 27:1905–1916
Popkin BM, Gordon-Larsen P (2004) The nutrition transition: worldwide obesity dynamics and their determinants. Int J Obes 28:S2–S9
Jones-Smith J, Barry M, Popkin BM (2011) Understanding community context and adult health changes in China: development of an urbanicity scale. Soc Sci Med 71:1436–1446
Popkin BM (2010) Cohort profile: the China Health and Nutrition Survey—monitoring and understanding socio-economic and health change in China, 1989–2011. Int J Epidemiol 39:1435–1440
Diez-Roux AV (2000) Multilevel analysis in public health research. Annu Rev Public Health 21:171–192
National Bureau of Statistics of China. Definitions. Available from http://www.stats.gov.cn/english/classificationsmethods/definitions/t20020419_402787586.htm, accessed 21 May 2009
WHO (2006) Definition and diagnosis of diabetes mellitus and intermediate hyperglycemica. World Health Oranization/International Diabetes Federation, Geneva
WHO Expert Consultation (2004) Appropriate body mass index for Asian populations and its implications for policy and intervention strategies. Lancet 363:157–163
Working group on Obesity in China. Department of Disease Control and Ministry of Health (2004) The guidelines for prevention and control of overweight and obesity in Chinese adults. Biomed Environ Sci 17:1–35
VanderWeele TJ (2010) Bias formulas for sensitivity analysis for direct and indirect effects. Epidemiology 21:540–551
WHO (2011) The global status report on noncommunicable diseases 2010. World Health Organization, Geneva, p 176
Zhang X, Kanbur R (2005) Spatial inequality in education and health care in China. China Econ Rev 16:189–204
Zheng X, Song X, Chen G et al (2011) Health inequalities during 20 years of rapid economic development in China (1980-2000): a mortality analysis. Biomed Environ Sci 24:329–334
Yang G, Kong L, Zhao W et al (2008) Emergence of chronic non-communicable diseases in China. Lancet 372:1697–1705
Wagner K-H, Brath H (2012) A global view on the development of non communicable diseases. Prev Med 54(Suppl 1):S38–S41
Allender S, Foster C, Hutchinson L, Arambepola C (2008) Quantification of urbanization in relation to chronic disease in developing countries: a systematic review. J Urban Health 85:938–951
McDade TW, Adair LS (2001) Defining the "urban" in urbanization and health: a factor analysis approach. Soc Sci Med 53:55–70
Mongomery MR, Ezeh AC (2005) The health of urban populations in developing countries: an overview. In: Galea S, Vlahov D (eds) Handbook of urban health: populations, methods, and practice. Springer, New York, pp 201–222
Zhang X, Zhang KH (2003) How does globalisation affect regional inequality within a developing country? Evidence from China. J Dev Stud 39:47–67
Popkin B (2008) Will China's nutrition transition overwhelm its health care system and slow economic growth. Health Aff 27:1064–1076
Matsudo VK, Matsudo SM, Araujo TL, Andrade DR, Oliveira LC, Hallal PC (2010) Time trends in physical activity in the state of São Paulo, Brazil: 2002–2008. Med Sci Sports Exerc 42:2231–2236
Matsudo V (2012) The role of partnerships in promotic physical activity: the experience of Agita São Paulo. Health Place 18:121–122
Nishtar S (2004) Newspaper articles as a tool for cardiovascular prevention programs in a developing country. J Health Commun 9:355–369
Lin CM, Liao CM, Li CY (2011) A time-series analysis of alcohol tax policy in relation to mortality from alcohol attributed causes in Taiwan. J Commun Health 36:986–991
Yang T, Xu X, Rockett IRH, Guo W, Zhou H (2011) Effects of household, workplace, and public plase smoking restrictions on smoking cessation. Health Place 17:954–960
Wang H, Du S, Zhai F, Popkin B (2007) Trends in the distribution of body mass index among Chinese adults, aged 20–45 years (1989–2000). Int J Obes 31:272–278
Sobngwi E, Mbanya JC, Unwin NC et al (2004) Exposure over the life course to an urban environment and its relation with obesity, diabetes, and hypertension in rural and urban Cameroon. Int J Epidemiol 33:769–776
Congdon P (2007) A model for spatial variations in life expectancy: mortality in Chinese regions in 2000. Int J Health Geogr 6:16
Carson AP, Reynolds K, Fonseca VA, Muntner P (2010) Comparison of A1C and fasting glucose criteria to diagnose diabetes among U.S. adults. Diabetes Care 33:95–97
Mann DM, Carson AP, Shimbo D, Fonseca V, Fox CS, Muntner P (2010) Impact of A1C screening criterion on the diagnosis of pre-diabetes among U.S. adults. Diabetes Care 33:2190–2195
Kim C-H, Kim H-K, Bae S-J, Park J-Y, Lee K-U (2011) Discordance between fasting glucose-based and hemoglobin A1c-based diagnosis of diabetes mellitus in Koreans. Diabetes Res Clin Pract 91:e8–e10
The Diamond Project Group (2006) Incidence and trends of childhood type 1 diabetes worldwide 1990–1999. Diabet Med 23:857–866
Acknowledgements
The authors are thankful to J. Jones-Smith (University of California San Francisco) for guidance regarding the urbanisation index and S. Albrecht (Carolina Population Center) for helpful comments on an earlier draft of the manuscript.
Funding
This work was supported by NIH: NHLBI (R01HL108427) and NIDDK (R21DK089306). NIH had no role in the design and conduct of the study, the collection, management, analysis and interpretation of the data or in the preparation, review or approval of the manuscript. This research uses data from the CHNS, funded by NIH: NICHD (R01-HD30880), although no direct support was received in the form of a grant for this analysis. J. B. Meigs is supported by National Institute for Diabetes and Digestive and Kidney Diseases (NIDDK) K24 DK080140. S. M. Attard is funded by NICHD-National Research Service Award (NRSA) (5T32DK007686-19). The authors are grateful to the Carolina Population Center (R24 HD050924) for general support.
Duality of interest
The authors declare that there is no duality of interest associated with this manuscript.
Contribution statement
All authors contributed to conception and design and interpretation of data, SMA, PGL and AHH contributed to data analysis, BMP and PGL contributed to the acquisition of data, SMA and PGL drafted the manuscript and AHH, EJMD, BMP and JBM contributed to critical revision of the manuscript. All authors have approved the final version of the manuscript. SMA and PGL had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary materials
Below is the link to the electronic supplementary material.
ESM Fig. 1
(PDF 79 kb)
ESM Fig. 2
(PDF 95 kb)
ESM Table 1
(PDF 94 kb)
ESM Table 2
(PDF 94 kb)
ESM Table 3
(PDF 97 kb)
ESM Table 4
(PDF 78 kb)
ESM Table 5
(PDF 76 kb)
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Attard, S.M., Herring, A.H., Mayer-Davis, E.J. et al. Multilevel examination of diabetes in modernising China: what elements of urbanisation are most associated with diabetes?. Diabetologia 55, 3182–3192 (2012). https://doi.org/10.1007/s00125-012-2697-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-012-2697-8