Abstract
Psychological stress predisposes our body to several disorders. Understanding the cellular and molecular mechanisms involved in the physiological responses to psychological stress is essential for the success of therapeutic applications. New studies show, by using in vivo inducible Cre/loxP-mediated approaches in combination with pharmacological blockage, that sympathetic nerves, activated by psychological stress, induce brown adipocytes to produce IL-6. Strikingly, this cytokine promotes gluconeogenesis in hepatocytes, that results in the decline of tolerance to inflammatory organ damage. The comprehension arising from this research will be crucial for the handling of many inflammatory diseases. Here, we review recent advances in our comprehension of the sympathetic nerve-adipocyte axis in the tissue microenvironment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stressful psychological circumstances are frequent in our daily life. The “fight or flight response” is presently well-defined as an evolutionary conserved physiological reaction of the organism to the eminent encounter with a stressor (threat or harmful event) [1]. This process was initially described at the first half of the twentieth century by the American physiologist Walter Bradford Cannon [2]. This phenomenon aims to preserve or restore organism homeostasis in vertebrates [3]. It is characterized by several physiological manifestations, including increase of respiratory and heart rates, rise in temperature, release of stocked energy, elevation in blood supply to skeletal muscles, dilation of eye pupils, among other changes [2, 4]. Nonetheless, although the consequences of this response are usually adaptive [5], they can also be damaging, affecting organ integrity and being detrimental to health [5, 6]. Hence, a unified in-depth mechanistic comprehension of the “fight or flight response” is crucial for discriminating pathological from physiological outcomes to which it leads, and for improving therapies designed to prevent organ damage resulting from this phenomenon.
The most well-studied effector organ that responds to stress is the adrenal gland, which releases catecholamines and glucocorticoids into the bloodstream [7]. Nonetheless, the fight or flight response also activates the sympathetic nervous system, which has been historically less explored partially due to its diffuse anatomy [8, 9]. Sympathetic nerves innervate most organs and are also involved in various pathophysiological responses to psychological stress [10, 11]. Sympathetic neurotransmitters released by these innervations, such as norepinephrine, ATP, neuropeptide Y, and nitric oxide, may affect the behavior of specific cell types in diverse tissue microenvironments [12, 13]. Albeit sympathetic nerves activated by psychological stress have long been suspected of participating in the origin of many disorders, the cellular and molecular mechanisms involved still remain incompletely understood. Understanding the role of sympathetic nerves and the signaling mechanisms involved during psychological stress may be crucial for the success of clinical applications.
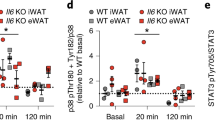
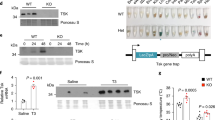
In a recent article in Cell, Qing and colleagues demonstrated elegantly that sympathetic nerves play a central role in the inflammatory organ damage that can be caused by psychological stress [14]. Using state-of-the-art technologies, such as sophisticated in vivo inducible genetic methods, including Cre/loxP-mediated systems, in combination with pharmacological approaches, the authors selectively eliminated different components from the tissue microenvironment to dissect the cellular and molecular mechanisms involved in acute stress-derived organ damage. The authors found that the level of interleukin-6 (IL-6) induced after psychological stress was higher than of all other cytokines tested. This level was sustained for several hours, and it was independent of circadian oscillations [14]. Interestingly, surgical removal of brown adipose tissue eliminated the increase in IL-6 after psychological stress. Additionally, Qing and colleagues, by using UCP1-Cre/IL-6-floxed mice in which IL-6 is deleted specifically from brown adipocytes, revealed that IL-6 levels after psychological stress decreased significantly in those mice [14]. These data indicated that the major source of IL-6 after psychological stress was brown adipocytes.
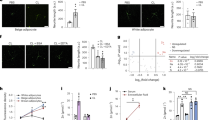
Remarkably, the authors discovered that pharmacological sympathetic denervation reduced IL-6 levels induced by psychological stress. Also, specific genetic ablation of β3 adrenergic receptors in brown adipocytes attenuated the levels of stress-induced IL-6, demonstrating that sympathetic nerves control brown adipocytes IL-6 release by β3 adrenergic signaling during acute stress. Moreover, Qing and colleagues showed that sympathetic nerve activation of adipocyte IL-6 secretion leads to hyperglycemia through gluconeogenesis in response to psychological stress [14]. Notably, pharmacologic blockage or genetic deletion of IL-6 receptors in hepatocytes suppressed hepatic gluconeogenesis after psychological stress. Overall, these results indicate that sympathetic nerves induce hyperglycemia in response to acute stress via adipocyte-derived interleukin-6 acting on hepatocytes [14].
Qing and colleagues demonstrated that lipopolysaccharide-induced inflammation can cause mortality in stressed animals. Strikingly, this mortality was dependent of sympathetic nerves signaling through β3-adrenergic receptors in adipocytes, of IL-6 release by those adipocytes, and of glucose production by hepatocytes in response to IL-6 [14]. Importantly, the mortality in stressed animals was caused by renal and cardiac damage. Altogether, this study reveals a key role of sympathetic nerves in decreasing tolerance to inflammatory organ damage via adipocyte-derived IL-6 (Fig. 1).
Sympathetic nerve-adipocyte-hepatocyte axis dictates physiologic response to acute psychological stress. Using state-of-the-art technologies, Qing and colleagues demonstrated that, after acute psychological stress, sympathetic nerves induce brown adipocytes to increase circulatory IL-6 levels. IL-6 signals to hepatocytes to increase glucose production via gluconeogenesis leading to hyperglycemia. This results in a decline in the organism tolerance to inflammatory organ damage [14]
This study reveals details of cellular and molecular mechanisms involved in the organism response to acute stress. It also identifies a systemic communication between the peripheral nervous system, brown adipocytes, and hepatocytes. These findings also offer novel therapeutic targets for treatments of disorders characterized by inflammatory organ damage. Here, we discuss the discoveries from this work and evaluate recent advances in our understanding of the influence of sympathetic nerve-adipocyte-hepatocyte axis in the tissue microenvironment.
Perspectives/future directions
Specificity of transgenic cre/loxP models
Qing and colleagues analyzed cell-specific null mutant mice models (Ucp1-CreER/β3-adrenergic receptor-floxed, Ucp1-CreER/IL-6-floxed, and Alb-Cre/IL-6 receptor a-floxed mice), and the principal discoveries from this study are based on the experimental results collected from these mice [14]. A limitation of such approaches is that they rely on the induction of the Cre recombinase [15,16,17]. Thus, caveats, that need to be given attention when using these models, include inadequate recombination leading to insufficient gene deletion, off-target Cre expression, and compensatory upregulation of other genes [18, 19]. Therefore, examination of gene expression levels in the targeted cells will clarify the level of achieved gene deletion, and whether there are compensatory changes in the expression of other genes in these specific cells.
Traditionally, it is well established that Ucp1 is expressed by adipocytes [20]. Nevertheless, not all adipocytes have this protein [21], and Cre-mediated expression based on this gene can be detected in other cells as well, for instance in renal collecting ducts [22]. Additionally, Ucp1 expression was previously detected outside of the adipose tissue as well [23]. Thus, in Ucp1-CreER/β3-adrenergic receptor-floxed and Ucp1-CreER/IL-6-floxed mice, β3-adrenergic receptor and IL-6 may be also eliminated from other cell types outside of the brown adipose tissue. Although these concerns do not change the outcome of this study, it is possible that some of the effects observed in those models are not exclusively due to brown adipocytes.
Brown adipocytes are present in diverse anatomical locations in mice and humans, including dorsal back of the interscapular and subscapular regions, cervical region between scapula and head, supraclavicular region, associated to kidneys, and attached to the thoracic aorta [24,25,26,27]. Additionally, they can be found also within the epididymal and inguinal white adipose tissue [28, 29] as beige/brite adipocyte. Qing and colleagues surgically removed intrascapular fat pads, suggesting the importance of brown adipocytes from this site [14]. Nevertheless, in all transgenic models analyzed, genetic deletions of β3-adrenergic receptor and IL-6 were done in brown adipocytes from all locations where they are present. Therefore, it remains to be explored whether the observed phenotype in these transgenic models is due to brown adipocytes from a specific anatomical location, or whether all brown adipocytes contribute to this phenomenon.
Heterogeneity within the sympathetic nerve-adipocyte axis
Mature adipocytes are the typical residents of the adipose tissue [30,31,32] and are classified into three distinct types: white, brown, and beige/brite (https://doi.org/10.1016/j.cmet.2016.10.005). White adipocytes are related to storing triacylglycerides (TGs). The brown adipocytes oxidize lipids to produce heat in part through a UCP1 associated uncoupling of electron transport from ATP production. Beige adipocytes (“brown-like”) can also support UCP1-independent thermogenesis (https://doi.org/10.1042/BCJ20200298). Beige cells resemble white adipocytes with a shallow basal expression of UCP1, but, like classical brown fat, they respond to cyclic AMP stimulation with high UCP1 expression and respiration rates (https://doi.org/10.1016/j.cell.2012.05.016). Nevertheless, this tissue comprises a variety of other components with important physiological roles, such as pre-adipocytes, mesenchymal stem cells, nerves, macrophages, neutrophils, lymphocytes, fibroblasts, pericytes, endothelial cells, and others [33,34,35,36]. The proportions of the different adipose tissue constituents may vary depending on the pathophysiological condition and the anatomical location [37]. Interestingly, most of these cells produce IL-6 [38]. Qing and colleagues demonstrated that adipocytes are the main source of IL-6 after psychological stress [14]. Future studies will reveal whether other sources of IL-6 also may be activated by sympathetic nerves and play important roles during the “fight or flight response”.
Adipocytes have been shown to be heterogeneous, based on molecular markers, embryonic origins, and anatomical locations [39,40,41]. Qing and colleagues consider brown adipocytes as a homogeneous population in their study [14]. Nonetheless, a recent study revealed the existence of two brown adipocyte subpopulations based on adiponectin expression [42]. This study showed that the two subtypes differ in their functions and metabolic signatures, characterizing them as low and high thermogenic brown adipocytes. Elegantly, by single-brown adipocyte RNA sequencing, it was revealed that there is molecular heterogeneity based on the transcriptomic patterns of the two brown adipocyte subtypes [42]. Curiously, only one of the subpopulations declined in number with aging. Thus, whether only a fraction of brown adipocytes responds, by producing IL-6, to sympathetic nerves in response to acute stress still needs to be elucidated. It would be important to examine whether different brown adipocytes’ subsets behave distinctly during sympathetic nerve activation.
Although all rodent brown adipose tissue depots receive sympathetic innervations [43], the tissue microenvironments of these depots differ [44, 45]. For instance, only the pericardial and minor mediastinal brown adipose tissue depots are innervated by parasympathetic nerve fibers [44, 45]. The sympathetic innervations may also vary in their morphologies and functions in different species [46,47,48,49,50,51]. Thus, the role of sympathetic neurons in the brown adipose tissue of distinct anatomical locations in particular species should be investigated in future studies.
Other roles of IL-6 signaling
IL-6 is a prototypical cytokine involved in the enhancement of multiple inflammatory pathways [52]. It can be induced by diverse stimuli, such as invasion of pathogens or other types of inflammation-linked damage [53]. IL-6 has been shown to be involved in both the innate and adaptive immune responses [38, 54]. It also activates the leukocytic chemotaxis towards the injured site [55, 56]. Importantly, decontrolled IL-6 release results in constant inflammation leading to tissue damage [57, 58]. IL-6 signaling involves canonical and non-canonical molecular mechanisms via a membrane bound or a soluble receptor, respectively. In canonical signaling, IL-6 binds to a membrane-anchored IL-6 receptor (IL-6R). This binding promotes an association with gp130, which activates signal transduction [59]. Non-canonical IL-6 signaling is mediated by the binding to a soluble form of IL-6R (sIL-6R) and forming the complex with gp130 [58]. The differences between downstream signaling mechanisms of IL-6 in canonical versus non-canonical pathways depend on the affected cells, leading to the activation of JAK/STAT3 and/or SHP2/Gab/MAPK pathways [59]. Canonical IL-6 signaling is essential in the chemoresistance of ovarian cancer [60], autoimmune diseases [61], colitis [62], and hepatic inflammation [63], while non-canonical IL-6 signaling influences rheumatoid arthritis, Castleman disease [64], osteoclastogenesis [65], and type 2 diabetes [66]. Increased IL-6 levels have been related to a series of stressors such as cold, infection, restraint, fatigue, sleep deprivation, and psychosocial stressors [67,68,69,70,71]. Thus, IL-6 increase may affect different tissues differently during psychological stress [72]. Future studies should explore whether canonical, non-canonical IL-6 signaling, or both are involved during psychological stress pathogenesis.
IL6 is expressed as distinct isoforms that may be responsible for different functions associated with IL6 signaling. For example, four IL-6 variants were detected in the human lung tissue: native IL-6, IL-6 missing exon 2 (IL-6Δ2), IL-6 missing exon 4 (IL-6Δ4), and IL-6 missing both exons 2 and 4 (IL-6Δ2,4). Nevertheless, proteins were coded exclusively by native IL-6 and IL-6Δ4. The IL-6Δ4 isoform can form a stable complex with IL-6Rα like native IL-6, but not with IL-6Rβ. Thus, IL-6Δ4 might have a regulatory influence on IL-6 signaling [73]. A spliced isoform of IL-6 was also detected in renal cell carcinoma which acts as IL-6 inhibitor [74]. Recently, there were also reported two IL-6 isoforms in turtles subjected to stress homologous to the mammalian IL-6 [67]. The two IL-6 transcripts were named psIL6 and psIL6ns. Future studies should explore whether different IL-6 isoforms act differently in stress-related contexts. Qing and colleagues demonstrate that after acute stress sympathetic nerves induce the increase in the levels of IL-6 which leads to other pathophysiologic effects [14]. It will be interesting to determine whether sympathetic nerves are also responsible for IL-6 increase in other pathological conditions, in which the role of this cytokine is well characterized, such as Alzheimer’s disease [75,76,77], Asthma [78, 79], atherosclerosis [80, 81], inflammatory bowel disease [82, 83], nephropathy [84], liver diseases [85], and others [38] (Fig. 2).
Schematic illustration summarizing the possible role of sympathetic nerves on multiple inflammatory diseases via IL-6. After acute psychological stress, sympathetic nerves induce the increase in the levels of IL-6 which leads to other pathophysiologic effects [14]. IL-6 plays important roles in the pathogenesis of multiple disorders. Future studies will reveal whether sympathetic nerves are also responsible for IL-6 production in these pathological conditions
Intriguingly, high levels of circulating IL-6 were associated with worse outcomes in COVID-19 patients, bringing attractive possibilities in terms of treatments [86]. An excessive inflammatory reaction is observed in patients infected by the SARS-CoV-2 virus [87,88,89,90]. COVID-19 infection can be characterized as a “cytokine storm” because the infection is followed by an intense inflammatory response with the release of a copious pro-inflammatory cytokines. The cytokine storm can be characterized by destructive systemic inflammation, hyperferritinemia, hemodynamic instability, and multiple organ failure that can lead to death. Multiple pro-inflammatory cytokines, including IFN-γ, TNF-α, IL-1, IL-6, and IL-18, participate in this uncontrolled immune response [87, 91]. IL-6 plays a fundamental role in the harmful systemic hyperactivated immune status, characterized as “cytokine storm”. IL-6-induced immune dysregulation is an important feature of SARS-CoV-2 infection, and the increase of this and other cytokines, including TNF-α, is associated with augmented viral load found in the severe form of the disease [91,92,93].
Three drugs that block IL-6 signaling, tocilizumab, sarilumab, and siltuximab, have been proposed to be used against COVID-19 [94, 95]. Yet, the cellular and molecular players involved in COVID-19 pathophysiology still remain poorly understood. It will be interesting to examine whether SARS-Cov-2 virus activates the sympathetic nerves–brown adipocytes axis to produce IL-6. During the pandemic, patients also suffer with social isolation what leads to acute psychological stress, with the possible involvement of sympathetic nerves in the production of IL-6. COVID-19 disease brought fear, lockdown, and precautionary measures that led to psychosocial stress which may result in depression [96,97,98]. Acute stress is related to isolated episodic events while chronic stress is associated with an accumulation of several episodic psychological stress events [99]. The prolongation of pandemic restrictions could lead to chronic stress. Although Qing et al. discussed IL-6 regulation of acute stress, IL-6 has been shown to be involved in both acute and chronic stress [71]. High levels of IL-6 are detected in patients with depression [100]. Furthermore, increased IL-6 concentration and systemic inflammation have been reported in psychosocial stress, similar to the observed after COVID-19 infection [100]. In spite of major epidemiological studies, stress has not yet been singled out as an essential risk factor in COVID-19 disease. Nevertheless, reports have shown that psychological stress and depression in COVID-19 patients may worsen disease prognosis [101, 102]. Interestingly, infants and children, which have more abundant brown adipose tissue [103,104,105,106], are the ones least affected by COVID-19 [107, 108]. This may be due to a variety of reasons, including lower expression of angiotensin-converting enzyme 2 (ACE2) receptors in children [109, 110], higher COVID-19 comorbidities in adults [111], increased chronic pro-inflammatory status with age [112,113,114,115], and others. Thus, it will be important to investigate in depth the mechanisms involved in the production of IL-6 in COVID-19 patients at different ages, exploring the possible cross-talk between sympathetic nerves and brown adipocytes (Fig. 3).
Possible role of sympathetic nerves and brown adipocytes in COVID-19 pathogenesis. High levels of circulating IL-6 are associated with worse outcomes in COVID-19 patients. It will be interesting to examine whether SARS-Cov-2 virus activates the sympathetic nerve-brown adipocyte axis to produce IL-6. During the pandemic, patients also suffer with social isolation what leads to acute psychological stress, with the possible involvement of sympathetic nerves in the production of IL-6
IL-6 signaling induces distinct acute and chronic pathophysiological effects. Initially, IL-6 is produced in the site of inflammation by the skeletal muscle, adipose tissue, adrenal gland, endothelial cells, and others [71], leading to the production of C-reactive protein, serum amyloid A, fibrinogen, and other acute-phase proteins [116, 117]. On the other hand, during the chronic response, IL-6 is produced by a variety of leukocytes mediating the switch from innate to adaptive immunity which restores the body homeostasis after inflammation [117, 118]. In obesity, although the main focus of studies has been the targeting of the white adipose tissue, increase in brown adipose tissue has emerged as a promising strategy against this pathology as well [119]. Indeed, ablation of UCP1, the brown-fat-specific uncoupling protein, has been shown sufficient to induce obesity, suggesting that brown adipose tissue may protect against this disease [120]. Nevertheless, an increase in IL-6 has been detected in the circulation and adipose tissue of obese patients [121,122,123], indicating that possibly this increase in IL-6 may be coming from a different source than during acute psychological stress. Interestingly, findings point to different and even sometimes contradictory outcomes when using IL-6 knockout mice. While some showed that these mice develop spontaneous obesity [124], other studies found different results [125, 126]. Such contradictory findings could be explained only in the frame of a more in-depth investigation on the role of IL-6 coming from different sources (cells/tissues).
Interactions within the tumor microenvironment
In addition to key roles of peripheral innervations within different organs, nerves infiltrate also inside tumors in several tissues, affecting cancer development in different ways [127,128,129,130,131,132,133,134]. Specifically, sympathetic nerves have been shown necessary for cancer progression [131]. Importantly, clinical studies reveal beneficial effects of treatments that affect the sympathetic nervous system in human cancer patients [135]. Still, the detailed molecular mechanisms by which sympathetic nerves influence cancer progression remain incompletely understood within the complexity of the tumor microenvironment [133, 136].
When adipose tissue is invaded by cancer cells, adipocytes act as a supply of lipids for neoplastic cells [137, 138]. Additionally, adipocytes directly interact with malignant cells affecting their behavior, including their proliferation and invasion capacities [139,140,141,142,143]. Adipocytes may also affect other components within the tumor microenvironment, such as newly formed blood vessels [144,145,146,147,148,149,150,151,152,153,154,155,156,157]. White and beige adipocytes, within the tumor microenvironment, also produce IL-6, and some of their effects on cancer cells have been attributed to IL-6 signaling [158, 159]. Additionally, brown adipocytes can transform and secrete IL‐6 upon other different stimulations [160, 161]. Cancer-associated cachexia is associated with switch from WAT to BAT [162] (https://doi.org/10.1038/s41598-018-36626-3). Increased circulating IL-6 levels have been associated with WAT browning, as consequence of the upregulation of the uncoupling protein-1 (UCP1) [162, 163] (https://doi.org/10.20900/immunometab20200032). Experiments blocking IL-6 production by cancer cells show a reduction in browning [162], which limits cachexia [164]. Additionally, treatment with anti-IL-6 blocks WAT atrophy [162]. The role of the sympathetic nervous system in IL-6 induction of cancer-associated cachexia remains to be explored.
Thus, it will be compelling to examine whether sympathetic nerves also act within tumors via IL-6 derived from intra-tumoral adipocytes (Fig. 4). New treatments targeting this possible mechanism could potentially be used in the anti-cancer fight, improving patient survival.
Potential new mechanism of sympathetic nerve role within the tumor microenvironment. Different nerve fibers, including sympathetic innervations, infiltrate the tumors, and affect their development. The detailed molecular mechanisms by which sympathetic nerves influence cancer progression remain incompletely understood. Future studies should examine whether sympathetic nerves also act within tumors via IL-6 derived from intra-tumoral adipocytes
Translating mouse research into humans
Qing and colleagues reveal a novel role of sympathetic nerves increasing circulatory IL-6 via brown adipocytes after psychological stress [14]. Mouse models aim to recreate features of human biology as closely as possible. Nevertheless, to translate animal research into human patients, these discoveries should be in the future validated in human tissues. Although it is known that in humans IL-6 levels increase after stress [14, 165, 166], the mechanisms involved in this phenomenon remain to be confirmed. It has been implied that β3-adrenergic response in the adipose tissue varies between species [167]. Comparing rodent and human brown adipose tissues, differences have been detected in composition, gene expression profiles, and anatomical location, being more widely dispersed in humans [168, 169]. IL-6 also presents species-specific characteristics, such as binding specificity [170, 171]. Also, the human and rodent IL-6 receptors differ, and tocilizumab does not activate the rodent receptors [172,173,174,175,176]. It is not yet clear whether these findings could be translated into clinic, thus future studies should examine whether the mechanistic discoveries by Qing et al. (2020) are also valid in humans. Enhancing the accessibility to human biopsies will be essential to achieve this aim. Importantly, although some BAT deposits have been reported [161, 177,178,179,180], the WAT is the predominant fat type in humans. IL-6 production by WAT has been suggested to participate in the pathophysiology of type 2 diabetes and obesity in humans [66, 181, 182]. Moreover, the white adipose tissue is also innervated by the sympathetic nervous system [180, 183, 184] and has been shown to secrete IL-6 [66]. This brings the question of whether the production of IL-6 in humans is activated in the WAT through sympathetic innervations stimulation as well. Thus, albeit IL-6 is secreted in humans from WAT, BAT and beige adipocytes, future work will explore whether and how the sympathetic nervous system is involved in these processes. Interestingly, several ongoing clinical trials are exploring the role of IL-6 biology in multiple human disorders including inflammation, rheumatoid arthritis, COVID-19, pneumonia, cardiovascular diseases, cancer, adipose tissue remodeling, stress, exercise, immune cell regulation, and obesity (Table 1).
Conclusion
Qing and colleagues provide a new and important insight into the cellular and molecular mechanisms involved in the response to acute psychological stress: Sympathetic nerves induce adipocytes to release IL-6 which activate hepatocytes for gluconeogenesis [14]. This new concept places sympathetic nerves, brown adipocytes, and hepatocytes as central players that might be pharmacologically targeted to alter the physiologic effects of acute psychological stress and improve the organism reactions. Future studies will reveal whether these cross-talks are important also in other physiopathologic conditions.
Availability of data and materials
Not applicable.
References
Goligorsky MS (2001) The concept of cellular “fight-or-flight” reaction to stress. Am J Physiol Renal Physiol 280:F551-561. https://doi.org/10.1152/ajprenal.2001.280.4.F551
Galassi FM, Boni T, Ruhli FJ, Habicht ME (2016) Fight-or-flight response in the ancient Egyptian novel “Sinuhe” (c. 1800 BCE). Auton Neurosci 195:27–28. https://doi.org/10.1016/j.autneu.2016.02.006
Ulrich-Lai YM, Herman JP (2009) Neural regulation of endocrine and autonomic stress responses. Nat Rev Neurosci 10:397–409. https://doi.org/10.1038/nrn2647
Rodrigues ACZ, Messi ML, Wang ZM, Abba MC, Pereyra A, Birbrair A, Zhang T, O’Meara M, Kwan P, Lopez EIS et al (2019) The sympathetic nervous system regulates skeletal muscle motor innervation and acetylcholine receptor stability. Acta Physiol (Oxf) 225:e13195. https://doi.org/10.1111/apha.13195
Dhabhar FS, McEwen BS (1997) Acute stress enhances while chronic stress suppresses cell-mediated immunity in vivo: a potential role for leukocyte trafficking. Brain Behav Immun 11:286–306. https://doi.org/10.1006/brbi.1997.0508
McEwen BS (1998) Protective and damaging effects of stress mediators. N Engl J Med 338:171–179. https://doi.org/10.1056/NEJM199801153380307
Kanczkowski W, Sue M, Bornstein SR (2016) Adrenal gland microenvironment and its involvement in the regulation of stress-induced hormone secretion during sepsis. Front Endocrinol (Lausanne) 7:156. https://doi.org/10.3389/fendo.2016.00156
Jansen AS, Nguyen XV, Karpitskiy V, Mettenleiter TC, Loewy AD (1995) Central command neurons of the sympathetic nervous system: basis of the fight-or-flight response. Science 270:644–646. https://doi.org/10.1126/science.270.5236.644
Jesus ICG, Araujo FM, Mesquita T, Junior NNS, Silva MM, Morgan HJN, Silva KSC, Silva CLA, Birbrair A, Amaral FA et al (2021) Molecular basis of period 1 regulation by adrenergic signaling in the heart. FASEB J 35:e21886. https://doi.org/10.1096/fj.202100441R
Sung CP, Arleth AJ, Feuerstein GZ (1991) Neuropeptide Y upregulates the adhesiveness of human endothelial cells for leukocytes. Circ Res 68:314–318. https://doi.org/10.1161/01.res.68.1.314
Claxson A, Morris C, Blake D, Siren M, Halliwell B, Gustafsson T, Lofkvist B, Bergelin I (1990) The anti-inflammatory effects of D-myo-inositol-1.2.6-trisphosphate (PP56) on animal models of inflammation. Agents Actions 29:68–70. https://doi.org/10.1007/BF01964724
Burnstock G (2013) Cotransmission in the autonomic nervous system. Handb Clin Neurol 117:23–35. https://doi.org/10.1016/B978-0-444-53491-0.00003-1
Coimbra-Campos LMC, Silva WN, Baltazar LM, Costa PAC, Prazeres PHDM, Picoli CC, Costa AC, Rocha BGS, Santos GSP, Oliveira FMS et al (2021) Circulating Nestin-GFP+ cells participate in the pathogenesis of Paracoccidioides brasiliensis in the lungs. Stem Cell Rev Rep 17:1874–1888 (2021). https://doi.org/10.1007/s12015-021-10181-3
Qing H, Desrouleaux R, Israni-Winger K, Mineur YS, Fogelman N, Zhang C, Rashed S, Palm NW, Sinha R, Picciotto MR et al (2020) Origin and function of stress-induced IL-6 in murine models. Cell 182(372–387):e314. https://doi.org/10.1016/j.cell.2020.05.054
Khan JA, Mendelson A, Kunisaki Y, Birbrair A, Kou Y, Arnal-Estape A, Pinho S, Ciero P, Nakahara F, Ma’ayan A et al (2016) Fetal liver hematopoietic stem cell niches associate with portal vessels. Science 351:176–180. https://doi.org/10.1126/science.aad0084
Asada N, Kunisaki Y, Pierce H, Wang Z, Fernandez NF, Birbrair A, Ma’ayan A, Frenette PS (2017) Differential cytokine contributions of perivascular haematopoietic stem cell niches. Nat Cell Biol 19:214–223. https://doi.org/10.1038/ncb3475
Nobre AR, Risson E, Singh DK, Martino JD, Cheung JF, Wang J, Johnson J, Russnes HG, Bravo-Cordero JJ, Birbrair A et al (2021) Bone marrow NG2+/Nestin+ mesenchymal stem cells drive DTC dormancy via TGFβ2. Nature Cancer 2:327–339
Kastner P, Mark M, Chambon P (1995) Nonsteroid nuclear receptors: what are genetic studies telling us about their role in real life? Cell 83:859–869. https://doi.org/10.1016/0092-8674(95)90202-3
Nassar MA, Stirling LC, Forlani G, Baker MD, Matthews EA, Dickenson AH, Wood JN (2004) Nociceptor-specific gene deletion reveals a major role for Nav1.7 (PN1) in acute and inflammatory pain. Proc Natl Acad Sci U S A 101:12706–12711. https://doi.org/10.1073/pnas.0404915101
Challa TD, Dapito DH, Kulenkampff E, Kiehlmann E, Moser C, Straub L, Sun W, Wolfrum C (2020) A genetic model to study the contribution of brown and brite adipocytes to metabolism. Cell Rep 30(3424–3433):e3424. https://doi.org/10.1016/j.celrep.2020.02.055
Ikeda K, Maretich P, Kajimura S (2018) The common and distinct features of brown and beige adipocytes. Trends Endocrinol Metab 29:191–200. https://doi.org/10.1016/j.tem.2018.01.001
Craft CS, Robles H, Lorenz MR, Hilker ED, Magee KL, Andersen TL, Cawthorn WP, MacDougald OA, Harris CA, Scheller EL (2019) Bone marrow adipose tissue does not express UCP1 during development or adrenergic-induced remodeling. Sci Rep 9:17427. https://doi.org/10.1038/s41598-019-54036-x
Grant L, Lees EK, Forney LA, Mody N, Gettys T, Brown PA, Wilson HM, Delibegovic M (2016) Methionine restriction improves renal insulin signalling in aged kidneys. Mech Ageing Dev 157:35–43. https://doi.org/10.1016/j.mad.2016.07.003
Vitali A, Murano I, Zingaretti MC, Frontini A, Ricquier D, Cinti S (2012) The adipose organ of obesity-prone C57BL/6J mice is composed of mixed white and brown adipocytes. J Lipid Res 53:619–629. https://doi.org/10.1194/jlr.M018846
Frontini A, Cinti S (2010) Distribution and development of brown adipocytes in the murine and human adipose organ. Cell Metab 11:253–256. https://doi.org/10.1016/j.cmet.2010.03.004
de Jong JM, Larsson O, Cannon B, Nedergaard J (2015) A stringent validation of mouse adipose tissue identity markers. Am J Physiol Endocrinol Metab 308:E1085-1105. https://doi.org/10.1152/ajpendo.00023.2015
Mo Q, Salley J, Roshan T, Baer LA, May FJ, Jaehnig EJ, Lehnig AC, Guo X, Tong Q, Nuotio-Antar AM et al (2017) Identification and characterization of a supraclavicular brown adipose tissue in mice. JCI Insight 2. https://doi.org/10.1172/jci.insight.93166
Wu J, Bostrom P, Sparks LM, Ye L, Choi JH, Giang AH, Khandekar M, Virtanen KA, Nuutila P, Schaart G et al (2012) Beige adipocytes are a distinct type of thermogenic fat cell in mouse and human. Cell 150:366–376. https://doi.org/10.1016/j.cell.2012.05.016
Petrovic N, Walden TB, Shabalina IG, Timmons JA, Cannon B, Nedergaard J (2010) Chronic peroxisome proliferator-activated receptor gamma (PPARgamma) activation of epididymally derived white adipocyte cultures reveals a population of thermogenically competent, UCP1-containing adipocytes molecularly distinct from classic brown adipocytes. J Biol Chem 285:7153–7164. https://doi.org/10.1074/jbc.M109.053942
Kahn CR, Wang G, Lee KY (2019) Altered adipose tissue and adipocyte function in the pathogenesis of metabolic syndrome. J Clin Invest 129:3990–4000. https://doi.org/10.1172/JCI129187
Guerra DAP, Paiva AE, Sena IFG, Azevedo PO, Batista ML Jr, Mintz A, Birbrair A (2018) Adipocytes role in the bone marrow niche. Cytometry A 93:167–171. https://doi.org/10.1002/cyto.a.23301
Henriques F, Lopes MA, Franco FO, Knobl P, Santos KB, Bueno LL, Correa VA, Bedard AH, Guilherme A, Birbrair A et al (2018) Toll-like receptor-4 disruption suppresses adipose tissue remodeling and increases survival in cancer cachexia syndrome. Sci Rep 8:18024. https://doi.org/10.1038/s41598-018-36626-3
Cannon B, Nedergaard J (2004) Brown adipose tissue: function and physiological significance. Physiol Rev 84:277–359. https://doi.org/10.1152/physrev.00015.2003
Tchoukalova YD, Sarr MG, Jensen MD (2004) Measuring committed preadipocytes in human adipose tissue from severely obese patients by using adipocyte fatty acid binding protein. Am J Physiol Regul Integr Comp Physiol 287:R1132-1140. https://doi.org/10.1152/ajpregu.00337.2004
Elgazar-Carmon V, Rudich A, Hadad N, Levy R (2008) Neutrophils transiently infiltrate intra-abdominal fat early in the course of high-fat feeding. J Lipid Res 49:1894–1903. https://doi.org/10.1194/jlr.M800132-JLR200
Kintscher U, Hartge M, Hess K, Foryst-Ludwig A, Clemenz M, Wabitsch M, Fischer-Posovszky P, Barth TF, Dragun D, Skurk T et al (2008) T-lymphocyte infiltration in visceral adipose tissue: a primary event in adipose tissue inflammation and the development of obesity-mediated insulin resistance. Arterioscler Thromb Vasc Biol 28:1304–1310. https://doi.org/10.1161/ATVBAHA.108.165100
Weinstock A, Moura Silva H, Moore KJ, Schmidt AM, Fisher EA (2020) Leukocyte heterogeneity in adipose tissue, including in obesity. Circ Res 126:1590–1612. https://doi.org/10.1161/CIRCRESAHA.120.316203
Hunter CA, Jones SA (2015) IL-6 as a keystone cytokine in health and disease. Nat Immunol 16:448–457. https://doi.org/10.1038/ni.3153
Ussar S, Lee KY, Dankel SN, Boucher J, Haering MF, Kleinridders A, Thomou T, Xue R, Macotela Y, Cypess AM et al (2014) ASC-1, PAT2, and P2RX5 are cell surface markers for white, beige, and brown adipocytes. Sci Transl Med 6:247ra103. https://doi.org/10.1126/scitranslmed.3008490
Xue B, Rim JS, Hogan JC, Coulter AA, Koza RA, Kozak LP (2007) Genetic variability affects the development of brown adipocytes in white fat but not in interscapular brown fat. J Lipid Res 48:41–51. https://doi.org/10.1194/jlr.M600287-JLR200
Seale P, Bjork B, Yang W, Kajimura S, Chin S, Kuang S, Scime A, Devarakonda S, Conroe HM, Erdjument-Bromage H et al (2008) PRDM16 controls a brown fat/skeletal muscle switch. Nature 454:961–967. https://doi.org/10.1038/nature07182
Song A, Dai W, Jang MJ, Medrano L, Li Z, Zhao H, Shao M, Tan J, Li A, Ning T et al (2020) Low- and high-thermogenic brown adipocyte subpopulations coexist in murine adipose tissue. J Clin Invest 130:247–257. https://doi.org/10.1172/JCI129167
Kooijman S, van den Heuvel JK, Rensen PCN (2015) Neuronal control of brown fat activity. Trends Endocrinol Metab 26:657–668. https://doi.org/10.1016/j.tem.2015.09.008
Giordano A, Frontini A, Castellucci M, Cinti S (2004) Presence and distribution of cholinergic nerves in rat mediastinal brown adipose tissue. J Histochem Cytochem 52:923–930. https://doi.org/10.1369/jhc.3A6246.2004
Schafer MK, Eiden LE, Weihe E (1998) Cholinergic neurons and terminal fields revealed by immunohistochemistry for the vesicular acetylcholine transporter. I Central nervous system Neuroscience 84:331–359. https://doi.org/10.1016/s0306-4522(97)00516-2
Wiedmann NM, Stefanidis A, Oldfield BJ (2017) Characterization of the central neural projections to brown, white, and beige adipose tissue. FASEB J 31:4879–4890. https://doi.org/10.1096/fj.201700433R
Stefanidis A, Wiedmann NM, Tyagi S, Allen AM, Watt MJ, Oldfield BJ (2018) Insights into the neurochemical signature of the innervation of beige fat. Mol Metab 11:47–58. https://doi.org/10.1016/j.molmet.2018.01.024
Bamshad M, Song CK, Bartness TJ (1999) CNS origins of the sympathetic nervous system outflow to brown adipose tissue. Am J Physiol 276:R1569-1578. https://doi.org/10.1152/ajpregu.1999.276.6.R1569
Francois M, Torres H, Huesing C, Zhang R, Saurage C, Lee N, Qualls-Creekmore E, Yu S, Morrison CD, Burk D et al (2019) Sympathetic innervation of the interscapular brown adipose tissue in mouse. Ann N Y Acad Sci 1454:3–13. https://doi.org/10.1111/nyas.14119
Hopkins DA, Armour JA (1984) Localization of sympathetic postganglionic and parasympathetic preganglionic neurons which innervate different regions of the dog heart. J Comp Neurol 229:186–198. https://doi.org/10.1002/cne.902290205
Buckley U, Yamakawa K, Takamiya T, Andrew Armour J, Shivkumar K, Ardell JL (2016) Targeted stellate decentralization: implications for sympathetic control of ventricular electrophysiology. Heart Rhythm 13:282–288. https://doi.org/10.1016/j.hrthm.2015.08.022
Kang S, Narazaki M, Metwally H, Kishimoto T (2020) Historical overview of the interleukin-6 family cytokine. J Exp Med 217. https://doi.org/10.1084/jem.20190347
Pandolfi F, Altamura S, Frosali S, Conti P (2016) Key role of DAMP in inflammation, cancer, and tissue repair. Clin Ther 38:1017–1028. https://doi.org/10.1016/j.clinthera.2016.02.028
Narazaki M, Kishimoto T (2018) The two-faced cytokine IL-6 in host defense and diseases. Int J Mol Sci 19. https://doi.org/10.3390/ijms19113528
Weissenbach M, Clahsen T, Weber C, Spitzer D, Wirth D, Vestweber D, Heinrich PC, Schaper F (2004) Interleukin-6 is a direct mediator of T cell migration. Eur J Immunol 34:2895–2906. https://doi.org/10.1002/eji.200425237
Wright HL, Cross AL, Edwards SW, Moots RJ (2014) Effects of IL-6 and IL-6 blockade on neutrophil function in vitro and in vivo. Rheumatology (Oxford) 53:1321–1331. https://doi.org/10.1093/rheumatology/keu035
Tanaka T, Narazaki M, Kishimoto T (2014) IL-6 in inflammation, immunity, and disease. Cold Spring Harb Perspect Biol 6:a016295. https://doi.org/10.1101/cshperspect.a016295
Schaper F, Rose-John S (2015) Interleukin-6: biology, signaling and strategies of blockade. Cytokine Growth Factor Rev 26:475–487. https://doi.org/10.1016/j.cytogfr.2015.07.004
Su H, Lei CT, Zhang C (2017) Interleukin-6 signaling pathway and its role in kidney disease: an update. Front Immunol 8:405. https://doi.org/10.3389/fimmu.2017.00405
Xu S, Yu C, Ma X, Li Y, Shen Y, Chen Y, Huang S, Zhang T, Deng W, Wang Y (2021) IL-6 promotes nuclear translocation of HIF-1alpha to aggravate chemoresistance of ovarian cancer cells. Eur J Pharmacol 894:173817. https://doi.org/10.1016/j.ejphar.2020.173817
Zhao M, Tan Y, Peng Q, Huang C, Guo Y, Liang G, Zhu B, Huang Y, Liu A, Wang Z et al (2018) IL-6/STAT3 pathway induced deficiency of RFX1 contributes to Th17-dependent autoimmune diseases via epigenetic regulation. Nat Commun 9:583. https://doi.org/10.1038/s41467-018-02890-0
Zhang J, Wang C, Guo Z, Da B, Zhu W, Li Q (2021) miR-223 improves intestinal inflammation through inhibiting the IL-6/STAT3 signaling pathway in dextran sodium sulfate-induced experimental colitis. Immun Inflamm Dis 9:319–327. https://doi.org/10.1002/iid3.395
Wunderlich FT, Strohle P, Konner AC, Gruber S, Tovar S, Bronneke HS, Juntti-Berggren L, Li LS, van Rooijen N, Libert C et al (2010) Interleukin-6 signaling in liver-parenchymal cells suppresses hepatic inflammation and improves systemic insulin action. Cell Metab 12:237–249. https://doi.org/10.1016/j.cmet.2010.06.011
Nishimoto N, Terao K, Mima T, Nakahara H, Takagi N, Kakehi T (2008) Mechanisms and pathologic significances in increase in serum interleukin-6 (IL-6) and soluble IL-6 receptor after administration of an anti-IL-6 receptor antibody, tocilizumab, in patients with rheumatoid arthritis and Castleman disease. Blood 112:3959–3964. https://doi.org/10.1182/blood-2008-05-155846
Feng W, Liu H, Luo T, Liu D, Du J, Sun J, Wang W, Han X, Yang K, Guo J et al (2017) Combination of IL-6 and sIL-6R differentially regulate varying levels of RANKL-induced osteoclastogenesis through NF-kappaB, ERK and JNK signaling pathways. Sci Rep 7:41411. https://doi.org/10.1038/srep41411
Aparicio-Siegmund S, Garbers Y, Flynn CM, Waetzig GH, Gouni-Berthold I, Krone W, Berthold HK, Laudes M, Rose-John S, Garbers C (2019) The IL-6-neutralizing sIL-6R-sgp130 buffer system is disturbed in patients with type 2 diabetes. Am J Physiol Endocrinol Metab 317:E411–E420. https://doi.org/10.1152/ajpendo.00166.2019
Zhang Z, Tian M, Song R, Xing X, Fan Y, Wang L, Niu C, Dalmo RA (2020) A new IL6 isoform in Chinese soft-shelled turtle (Pelodiscus sinesis) discovered: its regulation during cold stress and infection. Biology (Basel) 9. https://doi.org/10.3390/biology9050111
Carpenter LL, Gawuga CE, Tyrka AR, Lee JK, Anderson GM, Price LH (2010) Association between plasma IL-6 response to acute stress and early-life adversity in healthy adults. Neuropsychopharmacology 35:2617–2623. https://doi.org/10.1038/npp.2010.159
LeMay LG, Vander AJ, Kluger MJ (1990) The effects of psychological stress on plasma interleukin-6 activity in rats. Physiol Behav 47:957–961. https://doi.org/10.1016/0031-9384(90)90024-x
Pedersen BK, Fischer CP (2007) Beneficial health effects of exercise–the role of IL-6 as a myokine. Trends Pharmacol Sci 28:152–156. https://doi.org/10.1016/j.tips.2007.02.002
Rohleder N, Aringer M, Boentert M (2012) Role of interleukin-6 in stress, sleep, and fatigue. Ann N Y Acad Sci 1261:88–96. https://doi.org/10.1111/j.1749-6632.2012.06634.x
Wolf J, Rose-John S, Garbers C (2014) Interleukin-6 and its receptors: a highly regulated and dynamic system. Cytokine 70:11–20. https://doi.org/10.1016/j.cyto.2014.05.024
Bihl MP, Heinimann K, Rudiger JJ, Eickelberg O, Perruchoud AP, Tamm M, Roth M (2002) Identification of a novel IL-6 isoform binding to the endogenous IL-6 receptor. Am J Respir Cell Mol Biol 27:48–56. https://doi.org/10.1165/ajrcmb.27.1.4637
Alberti L, Bachelot T, Duc A, Biota C, Blay JY (2005) A spliced isoform of interleukin 6 mRNA produced by renal cell carcinoma encodes for an interleukin 6 inhibitor. Cancer Res 65:2–5
Rothaug M, Becker-Pauly C, Rose-John S (2016) The role of interleukin-6 signaling in nervous tissue. Biochim Biophys Acta 1863:1218–1227. https://doi.org/10.1016/j.bbamcr.2016.03.018
Parks EE, Logan S, Yeganeh A, Farley JA, Owen DB, Sonntag WE (2020) Interleukin 6 reduces allopregnanolone synthesis in the brain and contributes to age-related cognitive decline in mice. J Lipid Res. https://doi.org/10.1194/jlr.RA119000479
Escrig A, Molinero A, Mendez B, Giralt M, Comes G, Sanchis P, Fernandez-Gayol O, Gimenez-Llort L, Becker-Pauly C, Rose-John S et al (2020) IL-6 trans-signaling in the brain influences the metabolic phenotype of the 3xTg-AD mouse model of Alzheimer’s disease. Cells 9. https://doi.org/10.3390/cells9071605
Gubernatorova EO, Gorshkova EA, Namakanova OA, Zvartsev RV, Hidalgo J, Drutskaya MS, Tumanov AV, Nedospasov SA (2018) Non-redundant functions of IL-6 produced by macrophages and dendritic cells in allergic airway inflammation. Front Immunol 9:2718. https://doi.org/10.3389/fimmu.2018.02718
Jevnikar Z, Ostling J, Ax E, Calven J, Thorn K, Israelsson E, Oberg L, Singhania A, Lau LCK, Wilson SJ et al (2019) Epithelial IL-6 trans-signaling defines a new asthma phenotype with increased airway inflammation. J Allergy Clin Immunol 143:577–590. https://doi.org/10.1016/j.jaci.2018.05.026
Hartman J, Frishman WH (2014) Inflammation and atherosclerosis: a review of the role of interleukin-6 in the development of atherosclerosis and the potential for targeted drug therapy. Cardiol Rev 22:147–151. https://doi.org/10.1097/CRD.0000000000000021
Lavin B, Phinikaridou A, Andia ME, Potter M, Lorrio S, Rashid I, Botnar RM (2020) Sustained focal vascular inflammation accelerates atherosclerosis in remote arteries. Arterioscler Thromb Vasc Biol ATVBAHA120314387. https://doi.org/10.1161/ATVBAHA.120.314387
Parisinos CA, Serghiou S, Katsoulis M, George MJ, Patel RS, Hemingway H, Hingorani AD (2018) Variation in interleukin 6 receptor gene associates with risk of Crohn’s disease and ulcerative colitis. Gastroenterology 155(303–306):e302. https://doi.org/10.1053/j.gastro.2018.05.022
Liu G, Jin S, Jiang Q (2019) Interleukin-6 receptor and inflammatory bowel disease: a Mendelian randomization study. Gastroenterology 156:823–824. https://doi.org/10.1053/j.gastro.2018.09.059
Donate-Correa J, Luis-Rodriguez D, Martin-Nunez E, Tagua VG, Hernandez-Carballo C, Ferri C, Rodriguez-Rodriguez AE, Mora-Fernandez C, Navarro-Gonzalez JF (2020) Inflammatory targets in diabetic nephropathy. J Clin Med 9. https://doi.org/10.3390/jcm9020458
Wang X, Yan Z, Ye Q (2019) Interleukin-6 gene polymorphisms and susceptibility to liver diseases: a meta-analysis. Medicine (Baltimore) 98:e18408. https://doi.org/10.1097/MD.0000000000018408
Magro G (2020) SARS-CoV-2 and COVID-19: is interleukin-6 (IL-6)the ‘culprit lesion’ of ARDS onset? What is there besides tocilizumab? SGP130Fc. Cytokine X 100029. https://doi.org/10.1016/j.cytox.2020.100029
Ragab D, Salah Eldin H, Taeimah M, Khattab R, Salem R (2020) The COVID-19 cytokine storm; what we know so far. Front Immunol 11:1446. https://doi.org/10.3389/fimmu.2020.01446
Andrade BS, Rangel FS, Santos NO, Freitas ADS, Soares WRA, Siqueira S, Barh D, Goes-Neto A, Birbrair A, Azevedo VAC (2020) Repurposing approved drugs for guiding COVID-19 prophylaxis: a systematic review. Front Pharmacol 11:590598. https://doi.org/10.3389/fphar.2020.590598
Novaes TF, Jordao MC, Bonacina CF, Veronezi AO, de Araujo CAR, Olegario IC, de Oliveira DB, Ushakova V, Birbrair A, da Costa PD et al (2021) COVID-19 pandemic impact on dentists in Latin America’s epicenter: Sao-Paulo. Brazil PloS one 16:e0256092. https://doi.org/10.1371/journal.pone.0256092
Rocha ALS, Pinheiro JR, Nakamura TC, da Silva JDS, Rocha BGS, Klein RC, Birbrair A, Amorim JH (2021) Fomites and the environment did not have an important role in COVID-19 transmission in a Brazilian mid-sized city. Sci Rep 11:15960. https://doi.org/10.1038/s41598-021-95479-5
Turnquist C, Ryan BM, Horikawa I, Harris BT, Harris CC (2020) Cytokine storms in cancer and COVID-19. Cancer Cell 38:598–601. https://doi.org/10.1016/j.ccell.2020.09.019
Choy EH, De Benedetti F, Takeuchi T, Hashizume M, John MR, Kishimoto T (2020) Translating IL-6 biology into effective treatments. Nat Rev Rheumatol 16:335–345. https://doi.org/10.1038/s41584-020-0419-z
Del Valle DM, Kim-Schulze S, Huang HH, Beckmann ND, Nirenberg S, Wang B, Lavin Y, Swartz TH, Madduri D, Stock A et al (2020) An inflammatory cytokine signature predicts COVID-19 severity and survival. Nat Med 26:1636–1643. https://doi.org/10.1038/s41591-020-1051-9
Xu X, Han M, Li T, Sun W, Wang D, Fu B, Zhou Y, Zheng X, Yang Y, Li X et al (2020) Effective treatment of severe COVID-19 patients with tocilizumab. Proc Natl Acad Sci U S A 117:10970–10975. https://doi.org/10.1073/pnas.2005615117
Kim GW, Lee NR, Pi RH, Lim YS, Lee YM, Lee JM, Jeong HS, Chung SH (2015) IL-6 inhibitors for treatment of rheumatoid arthritis: past, present, and future. Arch Pharm Res 38:575–584. https://doi.org/10.1007/s12272-015-0569-8
Wang Y, Kala MP, Jafar TH (2020) Factors associated with psychological distress during the coronavirus disease 2019 (COVID-19) pandemic on the predominantly general population: a systematic review and meta-analysis. PLoS ONE 15:e0244630. https://doi.org/10.1371/journal.pone.0244630
Liu N, Zhang F, Wei C, Jia Y, Shang Z, Sun L, Wu L, Sun Z, Zhou Y, Wang Y et al (2020) Prevalence and predictors of PTSS during COVID-19 outbreak in China hardest-hit areas: gender differences matter. Psychiatry Res 287:112921. https://doi.org/10.1016/j.psychres.2020.112921
Brooks SK, Webster RK, Smith LE, Woodland L, Wessely S, Greenberg N, Rubin GJ (2020) The psychological impact of quarantine and how to reduce it: rapid review of the evidence. Lancet 395:912–920. https://doi.org/10.1016/S0140-6736(20)30460-8
Hammen C, Kim EY, Eberhart NK, Brennan PA (2009) Chronic and acute stress and the prediction of major depression in women. Depress Anxiety 26:718–723. https://doi.org/10.1002/da.20571
Roohi E, Jaafari N, Hashemian F (2021) On inflammatory hypothesis of depression: what is the role of IL-6 in the middle of the chaos? J Neuroinflammation 18:45. https://doi.org/10.1186/s12974-021-02100-7
Beck K, Vincent A, Becker C, Keller A, Cam H, Schaefert R, Reinhardt T, Sutter R, Tisljar K, Bassetti S et al (2021) Prevalence and factors associated with psychological burden in COVID-19 patients and their relatives: a prospective observational cohort study. PLoS ONE 16:e0250590. https://doi.org/10.1371/journal.pone.0250590
Zandifar A, Badrfam R, Yazdani S, Arzaghi SM, Rahimi F, Ghasemi S, Khamisabadi S, Khonsari NM, Qorbani M (2020) Prevalence and severity of depression, anxiety, stress and perceived stress in hospitalized patients with COVID-19. J Diabetes Metab Disord 1–8. https://doi.org/10.1007/s40200-020-00667-1
Drubach LA, Palmer EL 3rd, Connolly LP, Baker A, Zurakowski D, Cypess AM (2011) Pediatric brown adipose tissue: detection, epidemiology, and differences from adults. J Pediatr 159:939–944. https://doi.org/10.1016/j.jpeds.2011.06.028
Gilsanz V, Hu HH, Kajimura S (2013) Relevance of brown adipose tissue in infancy and adolescence. Pediatr Res 73:3–9. https://doi.org/10.1038/pr.2012.141
Christner N, Essler S, Hazzam A, Paulus M (2021) Children’s psychological well-being and problem behavior during the COVID-19 pandemic: an online study during the lockdown period in Germany. PLoS ONE 16:e0253473. https://doi.org/10.1371/journal.pone.0253473
Spinelli M, Lionetti F, Pastore M, Fasolo M (2020) Parents’ stress and children’s psychological problems in families facing the COVID-19 outbreak in Italy. Front Psychol 11:1713. https://doi.org/10.3389/fpsyg.2020.01713
Nogrady B (2020) How kids’ immune systems can evade COVID. Nature 588:382. https://doi.org/10.1038/d41586-020-03496-7
Zimmermann P, Curtis N (2020) Why is COVID-19 less severe in children? A review of the proposed mechanisms underlying the age-related difference in severity of SARS-CoV-2 infections. Arch Dis Child. https://doi.org/10.1136/archdischild-2020-320338
Bunyavanich S, Do A, Vicencio A (2020) Nasal gene expression of angiotensin-converting enzyme 2 in children and adults. JAMA 323:2427–2429. https://doi.org/10.1001/jama.2020.8707
Sharif-Askari NS, Sharif-Askari FS, Alabed M, Temsah MH, Al Heialy S, Hamid Q, Halwani R (2020) Airways expression of SARS-CoV-2 receptor, ACE2, and TMPRSS2 is lower in children than adults and increases with smoking and COPD. Mol Ther Methods Clin Dev 18:1–6. https://doi.org/10.1016/j.omtm.2020.05.013
Zhou F, Yu T, Du R, Fan G, Liu Y, Liu Z, Xiang J, Wang Y, Song B, Gu X et al (2020) Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. The Lancet 395:1054–1062. https://doi.org/10.1016/s0140-6736(20)30566-3
Mahbub S, Brubaker AL, Kovacs EJ (2011) Aging of the innate immune system: an update. Curr Immunol Rev 7:104–115. https://doi.org/10.2174/157339511794474181
Palmer DB (2013) The effect of age on thymic function. Front Immunol 4:316. https://doi.org/10.3389/fimmu.2013.00316
Franceschi C, Garagnani P, Parini P, Giuliani C, Santoro A (2018) Inflammaging: a new immune-metabolic viewpoint for age-related diseases. Nat Rev Endocrinol 14:576–590. https://doi.org/10.1038/s41574-018-0059-4
Franceschi C, Bonafe M, Valensin S, Olivieri F, De Luca M, Ottaviani E, De Benedictis G (2000) Inflamm-aging. An evolutionary perspective on immunosenescence. Ann N Y Acad Sci 908:244–254. https://doi.org/10.1111/j.1749-6632.2000.tb06651.x
Heinrich PC, Castell JV, Andus T (1990) Interleukin-6 and the acute phase response. Biochem J 265:621–636. https://doi.org/10.1042/bj2650621
Gabay C (2006) Interleukin-6 and chronic inflammation. Arthritis Res Ther 8(Suppl 2):S3. https://doi.org/10.1186/ar1917
Hansel A, Hong S, Camara RJ, von Kanel R (2010) Inflammation as a psychophysiological biomarker in chronic psychosocial stress. Neurosci Biobehav Rev 35:115–121. https://doi.org/10.1016/j.neubiorev.2009.12.012
Alcala M, Calderon-Dominguez M, Serra D, Herrero L, Viana M (2019) Mechanisms of impaired brown adipose tissue recruitment in obesity. Front Physiol 10:94. https://doi.org/10.3389/fphys.2019.00094
Feldmann HM, Golozoubova V, Cannon B, Nedergaard J (2009) UCP1 ablation induces obesity and abolishes diet-induced thermogenesis in mice exempt from thermal stress by living at thermoneutrality. Cell Metab 9:203–209. https://doi.org/10.1016/j.cmet.2008.12.014
El-Mikkawy DME, El-Sadek MA, El-Badawy MA, Samaha D (2020) Circulating level of interleukin-6 in relation to body mass indices and lipid profile in Egyptian adults with overweight and obesity. Egyptian Rheumatology and Rehabilitation 47. https://doi.org/10.1186/s43166-020-00003-8
Jonas MI, Kurylowicz A, Bartoszewicz Z, Lisik W, Jonas M, Wierzbicki Z, Chmura A, Pruszczyk P, Puzianowska-Kuznicka M (2015) Interleukins 6 and 15 levels are higher in subcutaneous adipose tissue, but obesity is associated with their increased content in visceral fat depots. Int J Mol Sci 16:25817–25830. https://doi.org/10.3390/ijms161025817
Fontana L, Eagon JC, Trujillo ME, Scherer PE, Klein S (2007) Visceral fat adipokine secretion is associated with systemic inflammation in obese humans. Diabetes 56:1010–1013. https://doi.org/10.2337/db06-1656
Wallenius V, Wallenius K, Ahren B, Rudling M, Carlsten H, Dickson SL, Ohlsson C, Jansson JO (2002) Interleukin-6-deficient mice develop mature-onset obesity. Nat Med 8:75–79. https://doi.org/10.1038/nm0102-75
Li L, Huang C, Yin H, Zhang X, Wang D, Ma C, Li J, Zhao Y, Li X (2021) Interleukin-6 mediated exercise-induced alleviation of adiposity and hepatic steatosis in mice. BMJ Open Diabetes Res Care 9. https://doi.org/10.1136/bmjdrc-2020-001431
Di Gregorio GB, Hensley L, Lu T, Ranganathan G, Kern PA (2004) Lipid and carbohydrate metabolism in mice with a targeted mutation in the IL-6 gene: absence of development of age-related obesity. Am J Physiol Endocrinol Metab 287:E182-187. https://doi.org/10.1152/ajpendo.00189.2003
Picoli CC, Costa AC, Rocha BGS, Silva WN, Santos GSP, Prazeres P, Costa PAC, Oropeza A, da Silva RA, Azevedo VAC et al (2021) Sensory nerves in the spotlight of the stem cell niche. Stem Cells Transl Med 10:346–356. https://doi.org/10.1002/sctm.20-0284
Hayakawa Y, Sakitani K, Konishi M, Asfaha S, Niikura R, Tomita H, Renz BW, Tailor Y, Macchini M, Middelhoff M et al (2017) Nerve growth factor promotes gastric tumorigenesis through aberrant cholinergic signaling. Cancer Cell 31:21–34. https://doi.org/10.1016/j.ccell.2016.11.005
Zhao CM, Hayakawa Y, Kodama Y, Muthupalani S, Westphalen CB, Andersen GT, Flatberg A, Johannessen H, Friedman RA, Renz BW et al (2014) Denervation suppresses gastric tumorigenesis. Sci Transl Med 6:250ra115. https://doi.org/10.1126/scitranslmed.3009569
Renz BW, Takahashi R, Tanaka T, Macchini M, Hayakawa Y, Dantes Z, Maurer HC, Chen X, Jiang Z, Westphalen CB et al (2018) beta2 Adrenergic-neurotrophin feedforward loop promotes pancreatic cancer. Cancer Cell 34:863–867. https://doi.org/10.1016/j.ccell.2018.10.010
Magnon C, Hall SJ, Lin J, Xue X, Gerber L, Freedland SJ, Frenette PS (2013) Autonomic nerve development contributes to prostate cancer progression. Science 341:1236361. https://doi.org/10.1126/science.1236361
Zahalka AH, Arnal-Estape A, Maryanovich M, Nakahara F, Cruz CD, Finley LWS, Frenette PS (2017) Adrenergic nerves activate an angio-metabolic switch in prostate cancer. Science 358:321–326. https://doi.org/10.1126/science.aah5072
Prazeres P, Leonel C, Silva WN, Rocha BGS, Santos GSP, Costa AC, Picoli CC, Sena IFG, Goncalves WA, Vieira MS et al (2020) Ablation of sensory nerves favours melanoma progression. J Cell Mol Med. https://doi.org/10.1111/jcmm.15381
Costa PAC, Silva WN, Prazeres PHDM, Picoli CC, Guardia GDA, Costa AC, Oliveira MA, Guimarães PPG, Gonçalves R, Pinto MCX et al (2021) Chemogenetic modulation of sensory neurons reveals their regulating role on melanoma progression. Acta Neuropathologica Communications In press. https://doi.org/10.1186/s40478-021-01273-9
Lemeshow S, Sorensen HT, Phillips G, Yang EV, Antonsen S, Riis AH, Lesinski GB, Jackson R, Glaser R (2011) beta-Blockers and survival among Danish patients with malignant melanoma: a population-based cohort study. Cancer Epidemiol Biomarkers Prev 20:2273–2279. https://doi.org/10.1158/1055-9965.EPI-11-0249
Sena IFG, Rocha BGS, Picoli CC, Santos GSP, Costa AC, Goncalves BOP, Garcia APV, Soltani-Asl M, Coimbra-Campos LMC, Silva WN et al (2021) C(3)1-TAg in C57BL/6 J background as a model to study mammary tumor development. Histochem Cell Biol. https://doi.org/10.1007/s00418-021-01995-w
Balaban S, Lee LS, Schreuder M, Hoy AJ (2015) Obesity and cancer progression: is there a role of fatty acid metabolism? Biomed Res Int 2015:274585. https://doi.org/10.1155/2015/274585
Ye H, Adane B, Khan N, Sullivan T, Minhajuddin M, Gasparetto M, Stevens B, Pei S, Balys M, Ashton JM et al (2016) Leukemic stem cells evade chemotherapy by metabolic adaptation to an adipose tissue niche. Cell Stem Cell 19:23–37. https://doi.org/10.1016/j.stem.2016.06.001
Laurent V, Guerard A, Mazerolles C, Le Gonidec S, Toulet A, Nieto L, Zaidi F, Majed B, Garandeau D, Socrier Y et al (2016) Periprostatic adipocytes act as a driving force for prostate cancer progression in obesity. Nat Commun 7:10230. https://doi.org/10.1038/ncomms10230
Nieman KM, Romero IL, Van Houten B, Lengyel E (2013) Adipose tissue and adipocytes support tumorigenesis and metastasis. Biochim Biophys Acta 1831:1533–1541. https://doi.org/10.1016/j.bbalip.2013.02.010
Dirat B, Bochet L, Dabek M, Daviaud D, Dauvillier S, Majed B, Wang YY, Meulle A, Salles B, Le Gonidec S et al (2011) Cancer-associated adipocytes exhibit an activated phenotype and contribute to breast cancer invasion. Cancer Res 71:2455–2465. https://doi.org/10.1158/0008-5472.CAN-10-3323
Picon-Ruiz M, Pan C, Drews-Elger K, Jang K, Besser AH, Zhao D, Morata-Tarifa C, Kim M, Ince TA, Azzam DJ et al (2016) Interactions between adipocytes and breast cancer cells stimulate cytokine production and drive Src/Sox2/miR-302b-mediated malignant progression. Cancer Res 76:491–504. https://doi.org/10.1158/0008-5472.CAN-15-0927
Balaban S, Shearer RF, Lee LS, van Geldermalsen M, Schreuder M, Shtein HC, Cairns R, Thomas KC, Fazakerley DJ, Grewal T et al (2017) Adipocyte lipolysis links obesity to breast cancer growth: adipocyte-derived fatty acids drive breast cancer cell proliferation and migration. Cancer Metab 5:1. https://doi.org/10.1186/s40170-016-0163-7
Park J, Morley TS, Kim M, Clegg DJ, Scherer PE (2014) Obesity and cancer–mechanisms underlying tumour progression and recurrence. Nat Rev Endocrinol 10:455–465. https://doi.org/10.1038/nrendo.2014.94
Lengyel E, Makowski L, DiGiovanni J, Kolonin MG (2018) Cancer as a matter of fat: the crosstalk between adipose tissue and tumors. Trends Cancer 4:374–384. https://doi.org/10.1016/j.trecan.2018.03.004
Birbrair A, Sattiraju A, Zhu D, Zulato G, Batista I, Nguyen VT, Messi ML, Sai KKS, Marini FC, Delbono O et al (2017) Novel peripherally derived neural-like stem cells as therapeutic carriers for treating glioblastomas. Stem Cells Transl Med 6:471–481. https://doi.org/10.5966/sctm.2016-0007
Birbrair A, Zhang T, Wang ZM, Messi ML, Olson JD, Mintz A, Delbono O (2014) Type-2 pericytes participate in normal and tumoral angiogenesis. Am J Physiol Cell Physiol 307:C25-38. https://doi.org/10.1152/ajpcell.00084.2014
Birbrair A, Frenette PS (2016) Niche heterogeneity in the bone marrow. Ann N Y Acad Sci 1370:82–96. https://doi.org/10.1111/nyas.13016
Paiva AE, Lousado L, Guerra DAP, Azevedo PO, Sena IFG, Andreotti JP, Santos GSP, Goncalves R, Mintz A, Birbrair A (2018) Pericytes in the premetastatic niche. Cancer Res 78:2779–2786. https://doi.org/10.1158/0008-5472.CAN-17-3883
Picoli CC, Goncalves BOP, Santos GSP, Rocha BGS, Costa AC, Resende RR, Birbrair A (2021) Pericytes cross-talks within the tumor microenvironment. Biochim Biophys Acta Rev Cancer 1876:188608. https://doi.org/10.1016/j.bbcan.2021.188608
Azevedo PO, Paiva AE, Santos GSP, Lousado L, Andreotti JP, Sena IFG, Tagliati CA, Mintz A, Birbrair A (2018) Cross-talk between lung cancer and bones results in neutrophils that promote tumor progression. Cancer Metastasis Rev 37:779–790. https://doi.org/10.1007/s10555-018-9759-4
Paiva AE, Lousado L, Almeida VM, Andreotti JP, Santos GSP, Azevedo PO, Sena IFG, Prazeres P, Borges IT, Azevedo V et al (2017) Endothelial cells as precursors for osteoblasts in the metastatic prostate cancer bone. Neoplasia 19:928–931. https://doi.org/10.1016/j.neo.2017.08.007
de Alvarenga EC, Silva WN, Vasconcellos R, Paredes-Gamero EJ, Mintz A, Birbrair A (2018) Promyelocytic leukemia protein in mesenchymal stem cells is essential for leukemia progression. Ann Hematol 97:1749–1755. https://doi.org/10.1007/s00277-018-3463-x
Guerra DAP, Paiva AE, Sena IFG, Azevedo PO, Silva WN, Mintz A, Birbrair A (2018) Targeting glioblastoma-derived pericytes improves chemotherapeutic outcome. Angiogenesis 21:667–675. https://doi.org/10.1007/s10456-018-9621-x
Sena IFG, Paiva AE, Prazeres P, Azevedo PO, Lousado L, Bhutia SK, Salmina AB, Mintz A, Birbrair A (2018) Glioblastoma-activated pericytes support tumor growth via immunosuppression. Cancer Med 7:1232–1239. https://doi.org/10.1002/cam4.1375
Valle IB, Schuch LF, da Silva JM, Gala-Garcia A, Diniz IMA, Birbrair A, Abreu LG, Silva TA (2020) Pericyte in oral squamous cell carcinoma: a systematic review. Head Neck Pathol 14:1080–1091. https://doi.org/10.1007/s12105-020-01188-2
Bernardes SS, Pinto MCX, Amorim JH, Azevedo VAC, Resende RR, Mintz A, Birbrair A (2020) Glioma pericytes promote angiogenesis by producing periostin. Cell Mol Neurobiol. https://doi.org/10.1007/s10571-020-00975-3
Incio J, Ligibel JA, McManus DT, Suboj P, Jung K, Kawaguchi K, Pinter M, Babykutty S, Chin SM, Vardam TD et al (2018) Obesity promotes resistance to anti-VEGF therapy in breast cancer by up-regulating IL-6 and potentially FGF-2. Sci Transl Med 10. https://doi.org/10.1126/scitranslmed.aag0945
Gyamfi J, Lee YH, Eom M, Choi J (2018) Interleukin-6/STAT3 signalling regulates adipocyte induced epithelial-mesenchymal transition in breast cancer cells. Sci Rep 8:8859. https://doi.org/10.1038/s41598-018-27184-9
Burysek L, Houstek J (1997) beta-Adrenergic stimulation of interleukin-1alpha and interleukin-6 expression in mouse brown adipocytes. FEBS Lett 411:83–86. https://doi.org/10.1016/s0014-5793(97)00671-6
Kristof E, Klusoczki A, Veress R, Shaw A, Combi ZS, Varga K, Gyory F, Balajthy Z, Bai P, Bacso Z et al (2019) Interleukin-6 released from differentiating human beige adipocytes improves browning. Exp Cell Res 377:47–55. https://doi.org/10.1016/j.yexcr.2019.02.015
Petruzzelli M, Schweiger M, Schreiber R, Campos-Olivas R, Tsoli M, Allen J, Swarbrick M, Rose-John S, Rincon M, Robertson G et al (2014) A switch from white to brown fat increases energy expenditure in cancer-associated cachexia. Cell Metab 20:433–447. https://doi.org/10.1016/j.cmet.2014.06.011
Han J, Meng Q, Shen L, Wu G (2018) Interleukin-6 induces fat loss in cancer cachexia by promoting white adipose tissue lipolysis and browning. Lipids Health Dis 17:14. https://doi.org/10.1186/s12944-018-0657-0
Narsale AA, Carson JA (2014) Role of interleukin-6 in cachexia: therapeutic implications. Curr Opin Support Palliat Care 8:321–327. https://doi.org/10.1097/SPC.0000000000000091
Felger JC, Lotrich FE (2013) Inflammatory cytokines in depression: neurobiological mechanisms and therapeutic implications. Neuroscience 246:199–229. https://doi.org/10.1016/j.neuroscience.2013.04.060
Khandaker GM, Pearson RM, Zammit S, Lewis G, Jones PB (2014) Association of serum interleukin 6 and C-reactive protein in childhood with depression and psychosis in young adult life: a population-based longitudinal study. JAMA Psychiat 71:1121–1128. https://doi.org/10.1001/jamapsychiatry.2014.1332
van Baak MA, Hul GB, Toubro S, Astrup A, Gottesdiener KM, DeSmet M, Saris WH (2002) Acute effect of L-796568, a novel beta 3-adrenergic receptor agonist, on energy expenditure in obese men. Clin Pharmacol Ther 71:272–279. https://doi.org/10.1067/mcp.2002.122527
Jespersen NZ, Larsen TJ, Peijs L, Daugaard S, Homoe P, Loft A, de Jong J, Mathur N, Cannon B, Nedergaard J et al (2013) A classical brown adipose tissue mRNA signature partly overlaps with brite in the supraclavicular region of adult humans. Cell Metab 17:798–805. https://doi.org/10.1016/j.cmet.2013.04.011
Guller I, McNaughton S, Crowley T, Gilsanz V, Kajimura S, Watt M, Russell AP (2015) Comparative analysis of microRNA expression in mouse and human brown adipose tissue. BMC Genomics 16:820. https://doi.org/10.1186/s12864-015-2045-8
van Dam M, Mullberg J, Schooltink H, Stoyan T, Brakenhoff JP, Graeve L, Heinrich PC, Rose-John S (1993) Structure-function analysis of interleukin-6 utilizing human/murine chimeric molecules. Involvement of two separate domains in receptor binding. J Biol Chem 268:15285–15290
Coulie PG, Stevens M, Van Snick J (1989) High- and low-affinity receptors for murine interleukin 6. Distinct distribution on B and T cells. Eur J Immunol 19:2107–2114. https://doi.org/10.1002/eji.1830191121
Wiesinger MY, Haan S, Wuller S, Kauffmann ME, Recker T, Kuster A, Heinrich PC, Muller-Newen G (2009) Development of an IL-6 inhibitor based on the functional analysis of murine IL-6Ralpha(1). Chem Biol 16:783–794. https://doi.org/10.1016/j.chembiol.2009.06.010
Okazaki M, Yamada Y, Nishimoto N, Yoshizaki K, Mihara M (2002) Characterization of anti-mouse interleukin-6 receptor antibody. Immunol Lett 84:231–240. https://doi.org/10.1016/s0165-2478(02)00202-x
Garbers C, Thaiss W, Jones GW, Waetzig GH, Lorenzen I, Guilhot F, Lissilaa R, Ferlin WG, Grotzinger J, Jones SA et al (2011) Inhibition of classic signaling is a novel function of soluble glycoprotein 130 (sgp130), which is controlled by the ratio of interleukin 6 and soluble interleukin 6 receptor. J Biol Chem 286:42959–42970. https://doi.org/10.1074/jbc.M111.295758
Nishimoto N, Kishimoto T, Yoshizaki K (2000) Anti-interleukin 6 receptor antibody treatment in rheumatic disease. Ann Rheum Dis 59(Suppl 1):i21-27. https://doi.org/10.1136/ard.59.suppl_1.i21
Lokau J, Kleinegger F, Garbers Y, Waetzig GH, Grotzinger J, Rose-John S, Haybaeck J, Garbers C (2020) Tocilizumab does not block interleukin-6 (IL-6) signaling in murine cells. PLoS ONE 15:e0232612. https://doi.org/10.1371/journal.pone.0232612
Verduci E, Calcaterra V, Di Profio E, Fiore G, Rey F, Magenes VC, Todisco CF, Carelli S, Zuccotti GV (2021) Brown adipose tissue: new challenges for prevention of childhood obesity. a narrative review. Nutrients 13. https://doi.org/10.3390/nu13051450
Koksharova E, Ustyuzhanin D, Philippov Y, Mayorov A, Shestakova M, Shariya M, Ternovoy S, Dedov I (2017) The relationship between brown adipose tissue content in supraclavicular fat depots and insulin sensitivity in patients with type 2 diabetes mellitus and prediabetes. Diabetes Technol Ther 19:96–102. https://doi.org/10.1089/dia.2016.0360
Scalzo RL, Peltonen GL, Giordano GR, Binns SE, Klochak AL, Paris HL, Schweder MM, Szallar SE, Wood LM, Larson DG et al (2014) Regulators of human white adipose browning: evidence for sympathetic control and sexual dimorphic responses to sprint interval training. PLoS ONE 9:e90696. https://doi.org/10.1371/journal.pone.0090696
Cao Q, Jing J, Cui X, Shi H, Xue B (2019) Sympathetic nerve innervation is required for beigeing in white fat. Physiol Rep 7:e14031. https://doi.org/10.14814/phy2.14031
Carey AL, Bruce CR, Sacchetti M, Anderson MJ, Olsen DB, Saltin B, Hawley JA, Febbraio MA (2004) Interleukin-6 and tumor necrosis factor-alpha are not increased in patients with type 2 diabetes: evidence that plasma interleukin-6 is related to fat mass and not insulin responsiveness. Diabetologia 47:1029–1037. https://doi.org/10.1007/s00125-004-1403-x
Wueest S, Konrad D (2020) The controversial role of IL-6 in adipose tissue on obesity-induced dysregulation of glucose metabolism. Am J Physiol Endocrinol Metab 319:E607–E613. https://doi.org/10.1152/ajpendo.00306.2020
Bartness TJ (2002) Dual innervation of white adipose tissue: some evidence for parasympathetic nervous system involvement. J Clin Invest 110:1235–1237. https://doi.org/10.1172/JCI17047
Bartness TJ, Liu Y, Shrestha YB, Ryu V (2014) Neural innervation of white adipose tissue and the control of lipolysis. Front Neuroendocrinol 35:473–493. https://doi.org/10.1016/j.yfrne.2014.04.001
Funding
Alexander Birbrair is supported by a grant from Instituto Serrapilheira/Serra-1708–15285, a grant from Pró-reitoria de Pesquisa/Universidade Federal de Minas Gerais (PRPq/UFMG) (Edital 05/2016), a grant from CNPQ (Universal, Process No. 405977/2018–2), a grant from National Institute of Science and Technology in Theranostics and Nanobiotechnology (CNPq/CAPES/FAPEMIG, Process No. 465669/2014–0), a grant from Fundação de Amparo à Pesquisa do Estado de Minas Gerais — FAPEMIG (Chamada N°01/2021 — Demanda Universal, APQ-01321–21), a grant from FAPEMIG (Rede Mineira de Engenharia de Tecidos e Terapia Celular (REMETTEC, RED-00570–16)], a grant from FAPEMIG [Rede De Pesquisa Em Doenças Infecciosas Humanas E Animais Do Estado De Minas Gerais (RED-00313–16)), and a productivity fellowship from the National Council for Scientific and Technological Development (CNPq); Akiva Mintz is supported by the National Institutes of Health (1R01CA179072-01A1) and by the American Cancer Society Mentored Research Scholar grant (124443-MRSG-13–121-01-CDD). CCP and ACC are supported by doctoral fellowships from CAPES. GSPS and SOS are supported by a doctoral fellowship from CNPq. BGSR is supported by a master fellowship from CAPES. Miguel L Batista Jr is supported a grant for FAPESP 2018/20905-1 and CNPq 311319/2018-1.
Author information
Authors and Affiliations
Contributions
GSPS, ACC, CCP, BGSR, SOS, DCR, MCXP, MLBJ, JHA, VACA, RRR, NOSC, AM, and AB performed the literature search, reviewed the content, edited the text, and critically revised the work. GSPS, ACC, CCP, BGSR, and SOS created the figures and table. AB wrote and approved the final manuscript. All the authors commented on the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Gabryella S. P. Santos Alinne C. Costa Caroline C. Picoli are co-first authors
Rights and permissions
About this article
Cite this article
Santos, G.S.P., Costa, A.C., Picoli, C.C. et al. Sympathetic nerve-adipocyte interactions in response to acute stress. J Mol Med 100, 151–165 (2022). https://doi.org/10.1007/s00109-021-02157-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00109-021-02157-0