Abstract
Background
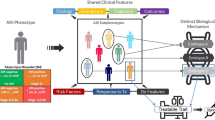
The miRNA profile is changed after burn or sepsis and is involved in regulating inflammatory reactions. However, the function and molecular mechanism of miRNAs in regulating burn sepsis-induced acute kidney injury (AKI) are still unclear.
Methods
In this study, animal and cell sepsis models were established after burned rats were injected with lipopolysaccharide (LPS) or NRK-52E cells treated with LPS, respectively. Cytokine expression, inflammatory cell infiltration, serum creatinine (Scr) and kidney injury molecule-1 (KIM-1) levels were analysed after the indicated treatments.
Results
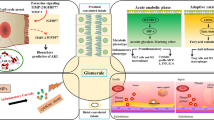
Burn sepsis increased the expression of inflammatory factors (TNF-α and IL-1β) and chemokines (MIP-1α, MIP-2 and MCP-1). Moreover, burn sepsis promoted macrophage and neutrophil infiltration into the kidney and upregulated the levels of Scr and KIM-1 in the kidney and urine. Ectopic expression of miR-181c significantly reduced LPS-induced TLR4 protein expression, suppressed KIM-1 mRNA levels and subsequently inhibited the activation of inflammatory genes (TNF-α and IL-1β) and chemokine genes (MIP-1α, MIP-2 and MCP-1).
Conclusions
Our results demonstrated that miR-181c could suppress TLR4 expression, reduce inflammatory factor and chemokine secretion, mitigate inflammatory cell infiltration into the kidney and downregulate KIM-1 expression, which might ultimately attenuate burn sepsis-induced AKI.





Similar content being viewed by others
References
Snell JA, Loh NH, Mahambrey T, Shokrollahi K. Clinical review: the critical care management of the burn patient. Crit Care. 2013;17(5):241. https://doi.org/10.1186/cc12706.
Jeschke MG, van Baar ME, Choudhry MA, Chung KK, Gibran NS, Logsetty S. Burn injury. Nat Rev Dis Primers. 2020;6(1):11. https://doi.org/10.1038/s41572-020-0145-5.
Cecconi M, Evans L, Levy M, Rhodes A. Sepsis and septic shock. Lancet. 2018;392(10141):75–87. https://doi.org/10.1016/S0140-6736(18)30696-2.
Rech MA, Mosier MJ, McConkey K, Zelisko S, Netzer G, Kovacs EJ, et al. Outcomes in burn-injured patients who develop sepsis. J Burn Care Res. 2019;40(3):269–73. https://doi.org/10.1093/jbcr/irz017.
AbuBakr HO, Aljuaydi SH, Abou-Zeid SM, El-Bahrawy A. Burn-induced multiple organ injury and protective effect of lutein in rats. Inflammation. 2018;41(3):760–72. https://doi.org/10.1007/s10753-018-0730-x.
Yu YH, Gaine GK, Zhou LY, Zhang JJ, Wang J, Sun BG. The classical and potential novel healthy functions of rice bran protein and its hydrolysates. Crit Rev Food Sci. 2021. https://doi.org/10.1080/10408398.2021.1929057.
Folkestad T, Brurberg KG, Nordhuus KM, Tveiten CK, Guttormsen AB, Os I, et al. Acute kidney injury in burn patients admitted to the intensive care unit: a systematic review and meta-analysis. Crit Care. 2020;24(1):2. https://doi.org/10.1186/s13054-019-2710-4.
Rakkolainen I, Lindbohm JV, Vuola J. Factors associated with acute kidney injury in the Helsinki Burn Centre in 2006–2015. Scand J Trauma Resusc Emerg Med. 2018;26(1):105. https://doi.org/10.1186/s13049-018-0573-3.
Emami A, Javanmardi F, Rajaee M, Pirbonyeh N, Keshavarzi A, Fotouhi M, et al. Predictive biomarkers for acute kidney injury in burn patients. J Burn Care Res. 2019;40(5):601–5. https://doi.org/10.1093/jbcr/irz065.
Assadi F, Sharbaf FG. Urine KIM-1 as a potential biomarker of acute renal injury after circulatory collapse in children. Pediatr Emerg Care. 2019;35(2):104–7. https://doi.org/10.1097/PEC.0000000000000886.
Munoz B, Suarez-Sanchez R, Hernandez-Hernandez O, Franco-Cendejas R, Cortes H, Magana JJ. From traditional biochemical signals to molecular markers for detection of sepsis after burn injuries. Burns. 2019;45(1):16–31. https://doi.org/10.1016/j.burns.2018.04.016.
Zou YF, Zhang W. Role of microRNA in the detection, progression, and intervention of acute kidney injury. Exp Biol Med (Maywood). 2018;243(2):129–36. https://doi.org/10.1177/1535370217749472.
Yu YH, Zhang JJ, Wang J, Sun BG. MicroRNAs: the novel mediators for nutrient-modulating biological functions. Trends Food Sci Tech. 2021;114:167–75. https://doi.org/10.1016/j.tifs.2021.05.028.
Liang P, Lv C, Jiang B, Long X, Zhang P, Zhang M, et al. MicroRNA profiling in denatured dermis of deep burn patients. Burns. 2012;38(4):534–40. https://doi.org/10.1016/j.burns.2011.10.014.
Zhang Y, Yin B, Shu B, Liu Z, Ding H, Jia C. Differential expression of microRNA let-7b-5p regulates burn-induced hyperglycemia. Oncotarget. 2017;8(42):72886–92. https://doi.org/10.18632/oncotarget.20543.
Yu Y, Chai J, Zhang H, Chu W, Liu L, Ma L, et al. miR-194 Promotes burn-induced hyperglycemia via attenuating IGF-IR expression. Shock. 2014;42(6):578–84. https://doi.org/10.1097/SHK.0000000000000258.
Yu Y, Li X, Liu L, Chai J, Haijun Z, Chu W, et al. miR-628 promotes burn-induced skeletal muscle atrophy via targeting IRS1. Int J Biol Sci. 2016;12(10):1213–24. https://doi.org/10.7150/ijbs.15496.
Yu Y, Yang L, Han S, Wu Y, Liu L, Chang Y, et al. MIR-190B alleviates cell autophagy and burn-induced skeletal muscle wasting via modulating PHLPP1/Akt/FoxO3A signaling pathway. Shock. 2019;52(5):513–21. https://doi.org/10.1097/SHK.0000000000001284.
Li X, Liu L, Yang J, Yu Y, Chai J, Wang L, et al. Exosome derived from human umbilical cord mesenchymal stem cell mediates MiR-181c attenuating burn-induced excessive inflammation. EBioMedicine. 2016;8:72–82. https://doi.org/10.1016/j.ebiom.2016.04.030.
Yu Y, Chai J. The function of miRNAs and their potential as therapeutic targets in burn-induced insulin resistance (review). Int J Mol Med. 2015;35(2):305–10. https://doi.org/10.3892/ijmm.2014.2023.
Yu Y, Chu W, Chai J, Li X, Liu L, Ma L. Critical role of miRNAs in mediating skeletal muscle atrophy (Review). Mol Med Rep. 2016;13(2):1470–4. https://doi.org/10.3892/mmr.2015.4748.
Ju M, Liu B, He H, Gu Z, Liu Y, Su Y, et al. MicroRNA-27a alleviates LPS-induced acute lung injury in mice via inhibiting inflammation and apoptosis through modulating TLR4/MyD88/NF-kappaB pathway. Cell Cycle. 2018;17(16):2001–18. https://doi.org/10.1080/15384101.2018.1509635.
Zhang W, Shu L. Upregulation of miR-21 by ghrelin ameliorates ischemia/reperfusion-induced acute kidney injury by inhibiting inflammation and cell apoptosis. DNA Cell Biol. 2016;35(8):417–25. https://doi.org/10.1089/dna.2016.3231.
Zhao F, Yu Y, Liu W, Zhang J, Liu X, Liu L, et al. Small molecular weight soybean protein-derived peptides nutriment attenuates rat burn injury-induced muscle atrophy by modulation of ubiquitin-proteasome system and autophagy signaling pathway. J Agric Food Chem. 2018;66(11):2724–34. https://doi.org/10.1021/acs.jafc.7b05387.
Napier BA, Andres-Terre M, Massis LM, Hryckowian AJ, Higginbottom SK, Cumnock K, et al. Western diet regulates immune status and the response to LPS-driven sepsis independent of diet-associated microbiome. Proc Natl Acad Sci USA. 2019;116(9):3688–94. https://doi.org/10.1073/pnas.1814273116.
Nair AR, Masson GS, Ebenezer PJ, Del Piero F, Francis J. Role of TLR4 in lipopolysaccharide-induced acute kidney injury: protection by blueberry. Free Radical Biol Med. 2014;71:16–25. https://doi.org/10.1016/j.freeradbiomed.2014.03.012.
Ronco C, Bellomo R, Kellum JA. Acute kidney injury. Lancet. 2019;394(10212):1949–64. https://doi.org/10.1016/S0140-6736(19)32563-2.
Harrois A, Libert N, Duranteau J. Acute kidney injury in trauma patients. Curr Opin Crit Care. 2017;23(6):447–56. https://doi.org/10.1097/MCC.0000000000000463.
Rabb H, Griffin MD, McKay DB, Swaminathan S, Pickkers P, Rosner MH, et al. Inflammation in AKI: current understanding, key questions, and knowledge gaps. J Am Soc Nephrol. 2016;27(2):371–9. https://doi.org/10.1681/ASN.2015030261.
Ren Q, Guo F, Tao S, Huang R, Ma L, Fu P. Flavonoid fisetin alleviates kidney inflammation and apoptosis via inhibiting Src-mediated NF-kappaB p65 and MAPK signaling pathways in septic AKI mice. Biomed Pharmacother. 2020;122:109772. https://doi.org/10.1016/j.biopha.2019.109772.
Inaba A, Tuong ZK, Riding AM, Mathews RJ, Martin JL, Saeb-Parsy K, et al. B lymphocyte-derived CCL7 augments neutrophil and monocyte recruitment. Exacerbating Acute Kidney Injury J Immunol. 2020;205(5):1376–84. https://doi.org/10.4049/jimmunol.2000454.
Rabadi MM, Han SJ, Kim M, D’Agati V, Lee HT. Peptidyl arginine deiminase-4 exacerbates ischemic AKI by finding NEMO. Am J Physiol Renal Physiol. 2019;316(6):F1180–90. https://doi.org/10.1152/ajprenal.00089.2019.
Martin-Sanchez D, Ruiz-Andres O, Poveda J, Carrasco S, Cannata-Ortiz P, Sanchez-Nino MD, et al. Ferroptosis, but not necroptosis, is important in nephrotoxic folic acid-induced AKI. J Am Soc Nephrol. 2017;28(1):218–29. https://doi.org/10.1681/ASN.2015121376.
Winchurch RA, Thupari JN, Munster AM. Endotoxemia in burn patients: levels of circulating endotoxins are related to burn size. Surgery. 1987;102(5):808–12.
O’Neill LA, Bowie AG. The family of five: TIR-domain-containing adaptors in Toll-like receptor signalling. Nat Rev Immunol. 2007;7(5):353–64. https://doi.org/10.1038/nri2079.
Suzuki N, Suzuki S, Yeh WC. IRAK-4 as the central TIR signaling mediator in innate immunity. Trends Immunol. 2002;23(10):503–6. https://doi.org/10.1016/s1471-4906(02)02298-6.
Yu Y, Zhou L, Li X, Liu J, Li H, Gong L, et al. The progress of nomenclature, structure, metabolism, and bioactivities of oat novel phytochemical: avenanthramides. J Agric Food Chem. 2022;70(2):446–57. https://doi.org/10.1021/acs.jafc.1c05704.
Gorina R, Font-Nieves M, Marquez-Kisinousky L, Santalucia T, Planas AM. Astrocyte TLR4 activation induces a proinflammatory environment through the interplay between MyD88-dependent NFkappaB signaling, MAPK, and Jak1/Stat1 pathways. Glia. 2011;59(2):242–55. https://doi.org/10.1002/glia.21094.
Yu Y, Zhang D, Huang H, Li J, Zhang M, Wan Y, et al. NF-kappaB1 p50 promotes p53 protein translation through miR-190 downregulation of PHLPP1. Oncogene. 2014;33(8):996–1005. https://doi.org/10.1038/onc.2013.8.
Gaede L, Liebetrau C, Blumenstein J, Troidl C, Dorr O, Kim WK, et al. Plasma microRNA-21 for the early prediction of acute kidney injury in patients undergoing major cardiac surgery. Nephrol Dial Transplant. 2016;31(5):760–6. https://doi.org/10.1093/ndt/gfw007.
Li YF, Jing Y, Hao J, Frankfort NC, Zhou X, Shen B, et al. MicroRNA-21 in the pathogenesis of acute kidney injury. Protein Cell. 2013;4(11):813–9. https://doi.org/10.1007/s13238-013-3085-y.
Zhang L, He S, Wang Y, Zhu X, Shao W, Xu Q, et al. miRNA-20a suppressed lipopolysaccharide-induced HK-2 cells injury via NFkappaB and ERK1/2 signaling by targeting CXCL12. Mol Immunol. 2020;118:117–23. https://doi.org/10.1016/j.molimm.2019.12.009.
Li X, Liao J, Su X, Li W, Bi Z, Wang J, et al. Human urine-derived stem cells protect against renal ischemia/reperfusion injury in a rat model via exosomal miR-146a-5p which targets IRAK1. Theranostics. 2020;10(21):9561–78. https://doi.org/10.7150/thno.42153.
Lech M, Grobmayr R, Ryu M, Lorenz G, Hartter I, Mulay SR, et al. Macrophage phenotype controls long-term AKI outcomes–kidney regeneration versus atrophy. J Am Soc Nephrol. 2014;25(2):292–304. https://doi.org/10.1681/ASN.2013020152.
Lv LL, Feng Y, Wu M, Wang B, Li ZL, Zhong X, et al. Exosomal miRNA-19b-3p of tubular epithelial cells promotes M1 macrophage activation in kidney injury. Cell Death Differ. 2020;27(1):210–26. https://doi.org/10.1038/s41418-019-0349-y.
Funding
This work was supported by the Beijing Nova Program (Z181100006218043), the National Natural Science foundation of China (81772067) and the Beijing Natural Science Foundation (7172210).
Author information
Authors and Affiliations
Contributions
YHY, XL, JJZ and JKC conceived the study; YHY and XL performed the experiments; YHY, XL, SFH, JW, JJZ and JKC analyzed the data; YHY and JJZ wrote the manuscript; JJZ and JKC approved the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethics approval and consent to participate
All procedures for animal model had been approved, and the approval number was PONY-2020-FL-43.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, Y., Li, X., Han, S. et al. miR-181c, a potential mediator for acute kidney injury in a burn rat model with following sepsis. Eur J Trauma Emerg Surg 49, 1035–1045 (2023). https://doi.org/10.1007/s00068-022-02124-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-022-02124-5