Abstract
Background
Perforated peptic ulcer (PPU) has been associated with substantially high incidence of morbidity and mortality. The aim of this study was to analyze the factors affecting the outcome of patients having perforated peptic ulcer undergoing surgical intervention.
Materials and methods
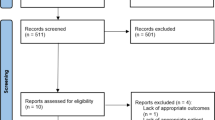
Medical records of 112 patients with PPU who underwent emergency laparotomy between December 2014 and November 2016 were prospectively analyzed. Primary suture of the perforation and pedicled omentoplasty was done in all the patients. Data regarding patients was collected and correlated with the postoperative outcome.
Results
The overall postoperative morbidity and mortality were 62.5% and 30.4%, respectively. On univariate analysis advanced age (≥ 60 years) [(p = 0.005), (OR = 3.6), (95% CI = 1.5–8.8)], pre-operative shock [(p < 0.001), (OR = 7.4), (95% CI = 2.6–21.0)], delayed presentation (> 24 h) [(p = 0.007), (OR = 4.0), (95% CI = 1.5–11.2)] and raised serum creatinine [(p < 0.001), (OR = 7.7), (95% CI = 3.1–19.0)] were found to be significantly associated with the post-operative morbidity. For mortality, advanced age (≥ 60 year) [(p < 0.001), (OR = 5.02), (95% CI = 2.1–11.9)], pre-operative shock [(p < 0.001), (OR = 19.3), (95% CI = 6.9–53.6)], comorbidity [(p = 0.03), (OR = 6.6), (95% CI = 1.2–35.7)] and raised serum creatinine [(p < 0.001), (OR = 13.1), (95% CI = 4.5–37.8)] were statistically significant factors. Multivariate analysis showed advanced age (≥ 60 years) (p = 0.05) and raised serum creatinine (p = 0.004) as significant factors for increased risk of post-operative morbidity. Advanced age (≥ 60 years), pre-operative shock and raised serum creatinine were found to be independent risk factors influencing post-operative mortality (p < 0.05).
Conclusion
A thorough clinical evaluation, adequate resuscitation, sepsis control, addressing comorbidities and early access to hospital can reduce the risk morbidity and mortality in patients with PPU.
Similar content being viewed by others
Availability of data and material
Available on request.
References
Unver M, Fırat Ö, Ünalp ÖV, Uğuz A, Gümüş T, Sezer TÖ, et al. Prognostic factors in peptic ulcer perforations: a retrospective 14-year study. Int Surg. 2015;100(5):942–8.
Søreide K, Thorsen K, Søreide JA. Strategies to improve the outcome of emergency surgery for perforated peptic ulcer. BJS. 2014;101(1):e51-64.
Moller MH, Adamsen S, Wojdemann M, Moller AM. Perforated peptic ulcer: how to improve outcome? Scand J Gastroenterol. 2009;44:15–22.
Moller MH, Adamsen S, Thomsen RW, Moller AM, Peptic Ulcer Perforation (PULP) trial group. Multicentre trial of a perioperative protocol to reduce mortality in patients with peptic ulcer perforation. Br J Surg. 2011;98:802–10.
Boey J, Wong J, Ong GB. Bacteria and septic complications in patients with perforated duodenal ulcers. Am J Surg. 1982;143:635–9.
Chan WH, Wong WK, Khin LW, Soo KC. Adverse operative risk factors for perforated peptic ulcer. Ann Acad Med. 2000;29:164–7.
Søreide K, Thorsen K, Harrison EM, Bingener J, Møller MH, Ohene-Yeboah M, Søreide JA. Perforated peptic ulcer. Lancet. 2015;386(10000):1288–98.
Tas I, Ulger BV, Onder A, Kapan M, Bozdag Z. Risk factors influencing morbidity and mortality in perforated peptic ulcer disease. Ulus Cerrahi Derg. 2015;31(1):20–5.
Lohsiriwat V, Prapasrivorakul S, Lohsiriwat D. Perforated peptic ulcer: clinical presentation, surgical outcomes, and the accuracy of the Boey Scoring System in predicting postoperative morbidity and mortality. World J Surg. 2008;33(1):80–5.
Menekse E, Kocer B, Topcu R, Olmez A, Tez M, Kayaalp C. A practical scoring system to predict mortality in patients with perforated peptic ulcer. World J Emerg Surg. 2015;10(1):7–13.
Testini M, Portincasa P, Piccinni G, Lissidini G, Pellegrini F, Greco L. Significant factors associated with fatal outcome in emergency open surgery for perforated peptic ulcer. World J Gastroenterol. 2003;9(10):2338–40.
Sivaram P, Sreekumar A. Preoperative factors influencing mortality and morbidity in peptic ulcer perforation. Eur J Trauma Emerg Surg. 2018;44(2):251–7.
Koc M, Yoldas O, Kılıc Y, Gocmen E, Ertan T, Dizen H, et al. Comparison and validation of scoring systems in a cohort of patients treated for perforated peptic ulcer. Langenbecks Arch Surg. 2007;392(5):581–5.
Kim J, Jeong S, Lee Y, Park S, Choi S, Hong S, et al. Analysis of risk factors for postoperative morbidity in perforated peptic ulcer. J Gastric Cancer. 2012;12(1):26–35.
Lau JY, Sung J, Hill C, Henderson C, Howden CW, Metz DC. Systematic review of the epidemiology of complicated peptic ulcer disease: incidence, recurrence, risk factors and mortality. Digestion. 2011;84(2):102–13.
Kujath P, Schwandner O, Bruch HP. Morbidity and mortality of perforated peptic gastroduodenal ulcer following emergency surgery. Langenbecks Arch Surg. 2002;387:298–302.
Thorsen K, Søreide JA, Søreide K. What is the best predictor of mortality in perforated peptic ulcer disease? A population-based, multivariable regression analysis including three clinical scoring systems. J Gastrointest Surg. 2014;18:1261–8.
Mulari K, Leppäniemi A. Severe secondary peritonitis following gastrointestinal tract perforation. Scand J Surg. 2004;93(3):204.
Funding
The authors have not received any fund for this study.
Author information
Authors and Affiliations
Contributions
MA conception and design; analysis and interpretation of the data; drafting of the article. TM conception and design; final approval of the article. AZR conception and design; critical revision of the article for important intellectual content; final approval of the article. SAAR final approval of the article.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Approved from institute ethics committee. The work has been reported in line with the STROCSS criteria.
Consent to participate
Informed consent obtained from participants.
Consent for publication
All authors agree for publication of the manuscript.
Rights and permissions
About this article
Cite this article
Ahmed, M., Mansoor, T., Rab, A.Z. et al. Risk factors influencing postoperative outcome in patients with perforated peptic ulcer: a prospective cohort study. Eur J Trauma Emerg Surg 48, 81–86 (2022). https://doi.org/10.1007/s00068-020-01597-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01597-6