Abstract
Purpose
In this systematic review, we analyzed the optimal time range to evacuate traumatic-retained hemothorax using video-assisted thoracoscopic surgery (VATS).
Methods
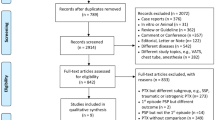
We searched PubMed, EMBASE, the Cochrane Register of Controlled Trials, Google Scholar, and the U.S. National Library of Medicine clinical trials database up to February 2019. Randomized controlled trials (RCTs) and observational studies with relevant data were included. Data were extracted from studies that reported the success, mortality, or length of hospital stay (LOS) after using VATS during at least two out of three of our time-ranges of interest: days 1–3 (group A), days 4–6 (group B), and day 7 or later (group C).
Results
Six cohort studies with 476 total participants were included in the meta-analysis. The patients in group A had a significantly higher success rate than those in group C (RR = 0.42; 95% CI = 0.21–0.84, p = 0.01). The total LOS for patients whose retained hemothorax was evacuated in group A was 4.7 days shorter than that for those in group B (95% CI = − 5.6 to − 3.8, p = 0.006). Likewise, group B patients were discharged 18.1 days earlier than group C patients (95% CI = − 22.3 to − 14, p < 0.001). Short-term mortality was not decreased by early VATS.
Conclusions
Our results indicate that VATS should be considered within the first three days of admission if this intervention is the clinician's choice to evacuate a traumatic-retained hemothorax.
Protocol registration number in PROSPERO: CRD42017046856






Similar content being viewed by others
References
Karmy-Jones R, Sappington C, Wheeler N. Hemothorax. Curr Respir Med Rev. 2012;8:268–73.
Broderick SR. Hemothorax: etiology, diagnosis, and management. Thorac Surg Clin. 2013;23:89–96.
Eren S, Esme H, Sehitogullari A, Durkan A. The risk factors and management of posttraumatic empyema in trauma patients. Injury. 2008;39:44–9.
Karmy-Jones R, Holevar M, Sullivan RJ, Jurkovich GJ. Residual hemothorax after chest tube placement correlates with increased risk of empyema following traumatic injury. Can Respir J. 2008;15:255–8.
DuBose J, Inaba K, Okoye O, Demetriades D, Scalea T, O’Connor J, et al. Development of posttraumatic empyema in patients with retained hemothorax: results of a prospective, observational AAST study. J Trauma Acute Care Surg. 2012;73:752–7.
De Hoyos A. Complications of pleural operations and procedures. Complicat Cardiothorac Surg Avoid Treat Second Ed. 2009;14:295–324.
Oǧuzkaya F, Akçali Y, Bilgin M. Videothoracoscopy versus intrapleural streptokinase for management of post traumatic retained haemothorax: a retrospective study of 65 cases. Injury. 2005;36:526–9.
Navsaria PH, Vogel RJ, Nicol AJ. Thoracoscopic evacuation of retained posttraumatic hemothorax. Ann Thorac Surg. 2004;78:282–5.
Velmahos GC, Demetriades D. Early thoracoscopy for the evacuation of undrained haemothorax. Eur J Surg. 1999;165:924–9.
DuBose J, Inaba K, Demetriades D, Scalea TM, O’Connor J, Menaker J, et al. Management of post-traumatic retained hemothorax: a prospective, observational, multicenter AAST study. J Trauma Acute Care Surg. 2012;72:11–22.
Łochowski MP, Kozak J. Video-assisted thoracic surgery complications Wideochirurgia i inne Tech maloinwazyjne. Videosurg Miniinvas Tech. 2014;9:495–500.
Mowery NT, Gunter OL, Collier BR, Diaz JJ, Haut E, Hildreth A, et al. Practice management guidelines for management of hemothorax and occult pneumothorax. J Trauma. 2011;70:510–8.
Billeter AT, Druen D, Franklin GA, Smith JW, Wrightson W, Richardson JD. Video-assisted thoracoscopy as an important tool for trauma surgeons: a systematic review. Langenbeck’s Arch Surg. 2013;398:515–23.
Smith JW, Franklin GA, Harbrecht BG, Richardson JD. Early VATS for blunt chest trauma: a management technique underutilized by acute care surgeons. J Trauma Inj Infect Crit Care. 2011;71:102–7.
Reddy NS, Hornick P. Haemothorax. Br J Hosp Med. 2007;68:M71–M7373.
Meyer DM, Jessen ME, Wait MA, Estrera AS. Early evacuation of traumatic retained hemothoraces using thoracoscopy: a prospective, randomized trial. Ann Thorac Surg. 1997;64:1396–401.
Cooper HM. Synthesizing research: a guide for literature reviews, 3rd ed. SAGE Publications; 1998.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLOS Med. 2009;6:e1000100.
Mantel N, Haenszel W. Statistical aspects of the analysis of data from retrospective studies of disease. J Natl Cancer Inst. 1959;22:719–48.
Sweeting JM, Sutton JA, Lambert CP (2004) What to add to nothing? Use and avoidance of continuity corrections in meta-analysis of sparse data. Stat Med 23:1351–75
Thompson SG, Higgins JPT. How should meta-regression analyses be undertaken and interpreted? Stat Med. 2002;21:1559–733.
Tobias A. Assessing the influence of a single study in the meta-anyalysis estimate. Stata Tech Bull. 1999;8:15–7.
Higgins JPT, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Higgins JPT, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58.
Lin HL, Huang WY, Yang C, Chou SM, Chiang HI, Kuo LC, et al. How early should VATS be performed for retained haemothorax in blunt chest trauma? Injury. 2014;45:1359–64.
Morales Uribe CH, Villegas Lanau MI, Petro Sánchez RD. Best timing for thoracoscopic evacuation of retained post-traumatic hemothorax. Surg Endosc Other Interv Tech. 2008;22:91–5.
Morrison CA, Lee TC, Wall MJ Jr, Carrick MM. Use of a trauma service clinical pathway to improve patient outcomes for retained traumatic hemothorax. World J Surg. 2009;33:1851–6.
Vassiliu P, Velmahos GC, Toutouzas KG. Timing, safety, and efficacy of thoracoscopic evacuation of undrained post-traumatic hemothorax. Am Surg. 2001;67:1165–9.
Ahmad T, Ahmed SW, Soomro NH, Sheikh KA. Thoracoscopic evacuation of retained post-traumatic hemothorax. J Coll Physicians Surg Pakistan. 2013;23:234–6.
Abolhoda A, Livingston DH, Donahoo JS, Allen K. Diagnostic and therapeutic video assisted thoracic surgery (VATS) following chest trauma. Eur J Cardio-Thoracic Surg. 1997;12:356–60.
Higgins JPT, Thompson SG. Controlling the risk of spurious findings from meta-regression. Stat Med. 2004;23:1663–822.
Fabbrucci P, Nocentini L, Secci S, Manzoli D, Bruscino A, Fedi M, et al. Video-assisted thoracoscopy in the early diagnosis and management of post-traumatic pneumothorax and hemothorax. Surg Endosc Other Interv Tech. 2008;22:1227–311.
Velmahos GC, Demetriades D, Chan L, Tatevossian R, Cornwell Iii EE, Yassa N, et al. Predicting the need for thoracoscopic evacuation of residual traumatic hemothorax: Chest radiograph is insufficient. J Trauma Inj Infect Crit Care. 1999;46:65–70.
Oosthuizen GV, Clarke DL, Laing GL, Bruce J, Kong VY, Van Staden N, et al. Introducing video-assisted thoracoscopy for trauma into a South African township hospital. World J Surg. 2013;37:1652–5.
Huang F-D, Yeh W-B, Chen S-S, Liu Y-Y, Lu I-Y, Chou Y-P, et al. Early management of retained hemothorax in blunt head and chest Trauma. World J Surg. 2018;42:2061–6.
Villavicencio RT, Aucar JA, Wall MJ Jr. Analysis of thoracoscopy in trauma. Surg Endosc. 1999;13:3–9.
Heniford BT, Carrillo EH, Spain DA, Sosa JL, Fulton RL, Richardson JD. The role of thoracoscopy in the management of retained thoracic collections after trauma. Ann Thorac Surg. 1997;63:940–3.
Bradley M, Okoye O, DuBose J, Inaba K, Demetriades D, Scalea T, et al. Risk factors for post-traumatic pneumonia in patients with retained haemothorax: results of a prospective, observational AAST study. Injury. 2013;44:1159–64.
Bailey RC. Complications of tube thoracostomy in trauma. J Accid Emerg Med. 2000;17:111–4.
Hussain N, Javed A, Kamran J, Wahab S. Complications and technical errors of tube thoracostomy and its underwater seal system. J Surg Pakistan. 2014;19:75–8.
Aylwin CJ, Brohi K, Davies GD, Walsh MS. Pre-hospital and in-hospital thoracostomy: indications and complications. Ann R Coll Surg Engl. 2008;90:54–7.
Scott MF, Khodaverdian RA, Shaheen JL, Ney AL, Nygaard RM. Predictors of retained hemothorax after trauma and impact on patient outcomes. Eur J Trauma Emerg Surg. Germany 2017;43:179–84.
Villegas MI, Hennessey RA, Morales CH, Londoño E. Risk factors associated with the development of post-traumatic retained hemothorax. Eur J Trauma Emerg Surg. 2011;37:583–9.
Kehlet H, Wilmore DW. Evidence-based surgical care and the evolution of fast-track surgery. Ann Surg. 2008;248:189–98.
Faber T, Ravaud P, Riveros C, Perrodeau E, Dechartres A. Meta-analyses including non-randomized studies of therapeutic interventions: a methodological review. BMC Med Res Methodol BioMed Central. 2016;16:35.
Shapiro S. Meta-analysis/Shmeta-analysis. Am J Epidemiol. 1994;140:771–8.
Sox HC. Defining comparative effectiveness research: the importance of getting it right. Med Care. 2010;48:S7–8.
Alemayehu D, Cappelleri JC. Revisiting issues, drawbacks and opportunities with observational studies in comparative effectiveness research. J Eval Clin Pract. 2013;19:579–83.
Norris SL, Atkins D, Bruening W, Fox S, Johnson E, Kane R, et al. Observational studies in systematic [corrected] reviews of comparative effectiveness: AHRQ and the effective health care program. J Clin Epidemiol. 2011;64:1178–86.
Navarese EP, Kozinski M, Pafundi T, Andreotti F, Buffon A, De SS, et al. Practical and updated guidelines on performing meta-analyses of non-randomized studies in interventional cardiology. Cardiol J. 2011;18:3–7.
Takkouche B, Cadarso-Suarez C, Spiegelman D. Evaluation of old and new tests of heterogeneity in epidemiologic meta-analysis. Am J Epidemiol. 1999;150:206–15.
Harbord R, Higgins JPT. Meta-regression in stata. Stata J. 2008;8:493–519.
Mathur MB, VanderWeele TJ. Sensitivity analysis for unmeasured confounding in meta-analyses. J Am Stat Assoc. 2019. https://doi.org/10.1080/01621459.2018.1529598.
Groenwold RHH, Nelson DB, Nichol KL, Hoes AW, Hak E. Sensitivity analyses to estimate the potential impact of unmeasured confounding in causal research. Int J Epidemiol. 2009;39:107–17.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–34.
Sterne JAC, Sutton AJ, Ioannidis JPA, Terrin N, Jones DR, Lau J, et al. Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ. 2011;343:d4002.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
This manuscript has not been published and is not under consideration for publication elsewhere. We have no conflicts of interest to disclose. All authors have read and approved the final version of the manuscript. All the above authors have read and approved the final version of the manuscript and confirm having no conflicts of interest to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ziapour, B., Mostafidi, E., Sadeghi-Bazargani, H. et al. Timing to perform VATS for traumatic-retained hemothorax (a systematic review and meta-analysis). Eur J Trauma Emerg Surg 46, 337–346 (2020). https://doi.org/10.1007/s00068-019-01275-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-019-01275-2