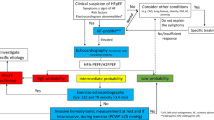
Abstract
Objective
The aim of this study was to evaluate the prognostic value of a novel scoring system, based on D‑dimer, total cholesterol, high-sensitivity cardiac troponin T (hs-cTnT), and serum albumin levels, in patients with heart failure.
Methods
A total of 221 patients diagnosed with heart failure between May 2016 to January 2020 were enrolled in this retrospective study. The prognostic significance of the biomarkers D‑dimer, total cholesterol, hs-cTnT, and serum albumin was determined with univariate and multivariate Cox proportional hazard models. A novel prognostic score based on these predictors was established. The Kaplan–Meier method and log-rank test were used to compare the adverse outcomes of patients in different risk groups.
Result
Results from univariate and multivariate analyses showed that high D‑dimer, low serum albumin, high hs-cTnT, and low total cholesterol levels were independent prognostic factors for adverse outcomes (D-dimer >0.63 mg/l, HR = 1.84, 95% CI = 1.16–2.94, p = 0.010; serum albumin >34 g/l, HR = 0.67, 95% CI = 0.45–0.99, p = 0.046; hs-cTnT >24.06 pg/ml, HR = 1.65, 95% CI = 1.08–2.53, p = 0.020; total cholesterol >3.68 mmol/l, HR = 0.63, 95% CI = 0.43–0.92, p = 0.017). Moreover, all the patients were stratified into low-risk or high-risk group according to a scoring system based on these four markers. Kaplan–Meier analyses demonstrated that patients in the high-risk group were more prone to having adverse outcomes compared with patients in the low-risk group.
Conclusion
D‑dimer, total cholesterol, hs-cTnT, and serum albumin levels were independent prognostic factors in the setting of heart failure. A novel and comprehensive scoring system based on these biomarkers is an easily available and effective tool for predicting the adverse outcomes of patients with heart failure.
Zusammenfassung
Ziel der Arbeit
Ziel der vorliegenden Studie war es, den prognostischen Wert eines neuen Score-Systems zu untersuchen, der auf den Werten für D‑Dimere, Gesamtcholesterin, hochsensitives kardiales Troponin (hs-cTnT) und Serumalbumin bei Patienten mit Herzinsuffizienz beruht.
Methoden
In diese retrospektive Studie wurden 221 Patienten mit Diagnosestellung einer Herzinsuffizienz zwischen Mai 2016 und Januar 2020 einbezogen. Die prognostische Bedeutung der Biomarker D‑Dimere, Gesamtcholesterin, hs-cTnT und Serumalbumin wurde anhand univariater und multivariater Cox-Proportional-Hazard-Modelle ermittelt. Es wurde ein neuer prognostischer Score auf der Grundlage dieser Prädiktoren etabliert. Um unerwünschte Ereignisse zwischen den Patienten in verschiedenen Risikogruppen zu vergleichen, wurden die Kaplan-Meier-Methode und der Log-Rank-Test eingesetzt.
Ergebnisse
Die Ergebnisse der univariaten und multivariaten Analysen zeigten, dass hohe Werte für D‑Dimere und hs-cTnT sowie niedrige Werte für Gesamtcholesterin und Serumalbumin unabhängige prognostische Faktoren für ungünstige Outcomes waren (D-Dimere >0,63 mg/l; Hazard Ratio, HR = 1,84; 95%-Konfidenzintervall, 95%-KI = 1,16–2,94; p = 0,010; Serumalbumin >34 g/l; HR = 0,67; 95%-KI = 0,45–0,99; p = 0,046; hs-cTnT >24,06 pg/ml; HR = 1,65; 95%-KI = 1,08–2,53; p = 0,020; Gesamtcholesterin >3,68 mmol/l; HR = 0,63; 95%-KI = 0,43–0,92; p = 0,017). Darüber hinaus wurden alle Patienten gemäß einem Scoring-System auf Grundlage dieser 4 Parameter in eine Niedrigrisikogruppe oder Hochrisikogruppe eingeteilt. Die Kaplan-Meier-Analysen ergaben, dass bei den Patienten in der Hochrisikogruppe eine höhere Tendenz zu ungünstigen Outcomes als bei den Patienten in der Niedrigrisikogruppe bestand.
Schlussfolgerung
Die Werte für D‑Dimere, Gesamtcholesterin, hs-cTnT sowie Serumalbumin stellten sich als unabhängige prognostische Faktoren bei Vorliegen einer Herzinsuffizienz heraus. Ein neues und umfassendes Scoring-System auf der Basis dieser Biomarker erwies sich als leicht verfügbares und effektives Instrument zur Vorhersage ungünstiger Outcomes bei Patienten mit Herzinsuffizienz.






Similar content being viewed by others
References
Ambrosy AP, Fonarow GC, Butler J et al (2014) The global health and economic burden of hospitalizations for heart failure: lessons learned from hospitalized heart failure registries. J Am Coll Cardiol 63:1123–1133
Taylor CJ, Ordóñez-Mena JM, Roalfe AK et al (2019) Trends in survival after a diagnosis of heart failure in the United Kingdom 2000–2017: population based cohort study. BMJ 364:l223
Maggioni AP, Dahlström U, Filippatos G et al (2013) EURObservational research programme: regional differences and 1‑year follow-up results of the heart failure pilot survey (ESC-HF pilot). Eur J Heart Fail 15:808–817
Uemura Y, Shibata R, Masuda A et al (2020) Utility of the nutritional screening in predicting adverse outcome of patients with overweight/obesity and acute heart failure. J Card Fail 26(7):566–573. https://doi.org/10.1016/j.cardfail.2020.02.005
Yasumura K, Abe H, Iida Y et al (2020) Prognostic impact of nutritional status and physical capacity in elderly patients with acute decompensated heart failure. ESC Heart Fail 7(4):1801–1808
Hirose S, Miyazaki S, Yatsu S et al (2020) Impact of the geriatric nutritional risk index on in-hospital mortality and length of hospitalization in patients with acute decompensated heart failure with preserved or reduced ejection fraction. J Clin Med 9(4):1169
Aimo A, Januzzi JL Jr, Vergaro G et al (2018) Prognostic value of high-sensitivity troponin T in chronic heart failure: an individual patient data meta-analysis. Circulation 137:286–297
Cho JH, Cho HJ, Lee HY et al (2020) Neutrophil-lymphocyte ratio in patients with acute heart failure predicts in-hospital and long-term mortality. J Clin Med 9(2):557
Benites-Zapata VA, Hernandez AV, Nagarajan V et al (2015) Usefulness of neutrophil-to-lymphocyte ratio in risk stratification of patients with advanced heart failure. Am J Cardiol 115:57–61
Silva N, Bettencourt P, Guimarães JT (2015) The lymphocyte-to-monocyte ratio: an added value for death prediction in heart failure. Nutr Metab Cardiovasc Dis 25:1033–1040
Lip GY, Gibbs CR (1999) Does heart failure confer a hypercoagulable state? Virchow’s triad revisited. J Am Coll Cardiol 33:1424–1426
Yan W, Liu J, Liu H et al (2019) Elevated D‑dimer levels predict adverse outcomes in hospitalised elderly patients with chronic heart failure. Intern Med J 49:1299–1306
Minami Y, Haruki S, Jujo K et al (2016) Elevated D‑dimer levels predict an adverse outcome in hospitalized patients with acute decompensated heart failure. Int J Cardiol 204:42–44
Yucel O, Yucel H, Zorlu A (2017) D‑dimer is a predictor of cardiovascular death, and new-onset atrial fibrillation in patients with systolic heart failure. Int J Cardiol 247:39
Huang B, Li YJ, Shen J et al (2019) D‑dimer level and long-term outcome in patients with end-stage heart failure secondary to idiopathic dilated cardiomyopathy. J Geriatr Cardiol 16:621–629
Nishi I, Seo Y, Hamada-Harimura Y et al (2017) Nutritional screening based on the controlling nutritional status (CONUT) score at the time of admission is useful for long-term prognostic prediction in patients with heart failure requiring hospitalization. Heart Vessels 32:1337–1349
Gotsman I, Shauer A, Zwas DR et al (2019) Low serum albumin: a significant predictor of reduced survival in patients with chronic heart failure. Clin Cardiol 42:365–372
Prenner SB, Pillutla R, Yenigalla S et al (2020) Serum albumin is a marker of myocardial fibrosis, adverse pulsatile aortic hemodynamics, and prognosis in heart failure with preserved ejection fraction. J Am Heart Assoc 9:e14716
Jabbour R, Ling HZ, Norrington K et al (2014) Serum albumin changes and multivariate dynamic risk modelling in chronic heart failure. Int J Cardiol 176:437–443
Rauchhaus M, Clark AL, Doehner W et al (2003) The relationship between cholesterol and survival in patients with chronic heart failure. J Am Coll Cardiol 42:1933–1940
Horwich TB, Hernandez AF, Dai D et al (2008) Cholesterol levels and in-hospital mortality in patients with acute decompensated heart failure. Am Heart J 156:1170–1176
Greene SJ, Vaduganathan M, Lupi L et al (2013) Prognostic significance of serum total cholesterol and triglyceride levels in patients hospitalized for heart failure with reduced ejection fraction (from the EVEREST trial). Am J Cardiol 111:574–581
Shirakabe A, Hata N, Kobayashi N et al (2018) The prognostic impact of malnutrition in patients with severely decompensated acute heart failure, as assessed using the prognostic nutritional index (PNI) and controlling nutritional status (CONUT) score. Heart Vessels 33:134–144
Kato T, Yaku H, Morimoto T et al (2020) Association with controlling nutritional status (CONUT) score and in-hospital mortality and infection in acute heart failure. Sci Rep 10:3320
Matsue Y, Kagiyama N, Yamaguchi T et al (2020) Clinical and prognostic values of ALBI score in patients with acute heart failure. Heart Lung Circ 29(9):1328–1337. https://doi.org/10.1016/j.hlc.2019.12.003
Heart Failure Group of Chinese Society of Cardiology of Chinese Medical Association, Chinese Heart Failure Association of Chinese Medical Doctor Association, Editorial Board of Chinese Journal of Cardiology (2018) Chinese guidelines for the diagnosis and treatment of heart failure 2018. Zhonghua Xin Xue Guan Bing Za Zhi 46:760–789
Teerlink JR, Cotter G, Davison BA et al (2013) Serelaxin, recombinant human relaxin‑2, for treatment of acute heart failure (RELAX-AHF): a randomised, placebo-controlled trial. Lancet 381:29–39
Massie BM, O’Connor CM, Metra M et al (2010) Rolofylline, an adenosine A1-receptor antagonist, in acute heart failure. N Engl J Med 363:1419–1428
Noveanu M, Breidthardt T, Potocki M et al (2011) Direct comparison of serial B‑type natriuretic peptide and NT-proBNP levels for prediction of short- and long-term outcome in acute decompensated heart failure. Crit Care 15:R1
Santaguida PL, Don-Wauchope AC, Oremus M et al (2014) BNP and NT-proBNP as prognostic markers in persons with acute decompensated heart failure: a systematic review. Heart Fail Rev 19:453–470
Wu AH, Ford L (1999) Release of cardiac troponin in acute coronary syndromes: ischemia or necrosis? Clin Chim Acta 284:161–174
Januzzi JL Jr, Filippatos G, Nieminen M et al (2012) Troponin elevation in patients with heart failure: on behalf of the third universal definition of myocardial infarction global task force: heart failure section. Eur Heart J 33:2265–2271
Pang PS, Teerlink JR, Voors AA et al (2016) Use of high-sensitivity troponin T to identify patients with acute heart failure at lower risk for adverse outcomes: an exploratory analysis from the RELAX-AHF trial. JACC Heart Fail 4:591–599
Suzuki S, Motoki H, Minamisawa M et al (2019) Prognostic significance of high-sensitivity cardiac troponin in patients with heart failure with preserved ejection fraction. Heart Vessels 34:1650–1656
Zannad F, Stough WG, Regnault V et al (2013) Is thrombosis a contributor to heart failure pathophysiology? Possible mechanisms, therapeutic opportunities, and clinical investigation challenges. Int J Cardiol 167:1772–1782
Sbarouni E, Bradshaw A, Andreotti F et al (1994) Relationship between hemostatic abnormalities and neuroendocrine activity in heart failure. Am Heart J 127:607–612
Weitz JI, Fredenburgh JC, Eikelboom JW (2017) A test in context: D‑dimer. J Am Coll Cardiol 70:2411–2420
Zorlu A, Yilmaz MB, Yucel H et al (2012) Increased d‑dimer levels predict cardiovascular mortality in patients with systolic heart failure. J Thromb Thrombolysis 33:322–328
Tarnow I, Falk T, Tidholm A et al (2007) Hemostatic biomarkers in dogs with chronic congestive heart failure. J Vet Intern Med 21:451–457
Ballmer PE (2001) Causes and mechanisms of hypoalbuminaemia. Clin Nutr 20:271–273
Lourenço BH, Vieira LP, Macedo A et al (2009) Nutritional status and adequacy of energy and nutrient intakes among heart failure patients. Arq Bras Cardiol 93:541–548
Liu M, Chan CP, Yan BP et al (2012) Albumin levels predict survival in patients with heart failure and preserved ejection fraction. Eur J Heart Fail 14:39–44
Bonilla-Palomas JL, Gámez-López AL, Moreno-Conde M et al (2014) Hypoalbuminemia in acute heart failure patients: causes and its impact on hospital and long-term mortality. J Card Fail 20:350–358
Uthamalingam S, Kandala J, Daley M et al (2010) Serum albumin and mortality in acutely decompensated heart failure. Am Heart J 160:1149–1155
Omran ML, Morley JE (2000) Assessment of protein energy malnutrition in older persons, part II: laboratory evaluation. Nutrition 16:131–140
Wrigley BJ, Lip GY, Shantsila E (2011) The role of monocytes and inflammation in the pathophysiology of heart failure. Eur J Heart Fail 13:1161–1171
Pugh RN, Murray-Lyon IM, Dawson JL et al (1973) Transection of the oesophagus for bleeding oesophageal varices. Br J Surg 60:646–649
Herzer K, Kneiseler G, Bechmann LP et al (2011) Onset of heart failure determines the hepatic cell death pattern. Ann Hepatol 10:174–179
Hesse B, Parving HH, Lund-Jacobsen H et al (1976) Transcapillary escape rate of albumin and right atrial pressure in chronic congestive heart failure before and after treatment. Circ Res 39:358–362
Battin DL, Ali S, Shahbaz AU et al (2010) Hypoalbuminemia and lymphocytopenia in patients with decompensated biventricular failure. Am J Med Sci 339:31–35
Fanali G, di Masi A, Trezza V et al (2012) Human serum albumin: from bench to bedside. Mol Aspects Med 33:209–290
Yoon CH, Youn TJ, Ahn S et al (2012) Low serum total cholesterol level is a surrogate marker, but not a risk factor, for poor outcome in patients hospitalized with acute heart failure: a report from the Korean heart failure registry. J Card Fail 18:194–201
Greene SJ, Vaduganathan M, Lupi L et al (2013) Prognostic significance of serum total cholesterol and triglyceride levels in patients hospitalized for heart failure with reduced ejection fraction (from the EVEREST trial). Am J Cardiol 111:574–581
Anker SD, Ponikowski P, Varney S et al (1997) Wasting as independent risk factor for mortality in chronic heart failure. Lancet 349:1050–1053
Niebauer J, Volk HD, Kemp M et al (1999) Endotoxin and immune activation in chronic heart failure: a prospective cohort study. Lancet 353:1838–1842
Rauchhaus M, Coats AJ, Anker SD (2000) The endotoxin-lipoprotein hypothesis. Lancet 356:930–933
Acknowledgements
The authors thank Dr. Jin Meng for his continuous support in data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
T.‑J. Zhao, Q.‑K. Yang, L.‑D. Bi, J. Li, C.‑Y. Tan and Z.‑L. Miao declare that they have no competing interests.
The present study was performed in accordance with the World Medical Association Declaration of Helsinki and was approved by the Ethics Board of The People’s Hospital of China Medical University. This study was a retrospective study and all the data used in the final analysis was anonymous. Therefore, the informed consent from the enrolled patients was waived. The institutional review board of our hospital gave the ethical approval for this study.
Additional information
Tian-Jun Zhao and Qian-Kun Yang contributed equally to this work and shared the co-authorship.
Author contributions
Tian-Jun Zhao and Qian-Kun Yang performed the experiment and wrote the manuscript. Tian-Jun Zhao was responsible for the design of the experiment. Li-Dan Bi and Chun-Yu Tan analyzed the data. Jie Li helped with the statistical analysis. Zhi-Lin Miao provided professional support and revised the manuscript. All authors read and approved the final manuscript.
Availability of data and materials
The datasets used and/or analyzed during the present study are available from the corresponding author on reasonable request.
Rights and permissions
About this article
Cite this article
Zhao, TJ., Yang, QK., Bi, LD. et al. Prognostic value of DCTA scoring system in heart failure. Herz 46 (Suppl 2), 243–252 (2021). https://doi.org/10.1007/s00059-020-04993-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-020-04993-1