Summary
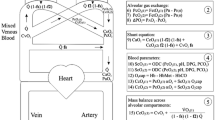
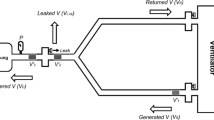
A lung model was used to simulate gas exchange for a 70 kg adult under anaesthesia. It was demonstrated that the modified Mapleson D circuit (Bain) with low fresh gas flows determined according to body weight is a partial rebreathing system. With controlled ventilation this can be compensated for by increasing minute ventilation above the predicted and the arterial carbon dioxide level can then be regulated by adjusting the fresh gas flow. During spontaneous ventilation this compensation is critically dependent on the patient's ability to increase minute ventilation. Therefore in any particular case the arterial carbon dioxide is unpredictable and totally dependent on carbon dioxide responsiveness, carbon dioxide production, physiological dead-space, respiratory wave form, and apparatus dead-space. Although normocarbia can be achieved by certain ideal patients despite low fresh gas flows it can be done only if minute ventilation is markedly increased. This enforced hyperpnoea will significantly encroach on the respiratory reserve of these patients and may well be unattainable in some. We conclude that any decrease in respiratory drive, increase in carbon dioxide production, increase in physiological or apparatus dead-space (i.e. a mask) will produce potentially dangerous hypercarbia using a Bain circuit with a fresh gas flow of 100 ml/kg/minute. This hazard is not easily recognized. The only way to minimize these factors during spontaneous ventilation is by the use of a non-rebreathing circuit. To do this with a T-piece or Bain circuit the fresh gas flow must be between 200 and 300 ml/kg/min for an average adult, with this requirement being highly dependent on all the variables outlined. One must decide whether the low economy and high level of operating room pollution with this wide range of flow outweigh the advantages of trying to make the Mapleson D a universal circuit.
Résumé
Un modèle a été employé pour simuler les échanges gazeux ďun adulte de 70 kg. On a déjà démontré qu’en circuit Mapleson D modifié ou circuit Bain alimenté par des gaz frais à bas débits estimés selon le poids du malade se comportait comme un système à rebreathing partiel. En ventilation contrôlée, ľaugmentation de la ventilation au-delà de la valeur prédite compense et c’est le débit de gaz frais détermine la Pco2 artérielle. En ventilation spontanée, cette compensation dépend essentiellement de ľhabileté du malade à hyperventiler. En ventilation spontanée, il est donc impossible de prédire la Pco2 artérielle dépendant maintenant de la capacité de réponse à la stimulation du CO2 et de sa production, de ľespace mort physiologique, des caractéristiques du cycle respiratoire et de ľespace mort du montage. On peut quelquefois maintenir la normocarbie avec des débits peu élevés de gaz frais mais ceci nécessite une augmentation importante de la ventilation. Ľhyperpnée nécessaire sera possible pour les sujets ayant des réserves respiratoires suffisantes et impossible pour les autres. Les auteurs en concluent que la perte du stimulus respiratoire, ľaugmentation de la production de gaz carbonique et de ľespace mort physiologique ou mécanique (par exemple, celle causée par un masque) produiront une hypercarbie qui peut s’avérer dangereuse lorsqu’on utilise le circuit Bain avec une alimentation en gaz frais de ľordre de 100 ml/kg/min. C’est là un danger qui risque de passer inaperçu. Le seul moyen ďéviter ce danger pendant la ventilation spontanée est ďutiliser un circuit sans rebreathing. Avec une tube en T ou sur circuit Bain, le débit de gaz frais doit se situer entre 200 et 300 ml/kg/min pour un adulte moyen tout en tenant compte des facteurs déjà mentionnés. A chacun de décider si les avantages obtenus en faisant du circuit Mapleson D un circuit universel seront annulés par son coût élevé ďopération et le haut degré de pollution causés par de tels débits.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Bain, J.A. &Spoerel, W.E. A streamlined anaesthetic system. Canad. Anaesth. Soc. J.19: 426 (1972).
Henville, J.D. &Adams, A.P. The Bain anaesthetic system. Anaesthesia31: 247 (1976).
Chu, Y.K., Rah, K.H., &Boyan, C.P. Is the Bain circuit the future anaesthesia system? An evaluation. Anesthesia and Analgesia, Current Researches56: 84 (1977).
Mapleson, W.W. The elimination of rebreathing in various anaesthetic systems. Brit. J. Anaesth.26: 323 (1954).
Conway, C.M., Seeley, H.F., &Barnes, P.K. Spontaneous ventilation with a Bain anaesthetic system. Brit. J. Anaesth.49: 1245 (1977).
Ungerer, M.J. A comparison between the Bain and Magill systems during spontaneous breathing. Canad. Anaesth. Soc. J.25: 122 (1978).
Grey, T.C. &Nunn, J.F. General Anaesthesia, 3rd ed, London, Butterworth (1971).
Harrison, G.A. The effect of the respiratory flow pattern on rebreathing in a T-piece system. Brit. J. Anaesth.36: 206 (1964).
Spoerel, W.E., Aitken, R.R., &Bain, J.A. Spontaneous respiration with the Bain breathing circuit. Canad. Anaesth. Soc. J.25: 30 (1978).
West, J.B. Respiratory physiology — the essentials, 1st ed., Baltimore: Williams and Wilkins (1975).
Conway, C.M. Alveolar gas relationships during use of semi-closed rebreathing anaesthetic systems. Brit. J. Anaesth.48: 865 (1976).
Nunn, J.F. Prediction of carbon dioxide during anaesthesia. Anaesthesia15: 123 (1960).
Ramanathan, S., Chalon, J., Capan, L., Patel, C., &Turndorf, H. Rebreathing characteristics of the Bain anaesthesia circuit. Anesth. Analg.56: 822 (1978).
Keenan, R.L. &Boynan, C.P. How rebreathing anaesthetic systems control\(Pa_{CO_2 } \): studies with a mechanical and mathematical model. Canad. Anaesth. Soc. J.25: 117 (1978).
Nunn, J.F. &Ezi-Ashi, T.I. The accuracy of re-spirometer and ventigrator. Brit. J. Anaesth.34: 422 (1962).
Willis, B.A., Pender, J.W., &Mapleson, W.W. Rebreathing in a T-piece: volunteer and theoretical studies of the Jackson-Rees modification of Ayre’s T-piece during spontaneous respiration. Brit. J. Anaesth.47: 1239 (1975).
Munson, E.S., Farnham, M., &Hamilton, W.K. Studies of respiratory gas flows. A comparison using different anaesthetic agents. Anesthesiology24: 61 (1963).
Severinghaus, J.W. &Stupfel, M. Alveolar dead space as an index of distribution of blood flow in pulmonary capillaries. J. Appl. Physiol.10: 335 (1957).
Nunn, J.F. &Hill, D.W. Respiratory dead space and arterial to end-tidal CO2 tension difference in anesthetized man. J. Appl. Physiol.15: 583 (1960).
Hedenstierna, S. &McCarthy, G. The effect of anaesthesia and intermittent positive pressure ventilation with different frequencies on the anatomical and alveolar deadspace. Brit. J. Anaesth.47: 847 (1975).
Inkster, J.S. The T-piece technique in anaesthesia. Brit. J. Anaesth.28: 512 (1956).
Bates, D.V., Macklem, P.T., &Christie, R.V. Respiratory function in disease. 2nd ed. Philadelphia: Saunders (1971).
Nunn, J.F. Applied Respiratory Physiology, 1st ed. London: Butterworth (1969).
Seeley, H.F., Barnes, P.K., &Conway, C.M. Controlled ventilation with Mapleson D system, a theoretical and experimental study. Brit. J. Anaesth.49: 107 (1977).
Pengelly, L.D., Rebuck, A.S., &Campbell, E.J.M. Loaded Breathing, 1st ed. Toronto: Longman (1974).
Munson, E.S., Larson, P.C., Babad, A.A., Regan, M.J., Beuchel, D.R., &Eger, E.. The effects of halothane, fluroxene and cyclopropane on ventilation: a comparative study in man. Anesthesiology27: 716 (1966).
Larson, C.P., Eger, E., Muallem, M., Buechel, D.R., Munson, E.S., &Eisele, J.H. The effects of diethyl ether and methoxyflurane on ventilation: II. a comparative study in man. Anesthesiology30: 714 (1969).
Eger, E., Dolan, W.M., Stevens, W.C., Miller, R.D., &Way, W.L. Surgical stimulation antagonizes the respiratory depression produced by forane. Anesthesiology36: 544 (1972).
Kain, M.L., Panday, J., &Nunn, J.F. The effect of intubation on dead space during halothane anaesthesia. Brit. J. Anaesth.41: 94 (1969).
Black, G.W. &McKane, R.V. Respiratory and metabolic changes during methoxyflurane and halothane anaesthesia. Brit. J. Anaesth.37: 409 (1965).
Mansell, W.H. Spontaneous breathing with the Bain circuit at low flow rates: a case report. Canad. Anaesth. Soc. J.23: 432 (1976).
Bain, J.A. &Spoerel, W.E. Flow requirements for a modified Mapleson D system during controlled ventilation. Canad. Anaesth. Soc. J.20: 629 (1973).
Author information
Authors and Affiliations
Additional information
Formerly at Hospital for Sick Children.
Rights and permissions
About this article
Cite this article
Rose, D.K., Byrick, R.J. & Froese, A.B. Carbon dioxide elimination during spontaneous ventilation with a modified mapleson D system: Studies in a lung model. Canad. Anaesth. Soc. J. 25, 353–365 (1978). https://doi.org/10.1007/BF03006564
Issue Date:
DOI: https://doi.org/10.1007/BF03006564