Abstract
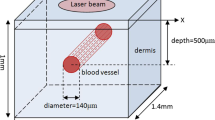
A model has been developed to calculate distal tissue necrosis in vascular tissue after application of a 100μ laser pulse from a Nd-YAG laser (5 kW peak pulse power on a 0.13 mm2 spot size). The model assumes that the temperature profile in the tissue is proportional to the laser light fluence rate and that the distal tissue necrosis depth is that depth in the tissue where there is a temperature increase of 42 °C minus the etch rate (ablation depth per laser pulse). The fluence rate has been calculated using the diffusion approximation to the radiative transport equation. The tissue optical parameters (absorption and reduced scattering coefficients) have been derived from published data. The etch rate used (10μm per pulse) is derived from in vivo experimental results. The model predicts a damage depth varying between 0 and 2.33 mm (mean 1.10 mm) and this is compared with an experimental result (0.77 mm) in dog aorta.
Similar content being viewed by others
References
Cumberland DC, Sanborn TA, Tayler DI et al. Percutaneous laser thermal angioplasty: initial clinical results with a laser probe in total peripheral artery occlusions.Lancet 1986,i:1457–9
Michaels JA, Cross FW, Shaw P et al. Laser angioplasty with a pulsed Nd-YAG laser: early clinical experience.Br J Surg 1989,76:921–4
Sanborn TA, Cumberland DC, Greenfield AJ et al. Percutaneous laser thermal angioplasty: initial results and 1-year follow-up in 129 femoropopliteal lesions.Radiology 1988,168:121–5
Goldenburg T, Anderson WB, Litvak F et al. Percutaneous excimer laser coronary angioplasty.SPIE Vol 1201—Optical Fibres in Medicine 1990:190–4
Duda SH, Karsch K, Haase KK et al. Laser ring catheters in excimer laser angioplasty.Radiology 1990,175:269–70
Abela GS, Normann SJ, Cohen DM et al. Laser recanalization of occluded atherosclerotic arteries in vivo and in vitro.Circulation 1985,71:403–11
Diethrich EB, Timbadia E, Bahadir I. Applications and limitations of laser-assisted angioplasty.Eur J Vasc Surg 1989,3:61–70
Borst C. Percutaneous recanalization of arteries: status and prospects of laser angioplasty with modified fibre tips.Lasers Med Sci 1987,2:137–51
Lammer J, Pilger E, Kleinert R. Laser angioplasty by sapphire contact probe. Experimental and clinical results.J Int Radiol 1988,3:53–8
Fourrier JL, Maravche Ph, Brunetaud JM et al. Nouvelle méthode d'angioplastie laser par saphir de contactes artères périphériques: résultats préliminaires.Arch Mal Coeur 1988,81:253–8
Deckelbaum LI, Isner JM, Donaldson RF et al. Reduction of laser induced pathologic tissue injury using pulsed energy delivery.Amer J Cardiol 1985,56:662–7
Isner JM, Steg G, Clarke RH. Current status of cardiovascular laser therapy, 1987.IEEE J Quantum Electron 1987,QE-23:1756–71
Murray A, Wood RFM. Peripheral laser angioplasty with pulsed dye laser and ball-tipped optical fibres.Lancet 1989ii:1471–4
Cross FW, Wright JK, Bowker TJ, Bown SG. The role of pulse length in limiting distant tissue damage to vascular tissue caused by the Nd-YAG laser.Lasers Med Sci 1987,2:175–81
Cross FW, Bowker TJ, Bown SG. Arterial healing in the dog after intraluminal delivery of pulsed Nd-YAG laser energy.Br J Surg 1987,74:430–5
Groenhuis RAJ, Ferwerda HA, Ten Bosch JJ. Scattering and absorption of turbid materials determined for reflection measurements. I.Theory. Appl Optics 1983,22:2456–67
Star WS, Marijnissen JPA, van Gemert MJC. Light dosimetry in optical phantoms and in tissues. i. Multiple flux and transport theory.Phys Med Biol 1988,33:437–54
van Gemert MJC, Welch AJ, Bonnier JJM et al. Some physical concepts in laser angioplasty.Seminars in Interventional Radiology 1986,3:27–38
Yoon G, Welch AJ, Motamedi M et al. Development and application of three-dimensional light distribution model for laser irradiated tissue.IEEE J Quantum Electron 1987,QE-23:1721–33
Prince MR, Deutsch TF, Mathews-Roth MM et al. Preferential light absorbtion in atheromas in vitro. Implications for laser angioplasty.J Clin Invest 1986,78:295–302
Lahaye CTW, van Gemert MJC. Optical laser parameters for port wine stain therapy: a theoretical approach.Phys Med Biol 1985,30:573–87
McKenzie AL. A three-zone model of soft-tissue damage by a CO2 laser.Phys Med Biol 1986,31:967–83
Partovi F, Izatt JA, Cothren RM et al. A model for thermal ablation of biological tissue using laser radiation.Lasers Surg Med 1987,7:141–54
van Gemert MJC, Welch AJ. Time constants in thermal laser medicine.Lasers Surg Med 1989,9:405–21
van Gemert MJC, Welch AJ, Jacques SL et al. Light distribution, optical properties and cardiovascular tissues. In: Abela GS (ed)Lasers in Cardiovascular Medicine. New York: Kluwer, pp. 93–110
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Cross, F.W., Van Gemert, M.J.C. A thermal appraisal of the ablation process in canine aorta in vivo using a 100 μm pulsed Nd-YAG laser. Laser Med Sci 6, 373–378 (1991). https://doi.org/10.1007/BF02042459
Received:
Issue Date:
DOI: https://doi.org/10.1007/BF02042459