Abstract
Introduction
Inflammatory processes have previously been shown to influence cognition and progression of dementia. An involvement of interleukin (IL)-6 has in particular been suggested as altered levels of IL-6 in cerebrospinal fluid (CSF) have been found in patients with Alzheimer’s disease (AD). Also, an association between cognitive decline and levels of IL-6 in CSF have been reported. The aim of the present study was to investigate whether patients clinically diagnosed with dementia with Lewy bodies (DLB) display altered CSF IL-6 levels in comparison with patients with AD and control subjects without dementia and whether the IL-6 levels are correlated with cognitive status and biomarkers for AD and synucleinopathy.
Methods
To analyse CSF of patients with AD (n = 45), patients with DLB (n = 29) and control subjects without dementia (n = 36), we used immunoassays to measure levels of IL-6 (multiplex electrochemiluminescence); AD markers phosphorylated tau, total tau and amyloid-β1–42 (enzyme-linked immunosorbent assay [ELISA]); and α-synuclein (ELISA). Cognitive status was evaluated using the Mini Mental State Examination (MMSE).
Results
Our analysis showed significantly lower levels of IL-6 in CSF from patients with DLB than in CSF from patients with AD and control subjects without dementia. The IL-6 levels were also negatively correlated with MMSE and positively correlated with α-synuclein CSF levels.
Conclusions
Our findings support previous studies by demonstrating a link between inflammatory processes and dementia progression and further strengthen the hypothesis that IL-6 is involved in dementia pathology and cognitive decline.
Similar content being viewed by others
Introduction
Glial secretion of interleukin-6 (IL-6), along with other pro- and anti-inflammatory cytokines and chemokines, is drastically increased in response to infection or harmful changes in the brain. The increase in IL-6 secretion has been shown to be beneficial [1–5], but sometimes also detrimental [6–9], for the neuronal network, depending on variables such as cytokine concentration, brain region, target cell and developmental stage. The impact of IL-6 on neuronal network formation and function is noticeable in a number of in vivo rodent studies. For example, foetal exposure to IL-6 has been shown to alter rat hippocampal structure and impair spatial learning [10], and deficiency of IL-6 has been shown to improve long-term memory [11] and lipopolysaccharide-induced impairment of working memory [12]. Also, results of clinical studies point towards a relationship between IL-6 and brain function, as cognitive decline has been associated with elevated levels of IL-6 in plasma and/or serum [13–16] and cerebrospinal fluid (CSF) [17, 18].
Given the role of IL-6 in neuroinflammatory actions and its potential impact on cognitive function, it is not surprising that IL-6 secretion has been found to be altered in neurodegenerative dementia disorders linked to neuroinflammation. Examinations of post-mortem brain tissue from patients with Alzheimer’s disease (AD) have revealed activated glial cells as well as elevated expression of IL-6 adjacent to amyloid-β (Aβ)1–42 forming senile plaques [19, 20], a hallmark of AD pathology [21]. Increased numbers of activated microglia and elevated levels of IL-6 mRNA have also been found in the hippocampus of patients with dementia with Lewy bodies (DLB) [22], a neurodegenerative dementia disorder characterised by the presence of both senile plaques and α-synuclein occlusions [23]. Although studies investigating the impact of IL-6 on cognitive decline in AD and patients are few, a couple of studies support the idea. An association between increased levels of IL-6 and worse cognitive performance has been shown in patients with Parkinson’s disease (PD) and dementia [24] (a condition resembling DLB in regard to neuropathological changes and symptoms [23]) and patients with PD with cognitive impairment [18]. Patients with mild cognitive impairment (MCI), a condition associated with increased risk of dementia [25], show improvement of cognitive function as well as reduced peripheral IL-6 and tumour necrosis factor α (TNF-α) levels after repetitive physical exercise [26]. Additionally, increased levels of peripheral IL-1β and TNF-α, two glia-derived proinflammatory cytokines acting conjointly with IL-6 [27], have been found to be associated with marked cognitive decline in patients with AD [28, 29].
The altered brain expression of IL-6 in AD and DLB patients and the found link between elevated peripheral IL-6 and cognitive decline has led to studies attempting to monitor ongoing pathological neuroinflammation by analysing IL-6 concentration in CSF. These studies, in particular studies on patients with AD, have led to inconsistent results, with reports of increased levels [30–32], decreased levels [33] and unchanged levels [34, 35] of IL-6 in CSF.
To our knowledge, there is so far only one published study on CSF IL-6 levels in patients with DLB. That study showed a slight, although not significant, increase in CSF IL-6 levels in patients with DLB compared with age-matched controls [36]. Given this finding, together with the previous studies demonstrating increased neuroinflammation in relation to senile plaque as well as the many studies showing an impact of IL-6 on cognition, we find it likely that IL-6 plays a role in DLB pathology. To further investigate this hypothesis and to further explore whether DLB pathology affects CSF IL-6 levels differently compared with AD pathology, we here compared IL-6 CSF concentrations in patients with DLB, patients with AD and control subjects without dementia and examined the potential association between the IL-6 levels and biomarkers correlating with neuropathological changes characteristic of AD and DLB. We also examined the relationship between CSF IL-6 levels and Mini Mental State Examination (MMSE) scores to investigate whether IL-6 may be an underlying factor involved in the cognitive changes seen in patients with DLB.
Methods
Patients
The study included dementia patients and control subjects without dementia recruited through the Neurology Clinic and the Memory Clinic at Skåne University Hospital, Malmö, Sweden. The cohort has been described previously [37, 38]. It consisted of 36 control subjects without dementia, 45 patients with AD and 29 patients with DLB. The control subjects without dementia were individuals with mild cognitive symptoms, but these symptoms were not to the extent of a formal MCI or dementia diagnosis. Clinical diagnoses were made according to the American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition [39], combined with the diagnostic criteria of the National Institute of Neurological and Communicative Disorders and Stroke and the Alzheimer’s Disease and Related Disorders Association [40] for probable AD. Diagnoses of probable DLB were made according to the DLB consensus criteria [23, 41]. The cognitive status of the patients and the control subjects without dementia was evaluated using the MMSE [42]. The CSF AD biomarkers (Aβ1–42, total tau [T-tau], tau phosphorylated at threonine 181 [P-tau181]) were analysed according to clinical routine by commercial enzyme-linked immunosorbent assay (ELISA) kits (Innogenetics, Ghent, Belgium). Quantification of CSF α-synuclein levels was performed by the use of sandwich ELISA kits (Invitrogen, Carlsbad, CA, USA) as previously described [38, 43]. Individuals with acute or chronic inflammatory conditions (14 % of control subjects without dementia, 11 % of patients with AD and 13 % of patients with DLB) were excluded from the study. All individuals provided their informed consent, either (1) by use of a passive consent procedure whereby consent for retrospective use of banked clinical samples and data were assumed if individuals did not actively retract permission, as instructed in repeated local press advertisements; or (2) by active written informed consent. Informed consent was documented in two separate registries, including the patient’s medical chart, and in the local clinical research database. The study protocol was approved by the local ethics committee at Lund University and carried out in accordance with the Declaration of Helsinki.
IL-6 quantification analysis
Levels of IL-6 in CSF were measured with a human proinflammatory 4-plex ultra-sensitive electrochemiluminescence immunoassay (Meso Scale Discovery, Rockville, MD, USA). This immunoassay is designed to analyse IL-6, interferon γ, TNF-α and IL-1β; however, only IL-6 levels were within detection range and are therefore the only values presented in this article. Standards and samples were analysed in duplicates. The detection limit for IL-6 was 0.055 pg/ml.
Statistical analysis
Statistical analysis was performed using IBM SPSS software (version 20.0 for Windows; IBM, Armonk, NY, USA). The Kolmogorov–Smirnov test was used to assess the normality of distributions. The IL-6 levels were non-normally distributed within the three different groups and were therefore transformed into logarithms before analysis. One-way analysis of variance (ANOVA), followed by the Bonferroni post hoc correction (comparisons for n = 3), was used for comparisons between the three patients groups. Spearman correlation test were used for correlation between MMSE and IL-6 and the correlation between IL-6 and AD markers as well as α-synuclein were analysed using the Pearson correlation test. The results are presented as mean ± standard deviation. p < 0.05 was considered significant.
Results
Characteristics of individuals included in the study
The demographic data of individuals included in the study are presented in Table 1. The number of women and men was roughly the same in the control and DLB patient groups, but the AD patient group consisted of more women than men. The patients with dementia scored significantly lower than control subjects without dementia on the MMSE (p < 0.001). Both patients with AD and patients with DLB had significantly lower CSF levels of Aβ1–42 than control subjects (p < 0.001 and p < 0.001, respectively). P-tau and T-tau were significantly increased in patients with AD (p < 0.001 and p < 0.001, respectively), but not in patients with DLB, compared with control subjects without dementia. Levels of α-synuclein were significantly lower in CSF from patients with DLB than in control subjects without dementia. The patients with AD and patients with DLB were significantly older than control subjects without dementia (p < 0.001 and p < 0.001, respectively), but there were no age differences between the two patient groups.
Cerebrospinal fluid levels of IL-6 are decreased in patients with DLB
Our first aim was to determine whether IL-6 levels are altered in patients with DLB compared with patients with AD and control subjects without dementia. Because the IL-6 levels were not normally distributed, we transformed the IL-6 values by taking the logarithms (log) of the data before analysis. A multiple-comparisons analysis of log-transformed IL-6 values revealed significant differences between groups (p < 0.001 by ANOVA). Patients with DLB had significantly lower log-transformed IL-6 values than patients with AD and control subjects without dementia (p < 0.001 and p = 0.002, respectively), whereas the log-transformed IL-6 values of patients with AD did not differ from those of control subjects without dementia (Fig. 1a). The analysis further showed that gender had no impact on log-transformed IL-6 values in any of the analysed groups. Although we found no relationship between age and IL-6 levels, we considered the fact that control subjects without dementia were significantly younger than patients with DLB. Thus, to avoid potential biases, we analysed the log-transformed IL-6 values with age as a covariate (analysis of covariance [ANCOVA]). The analysis showed that the log-transformed IL-6 levels were still significantly lower in patients with DLB than in patients with AD and control subjects without dementia (p < 0.001 and p = 0.006, respectively). Finally, we analysed CSF from a randomly selected subset of individually age-matched patients with DLB and control pairs (n = 21). Values of log-transformed IL-6 in this subset of patients with DLB were also significantly lower than those of control subjects without dementia (p = 0.003).
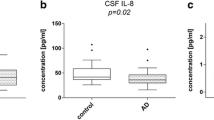
Log-transformed interleukin-6 (logIL-6) levels in cerebrospinal fluid (CSF) of control subjects without dementia (Ctrl), patients with Alzheimer’s disease (AD) and patients with dementia with Lewy bodies (DLB). a Box plot represents the mean ± standard deviation of logIL-6 levels in Ctrl, AD and DLB. b Plot shows correlations between CSF levels of α-synuclein and logIL-6 in patients with DLB (p < 0.01). c Plot demonstrates the negative correlation between Mini Mental State Examination (MMSE) score and logIL-6 in patients with DLB. *Significant difference at p < 0.05 level; **significant difference at p < 0.01 level; ***significant difference at p < 0.001 level
Cerebrospinal fluid levels of IL-6 correlate with MMSE and α-synuclein in patients with DLB
Next, we analysed the association between log-transformed IL-6 and biomarkers for AD and synucleinopathy. We found no correlation between log-transformed IL-6 and the AD markers Aβ1–42, P-tau and T-tau in control subjects without dementia, patients with AD or patients with DLB. We did, however, find a significant positive correlation between log-transformed IL-6 and α-synuclein in patients with DLB (r = 0.383, p = 0.048) (Fig. 1b), but not in patients with AD or control subjects without dementia. Finally, we investigated whether log-transformed IL-6 correlates with cognitive decline in patients with AD and patients with DLB. We detected a significant negative correlation between MMSE score and log-transformed IL-6 in patients with DLB (r = −0.464, p = 0.01) (Fig. 1c) and a trend to significance in patients with AD (r = −0.260, p = 0.089), but not in control subjects without dementia. Correlation analysis of the pairwise age-matched DLB patient and control subgroup showed that the IL-6 correlation with α-synuclein in patients with DLB stayed significant (r = 0.601, p = 0.006), whereas the significance between IL-6 and MMSE was lost and only a trend toward significance remained (r = −0.417, p = 0.060).
Discussion
In line with the many previous preclinical and clinical studies demonstrating a link between cognition and IL-6, we show that CSF levels of IL-6 in patients with DLB significantly and negatively correlated with MMSE score. A similar, although not significant, association trend between these two variables was also seen in patients with AD. These findings indicate that increased IL-6 levels are linked to cognitive disabilities in patients with DLB and patients with AD and could be interpreted as further evidence of involvement of neuroinflammatory processes in both of these disorders. However, our results also show that patients with DLB displayed significantly lower CSF concentrations of IL-6 than both control subjects without dementia and patients with AD. This result inevitably contradicts the idea that neuroinflammatory processes, or at least IL-6 secretion, is a prominent feature of DLB pathology. Interestingly, a lack of protuberant neuroinflammatory processes in patients with DLB, as opposed to in patients with AD, has been described before. As noted in the Introduction section, studies imply that Aβ1–42 pathology underlies the altered IL-6 levels in patients with AD because elevated expression of IL-6 has been found in close vicinity to Aβ1–42 plaques in these patients [19, 20]. If this scenario holds true, one would expect that patients with DLB, who frequently also have Aβ1–42 plaques, would show elevated CSF concentration of IL-6. However, in a previous brain tissue study, researchers compared the amount of activated microglia in patients with AD and patients with DLB and found that, although activated microglia were present in all cortical regions of patients with AD, the number of activated microglia in patients with DLB did not differ from numbers found in control subjects without dementia [44]. The authors of the study pointed out that their patients with DLB, just like patients with DLB in general [23], did not display neurofibrillary tangles (NFT) characteristic of AD and suggested that NFT pathology rather than Aβ1–42 pathology is the underlying cause of the neuroinflammatory processes in AD [44]. This reasoning would explain the difference in IL-6 levels between patients with AD and patients with DLB in our study, as the patients with DLB showed unaltered P-tau concentrations (considered to be indicative of few or no NFT), whereas the P-tau levels in the patients with AD were significantly elevated (considered to be indicative of NFT presence).
Quantification of IL-6 in CSF from patients with DLB has (to our knowledge) been performed only once previously. That study, in contrast to ours, demonstrated a slight, non-significant increase in IL-6 levels [36]. The discrepancy between the previous finding and our results could be explained by the fact that the earlier study used a different IL-6 assay, but other variables may also be accounted for. For example the mean MMSE score of patients with DLB in the earlier study was lower than the mean MMSE score in our DLB patient groups (18.0 ± 4.8 vs 20.4 ± 5.5). Admittedly, the difference in MMSE is small, but in view of our findings demonstrating an increase in IL-6 levels in patients with lower MMSE scores, it may well be that an analysis of CSF from DLB patient groups with lower mean MMSE scores fails to reveal a potential disease-induced decrease in IL-6 levels. Further, the control subjects without dementia included in our study were significantly younger than the patients with DLB and patients with AD, which is a limitation, particularly considering that previous studies have demonstrated an age-dependent increase of IL-6 levels in CSF [45] and serum (for review, see [46]). However, no significant correlation between age and CSF IL-6 levels was found in our study, a finding also reported by other researchers [17, 24, 47]. The IL-6 levels were still significantly decreased in patients with DLB compared with both control subjects without dementia and patients with AD when the IL-6 values were analysed after age adjustment (ANCOVA). In addition, the levels of IL-6 in patients with DLB were significantly lower than those of patients with AD, who were within the same age range as the patients with DLB. Nevertheless, to exclude any potential cofounding effect of age, we selected 21 age-matched DLB patient–control pairs. Analysis of CSF from this subcohort still showed decreased levels of IL-6 in patients with DLB compared with control subjects without dementia (p = 0.003). From a clinical perspective it is important to point out that DLB has a male preponderance [48] and that our DLB cohort therefore should be considered atypical. However, because levels of IL-6 were unaffected by gender in all patient groups, we concluded that gender preponderance did not affect the results in this study.
Further, the size of our cohorts is rather small, which undoubtedly is a limitation of the study. Another limitation is the fact that we had access only to CSF from the individuals included in the study and therefore were not able to analyse IL-6 levels in serum or blood in the same individuals. Indeed, a comparison of IL-6 levels in blood and CSF could potentially indicate whether the IL-6 source is of peripheral or brain parenchymal nature. We would therefore like to emphasise the importance that future ante-mortem clinical studies on the implication of IL-6 in DLB and AD pathology should include larger cohorts as well as analysis of both CSF and serum and blood.
In recent years, levels of α-synuclein have been proposed as a biomarker for synucleinopathy, as patients with PD, DLB and multiple system atrophy often show decreased CSF levels of the peptide compared with patients with AD [1, 49–53] and controls [52, 54, 55]. It should be pointed out, however, that a couple of studies have shown contradicting results, with patients with DLB displaying unaltered [56, 57] or even increased [58] levels of α-synuclein compared with patients with AD. Additionally, in two studies researchers reported unaltered α-synuclein levels in patients with DLB compared with controls [49, 58], although the mean α-synuclein value in one study was lower than in controls. The α-synuclein values in patients with DLB included in our study were significantly decreased, which is in line with results in the majority of previous studies. Although the mean value of α-synuclein in patients with AD was increased, it did not reach significance. This discrepancy seen in our results and others’ could be due to several factors, including diagnostic criteria and cohort sample sizes. The fact that all the previously reported CSF α-synuclein studies used different analytical methods, including in-house ELISAs with various antibodies, mass spectrometry and Luminex technology (Luminex, Austin, TX, USA), is most probably also an important aspect to consider and highlights the importance of finding a global ‘gold standard’ when analysing CSF α-synuclein in the future. Nevertheless it should be underscored that the majority of studies, regardless of analytical method, point towards α-synuclein as a promising biomarker for distinguishing synucleinopathies such as DLB and PD with dementia from other forms of dementia.
Our study shows a positive correlation between IL-6 and α-synuclein levels in CSF from patients with DLB. This finding could be viewed from the perspective that lowered α-synuclein concentration is thought to mirror the synucleinopathy characteristic of entrapment of α-synuclein in the brain parenchyma. If this hypothesis holds true, IL-6 secretion must decrease as α-synuclein pathology increases. Such a scenario would be in line with our results showing decreased levels of IL-6 in patients with DLB compared with patients with AD and control subjects without dementia. The suggested scenario, however, inevitably also contradicts the earlier results demonstrating activated microglia and enhanced mRNA IL-6 levels adjacent to α-synuclein occlusions in the hippocampus of patients with DLB and patients with PD [22]. In vitro studies have additionally shown increased microglial activation [59, 60] and IL-6 secretion [59] in the presence of α-synuclein. Moreover, studies of patients with PD, another neurodegenerative disorder characterised by synucleinopathy, display microglial activation, increased mRNA expression of IL-6 [22, 61] and elevated CSF levels of IL-6 [30, 62]. With regard to these findings, and considering the fact that we found increased IL-6 levels in patients with DLB with very low MMSE scores, it is important not to rule out the possibility that IL-6 plays a vital role in DLB pathology. Future studies using animal and cell culture models are required, however, to fully understand the impact of IL-6 on brain cell integrity and function in relation to DLB pathology.
Conclusions
Our study, by demonstrating lower CSF IL-6 levels as well as a correlation between IL-6 and α-synuclein in patients with DLB but not in patients with AD, underscores the differences in pathological and disease mechanisms between these two neurodegenerative dementia forms. Future studies with larger cohorts are required to ratify the potential use of IL-6 as a clinical biomarker to distinguish DLB pathology from AD pathology in early dementia stages.
The negative correlation we found between IL-6 and MMSE score in patients with DLB, as well as the tendency toward a correlation in patients with AD, adds to the growing evidence pointing towards a potential role of this cytokine in cognitive alterations.
Abbreviations
- Aβ1–42 :
-
amyloid-β peptide 1–42
- AD:
-
Alzheimer’s disease
- ANCOVA:
-
analysis of covariance
- ANOVA:
-
analysis of variance
- CSF:
-
cerebrospinal fluid
- DLB:
-
dementia with Lewy bodies
- ELISA:
-
enzyme-linked immunosorbent assay
- IL:
-
interleukin
- logIL-6:
-
log-transformed interleukin-6 values
- MCI:
-
mild cognitive impairment
- MMSE:
-
Mini Mental State Examination
- NFT:
-
neurofibrillary tangles
- PD:
-
Parkinson’s disease
- P-tau:
-
phosphorylated tau
- TNF-α:
-
tumour necrosis factor-alpha
- T-tau:
-
total tau
References
Nakanishi M, Niidome T, Matsuda S, Akaike A, Kihara T, Sugimoto H. Microglia-derived interleukin-6 and leukaemia inhibitory factor promote astrocytic differentiation of neural stem/progenitor cells. Eur J Neurosci. 2007;25:649–58. doi:10.1111/j.1460-9568.2007.05309.x.
Oh J, McCloskey MA, Blong CC, Bendickson L, Nilsen-Hamilton M, Sakaguchi DS. Astrocyte-derived interleukin-6 promotes specific neuronal differentiation of neural progenitor cells from adult hippocampus. J Neurosci Res. 2010;88:2798–809. doi:10.1002/jnr.22447.
Peng YP, Qiu YH, Lu JH, Wang JJ. Interleukin-6 protects cultured cerebellar granule neurons against glutamate-induced neurotoxicity. Neurosci Lett. 2005;374:192–6. doi:10.1016/j.neulet.2004.10.069.
Pizzi M, Sarnico I, Boroni F, Benarese M, Dreano M, Garotta G, et al. Prevention of neuron and oligodendrocyte degeneration by interleukin-6 (IL-6) and IL-6 receptor/IL-6 fusion protein in organotypic hippocampal slices. Mol Cell Neurosci. 2004;25:301–11. doi:10.1016/j.mcn.2003.10.022.
Wang XC, Qiu YH, Peng YP. Interleukin-6 protects cerebellar granule neurons from NMDA-induced neurotoxicity. Sheng Li Xue Bao. 2007;59:150–6.
Chao CC, Hu S, Ehrlich L, Peterson PK. Interleukin-1 and tumor necrosis factor-α synergistically mediate neurotoxicity: involvement of nitric oxide and of N-methyl-d-aspartate receptors. Brain Behav Immun. 1995;9:355–65.
Samuelsson AM, Jennische E, Hansson HA, Holmang A. Prenatal exposure to interleukin-6 results in inflammatory neurodegeneration in hippocampus with NMDA/GABAA dysregulation and impaired spatial learning. Am J Physiol Regul Integr Comp Physiol. 2006;290:R1345–56. doi:10.1152/ajpregu.00268.2005.
Steffensen SC, Campbell IL, Henriksen SJ. Site-specific hippocampal pathophysiology due to cerebral overexpression of interleukin-6 in transgenic mice. Brain Res. 1994;652:149–53.
Vallières L, Campbell IL, Gage FH, Sawchenko PE. Reduced hippocampal neurogenesis in adult transgenic mice with chronic astrocytic production of interleukin-6. J Neurosci. 2002;22:486–92.
Samuelsson AM, Alexanderson C, Mölne J, Haraldsson B, Hansell P, Holmäng A. Prenatal exposure to interleukin-6 results in hypertension and alterations in the renin-angiotensin system of the rat. J Physiol. 2006;575:855–67. doi:10.1113/jphysiol.2006.111260.
Balschun D, Wetzel W, Del Rey A, Pitossi F, Schneider H, Zuschratter W, et al. Interleukin-6: a cytokine to forget. FASEB J. 2004;18:1788–90. doi:10.1096/fj.04-1625fje.
Sparkman NL, Buchanan JB, Heyen JR, Chen J, Beverly JL, Johnson RW. Interleukin-6 facilitates lipopolysaccharide-induced disruption in working memory and expression of other proinflammatory cytokines in hippocampal neuronal cell layers. J Neurosci. 2006;26:10709–16. doi:10.1523/JNEUROSCI.3376-06.2006.
Adriaensen W, Matheï C, Vaes B, van Pottelbergh G, Wallemacq P, Degryse JM. Interleukin-6 predicts short-term global functional decline in the oldest old: results from the BELFRAIL study. Age (Dordr). 2014;36:9723. doi:10.1007/s11357-014-9723-3.
Marioni RE, Strachan MW, Reynolds RM, Lowe GD, Mitchell RJ, Fowkes FG, et al. Association between raised inflammatory markers and cognitive decline in elderly people with type 2 diabetes: the Edinburgh Type 2 Diabetes Study. Diabetes. 2010;59:710–3. doi:10.2337/db09-1163.
Weaver JD, Huang MH, Albert M, Harris T, Rowe JW, Seeman TE. Interleukin-6 and risk of cognitive decline: MacArthur studies of successful aging. Neurology. 2002;59:371–8.
Wright CB, Sacco RL, Rundek T, Delman J, Rabbani L, Elkind M. Interleukin-6 is associated with cognitive function: the Northern Manhattan Study. J Stroke Cerebrovasc Dis. 2006;15:34–8. doi:10.1016/j.jstrokecerebrovasdis.2005.08.009.
Lindqvist D, Janelidze S, Hagell P, Erhardt S, Samuelsson M, Minthon L, et al. Interleukin-6 is elevated in the cerebrospinal fluid of suicide attempters and related to symptom severity. Biol Psychiatry. 2009;66:287–92. doi:10.1016/j.biopsych.2009.01.030.
Yu SY, Zuo LJ, Wang F, Chen ZJ, Hu Y, Wang YJ, et al. Potential biomarkers relating pathological proteins, neuroinflammatory factors and free radicals in PD patients with cognitive impairment: a cross-sectional study. BMC Neurol. 2014;14:113. doi:10.1186/1471-2377-14-113.
Huell M, Strauss S, Volk B, Berger M, Bauer J. Interleukin-6 is present in early stages of plaque formation and is restricted to the brains of Alzheimer’s disease patients. Acta Neuropathol. 1995;89:544–51.
Hull M, Strauss S, Berger M, Volk B, Bauer J. The participation of interleukin-6, a stress-inducible cytokine, in the pathogenesis of Alzheimer’s disease. Behav Brain Res. 1996;78:37–41.
Blennow K, de Leon MJ, Zetterberg H. Alzheimer’s disease. Lancet. 2006;368:387–403. doi:10.1016/S0140-6736(06)69113-7.
Imamura K, Hishikawa N, Ono K, Suzuki H, Sawada M, Nagatsu T, et al. Cytokine production of activated microglia and decrease in neurotrophic factors of neurons in the hippocampus of Lewy body disease brains. Acta Neuropathol. 2005;109:141–50. doi:10.1007/s00401-004-0919-y.
McKeith IG, Dickson DW, Lowe J, Emre M, O’Brien JT, Feldman H, et al. Diagnosis and management of dementia with Lewy bodies: third report of the DLB Consortium. Neurology. 2005;65:1863–72.
Lindqvist D, Hall S, Surova Y, Nielsen HM, Janelidze S, Brundin L, et al. Cerebrospinal fluid inflammatory markers in Parkinson’s disease – associations with depression, fatigue, and cognitive impairment. Brain Behav Immun. 2013;33:183–9. doi:10.1016/j.bbi.2013.07.007.
Hansson O, Zetterberg H, Buchhave P, Londos E, Blennow K, Minthon L. Association between CSF biomarkers and incipient Alzheimer’s disease in patients with mild cognitive impairment: a follow-up study. Lancet Neurol. 2006;5:228–34. doi:10.1016/S1474-4422(06)70355-6.
Nascimento CM, Pereira JR, de Andrade LP, Garuffi M, Talib LL, Forlenza OV, et al. Physical exercise in MCI elderly promotes reduction of pro-inflammatory cytokines and improvements on cognition and BDNF peripheral levels. Curr Alzheimer Res. 2014;11:799–805.
Brebner K, Hayley S, Zacharko R, Merali Z, Anisman H. Synergistic effects of interleukin-1β, interleukin-6, and tumor necrosis factor-α: central monoamine, corticosterone, and behavioral variations. Neuropsychopharmacology. 2000;22:566–80. doi:10.1016/S0893-133X(99)00166-9.
Holmes C, Cunningham C, Zotova E, Woolford J, Dean C, Kerr S, et al. Systemic inflammation and disease progression in Alzheimer disease. Neurology. 2009;73:768–74. doi:10.1212/WNL.0b013e3181b6bb95.
Holmes C, El-Okl M, Williams AL, Cunningham C, Wilcockson D, Perry VH. Systemic infection, interleukin 1β, and cognitive decline in Alzheimer’s disease. J Neurol Neurosurg Psychiatry. 2003;74:788–9.
Blum-Degen D, Müller T, Kuhn W, Gerlach M, Przuntek H, Riederer P. Interleukin-1β and interleukin-6 are elevated in the cerebrospinal fluid of Alzheimer’s and de novo Parkinson’s disease patients. Neurosci Lett. 1995;202:17–20.
Jia JP, Meng R, Sun YX, Sun WJ, Ji XM, Jia LF. Cerebrospinal fluid tau, Aβ1–42 and inflammatory cytokines in patients with Alzheimer’s disease and vascular dementia. Neurosci Lett. 2005;383:12–6. doi:10.1016/j.neulet.2005.03.051.
Martínez M, Fernández-Vivancos E, Frank A, De la Fuente M, Hernanz A. Increased cerebrospinal fluid Fas (Apo-1) levels in Alzheimer’s disease: relationship with IL-6 concentrations. Brain Res. 2000;869:216–9.
Yamada K, Kono K, Umegaki H, Iguchi A, Fukatsu T, Nakashima N, et al. Decreased interleukin-6 level in the cerebrospinal fluid of patients with Alzheimer-type dementia. Neurosci Lett. 1995;186:219–21.
Engelborghs S, De Brabander M, De Cree J, D’Hooge R, Geerts H, Verhaegen H, et al. Unchanged levels of interleukins, neopterin, interferon-γ and tumor necrosis factor-α in cerebrospinal fluid of patients with dementia of the Alzheimer type. Neurochem Int. 1999;34:523–30.
März P, Heese K, Hock C, Golombowski S, Müller-Spahn F, Rose-John S, et al. Interleukin-6 (IL-6) and soluble forms of IL-6 receptors are not altered in cerebrospinal fluid of Alzheimer’s disease patients. Neurosci Lett. 1997;239:29–32.
Gómez-Tortosa E, Gonzalo I, Fanjul S, Sainz MJ, Cantarero S, Cemillán C, et al. Cerebrospinal fluid markers in dementia with Lewy bodies compared with Alzheimer disease. Arch Neurol. 2003;60:1218–22. doi:10.1001/archneur.60.9.1218.
Nielsen H, Ek D, Avdic U, Orbjörn C, Hansson O, The Netherlands Brain Bank, et al. NG2 cells, a new trail for Alzheimer’s disease mechanisms? Acta Neuropathol Commun. 2013;1:7.
Wennström M, Surova Y, Hall S, Nilsson C, Minthon L, Boström F, et al. Low CSF levels of both α-synuclein and the α-synuclein cleaving enzyme neurosin in patients with synucleinopathy. PLoS One. 2013;8:e53250. doi:10.1371/journal.pone.0053250.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Washington, DC: American Psychiatric Press; 1994.
McKhann G, Drachman D, Folstein M, Katzman R, Price D, Stadlan EM. Clinical diagnosis of Alzheimer’s disease: report of the NINCDS-ADRDA Work Group under the auspices of Department of Health and Human Services Task Force on Alzheimer’s Disease. Neurology. 1984;34:939–44.
McKeith IG, Galasko D, Kosaka K, Perry EK, Dickson DW, Hansen LA, et al. Consensus guidelines for the clinical and pathologic diagnosis of dementia with Lewy bodies (DLB): report of the Consortium on DLB international workshop. Neurology. 1996;47:1113–24.
Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:189–98.
Wennström M, Londos E, Minthon L, Nielsen HM. Altered CSF orexin and alpha-synuclein levels in dementia patients. J Alzheimers Dis. 2012;29:125–32. doi:10.3233/JAD-2012-111655.
Shepherd CE, Thiel E, McCann H, Harding AJ, Halliday GM. Cortical inflammation in Alzheimer disease but not dementia with Lewy bodies. Arch Neurol. 2000;57:817–22.
Kálmán J, Juhász A, Laird G, Dickens P, Járdánházy T, Rimanóczy A, et al. Serum interleukin-6 levels correlate with the severity of dementia in Down syndrome and in Alzheimer’s disease. Acta Neurol Scand. 1997;96:236–40.
Ershler WB, Keller ET. Age-associated increased interleukin-6 gene expression, late-life diseases, and frailty. Annu Rev Med. 2000;51:245–70. doi:10.1146/annurev.med.51.1.245.
Baker DG, Ekhator NN, Kasckow JW, Hill KK, Zoumakis E, Dashevsky BA, et al. Plasma and cerebrospinal fluid interleukin-6 concentrations in posttraumatic stress disorder. Neuroimmunomodulation. 2001;9:209–17.
Nelson PT, Schmitt FA, Jicha GA, Kryscio RJ, Abner EL, Smith CD, et al. Association between male gender and cortical Lewy body pathology in large autopsy series. J Neurol. 2010;257:1875–81. doi:10.1007/S00415-010-5630-4.
Hansson O, Hall S, Ohrfelt A, Zetterberg H, Blennow K, Minthon L, et al. Levels of cerebrospinal fluid α-synuclein oligomers are increased in Parkinson’s disease with dementia and dementia with Lewy bodies compared to Alzheimer’s disease. Alzheimers Res Ther. 2014;6:25. doi:10.1186/alzrt255.
Kasuga K, Tokutake T, Ishikawa A, Uchiyama T, Tokuda T, Onodera O, et al. Differential levels of α-synuclein, β-amyloid42 and tau in CSF between patients with dementia with Lewy bodies and Alzheimer’s disease. J Neurol Neurosurg Psychiatry. 2010;81:608–10. doi:10.1136/jnnp.2009.197483.
Mollenhauer B, Locascio JJ, Schulz-Schaeffer W, Sixel-Döring F, Trenkwalder C, Schlossmacher MG. α-Synuclein and tau concentrations in cerebrospinal fluid of patients presenting with parkinsonism: a cohort study. Lancet Neurol. 2011;10:230–40. doi:10.1016/S1474-4422(11)70014-X. A published erratum appears in Lancet Neurol. 2011;10:297.
Parnetti L, Chiasserini D, Bellomo G, Giannandrea D, De Carlo C, Qureshi MM, et al. Cerebrospinal fluid tau/α-synuclein ratio in Parkinson’s disease and degenerative dementias. Mov Disord. 2011;26:1428–35. doi:10.1002/mds.23670.
Tateno F, Sakakibara R, Kawai T, Kishi M, Murano T. α-Synuclein in the cerebrospinal fluid differentiates synucleinopathies (Parkinson disease, dementia with Lewy bodies, multiple system atrophy) from Alzheimer disease. Alzheimer Dis Assoc Disord. 2012;26:213–6. doi:10.1097/WAD.0b013e31823899cc.
Mollenhauer B, Cullen V, Kahn I, Krastins B, Outeiro TF, Pepivani I, et al. Direct quantification of CSF α-synuclein by ELISA and first cross-sectional study in patients with neurodegeneration. Exp Neurol. 2008;213:315–25. doi:10.1016/j.expneurol.2008.06.004.
Sako W, Murakami N, Izumi Y, Kaji R. Reduced α-synuclein in cerebrospinal fluid in synucleinopathies: evidence from a meta-analysis. Mov Disord. 2014;29:1599–605. doi:10.1002/mds.26036.
Noguchi-Shinohara M, Tokuda T, Yoshita M, Kasai T, Ono K, Nakagawa M, et al. CSF α-synuclein levels in dementia with Lewy bodies and Alzheimer’s disease. Brain Res. 2009;1251:1–6. doi:10.1016/j.brainres.2008.11.055.
Spies PE, Melis RJ, Sjögren MJ, Rikkert MG, Verbeek MM. Cerebrospinal fluid α-synuclein does not discriminate between dementia disorders. J Alzheimers Dis. 2009;16:363–9. doi:10.3233/JAD-2009-0955.
Kapaki E, Paraskevas GP, Emmanouilidou E, Vekrellis K. The diagnostic value of CSF α-synuclein in the differential diagnosis of dementia with Lewy bodies vs normal subjects and patients with Alzheimer’s disease. PLoS One. 2013;8, e81654. doi:10.1371/journal.pone.0081654.
Ingham V, Williams A, Bate C. Glimepiride reduces CD14 expression and cytokine secretion from macrophages. J Neuroinflammation. 2014;11:115. doi:10.1186/1742-2094-11-115.
Zhang W, Wang T, Pei Z, Miller DS, Wu X, Block ML, et al. Aggregated α-synuclein activates microglia: a process leading to disease progression in Parkinson’s disease. FASEB J. 2005;19:533–42. doi:10.1096/fj.04-2751com.
Garcia-Esparcia P, Llorens F, Carmona M, Ferrer I. Complex deregulation and expression of cytokines and mediators of the immune response in Parkinson’s disease brain is region dependent. Brain Pathol. 2014;24:584–98. doi:10.1111/bpa.12137.
Müller T, Blum-Degen D, Przuntek H, Kuhn W. Interleukin-6 levels in cerebrospinal fluid inversely correlate to severity of Parkinson’s disease. Acta Neurol Scand. 1998;98:142–4.
Acknowledgements
This work was supported by the Swedish Dementia Foundation (MW), ALF (OH, KN, LM), the Royal Physiographic Society of Lund (MW), the Greta and Johan Kockska foundations (MW), Crafoord Foundation (MW) and the Swedish Research Council (521-2013-3448) (MW). The authors thank Camilla Orbjörn for technical support.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors’ contributions
MW designed the study, carried out the IL-6 analysis, analysed data and drafted the manuscript. SH, KN, EL and LM participated in patient recruitment and revised the manuscript. OH participated in study design and edited the final version of manuscript. All authors read and approved the final manuscript.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Wennström, M., Hall, S., Nägga, K. et al. Cerebrospinal fluid levels of IL-6 are decreased and correlate with cognitive status in DLB patients. Alz Res Therapy 7, 63 (2015). https://doi.org/10.1186/s13195-015-0145-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13195-015-0145-y