Abstract
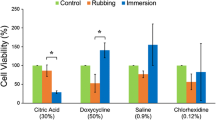
Detoxification with citric acid is an effective method of biofilm removal from titanium (Ti) dental implant surfaces affected by peri-implantitis, but its effects on Ti surface properties is not well understood. This study aimed at evaluating the surface characteristics and biological response to Ti after bacterial biofilm formation followed by citric acid detoxification. Ti specimens were immersed with oral bacteria under aerobic (Streptococcus mutans, Streptococcus sanguinis, Streptococcus salivarius and Aggregatibacter actinomycetemcomitans) and anaerobic (aerobic polyculture with Fusobacterium nucleatum and Porphyromonas gingivalis) conditions for 4 h or 7 days (n = 3). Immersion was followed by rubbing treatment with 0.9% saline or 40% citric acid for 8 min. Post-treatment, the surface morphology and microstructure were studied by optical microscopy and Raman spectroscopy, respectively. Osteoblast viability after 3 days on Ti post-treatment was assessed. Electrochemical testing revealed corrosion behavior post-treatment while X-ray photoelectron spectroscopy indicated oxide layer state. While signs of pitting and corrosion attack on Ti exposed to bacteria and/or detoxification were evident, no surface oxide phase changes were detected. Samples treated with citric acid had lower polarization resistance and higher corrosion rate after aerobic and anaerobic immersion. Samples exposed to bacteria and citric acid treatment had higher oxide thickness under aerobic but not anaerobic immersion after 4 h and 7 days. Osteoblast viability was not significantly affected by immersion and treatment. Within the study’s limitations, citric acid detoxification on Ti post-bacterial exposure is not expected to adversely change oxide composition, thickness, and corrosion behavior while maintaining host cell growth.






Similar content being viewed by others
Data Availability
Data available within the article.
References
Elias CN (2011) Factors affecting the success of dental implants. IntechOpen, London. https://doi.org/10.5772/18746
Paridah M, Moradbak A, Mohamed A, Abdulwahab Taiwo Owolabi F, Asniza M, Abdul Khalid SH (2015) We are IntechOpen , the world ’ s leading publisher of Open Access books Built by scientists , for scientists TOP 1%, vol i, no. tourism, p 13. Intech, London. https://doi.org/10.5772/57353
Guglielmotti MB, Olmedo DG, Cabrini RL (2019) Research on implants and osseointegration. Periodontol 2000 79(1):178–189. https://doi.org/10.1111/prd.12254
Wheelis SE, Gindri IM, Valderrama P, Wilson TG, Huang J, Rodrigues DC (2016) Effects of decontamination solutions on the surface of titanium: investigation of surface morphology, composition, and roughness. Clin Oral Implants Res 27(3):329–340. https://doi.org/10.1111/clr.12545
Ramesh D, Sridhar S, Siddiqui DA, Valderrama P, Rodrigues DC (2017) Detoxification of titanium implant surfaces: evaluation of surface morphology and bone-forming cell compatibility. J Bio Tribo-Corros 3(4):1–13. https://doi.org/10.1007/s40735-017-0111-2
Palmquist A, Omar OM, Esposito M, Lausmaa J, Thomsen P (2010) Titanium oral implants: surface characteristics, interface biology and clinical outcome. J R Soc Interface 7(Suppl. 5):515–527. https://doi.org/10.1098/rsif.2010.0118.focus
Sakka S, Baroudi K, Nassani MZ (2012) Factors associated with early and late failure of dental implants. J Invest Clin Dent 3(4):258–261. https://doi.org/10.1111/j.2041-1626.2012.00162.x
Murphy C (2019) Dental implant failure signs, treatment and replacement. See Pictures
Cochran D, Froum S (2013) Academy Report: peri-implant mucositis and peri-implantitis: a current understanding of their diagnoses and clinical implications. J Periodontol 84(4):436–443. https://doi.org/10.1902/jop.2013.134001
Prathapachandran J, Suresh N (2019) Management of peri-implantitis. Dent Res J (Isfahan) 9(5):516–521
Mellado-Valero A, Buitrago-Vera P, Solá-Ruiz MF, Ferrer-García JC (2013) Decontamination of dental implant surface in peri-implantitis treatment: a literature review. Med Oral Patol Oral Cir Bucal. https://doi.org/10.4317/medoral.19420
Valderrama P, Wilson TG (2013) Detoxification of implant surfaces affected by peri-implant disease: an overview of surgical methods. Int J Dent. https://doi.org/10.1155/2013/740680
Delgado-Ruiz R, Romanos G (2018) Potential causes of titanium particle and ion release in implant dentistry: a systematic review. Int J MolSci 19(11):3585. https://doi.org/10.3390/ijms19113585
Gia D, Hong K, Oh J (2017) Recent advances in dental implants. MaxillofacPlastReconstrSurg. https://doi.org/10.1186/s40902-017-0132-2
Souza JGS, Cordeiro JM, Lima CV, Barão VAR (2019) Citric acid reduces oral biofilm and influences the electrochemical behavior of titanium: an in situ and in vitro study. J Periodontol 90(2):149–158. https://doi.org/10.1002/JPER.18-0178
Mouhyi J, Sennerby L, Pireaux JJ, Dourov N, Nammour S, Van Reck J (1998) An XPS and SEM evaluation of six chemical and physical techniques for cleaning of contaminated titanium implants. Clin Oral Implant Res 9(3):185–194. https://doi.org/10.1034/j.1600-0501.1998.090306.x
Hanawa T, Asami K, Asaoka K (1998) Repassivation of titanium and surface oxide film regenerated in simulated bioliquid. J Biomed Mater Res 40(4):530–538. https://doi.org/10.1002/(SICI)1097-4636(19980615)40:4%3c530::AID-JBM3%3e3.0.CO;2-G
Claffey N, Clarke E, Polyzois I, Renvert S (2008) Surgical treatment of peri-implantitis. J ClinPeriodontol 35(SUPPL. 8):316–332. https://doi.org/10.1111/j.1600-051X.2008.01277.x
Ungvári K et al (2010) Effects on titanium implant surfaces of chemical agents used for the treatment of peri-implantitis. J Biomed Mater Res Part B ApplBiomater 94(1):222–229. https://doi.org/10.1002/jbm.b.31644
Wheelis SE (2017) Investigation of titanium oxide characteristics on healing abutments: retrieval characterization and soft-tissue compatibility. UTD Theses and Dissertations
RRUFF, Shigley J. Anatase R070582. Asker, Akershus, Norway
Souza JCM, Henriques M, Teughels W, Ponthiaux P, Celis JP, Rocha LA (2015) Wear and corrosion interactions on titanium in oral environment: literature review. J Bio Tribo-Corros. https://doi.org/10.1007/s40735-015-0013-0
Lang NP, Berglundh T (2011) Periimplant diseases: where are we now?—Consensus of the Seventh European workshop on periodontology. J ClinPeriodontol 38(SUPPL. 11):178–181. https://doi.org/10.1111/j.1600-051X.2010.01674.x
Jepsen S et al (2015) Primary prevention of peri-implantitis: managing peri-implant mucositis. J ClinPeriodontol 42(S16):S152–S157. https://doi.org/10.1111/jcpe.12369
Adya N, Alam M, Ravindranath T, Mubeen A, Saluja B (2005) Corrosion in titanium dental implants: literature review. J Indian ProsthodontSoc 5(3):126–131. https://doi.org/10.4103/0972-4052.17104
Chin MYH, Sandham A, de Vries J, van der Mei HC, Busscher HJ (2007) Biofilm formation on surface characterized micro-implants for skeletal anchorage in orthodontics. Biomaterials 28(11):2032–2040. https://doi.org/10.1016/j.biomaterials.2006.12.014
Zablotsky MH, Wittrig EE, Diedrich DL, Layman DL, Meffert RM (1992) FIBROBLASTIC GROWTH AND ATTACHMENT ON HYDROXYAPATITE-COATED TITANIUM SURFACES FOLLOWING THE USE OF VARIOUS DETOXIFICATION MODALITIES. PART II: CONTAMINATED HYDROXYAPATITE. Implant Dent 1(3):195–202. https://doi.org/10.1097/00008505-199200130-00006
Ferreira R et al (2018) Comparison of the effect of root surface modification with citric acid, EDTA, and aPDT on adhesion and proliferation of human gingival fibroblasts and osteoblasts: an in vitro study. Lasers Med Sci 33(3):533–538. https://doi.org/10.1007/s10103-017-2395-3
Alhag M, Renvert S, Polyzois I, Claffey N (2008) Re-osseointegration on rough implant surfaces previously coated with bacterial biofilm: an experimental study in the dog. Clin Oral Implants Res 19(2):182–187. https://doi.org/10.1111/j.1600-0501.2007.01429.x
Acknowledgements
The authors acknowledge the University of Texas at Dallas (UTD) for providing financial support for this study, the Biomaterials for Osseointegration and Novel Engineering (BONE) Lab for providing the facilities and funding for this research. The authors would like to thank Yutika Ineni for her assistance with experiments.
Funding
The work was supported by the Biomaterials for Osseointegration and Novel Engineering (BONE) Lab, Department of Bioengineering, The University of Texas at Dallas (UTD), Richardson.
Author information
Authors and Affiliations
Contributions
DCR and BLC conceived the ideas. BLC collected and analyzed the data. KLP and DAS provided their microbiology and surface characterization expertise respectively on the experiments and the manuscript. DCR supervised and secured funding for the project and assisted with manuscript writing. BLC conducted all the experiments and wrote the manuscript with input and revision by all coauthors.
Corresponding author
Ethics declarations
Conflict of interest
Bhuvana Lakkasetter Chandrashekar declares that she has no conflict of interest. Danyal A. Siddiqui declares that he has no conflict of interest. Kelli L. Palmer declares that she has no conflict of interest. Danieli C. Rodrigues declares that she has no conflict of interest.
Consent for Publication
All the authors consent to the publication of current manuscript, should the article be accepted by the Editor-in-chief upon completion.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lakkasetter Chandrashekar, B., Siddiqui, D.A., Palmer, K.L. et al. Titanium Surfaces and Detoxification Procedures: Effects of Bacterial Biofilm and Citric Acid Exposure on Oxide Layer Behavior. J Bio Tribo Corros 7, 48 (2021). https://doi.org/10.1007/s40735-021-00484-w
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40735-021-00484-w