Abstract
Background
Patients with chronic kidney disease (CKD) have an increased risk of venous thromboembolism (VTE) and atrial fibrillation (AF). Anticoagulants have not been studied in randomised controlled trials with CrCl < 30 ml/min. The objective of this review was to identify the impact of different anticoagulant strategies in patients with advanced CKD including dialysis.
Methods
We conducted a systematic review of randomized controlled trials and cohort studies, searching electronic databases from 1946 to 2022. Studies that evaluated both thrombotic and bleeding outcomes with anticoagulant use in CrCl < 50 ml/min were included.
Results
Our initial search yielded 14,503 papers with 53 suitable for inclusion. RCTs comparing direct oral anticoagulants (DOACs) versus warfarin for patients with VTE and CrCl 30-50 ml/min found no difference in recurrent VTE events (RR 0.68(95% CI 0.42–1.11)) with reduced bleeding (RR 0.65 (95% CI 0.45–0.94)). Observational data in haemodialysis suggest lower risk of recurrent VTE and major bleeding with apixaban versus warfarin. Very few studies examining outcomes were available for therapeutic and prophylactic dose low molecular weight heparin for CrCl < 30 ml/min. Findings for patients with AF on dialysis were that warfarin or DOACs had a similar or higher risk of stroke compared to no anticoagulation. For patients with AF and CrCl < 30 ml/min not on dialysis, anticoagulation should be considered on an individual basis, with limited studies suggesting DOACs may have a preferable safety profile.
Conclusion
Further studies are still required, some ongoing, in patients with advanced CKD (CrCl < 30 ml/min) to identify the safest and most effective treatment options for VTE and AF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Patients with chronic kidney disease have an increased risk of venous thromboembolism (VTE), which includes both deep vein thrombosis (DVT) and pulmonary embolism. Patients with chronic kidney disease (CKD) stage 3 and 4 (eGFR 30–60 and eGFR15-29 ml/min/1.73 m2) have an adjusted relative risk 1.71 (95% CI 1.18 to 2.49) of developing DVT compared to those with normal renal function [1]. The risk is further heightened in those on dialysis where the age-adjusted pulmonary embolism incidence ratio is 2.34 compared to those with normal renal function [2]. With hospital-acquired VTE being a potentially preventable cause of in-hospital mortality the increased risk of VTE also highlights the need for appropriate VTE prophylaxis in a CKD population. Patients with CKD are also at increased risk of developing atrial fibrillation (AF) which may predispose them to thromboembolic stroke (ischaemic stroke). The prevalence of AF in the general population is estimated at around 1–2% [3], this rate is reported to be much higher as renal function declines, with reports of up to 10–25% of patients on dialysis [4,5,6,7,8,9].
Conversely, bleeding risk is also increased in the CKD population. It has been shown that the frequency of cerebral haemorrhage is over ten times higher in CKD patients than in the non-renal failure population [10], with an unpublished analysis from the Fresenius Medical Care Research database showing that 2.7% of all deaths in dialysis patients were secondary to haemorrhage [11].
Vitamin K antagonists (VKA) have been the mainstay of therapy for VTE treatment and AF in CKD. However, vitamin K antagonists are not without concerns in this population with difficulties obtaining time in therapeutic range [12], regular monitoring requirements, potential risks of vascular calcification and the rare condition calciphylaxis [13]. The use of direct oral anticoagulants (DOACs) is currently on the rise for both VTE and AF, however, in more severe renal impairment, CrCl < 30 ml/min, they have not been studied in randomised controlled trials (RCTs). Low molecular weight heparins (LMWHs) have been widely used for the initial treatment of VTE and are the mainstay of therapy for VTE prophylaxis, however, they have not been well studied in subjects with severe renal impairment, CrCl < 30 ml/min.
The aim of this systematic review is to identify the impact of different anticoagulant strategies in patients with advanced CKD CrCl < 50 ml/min, in terms of thrombotic and bleeding outcomes. This review provides the most up-to-date literature for anticoagulant strategies in AF, VTE and VTE prophylaxis for the various stages of advanced CKD including dialysis.
Materials and methods
Information sources and search strategy
The protocol for this review has been published in the International Prospective Register of Systematic Reviews (https://www.crd.york.ac.uk/prospero/, registration number CRD42020219449).
The following databases were used to undertake the search: Ovid MEDLINE (1946 to May 23, 2022), Embase (1974 to 2022 May 23), EBM Reviews—Cochrane Database of Systematic Reviews (2005 to May 18, 2022). Review papers were screened to identify any other relevant studies that had not been identified in the search. The search strategy was supported by a specialist librarian at the University of Manchester and was developed using MeSH terms and keywords relating to current anticoagulants in use. The full search strategy is detailed in supplementary appendix 1.
Study selection
Randomised controlled studies and prospective or retrospective observational cohort studies were included. Included studies related to advanced CKD defined as CrCl or eGFR < 50 ml/min. Participants had either AF, VTE or required VTE prophylaxis. Studies that involved children < 18 years were excluded along with studies solely examining the use of anticoagulation to prevent clotting of the extracorporeal circuit. Other papers such as case studies, editorials, review articles, non-English studies and guidelines were excluded, although review papers were screened for relevant studies.
Only studies that reported both thrombotic and bleeding outcomes in patients taking an anticoagulant versus another anticoagulant or no anticoagulant were included.
Data extraction
KP and AS screened the search results with any uncertainties being discussed with SM, PL and JT. At least two among KP, AS, RM and JH independently undertook data extraction into a modified version of the Cochrane data collection form. Extracted data included relevant baseline characteristics e.g. age, renal function, thrombotic and bleeding risk factors, methods (study design, duration of follow up), interventions (treatment and comparator) and outcomes. Efficacy outcomes included the incidence of stroke and systemic embolism for AF and incidence of VTE/VTE recurrence in the treatment or prophylaxis of VTE. Safety outcomes included the incidence and severity of bleeding episodes.
Risk of bias
For randomised controlled studies the revised Cochrane Risk-Of-Bias tool (ROB 2) was used [14]. For non-randomised studies the Risk Of Bias In Non-randomized Studies – of Interventions (ROBINS-I) tool was used [15]. KP, AS, RM and JH independently undertook bias assessment to determine study quality with disagreement being resolved by PL.
Results
Study yield
Our initial search yielded 14,503 papers, of which 14,103 were screened after duplicates were removed. Another 13,848 were removed due to being irrelevant to anticoagulant use in CKD, related only to dialysis circuit anticoagulation or being an editorial, case report, review or guideline. There were 255 papers that included anticoagulant use in CKD, and after further assessment, 53 papers were suitable for inclusion. The overall study selection process is detailed in Fig. 1.
VTE treatment in patients with CrCl < 50 ml/min
Study characteristics
An overview of the selected VTE studies is presented in Table 1. There were four RCTs of DOACs versus VKA, of which two were analyses of the CKD subgroup [16,17,18,19]. One cohort study was included that studied cancer-associated VTE [20]. These studies focused mainly on patients with CrCl 30–50 ml/min, however, there were small numbers of patients with a CrCl < 30 ml/min in two of the RCTs and within the cohort study [16, 18, 20]. All of the RCTs used Cockcroft-Gault creatinine clearance and the cohort study used Modified Diet in Renal Disease equation [21]. An observational study in dialysis patients is also included which compared apixaban to warfarin in the acute treatment of VTE [22].
Quality assessment
Assessment of the quality of the four RCTs found the studies to be of high quality and of low risk of bias [16,17,18,19]. The two cohort studies were deemed at low [22] or moderate risk of bias [20], Supplementary Tables 1 and 2.
Recurrent VTE outcomes
Six studies reported on recurrent VTE during treatment of VTE. An overview of these outcomes is presented in Table 1.
DOACs vs warfarin
There were four RCTs comparing DOACs to warfarin for the treatment of VTE [16,17,18,19]. There was no significant difference between the efficacy of the DOACs compared to warfarin for patients with CrCl 30-50 ml/min although there was a trend for increased efficacy of dabigatran [19], Fig. 2. The cohort study found apixaban had a reduction in recurrent VTE compared to warfarin in a haemodialysis population being treated for acute VTE (HR 0.58 (95%CI 0.43–0.77)) [22].
Recurrent VTE events from RCTs in patients with CrCl 30-50 ml/min [16,17,18,19]. Figure created using RevMan software [23]. Please note the number of patients from Agnelli 2013 in this analysis differs from the total number of patients in Table 1. The numbers are taken directly from the paper and it is assumed the difference relates to missing outcome data or loss of follow up [18]
LMWH vs warfarin
One retrospective cohort study examined patients treated for cancer-related VTE [20]. For those with an eGFR 30–45, warfarin was associated with less recurrent VTE than LMWH, 2.9/100 person years versus 25.5/100 person years [20]. The major limitation to this study is that the type of LMWH and dose used was not reported and a number of patients (285/1684) switched between treatment regimens [20].
Major bleeding
An overview of the definition and incidences of bleeding is presented in Table 1.
DOACs vs warfarin
The RCT sub-analyses looking at apixaban and rivaroxaban found lower rates of major bleeding in patients with CrCl 30–49 ml/min versus warfarin [16, 18]. For apixaban, major bleeding was 2.9% vs 5.5% in the warfarin arm [18] and rivaroxaban 0.9% vs 3.9% in the warfarin arm [16]. The major bleeding rates for dabigatran were similar to warfarin [19]. Major bleeding of the DOACs versus warfarin is presented in Fig. 3. The cohort study found that for patients on haemodialysis apixaban use was associated with a HR 0.78 (95% CI 0.62–0.98).
Major bleeding events from RCTs in patients with CrCl 30-50 ml/min [16,17,18,19]. Note that the Buller study is a composite outcome of major bleeding and CRNMB. Figure created using RevMan software [23]. Please note the number of patients from Bauersachs 2014 and Goldhaber 2017 in this analysis differs from the total included patients in Table 1. The numbers are taken directly from the papers and it is assumed the difference relates to missing outcome data or loss of follow up [16, 19]
LMWH vs warfarin
The cohort study found that LMWH was associated with both higher major and fatal bleeding in patients with GFR < 30 ml/min, VKA vs LMWH, aHR 0.5 (95% CI 0.1–2.8) [20], although these findings should be interpreted with caution given the wide confidence intervals and lower interval close to no difference. In subjects with CrCl 30–49 ml/min there was no real difference in bleeding events [20].
VTE Prophylaxis in non-surgical patients with CrCl < 50 ml/min
Two cohort studies met inclusion criteria, both in the haemodialysis population [24, 25], Supplementary Table 3. These studies examined VTE prophylaxis for patients with an acute medical illness or a recent hospital admission with ongoing risk factors for VTE. Both studies used enoxaparin compared to unfractionated heparin (UFH); one study used the FDA licensed dose of enoxaparin 30 mg daily [25], whilst the second study had variable enoxaparin dosing ranging from 20 mg daily to 60 mg daily [24]. The heparin dose remained consistent in the first cohort study at 5000units three times daily [25] with doses ranging from 5000units twice to three times daily in the second study [24].
Quality
The largest cohort study was deemed to have moderate bias due to potential selection bias and varying doses of both treatments [24]. The second cohort study was deemed to have a serious/critical bias as it did not use any statistical methods to take into consideration confounders between the treatment and comparator groups [25], Supplementary Table 2.
Venous thromboembolism outcomes with VTE prophylaxis in patients with CrCl < 50 ml/min
An overview of VTE outcomes is presented in Supplementary Table 3.
Enoxaparin versus subcutaneous unfractionated heparin
The short follow up period in one of the cohort studies meant no VTE events were seen in either group [25]. The second cohort study examined a much more prolonged period of prophylaxis and event rates were the same between the enoxaparin and UFH groups, 2.7 per 100 patient years [24].
Major bleeding outcomes with VTE prophylaxis in patients with CrCl < 50 ml/min
The details of major bleeding outcomes are reported in Supplementary Table 3.
Enoxaparin versus subcutaneous unfractionated heparin
With the short follow up in one cohort study no major or clinically relevant non major bleeding were reported in either group [25]. In the second cohort study there was no difference in major bleeding between the groups, UFH 17.2 bleeds per 100 patient years vs enoxaparin 16.9 per 100 patient years [24], p = 0.02 [24] for equivalence.
Anticoagulant treatment in patients with AF and CrCl < 50 ml/min
Study characteristics
There were 45 studies that included anticoagulant use in patients with CrCl < 50 ml/min, five RCTs and 40 cohort studies. An overview is provided in Supplementary Table 4. Due to the heterogeneity in the way bleeding and stroke outcomes were reported, alongside variations in renal function and varying doses of anticoagulants, a meta-analysis was not conducted.
Quality
Four of the RCTs were found to be of high quality and of low risk of bias and one RCT showed some concerns relating to it being powered to detect an alternative outcome. Of the 40 cohort studies twelve were deemed of good quality with low bias, nineteen were deemed to be of moderate quality, whilst the remaining nine had severe risk of bias, Supplementary Tables 1 and 2.
Stroke outcomes in studies comparing DOACs to warfarin in patients with AF and CrCl < 50 ml/min
An overview of stroke outcomes is presented in Supplementary Table 5.
Four RCT sub-analyses looking at DOACs versus warfarin included patients with CrCl 30–50 ml/min (25–50 ml/min for apixaban) [26,27,28,29]. They found the risk of stroke or systemic embolism (SSE) was similar between the DOACs and warfarin, Fig. 4. Four cohort studies examining patients with CrCl ≤ 45 ml/min found that rivaroxaban had a reduced risk of SSE compared to warfarin [30,31,32,33]. Doses of rivaroxaban used in these studies were variable and included 20 mg, 15 mg and 10 mg daily. A Japanese study by Koretsune et al. found that apixaban reduced the risk of SSE in patients with a CrCl 15–49 ml/min compared with warfarin [34]. In a haemodialysis population there were four studies comparing DOACs to warfarin [35,36,37,38]. A RCT studied rivaroxaban 10 mg daily in a haemodialysis population and found a reduction in SSE with rivaroxaban but this study was not powered to detect a difference in stroke [35]. The use of apixaban in two retrospective studies of dialysis patients found no significant reduction in stroke compared to those on warfarin, with patients taking apixaban 2.5 mg or 5 mg twice daily [36, 38]. Conversely, in a haemodialysis population, Chan et al. found that rivaroxaban and dabigatran had an increased risk of embolic stroke and arterial embolism compared to warfarin [37]. The remaining five studies in patients with CrCl < 60 ml/min found no difference in stroke between the DOAC and warfarin groups [39,40,41,42,43].
Stroke reported from RCTs in patients with AF and CrCl < 50 ml/min. Figure created using RevMan software [23]
Stroke outcomes from studies comparing oral anticoagulation to no anticoagulation in patients with AF and CrCl < 50 ml/min
Of the 27 studies looking at oral anticoagulation versus no anticoagulation, 23 were based in a dialysis population and the remaining four studies in patients with eGFR < 60 ml/min/1.73 m2, Supplementary Table 5.
Two studies in patients with CrCl < 60 ml/min found a benefit from warfarin compared to no anticoagulation [44, 45]. The third study in patients with eGFR < 30 ml/min/1.73 m2 found stroke rates were higher in those on DOACs or VKAs compared to no anticoagulation [46], whilst a fourth found a reduction in stroke with DOACs but not warfarin compared to no anticoagulation [47]. In a dialysis population, Mavrakanas et al. found no difference in the incidence of stroke when apixaban was compared to no treatment in a propensity matched dialysis cohort, HR1.24 (0.69–2.23) [48]. From a national Taiwan database See et al. also found no benefit of warfarin or DOACs in reducing the risk of ischaemic stroke in those on dialysis [49], whilst a large retrospective study by Agarwal et al. found that warfarin increased the risk of ischaemic stroke compared to no anticoagulation [50]. Of the remaining dialysis studies, five found benefit from warfarin in reducing the risk of ischaemic stroke [51,52,53,54,55], eleven studies found no benefit of warfarin in reducing the risk of stroke [5, 56,57,58,59,60,61,62,63,64,65] and four studies found warfarin led to an increased risk of stroke [66,67,68,69], Supplementary Table 5.
Major bleeding outcomes from studies comparing DOACs to warfarin in patients with AF and CrCl < 50 ml/min
An overview of major bleeding outcomes is presented in Supplementary Table 6.
From the RCTs Hohnloser et al. found that apixaban was associated with a reduced risk of major bleeding compared to warfarin in patients with a CrCl < 50 ml/min [29], Fig. 5. This was also seen with edoxaban [28], but not with rivaroxaban and dabigatran where bleeding was similar to warfarin [27]. Edoxaban was also found to have significant reduction in the risk of intracranial haemorrhage, HR 0.46 (95% CI 0.26–0.82) p = 0.009, in patients with CrCl 30–50 ml/min compared to warfarin [26, 28]. Similar findings of intracranial haemorrhage reduction were seen with dabigatran in CrCl < 50 ml/min for both 150 mg and 110 mg, respectively, HR 0.31 (95% CI 0.14–0.66) and 0.40 (95% CI 0.20–0.80) [27].
Major bleeding from RCTs in patients with AF and CrCl < 50 ml/min. Figure created using RevMan software [23]
De Vriese et al. found a significant reduction in major bleeding with rivaroxaban compared to warfarin in haemodialysis patients, although the study was small [35]. Similar findings were seen by Siontis and Wetmore who both found a reduction in major bleeding with apixaban compared to warfarin in dialysis patients, HR 0.72 (95% CI 0.59–0.87) p < 0.001 [36] and HR 0.67 (95% CI 0.55–0.81) label dose, respectively [38]. Conversely, an observational study by Chan et al. in haemodialysis patients found that compared to warfarin rivaroxaban and dabigatran had higher rates of major bleeding including higher rates of death from bleeding [37]. Despite being on haemodialysis, 15.3% patients on dabigatran and 32.1% on rivaroxaban were still on non-renal adjusted doses [37], Supplementary Table 6.
The remaining ten observational studies were in patients with eGFR < 60 ml/min/1.73 m2. Six of these studies found DOACs had a lower risk of major bleeding compared to warfarin [30, 31, 34, 36, 39, 40], three found no difference [33, 42, 43], whilst a study by Shin et al. showed that rivaroxaban and dabigatran compared to warfarin had a higher risk of major bleeding [41], Supplementary Table 6.
Major bleeding outcomes from studies comparing OAC to no anticoagulation in patients with AF and CrCl < 50 ml/min
Of the 27 studies comparing oral anticoagulation versus no anticoagulation, 23 were based in a dialysis population and the remaining four studies in patients with eGFR < 60 ml/min/1.73 m2, Supplementary Table 6.
From the four studies in patients with eGFR < 60 ml/min/1.73 m2 there was less major bleeding in patients not taking anticoagulants, and the difference in major bleeding was more evident as renal function declined [44,45,46,47], supplementary table 6. Fourteen studies in dialysis patients found an increased risk of bleeding events with anticoagulation as compared to none [48, 50, 53, 54, 56,57,58,59,60,61,62, 65, 67, 69]. However, there were nine studies in dialysis patients that found no difference in major bleeding between those anticoagulated and not [5, 49, 51, 52, 55, 63, 64, 66, 68].
Discussion
This is the first systematic review of VTE prophylaxis in patients with renal impairment that focuses on both thrombotic and bleeding outcomes for medical patients and the most up-to-date review of bleeding and thrombotic outcomes in the treatment of VTE and AF. This review includes the available evidence for anticoagulants across the various stages of CKD, Table 2, which highlights a distinct lack of studies that describe both thrombotic and bleeding outcomes in patients with a CrCl < 30 ml/min. Inclusion of multiple indications for anticoagulant use makes this review a holistic resource for nephrology professionals.
The first issue on which the review is focused regards the use of DOACs for patients with VTE and CrCl <50 mL/min. Four RCTs compared DOACs versus warfarin in patients with CrCl 30–50 ml/min with no difference in recurrent VTE events. Dabigatran had a trend towards increased efficacy but due to its high renal excretion it would not be the first choice in a CKD population. There was no significant difference in major bleeding between the DOACs and warfarin although apixaban and rivaroxaban had lower rates of major bleeding making them a suitable treatment option for VTE treatment in patients with CrCl ≥ 30 ml/min.
Overall findings from a recent systematic review showed DOACs had a reduced major bleeding risk compared to VKAs in CKD patients (this included patients with mild renal impairment) [70]. Cheung et al. compared DOACs with warfarin for VTE treatment in dialysis patients [71] and suggested apixaban as an option without a loading dose and a reduced maintenance dose. However, this review included studies reporting combined outcomes for patients with indications not limited to VTE, with the majority having AF [72,73,74,75,76,77], and studies failed to report VTE risk factors (Supplementary Table 7). Heterogeneity of apixaban dosing for VTE is also seen, particularly in terms of loading doses. Based on the more recent observational study from Wetmore et al. [22], where the majority of dialysis patients are believed to be taking the Food and Drug Administration licensed apixaban dose of 10 mg twice daily for a week followed by 5 mg twice daily (personal correspondence James Wetmore), this would support the use of higher doses in haemodialysis than that proposed by Cheung et al. [71]. The reduced risk of recurrent VTE and major bleeding shown by Wetmore and colleagues may in part be explained by the problems in achieving and maintaining INR target ranges with warfarin in a dialysis population [12].
An observational study comparing rivaroxaban to standard anticoagulation, [78], found that major bleeding was similar between rivaroxaban, warfarin and LMWH/fondaparinux. In terms of recurrent VTE, the findings were similar for rivaroxaban and warfarin with higher rates for those on LMWH/fondaparinux. Baseline characteristics were not available for CKD patients, thus selection bias is possible.
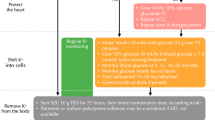
Anti-Xa agents are licensed for treating VTE in patients with CrCl 15–29 ml/min, based on limited clinical outcome data. Venous Thromboembolism in Renally Impaired Patients and Direct Oral Anticoagulants (VERDICT), is currently investigating reduced doses of apixaban and rivaroxaban for the treatment of VTE in patients with CrCl 15–50 ml/min compared to conventional therapy with LMWH and VKAs. At present there is still limited information about the use of DOACs for VTE treatment in those with CrCl < 15 ml/min but apixaban may be an option for those on dialysis, although the optimal dosing regimen is still unclear. The authors of this review present their suggestions for the use of DOACs in acute VTE based on renal function in Fig. 6.
The second issue on which the review is focused regards the use of LMWH in the treatment of VTE in patients with CrCl<50 mL/min. Similar to the REMOTEV study [78], Kooiman et al. found LMWH was less effective in preventing recurrent VTE than warfarin in patients with cancer and CrCl 30–49 ml/min [20]. This study highlighted an increase in both major bleeding and fatal bleeding with LMWH in patients with a CrCl < 30 ml/min. The manufacturers of the LMWHs advise caution with their use in these populations due to potential accumulation [79,80,81].
No studies examining outcomes of therapeutic LMWH use in CKD met inclusion for this review. Pon et al. undertook a review of haemodialysis patients taking intravenous UFH or therapeutic subcutaneous (SC) enoxaparin finding that there was no difference in major bleeding or thromboembolic events [82]. Similarly, Thorevska 2003 found no difference in major bleeding between intravenous UFH and twice-daily enoxaparin in patients with CrCl < 20 ml/min [83]. A retrospective review of therapeutic UFH versus enoxaparin in patients with eGFR < 60 ml/min found UFH was associated with an increase in major bleeding, HR 4.79 [95% CI, 1.85–12.36] [84].
The Comparison of Acute Treatments in Cancer Haemostasis (CATCH) study which compared tinzaparin with warfarin in cancer-associated thrombosis (including those with an eGFR < 60 ml/min/1.73 m2 [85] found no difference in recurrent VTE or major bleeding. The Innohep® in Renal Insufficiency Study (IRIS) designed to look at bleeding and safety outcomes of tinzaparin vs therapeutic UFH SC in patients with VTE and CrCl < 30 ml/min was terminated early due to excess mortality within the tinzaparin group although r review has deemed this not related to bleeding or thrombotic events. A sub-study of the IRIS trial looking at accumulation of tinzaparin in 21 patients with CrCl < 30 ml/min (dialysis excluded) found no accumulation over 8 days when dosed at 175units/kg SC daily [86]. A further study also demonstrated no tinzaparin accumulation in patients with CrCl 20-34 ml/min for up to 30 days [87].
A study of therapeutic dalteparin compared to intravenous UFH in patients with an eGFR < 60 ml/min found a significant reduction in major bleeding in the dalteparin arm, even in those with eGFR < 30 ml/min [88]. Schmid et al. however found significant dalteparin accumulation in those with CrCl < 30 ml/min which led them to recommend anti-Xa monitoring in this population [89].
When using therapeutic doses of LMWH in patients with severe renal impairment, CrCl < 30 ml/min, anti-Xa level monitoring should be considered [79,80,81] with dose reductions as appropriate [90, 91]. The European Society of Cardiology (ESC) recommends that if LMWH is prescribed in patients with CrCl 15 − 30 mL/min, an adapted dosing scheme should be used [92].
The third issue regards VTE prophylaxis in non-surgical patients with CrCl <50 mL/min. There were limited studies in this group. The two included studies both looked at enoxaparin versus UFH prophylaxis in haemodialysis patients. Green et al. showed short duration of prophylaxis and noted no thromboembolic or bleeding events in either group [25]. The much larger study by Chan et al. showed there was no difference in major bleeding rates between enoxaparin and UFH [24]. However, both studies used the FDA licensed dose (30 mg –daily) which differs from European dosing (20 mg or 40 mg). Chan et al. also used off-license dosing of up to 60 mg SC daily; however,indications were unclear, and 28% of patients were defined as obese [24]. Mahe examined accumulation of LWMH prophylaxis in elderly patients with CrCl 20–50 ml/min and lower bodyweight (mean 52 kg) [93]. After eight days, they found accumulation of enoxaparin but not tinzaparin [93].
A systematic review investigating anti-Xa monitoring of LMWHs for VTE prophylaxis in CKD patients concluded that prophylactic doses of dalteparin and tinzaparin did not accumulate, but enoxaparin did in those with CrCl < 30 ml/min, and thus a dose reduction would be required [94].
The fourth issue regards anticoagulant use in atrial fibrillation in patients on dialysis. The benefits of anticoagulation in reducing the risk of SSE in dialysis patients with AF are uncertain. The majority of studies found that warfarin or DOACs had either a similar risk of stroke or a higher risk compared to no anticoagulation. The heterogeneity in which stroke was defined in these studies and the difference in baseline population characteristics makes it difficult to compare these studies. In terms of safety outcomes, anticoagulation had a similar or elevated risk of major bleeding versus no anticoagulation. An increase in intracranial haemorrhage with the use of anticoagulation was a notable finding. Some studies reporting gastrointestinal (GI) bleeding found similar rates between those taking and not taking anticoagulation. This may be related to the pre-existing high rates of gastrointestinal bleeding [51, 52, 59, 67] that are observed in a dialysis population, independent of anticoagulant use [95, 96], which is mainly related to increased angiodysplasia [97].
For patients with AF and end-stage renal disease clinical equipoise exists where the risk of bleeding with any anticoagulant may outweigh any potential benefits [98,99,100,101]. To investigate whether anticoagulation is appropriate for dialysis patients with AF, the ongoing AVKDIAL, DANWARD, SACK and SAFE-D studies may provide some answers [102,103,104,105]. AVKDIAL and DANWARD are both open-label RCTs looking at vitamin K antagonist versus no anticoagulation on the risk of stroke and major bleeding [102, 104]. Whilst the Swedish SACK study is looking at apixaban 2.5 mg twice daily versus no treatment in patients with eGFR < 15 ml/min/1.73 m2, including dialysis, on stroke and bleeding outcomes [105]. The SAFE-D pilot trial aims to assess the feasibility of setting up a larger RCT in AF patients on dialysis [103]. This trial is currently randomising patients to one of three arms: warfarin, apixaban 2.5 mg bd or no anticoagulation.
We noted no advantage of DOACs in reducing the risk of SSE as compared to warfarin, with one study showing an increased risk of stroke with dabigatran and rivaroxaban [37]. In terms of major bleeding, Siontis et al. [36] and Wetmore et al. [38] showed a significant reduction in major bleeding with apixaban compared to warfarin as did De Vriese et al. [35] with rivaroxaban 10 mg daily. Conversely Chan et al. showed a significant increase in major bleeding, including fatal bleeding, with dabigatran and rivaroxaban 20 mg or 15 mg daily compared to warfarin [37]. US observational studies looking at DOACs versus warfarin in dialysis included multiple indications making it difficult to extract the patient outcomes (Supplementary Table 7).
Unfortunately, the RENAL-AF study, an open-label RCT looking at apixaban versus warfarin for AF in haemodialysis, failed to recruit sufficient participants [106]. although the preliminary findings suggested no difference in terms of SSE and major bleeding.
The AXADIA study (Compare Apixaban and Vitamin K antagonists in patients with atrial fibrillation and End- stage kidney disease), is an open-label German clinical trial investigating apixaban 2.5 mg bd versus phenprocoumarin in patients on dialysis [107]. The primary outcome being safety in terms of risk of bleeding events and secondary outcome looking at efficacy in preventing thromboembolic events.
The fifth issue regards anticoagulant use in atrial fibrillation in patients with CrCl <50 ml/min. From the RCTs in people with AF and a CrCl 25–50 ml/min, there was no significant difference in stroke between the DOACs and warfarin, except for dabigatran 150 mg which had a reduced risk of stroke and systemic embolism, HR 0.56 (0.37–0.85) [27]. In terms of primary safety outcomes from the RCT sub-analyses apixaban and edoxaban were found to have a significantly reduced risk of major bleeding compared to warfarin [28, 29]. This reduction in major bleeding was not seen with dabigatran and rivaroxaban and this may in part relate to their increased risk of GI bleeding presented in the RE-LY and ROCKET- AF trials [108, 109]. However, when looking at intracranial haemorrhage within the CKD sub-analyses, both dabigatran and edoxaban reported a reduced risk of intracranial haemorrhage compared to warfarin [27, 28]. Intracranial haemorrhage was not presented in the CKD sub-analyses of apixaban but the overall ARISTOTLE trial found reduced likelihood compared to warfarin [110]. These findings would suggest that in terms of their safety profile, apixaban and edoxaban may be preferable for AF anticoagulation in CrCl 25–50 ml/min given their non-inferior efficacy to warfarin. It should be noted that due to dabigatran having the highest degree of renal excretion (around 85%), with no license in Europe for those with a CrCl < 30 ml/min [111] its use is likely to be limited in patients with CKD.
The sixth point regards anticoagulant use in atrial fibrillation in patients with a CrCl <30 ml/min not on dialysis. There were fourteen retrospective cohort studies that included patients with AF and a CrCl < 30 ml/min. Two studies found that warfarin reduced the risk of stroke versus no anticoagulation, one study found no difference and a fourth study identified an increased risk of stroke with warfarin as compared to no anticoagulation. Three studies showed that DOACs reduced the risk of stroke compared to warfarin with seven studies finding no difference in stroke between DOACs and warfarin. Unfortunately, there was significant heterogeneity between studies in terms of DOAC dosing (if reported) and how the results were presented in relation to renal function, making it difficult to draw conclusions.
In terms of major bleeding in CrCl < 30 ml/min, the majority of studies found lower bleeding with DOACS versus warfarin with the remainder finding similar rates of bleeding. A recent study by Sy et al. found that for AF in patients with eGFR < 60 ml/min/1.73 m2 including dialysis, DOACs had a lower risk of major bleeding compared to warfarin [112] which would support the safety profile of DOACs compared to warfarin in this population.
In a population with a CrCl < 30 ml/min not on dialysis, anticoagulation should be considered on an individual patient basis with clinical assessment of the risks and benefits. From the limited available studies, DOACs may have a preferable safety profile over warfarin for patients with AF in this group. DOACs are not licensed in patients with a CrCl < 15 ml/min and more data is required before the safety and efficacy of DOACs in this group of patients are known. The authors of this review have presented their thoughts on the use of DOACs in patients with AF and varying degrees of renal impairment in Fig. 7, which are not dissimilar to a recent position statement published by the three Italian scientific societies [113].
One of the major limitations to this review are the small number of RCTs identified. Most studies are retrospective cohort studies with significant heterogeneity making performance of meta-analysis difficult. Differences existed in the definitions of major bleeding and stroke, renal function reporting (range and estimating equation), and anticoagulant doses used, making it difficult to draw conclusions from the data.
Conclusions
In patients with VTE or AF and a CrCl ≥ 30 ml/min, DOACs may be preferable to warfarin with lower major bleeding and similar efficacy. Apixaban may be a safer and more effective option for the treatment of VTE in dialysis patients compared to warfarin, although this systematic review highlights the need for further studies in patients taking anticoagulation for VTE treatment or VTE prophylaxis in patients with advanced CKD (CrCl < 30 ml/min) to identify the safest and most effective options. The VERDICT trial is currently ongoing and may support future prescribing practice for VTE in more advanced CKD. For AF there is limited information for patients with a CrCl < 30 ml/min in terms of the risks and benefits of anticoagulation in reducing the risk of stroke. Until further data is available individualised decisions made with the patient and clinician are essential in this population, especially for those on dialysis. The ongoing AVKDIAL, AXADIA, DANWARD, SACK and SAFE-D trials in dialysis patients may help guide management of AF in the future.
Data availability
The data underlying this article are available in the article and in its online supplementary material.
References
Wattanakit K, Cushman M, Stehman-Breen C, Heckbert SR, Folsom AR (2008) Chronic kidney disease increases risk for venous thromboembolism. J Am Soc Nephrol 19(1):135–140
Tveit DP, Hypolite IO, Hshieh P, Cruess D, Agodoa LY, Welch PG et al (2002) Chronic dialysis patients have high risk for pulmonary embolism. Am J Kidney Dis 39(5):1011–1017
Go AS, Hylek EM, Phillips KA, Chang Y, Henault LE, Selby JV et al (2001) Prevalence of diagnosed atrial fibrillation in adults: national implications for rhythm management and stroke prevention: the AnTicoagulation and Risk Factors in Atrial Fibrillation (ATRIA) Study. JAMA 285(18):2370–2375
Tanaka A, Inaguma D, Shinjo H, Murata M, Takeda A (2016) Presence of atrial fibrillation at the time of dialysis initiation is associated with mortality and cardiovascular events. Nephron 132(2):86–92
Mitsuma W, Matsubara T, Hatada K, Imai S, Saito N, Shimada H et al (2016) Clinical characteristics of hemodialysis patients with atrial fibrillation: the RAKUEN (Registry of atrial fibrillation in chronic kidney disease under hemodialysis from Niigata) study. J Cardiol 68(2):148–155
Zimmerman D, Sood MM, Rigatto C, Holden RM, Hiremath S, Clase CM (2012) Systematic review and meta-analysis of incidence, prevalence and outcomes of atrial fibrillation in patients on dialysis. Nephrol Dial Transplant 27(10):3816–3822
Tsagalis G, Bakirtzi N, Manios E, Chouliaras I, Papagiannidou P, Stamellou E et al (2011) Atrial fibrillation in chronic hemodialysis patients: prevalence, types, predictors, and treatment practices in Greece. Artif Organs 35(10):916–922
To AC, Yehia M, Collins JF (2007) Atrial fibrillation in haemodialysis patients: do the guidelines for anticoagulation apply? Nephrology (Carlton) 12(5):441–447
Wizemann V, Tong L, Satayathum S, Disney A, Akiba T, Fissell RB et al (2010) Atrial fibrillation in hemodialysis patients: clinical features and associations with anticoagulant therapy. Kidney Int 77(12):1098–1106
Iseki K, Kinjo K, Kimura Y, Osawa A, Fukiyama K (1993) Evidence for high risk of cerebral hemorrhage in chronic dialysis patients. Kidney Int 44(5):1086–1090
Chan KE, Giugliano RP, Patel MR, Abramson S, Jardine M, Zhao S et al (2016) Nonvitamin K anticoagulant agents in patients with advanced chronic kidney disease or on dialysis with AF. J Am Coll Cardiol 67(24):2888–2899
Quinn LM, Richardson R, Cameron KJ, Battistella M (2015) Evaluating time in therapeutic range for hemodialysis patients taking warfarin. Clin Nephrol 83(2):80–85
Brandenburg VM, Kramann R, Rothe H, Kaesler N, Korbiel J, Specht P et al (2017) Calcific uraemic arteriolopathy (calciphylaxis): data from a large nationwide registry. Nephrol Dial Transplant 32(1):126–132
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M et al (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919
Bauersachs RM, Lensing AW, Prins MH, Kubitza D, Pap ÁF, Decousus H et al (2014) Rivaroxaban versus enoxaparin/vitamin K antagonist therapy in patients with venous thromboembolism and renal impairment. Thromb J 12:25
Büller HR, Décousus H, Grosso MA, Mercuri M, Middeldorp S, Prins MH et al (2013) Edoxaban versus warfarin for the treatment of symptomatic venous thromboembolism. N Engl J Med 369(15):1406–1415
Agnelli G, Buller HR, Cohen A, Curto M, Gallus AS, Johnson M et al (2013) Oral Apixaban for the treatment of acute venous thromboembolism. N Engl J Med 369(9):799–808
Goldhaber SZ, Schulman S, Eriksson H, Feuring M, Fraessdorf M, Kreuzer J et al (2017) Dabigatran versus warfarin for acute venous thromboembolism in elderly or impaired renal function patients: pooled analysis of RE-COVER and RE-COVER II. Thromb Haemost 117(11):2045–2052
Kooiman J, den Exter PL, Cannegieter SC, le Cessie S, del Toro J, Sahuquillo JC et al (2013) Impact of chronic kidney disease on the risk of clinical outcomes in patients with cancer-associated venous thromboembolism during anticoagulant treatment. J Thromb Haemost 11(11):1968–1976
Levey AS, Coresh J, Greene T, Stevens LA, Zhang Y, Hendriksen S, Kusek JW, Van Lente F (2006) Using standardized serum creatinine values in the modification of diet in renal disease study equation for estimating glomerular filtration rate. Ann Internal Med 145(4):247–254
Wetmore JB, Herzog CA, Yan H, Reyes JL, Weinhandl ED, Roetker NS (2022) Apixaban versus warfarin for treatment of venous thromboembolism in patients receiving long-term dialysis. Clin J Am Soc Nephrol 17(5):693–702
Collaboration TC (2020) Review Manager (RevMan) [Computer program]. Version 5.4, 2020. 5.4 ed: The Cochrane Collaboration
Chan KE, Thadhani RI, Maddux FW (2013) No difference in bleeding risk between subcutaneous enoxaparin and heparin for thromboprophylaxis in end-stage renal disease. Kidney Int 84(3):555–561
Green MS, Tellor KB, Buckallew AR (2017) Safety and efficacy of enoxaparin compared with unfractionated heparin for venous thromboembolism prophylaxis in hemodialysis patients. Hosp Pharm 52(9):623–627
Fox KA, Piccini JP, Wojdyla D, Becker RC, Halperin JL, Nessel CC et al (2011) Prevention of stroke and systemic embolism with rivaroxaban compared with warfarin in patients with non-valvular atrial fibrillation and moderate renal impairment. Eur Heart J 32(19):2387–2394
Hijazi Z, Hohnloser SH, Oldgren J, Andersson U, Connolly SJ, Eikelboom JW et al (2014) Efficacy and safety of dabigatran compared with warfarin in relation to baseline renal function in patients with atrial fibrillation. Circulation 129(9):961–970
Bohula EA, Giugliano RP, Ruff CT, Kuder JF, Murphy SA, Antman EM et al (2016) Impact of renal function on outcomes with edoxaban in the ENGAGE AF-TIMI 48 trial. Circulation 134(1):24–36
Hohnloser SH, Hijazi Z, Thomas L, Alexander JH, Amerena J, Hanna M et al (2012) Efficacy of apixaban when compared with warfarin in relation to renal function in patients with atrial fibrillation: insights from the ARISTOTLE trial. Eur Heart J 33(22):2821–2830
Di Lullo L, Tripepi G, Ronco C, De Pascalis A, Barbera V, Granata A et al (2018) Safety and effectiveness of rivaroxaban and warfarin in moderate-to-advanced CKD: real world data. J Nephrol 31(5):751–756
Coleman CI, Kreutz R, Sood NA, Bunz TJ, Eriksson D, Meinecke A-K et al (2019) Rivaroxaban versus warfarin in patients with nonvalvular atrial fibrillation and severe kidney disease or undergoing hemodialysis. Am J Med 132(9):1078–1083
Weir MR, Ashton V, Moore KT, Shrivastava S, Peterson ED, Ammann EM (2020) Rivaroxaban versus warfarin in patients with nonvalvular atrial fibrillation and stage IV–V chronic kidney disease. Am Heart J 223:3–11
Lin YC, Chen BL, Shih CM, Lin FY, Chen CW, Hsu CY et al (2021) Effectiveness and safety of rivaroxaban versus warfarin in Taiwanese patients with end-stage renal disease and nonvalvular atrial fibrillation: a real-world nationwide cohort study. PLoS ONE 16(4):e0249940
Koretsune Y, Hoshino H, Matsuo Y, Ibuki T, Morimoto T (2022) Comparative safety and effectiveness of Apixaban vs warfarin in oral anticoagulant-naive Japanese patients with non-valvular atrial fibrillation—a retrospective chart review study. Circ J 86(2):213–221
De Vriese AS, Caluwé R, Van Der Meersch H, De Boeck K, De Bacquer D (2021) Safety and efficacy of Vitamin K antagonists versus rivaroxaban in hemodialysis patients with atrial fibrillation: a multicenter randomized controlled trial. J Am Soc Nephrol 32(6):1474–1483
Siontis KC, Zhang X, Eckard A, Bhave N, Schaubel DE, He K et al (2018) Outcomes associated with Apixaban use in patients with end-stage kidney disease and atrial fibrillation in the United States. Circulation 138(15):1519–1529
Chan KE, Edelman ER, Wenger JB, Thadhani RI, Maddux FW (2015) Dabigatran and rivaroxaban use in atrial fibrillation patients on hemodialysis. Circulation 131(11):972–979
Wetmore JB, Weinhandl ED, Yan H, Reyes JL, Herzog CA, Roetker NS (2022) Apixaban dosing patterns versus warfarin in patients with nonvalvular atrial fibrillation receiving dialysis: a retrospective cohort study. Am J Kidney Dis. https://doi.org/10.1053/j.ajkd.2022.03.007
Wetmore JB, Roetker NS, Yan H, Reyes JL, Herzog CA (2020) Direct-acting oral anticoagulants versus warfarin in medicare patients with chronic kidney disease and atrial fibrillation. Stroke 51(8):2364–2373
Laugesen EK, Staerk L, Carlson N, Kamper A-L, Olesen JB, Torp-Pederson C, et al (2019) Non-vitamin K antagonist oral anticoagulants vs. vitamin-K antagonists in patients with atrial fibrillation and chronic kidney disease: a nationwide cohort study. Thrombosis Journal. E.K. Laugesen, Department of Cardiology, Copenhagen University Hospital Herlev and Gentofte, Kildegaardsvej 28, Hellerup 2900, Denmark. E-mail: emma.laugesen@hotmail.com: BioMed Central Ltd. (E-mail: info@biomedcentral.com). pp 21
Shin J-I, Secora A, Alexander GC, Inker LA, Coresh J, Chang AR et al (2018) Risks and benefits of direct oral anticoagulants across the spectrum of GFR among incident and prevalent patients with atrial fibrillation. Clin J Am Soc Nephrol 13(8):1144–1152
Heleniak Z, Papuga-Szela E, Krzysztof P, Anetta U (2020) Efficacy and safety of non-vitamin K antagonist oral anticoagulants in patients with atrial fibrillation and chronic kidney disease Stage G4: a single-center experience. J Cardiovasc Pharmacol 76(6):671–677
Vaitsiakhovich T, Coleman CI, Kleinjung F, Vardar B, Schaefer B (2022) Worsening of kidney function in patients with atrial fibrillation and chronic kidney disease: evidence from the real-world CALLIPER study. Curr Med Res Opin 38(6):937–945
Jun M, James MT, Ma Z, Zhang J, Tonelli M, McAlister FA et al (2017) Warfarin initiation, atrial fibrillation, and kidney function: comparative effectiveness and safety of warfarin in older adults with newly diagnosed atrial fibrillation. Am J Kidney Dis 69(6):734–743
Lai HM, Aronow WS, Kalen P, Adapa S, Patel K, Goel A et al (2009) Incidence of thromboembolic stroke and of major bleeding in patients with atrial fibrillation and chronic kidney disease treated with and without warfarin. Int J Nephrol Renovasc Dis 2:33–37
Chang SH, Wu CV, Yeh YH, Kuo CF, Chen YL, Wen MS et al (2019) Efficacy and safety of oral anticoagulants in patients with atrial fibrillation and Stages 4 or 5 chronic kidney disease. Am J Med 132(11):1335–43.e6
Chantrarat T, Krittayaphong R (2021) Oral anticoagulation and cardiovascular outcomes in patients with atrial fibrillation and chronic kidney disease in Asian Population, Data from the COOL-AF Thailand registry. Int J Cardiol 323:90–99
Mavrakanas TA, Garlo K, Charytan DM (2020) Apixaban vs no anticoagulation in patients undergoing long-term dialysis with incident atrial fibrillation. Clin J Am Soc Nephrol 15(8):1146–1154
See LC, Lee HF, Chao TF, Li PR, Liu JR, Wu LS et al (2020) Effectiveness and safety of direct oral anticoagulants in an Asian population with atrial fibrillation undergoing dialysis: a population-based cohort study and meta-analysis. Cardiovasc Drugs Therapy 35(5):975–986
Agarwal MA, Potukuchi PK, Sumida K, Naseer A, Molnar MZ, George LK et al (2020) Clinical outcomes of warfarin initiation in advanced chronic kidney disease patients with incident atrial fibrillation. JACC Clin Electrophysiol 6(13):1658–1668
Kai B, Bogorad Y, Nguyen L-AN, Yang S-J, Chen W, Spencer HT et al (2017) Warfarin use and the risk of mortality, stroke, and bleeding in hemodialysis patients with atrial fibrillation. Heart Rhythm 14(5):645–651
Shen JI, Montez-Rath ME, Lenihan CR, Turakhia MP, Chang TI, Winkelmayer WC (2015) Outcomes after warfarin initiation in a cohort of hemodialysis patients with newly diagnosed atrial fibrillation. Am J Kidney Dis 66(4):677–688
Genovesi S, Rebora P, Gallieni M, Stella A, Badiali F, Conte F et al (2017) Effect of oral anticoagulant therapy on mortality in end-stage renal disease patients with atrial fibrillation: a prospective study. J Nephrol 30(4):573–581
Olesen JB, Lip GYH, Kamper A-L, Hommel K, Kober L, Lane DA et al (2012) Stroke and bleeding in atrial fibrillation with chronic kidney disease. N Engl J Med 367(7):625–635
Chan P-H, Huang D, Yip P-S, Hai J, Tse H-F, Chan T-M et al (2016) Ischaemic stroke in patients with atrial fibrillation with chronic kidney disease undergoing peritoneal dialysis. Europace 18(5):665–671
Tan J, Bae S, Segal JB, Zhu J, Alexander GC, Segev DL et al (2019) Warfarin use and the risk of stroke, bleeding, and mortality in older adults on dialysis with incident atrial fibrillation. Nephrology (Carlton) 24(2):234–244
Shah M, Avgil Tsadok M, Jackevicius CA, Essebag V, Eisenberg MJ, Rahme E et al (2014) Warfarin use and the risk for stroke and bleeding in patients with atrial fibrillation undergoing dialysis. Circulation 129(11):1196–1203
Genovesi S, Rossi E, Gallieni M, Stella A, Badiali F, Conte F et al (2015) Warfarin use, mortality, bleeding and stroke in haemodialysis patients with atrial fibrillation. Nephrol Dialysis Transplant 30(3):491–498
Winkelmayer WC, Liu J, Setoguchi S, Choudhry NK (2011) Effectiveness and safety of warfarin initiation in older hemodialysis patients with incident atrial fibrillation. Clin J Am Soc Nephrol 6(11):2662–2668
Lohit G, Charity C, David EH (2016) Atrial fibrillation and chronic kidney disease requiring hemodialysis—Does warfarin therapy improve the risks of this lethal combination? Int J Cardiol 222:47–50
Yoon C-Y, Noh J, Jhee JH, Chang TI, Kang EW, Kee YK et al (2017) Warfarin use in patients with atrial fibrillation undergoing hemodialysis: a nationwide population-based study. Stroke 48(9):2472–2479
Yodogawa K, Mii A, Fukui M, Iwasaki YK, Hayashi M, Kaneko T et al (2016) Warfarin use and incidence of stroke in Japanese hemodialysis patients with atrial fibrillation. Heart Vessels 31(10):1676–1680
Sy J, Wenziger C, Marroquin M, Kalantar-Zadeh K, Kovesdy C, Streja E (2022) Warfarin use, stroke, and bleeding risk among pre-existing atrial fibrillation US veterans transitioning to dialysis. Nephron 146(6):360–368
Akbar MR, Febrianora M, Iqbal M (2022) Warfarin usage in patients with atrial fibrillation undergoing hemodialysis in indonesian population. Curr Prob Cardiol. https://doi.org/10.1016/j.cpcardiol.2022.101104 (no pagination)
Wang TKM, Sathananthan J, Marshall M, Kerr A, Hood C (2016) Relationships between anticoagulation, risk scores and adverse outcomes in dialysis patients with atrial fibrillation. Heart Lung Circ 25(3):243–249
Chan KE, Lazarus JM, Thadhani R, Hakim RM (2009) Warfarin use associates with increased risk for stroke in hemodialysis patients with atrial fibrillation. J Am Soc Nephrol 20(10):2223–2233
Phan D, Yang S-J, Shen AYJ, Lee M-S (2019) Effect of warfarin on ischemic stroke, bleeding, and mortality in patients with atrial fibrillation receiving peritoneal dialysis. Am J Cardiovasc Drugs 19(5):509–515
Wakasugi M, Kazama JJ, Tokumoto A, Suzuki K, Kageyama S, Ohya K et al (2014) Association between warfarin use and incidence of ischemic stroke in Japanese hemodialysis patients with chronic sustained atrial fibrillation: a prospective cohort study. Clin Exp Nephrol 18(4):662–669
Konigsbrugge O, Meisel H, Beyer A, Schmaldienst S, Klauser-Braun R, Lorenz M et al (2021) Anticoagulation use and the risk of stroke and major bleeding in patients on hemodialysis: from the VIVALDI, a population-based prospective cohort study. J Thromb Haemost 19(12):2984–2996
Alhousani M, Malik SU, Abu-Hashyeh A, Poznanski NJ, Al-Hasan S, Roth DF et al (2021) Using oral anticoagulants among chronic kidney disease patients to prevent recurrent venous thromboembolism: a systematic review and meta-analysis. Thromb Res 198:103–114
Cheung CYS, Parikh J, Farrell A, Lefebvre M, Summa-Sorgini C, Battistella M (2021) Direct oral anticoagulant use in chronic kidney disease and dialysis patients with venous thromboembolism: a systematic review of thrombosis and bleeding outcomes. Ann Pharmacother 55(6):711–722
Reed D, Palkimas S, Hockman R, Abraham S, Le T, Maitland H (2018) Safety and effectiveness of apixaban compared to warfarin in dialysis patients. Res Pract Thromb Haemost 2(2):291–298
Schafer JH, Casey AL, Dupre KA, Staubes BA (2018) Safety and efficacy of apixaban versus warfarin in patients with advanced chronic kidney disease. Ann Pharmacother 52(11):1078–1084
Stanton BE, Barasch NS, Tellor KB (2017) Comparison of the safety and effectiveness of apixaban versus warfarin in patients with severe renal impairment. Pharmacotherapy 37(4):412–419
Herndon K, Guidry TJ, Wassell K, Elliott W (2020) Characterizing the safety profile of apixaban versus warfarin in moderate to severe chronic kidney disease at a veterans affairs hospital. Ann Pharmacother 54(6):554–560
Hanni C, Petrovitch E, Ali M, Gibson W, Giuliano C, Holzhausen J et al (2020) Outcomes associated with apixaban vs warfarin in patients with renal dysfunction. Blood Adv 4(11):2366–2371
Sarratt SC, Nesbit R, Moye R (2017) Safety outcomes of apixaban compared with warfarin in patients with end-stage renal disease. Ann Pharmacother 51(6):445–450
Gaertner S, Cordeanu EM, Nouri S, Faller AM, Frantz AS, Mirea C et al (2017) Rivaroxaban versus standard anticoagulation for symptomatic venous thromboembolism (REMOTEV observational study): analysis of 6-month outcomes. Int J Cardiol 226:103–109
Prescribing information for Innohep injections [updated 02/12/2020]. https://www.medicines.org.uk/emc/product/3632/smpc
Prescribing information for Fragmin injection [updated 08/10/2020]. https://www.medicines.org.uk/emc/product/4245/smpc
Prescribing information for Clexane pre-filled syringes [updated 26/05/2020]. https://www.medicines.org.uk/emc/product/4499/smpc
Pon TK, Dager WE, Roberts AJ, White RH (2014) Subcutaneous enoxaparin for therapeutic anticoagulation in hemodialysis patients. Thrombosis Research. T.K. Pon, Clinical Pharmacy, University of California, 2315 Stockton Blvd, Sacramento, CA 95815, United States. E-mail: tiffany.pon@ucsf.edu: Elsevier Ltd; pp 1023–1028
Thorevska N, Amoateng-Adjepong Y, Sabahi R, Schiopescu I, Salloum A, Muralidharan V et al (2004) Anticoagulation in hospitalized patients with renal insufficiency: a comparison of bleeding rates with unfractionated heparin vs enoxaparin. Chest 125(3):856–863
Saheb Sharif-Askari F, Syed Sulaiman SA, Saheb Sharif-Askari N, Alsayed Hussain A, Railey MJ (2014) Adverse outcomes of anticoagulant use among hospitalized patients with chronic kidney disease: a comparison of the rates of major bleeding events between unfractionated heparin and enoxaparin. PLoS One 9(9):e106517
Bauersachs R, Lee AYY, Kamphuisen PW, Meyer G, Janas MS, Jarner MF et al (2018) Renal impairment, recurrent venous thromboembolism and bleeding in cancer patients with acute venous thromboembolism—analysis of the CATCH study. Thromb Haemost 118(05):914–921
Siguret V, Gouin-Thibault I, Pautas E, Leizorovicz A (2011) No accumulation of the peak anti-factor Xa activity of tinzaparin in elderly patients with moderate-to-severe renal impairment: the IRIS substudy. J Thromb Haemost 9(10):1966–1972
Pautas E, Gouin I, Bellot O, Andreux JP, Siguret V (2002) Safety profile of tinzaparin administered once daily at a standard curative dose in two hundred very elderly patients. Drug Saf 25(10):725–733
Park D, Southern W, Calvo M, Kushnir M, Solorzano C, Sinnet M et al (2016) Treatment with dalteparin is associated with a lower risk of bleeding compared to treatment with unfractionated heparin in patients with renal insufficiency. J Gen Intern Med 31(2):182–187
Schmid P, Brodmann D, Odermatt Y, Fischer AG, Wuillemin WA (2009) Study of bioaccumulation of dalteparin at a therapeutic dose in patients with renal insufficiency. J Thromb Haemost 7(10):1629–1632
[NG158] Ng. Venous thromboembolic diseases: diagnosis, management and thrombophilia testing https://www.nice.org.uk/guidance/ng158/chapter/recommendations#anticoagulation-treatment-for-dvt-or-pe-with-renal-impairment-or-established-renal-failure2020
Hughes S, Szeki I, Nash MJ, Thachil J (2014) Anticoagulation in chronic kidney disease patients-the practical aspects. Clin Kidney J 7(5):442–449
Konstantinides SV, Meyer G, Becattini C, Bueno H, Geersing G-J, Harjola V-P et al (2019) 2019 ESC Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS). The Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC) 54(3):1901647
Mahé I, Aghassarian M, Drouet L, Dit-Sollier CB, Lacut K, Heilmann J-J et al (2007) Tinzaparin and enoxaparin given at prophylactic dose for eight days in medical elderly patients with impaired renal function. Thromb Haemost 97(04):581–586
Atiq F, van den Bemt PM, Leebeek FW, van Gelder T, Versmissen J (2015) A systematic review on the accumulation of prophylactic dosages of low-molecular-weight heparins (LMWHs) in patients with renal insufficiency. Eur J Clin Pharmacol 71(8):921–929
Chao TF, Liu CJ, Wang KL, Lin YJ, Chang SL, Lo LW et al (2014) Incidence and prediction of ischemic stroke among atrial fibrillation patients with end-stage renal disease requiring dialysis. Heart Rhythm 11(10):1752–1759
Sood P, Kumar G, Nanchal R, Sakhuja A, Ahmad S, Ali M et al (2012) Chronic kidney disease and end-stage renal disease predict higher risk of mortality in patients with primary upper gastrointestinal bleeding. Am J Nephrol 35(3):216–224
Zuckerman GR, Cornette GL, Clouse RE, Harter HR (1985) Upper gastrointestinal bleeding in patients with chronic renal failure. Ann Intern Med 102(5):588–592
Parker K, Mitra S, Thachil J (2018) Is anticoagulating haemodialysis patients with non-valvular atrial fibrillation too risky? Br J Haematol 181(6):725–736
Belley-Cote EP, Eikelboom JW (2020) Anticoagulation for stroke prevention in patients with atrial fibrillation and end-stage renal disease—first, do no harm. JAMA Netw Open 3(4):e202237
Randhawa MS, Vishwanath R, Rai MP, Wang L, Randhawa AK, Abela G et al (2020) Association between use of warfarin for atrial fibrillation and outcomes among patients with end-stage renal disease: a systematic review and meta-analysis. JAMA Netw Open 3(4):e202175
Kuno T, Takagi H, Ando T, Sugiyama T, Miyashita S, Valentin N et al (2020) Oral anticoagulation for patients with atrial fibrillation on long-term dialysis. J Am Coll Cardiol 75(3):273–285
ClinicalTrials.gov. Oral Anticoagulation in Haemodialysis Patients (AVKDIAL). (2016). Available online at: https://clinicaltrials.gov/ct2/show/NCT02933697
ClinicalTrials.gov. Strategies for the Management of Atrial Fibrillation in patiEnts Receiving Dialysis (SAFE-D). (2019). Available online at: https://clinicaltrials.gov/ct2/show/NCT03987711
ClinicalTrials.gov. The Danish warfarin-dialysis study—safety and efficacy of warfarin in patients with atrial fibrillation on dialysis (DANWARD). (2019). Available online at: https://clinicaltrials.gov/ct2/show/NCT03862859
Stroke prophylaxis with Apixaban in CKD5 patients with atrial fibrillation (SACK). SACK trial information (2022) Available online at: https://njurmed.se/stroke-prophylaxis-with-apixaban-in-ckd5-patients-with-atrial-fibrillation-sack/
ClinicalTrials.gov. Trial to evaluate anticoagulation therapy in hemodialysis patients with atrial fibrillation. RENal Hemodialysis Patients ALlocated Apixaban Versus Warfarin in Atrial Fibrillation (RENAL-AF) (2016) Available online at: https://clinicaltrials.gov/ct2/show/results/NCT02942407
ClinicalTrials.gov. Compare Apixaban and Vitamin-K Antagonists in Patients With Atrial Fibrillation (AF) and End-Stage Kidney Disease (ESKD) (AXADIA) (2016). Available online at: https://clinicaltrials.gov/ct2/show/NCT02933697
Connolly SJ, Ezekowitz MD, Yusuf S, Eikelboom J, Oldgren J, Parekh A et al (2009) Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med 361(12):1139–1151
Patel MR, Mahaffey KW, Garg J, Pan G, Singer DE, Hacke W et al (2011) Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. N Engl J Med 365(10):883–891
Granger CB, Alexander JH, McMurray JJV, Lopes RD, Hylek EM, Hanna M et al (2011) Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med 365(11):981–992
Prescribing information for Pradaxa capsules [updated 11 Jan 2022]. https://www.medicines.org.uk/emc/product/6229/smpc
Sy J, Hsiung JT, Edgett D, Kalantar-Zadeh K, Streja E, Lau WL (2021) Cardiovascular and bleeding outcomes with anticoagulants across kidney disease stages: analysis of a national US cohort. Am J Nephrol 52(3):199–208
Grandone E, Aucella F, Barcellona D, Brunori G, Forneris G, Gresele P et al (2021) Position paper on the safety/efficacy profile of Direct Oral Anticoagulants in patients with Chronic Kidney Disease: consensus document of Società Italiana di Nefrologia (SIN), Federazione Centri per la diagnosi della trombosi e la Sorveglianza delle terapie Antitrombotiche (FCSA) and Società Italiana per lo Studio dell’Emostasi e della Trombosi (SISET). J Nephrol 34(1):31–38
Acknowledgements
Thank you to the University of Manchester specialist librarians who supported with the search strategy design.
Funding
KP is supported by the National Institute for Health Research (HEE/NIHR ICA Programme Clinical Doctoral Research Fellowship, Miss Kathrine Parker, NIHR300545). SM is supported by NIHR Infrastructure in Manchester and Devices for Dignity MIC, Sheffield. The views expressed in this publication are those of the authors and not necessarily those of the NHS, the National Institute for Health Research or the Department of Health and Social Care.
Author information
Authors and Affiliations
Contributions
KP, JT, SM, AP, SC and PI had the idea for the article. KP, JH, AS, RM performed the literature search and data analysis. KP drafted the paper and all authors critically revised the work.
Corresponding author
Ethics declarations
Conflict of interest
Results presented in this paper have not been published previously in whole or part, except in abstract form. Within the last 3 years KP has received honoraria from Bayer. JT has received honoraria from Bayer, Boehringer Ingelheim, BMS-Pfizer, Daichi-Sankyo, Octapharma, Leo Pharma. JH, AS, RM, AP, SC, PL have no competing interests to declare that are relevant to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Parker, K., Hartemink, J., Saha, A. et al. A systematic review of the efficacy and safety of anticoagulants in advanced chronic kidney disease. J Nephrol 35, 2015–2033 (2022). https://doi.org/10.1007/s40620-022-01413-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-022-01413-x