Abstract
Background
The aim of this study was to evaluate, in a cohort of haemodialysis patients with atrial fibrillation (AF), the relationship between oral anticoagulant therapy (OAT) and mortality, thromboembolic events and haemorrhage.
Methods
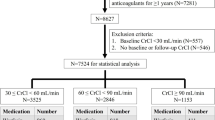
Two hundred and ninety patients with AF were prospectively followed for 4 years. Warfarin and antiplatelet intake, age, dialytic age, comorbidities, CHA2DS2-VASc and HAS-BLED scores were considered as predictors of risk of death, thromboembolism and bleeding events. In patients taking OAT, the international normalized ratio (INR) was assessed and the percentage time in the target therapeutic range (TTR) was calculated.
Results
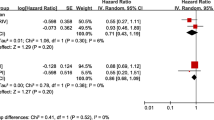
At recruitment, 134/290 patients were taking warfarin. During follow-up there were 170 deaths, 28 thromboembolic events and 95 bleedings. After balancing for treatment propensity, intention-to-treat analysis on OAT intake at recruitment did not show differences in total mortality, thromboembolic events and bleedings, while the as-treated analysis, accounting for treatment switch, showed that patients taking OAT at recruitment had a significantly lower mortality than those not taking it [hazard ratio, HR 0.53 (95% confidence interval 0.28–0.90), p = 0.04], with a decrease of thromboembolic events [HR 0.36 (0.13–1.05), p = 0.06], and an increase of bleedings [HR 1.79 (0.72–4.39), p = 0.20], both non-significant. Among patients taking OAT at recruitment, those continuing to take warfarin had a significant reduction in the risk of total [HR 0.28 (0.14–0.53), p < 0.001] and cardiovascular [HR 0.21 (0.11–0.40), p < 0.001] mortality compared to patients stopping OAT.
Conclusions
In haemodialysis patients with AF, continuously taking warfarin is associated with a reduction of the risk of total and cardiovascular mortality.


Similar content being viewed by others
References
Chan KE, Lazarus JM, Thadhani R et al (2009) Warfarin use associates with increased risk for stroke in hemodialysis patients with atrial fibrillation. J Am Soc Nephrol 20:2223–2233
Shah M, Avgil Tsadok M, Jackevicius CA et al (2014) Warfarin use and the risk for stroke and bleeding in patients with atrial fibrillation undergoing dialysis. Circulation 129:1196–1203
Olesen JB, Lip GY, Kamper AL et al (2012) Stroke and bleeding in atrial fibrillation with chronic kidney disease. N Engl J Med 367:625–635
Carrero JJ, Evans M, Szummer K et al (2014) Warfarin, kidney dysfunction, and outcomes following acute myocardial infarction in patients with atrial fibrillation. J Am Med Assoc 311:919–928
Genovesi S, Rossi E, Pogliani D et al (2014) The nephrologist’s anticoagulation treatment patterns/regimens in chronic hemodialysis patients with atrial fibrillation. J Nephrol 27:187–192
Shen JI, Montez-Rath ME, Lenihan CR et al (2015) Outcomes after warfarin initiation in a cohort of hemodialysis patients with newly diagnosed atrial fibrillation. Am J Kidney Dis 66:677–688
Genovesi S, Rossi E, Gallieni M et al (2015) Warfarin use, mortality, bleeding and stroke in haemodialysis patients with atrial fibrillation. Nephrol Dial Transplant 30:491–498
Camm AJ, Lip GY, De Caterina R et al (2012) 2012 focused update of the ESC guidelines for the management of atrial fibrillation: an update of the 2010 ESC guidelines for the management of atrial fibrillation. Developed with the special contribution of the European Heart Rhythm Association. Eur Heart J 33:2719–2747
Rosendaal FR, Cannegieter SC, van der Meer FJ et al (1993) A method to determine the optimal intensity of oral anticoagulant therapy. Thromb Haemost 69:236–239
Hernán MA, Brumback B, Robins JM (2000) Marginal structural models to estimate the causal effect of zidovudine on the survival of HIV-positive men. Epidemiology 11:561–570
Austin PC (2009) Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 28:3083–3107
Gran JM, Røysland K, Wolbers M et al (2010) A sequential Cox approach for estimating the causal effect of treatment in the presence of time-dependent confounding applied to data from the Swiss HIV Cohort Study. Stat Med 29:2757–2768
Pisters R, Lane DA, Nieuwlaat R et al (2010) A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation: the Euro Heart Survey. Chest 138:1093–1100
Chan KE, Lazarus JM, Thadhani R et al (2009) Anticoagulant and antiplatelet usage associates with mortality among hemodialysis patients. J Am Soc Nephrol 20:872–881
Sood MM, Larkina M, Thumma JR et al (2013) Major bleeding events and risk stratification of antithrombotic agents in hemodialysis: results from the DOPPS. Kidney Int 84:600–608
Bonde AN, Lip GY, Kamper AL et al (2014) Net clinical benefit of antithrombotic therapy in patients with atrial fibrillation and chronic kidney disease: a nationwide observational cohort study. J Am Coll Cardiol 64:2471–2482
Chen JJ, Lin LY, Yang YH et al (2014) Anti-platelet or anti-coagulant agent for the prevention of ischemic stroke in patients with end-stage renal disease and atrial fibrillation-a nation-wide database analyses. Int J Cardiol 177:1008–1011
Fusaro M, Gallieni M, Rebora P,et al (2016) Atrial fibrillation and low vitamin D levels are associated with severe vascular calcifications in hemodialysis patients. J Nephrol 29:419–426
Shih CJ, Ou SM, Chao PW et al (2016) Risks of death and stroke in patients undergoing hemodialysis with new-onset atrial fibrillation: a competing-risk analysis of a nationwide cohort. Circulation 133:265–272
Genovesi S, Vincenti A, Rossi E et al (2008) Atrial fibrillation and morbidity and mortality in a cohort of long-term hemodialysis patients. Am J Kidney Dis 51:255–262
Wizemann V, Tong L, Satayathum S et al (2010) Atrial fibrillation in hemodialysis patients: clinical features and associations with anticoagulant therapy. Kidney Int 77:1098–1106
Seliger SL, Gillen DL, Longstreth WT et al (2003) Elevated risk of stroke among patients with end-stage renal disease. Kidney Int 64:603–609
Ng KP, Edwards NC, Lip GY et al (2013) Atrial fibrillation in CKD: balancing the risks and benefits of anticoagulation. Am J Kidney Dis 62:615–632
Anand SS, Yusuf S (2003) Oral anticoagulants in patients with coronary artery disease. J Am Coll Cardiol 41:62S–69S
Lamberts M, Gislason GH, Lip GY et al (2014) Antiplatelet therapy for stable coronary artery disease in atrial fibrillation patients taking an oral anticoagulant: a nationwide cohort study. Circulation 129:1577–1585
Pilotto A, Gallina P, Copetti M et al (2016) Warfarin treatment and all-cause mortality in community-dwelling older adults with atrial fibrillation: a retrospective observational study. J Am Geriatr Soc 64:1416–1424
Brancaccio D, Neri L, Bellocchio F et al (2016) Patients’ characteristics affect the survival benefit of warfarin treatment for hemodialysis patients with atrial fibrillation. A historical cohort study. Am J Nephrol 44:258–267
Reddy VY, Sievert H, Halperin J et al (2014) Percutaneous left atrial appendage closure vs warfarin for atrial fibrillation: a randomized clinical trial. J Am Med Assoc 312:1988–1998
Zimmerman D, Sood MM, Rigatto C, Holden RM, Hiremath S, Clase CM (2012) Systematic review and meta-analysis of incidence, prevalence and outcomes of atrial fibrillation in patients on dialysis. Nephrol Dial Transplant 27:3816–3822
Danaei G, Tavakkoli M, Hernán MA (2012) Bias in observational studies of prevalent users: lessons for comparative effectiveness research from a meta-analysis of statins. Am J Epidemiol 175:250–262
Acknowledgements
PR was supported by the Grant SIR RBSI14LOVD of the Italian Ministry of Education, University and Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human rights
Procedures were performed according to the Helsinki declaration for ethical treatment of human subjects and approved by the local ethical committee.
Informed consent
Informed consent was obtained from the enrolled subjects.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Genovesi, S., Rebora, P., Gallieni, M. et al. Effect of oral anticoagulant therapy on mortality in end-stage renal disease patients with atrial fibrillation: a prospective study. J Nephrol 30, 573–581 (2017). https://doi.org/10.1007/s40620-016-0364-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-016-0364-8