Abstract
Introduction
Vitamin D (VD) insufficiency has been repeatedly observed in the medical conditions associated with inflammation, such as cardiovascular disease, diabetes and depression. However, contrasting to the observational evidence, randomized trials of VD supplementation failed to demonstrate such link. Given the recent evidence that the inflammatory process can in turn alter VD metabolism, it has been hypothesized that the insufficient VD status could be the result rather than the cause of chronic inflammation involved in the onset of depression and other disease conditions.
Materials and methods
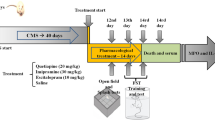
Chronic mild stress (CMS) is a valid animal model of depression that accompanied with neuroendocrine-immune disturbances. In the present research, we assessed serum VD concentrations and renal expression of the cytochromes P450 enzymes involved in VD activation (CYP27B1) and catabolism (CYP24A1) of rats following 8-week exposure to CMS.
Results
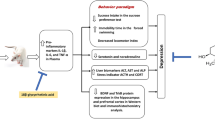
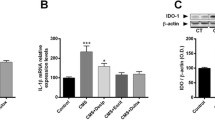
While CMS induced the rats to a depression-like state and increased serum levels of the proinflammatory cytokines and corticosterone, and the antidepressant, sertraline, mitigated depression-like behaviors and neuroendocrine-immune disturbances, neither the stress regimen nor sertraline significantly affected endocrine metabolism of VD.
Conclusion
Our data suggest that the stress-induced neuroendocrine-immune disturbances may account for the development of depression, but are not responsible for the insufficient VD status that frequently observed in depressed patients.




Similar content being viewed by others
References
Song HR, Park CH (2013) Low serum vitamin D level is associated with high risk of metabolic syndrome in post-menopausal women. J Endocrinol Invest 36(10):791–796
Holick MF (2011) Vitamin D: a d-lightful solution for health. J Investig Med 59(6):872–880
Gannage-Yared MH, Azoury M, Mansour I, Baddoura R, Halaby G, Naaman R (2003) Effects of a short-term calcium and vitamin D treatment on serum cytokines, bone markers, insulin and lipid concentrations in healthy post-menopausal women. J Endocrinol Invest 26(8):748–753
Fernandes de Abreu DA, Eyles D, Feron F (2009) Vitamin D, a neuro-immunomodulator: implications for neurodegenerative and autoimmune diseases. Psychoneuroendocrinology 34(Suppl 1):S265–S277
Bolland MJ, Grey A, Gamble GD, Reid IR (2014) The effect of vitamin D supplementation on skeletal, vascular, or cancer outcomes: a trial sequential meta-analysis. Lancet Diabetes Endocrinol 2(4):307–320
Belvederi Murri M, Respino M, Masotti M, Innamorati M, Mondelli V, Pariante C, Amore M (2013) Vitamin D and psychosis: mini meta-analysis. Schizophr Res 150(1):235–239
Bikle DD (2014) Vitamin D metabolism, mechanism of action, and clinical applications. Chem Biol 21(3):319–329
Xiang F, Jiang J, Li H, Yuan J, Yang R, Wang Q, Zhang Y (2013) High prevalence of vitamin D insufficiency in pregnant women working indoors and residing in Guiyang. China J Endocrinol Invest 36(7):503–507
Milaneschi Y, Hoogendijk W, Lips P, Heijboer AC, Schoevers R, van Hemert AM, Beekman AT, Smit JH, Penninx BW (2014) The association between low vitamin D and depressive disorders. Mol Psychiatry 19(4):444–451
Milaneschi Y, Shardell M, Corsi AM, Vazzana R, Bandinelli S, Guralnik JM, Ferrucci L (2010) Serum 25-hydroxyvitamin D and depressive symptoms in older women and men. J.Clin Endocrinol Metab 95(7):3225–3233
Hewison M (2012) An update on vitamin D and human immunity. Clin Endocrinol (Oxf) 76(3):315–325
Haroon E, Raison CL, Miller AH (2012) Psychoneuroimmunology meets neuropsychopharmacology: translational implications of the impact of inflammation on behavior. Neuropsychopharmacology 37(1):137–162
Moylan S, Berk M, Dean OM, Samuni Y, Williams LJ, O’Neil A, Hayley AC, Pasco JA, Anderson G, Jacka FN, Maes M (2014) Oxidative & nitrosative stress in depression: why so much stress? Neurosci Biobehav Rev 45C:46–62
Felger JC, Lotrich FE (2013) Inflammatory cytokines in depression: neurobiological mechanisms and therapeutic implications. Neuroscience 246:199–229
Obradovic D, Gronemeyer H, Lutz B, Rein T (2006) Cross-talk of vitamin D and glucocorticoids in hippocampal cells. J Neurochem 96(2):500–509
Jiang P, Xue Y, Li HD, Liu YP, Cai HL, Tang MM, Zhang LH (2014) Dysregulation of vitamin D metabolism in the brain and myocardium of rats following prolonged exposure to dexamethasone. Psychopharmacology. doi:10.1007/s00213-014-3440-6
Theodoratou E, Tzoulaki I, Zgaga L, Ioannidis JP (2014) Vitamin D and multiple health outcomes: umbrella review of systematic reviews and meta-analyses of observational studies and randomised trials. BMJ 348:g2035
Autier P, Boniol M, Pizot C, Mullie P (2014) Vitamin D status and ill health: a systematic review. Lancet Diabetes Endocrinol 2(1):76–89
Slavich GM, Irwin MR (2014) From stress to inflammation and major depressive disorder: a social signal transduction theory of depression. Psychol Bull 140(3):774–815
Liu N, Nguyen L, Chun RF, Lagishetty V, Ren S, Wu S, Hollis B, DeLuca HF, Adams JS, Hewison M (2008) Altered endocrine and autocrine metabolism of vitamin D in a mouse model of gastrointestinal inflammation. Endocrinology 149(10):4799–4808
Zehnder D, Quinkler M, Eardley KS, Bland R, Lepenies J, Hughes SV, Raymond NT, Howie AJ, Cockwell P, Stewart PM, Hewison M (2008) Reduction of the vitamin D hormonal system in kidney disease is associated with increased renal inflammation. Kidney Int 74(10):1343–1353
Ebert R, Jovanovic M, Ulmer M, Schneider D, Meissner-Weigl J, Adamski J, Jakob F (2004) Down-regulation by nuclear factor kappaB of human 25-hydroxyvitamin D3 1alpha-hydroxylase promoter. Mol Endocrinol 18(10):2440–2450
Anglin RE, Samaan Z, Walter SD, McDonald SD (2013) Vitamin D deficiency and depression in adults: systematic review and meta-analysis. Br J Psychiatry 202:100–107
Farooq RK, Isingrini E, Tanti A, Le Guisquet AM, Arlicot N, Minier F, Leman S, Chalon S, Belzung C, Camus V (2012) Is unpredictable chronic mild stress (UCMS) a reliable model to study depression-induced neuroinflammation? Behav Brain Res 231(1):130–137
Xia X, Pan Y, Zhang WY, Cheng G, Kong LD (2006) Ethanolic extracts from curcuma longa attenuates behavioral, immune, and neuroendocrine alterations in a rat chronic mild stress model. Biol Pharm Bull 29(5):938–944
Liu XL, Luo L, Liu BB, Li J, Geng D, Liu Q, Yi LT (2014) Ethanol extracts from hemerocallis citrina attenuate the upregulation of proinflammatory cytokines and indoleamine 2,3-dioxygenase in rats. J Ethnopharmacol 153(2):484–490
Sukoff Rizzo SJ, Neal SJ, Hughes ZA, Beyna M, Rosenzweig-Lipson S, Moss SJ, Brandon NJ (2012) Evidence for sustained elevation of IL-6 in the CNS as a key contributor of depressive-like phenotypes. Transl Psychiatry 2:e199
Liu W, Sheng H, Xu Y, Liu Y, Lu J, Ni X (2013) Swimming exercise ameliorates depression-like behavior in chronically stressed rats: relevant to proinflammatory cytokines and IDO activation. Behav Brain Res 242:110–116
Voorhees JL, Tarr AJ, Wohleb ES, Godbout JP, Mo X, Sheridan JF, Eubank TD, Marsh CB (2013) Prolonged restraint stress increases IL-6, reduces IL-10, and causes persistent depressive-like behavior that is reversed by recombinant IL-10. PLoS One 8(3):e58488
Kalinichenko LS, Pertsov SS, Koplik EV (2014) Melatonin effects on serum cytokine profiles of rats with different behavioral parameters in acute emotional stress. Bull Exp Biol Med 156(5):627–630
Shaashua L, Rosenne E, Neeman E, Sorski L, Sominsky L, Matzner P, Page GG, Ben-Eliyahu S (2014) Plasma IL-12 levels are suppressed in vivo by stress and surgery through endogenous release of glucocorticoids and prostaglandins but not catecholamines or opioids. Psychoneuroendocrinology 42:11–23
Capellino S, Straub RH, Cutolo M (2014) Aromatase and regulation of the estrogen-to-androgen ratio in synovial tissue inflammation: common pathway in both sexes. Ann N Y Acad Sci 1317:24–31
Vignozzi L, Morelli A, Sarchielli E, Comeglio P, Filippi S, Cellai I, Maneschi E, Serni S, Gacci M, Carini M, Piccinni MP, Saad F, Adorini L, Vannelli GB, Maggi M (2012) Testosterone protects from metabolic syndrome-associated prostate inflammation: an experimental study in rabbit. J Endocrinol 212(1):71–84
Carrier N, Kabbaj M (2012) Testosterone and imipramine have antidepressant effects in socially isolated male but not female rats. Horm Behav 61(5):678–685
Johnson JM, Nachtigall LB, Stern TA (2013) The effect of testosterone levels on mood in men: a review. Psychosomatics 54(6):509–514
Zarrouf FA, Artz S, Griffith J, Sirbu C, Kommor M (2009) Testosterone and depression: systematic review and meta-analysis. J Psychiatr Pract 15(4):289–305
Acknowledgments
This research was supported by National Natural Science Foundation of China (No. 81101001).
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jiang, P., Zhang, L., Zhu, W. et al. Chronic stress causes neuroendocrine-immune disturbances without affecting renal vitamin D metabolism in rats. J Endocrinol Invest 37, 1109–1116 (2014). https://doi.org/10.1007/s40618-014-0191-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-014-0191-5