Abstract
Background and Objective
Hepatocellular carcinoma (HCC) is the fourth leading cause of cancer-related mortality worldwide. Despite recent advances, more effective therapeutic options for patients with advanced HCC are still required. The aim of this Phase 2, multicenter, multinational, randomized, double-blind, placebo-controlled study (NCT02528643) was to investigate the potential benefit of enzalutamide in the treatment of patients with advanced HCC.
Methods
Patients aged ≥ 18 years diagnosed with advanced HCC (Barcelona Clinic Liver Cancer stage B or C and Child-Pugh class A at screening who had progressed on, or were intolerant to, sorafenib or other anti-vascular endothelial growth factor therapies) were randomized 2:1 to receive either enzalutamide 160 mg daily or placebo. The primary endpoint was overall survival (OS); secondary endpoints included progression-free survival (PFS) and safety.
Results
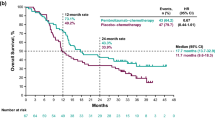
In total, 165 patients were randomized to enzalutamide (n = 110) or placebo (n = 55). The hazard ratio (HR) (95% confidence interval [CI]) for OS was 1.15 (0.774–1.696) and median OS was 7.8 months and 7.7 months for enzalutamide and placebo, respectively. The HR (95% CI) for PFS was 1.04 (0.732–1.474) and median PFS was 2.2 months and 1.9 months for enzalutamide and placebo, respectively. The overall frequency of treatment-emergent adverse events (TEAEs) was broadly similar between the groups: 105 (98.1%) enzalutamide patients experienced ≥1 TEAEs compared with 49 (89.1%) placebo patients.
Conclusions
The results of this study indicate that enzalutamide does not provide a benefit in patients with advanced HCC. No unexpected safety findings were observed in the trial.
ClinicalTrials.gov identifier
NCT02528643.



Similar content being viewed by others
Change history
27 February 2022
A Correction to this paper has been published: https://doi.org/10.1007/s40261-022-01132-y
References
Global Burden of Disease Cancer Collaboration. Global, regional, and national cancer incidence, mortality, years of life lost, years lived with disability, and disability-adjusted life-years for 32 cancer groups, 1990 to 2015: a systematic analysis for the global burden of disease study. JAMA Oncol. 2017;3(4):524–48.
Perz JF, Armstrong GL, Farrington LA, Hutin YJF, Bell BP. The contributions of hepatitis B virus and hepatitis C virus infections to cirrhosis and primary liver cancer worldwide. J Hepatol. 2006;45(4):529–38.
McGlynn KA, London WT. The global epidemiology of hepatocellular carcinoma: present and future. Clin Liver Dis. 2011;15(2):223–43.
Llovet JM, Ricci S, Mazzaferro V, Hilgard P, Gane E, Blanc JF, et al. Sorafenib in advanced hepatocellular carcinoma. N Engl J Med. 2008;359(4):378–90.
Cidon EU. Systemic treatment of hepatocellular carcinoma: past, present and future. World J Hepatol. 2017;9(18):797–807.
Feng H, Cheng AS, Tsang DP, Li MS, Go MY, Cheung YS, et al. Cell cycle-related kinase is a direct androgen receptor-regulated gene that drives beta-catenin/T cell factor-dependent hepatocarcinogenesis. J Clin Invest. 2011;121(8):3159–75.
Chiu CM, Yeh SH, Chen PJ, Kuo TJ, Chang CJ, Chen PJ, et al. Hepatitis B virus X protein enhances androgen receptor-responsive gene expression depending on androgen level. Proc Natl Acad Sci U S A. 2007;104(8):2571–8.
Nagasue N, Chang YC, Hayashi T, Galizia G, Kohno H, Nakamura T, et al. Androgen receptor in hepatocellular carcinoma as a prognostic factor after hepatic resection. Ann Surg. 1989;209(4):424–7.
Nagasue N, Ito A, Yukaya H, Ogawa Y. Androgen receptors in hepatocellular carcinoma and surrounding parenchyma. Gastroenterology. 1985;89(3):643–7.
Acosta-Lopez S, Diaz-Bethencourt D, Concepcion-Massip T, de Basoa M-FMC, Plata-Bello A, Gonzalez-Rodriguez A, et al. The androgen receptor expression and its activity have different relationships with prognosis in hepatocellular carcinoma. Sci Rep. 2020;10(1):22046.
Tran C, Ouk S, Clegg NJ, Chen Y, Watson PA, Arora V, et al. Development of a second-generation antiandrogen for treatment of advanced prostate cancer. Science. 2009;324(5928):787–90.
Scher HI, Fizazi K, Saad F, Taplin ME, Sternberg CN, Miller K, et al. Increased survival with enzalutamide in prostate cancer after chemotherapy. N Engl J Med. 2012;367(13):1187–97.
Beer TM, Armstrong AJ, Rathkopf DE, Loriot Y, Sternberg CN, Higano CS, et al. Enzalutamide in metastatic prostate cancer before chemotherapy. N Engl J Med. 2014;371(5):424–33.
Armstrong AJ, Szmulewitz RZ, Petrylak DP, Holzbeierlein J, Villers A, Azad A, et al. ARCHES: a randomized, Phase III study of androgen deprivation therapy with enzalutamide or placebo in men with metastatic hormone-sensitive prostate cancer. J Clin Oncol. 2019;37(32):2974–86.
Hussain M, Fizazi K, Saad F, Rathenborg P, Shore N, Ferreira U, et al. Enzalutamide in men with nonmetastatic, castration-resistant prostate cancer. N Engl J Med. 2018;378(26):2465–74.
Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45(2):228–47.
Gibbons JA, Ouatas T, Krauwinkel W, Ohtsu Y, van der Walt JS, Beddo V, et al. Clinical pharmacokinetic studies of enzalutamide. Clin Pharmacokinet. 2015;54(10):1043–55.
Tombal B, Borre M, Rathenborg P, Werbrouck P, Van Poppel H, Heidenreich A, et al. Enzalutamide monotherapy in hormone-naive prostate cancer: primary analysis of an open-label, single-arm, phase 2 study. Lancet Oncol. 2014;15(6):592–600.
Nowak AK, Stockler MR, Chow PKH, Findlay M. Use of tamoxifen in advanced-stage hepatocellular carcinoma. A systematic review. Cancer. 2005;103(7):1408–14.
Villa E, Ferretti I, Grottola A, Buttafoco P, Buono MG, Giannini F, et al. Hormonal therapy with megestrol in inoperable hepatocellular carcinoma characterized by variant oestrogen receptors. Br J Cancer. 2001;84(7):881–5.
Chow PK, Machin D, Chen Y, Zhang X, Win KM, Hoang HH, et al. Randomised double-blind trial of megestrol acetate vs placebo in treatment-naive advanced hepatocellular carcinoma. Br J Cancer. 2011;105(7):945–52.
Xidakis C, Kolios G, Valatas V, Notas G, Mouzas I, Kouroumalis E. Effect of octreotide on apoptosis-related proteins in rat Kupffer cells: a possible anti-tumour mechanism. Anticancer Res. 2004;24(2b):833–42.
Ji XQ, Ruan XJ, Chen H, Chen G, Li SY, Yu B. Somatostatin analogues in advanced hepatocellular carcinoma: an updated systematic review and meta-analysis of randomized controlled trials. Med Scie Monit. 2011;17(8):RA1169–76.
Jia WD, Zhang CH, Xu GL, Ge YS, Wang W. Octreotide therapy for hepatocellular carcinoma: a systematic review of the evidence from randomized controlled trials. Hepatogastroenterology. 2010;57(98):292–9.
Dauki AM, Blachly JS, Kautto EA, Ezzat S, Abdel-Rahman MH, Coss CC. Transcriptionally active androgen receptor splice variants promote hepatocellular carcinoma progression. Cancer Res. 2020;80(3):561–75.
Chen JY, Liu LP, Xu JF. Decrease of RBM4 indicates poor prognosis in patients with hepatocellular carcinoma after hepatectomy. Onco Targets Ther. 2017;10:339–45.
Bruix J, Qin S, Merle P, Granito A, Huang YH, Bodoky G, et al. Regorafenib for patients with hepatocellular carcinoma who progressed on sorafenib treatment (RESORCE): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet. 2017;389(10064):56–66.
Abou-Alfa GK, Meyer T, Cheng AL, El-Khoueiry AB, Rimassa L, Ryoo BY, et al. Cabozantinib in patients with advanced and progressing hepatocellular carcinoma. N Engl J Med. 2018;379(1):54–63.
Bergerot P, Lamb P, Wang E, Pal SK. Cabozantinib in combination with immunotherapy for advanced renal cell carcinoma and urothelial carcinoma: rationale and clinical evidence. Mol Cancer Ther. 2019;18(12):2185–93.
Zhu AX, Kang YK, Yen CJ, Finn RS, Galle PR, Llovet JM, et al. Ramucirumab after sorafenib in patients with advanced hepatocellular carcinoma and increased alpha-fetoprotein concentrations (REACH-2): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Oncol. 2019;20(2):282–96.
Kudo M, Finn RS, Qin S, Han KH, Ikeda K, Piscaglia F, et al. Lenvatinib versus sorafenib in first-line treatment of patients with unresectable hepatocellular carcinoma: a randomised phase 3 non-inferiority trial. Lancet. 2018;391(10126):1163–73.
El-Khoueiry AB, Sangro B, Yau T, Crocenzi TS, Kudo M, Hsu C, et al. Nivolumab in patients with advanced hepatocellular carcinoma (CheckMate 040): an open-label, non-comparative, phase 1/2 dose escalation and expansion trial. Lancet. 2017;389(10088):2492–502.
Zhu AX, Finn RS, Edeline J, Cattan S, Ogasawara S, Palmer D, et al. Pembrolizumab in patients with advanced hepatocellular carcinoma previously treated with sorafenib (KEYNOTE-224): a non-randomised, open-label phase 2 trial. Lancet Oncol. 2018;19(7):940–52.
Yau T, Park JW, Finn RS, Cheng A-L, Mathurin P, Edeline J, et al. LBA38_PR - CheckMate 459: A randomized, multi-center phase III study of nivolumab (NIVO) vs sorafenib (SOR) as first-line (1L) treatment in patients (pts) with advanced hepatocellular carcinoma (aHCC). Ann Oncol. 2019; p. LBA38_PR.
Finn RS, Ryoo BY, Merle P, Kudo M, Bouattour M, Lim HY, et al. Pembrolizumab As second-line therapy in patients with advanced hepatocellular carcinoma in KEYNOTE-240: a randomized, double-blind. Phase III Trial J Clin Oncol. 2020;38(3):193–202.
Finn RS, Qin S, Ikeda M, Galle PR, Ducreux M, Kim TY, et al. Atezolizumab plus bevacizumab in unresectable hepatocellular carcinoma. N Engl J Med. 2020;382(20):1894–905.
Finn RS, Qin S, Ikeda M, Galle PR, Ducreux M, Kim T-Y, et al. IMbrave150: updated overall survival data from a global, randomized, open-label Phase III study of atezolizumab + bevacizumab vs sorafenib in patients with unresectable hepatocellular carcinoma. In: Carducci MA, editor. In: 2021 Gastrointestinal Cancer Proceedings; Virtual: American Society of Clinical Oncology. 2021.
FDA approves Roche's Tecentriq in combination with Avastin for people with the most common form of liver cancer [press release]. Noivember 19, 2020 2020. Roche Group Media Relations.
Yau T, Kang YK, Kim TY, El-Khoueiry AB, Santoro A, Sangro B, et al. Efficacy and safety of nivolumab plus ipilimumab in patients with advanced hepatocellular carcinoma previously treated with sorafenib: the CheckMate 040 randomized clinical trial. JAMA Oncol. 2020.
Finn RS, Ikeda M, Zhu AX, Sung MW, Baron AD, Kudo M, et al. Phase Ib study of lenvatinib plus pembrolizumab in patients with unresectable hepatocellular carcinoma. J Clin Oncol. 2020;38(26):2960–70.
Abou-Alfa GK, Chan SL, Furuse J, Galle PR, Kelley RK, Qin S, et al. A randomized, multicenter phase 3 study of durvalumab (D) and tremelimumab (T) as first-line treatment in patients with unresectable hepatocellular carcinoma (HCC): HIMALAYA study. J Clin Oncol. 2018;36(15 Suppl).
Llovet J, Masatoshi K, Cheng AL, Finn RS, Galle PR, Kaneko S, et al. Lenvatinib (len) plus pembrolizumab (pembro) for the first-line treatment of patients (pts) with advanced hepatocellular carcinoma (HCC): Phase 3 LEAP-002 study. J Clin Oncol. 2019;13(15 suppl).
Kang RK, Oliver JW, Hazra S, Benzaghou F, Yau T, Cheng AL, et al. Cabozantinib in combination with atezolizumab versus sorafenib in treatment-naive advanced hepatocellular carcinoma: COSMIC-312 Phase III study designCabozantinib in design. Future Oncol. 2020;16(21):1525–36.
Zhu AX, Kang YK, Yen CJ, Finn RS, Galle PR, Llovet JM, et al. J Clin Oncol. 2018;36(suppl):abstract 44003.
Acknowledgements
Medical writing and editorial assistance were provided by Caitlin Watson, PhD, and Rebecca Fletcher from Complete HealthVizion, funded by the study sponsors. A list of the study investigators and sub-investigators is provided in the supplementary material.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Author contributions
The authors meet criteria for authorship as recommended by the International Committee of Medical Journal Editors. All authors had full access to all of the data in the study and had final responsibility for the decision to submit for publication; they take full responsibility for the scope, direction and content of the manuscript and have approved the submitted manuscript. The authors received no compensation related to the development of the manuscript. Study conception and design: B-YR, JS, and HYL. Material preparation, data collection and analysis: B-YR, DHP, SRP, LR, DS, BD, JS, BL, and HYL. Writing—original draft preparation: LR, JS, BL. Writing—review and editing: B-YR, DHP, SRP, LR, DS, BD, JS, BL, and HYL. Supervision: B-YR, JS.
Data availability
Researchers may request access to anonymized participant level data, trial level data and protocols from Astellas sponsored clinical trials at www.clinicalstudydatarequest.com. For the Astellas criteria on data sharing see: https://clinicalstudydatarequest.com/Study-Sponsors/Study-Sponsors-Astellas.aspx.
Funding
This study was funded by Astellas Pharma Inc. and Pfizer Inc., the co-developers of enzalutamide. The study sponsors were involved in the design and conduct of the study, the collection, management, analysis and interpretation of the data, and the review and approval of the manuscript.
Conflict of interest
B.-Y. Ryoo received grants from Astellas Pharma Inc. during the conduct of the study. D.H. Palmer received personal fees from Astellas Pharma Inc. during the conduct of the study; grants and personal fees from Bayer, NuCana, and Sirtex outside the submitted work; and personal fees from BMS, Celgene, Halozyme, and Targovax outside the submitted work. The institution of L. Rimassa received grants from Astellas Pharma Inc. during the conduct of the study; grants from Agios, ARMO Biosciences, AstraZeneca, Beigene, Eisai, Exelixis, Fibrogen, Incyte, Ipsen, Lilly, MSD, Nerviano Medical Services, Roche, and Zymeworks outside the submitted work; personal fees from AbbVie, Amgen, ArQule, AstraZeneca, Basilea, Bayer, BMS, Celgene, Eisai, Exelixis, Genenta, Gilead, Hengrui Therapeutics, Incyte, Ipsen, IQVIA, Lilly, Merck Serono, MSD, Nerviano Medical Sciences, Roche, Sanofi and Zymeworks outside the submitted work; and non-financial support from Ipsen outside the submitted work. D. Sarker has received advisory board payments from Eisai, Ipsen, Novartis, and Surface Oncology outside the submitted work; honoraria from the speakers bureaus of AstraZeneca, Bayer, Eisai, Ipsen, MSD, and Pfizer outside the submitted work; and travel payments from Bayer, Eisai, and MiNA Therapeutics outside the submitted work. B. Daniele has received personal fees from Amgen, Astra Zeneca, Bayer, Ipsen, Lilly, MSD, Roche, and Sanofi outside the submitted work; and personal fees and payment for lectures from Eisai outside the submitted work. H.Y. Lim has received consulting fees or honorarium from AstraZeneca, Bayer, BMS, Eisai, and Ipsen outside the submitted work. J. Steinberg is an employee of Astellas Pharma Inc. and B. López was an employee of Astellas Pharma Inc. at the time of the study. S.R. Park reports no conflicts of interest.
Ethics approval
The study was performed in accordance with the Declaration of Helsinki and the International Conference on Harmonisation for Good Clinical Practice Guidelines. The trial protocol, patient information sheets, and consent forms were reviewed and approved by the independent ethics committee and/or institutional review board (IRB) of each participating institution. This study had 37 study sites and 27 approving IRBs; the full list of IRBs can be found in the supplementary material.
Informed consent
Informed consent was received from each patient prior to any study-related procedures.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ryoo, BY., Palmer, D.H., Park, S.R. et al. Efficacy and Safety Results from a Phase 2, Randomized, Double-Blind Study of Enzalutamide Versus Placebo in Advanced Hepatocellular Carcinoma. Clin Drug Investig 41, 795–808 (2021). https://doi.org/10.1007/s40261-021-01063-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40261-021-01063-0