Abstract
Purpose
Ovarian granulosa cell tumors (GCTs) typically exhibit an excellent prognosis, but their recurrences are associated with high mortality rates. In the past, immunohistochemistry (IHC)-based approaches have been used to facilitate the distinction between GCTs and other, more frequently occurring, primary or metastatic tumors. The purpose of this study was to assess the added value of H1.5 and PLZF protein expression in the correct delineation of GCTs.
Methods
Consecutive 5-μm thick sections from routinely fixed and paraffin embedded tissues from 30 GCTs and 33 benign ovaries were processed for IHC using anti-PLZF and anti-H1.5 monoclonal antibodies. The respective protein staining intensities and distributions were quantified into reported scores for all tissue samples. Student’s t-test and Fisher’s exact test were used to compare the mean scores for each group. A p-value of <0.05 was considered statistically significant. Also, both the sensitivity and the specificity of the two antibodies were evaluated.
Results
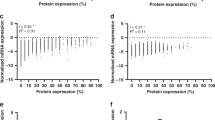
A statistically significant difference in the expression of H1.5 between the GCT and normal ovary groups was observed (p < 0.0001). Normal ovarian tissues were found to strongly express H1.5, whereas GCTs were found to weakly express this protein. In contrast, PLZ expression was not found to be significantly different between both study groups.
Conclusions
From our results we conclude that H1.5 is down-regulated in GCTs compared to normal ovarian tissues. Additional investigations on larger and more heterogeneous study populations, and on the molecular mechanism (s) underlying down-regulation of the H1.5 protein, may further substantiate the use of H1.5 as a diagnostic/prognostic marker and, in addition, provide insight into the pathogenesis of GCTs.


Similar content being viewed by others
References
S.T. Schumer, S.A. Cannistra, Granulosa cell tumor of the ovary. J. Clin. Oncol. 21, 1180–1189 (2003)
L. Unkila-Kallio, A. Tiitinen, T. Wahlstrom, P. Lehtovirta, A. Leminen, Reproductive features in women developing ovarian granulosa cell tumour at a fertile age. Hum. Reprod. 15(3), 589–593 (2000)
D. Pectasides, E. Pectasides, A. Psyrri, Granulosa cell tumor of the ovary. Cancer Treat. Rev. 34, 1–12 (2008)
L. Merras-Salmio, K. Vettenranta, M. Mottonen, M. Heikinheimo, Ovarian granulosa cell tumors in childhood. Pediatr. Hematol. Oncol. 19, 145–156 (2002)
T. Fujimoto, N. Sakuragi, K. Okuyama, T. Fujino, K. Yamashita, S. Yamashiro, M. Shimizu, S. Fujimoto, Histopathological prognostic factors of adult granulosa cell tumors of the ovary. Acta Obstet. Gynecol. Scand. 80, 1069–1074 (2001)
H.S. Cronje, I. Niemand, R.H. Bam, J.D. Woodruff, Review of the granulosa-theca cell tumors from the Emil Novak ovarian tumor registry. Am. J. Obstet. Gynecol. 180, 323–327 (1999)
R.H. Young, R.E. Scully, Ovarian sex cord-stromal tumors. Problems in differential diagnosis. Pathol. Annu. 23, 237–296 (1988)
S. Nofech-Mozes, N. Ismiil, V. Dubé, R.S. Saad, M.A. Khalifa, O. Moshkin, Z. Ghorab, Immunohistochemical characterization of primary and recurrent adult granulosa cell tumors. Int. J. Gynecol. Pathol. 31(1), 80–90 (2012)
P.L. Yeyati, R. Shaknovich, S. Boterashvili, J. Li, H.J. Ball, S. Waxman, K. Nason-Burchenal, E. Dmitrovsky, A. Zelent, J.D. Licht, Leukemia translocation protein PLZF inhibits cell growth and expression of cyclin A. Oncogene 18(4), 925–934 (1999)
F. Felicetti, L. Bottero, N. Felli, G. Mattia, C. Labbaye, E. Alvino, C. Peschle, M.P. Colombo, A. Carè, Role of PLZF in melanoma progression. Oncogene 23(26), 4567–4576 (2004)
M. Cheung, J. Pei, Y. Pei, S.C. Jhanwar, H.I. Pass, J.R. Testa, The promyelocytic leukemia zinc-finger gene, PLZF, is frequently downregulated in malignant mesothelioma cells and contributes to cell survival. Oncogene 29(11), 1633–1640 (2010). doi:10.1038/onc.2009.455. Epub 2009 Dec 14
D.A. Hill, Influence of linker histone H1 on chromatin remodeling. Biochem. Cell Biol. 79(3), 317–324 (2001)
N. Happel, S. Stoldt, B. Schmidt, D. Doenecke, M phase-specific phosphorylation of histone H1.5 at threonine 10 by GSK-3. J. Mol. Biol. 386(2), 339–350 (2009)
Sato S, Takahashi S, Asamoto M, Nakanishi M, Wakita T, Ogura Y, Yatabe Y, Shirai T. Histone H1 expression in human prostate cancer tissues and cell lines. Pathol Int. 2012 Feb;62(2):84–92. doi: 10.1111/j.1440-1827.2011.02755.x. Epub 2011 Nov 28.
J.F. Hechtman, M.B. Beasley, Y. Kinoshita, H.M. Ko, K. Hao, D.E. Burstein, Promyelocytic leukemia zinc finger and histone H1.5 differentially stain low- and high-grade pulmonary neuroendocrine tumors: a pilot immunohistochemical study. Hum. Pathol. 44, 1400–1405 (2013)
M. Markman, M.E. Randall, R.R. Barakat, Principles and practice of gynecologic oncology (Lippencott Williams & Wilkins, Philadelphia, 2009)
R.H. Young, G.R. Dickersin, R.E. Scully, Juvenile granulosa cell tumor of the ovary. A clinicopathological analysis of 125 cases. Am. J. Surg. Pathol. 8(8), 575–596 (1984)
R.H. Young, Sex cord-stromal tumors of the ovary and testis: their similarities and differences with consideration of selected problems. Mod. Pathol. 18, S81–S98 (2005)
W.G. McCluggage, Immunoreactivity of ovarian juvenile granulosa cell tumours with epithelial membrane antigen. Histopathology 46, 235–236 (2005)
A.C. Assis Neto, B.A. Ball, P. Browne, A.J. Conley, Cellular localization of androgen synthesis in equine granulosa-theca cell tumors: Immunohistochemical expression of 17α-hydroxylase/17,20-lyase cytochrome P450. Theriogenology 74, 393–401 (2010)
K.T. Loo, A.K.F. Leung, J.K.C. Chan, Immunohistochemical staining of ovarian granulosa cell tumours with MIC2 antibody. Histopathology 27, 388–390 (1995)
C. Zhao, T.N. Vinh, K.Q.I.H.C. McManus, D. Dabbs, R. Barner, R. Vang, Identification of the most sensitive and robust immunohistochemical markers in different categories of ovarian sex cord-stromal tumors. Am. J. Surg. Pathol. 33, 354–366 (2009)
B.A. Ball, A.J. Conley, D.T. MacLaughlin, S.A. Grundy, K. Sabeur, I.K.M. Liu, Expression of anti-mullerian hormone (AMH) in equine granulosa-cell tumors and in normal equine ovaries. Theriogenology 70, 968–977 (2008)
C. Barcena, E. Oliva, WT1 expression in the female genital tract. Advanced Anatomic Patholology 18(6), 454–465 (2011)
A. Farkkila, M. Anttonen, J. Pociuviene, A. Leminen, R. Butzow, M. Heikinheimo, L. Unkila-Kallio, Vascular endothelial growth factor (VEGF) and its receptor VEGFR-2 are highly expressed in ovarian granulosa cell tumors. Eur. J. Endocrinol. 164, 115–122 (2011)
Y. Ohishi, T. Kaku, M. Oya, H. Kobayashi, N. Wake, M. Tsuneyoshi, CD56 expression in ovarian granulosa cell tumors, and its diagnostic utility and pitfalls. Gynecol. Oncol. 107, 30–38 (2007)
E. Oliva, N. Garcia-Miralles, Q. Vu, R.H. Young, CD10 expression in pure stromal and sex cord-stromal tumors of the ovary: an immunohistochemical analysis of 101 cases. Int. J. Gynecol. Pathol. 26, 359–367 (2007)
L. Wang, X. Chang, G. Yuan, Y. Zhao, P. Wang, Expression of peptidylarginine deiminase type 4 in ovarian tumors. Int. J. Biol. Sci. 6, 454–464 (2010)
Y. Fan, T. Nikitina, J. Zhao, T.J. Fleury, R. Bhattacharyya, E.E. Bouhassira, A. Stein, C.L. Woodcock, A.I. Skoultchi, Histone H1 depletion in mammals alters global chromatin structure but causes specific changes in gene regulation. Cell 123(7), 1199–1212 (2005)
X. Shen, M.A. Gorovsky, Linker histone H1 regulates specific gene expression but not global transcription in vivo. Cell 86(3), 475–483 (1996)
H. Lee, R. Habas, C. Abate-Shen, MSX1 cooperates with histone H1b for inhibition of transcription and myogenesis. Science 304(5677), 1675–1678 (2004)
N.N. Kostova, L.N. Srebreva, A.D. Milev, O.G. Bogdanova, I. Rundquist, H.H. Lindner, D.V. Markov, Immunohistochemical demonstration of histone H1° in human breast carcinoma. Histochem. Cell Biol. 124, 435–443 (2005)
S.J. Chen, A. Zelent, J.H. Tong et al., Rearrangements of the retinoic acid receptor alpha and promyelocytic leukemia zinc finger genes resulting from t (11; 17) (q 23; q 21) in a patient with acute promyelocytic leukemia. J. Clin. Invest. 91, 2260–2267 (1993)
L. Buluwela, J. Pike, D. Mazhar, T. Kamalati, S.M. Hart, R. Al-Jehani, H. Yahaya, N. Patel, N. Sarwarl, D.A. Heathcote, O. Schwickerath, F. Phoenix, R. Hill, E. Aboagye, S. Shousha, J. Waxman, N.R. Lemoine, A. Zelent, R.C. Coombes, S. Ali, Inhibiting estrogen responses in breast cancer cells using a fusion protein encoding estrogen receptor-α and the transcriptional repressor PLZF. Gene Ther. 12, 452–460 (2005)
Disclosure
The authors report no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Momeni, M., Kalir, T., Farag, S. et al. Expression of H1.5 and PLZF in granulosa cell tumors and normal ovarian tissues: a short report. Cell Oncol. 37, 229–234 (2014). https://doi.org/10.1007/s13402-014-0174-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-014-0174-8