Abstract
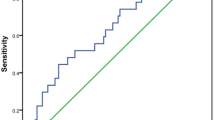
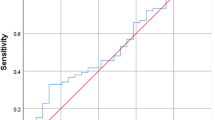
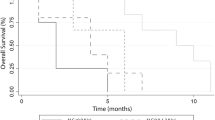
Recently, absolute lymphocyte count (ALC) at diagnosis, as a surrogate marker of host immunity, has been reported to be a prognostic factor for clinical outcomes in extranodal NK/T cell lymphoma (ENKTL). In this retrospective study, we set out to investigate whether ALC at the time of confirmed relapse or at last follow-up is a marker for relapse after chemoradiotherapy in 84 patients with stage I/II ENKTL. Receiver operating characteristics (ROC) curve and area under the curve (AUC) analysis showed that ALC at follow-up was a significant marker for relapse (AUC = 0.883, P < 0.001). Using 1.215 × 109/L as the optimal cutoff value of ALC, 44 patients (52.4 %) were in lower ALC group and 40 patients (47.6 %) were in higher ALC group. The sensitivity and specificity for ALC at the time of confirmed relapse or at last follow-up was 94.1 and 76.0 %, respectively. The relative risk of relapse with an ALC < 1.215 × 109/L was 14.5. The positive predictive value with an ALC < 1.215 × 109/L was 72.7 %, and the negative predictive value with an ALC ≥ 1.215 × 109/L was 95.0 %. The 4-year cumulative incidence rate for an ALC < 1.215 × 109/L was 73.2 % compared with 3.2 % for an ALC ≥ 1.215 × 109/L (P < 0.001). In a multivariate regression analysis, ALC at the time of confirmed relapse or last follow-up remained to be a significant factor for relapse (P < 0.001). In conclusion, lymphopenia observed during routine follow-up can predict relapse in patients with ENKTL, which needs further validation in prospective trials.



Similar content being viewed by others
References
Li YX, Liu QF, Fang H, et al. Variable clinical presentations of nasal and Waldeyer ring natural killer/T-cell lymphoma. Clin Cancer Res. 2009;15(8):2905–12.
Li YX, Yao B, Jin J, et al. Radiotherapy as primary treatment for stage IE and IIE nasal natural killer/T-cell lymphoma. J Clin Oncol. 2006;24:181–9.
Yamaguchi M, Tobinai K, Oguchi M, Ishizuka N, Kobayashi Y, Isobe Y, et al. Phase I/II study of concurrent chemoradiotherapy for localized nasal natural killer/T-cell lymphoma: Japan Clinical Oncology Group Study JCOG0211. J Clin Oncol. 2009;27(33):5594–600.
Wang L, Wang ZH, Chen XQ, Li YJ, Wang KF, Xia YF, et al. First-line combination of gemcitabine, oxaliplatin, and l-asparaginase (GELOX) followed by involved-field radiation therapy for patients with stage IE/IIE extranodal natural killer/T-cell lymphoma. Cancer. 2013;119:348–55.
Wang B, Li XQ, Ma X, Hong X, Lu H, Guo Y. Immunohistochemical expression and clinical significance of P-glycoprotein in previously untreated extranodal NK/T-cell lymphoma, nasal type. Am J Hematol. 2008;83:795–9.
Yamaguchi M, Kwong YL, Kim WS, et al. Phase II study of SMILE chemotherapy for newly diagnosed stage IV, relapsed, or refractory extranodal natural killer (NK)/T-cell lymphoma, nasal type: the NK-Cell Tumor Study Group study. J Clin Oncol. 2011;29:4410–6.
Jaccard A, Gachard N, Marin B, et al. Efficacy of l-asparaginase with methotrexate and dexamethasone (AspaMetDex regimen) in patients with refractory or relapsing extranodal NK/T-cell lymphoma, a phase 2 study. Blood. 2011;117:1834–9.
Zhang Y, Wei Y, Wang X, et al. Midline NK/T-cell lymphoma nasal-type: treatment outcome, the effect of l-asparaginase based regimen, and prognostic factors. Hematol Oncol. 2006;24:28–32.
Kim GE, Cho JH, Yang WI, et al. Angiocentric lymphoma of the head and neck: patterns of systemic failure after radiation treatment. J Clin Oncol. 2000;18:54–63.
Wang L, Xia ZJ, Huang HQ, Lu Y, Zhang YJ. Cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP) in the treatment of stage IE/IIE extranodal natural killer/T cell lymphoma, nasal type: 13-year follow-up in 135 patients. Int J Hematol. 2012;96(5):617–23.
National Comprehensive Cancer Network (NCCN). Extranodal NK/T-cell lymphoma, nasal type. Pract Guidel Oncol. 2013;1.
National Comprehensive Cancer Network (NCCN). Diffuse large B-cell lymphoma. Practice Guidel Oncol. 2013;1.
Schoulten HC. Response evaluation and long term follow-up. Ann Oncol. 2007;18 Suppl 1:i33–6.
Huang JJ, Jiang WQ, Lin TY, Huang Y, Xu RH, Huang HQ, et al. Absolute lymphocyte count is novel prognostic indicator in extranodal natural killer/T-cell lymphoma, nasal type. Ann Oncol. 2011;22(1):149–55.
Cox MC, Nofroni I, Ruco L, Amodeo R, Ferrari A, La Verde G, et al. Low absolute lymphocyte count is a poor prognostic factor in diffuse large B-cell lymphoma. Leuk Lymphoma. 2008;49:745–51.
Porrata LF, Rsitow K, Inwards DJ, Ansell SM, Micallef IN, Johnston PB. Lymphopenia assessed during routine follow-up after immunochemotherapy (R-CHOP) is a risk factor for predicting relapse in patients with diffuse large B-cell lymphoma. Leukemia. 2010;24(7):1343–9.
Chan JK, Quintanilla-Martinez L, Ferry JA, Peh S-C. Extranodal NK/T-cell lymphoma, nasal type. In: Swerdlow SH, Campo E, Harris NL, et al., editors. WHO classification of tumours of haematopoietic and lymphoid tissues. Lyon: IARC; 2008. p. 285–8.
Wang L, Wang WD, Xia ZJ, Zhang YJ, Xiang J, Lu Y. Combination of gemcitabine, l-asparaginase, and oxaliplatin (GELOX) is superior to EPOCH or CHOP in thetreatment of patients with stage IE/IIE extranodal natural killer/T cell lymphoma: a retrospective study in a cohort of 227 patients with long-term follow-up. Med Oncol. 2014;31(3):860.
Cheson BD, Horning SJ, Coiffier B, et al. Report of an international workshop to standardize response criteria for non-Hodgkin’s lymphomas. NCI Sponsored International Working Group. J Clin Oncol. 1999;17:1244.
Thompson CA, Maurer MJ, Ghesquieres H, et al. Utility of post-therapy surveillance scans in DLBCL. J Clin Oncol. 2013;(suppl; abstr 8504).
Adami J, Gabel H, Lindelof B, et al. Cancer risk following organ transplantation: a nationwide cohort study in Sweden. Br J Cancer. 2003;89:1221–7.
Kim DH, Baek JH, Chae YS, et al. Absolute lymphocyte counts predicts response to chemotherapy and survival in diffuse large B-cell lymphoma. Leukemia. 2007;21:2227–30.
Wilcox RA, Ristow K, Habermann TM, et al. The absolute monocyte and lymphocyte prognostic score predicts survival and identifies high-risk patients in diffuse large-B-cell lymphoma. Leukemia. 2011;25(9):1502–9.
Porrata LF, Ristow KM, Habermann TM, et al. Peripheral blood absolute lymphocyte/monocyte ratio during rituximab, cyclophosphamide, doxorubicin, vincristine and prednisone treatment cycles predicts clinical outcomes in diffuse large B-cell lymphoma. Leuk Lymphoma. 2014 Mar 19.
Huang JJ, Li YJ, Xia Y, et al. Prognostic significance of peripheral monocyte count in patients with extranodal natural killer/T-cell lymphoma. BMC Cancer. 2013;13:222.
Habermann TM. Posttransplant lymphoproliferative disorders. Cancer Treat Res. 2008;142:273–92.
Wang L, Liao DZ, Zhang J, Xia ZJ, Peng XW, Lu Y. Clinical significance of serum soluble interleukin-2 receptor-α in extranodal natural killer/T-cell lymphoma (ENKTL): a predictive biomarker for treatment efficacy and valuable prognostic factor. Med Oncol. 2013;30(4):723.
Smith KA. Interleukin-2: inception, impact, and implications. Science. 1988;240:1169–76.
Acknowledgments
We thank all of the physicians at Sun Yat-sen University Cancer Center for allowing us to include their patients. We also appreciate the cooperation of all the pathologists at Sun Yat-sen University Cancer Center for their support.
Financial support
This work received grant support from National Natural Science Foundation of China (contract/grant number: 81400159), Medical Research Foundation of Guangdong Province (grant number: B2014158), Young Teachers’ Cultivation Project of Sun Yat-sen University (No. 12ykpy54), and Outstanding Young Talents Project of Sun Yat-sen University Cancer Center (No. 04190101#).
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wang, L., Wang, Jh., Wu-Xiao, Zj. et al. Lymphopenia during routine follow-up may predict relapse in patients with extranodal NK/T cell lymphoma. Tumor Biol. 36, 1747–1753 (2015). https://doi.org/10.1007/s13277-014-2776-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-014-2776-1