Abstract
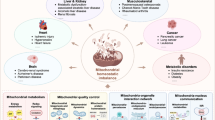
Diabetic cardiomyopathy describes decreased myocardial function in diabetic patients in the absence of other heart diseases such as myocardial ischemia and hypertension. Recent studies have defined numerous molecular interactions and signaling events that may account for deleterious changes in mitochondrial dynamics and functions influenced by hyperglycemic stress. A metabolic switch from glucose to fatty acid oxidation to fuel ATP synthesis, mitochondrial oxidative injury resulting from increased mitochondrial ROS production and decreased antioxidant capacity, enhanced mitochondrial fission and defective mitochondrial fusion, impaired mitophagy, and blunted mitochondrial biogenesis are major signatures of mitochondrial pathologies during diabetic cardiomyopathy. This review describes the molecular alterations underlying mitochondrial abnormalities associated with hyperglycemia and discusses their influence on cardiomyocyte viability and function. Based on basic research findings and clinical evidence, diabetic treatment standards and their impact on mitochondrial function, as well as mitochondria-targeted therapies of potential benefit for diabetic cardiomyopathy patients, are also summarized.



Similar content being viewed by others
References
Abdel-Raheem MH, Salim SU, Mosad E et al (2015) Antiapoptotic and antioxidant effects of carvedilol and vitamin E protect against diabetic nephropathy and cardiomyopathy in diabetic Wistar albino rats. Horm Metab Res 47:97–106. https://doi.org/10.1055/s-0034-1385855
Akinbiyi EO, Abramowitz LK, Bauer BL et al (2021) Blocked O-GlcNAc cycling alters mitochondrial morphology, function, and mass. Sci Rep 11:22106. https://doi.org/10.1038/s41598-021-01512-y
Alizadeh Pahlavani H (2022) Possible roles of exercise and apelin against pregnancy complications. Front Endocrinol (Lausanne) 13:965167. https://doi.org/10.3389/fendo.2022.965167
Alvarado-Vásquez N, Zapata E, Alcázar-Leyva S, Massó F, Montaño LF (2007) Reduced NO synthesis and eNOS mRNA expression in endothelial cells from newborns with a strong family history of type 2 diabetes. Diabetes Metab Res Rev 23:559–566. https://doi.org/10.1002/dmrr.743
Anderson EJ, Kypson AP, Rodriguez E et al (2009) Substrate-specific derangements in mitochondrial metabolism and redox balance in the atrium of the type 2 diabetic human heart. J Am Coll Cardiol 54:1891–1898. https://doi.org/10.1016/j.jacc.2009.07.031
Aon MA, Tocchetti CG, Bhatt N, Paolocci N, Cortassa S (2015) Protective mechanisms of mitochondria and heart function in diabetes. Antioxid Redox Signal 22:1563–1586. https://doi.org/10.1089/ars.2014.6123
Arkat S, Umbarkar P, Singh S, Sitasawad SL (2016) Mitochondrial peroxiredoxin-3 protects against hyperglycemia induced myocardial damage in diabetic cardiomyopathy. Free Radic Biol Med 97:489–500. https://doi.org/10.1016/j.freeradbiomed.2016.06.019
Ather S, Chan W, Bozkurt B et al (2012) Impact of noncardiac comorbidities on morbidity and mortality in a predominantly male population with heart failure and preserved versus reduced ejection fraction. J Am Coll Cardiol 59:998–1005. https://doi.org/10.1016/j.jacc.2011.11.040
Avagimyan A, Popov S, Shalnova S (2022) The pathophysiological basis of diabetic cardiomyopathy development. Curr Probl Cardiol 47:101156. https://doi.org/10.1016/j.cpcardiol.2022.101156
Belke DD, Betuing S, Tuttle MJ et al (2002) Insulin signaling coordinately regulates cardiac size, metabolism, and contractile protein isoform expression. J Clin Invest 109:629–639. https://doi.org/10.1172/jci13946
Bhansali S, Bhansali A, Dutta P, Walia R, Dhawan V (2020) Metformin upregulates mitophagy in patients with T2DM: a randomized placebo-controlled study. J Cell Mol Med 24:2832–2846. https://doi.org/10.1111/jcmm.14834
Bhatti JS, Sehrawat A, Mishra J et al (2022) Oxidative stress in the pathophysiology of type 2 diabetes and related complications: current therapeutics strategies and future perspectives. Free Radic Biol Med 184:114–134. https://doi.org/10.1016/j.freeradbiomed.2022.03.019
Boudina S, Sena S, Theobald H et al (2007) Mitochondrial energetics in the heart in obesity-related diabetes: direct evidence for increased uncoupled respiration and activation of uncoupling proteins. Diabetes 56:2457–2466. https://doi.org/10.2337/db07-0481
Bravo-San Pedro JM, Kroemer G, Galluzzi L (2017) Autophagy and mitophagy in cardiovascular disease. Circ Res 120:1812–1824. https://doi.org/10.1161/circresaha.117.311082
Brown GC, Borutaite V (2004) Inhibition of mitochondrial respiratory complex I by nitric oxide, peroxynitrite and S-nitrosothiols. Biochim Biophys Acta 1658:44–49. https://doi.org/10.1016/j.bbabio.2004.03.016
Buchanan J, Mazumder PK, Hu P et al (2005) Reduced cardiac efficiency and altered substrate metabolism precedes the onset of hyperglycemia and contractile dysfunction in two mouse models of insulin resistance and obesity. Endocrinology 146:5341–5349. https://doi.org/10.1210/en.2005-0938
Bugger H, Abel ED (2014) Molecular mechanisms of diabetic cardiomyopathy. Diabetologia 57:660–671. https://doi.org/10.1007/s00125-014-3171-6
Byrne NJ, Rajasekaran NS, Abel ED, Bugger H (2021) Therapeutic potential of targeting oxidative stress in diabetic cardiomyopathy. Free Radic Biol Med 169:317–342. https://doi.org/10.1016/j.freeradbiomed.2021.03.046
Cagnin S, Brugnaro M, Millino C et al (2022) Monoamine oxidase-dependent pro-survival signaling in diabetic hearts is mediated by miRNAs. Cells 11. https://doi.org/10.3390/cells11172697
Cai C, Guo Z, Chang X et al (2022a) Empagliflozin attenuates cardiac microvascular ischemia/reperfusion through activating the AMPKα1/ULK1/FUNDC1/mitophagy pathway. Redox Biol 52:102288. https://doi.org/10.1016/j.redox.2022.102288
Cai C, Wu F, He J et al (2022b) Mitochondrial quality control in diabetic cardiomyopathy: from molecular mechanisms to therapeutic strategies. Int J Biol Sci 18:5276–5290. https://doi.org/10.7150/ijbs.75402
Cai C, Wu F, Zhuang B et al (2022c) Empagliflozin activates Wnt/β-catenin to stimulate FUNDC1-dependent mitochondrial quality surveillance against type-3 cardiorenal syndrome. Mol Metab 64:101553. https://doi.org/10.1016/j.molmet.2022.101553
Cameron AR, Morrison VL, Levin D et al (2016) Anti-inflammatory effects of metformin irrespective of diabetes status. Circ Res 119:652–665. https://doi.org/10.1161/circresaha.116.308445
Celik T, Yuksel C, Iyisoy A (2010) Alpha tocopherol use in the management of diabetic cardiomyopathy: lessons learned from randomized clinical trials. J Diabetes Complications 24:286–288. https://doi.org/10.1016/j.jdiacomp.2009.02.005
Chandel NS, McClintock DS, Feliciano CE et al (2000) Reactive oxygen species generated at mitochondrial complex III stabilize hypoxia-inducible factor-1alpha during hypoxia: a mechanism of O2 sensing. J Biol Chem 275:25130–25138. https://doi.org/10.1074/jbc.M001914200
Chang X, Lochner A, Wang HH et al (2021) Coronary microvascular injury in myocardial infarction: perception and knowledge for mitochondrial quality control. Theranostics 11:6766–6785. https://doi.org/10.7150/thno.60143
Chang X, Li Y, Cai C et al (2022a) Mitochondrial quality control mechanisms as molecular targets in diabetic heart. Metabolism 137:155313. https://doi.org/10.1016/j.metabol.2022.155313
Chang X, Toan S, Li R, Zhou H (2022b) Therapeutic strategies in ischemic cardiomyopathy: focus on mitochondrial quality surveillance. EBioMedicine 84:104260. https://doi.org/10.1016/j.ebiom.2022.104260
Chen Y, Liu Y, and Dorn G W, 2nd (2011). Mitochondrial fusion is essential for organelle function and cardiac homeostasis. Circ Res 109:1327-1331. https://doi.org/10.1161/circresaha.111.258723.
Chen X, Zhang L, He H et al (2020) Increased O-GlcNAcylation induces myocardial hypertrophy. In Vitro Cell Dev Biol Anim 56:735–743. https://doi.org/10.1007/s11626-020-00503-z
Choi J, Ravipati A, Nimmagadda V et al (2014) Potential roles of PINK1 for increased PGC-1α-mediated mitochondrial fatty acid oxidation and their associations with Alzheimer disease and diabetes. Mitochondrion 18:41–48. https://doi.org/10.1016/j.mito.2014.09.005
Cividini F, Scott BT, Dai A et al (2016) O-GlcNAcylation of 8-oxoguanine DNA glycosylase (Ogg1) impairs oxidative mitochondrial DNA lesion repair in diabetic hearts. J Biol Chem 291:26515–26528. https://doi.org/10.1074/jbc.M116.754481
Czajka A, Ajaz S, Gnudi L et al (2015) Altered mitochondrial function, mitochondrial DNA and reduced metabolic flexibility in patients with diabetic nephropathy. EBioMedicine 2:499–512. https://doi.org/10.1016/j.ebiom.2015.04.002
Das Evcimen N, King GL (2007) The role of protein kinase C activation and the vascular complications of diabetes. Pharmacol Res 55:498–510. https://doi.org/10.1016/j.phrs.2007.04.016
De Geest B, Mishra M (2022) Role of oxidative stress in diabetic cardiomyopathy. Antioxidants (Basel) 11. https://doi.org/10.3390/antiox11040784
Derakhshanian H, Djazayery A, Javanbakht MH et al (2019) Vitamin D downregulates key genes of diabetes complications in cardiomyocyte. J Cell Physiol 234:21352–21358. https://doi.org/10.1002/jcp.28743
Dia M, Leon C, Chanon S, et al. (2022). Effect of metformin on T2D-induced MAM Ca(2+) uncoupling and contractile dysfunction in an early mouse model of diabetic HFpEF. Int J Mol Sci 23. 10.3390/ijms23073569.
Diao J, Wei J, Yan R et al (2019) Effects of resveratrol on regulation on UCP2 and cardiac function in diabetic rats. J Physiol Biochem 75:39–51. https://doi.org/10.1007/s13105-018-0648-7
Ding H, Zhang Y, Ma X et al (2022) Bariatric surgery for diabetic comorbidities: a focus on hepatic, cardiac and renal fibrosis. Front Pharmacol 13:1016635. https://doi.org/10.3389/fphar.2022.1016635
Dodd MS, Sousa Fialho MDL, Montes Aparicio CN et al (2018) Fatty acids prevent hypoxia-inducible factor-1α signaling through decreased succinate in diabetes. JACC Basic Transl Sci 3:485–498. https://doi.org/10.1016/j.jacbts.2018.04.005
Donahoe SM, Stewart GC, McCabe CH et al (2007) Diabetes and mortality following acute coronary syndromes. Jama 298:765–775. https://doi.org/10.1001/jama.298.7.765
Ducheix S, Magré J, Cariou B, Prieur X (2018) Chronic O-GlcNAcylation and diabetic cardiomyopathy: the bitterness of glucose. Front Endocrinol (Lausanne) 9:642. https://doi.org/10.3389/fendo.2018.00642
Durcan TM, Fon EA (2015) The three ‘P’s of mitophagy: PARKIN, PINK1, and post-translational modifications. Genes Dev 29:989–999. https://doi.org/10.1101/gad.262758.115
Fang WJ, Wang CJ, He Y et al (2018) Resveratrol alleviates diabetic cardiomyopathy in rats by improving mitochondrial function through PGC-1α deacetylation. Acta Pharmacol Sin 39:59–73. https://doi.org/10.1038/aps.2017.50
Frangogiannis NG (2019) Cardiac fibrosis: Cell biological mechanisms, molecular pathways and therapeutic opportunities. Mol Aspects Med 65:70–99. https://doi.org/10.1016/j.mam.2018.07.001
Fukushima K, Kitamura S, Tsuji K, Sang Y, Wada J (2020) Sodium glucose co-transporter 2 inhibitor ameliorates autophagic flux impairment on renal proximal tubular cells in obesity mice. Int J Mol Sci 21. https://doi.org/10.3390/ijms21114054
Gollmer J, Zirlik A, Bugger H (2020) Mitochondrial mechanisms in diabetic cardiomyopathy. Diabetes Metab J 44:33–53. https://doi.org/10.4093/dmj.2019.0185
Gu W, Geng J, Zhao H, Li X, Song G (2022) Effects of resveratrol on metabolic indicators in patients with type 2 diabetes: a systematic review and meta-analysis. Int J Clin Pract 2022:9734738. https://doi.org/10.1155/2022/9734738
Haffner SM, Lehto S, Rönnemaa T, Pyörälä K, Laakso M (1998) Mortality from coronary heart disease in subjects with type 2 diabetes and in nondiabetic subjects with and without prior myocardial infarction. N Engl J Med 339:229–234. https://doi.org/10.1056/nejm199807233390404
Hansen SS, Aasum E, Hafstad AD (2018) The role of NADPH oxidases in diabetic cardiomyopathy. Biochim Biophys Acta Mol Basis Dis 1864:1908–1913. https://doi.org/10.1016/j.bbadis.2017.07.025
Hausenblas HA, Schoulda JA, Smoliga JM (2015) Resveratrol treatment as an adjunct to pharmacological management in type 2 diabetes mellitus--systematic review and meta-analysis. Mol Nutr Food Res 59:147–159. https://doi.org/10.1002/mnfr.201400173
Hegab Z, Mohamed TMA, Stafford N et al (2017) Advanced glycation end products reduce the calcium transient in cardiomyocytes by increasing production of reactive oxygen species and nitric oxide. FEBS Open Bio 7:1672–1685. https://doi.org/10.1002/2211-5463.12284
Holman RR, Bethel MA, Mentz RJ et al (2017) Effects of once-weekly exenatide on cardiovascular outcomes in type 2 diabetes. N Engl J Med 377:1228–1239. https://doi.org/10.1056/NEJMoa1612917
Hu M, Ye P, Liao H, Chen M, Yang F (2016) Metformin protects H9C2 cardiomyocytes from high-glucose and hypoxia/reoxygenation injury via inhibition of reactive oxygen species generation and inflammatory responses: role of AMPK and JNK. J Diabetes Res 2016:2961954. https://doi.org/10.1155/2016/2961954
Hung CM, Lombardo PS, Malik N et al (2021) AMPK/ULK1-mediated phosphorylation of Parkin ACT domain mediates an early step in mitophagy. Sci Adv 7. https://doi.org/10.1126/sciadv.abg4544
Ikeda Y, Shirakabe A, Maejima Y et al (2015) Endogenous Drp1 mediates mitochondrial autophagy and protects the heart against energy stress. Circ Res 116:264–278. https://doi.org/10.1161/circresaha.116.303356
Jeffrey S, Samraj PI, Raj BS (2021) The role of alpha-lipoic acid supplementation in the prevention of diabetes complications: a comprehensive review of clinical trials. Curr Diabetes Rev 17:e011821190404. https://doi.org/10.2174/1573399817666210118145550
Jiménez-Cortegana C, Iglesias P, Ribalta J et al (2021) Nutrients and dietary approaches in patients with type 2 diabetes mellitus and cardiovascular disease: a narrative review. Nutrients 13. https://doi.org/10.3390/nu13114150
Jin SM, Youle RJ (2012) PINK1- and Parkin-mediated mitophagy at a glance. J Cell Sci 125:795–799. https://doi.org/10.1242/jcs.093849
Jin L, Geng L, Ying L et al (2022) FGF21-sirtuin 3 axis confers the protective effects of exercise against diabetic cardiomyopathy by governing mitochondrial integrity. Circulation 146:1537–1557. https://doi.org/10.1161/circulationaha.122.059631
Jubaidi FF, Zainalabidin S, Mariappan V, Budin SB (2020) Mitochondrial dysfunction in diabetic cardiomyopathy: the possible therapeutic roles of phenolic acids. Int J Mol Sci 21. https://doi.org/10.3390/ijms21176043
Kaludercic N, Di Lisa F (2020) Mitochondrial ROS formation in the pathogenesis of diabetic cardiomyopathy. Front Cardiovasc Med 7:12. https://doi.org/10.3389/fcvm.2020.00012
Kannel WB, Hjortland M, Castelli WP (1974) Role of diabetes in congestive heart failure: the Framingham study. Am J Cardiol 34:29–34. https://doi.org/10.1016/0002-9149(74)90089-7
Karwi QG, Zhang L, Altamimi TR et al (2019) Weight loss enhances cardiac energy metabolism and function in heart failure associated with obesity. Diabetes Obes Metab 21:1944–1955. https://doi.org/10.1111/dom.13762
Ketenci M, Zablocki D, Sadoshima J (2022) Mitochondrial quality control mechanisms during diabetic cardiomyopathy. Jma j 5:407–415. https://doi.org/10.31662/jmaj.2022-0155
Khang R, Park C, Shin JH (2015) Dysregulation of Parkin in the substantia nigra of db/db and high-fat diet mice. Neuroscience 294:182–192. https://doi.org/10.1016/j.neuroscience.2015.03.017
Kim HK, Ko TH, Song IS et al (2020) BH4 activates CaMKK2 and rescues the cardiomyopathic phenotype in rodent models of diabetes. Life Sci Alliance 3. https://doi.org/10.26508/lsa.201900619
Kobayashi S, Patel J, Zhao F et al (2020) Novel dual-fluorescent mitophagy reporter reveals a reduced mitophagy flux in type 1 diabetic mouse heart. J Am Osteopath Assoc 120:446–455. https://doi.org/10.7556/jaoa.2020.072
Koncsos G, Varga ZV, Baranyai T et al (2016) Diastolic dysfunction in prediabetic male rats: role of mitochondrial oxidative stress. Am J Physiol Heart Circ Physiol 311:H927–h943. https://doi.org/10.1152/ajpheart.00049.2016
Kruse R, Vind BF, Petersson SJ, Kristensen JM, Højlund K (2015) Markers of autophagy are adapted to hyperglycaemia in skeletal muscle in type 2 diabetes. Diabetologia 58:2087–2095. https://doi.org/10.1007/s00125-015-3654-0
Larsen TD, Sabey KH, Knutson AJ et al (2019) Diabetic pregnancy and maternal high-fat diet impair mitochondrial dynamism in the developing fetal rat heart by sex-specific mechanisms. Int J Mol Sci 20. https://doi.org/10.3390/ijms20123090
Lashin OM, Szweda PA, Szweda LI, Romani AM (2006) Decreased complex II respiration and HNE-modified SDH subunit in diabetic heart. Free Radic Biol Med 40:886–896. https://doi.org/10.1016/j.freeradbiomed.2005.10.040
Leopold JA, Cap A, Scribner AW, Stanton RC, Loscalzo J (2001) Glucose-6-phosphate dehydrogenase deficiency promotes endothelial oxidant stress and decreases endothelial nitric oxide bioavailability. FASEB J 15:1771–1773. https://doi.org/10.1096/fj.00-0893fje
Levelt E, Gulsin G, Neubauer S, McCann GP (2018) Mechanisms in endocrinology: diabetic cardiomyopathy: pathophysiology and potential metabolic interventions state of the art review. Eur J Endocrinol 178:R127–r139. https://doi.org/10.1530/eje-17-0724
Li A, Zhang S, Li J et al (2016) Metformin and resveratrol inhibit Drp1-mediated mitochondrial fission and prevent ER stress-associated NLRP3 inflammasome activation in the adipose tissue of diabetic mice. Mol Cell Endocrinol 434:36–47. https://doi.org/10.1016/j.mce.2016.06.008
Liesa M, Shirihai OS (2013) Mitochondrial dynamics in the regulation of nutrient utilization and energy expenditure. Cell Metab 17:491–506. https://doi.org/10.1016/j.cmet.2013.03.002
Li H, Xu C, Li Q et al (2017) Thioredoxin 2 offers protection against mitochondrial oxidative stress in H9c2 cells and against myocardial hypertrophy induced by hyperglycemia. Int J Mol Sci 18. https://doi.org/10.3390/ijms18091958
Lin CH, Kurup S, Herrero P et al (2011) Myocardial oxygen consumption change predicts left ventricular relaxation improvement in obese humans after weight loss. Obesity (Silver Spring) 19:1804–1812. https://doi.org/10.1038/oby.2011.186
Liu L, Yu S, Khan RS et al (2012) Diacylglycerol acyl transferase 1 overexpression detoxifies cardiac lipids in PPARγ transgenic mice. J Lipid Res 53:1482–1492. https://doi.org/10.1194/jlr.M024208
Liu XD, Li YG, Wang GY et al (2020) Metformin protects high glucose-cultured cardiomyocytes from oxidative stress by promoting NDUFA13 expression and mitochondrial biogenesis via the AMPK signaling pathway. Mol Med Rep 22:5262–5270. https://doi.org/10.3892/mmr.2020.11599
Lo MC, Chen MH, Lee WS et al (2015) Nε-(carboxymethyl) lysine-induced mitochondrial fission and mitophagy cause decreased insulin secretion from β-cells. Am J Physiol Endocrinol Metab 309:E829–E839. https://doi.org/10.1152/ajpendo.00151.2015
Lonn E, Bosch J, Yusuf S et al (2005) Effects of long-term vitamin E supplementation on cardiovascular events and cancer: a randomized controlled trial. Jama 293:1338–1347. https://doi.org/10.1001/jama.293.11.1338
Lu QB, Ding Y, Liu Y et al (2022) Metrnl ameliorates diabetic cardiomyopathy via inactivation of cGAS/STING signaling dependent on LKB1/AMPK/ULK1-mediated autophagy. J Adv Res. https://doi.org/10.1016/j.jare.2022.10.014
Madonna R, Moscato S, Cufaro MC et al (2023) Empagliflozin inhibits excessive autophagy through the AMPK/GSK3β signaling pathway in diabetic cardiomyopathy. Cardiovasc Res. https://doi.org/10.1093/cvr/cvad009
Ma N, Zhang Y (2022) Effects of resveratrol therapy on glucose metabolism, insulin resistance, inflammation, and renal function in the elderly patients with type 2 diabetes mellitus: a randomized controlled clinical trial protocol. Medicine (Baltimore) 101:e30049. https://doi.org/10.1097/md.0000000000030049
Ma G, Liu Y, Wang Y et al (2020) Liraglutide reduces hyperglycemia-induced cardiomyocyte death through activating glucagon-like peptide 1 receptor and targeting AMPK pathway. J Recept Signal Transduct Res 40:133–140. https://doi.org/10.1080/10799893.2020.1719517
Ma L, Zou R, Shi W et al (2022) SGLT2 inhibitor dapagliflozin reduces endothelial dysfunction and microvascular damage during cardiac ischemia/reperfusion injury through normalizing the XO-SERCA2-CaMKII-coffilin pathways. Theranostics 12:5034–5050. https://doi.org/10.7150/thno.75121
Ma XM, Geng K, Law BY et al (2023) Lipotoxicity-induced mtDNA release promotes diabetic cardiomyopathy by activating the cGAS-STING pathway in obesity-related diabetes. Cell Biol Toxicol 39:277–299. https://doi.org/10.1007/s10565-021-09692-z
Maalouf RM, Eid AA, Gorin YC et al (2012) Nox4-derived reactive oxygen species mediate cardiomyocyte injury in early type 1 diabetes. Am J Physiol Cell Physiol 302:C597–C604. https://doi.org/10.1152/ajpcell.00331.2011
Mahjabeen W, Khan DA, Mirza SA (2022) Role of resveratrol supplementation in regulation of glucose hemostasis, inflammation and oxidative stress in patients with diabetes mellitus type 2: a randomized, placebo-controlled trial. Complement Ther Med 66:102819. https://doi.org/10.1016/j.ctim.2022.102819
Mailleux F, Gélinas R, Beauloye C, Horman S, Bertrand L (2016) O-GlcNAcylation, enemy or ally during cardiac hypertrophy development? Biochim Biophys Acta 1862:2232–2243. https://doi.org/10.1016/j.bbadis.2016.08.012
Makrecka-Kuka M, Korzh S, Videja M et al (2020) Empagliflozin protects cardiac mitochondrial fatty acid metabolism in a mouse model of diet-induced lipid overload. Cardiovasc Drugs Ther 34:791–797. https://doi.org/10.1007/s10557-020-06989-9
Manninger M, Zweiker D, Dobrovnik M et al (2020) Acute hyperglycaemia is not associated with the development of atrial fibrillation in healthy pigs. Sci Rep 10:11881. https://doi.org/10.1038/s41598-020-68897-0
Marso SP, Daniels GH, Brown-Frandsen K et al (2016) Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med 375:311–322. https://doi.org/10.1056/NEJMoa1603827
Matsushima S, Kinugawa S, Ide T et al (2006) Overexpression of glutathione peroxidase attenuates myocardial remodeling and preserves diastolic function in diabetic heart. Am J Physiol Heart Circ Physiol 291:H2237–H2245. https://doi.org/10.1152/ajpheart.00427.2006
Mercer JR, Yu E, Figg N et al (2012) The mitochondria-targeted antioxidant MitoQ decreases features of the metabolic syndrome in ATM+/-/ApoE-/- mice. Free Radic Biol Med 52:841–849. https://doi.org/10.1016/j.freeradbiomed.2011.11.026
Montaigne D, Marechal X, Coisne A et al (2014) Myocardial contractile dysfunction is associated with impaired mitochondrial function and dynamics in type 2 diabetic but not in obese patients. Circulation 130:554–564. https://doi.org/10.1161/circulationaha.113.008476
Morales PE, Arias-Durán C, Ávalos-Guajardo Y et al (2020) Emerging role of mitophagy in cardiovascular physiology and pathology. Mol Aspects Med 71:100822. https://doi.org/10.1016/j.mam.2019.09.006
Mu J, Zhang D, Tian Y, Xie Z, Zou MH (2020) BRD4 inhibition by JQ1 prevents high-fat diet-induced diabetic cardiomyopathy by activating PINK1/Parkin-mediated mitophagy in vivo. J Mol Cell Cardiol 149:1–14. https://doi.org/10.1016/j.yjmcc.2020.09.003
Mughal W, Nguyen L, Pustylnik S et al (2015) A conserved MADS-box phosphorylation motif regulates differentiation and mitochondrial function in skeletal, cardiac, and smooth muscle cells. Cell Death Dis 6:e1944. https://doi.org/10.1038/cddis.2015.306
Nakai A, Yamaguchi O, Takeda T et al (2007) The role of autophagy in cardiomyocytes in the basal state and in response to hemodynamic stress. Nat Med 13:619–624. https://doi.org/10.1038/nm1574
Naruse G, Kanamori H, Yoshida A et al (2019) The intestine responds to heart failure by enhanced mitochondrial fusion through glucagon-like peptide-1 signalling. Cardiovasc Res 115:1873–1885. https://doi.org/10.1093/cvr/cvz002
Neal B, Perkovic V, Mahaffey KW et al (2017) Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med 377:644–657. https://doi.org/10.1056/NEJMoa1611925
Ni R, Cao T, Xiong S et al (2016) Therapeutic inhibition of mitochondrial reactive oxygen species with mito-TEMPO reduces diabetic cardiomyopathy. Free Radic Biol Med 90:12–23. https://doi.org/10.1016/j.freeradbiomed.2015.11.013
Nishikawa T, Araki E (2013) Mechanism-based antioxidant therapies promise to prevent diabetic complications? J Diabetes Investig 4:105–107. https://doi.org/10.1111/jdi.12041
Oberstein A, Jeffrey PD, Shi Y (2007) Crystal structure of the Bcl-XL-Beclin 1 peptide complex: Beclin 1 is a novel BH3-only protein. J Biol Chem 282:13123–13132. https://doi.org/10.1074/jbc.M700492200
Ohtake T, Yokoyama I, Watanabe T et al (1995) Myocardial glucose metabolism in noninsulin-dependent diabetes mellitus patients evaluated by FDG-PET. J Nucl Med 36:456–463
Ongwijitwat S, Wong-Riley MT (2005) Is nuclear respiratory factor 2 a master transcriptional coordinator for all ten nuclear-encoded cytochrome c oxidase subunits in neurons? Gene 360:65–77. https://doi.org/10.1016/j.gene.2005.06.015
Pan M, Han Y, Basu A et al (2018) Overexpression of hexokinase 2 reduces mitochondrial calcium overload in coronary endothelial cells of type 2 diabetic mice. Am J Physiol Cell Physiol 314:C732–c740. https://doi.org/10.1152/ajpcell.00350.2017
Parra V, Verdejo HE, Iglewski M et al (2014) Insulin stimulates mitochondrial fusion and function in cardiomyocytes via the Akt-mTOR-NFκB-Opa-1 signaling pathway. Diabetes 63:75–88. https://doi.org/10.2337/db13-0340
Peng X, Chen S, Wang Y et al (2022) SGLT2i reduces renal injury by improving mitochondrial metabolism and biogenesis. Mol Metab:101613. https://doi.org/10.1016/j.molmet.2022.101613
Peterson LR, Herrero P, Schechtman KB et al (2004) Effect of obesity and insulin resistance on myocardial substrate metabolism and efficiency in young women. Circulation 109:2191–2196. https://doi.org/10.1161/01.Cir.0000127959.28627.F8
Peterson LR, Saeed IM, McGill JB et al (2012) Sex and type 2 diabetes: obesity-independent effects on left ventricular substrate metabolism and relaxation in humans. Obesity (Silver Spring) 20:802–810. https://doi.org/10.1038/oby.2011.208
Pruett JE, Everman SJ, Hoang NH et al (2022) Mitochondrial function and oxidative stress in white adipose tissue in a rat model of PCOS: effect of SGLT2 inhibition. Biol Sex Differ 13:45. https://doi.org/10.1186/s13293-022-00455-x
Puigserver P, Wu Z, Park CW et al (1998) A cold-inducible coactivator of nuclear receptors linked to adaptive thermogenesis. Cell 92:829–839. https://doi.org/10.1016/s0092-8674(00)81410-5
Qin CX, Sleaby R, Davidoff AJ et al (2017) Insights into the role of maladaptive hexosamine biosynthesis and O-GlcNAcylation in development of diabetic cardiac complications. Pharmacol Res 116:45–56. https://doi.org/10.1016/j.phrs.2016.12.016
Rijzewijk LJ, van der Meer RW, Lamb HJ et al (2009) Altered myocardial substrate metabolism and decreased diastolic function in nonischemic human diabetic cardiomyopathy: studies with cardiac positron emission tomography and magnetic resonance imaging. J Am Coll Cardiol 54:1524–1532. https://doi.org/10.1016/j.jacc.2009.04.074
Rubler S, Dlugash J, Yuceoglu YZ et al (1972) New type of cardiomyopathy associated with diabetic glomerulosclerosis. Am J Cardiol 30:595–602. https://doi.org/10.1016/0002-9149(72)90595-4
Salau VF, Erukainure OL, Olofinsan KA et al (2023) Ferulic acid mitigates diabetic cardiomyopathy via modulation of metabolic abnormalities in cardiac tissues of diabetic rats. Fundam Clin Pharmacol 37:44–59. https://doi.org/10.1111/fcp.12819
Sammy MJ, Connelly AW, Brown JA et al (2021) Mito-Mendelian interactions alter in vivo glucose metabolism and insulin sensitivity in healthy mice. Am J Physiol Endocrinol Metab 321:E521–e529. https://doi.org/10.1152/ajpendo.00069.2021
Sesso HD, Buring JE, Christen WG et al (2008) Vitamins E and C in the prevention of cardiovascular disease in men: the Physicians’ Health Study II randomized controlled trial. JAMA 300:2123–2133. https://doi.org/10.1001/jama.2008.600
Shen X, Zheng S, Metreveli NS, Epstein PN (2006) Protection of cardiac mitochondria by overexpression of MnSOD reduces diabetic cardiomyopathy. Diabetes 55:798–805. https://doi.org/10.2337/diabetes.55.03.06.db05-1039
Smirnova E, Griparic L, Shurland DL, van der Bliek AM (2001) Dynamin-related protein Drp1 is required for mitochondrial division in mammalian cells. Mol Biol Cell 12:2245–2256. https://doi.org/10.1091/mbc.12.8.2245
Sun X, Chen RC, Yang ZH et al (2014) Taxifolin prevents diabetic cardiomyopathy in vivo and in vitro by inhibition of oxidative stress and cell apoptosis. Food Chem Toxicol 63:221–232. https://doi.org/10.1016/j.fct.2013.11.013
Sun Y, Teng Z, Sun X et al (2019) Exogenous H(2)S reduces the acetylation levels of mitochondrial respiratory enzymes via regulating the NAD(+)-SIRT3 pathway in cardiac tissues of db/db mice. Am J Physiol Endocrinol Metab 317:E284–e297. https://doi.org/10.1152/ajpendo.00326.2018
Sun D, Wang J, Toan S et al (2022) Molecular mechanisms of coronary microvascular endothelial dysfunction in diabetes mellitus: focus on mitochondrial quality surveillance. Angiogenesis 25:307–329. https://doi.org/10.1007/s10456-022-09835-8
Tan Y, Mui D, Toan S et al (2020) SERCA overexpression improves mitochondrial quality control and attenuates cardiac microvascular ischemia-reperfusion injury. Mol Ther Nucleic Acids 22:696–707. https://doi.org/10.1016/j.omtn.2020.09.013
Tan M, Yin Y, Ma X et al (2023) Glutathione system enhancement for cardiac protection: pharmacological options against oxidative stress and ferroptosis. Cell Death Dis 14:131. https://doi.org/10.1038/s41419-023-05645-y
Tao L, Huang X, Xu M, Yang L, Hua F (2020) MiR-144 protects the heart from hyperglycemia-induced injury by regulating mitochondrial biogenesis and cardiomyocyte apoptosis. FASEB J 34:2173–2197. https://doi.org/10.1096/fj.201901838R
Taye A, Abouzied MM, Mohafez OM (2013) Tempol ameliorates cardiac fibrosis in streptozotocin-induced diabetic rats: role of oxidative stress in diabetic cardiomyopathy. Naunyn Schmiedebergs Arch Pharmacol 386:1071–1080. https://doi.org/10.1007/s00210-013-0904-x
Tocchetti CG, Caceres V, Stanley BA et al (2012) GSH or palmitate preserves mitochondrial energetic/redox balance, preventing mechanical dysfunction in metabolically challenged myocytes/hearts from type 2 diabetic mice. Diabetes 61:3094–3105. https://doi.org/10.2337/db12-0072
Tong M, Saito T, Zhai P et al (2019) Mitophagy is essential for maintaining cardiac function during high fat diet-induced diabetic cardiomyopathy. Circ Res 124:1360–1371. https://doi.org/10.1161/circresaha.118.314607
Unuofin JO, Lebelo SL (2020) Antioxidant effects and mechanisms of medicinal plants and their bioactive compounds for the prevention and treatment of type 2 diabetes: an updated review. Oxid Med Cell Longev 2020:1356893. https://doi.org/10.1155/2020/1356893
Vincow ES, Merrihew G, Thomas RE et al (2013) The PINK1-Parkin pathway promotes both mitophagy and selective respiratory chain turnover in vivo. Proc Natl Acad Sci U S A 110:6400–6405. https://doi.org/10.1073/pnas.1221132110
Wang J, Zhou H (2020) Mitochondrial quality control mechanisms as molecular targets in cardiac ischemia-reperfusion injury. Acta Pharm Sin B 10:1866–1879. https://doi.org/10.1016/j.apsb.2020.03.004
Wang P, Lloyd SG, Zeng H, Bonen A, Chatham JC (2005) Impact of altered substrate utilization on cardiac function in isolated hearts from Zucker diabetic fatty rats. Am J Physiol Heart Circ Physiol 288:H2102–H2110. https://doi.org/10.1152/ajpheart.00935.2004
Wang F, Fisher SA, Zhong J, Wu Y, Yang P (2015) Superoxide dismutase 1 in vivo ameliorates maternal diabetes mellitus-induced apoptosis and heart defects through restoration of impaired Wnt signaling. Circ Cardiovasc Genet 8:665–676. https://doi.org/10.1161/circgenetics.115.001138
Wang Q, Zhang M, Torres G et al (2017) Metformin suppresses diabetes-accelerated atherosclerosis via the inhibition of Drp1-mediated mitochondrial fission. Diabetes 66:193–205. https://doi.org/10.2337/db16-0915
Wang S, Zhao Z, Fan Y et al (2019) Mst1 inhibits Sirt3 expression and contributes to diabetic cardiomyopathy through inhibiting Parkin-dependent mitophagy. Biochim Biophys Acta Mol Basis Dis 1865:1905–1914. https://doi.org/10.1016/j.bbadis.2018.04.009
Wang J, Toan S, Zhou H (2020a) Mitochondrial quality control in cardiac microvascular ischemia-reperfusion injury: new insights into the mechanisms and therapeutic potentials. Pharmacol Res 156:104771. https://doi.org/10.1016/j.phrs.2020.104771
Wang J, Zhu P, Li R et al (2020b) Bax inhibitor 1 preserves mitochondrial homeostasis in acute kidney injury through promoting mitochondrial retention of PHB2. Theranostics 10:384–397. https://doi.org/10.7150/thno.40098
Wang J, Zhu P, Toan S et al (2020c) Pum2-Mff axis fine-tunes mitochondrial quality control in acute ischemic kidney injury. Cell Biol Toxicol 36:365–378. https://doi.org/10.1007/s10565-020-09513-9
Wang D, Yin Y, Wang S et al (2021a) FGF1(ΔHBS) prevents diabetic cardiomyopathy by maintaining mitochondrial homeostasis and reducing oxidative stress via AMPK/Nur77 suppression. Signal Transduct Target Ther 6:133. https://doi.org/10.1038/s41392-021-00542-2
Wang F, Zhang D, Zhang D, Li P, Gao Y (2021b) Mitochondrial protein translation: emerging roles and clinical significance in disease. Front Cell Dev Biol 9:675465. https://doi.org/10.3389/fcell.2021.675465
Wang Y, Jasper H, Toan S et al (2021c) Mitophagy coordinates the mitochondrial unfolded protein response to attenuate inflammation-mediated myocardial injury. Redox Biol 45:102049. https://doi.org/10.1016/j.redox.2021.102049
Wang S, Zhu H, Li R et al (2022) DNA-PKcs interacts with and phosphorylates Fis1 to induce mitochondrial fragmentation in tubular cells during acute kidney injury. Sci Signal 15:eabh1121. https://doi.org/10.1126/scisignal.abh1121
Wiviott SD, Raz I, Bonaca MP et al (2019) Dapagliflozin and cardiovascular outcomes in type 2 diabetes. N Engl J Med 380:347–357. https://doi.org/10.1056/NEJMoa1812389
Wu QR, Zheng DL, Liu PM et al (2021) High glucose induces Drp1-mediated mitochondrial fission via the Orai1 calcium channel to participate in diabetic cardiomyocyte hypertrophy. Cell Death Dis 12:216. https://doi.org/10.1038/s41419-021-03502-4
Wu D, Yan L, Zheng C et al (2022) Akt-GSK3β-mPTP pathway regulates the mitochondrial dysfunction contributing to odontoblasts apoptosis induced by glucose oxidative stress. Cell Death Discov 8:168. https://doi.org/10.1038/s41420-022-00981-y
Xu X, Kobayashi S, Chen K et al (2013) Diminished autophagy limits cardiac injury in mouse models of type 1 diabetes. J Biol Chem 288:18077–18092. https://doi.org/10.1074/jbc.M113.474650
Xu K, Liu XF, Ke ZQ et al (2018) Resveratrol modulates apoptosis and autophagy induced by high glucose and palmitate in cardiac cells. Cell Physiol Biochem 46:2031–2040. https://doi.org/10.1159/000489442
Yan W, Zhang H, Liu P et al (2013) Impaired mitochondrial biogenesis due to dysfunctional adiponectin-AMPK-PGC-1α signaling contributing to increased vulnerability in diabetic heart. Basic Res Cardiol 108:329. https://doi.org/10.1007/s00395-013-0329-1
Ye G, Metreveli NS, Donthi RV et al (2004) Catalase protects cardiomyocyte function in models of type 1 and type 2 diabetes. Diabetes 53:1336–1343. https://doi.org/10.2337/diabetes.53.5.1336
Yu T, Robotham JL, Yoon Y (2006) Increased production of reactive oxygen species in hyperglycemic conditions requires dynamic change of mitochondrial morphology. Proc Natl Acad Sci U S A 103:2653–2658. https://doi.org/10.1073/pnas.0511154103
Yu J, He J, Yang W et al (2021) Diabetes impairs the protective effects of sevoflurane postconditioning in the myocardium subjected to ischemia/ reperfusion injury in rats: important role of Drp1. BMC Cardiovasc Disord 21:96. https://doi.org/10.1186/s12872-021-01906-w
Yu Q, Zhao G, Liu J et al (2023) The role of histone deacetylases in cardiac energy metabolism in heart diseases. Metabolism 142:155532. https://doi.org/10.1016/j.metabol.2023.155532
Yuan Q, Sun Y, Yang F et al (2023) CircRNA DICAR as a novel endogenous regulator for diabetic cardiomyopathy and diabetic pyroptosis of cardiomyocytes. Signal Transduct Target Ther 8:99. https://doi.org/10.1038/s41392-022-01306-2
Zhan M, Usman IM, Sun L, Kanwar YS (2015) Disruption of renal tubular mitochondrial quality control by Myo-inositol oxygenase in diabetic kidney disease. J Am Soc Nephrol 26:1304–1321. https://doi.org/10.1681/asn.2014050457
Zhang L, Li C, Zhu Q, Li N, Zhou H (2019) Liraglutide, a glucagon-like peptide-1 analog, inhibits high glucose-induced oxidative stress and apoptosis in neonatal rat cardiomyocytes. Exp Ther Med 17:3734–3740. https://doi.org/10.3892/etm.2019.7388
Zhang T, He Q, Liu Y, Chen Z, Hu H (2021) Efficacy and safety of resveratrol supplements on blood lipid and blood glucose control in patients with type 2 diabetes: a systematic review and meta-analysis of randomized controlled trials. Evid Based Complement Alternat Med 2021:5644171. https://doi.org/10.1155/2021/5644171
Zhang Y, Cao Y, Zheng R et al (2022) Fibroblast-specific activation of Rnd3 protects against cardiac remodeling in diabetic cardiomyopathy via suppression of Notch and TGF-β signaling. Theranostics 12:7250–7266. https://doi.org/10.7150/thno.77043
Zhang Z, Huang Q, Zhao D et al (2023) The impact of oxidative stress-induced mitochondrial dysfunction on diabetic microvascular complications. Front Endocrinol (Lausanne) 14:1112363. https://doi.org/10.3389/fendo.2023.1112363
Zhou H, Wang S, Zhu P et al (2018) Empagliflozin rescues diabetic myocardial microvascular injury via AMPK-mediated inhibition of mitochondrial fission. Redox Biol 15:335–346. https://doi.org/10.1016/j.redox.2017.12.019
Zhou H, Toan S, Zhu P et al (2020) DNA-PKcs promotes cardiac ischemia reperfusion injury through mitigating BI-1-governed mitochondrial homeostasis. Basic Res Cardiol 115:11. https://doi.org/10.1007/s00395-019-0773-7
Zhou H, Ren J, Toan S, Mui D (2021) Role of mitochondrial quality surveillance in myocardial infarction: from bench to bedside. Ageing Res Rev 66:101250. https://doi.org/10.1016/j.arr.2020.101250
Zhu H, Toan S, Mui D, Zhou H (2021) Mitochondrial quality surveillance as a therapeutic target in myocardial infarction. Acta Physiol (Oxf) 231:e13590. https://doi.org/10.1111/apha.13590
Zinman B, Wanner C, Lachin JM et al (2015) Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med 373:2117–2128. https://doi.org/10.1056/NEJMoa1504720
Zhou H, Toan S (2020) Pathological roles of mitochondrial oxidative stress and mitochondrial dynamics in cardiac microvascular ischemia/reperfusion injury. Biomolecules 10. https://doi.org/10.3390/biom10010085
Zorov DB, Juhaszova M, Sollott SJ (2014) Mitochondrial reactive oxygen species (ROS) and ROS-induced ROS release. Physiol Rev 94:909–950. https://doi.org/10.1152/physrev.00026.2013
Zou R, Shi W, Qiu J et al (2022a) Empagliflozin attenuates cardiac microvascular ischemia/reperfusion injury through improving mitochondrial homeostasis. Cardiovasc Diabetol 21:106. https://doi.org/10.1186/s12933-022-01532-6
Zou R, Tao J, Qiu J et al (2022b) DNA-PKcs promotes sepsis-induced multiple organ failure by triggering mitochondrial dysfunction. J Adv Res. https://doi.org/10.1016/j.jare.2022.01.014
Funding
This study was financially supported by grants from the National Natural Science Foundation of China (Nos. 82270279, 82200296, and 82170241) and Special Program for Training Outstanding Young Talents of Chinese Academy of Traditional Chinese Medicine (ZZ16-YQ-021) and Innovative Cultivation Project of Guang’anmen Hospital, Chinese Academy of Chinese Medical Sciences (2022s481). The funders had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhi, F., Zhang, Q., Liu, L. et al. Novel insights into the role of mitochondria in diabetic cardiomyopathy: molecular mechanisms and potential treatments. Cell Stress and Chaperones 28, 641–655 (2023). https://doi.org/10.1007/s12192-023-01361-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12192-023-01361-w